Research Article Open Access
Integrating Palliative Care in Life-Limiting Pediatric Neuromuscular Conditions: The Case of SMA-Type 1 and Duchene Muscular Dystrophy
Cynda H. Rushton1,2,3*, Lori H. Erby4, Ronald D. Cohn2,5,6 and Gail Geller2,3,4,6,71School of Nursing, Johns Hopkins University, Baltimore, MD, USA
2Department of Pediatrics, Johns Hopkins University School of Medicine, Baltimore, MD, USA
3Berman Institute of Bioethics, Johns Hopkins University, Baltimore, MD, USA
4Department of Health, Behavior & Society, Johns Hopkins University Bloomberg School of Public Health, Baltimore, MD, USA
5Department of Neurology, Johns Hopkins University School of Medicine, Baltimore, MD, USA
6McKusick-Nathans Institute of Genetic Medicine, Johns Hopkins University School of Medicine, Baltimore, MD, USA
7Department of Medicine, Johns Hopkins University School of Medicine, Baltimore, MD, USA
- *Corresponding Author:
- Dr. Cynda H. Rushton
School of Nursing, Johns Hopkins University
615 N. Wolfe St., Room 420
Baltimore, MD 21205, USA
Tel: (410) 614-2223
Fax: (410) 502-5481
E-mail: crushton@son.jhmi.edu
Received date: November 12, 2011; Accepted date: January 02, 2012; Published date: January 10, 2012
Citation: Rushton CH, Erby LH, Cohn RD, Geller G (2012) Integrating Palliative Care in Life-Limiting Pediatric Neuromuscular Conditions: The Case of SMA-Type 1 and Duchene Muscular Dystrophy. J Palliative Care Med 2:103. doi:10.4172/2165-7386.1000103
Copyright: ©2012 Rushton CH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Palliative Care & Medicine
Keywords
Pediatric palliative care; Duchenne muscular dystrophy; Spinal muscular atrophy type 1; Quality of life; Interdisciplinary working group
Introduction
Spinal Muscular Atrophy Type I (SMA-1) and Duchenne Muscular Dystrophy (DMD) are the two most common inherited pediatric lifethreatening neuromuscular disorders (NMDs) worldwide [1,2]. Both are fatal, but each is unique. Children with SMA-1 develop symptoms shortly after birth and usually die by age 2 [3], while boys with DMD manifest symptoms in pre- and early school years. Advances in respiratory and cardiac management [4,5] allow DMD patients to live into their 20’s, but their burden of disease is high, commensurate with the amount of weakness, and they often undergo major operations or require extended hospitalizations for routine childhood illnesses [6].
In both SMA-1 and DMD, the ability of children to comprehend their illness depends on their stage of development and their parents’ confidence in addressing their needs. Clinicians find it difficult to predict when affected children will die. These uncertainties and the availability of technologies to extend the lifespan of patients with NMDs [6-10] necessitate frequent clinical management decisions as the disease progresses.
Treatment decisions are complicated by the fragmented, highly specialized nature of the care these young patients receive [11,12]. Specialists may be unaccustomed to coordinating their efforts and have divergent approaches to clinical management. Recommendations for interventions, such as mechanical ventilation for children with SMA-1, vary widely; as a result [13], families working with several specialists may receive conflicting information.
These realities have fueled interest in applying the principles of palliative care, broadly understood, in the context of pediatric NMDs [11,12,14-16]. A holistic interdisciplinary model of care, palliative care integrates emotional, spiritual, developmental, and physical dimensions into the care of individuals living with life-limiting diseases [17-20]. Emerging from the hospice movement, palliative care first focused on end-of-life care, primarily in adult oncology and critical care settings. Now considered a model to relieve suffering and improve quality of life, as shown in (Figure 1), palliative care has expanded to include comprehensive care from the time of diagnosis of a variety of incurable, progressive diseases that may be life-limiting [21], including chronic pediatric diseases [22] such as HIV, cancer [23-26], and sickle cell disease [27-28]. The Association of Children’s Palliative Care has identified four categories of patients with life-limiting conditions who may benefit from palliative care [29]. These are reflected in (Table 1). Pediatric patients with conditions such as those with SMA-1 and DMD fall into the category of patients where premature death is inevitable. Although the timing of death varies by disease, their treatment is likely punctuated by periods of intensive life-prolonging treatment and full or partial resumption of prior activities and functional status. (Group 2). Arguably, these children could also be included in the group of children (Group 3) with progressive conditions without curative options where the focus is on the palliation, rather than cure, for their life span.
| Group 1 | “Curative treatment is feasible but can fail” |
| Group 2 | “Premature death is inevitable” |
| Group 3 | “Progressive conditions without curative treatment options” |
| Group 4 | “Irreversible but non-progressive conditions causing severe disability, leading to susceptibility to health complications and likelihood of premature death.” |
Table 1: Definitions of Life-Limiting Conditions [29].
The next horizon in palliative care is to integrate it more completely into managing other progressive, life-limiting conditions of childhood such as NMDs [30-31]. Because it is difficult to predict the rate and severity of disease progression in SMA-1 and DMD, the challenge is to offer guidance for living with these disorders. Pediatric palliative care (PPC) complements care with curative intent and offers support for the child and family as the disease progresses [20]. With no cures for DMD and SMA-1 currently available, the focus of care is necessarily palliation. Some specialists are integrating palliative care into the care of children with advanced forms/ manifestations of NMDs [4,5,32,33]. However, many are not for several reasons: the broader notion of palliative care is not included in their education and training; formal collaboration with palliative care specialists has been inadequate to date; and systems of care reinforce hierarchical rather than relational models of interaction-a key feature of palliative care.
Reaching this new horizon requires better understanding of the progression and critical decision points of NMDs, and training for clinicians to raise their awareness and create new knowledge and skills they can apply to the integration of PPC practices [34-35].
Methods
To advance palliative care integration, we formed an international consortium of patients and families affected by NMDs and an interdisciplinary group of clinicians who care for these families. We had three goals: identify transitions in disease progression; explore the challenges facing patients, families, and clinicians during these transitions; and identify opportunities for integrating PPC into the care of children affected by these conditions. The clinical focus of the consortium was on SMA-1 and DMD, both life-limiting NMDs punctuated by life-threatening events but significantly different in onset and duration.
One of the consortium’s activities was a summit, called “Heartsongs” in honor of Mattie J.T. Stepanek [36]. Held in Leeds, England, from April 16-19, 2008, the summit included “ambassadorial teams” of neuromuscular specialists, palliative care clinicians, and other health professionals (physical and occupational therapists, social workers, etc.), together with parents of affected children and representatives of muscular dystrophy associations from seven countries. Selection criteria for team members included leadership experience, commitment to improving care for children with NMDs, and willingness to explore palliative care integration and new models of engagement (Table 2).
| Countries | Australia | England | |||
| Canada | France | ||||
| Denmark (for Scandinavia) | Greece | ||||
| United States | |||||
| Selection Criteria |
|
||||
| Composition | |||||
| Discipline/Role | NMD Focus | PC Focus | TOTAL N | ||
| Nurses | 3 | 5 | 8 | ||
| Physicians | 8 | 7 | 15 | ||
| OT/PT | 5 | 4 | 9 | ||
| Psychologist/ Social Worker/ Counselor/ Social Scientist |
5 | 3 | 8 | ||
| Parents | 5 | 5 | |||
| MDA Representatives | 8 | 8 | |||
| Total N | 34 | 19 | 53 | ||
Table 2: Description of Participants.
To foster dialogue, the summit first divided participants into two groups, one for SMA-1, one for DMD. Drawing on the concept of disease trajectories in genetic conditions [30,31], each group described the typical trajectory for their respective condition, identified transition points, and created a visual representation of the trajectory.
The rest of the summit involved group discussions led by interdisciplinary professionals who were experienced facilitators. Based on their experience and expertise, participants were assigned to six groups, three focused on SMA-1, three on DMD. All six groups addressed elements of palliative care, with one group from each disease focused on (1) communication and decision making, (2) ethical and cultural challenges, and (3) pain/suffering and spiritual care.
Results
A total of 53 interdisciplinary professionals and families, including the project team, attended the summit. As shown in (Table 2), 40% of the participants were clinicians with expertise in pediatric NMDs, 35% were specialists in PPC, and 25% were patients and family members or their advocates. Among the parents were those who had lost a child and those whose children were still living.
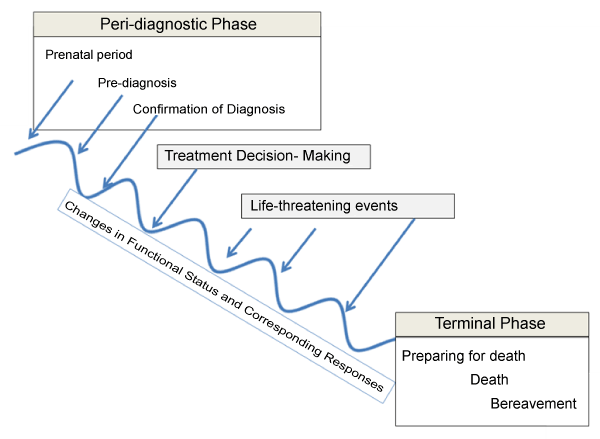
Participants identified four phases, predictable in sequence but variable in duration and velocity, in the life trajectories for children and families affected by SMA-1 and DMD, as depicted in (Figure 2).
The peri-diagnostic phase encompasses a long process that may begin prenatally, at birth, or during childhood. There may be suspicions that the fetus is abnormal before birth, if parents already have an affected child or non-specific findings such as ultrasound abnormalities are detected. Families characterize this process as an “odyssey” marked by uncertainty, anxiety, grief, and loss.
The treatment decision-making phase focuses on managing symptoms, optimizing function, enhancing quality of life, and monitoring developmental progress. It involves initiating treatments (possibly enrollment in a clinical trial) to slow the disease progression and anticipating life-threatening events that will require decision making. These decisions present a range of ethical considerations, such as whether to undergo genetic testing or involve their children in decision making.
The third phase involves life-threatening events such as respiratory failure, sepsis, and pneumonia. Life-sustaining therapies including mechanical ventilation, medications, or other invasive technologies are initiated; periodic discussions regarding their continuation follow. Each event creates uncertainty: can the child’s functional status be restored or does the latest crisis represent irreversible disease progression? Families characterize this phase as a “roller coaster ride”, accompanied by a resurgence of grief and loss. Eventually, life-sustaining therapies lose their efficacy, and dying seems inevitable.
The terminal phase involves a relatively predictable trajectory, although the length of the dying process is variable, especially for children with DMD who may live into their 20s, creating uncertainty as to when death will occur. This phase also includes the actual death and the bereavement process, times when families perceive the risk of abandonment to be high.
The four phases are marked by changes in functional status. Progressive muscle weakness results in impaired mobility, breathing, and activities of daily living. Complications and the need for interventions increase. The disease progression affects the developmental maturation that all children experience; children with DMD may develop learning disabilities or behavioral problems. Patients and families respond to declines in functional status with feelings of fear, anger, grief, loss, and spiritual distress.
Opportunities for Integration of Palliative Care
As shown in (Table 3), participants identified opportunities for integrating palliative care in each phase, while noting several distinctions due to differences between SMA-1 and DMD.
| Phase of Trajectory | Integration Opportunities | SMA-1 -1 | DMD |
|---|---|---|---|
| Peri-Diagnostic Phase | Communicating a new vision of hope and a commitment to companioning families throughout the process | X | X |
| Establishing realistic timelines and expectations for the diagnostic process | X | X | |
| Considering all options, including hospice, when planning for the delivery of infants who are diagnosed prenatally with SMA-1 | X | ||
| Eliciting parental preferences for communication, decision-making and continuity of care | X | X | |
| Framing the diagnosis as living with the disease rather than focusing on dying | X | X | |
| Anticipating and acknowledging parental grief | X | X | |
| Treatment Decision-Making | Offering the range of morally permissible options including hospice and end-of-life care | X | |
| Disclosing the limits of clinicians’ willingness to implement certain treatment options (including enrollment in clinical trial) | X | X | |
| Acknowledging the uncertainty in velocity of progression and severity throughout the disease process | X | X | |
| Appreciating the unique significance of the genetic aspect of the diagnosis on family dynamics such as parental guilt related to mode of transmission, communication of familial risks and family planning decisions. | X | X* | |
| Beginning advance care planning by anticipating decision points along the trajectory and assessing families’ priorities for quality of life, and expectations and boundaries for treatment | X | X | |
| Reframing definition of a “normal” child and honoring the range of bonding attitudes and behaviors | X | X | |
| Encouraging parents/families to begin “meaning-making” activities such as taking pictures, family gatherings, celebrating milestones | X | X | |
| Anticipating technology and therapy needs based on goals of care and values regarding quality of life | X | X | |
| Assessing pain and symptoms to establish patient baseline | X | X | |
| Changes in Functional Status | Discussing goals and preferences for treatment (resuscitation, ventilation, oxygen, feeding tubes, etc.) at regular intervals and appropriate times as the disease progresses - with parents - with affected children and adolescents who have cognitive and developmental capacities |
X | X X |
| Re-defining the morally permissible boundaries of treatment including aggressive technological interventions such as tracheostomy, mechanical ventilation, G-tube, etc. | X | X | |
| Re-visiting previous decisions in light of new information and experience, and offering options to continue care or redirect it to focus on palliation or end-of-life care | X | X | |
| Instituting measures to enhance quality of life such as -optimizing interaction, mobility, positioning -maximizing educational, social and community integration/access |
X | X X |
|
| Determining eligibility for services such as home nursing care, medical equipment, hospice, etc. | X | X | |
| Frequent monitoring of pain and symptoms including joint and muscle pain, discomfort associated with mobility and positioning, GI discomfort due to reflux, dyspnea, etc. | X | X | |
| Honoring child’s resilience and adaptive patterns | X | ||
| Anticipating grief responses at each loss of function and referring to appropriate specialist. | X | X | |
| Exploring family needs for respite, psychosocial and spiritual support | X | X | |
| Life-Threatening Events (many of the items listed above are ongoing) |
Clarifying the meaning of life-threatening events such as progressive respiratory failure, inability to feed orally, infections, pneumonia, etc., acknowledging the likelihood of death and offering psychosocial and spiritual support to: - parents - affected children and adolescents |
X | X X |
| Assessing whether prior preferences for life-sustaining therapies have changed and, if so, document changes in goals of care including use of intensive care, transfer to hospital, home hospice, etc., and, if appropriate, executing DNR or Allow Natural Death orders or other limitations of care and communicating these decisions to relevant entities and personnel including EMS, local hospital, etc. | X | X | |
| Considering if or when to involve ethics consultants or committees if disputes arise | X | X | |
| Re-assessing symptoms, functional status, and comfort | X | X | |
| Re-introducing opportunities for “meaning-making” to - parents - affected children and adolescents |
X | X X |
|
| Terminal Phase (many of the items listed above are ongoing) |
Acknowledging the uncertainty and variability in the dying process and offering grief counseling and support | X | X |
| Anticipating fears and concerns regarding terminal events and care at the end of life/time of death including managing breathing, comfort, impact of analgesia on awareness and interaction - of parents - of affected children and adolescents who have cognitive/ developmental capacities |
X | X X |
|
| Completing important life closure activities - among family members and - with affected child/adolescent |
X | X X |
|
| Exploring preferences for location of death – home, hospital, hospice, other. | X | X | |
| Assisting with plans for funeral, burial, cremation and care of the body at the time of death | X | X | |
| Death and Bereavement | Assessing family needs and preferences for bereavement services | X | X |
| Making referrals for spiritual, emotional and psychological support for the entire family | X | X | |
| Providing opportunities for post-death meeting with the interdisciplinary team to review new findings, autopsy, lingering questions, revisit genetic testing recommendations | X | X | |
| Offering involvement of health care team members in remembrance and memorial services | X | X | |
| Providing bereavement support for 1-2 years after the child’s death | X | X |
Table 3: Opportunities for Integration of Palliative Care.
First, the timeframes vary due to differences in life expectancy. As we had anticipated, participants were receptive to early discussions about end-of-life care for families of patients with SMA-1, but not for families with DMD. When death is not imminent but expected at some unspecified time in the future, participants perceived the focus on the end of life as signifying the abandonment of curative efforts. When palliative care was reframed to encompass activities, such as “meaningmaking”, that reinforce living life in the moment, participants embraced opportunities for early integration of palliative care, even for families with DMD.
Second, a distinction arises from the modes of inheritance. An X-linked disorder, DMD is transmitted by the mother alone; SMA- 1 is an autosomal recessive condition shared between parents. Both diagnoses carry reproductive risks for family members, but the nature and impact of those risks vary. In the case of DMD, the family may struggle with feelings of guilt and blame. In the case of SMA-1, parents adjusting to life with a new baby are confronted with decisions about diagnostic and genetic testing, treatment, and end-of-life care. These differences in genetics impact communication and decision making in the early stages of diagnosis and treatment.
A third distinction, unique to families with DMD, is how and when to involve children and adolescents in decisions about treatment, endof- life care, and quality of life issues related to developmental concerns such as dating, sexuality, reproductive issues, college, career choices, and independent living.
Five themes emerged spanning all phases of the trajectories and both diagnoses, regarding the relevance of palliative care principles and practices to members of the healthcare team. Focused primarily on communication and relationships, these themes highlighted the importance of the following:
1. Coordination across the range of specialists and care settings, including home care, hospitals, long-term care facilities, rehabilitation, and hospice.
2. Regular family and team meetings, including ethics and palliative care consultants, to discuss the patient’s condition, family needs, and future decisions.
3. The primary care team’s central role throughout the disease trajectory and involvement at each transition.
4. Support for children and their parents in addressing uncertainties throughout the diagnostic and treatment process and finding hope and meaning.
5. Formalized strategies to support clinicians who care for these children and families in their own self-care, coping, grief, bereavement, and moral distress.
The participants acknowledged that the uncertainties that arise in caring for children with life-threatening NMDs, coupled with the increasing availability of therapies and technologies, create complex ethical quandaries for families and clinicians [16]. Such quandaries are exacerbated by the certain knowledge, from an early age, that these diseases are fatal. Some of the ethical challenges include questions about the desirability and effectiveness of life sustaining therapies–both proven and experimental, advance care planning including involving minors in decision-making, and the moral implications of inherited disease including the benefits and risks of genetic testing and screening. Embedded in these issues are questions involving informed consent and end-of life care. The ethical permissibility of the various potential clinical paths is a source of concern and confusion for clinicians and parents.
Participants identified barriers to palliative care integration. Attitudinal barriers included, first, concern that adopting a palliative care framework could be interpreted as losing hope and abandoning curative efforts and, second, resistance to communicating with families and clinicians about values and preferences for life-sustaining therapies, palliation, and end-of-life care. Structural barriers included a lack of infrastructure within communities and health systems to support the integration of palliative care, and lack of sustainable funding and models for collaboration, decision making, and communication across disciplines and care settings.
Clinicians acknowledged that the more medically oriented aspects of palliative care focused on functional status, mobility, and symptom management are currently part of clinical practice but not viewed as “palliative care” per se. With few exceptions, the components of palliative care focused on psychosocial and spiritual issues have yet to be integrated. Moreover, countries vary significantly on how to integrate end-of-life and neuromuscular care.
Discussion
The summit validated the relevance of palliative care principles in cases of SMA-1 and DMD, and articulated a framework to guide clinicians, families, and patients as they navigate the disease progression, regardless of timing or duration. The framework includes advance care planning, concurrent provision of disease-focused care and palliation, enhanced communication and decision making, attention to ethical issues, team functioning and support, and improved quality of life by reducing pain and suffering. These are complementary to recent guidelines for the care of patients with Duchenne Musclar Dystrophy [4,5] which call for greater attention to wholistic, patient/family centered, coordinated care.
The summit affirmed that restoring health means more than curing an illness or eradicating a disease. It enables children and their families to respond to health, illness, disability, and death in their own unique ways, while clinicians apply their knowledge and skills to achieve shared goals. A palliative care framework focused on goals and outcomes creates a shared process and language for communication and decision making [37], aspects often lacking in neuromuscular care. The integration of PPC with curative interventions empowers healthcare professionals, patients, and families to simultaneously seek cures and pursue the day-to-day goal of optimizing life.
Participants, particularly clinicians, worried how acknowledging death as a predictable outcome of the disease would affect children and their families. Several strategies may help resolve between this tension between “hoping for the best” while “planning for the worst” [38]: (1) Lessen resistance to end-of-life discussions by creating more opportunities early on for clinicians, children, and families to explore issues and engage in shared decision making; (2) Foster collaboration by addressing the perception of some clinicians that shared decision making requires them to relinquish control over decisions; and (3) Facilitate communication by reframing palliative care as a new vision of hope [39-43] focused on living rather than dying, and (4) developing systems to address the ethical issues that arise in the care of these patients [16].
Removing the barriers to PPC will require education about the intersection of palliative care and neuromuscular disease care. Implementing system-wide changes will be influenced by broader healthcare system constraints that are unique to each country.
Barriers to integration vary between countries. For example, the United Kingdom has been a global leader in offering comprehensive care through regional hospice programs [29]. Although we did not conduct a systematic comparison of participating countries, evidence suggests a number of cultural differences [44-45]: willingness to talk about death and dying or to involve children in decision making; paternalistic vs. autonomous decision making; and differences in integration of people with disabilities into their communities. Longitudinal studies exploring the disease trajectories and their impact on patients, families, and care provision are needed [46].
The generalizability of our findings is limited by two aspects of study design. Selection criteria required a muscular dystrophy association as well as palliative care and neuromuscular disease teams, keeping the number of participating countries small. Interdisciplinary representation varied among teams; frequently clinician leaders did not identify nurses as key team members, perhaps reflecting countrywide differences in the status of various disciplines.
Despite these limitations, our findings support the early integration of palliative care for children with NMDs. Although perhaps more immediately relevant in cases of SMA-1[33], a palliative care framework can facilitate goals for DMD, including pain and symptom relief, enhanced quality of life, creation of meaningful experiences with family and friends, and spiritual well-being. Advance care planning [47] is especially important in cases of DMD, given the increasing life expectancy and periods of stability and crisis [48] that characterize its trajectory.
Integration of palliative care can help clinicians balance professional and ethical obligations. Clinician integrity is threatened by myriad factors: the competing interests of patients, families, and other team members; the organization where they practice; even their own behaviors and feelings. Pediatric professionals need support systems [49], and the palliative care framework provides clinicians with the knowledge and skills the care of children with NMDs demands.
The summit underscored two conclusions. First, clinicians can discuss difficult issues with NMD patients and their families, explore challenges, and create a shared vision of care. Second, there are opportunities to integrate PPC at each point of transition in the progression of NMDs.
These findings provide the foundation for a global dialogue about cultural differences and spiritual aspects of palliative care [50] and experiences in integrating palliative principles into care for children with NMDs. In addition, these findings offer a foundation for integrating palliative principles in the care of children with life-limiting conditions such as cystic fibrosis and sickle cell disease, and strengthen the recently released Practice Guidelines for Quality Palliative Care, developed as a blueprint for such care [22].
Acknowledgements
This project is dedicated to Mattie J. T. Stepanek and all the children and their families worldwide who live with neuromuscular diseases. We are deeply grateful to the Heartsongs participants, the clinicians and staff of Martin House Pediatric Hospice, Lois Gould, Judith Douglas, the Berman Institute of Bioethics, and the generous funding from the Stavros Niarchos Foundation. The funders were not involved in the design and conduct of the project, or collection, analysis, or interpretation of data or manuscript preparation. Drs. Rushton and Geller as International Co-Directors had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
References
- Jones HR, De Vivo DC, Darras BT (2003) Neuromuscular Disorders of Infancy, Childhood and Adolescence: A Clinician's Approach. Butterworth Heinemann, Philadelphia, Pennsylvania ,USA.
- Roland EH (2000) Muscular dystrophy. Pediatr Rev 21: 233-237.
- Crawford TO, Pardo CA (1996) The neurobiology of childhood spinal muscular atrophy. Neurobio Dis 3: 97-110.
- Bushby K, Finkel R, Birnkrant DJ, Case LE, Clemens PR, et al. (2010) Diagnosis and management of Duchenne muscular dystrophy, part 1: diagnosis, and pharmacological and psychosocial management. Lancet Neurol 9: 77-93
- Bushby K, Finkel R, Birnkrant DJ, Case LE, Clemens PR, et al. (2010) Diagnosis and management of Duchenne muscular dystrophy, part 2: implementation of multidisciplinary care. Lancet Neurol 9: 177-189.
- Kohler M, Clarenbach CF, Bahler C, Brack T, Russi EW, et al. (2009) Disability and survival in Duchenne muscular dystrophy. J Neurol Neurosurg Psychiatry 80: 320-325.
- Manzur AY, Kinali M, Muntoni F (2008) Update on the management of Duchenne muscular dystrophy. Arch Dis Child 93: 986-990.
- Lunn MR, Wang CH (2008) Spinal muscular atrophy. Lancet 371: 2120-2133.
- Oskoui M, Levy G, Garland CJ, Gary JM, O'Hagen J, et al. (2007)The changing natural history of spinal muscular atrophy type 1. Neurology 69: 1931-1936.
- Eagle M, Bourke J, Bullock R, Gibson M, Mehta J, et al. (2007) Managing Duchenne muscular dystrophy--the additive effect of spinal surgery and home nocturnal ventilation in improving survival. Neuromuscul Disord 17: 470-475.
- Parker D, Maddocks I, Stern LM (1999) The role of palliative care in advance muscular dystrophy and spinal muscular atrophy. J Paediatr Child Health 35: 245-250.
- Erby LH, Rushton CH, Geller G (2006) "My son is still walking": stages of receptivity to discussions of advance care planning among parents of sons with Duchenne Muscular Dystrophy. Semin Pediatr Neurol 13: 132-140.
- Hardart MKM, Burns J, Truog RD (2002) Respiratory support in spinal muscular atrophy type 1: a survey of physician practices and attitudes. Pediatrics 110: e24.
- Graham RJ, Robinson WM (2005) Integrating palliative care into chronic care for children with severe neurodevelopmental disabilities. J Dev Behav Pediatr 26: 361-365.
- Weidner NJ (2005) Developing an Interdisciplinary palliative care plan for the patient with muscular dystrophy. Pediatric Annals 34: 546-554.
- Rushton CH, Geller G (2010) A vision of hope for children and families living with life-threatening neuromuscular disorders: The expanding role of pediatric palliative care. Médecine palliative: Soins de Support - Accompagnement - Ethique 9: 283-290.
- Field MJ, Behrman R (2003) When Children Die: Improving Palliative and End-Of-Life Care for Children and Their Families. IOM Committee, National Academies Press, Washington DC, USA.
- American Academy of Pediatrics (2000) Palliative care for children. Pediatrics 106: 351-357.
- http://www.lastacts.org/files/publications/pedprecept.pdf
- Goldman A, Heller KS (2000) Integrating palliative and curative approaches in the care of children with life-threatening illnesses. J Palliat Med 3: 353-359.
- Sourkes B, Frankel L, Brown M, Contro N, Benitz W, et al. (2005) Food, toys, and love: Pediatric palliative care. Curr Probl Pediatr Adolesc Health Care 35: 350-386.
- http://www.nationalconsensusproject.org/guideline.pdf.
- Hinds PS, Oakes L, Furman W, Quargnenti A, Olson MS, et al. (2001) Endof- life decision-making by children and adolescents, parents, and healthcare health care practitioners in pediatric oncology: Research to evidence-based practice guidelines. Cancer Nurs 24: 122-134.
- James L, Johnson B (1997) The needs of parents of pediatric oncology patients during the palliative care phase. J Pediatr Oncol Nurs 14: 83-95.
- Scott JT, Harmsen M, Prictor MJ, Sowden AJ, Watt I (2003) Interventions for improving communication with children and adolescents about their cancer. Cochrane Database Syst Rev 3: CD002969.
- Wissow LS, Hutton N, Kass N (2001) Preliminary study of a values-history advance directive interview in a pediatric HIV clinic. J Clin Ethics 12: 161-172.
- McClain B, Kain ZN (2007) Pediatric palliative care: A novel approach to children with sickle cell disease. Pediatrics 119: 612-614.
- Benjamin L (2008) Pain management in sickle cell disease: Palliative care begins at birth? Hematology Am Soc Hematol Educ Program 466-474.
- Association of Children's Palliative Care (ACT) (2009) A guide to the development of children's palliative care services, 3rd Eds, Royal College of Paediatrics and Child Health, Bristol, UK.
- Knebel AR, Hudgings C (2002) End-of-life issues in genetic disorders: Summary of workshop held at the National Institutes of Health on September 26, 2001. Genet Med 4: 373-378.
- Knebel AR, Hudgings C (2002 ) End-of-life issues in genetic disorders: Literature and research directions. Genet Med 4: 366-372.
- http://jcn.sagepub.com/cgi/content/abstract/22/8/1027
- Rushton CH, Reder E, Hall B, Comello K, Sellers D, et al. (2006) Interdisciplinary interventions to improve pediatric palliative care and reduce health care professional suffering. J Palliat Med 9: 922-933.
- http://www.ippcweb.org/curriculum.asp
- Browning DM, Solomon MZ (2006) Relational learning in pediatric palliative care: transformative education and the culture of medicine. Child Adolesc Psychiatr Clin N Am 15: 795-815.
- Stepanek, MJT (2002) Journey Through Heartsongs. Hyperion Press, Boston, MA, USA.
- Carter BS, Levetown M (2004) Palliative Care for Infants, Children and Adolescents: A Practical Handbook. (1stedn) Johns Hopkins University Press, Baltimore, MD, USA
- Tulsky JA (2005) Beyond advance directives: importance of communication skills at the end of life. JAMA 294: 359-365.
- Gum A, Snyder CR (2002) Coping with terminal illness: the role of hopeful thinking. J Palliat Med 5: 883-894.
- Nekolaichuk CL, Jevne RF, Maguire TO (1999) Structuring the meaning of hope in health and illness. Soc Sci Med 48: 591-605.
- Rustoen T, Wahl AK, Hanestad BR, Gjengedal E, Moum T (2004) Expressions of hope in cystic fibrosis patients: a comparison with the general population. Heart Lung 33: 111-118.
- Sullivan MD (2003) Hope and hopelessness at the end of life. Am J Geriatr Psychiatry 11: 393-405.
- Reder EA, Serwint JR (2009) Until the last breath: exploring the concept of hope for parents and health care professionals during a child's serious illness. Arch Pediatr Adolesc Med 163: 653-657.
- Koenig BA, Gates-Williams J (1995) Understanding cultural difference in caring for dying patients. West J Med 163: 244-249.
- Devictor DJ, Tissieres P, Gillis J, Truog R; WFPICCS Task Force on Ethics (2008) Intercontinental differences in end-of-life attitudes in the pediatric intensive care unit: Results of a worldwide survey. Pediatr Crit Care Med 9: 560-566.
- http://www.biomedcentral.com/14712431/10/67.
- Kolarik RC, Arnold RM, Fischer GS, Tulsky JA (2002) Objectives for advance care planning. J Palliat Med 5: 697-704.
- Gibson BE, Zitzelsberger H, McKeever P. (2009) ,Futureless persons': shifting life expectancies and the vicissitudes of progressive illness. Sociol Health Illness. 31: 554-568.
- Carter BS, Levetown M, Friebert SE (2011) Palliative Care for Infants, Children and Adolescents: A Practical Handbook. (2nd edn) Johns Hopkins University Press, Baltimore, MD, USA
- Puchalski C, Ferrell B, Virani R, Otis-Green S, Baird P, et al. (2009) Improving the quality of spiritual care as a dimension of palliative care: the report of the Consensus Conference. J Palliat Med 12: 885-904.
Relevant Topics
- Caregiver Support Programs
- End of Life Care
- End-of-Life Communication
- Ethics in Palliative
- Euthanasia
- Family Caregiver
- Geriatric Care
- Holistic Care
- Home Care
- Hospice Care
- Hospice Palliative Care
- Old Age Care
- Palliative Care
- Palliative Care and Euthanasia
- Palliative Care Drugs
- Palliative Care in Oncology
- Palliative Care Medications
- Palliative Care Nursing
- Palliative Medicare
- Palliative Neurology
- Palliative Oncology
- Palliative Psychology
- Palliative Sedation
- Palliative Surgery
- Palliative Treatment
- Pediatric Palliative Care
- Volunteer Palliative Care
Recommended Journals
- Journal of Cardiac and Pulmonary Rehabilitation
- Journal of Community & Public Health Nursing
- Journal of Community & Public Health Nursing
- Journal of Health Care and Prevention
- Journal of Health Care and Prevention
- Journal of Paediatric Medicine & Surgery
- Journal of Paediatric Medicine & Surgery
- Journal of Pain & Relief
- Palliative Care & Medicine
- Journal of Pain & Relief
- Journal of Pediatric Neurological Disorders
- Neonatal and Pediatric Medicine
- Neonatal and Pediatric Medicine
- Neuroscience and Psychiatry: Open Access
- OMICS Journal of Radiology
- The Psychiatrist: Clinical and Therapeutic Journal
Article Tools
Article Usage
- Total views: 8791
- [From(publication date):
January-2012 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 4367
- PDF downloads : 4424