Research Article Open Access
Interventional Cardiology-Eight Years of Practice: Do Increased Experience and Technological Evolution Lead to Undertaking More Difficult Cases and Higher Patient Doses?
Tsapaki V1, Kottou S2, Fotos N1, Nikolopoulos D3* and Patsilinakos S11Konstantopoulio General Hospital, Nea Ionia of Athens, Greece
2Medical Physics Laboratory, National and Kapodistrian University of Athens, Athens, Greece
3Piraeus University of Applied Sciences (TEI of Piraeus), Electronic Computer Systems Engineering, Athens, Greece
- *Corresponding Author:
- Nikolopoulos D
Piraeus University of Applied Sciences (TEI of Piraeus)
Electronic Computer Systems Engineering
Athens, Greece
Tel: +0030-6977-208318
E-mail: dniko@teipir.gr
Received date: December 25, 2016; Accepted date: January 20, 2017; Published date: January 27, 2017
Citation: Tsapaki V, Kottou S, Fotos N, Nikolopoulos D, Patsilinakos S (2017) Interventional Cardiology-Eight Years of Practice: Do Increased Experience and Technological Evolution Lead to Undertaking More Difficult Cases and Higher Patient Doses? OMICS J Radiol 6:248. doi: 10.4172/2167-7964.1000248
Copyright: © 2017 Tsapaki V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Radiology
Abstract
In our dedicated catheterization laboratory, within the years 2009–2016, 8286 Interventional Cardiology (IC) procedures were performed by two interventional cardiologists with more than 10 years of experience. There were 5469 Coronary Angiographies (CA) and 2817 Percutaneous Coronary Interventions (PCI). The purpose was to analyze annual patient radiation data, investigate trends and compare with national and international literature and Dose Reference Levels (DRL). Patient doses were determined in terms of: kerma-area product PKA, fluoroscopy time FT and reference air-kerma Ka,r. Concerning the number of frames F, in 1.8% of CA cases and in 40% of PCI cases, was higher than Greek DRLs. PKA, in 13% of CA cases and in 31% of PCI cases, was higher than Greek DRLs. In 0.4% of CA cases, the calculated effective dose values were higher than 40 mSv, whereas in 0.9% PCI cases higher than 80 mSv. In 0.2% of CA cases, PSD was higher than 2 Gy and in 0.04% cases higher than 3 Gy. In 13% of PCI cases, PSD was higher than 2 Gy, in 3% higher than 3 Gy and in 0.4% higher than 5 Gy. FT in 19.2% of CA cases and in 32% of PCI cases was higher than Greek DRLs. The radiation dose trends in IC procedures in this hospital, for the last 8 years, suggest that patient radiation doses in CA are less variable through the years compared to PCI. Doses are comparable to the literature and median values are lower than Greek and European DRLs. The practice of the well experienced interventionalists, with the support of evolving technology, shows that simpler procedures, like CA, need slight shorter FT, while the most demanding procedures like PCI, appear to require more frames without increasing in FT or PSD.
Keywords
Interventional Cardiology; Patient dose; Fluoroscopy time; Peak skin dose; Effective dose
Introduction
Several studies have been published, in the field of Interventional Cardiology (IC) procedures, focused on factors that may influence patient radiation exposure [1-10]. Radiation involves a probability of carcinogenic effects (the risk of stochastic effects), the actual probability increasing with the magnitude of the dose. Effective dose (E) is a dose quantity used to roughly estimate the radiogenic risk to an individual (radiation induced cancer is an example). The stochastic risk to an average member of an irradiated population is expressed in terms of sieverts (Sv). Effective dose also enables medical examinations or techniques to be compared in terms of radiation dose.
Radiation also involves detrimental health effect (i.e., skin injury, hair loss, cataracts) for which the severity increases with the dose of radiation. The effect is not observed unless the threshold is exceeded, although the threshold dose is subject to biologic variation [11]. In interventional fluoroscopy procedures, the tissue of concern is the skin, although the lens of the eye is another consideration. The skin at the site where radiation enters the body receives the highest radiation dose of any body tissue. Once the threshold dose is exceeded, the injury becomes progressively more severe with increasing dose, although the true severity of major injuries will only become apparent weeks to months after the procedure. Peak Skin Dose (PSD) is a dose quantity estimating the highest dose at any portion of a patient’s skin during a procedure. Peak skin dose includes contributions from both the primary X-ray beam and from scatter. Peak skin dose is measured in grays (to soft tissue).
The prime objective of radiation protection is not only to minimize the stochastic risks but also to avoid deterministic injuries, by keeping radiation dose as low as reasonably achievable. However, the potential risk of patient radiation damage must be viewed in the context of the general benefit of these procedures and the likelihood of greater trauma associated with heart surgical interventions and perhaps with imminent death if the intervention was not performed. Radiation dose associated with IC procedures is a complex function of a large number of variables including the X-ray tube voltage (kVp) and the product of tube current and exposure time (mAs), the X-ray field size, the number of projections, focus-skin distance as well as practical skill of the operator [12]. Therefore, for optimizing radiation exposure in such procedures, it is essential to measure patient doses in a given set-up of cardiac catheterization laboratory. During IC procedures, both PSD and E need to be determined. However, neither PSD nor E is measured on a routine basis, because the patient dose monitors commonly available to the operator are kerma-area product (PKA), fluoroscopy time (FT) and reference air-kerma (Ka,r), which can be recorded in real time from the control console of the IC equipment. The kerma-area product, PKA, is defined as the integral of dose across the X-ray beam (Gy�??cm2) and provides information about patient dose as well as the irradiated skin area. It is a unit historically known as dose-area product (DAP) and currently named kerma-area product (KAP, current notation PKA). PKA provides a good index for estimating stochastic risk but is not directly useful for estimating tissue reactions. It is also a wellaccepted dosimetric parameter for comparison between patient doses during different interventional procedures and is also used to assess E [13]. Air Kerma is the energy extracted from an X-ray beam per unit mass of air in a small irradiated air volume. Air kerma is measured in grays. The reference air-kerma (Ka,r) is the air kerma accumulated at a reference point in space which is located along the central ray of the X-ray beam of the C-arm fluoroscopic system at a distance of 15 cm away from the isocenter toward the X-ray tube focal spot and is provided by the manufacturer. Ka,r was introduced by the International Electrotechnical Commission for standardization purposes and is similar to the Cumulative Dose (CD) used in the past [14]. Reference point air kerma does not include backscatter and is measured in grays (Gy). Reference point air kerma is sometimes referred to as reference dose, or cumulative air kerma. FT is required by the US Food and Drug Administration on all fluoroscopy equipment manufactured. However, it lacks information regarding X-ray beam area, thickness of patient and technique employed [15].
It is desirable to measure the PSD to map skin doses in a given IC set-up. However, this does not reflect the entire dose delivered during the course of the procedure. So, the information about the peak as well as overall dose to the patient during IC procedure can be obtained in terms of PSD as well as other dose metrics such as PKA, FT and Ka,r. Each patient record should contain PKA and/or reference point air kerma (Ka,r).
The number of fluoroscopy-guided procedures in cardiology is increasing over time, a fact that led European countries to investigate closely this field and to gather information in the attempt to define Dose Reference Levels (DRLs) [16-19]. The concept of DRLs was first introduced by the International Commission on Radiological Protection in Publication 60 [20] and further expanded in Publication 73 [21]. The results of patient dose surveys could then be compared with the corresponding DRL value, to discover which IC departments have doses above the reference values. An audit process could then be initiated to determine the underlying cause of higher doses and an action plan developed to improve radiological techniques for dose reduction purposes. In practice, DRL values may be regarded as an optimization tool for the reduction of patient doses. In order to establish DRLs, the third quartile of value from survey data distribution is calculated. The median values of the distribution must also be assessed in order to estimate the variation in values.
The purpose of this study was to evaluate patient radiation doses during coronary angiography (CA) and Percutaneous Coronary Intervention (PCI) procedures in a dedicated catheterization laboratory and to analyze annual patient radiation data performed the last 8 years, investigate trends and compare with national and international literature and DRL values. The dosimetry approach was to determine patient doses in terms of three dose metrics: PKA, FT and Ka,r. The PSD was calculated to take into consideration the likelihood of deterministic skin effects and to isolate procedures involving PSDs higher than 2 Gy. Radiation induced skin effects are deterministic in nature, with a generally accepted threshold dose of 2 Gy [11]. A Belgian study has proposed two PKA action levels for skin dose [13,19,22]. A first PKA action level of 125 Gy�??cm2 corresponds to 2 Gy which is the threshold dose for erythema. A PKA value >125 Gy�??cm2 would imply an optional radio pathological follow-up depending on the cardiologist’s decision. The second action level of 250 Gy�??cm2 corresponds to 3 Gy skin dose and would imply a systematic follow-up. To cover the stochastic risk associated with IC procedures, the effective dose to patients was also evaluated by using proposed factors for conversion of PKA to E [22].
Materials and Methods
The IC procedures were performed by two interventional cardiologists with more than 10 years of experience. Coronary Angiography (CA) and Percutaneous Coronary Intervention (PCI) were included in the sample. The procedures were carried out with a Philips Integris Allura Xper FD20 fully digital monoplane machine with flat detector (FD) (Philips Medical Systems, Best, The Netherlands) in a C-arm configuration.
The radiation dose for each patient was provided by the X-ray system in terms of kerma-area product (PKA) and reference point air kerma (Ka,r). Patient radiation metrics in terms of patients age, kermaarea product (PKA) in Gy�??cm2, reference air-kerma (Ka,r) in mGy, fluoroscopy time (FT) in min and total number of frames (F) were analyzed from a pool of data ranging from January 2009 to May 2016.
Quality control was also routinely assessed (including kVp, mA, beam quality [Half-Value Layer, [HVL]) assessment, image quality and radiation dose evaluation) as per the Hellenic Quality Control Angiography machine Protocol set by the Greek Atomic Energy Commission [23]. The PKA meter was calibrated against a digital multimeter (Piranha, RTI Electronics, Molndal, Sweden) with a solidstate detector (CB2-11110201) that has calibration traceable to a standard laboratory. As quoted by the manufacturer, the inaccuracy of the instrument in dose measurements is 2.3%. The calibration was made according to the method summarised in ‘The National Protocol for Patient Dose Measurements in Diagnostic Radiology’ [24], without the table and mattress routinely used.
Conversion factors and equations
Effective dose: Effective dose (E) is estimated by adding the products of the dose in an organ or tissue and the specific weighting factor for that tissue. The weighting factors are values that express the sensitivity of each particular tissue or organ to radiation. Each weighting factor relates to the risk associated with stochastic effects and has specific value for every organ. E is expressed in millisieverts (mSv). In practice, it is very difficult to determine E, since the radiation doses in 12 organs would have to be measured during each cardiological procedure. Therefore, the use of a special conversion factor provides a practical way to estimate E. Modern fluoroscopy machines calculate kerma-area product PKA using generator and collimator settings. PKA does not depend on the distance of the measuring plane from the X-ray source because dose decreases according to the inverse square law and the area of the field increases with the square of the distance. This keeps the PKA value constant at any distance. PKA represents the total energy incident on the patent. PKA is combined with a coefficient depending on the irradiated portion of the body and protocol (irradiated organs) to estimate E. The coefficients range from 0.028 to 0.29 (mSv/Gy�??cm2) depending on type of X-ray procedure with regards to the beam geometry and beam quality. They are derived from Monte-Carlo simulations using anthropomorphic digital phantoms. For coronary angiographies, the most recent studies determine E from PKA using a conversion factor of 0.185 mSv/Gy�??cm2 for normal adult patient, although the precise factor value depended on whether an additional copper filtration was available during cine mode [22].
Peak skin dose: The estimation of absorbed dose at the surface of the skin by fluoroscopy, to account for deterministic effects, is a difficult task since the examination is conducted with changing regularly the incidence X-ray beam. However, it is possible to have an idea of the dose to the skin using a particular operational quantity, called the cumulative dose. This quantity estimates the dose that would have received the skin if the geometry was kept unchanged throughout the procedure. It may be considered that the cumulative dose indicated by the facility in cardiology in many (but not all cases) overestimates the dose to the skin by a factor of 2-3 since several tube-detector incidences are used that distributes the exposure of the skin. If this operational quantity is not available, the skin dose could be estimated from the PKA [25]. So, kerma-area product PKA correlates with peak skin dose (PSD) as it expresses the total X-ray flux in the beam. Reference point air kerma (Ka,r) correlates better with peak skin dose (PSD) and possible radiation injuries, as this quantity indicates the cumulative air kerma at the reference point during the procedure. PSD has been implemented as a function of the highest radiation dose at any point of the patient’s skin to stand for the likelihood and severity of radiation-induced skin injury to the patient. Ka,r is clinically useful as a real-time safety indicator. It does not take into account the scattered radiation and, therefore, is not the actual dose to the patient’s skin. For this reason, the latest guidelines of the Society of Interventional Radiology (SIR) Safety and Health Committee presented a conversion formula to help operators estimate the PSD from the Ka,r shown on the X-ray machine at the end of interventional procedure [11]:
PSD = 206 + 0.513 × Ka,r (mGy) (for Ka,r >500 mGy) (1)
It should be underlined that these are broad estimations that on the other hand provide an immediate estimate of patient PSD easily and quickly in every day routine practice. Of course, accurate estimation of PSD must account for gantry motion, patient size and patient location relative to the gantry but is not possible without dedicated expensive software purchased additionally to the angiography machine.
Results
Our data resulted in 8286 IC procedures (diagnostic and therapeutic interventions) within the years 2009–2016. There were 5469 (66%) diagnostic Coronary Angiographies (CA) and 2817 (34%) Percutaneous Coronary Interventions (PCI). The range of kVp used in these procedures was 50-125 kVp. Patient demographic data collected included age (63±12, 20-92 years), weight (84±18 kgr) and height (168±15 cm). The patient exposure-related parameters recorded for each IC procedure were number of images F, FT, Ka,r and PKA, as they are presented in Table 1.
| Year | Procedure | # of patients | # of frames median | # of frames 3rd | # of frames max | FT median (min) |
FT 3rd (min) | FT max (min) | Karmedian (mGy) | Kar3rd (mGy) | Karmax mGy | PKA median (Gy�??cm2) | PKA 3rd (Gy�??cm2) | PKA max (Gy�??cm2) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2009 | CA | 438 | 453 | 639 | 3326 | 3.6 | 7.2 | 21.3 | 444 | 729 | 3325 | 27.047 | 46.537 | 189.187 |
| PCI | 307 | 1126 | 1456 | 3826 | 12.7 | 22 | 63 | 1771 | 2598 | 12217 | 97.066 | 144.695 | 376.401 | |
| 2010 | CA | 523 | 436 | 570 | 1197 | 3.2 | 6.4 | 49 | 414 | 617 | 3549 | 27.918 | 425.231 | 276.474 |
| PCI | 356 | 1082 | 1437 | 3828 | 13.6 | 20.2 | 58 | 1711 | 2539 | 8773 | 103.709 | 154.889 | 464.954 | |
| 2011 | CA | 355 | 446 | 555 | 1782 | 3.3 | 6.5 | 28.3 | 402 | 615 | 2212 | 28.028 | 44.310 | 226.154 |
| PCI | 235 | 1125 | 1523 | 3254 | 13.8 | 20 | 68 | 1532 | 2295 | 7290 | 96.985 | 138.589 | 458.816 | |
| 2012 | CA | 765 | 497 | 607 | 1633 | 3.2 | 5.8 | 61 | 409 | 613 | 6773 | 27.764 | 40.865 | 639.103 |
| PCI | 386 | 1167 | 1578 | 3960 | 14.3 | 21.5 | 99 | 1619 | 2489 | 11310 | 93.956 | 142.866 | 669.506 | |
| 2013 | CA | 906 | 492 | 619 | 2777 | 3.0 | 5.1 | 48 | 436 | 624 | 9351 | 27.626 | 40.318 | 460.071 |
| PCI | 415 | 1294 | 1741 | 4272 | 14.8 | 22.8 | 91 | 1942 | 3044 | 13505 | 103.011 | 155.898 | 746.534 | |
| 2014 | CA | 1024 | 489 | 635 | 1762 | 2.6 | 4.5 | 103 | 417 | 588 | 4958 | 27.296 | 39.652 | 391.367 |
| PCI | 430 | 1242 | 1644 | 3026 | 14 | 21.7 | 73 | 1777 | 2767 | 11592 | 95.336 | 144.686 | 667.674 | |
| 2015 | CA | 1127 | 475 | 648 | 2295 | 2 | 3.8 | 41 | 365 | 565 | 3432 | 24.503 | 38.107 | 257.393 |
| PCI | 541 | 1143 | 1545 | 6535 | 13 | 19.9 | 94 | 1577 | 2676 | 12593 | 85.759 | 142.908 | 818.086 | |
| 2016 | CA | 330 | 514 | 678 | 2178 | 2.4 | 4.1 | 33 | 447 | 642 | 3595 | 30.523 | 43.699 | 280.778 |
| PCI | 148 | 1194 | 1591 | 4105 | 13.5 | 20.8 | 62 | 1730 | 2825 | 10594 | 93.830 | 150.277 | 452.099 | |
| All years | CA | 5469 | 475 | 619 | 2119 | 2.9 | 5.4 | 48 | 417 | 624 | 4649 | 27.588 | 42.001 | 340.066 |
| PCI | 2817 | 1172 | 1564 | 4101 | 13.7 | 21 | 76 | 1707 | 2654 | 10984 | 96.206 | 146.851 | 581.759 |
Table 1: Median, 3rd quartile and maximum values for number of frames, FT, Ka,r and PKA, along with number of patients, per procedure, per year.
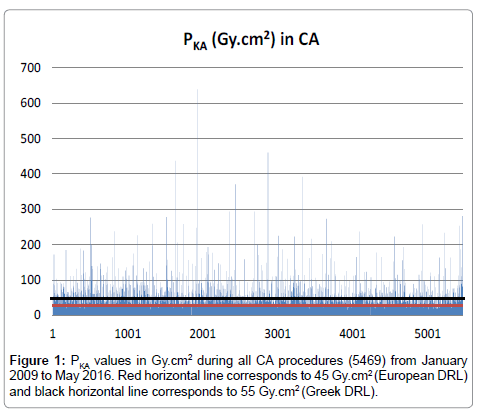
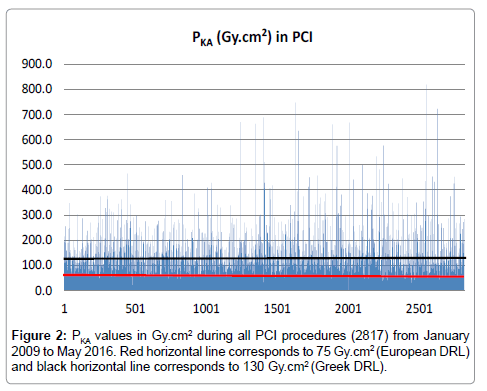
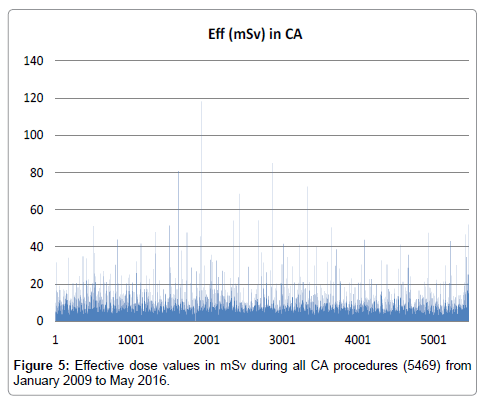
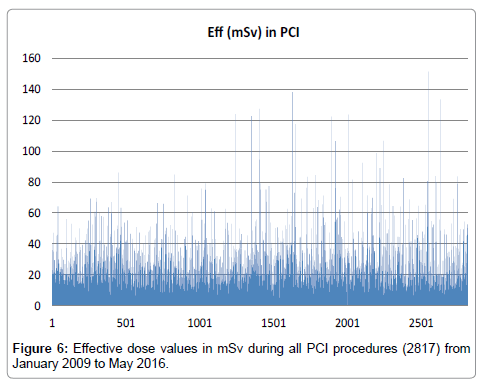
For CA procedures, median values of PKA, Ka,r, FT, and F ranged from 24.5-30.5 Gy�??cm2, 365–447 mGy, 2.3-3.6 min and 436-514 respectively. The PKA, Ka,rand FT values reached 639 Gy�??cm2 (Figure 1), 6.8 Gy and 103 min respectively. The max number of frames was 3326. On the other hand, for PCI procedures, median values of PKA, Ka,r, FT, and F ranged from 86–104 Gy�??cm2, 1532–1942 mGy, 12.7-14.8 min and 1082-1294 respectively. The PKA values reached 818 Gy�??cm2 (Figure 2), Ka,r max was 13.5 Gy, FT reached 99 min and the max number of frames was 6535. Looking closer to these results, for CA cases, the concentration of higher PKA values is noted to be almost stable over time. On the other hand, for PCI cases, this concentration seems to be increased for the second half of the total number.
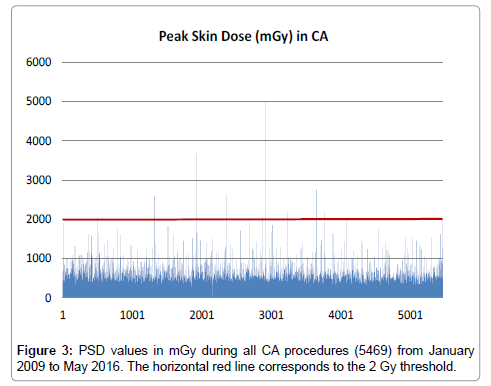
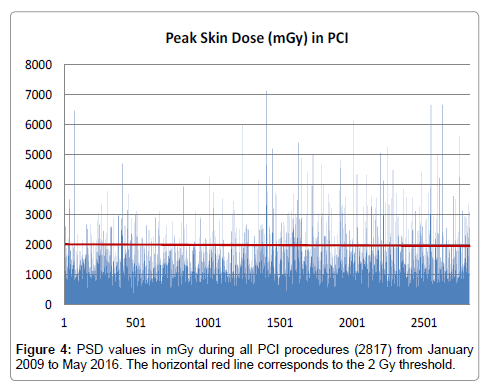
PSD value was calculated by applying equation (1). Median PSD ranged from 393 to 435 and from 992 to 1202 mGy for CA and PCI procedures respectively (Table 2). During CA, PSDmax was found 5003 mGy (Figure 3), whereas during PCI, PSDmax was found 7134 mGy (Figure 4). Looking closer to these results, for CA cases, the concentration of higher PSD values is noted to be almost stable over time. On the other hand, for PCI cases, this concentration seems to be increased for the second half of the total number.
| Year | Procedure | # of patients | # of frames mean | # of frames SD |
Karmean (mGy) | Kar SD (mGy) |
PSD mean (mGy) | PSD SD (mGy) | PSD median (mGy) | PKA mean (Gy�??cm2) | PKA SD (Gy�??cm2) |
E mean (mSv) |
E SD (mSv) |
E median (mSv) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 2009 | CA | 438 | 542 | 290 | 579 | 407 | 503 | 209 | 434 | 35.605 | 26.366 | 6.59 | 4.88 | 5.00 |
| PCI | 307 | 1202 | 488 | 2014 | 1292 | 1239 | 663 | 1115 | 111.934 | 66.582 | 20.71 | 12.32 | 17.96 | |
| 2010 | CA | 523 | 482 | 179 | 534 | 418 | 480 | 214 | 418 | 36.631 | 29.673 | 6.78 | 5.49 | 5.16 |
| PCI | 356 | 1217 | 544 | 1981 | 1248 | 1222 | 640 | 1084 | 118.187 | 70.393 | 21.86 | 13.02 | 19.19 | |
| 2011 | CA | 355 | 502 | 237 | 508 | 351 | 467 | 180 | 412 | 36.211 | 27.226 | 6.70 | 5.04 | 5.19 |
| PCI | 235 | 1252 | 495 | 1775 | 1066 | 1117 | 547 | 992 | 109.021 | 66.746 | 20.17 | 12.35 | 17.94 | |
| 2012 | CA | 765 | 533 | 211 | 528 | 490 | 477 | 251 | 416 | 36.955 | 40.299 | 6.84 | 7.46 | 5.14 |
| PCI | 386 | 1291 | 556 | 1954 | 1303 | 1208 | 668 | 1037 | 115.202 | 75.733 | 21.31 | 14.01 | 17.38 | |
| 2013 | CA | 906 | 541 | 231 | 536 | 496 | 481 | 254 | 430 | 34.898 | 32.128 | 6.46 | 5.94 | 5.11 |
| PCI | 415 | 1450 | 600 | 2355 | 1626 | 1414 | 834 | 1202 | 124.815 | 92.835 | 23.09 | 17.17 | 19.06 | |
| 2014 | CA | 1024 | 544 | 229 | 511 | 398 | 468 | 204 | 420 | 34.435 | 29.103 | 6.37 | 5.38 | 5.05 |
| PCI | 430 | 1351 | 526 | 2227 | 1576 | 1348 | 808 | 1118 | 119.382 | 89.061 | 22.09 | 16.48 | 17.64 | |
| 2015 | CA | 1127 | 551 | 255 | 466 | 356 | 445 | 182 | 393 | 31.662 | 24.488 | 5.86 | 4.53 | 4.53 |
| PCI | 541 | 1299 | 654 | 2140 | 1677 | 1304 | 860 | 1015 | 116.334 | 93.965 | 21.52 | 17.38 | 15.87 | |
| 2016 | CA | 330 | 582 | 271 | 542 | 408 | 484 | 209 | 435 | 37.881 | 32.851 | 7.01 | 6.08 | 5.65 |
| PCI | 148 | 1320 | 579 | 2209 | 1530 | 1339 | 785 | 1093 | 117.969 | 76.582 | 21.82 | 14.17 | 17.36 | |
| All years | CA | 5469 | 535 | 238 | 525 | 416 | 475 | 213 | 416 | 35.535 | 30.267 | 6.57 | 5.60 | 5.03 |
| PCI | 2817 | 1298 | 555 | 2082 | 1415 | 1274 | 726 | 1082 | 116.605 | 78.987 | 21.6 | 14.6 | 17.75 |
Table 2: Mean values and SD of number of frames, Kar, PSD, PKA and E effective and median values PSD and E, along with number of patients, per procedure, per year.
The effective dose E was also calculated from the corresponding value of PKA by using the factor 0.185 mSv/Gy�??cm2, for converting PKA to E [17,21]. Median E effective ranged from 4.5 to 5.7 mSv and from 15.9 to 19.1 mSv for CA and PCI procedures respectively (Table 2). During CA, Emax was found 118 mSv (Figure 5), whereas during PCI, Emax was found 151 mSv (Figure 6). In Table 2 mean values and SD of F, Ka,r, PSD, PKA and E, per year, per procedure, are also presented for comparison reasons (Discussion section).
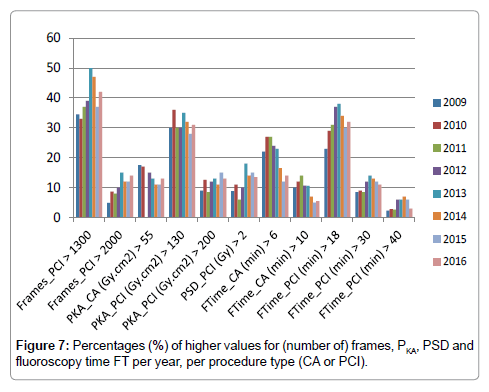
Concerning the number of frames F, for 99 CA cases (1.8%) F value was higher than 1250 (Greek DRL) (Table 3 and Figure 7). Among 2817 PCI cases, 1128 (40%) F value was higher than 1300 (Greek DRL), for 302 cases (11%) F value was higher than 2000 and for 37 cases (1%) F value was higher than 3000 (Table 3 and Figure 7).
| 2009 | Percentages (%) | |||||||
|---|---|---|---|---|---|---|---|---|
| 2010 | 2011 | 2012 | 2013 | 2014 | 2015 | 2016 | ||
| Frames_CA>1250 | 2.7 | 0 | 2 | 1.4 | 1.4 | 2 | 3 | 3 |
| Frames_PCI>1300 | 34.5 | 33 | 37 | 39 | 50 | 47 | 37 | 42 |
| Frames_PCI>2000 | 4.9 | 8.7 | 8 | 10 | 15 | 12 | 12 | 14 |
| Frames_PCI>3000 | 0.7 | 0.8 | 0.4 | 0.8 | 2 | 0.5 | 3 | 0.7 |
| PKA_CA (Gy.cm2)>55 | 17.5 | 17 | 0 | 15 | 13 | 11 | 11 | 13 |
| PKA_CA (Gy.cm2)>100 | 2.7 | 4 | 0 | 4 | 3.4 | 3 | 2 | 4.6 |
| PKA_PCI (Gy.cm2)>130 | 30 | 36 | 30 | 30 | 35 | 32 | 28 | 31 |
| PKA_PCI (Gy.cm2)>200 | 9 | 12.6 | 8.5 | 12 | 13 | 11 | 15 | 13 |
| PKA_PCI (Gy.cm2)>300 | 2.3 | 2.2 | 1.3 | 3 | 4 | 5 | 5 | 2 |
| PSD_CA (Gy)>2 | 0 | 0.2 | 0.4 | 0.4 | 0.4 | 0.3 | 0 | 0.3 |
| PSD_PCI (Gy)>2 | 8.8 | 11 | 6 | 10 | 18 | 14 | 15 | 13.5 |
| PSD_PCI (Gy)>3 | 2.3 | 1.7 | 0.9 | 2 | 4 | 5 | 5 | 4.7 |
| FTime_CA (min)>6 | 22 | 27 | 27 | 24 | 23 | 16.5 | 12 | 14 |
| FTime_CA (min)>10 | 10 | 12 | 14 | 10.7 | 10.6 | 7 | 5 | 5.5 |
| FTime_PCI (min)>18 | 23 | 29 | 31 | 37 | 38 | 34 | 30 | 32 |
| FTime_PCI (min)>30 | 8.5 | 9 | 8.5 | 12 | 14 | 13 | 12 | 11 |
| FTime_PCI (min)>40 | 2.3 | 2.8 | 2.6 | 6 | 6 | 7 | 6 | 3 |
Table 3: Percentages (%) of higher values for (number of) frames, PKA, PSD and fluoroscopy time FT per year, per procedure type. Bold numbers correspond to the Greek DRLs.
Concerning PKA, for 719 CA cases (13%) PKA value was higher than 55 Gy�??cm2 (Greek DRL) and for 15 cases (0.3%) PKA value was higher than 250 Gy�??cm2 (Table 3 and Figure 7). Among 2817 PCI cases, 885 (31%) PKA value was higher than 130 Gy�??cm2 (Greek DRL) and for 172 cases (6%) PKA value was higher than 250 Gy�??cm2 (Table 3 and Figure 7).
In accordance with the PKA values, the same shape is followed by the effective dose E values, as can be seen in Figures 5 and 6. It is calculated that 24 CA cases (0.4%) received more than 40 mSv, whereas 25 PCI cases (0.9%) received more than 80 mSv.
Among 5469 CA cases, 11 (0.2%) received PSD higher than 2 Gy and 2 cases (0.04%) received PSD higher than 3 Gy (Table 3 and Figure 7). Among 2817 PCI cases, 357 (13%) received PSD higher than 2 Gy, 97 cases (3%) received PSD higher than 3 Gy and 12 cases (0.4%) received PSD higher than 5 Gy (Table 3 and Figure 7).
Concerning the time FT, for 1049 CA cases (19.2%) FT value was higher than 6 min (Greek DRL) and for 471 CA cases (8.6%) FT value was higher than 10 min (Table 3 and Figure 7). Among 2817 PCI cases, 899 (32%) FT value was higher than 18 min (Greek DRL), for 320 cases (11%) FT value was higher than 30 min and for 137 cases (5%) FT value was higher than 40 min (Table 3 and Figure 7).
Discussion
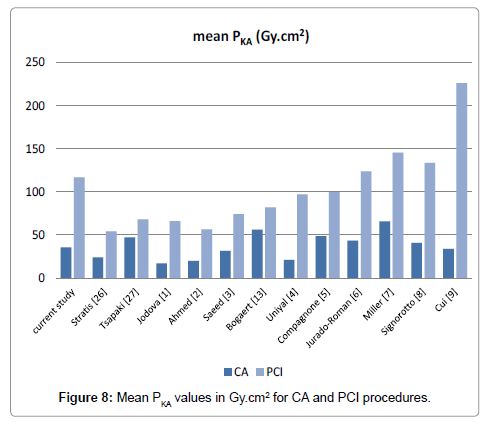
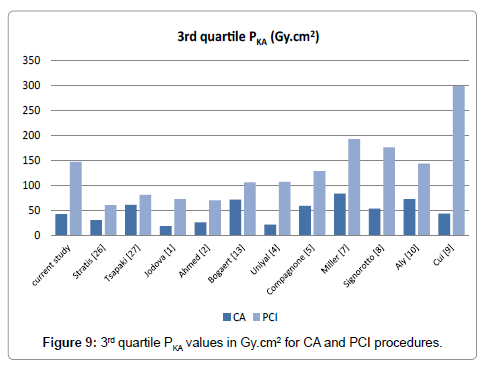
The mean and 3rdquartile PKA values recorded during both CA and PCI procedures in the present study were compared with those published in the literature (Figures 8 and 9). Mean values for patient doses are not essential, as they do not represent the dominant daily practice in every laboratory. The IC procedures present wide variation in patient dose resulting from complexity. Median and 3rd quartile values have been established as they are identified to be more representative, the radiation dose data being not normally distributed. It can be seen however that in both figures, current study’s CA PKA value is lower than half of the presented laboratories, whereas current study’s PCI PKA value is the 4th(13 centers) and 3rd(12 centers) higher respectively. It is generally accepted that the large variability in the recorded values of PKA, especially during PCI procedures, is mainly attributed to different levels of procedure complexity, patient thickness and skill of the cardiologist.
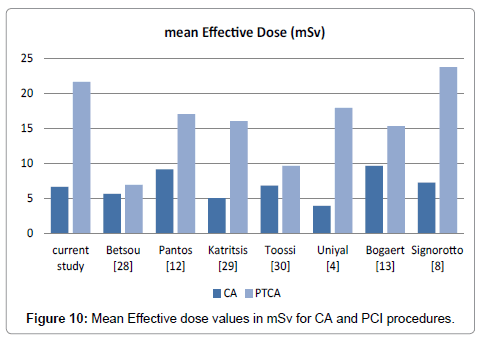
Concerning mean effective dose, for CA procedures current study has the 4thhigher value (8 centers) and for PCI procedures it has the 2nd higher value (Figure 10). It has to be highlighted however that slight differences were noticed between the values of conversion factor calculated by Uniyal et al. [4] and Betsou et al., which were 0.183 mSv/ Gy�??cm2. Nevertheless, although E is derived from PKA by using a single multiplicative factor, it provides a convenient way to judge patient doses [26-35].
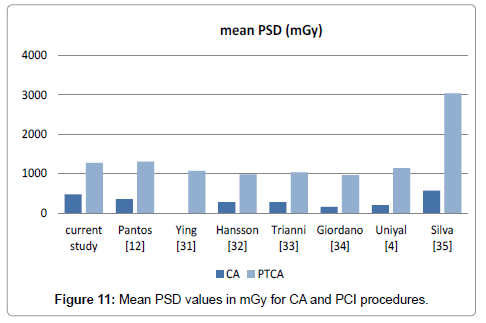
Concerning mean PSD value, for CA procedures current study has the 2nd higher value (7 centers) and for PCI procedures it has the 3rd higher value (Figure 11). Although the mean PSD (median values are even lower) for CA and PCI procedures in this study were well below the deterministic threshold of skin injury, 13%, 3% and 0.4% of patients received PSDs during PCI exceeding 2, 3 and 5 Gy, respectively (Table 3 and Figure 7). Dose Reference Levels are the guide to what is achievable with current good practice, rather than optimum performance, and are dose neither limits nor thresholds that define competent performance of the operator or the equipment. A mean dose for a procedure that is less than the RL does not guarantee that the procedure is being performed optimally. On the other hand, even with optimal technique, it is not always possible to keep peak skin dose below the threshold for skin effects. This does not necessarily indicate poor operator technique. It is not necessarily a contraindication to performing or continuing a procedure. However, no deterministic injury was reported from any patient during these eight years of practice in this unit. An event that can be explained by the fact that interventionists are well trained and have always in mind to move the X-ray source as often as possible, so as none patient small skin region to receive large portion of the incident radiation. Nevertheless, the operator is always notified when a significant radiation dose has been administered. The patients are also instructed to notify the operator if any signs or symptoms of a possible radiogenic deterministic effect are observed. The operator writes an appropriate note in the patient’s medical record. Follow-up of patients who have received a significant radiation dose applies at 10–14 days and 1 month after the procedure, according to the guidelines [11].
The everyday practice of the two well-experienced interventionists, with the help of evolving technology, shows that simpler procedures, like CA, need slight shorter fluoroscopy time, while the most demanding procedures like PCI, appear to require more frames without increasing in fluoroscopy time or patient’s skin dose.
Conclusion
The data of this study resulted in 8286 IC procedures within the years 2009–2016. There were 5469 (66%) Coronary Angiographies (CA) and 2817 (34%) Percutaneous Coronary Interventions (PCI). Concerning the number of frames F, for 99 CA cases (1.8%) F value was higher than 1250 (Greek DRL). Among PCI cases, 1128 (40%) F value was higher than 1300 (Greek DRL), for 302 cases (11%) F value was higher than 2000 and for 37 cases (1%) F value was higher than 3000.
Concerning PKA, for 719 CA cases (13%) PKA value was higher than 55 Gy�??cm2 (Greek DRL) and for 15 cases (0.3%) PKA value was higher than 250 Gy�??cm2. Among PCI cases, 885 (31%) PKA value was higher than 130 Gy�??cm2 (Greek DRL) and for 172 cases (6%) PKA value was higher than 250 Gy�??cm2. The calculated effective dose values showed that in 24 CA cases (0.4%) patients received more than 40 mSv, whereas in 25 PCI cases (0.9%) they received more than 80 mSv. Among the CA cases, 11 (0.2%) received PSD higher than 2 Gy and 2 cases (0.04%) received PSD higher than 3 Gy. Among the PCI cases, 357 (13%) received PSD higher than 2 Gy, 97 cases (3%) received PSD higher than 3 Gy and 12 cases (0.4%) received PSD higher than 5 Gy. Concerning the fluoroscopy time (FT), for 1049 CA cases (19.2%) FT value was higher than 6 min (Greek DRL) and for 471 CA cases (8.6%) FT value was higher than 10 min. Among the PCI cases, 899 (32%) FT value was higher than 18 min (Greek DRL), for 320 cases (11%) FT value was higher than 30 min and for 137 cases (5%) FT value was higher than 40 min. The radiation dose trends in IC procedures in the hospital of this study for the last 8 years suggest that patient radiation doses in CA are less variable through the years compared to PCI. Doses are comparable to the literature and median values are lower that Greek and European DRLs. Even with optimal technique, it is not always possible to keep patient radiation dose below the threshold for skin effects. However, no deterministic injury was reported from any patient during these eight years of practice in this unit, while the appropriate actions and the recommended follow-up of patients who have received a significant radiation dose were strictly followed.
The daily practice of two well-experienced interventionists, with the help of evolving technology, shows that simpler procedures, like CA, need slight shorter fluoroscopy time, while the most demanding procedures like PCI, and appear to require more frames without increasing in fluoroscopy time or patient’s skin dose.
References
- Zotova R, Vassileva J, Hristova J, Pirinen M, Järvinen H (2012) A national patient dose survey and setting of reference levels for interventional radiology in Bulgaria. EurRadiol 22: 1240-1249.
- Ahmed NA, Ibraheem SB,Habbani FI (2013) Patient doses in interventional cardiology procedures in Sudan. RadiatProtDosim 153: 425-430.
- Saeed MK (2016) Dose measurement using Gafchromic film for patients undergoing interventional cardiology procedures. RadiatProtDosim p: ncw082.
- Uniyal SC, Chaturvedi V, Sharma SD, Rawat A (2016) Patient dosimetry during interventional cardiac procedures in a dedicated catheterization laboratory.RadiatProtDosimetry.
- Compagnone G, Campanella F, Domenichelli S, Lo Meo S, Bonelli M, et al. (2012) Survey of the interventional cardiology procedures in Italy. RadiatProtDosim 150: 316-324.
- Jurado-Román A, Sánchez-Pérez I, Lozano Ruíz-Poveda F, López-Lluva MT, Pinilla-Echeverri N, et al. (2016) Effectiveness of the implementation of a simple radiation reduction protocol in the catheterization laboratory. CardiovascRevasc Med 17: 328-332.
- Miller DL, Hilohi CM,Spelic DC (2012) Patient radiation doses in interventional cardiology in the US: advisory data sets and possible initial values for US reference levels. Med Phys 39: 6276-6286.
- Signorotto P, delVecchio A, Montorfano M, Maisano F, Giagnorio M, et al. (2010)Dosimetric data and radiation risk analysis for new procedures in interventional cardiology. RadiatProtDosim 142: 201-208.
- Cui Y, Zhang H, Zheng J, Yang X, Liang C (2013)An investigation of patient doses during coronary interventional procedures in China. RadiatProtDosim 156: 296-302.
- Aly AE, Duhaini IM, Manaa SM, Tarique SM, Kuniyil SE, et al. (2015) Patient peak skin dose and dose area product from interventional cardiology procedures. Int J Med PhysClinEngRadiatOncol 4: 7-12.
- Stecker MS, Balter S, Towbin RB (2009) Guidelines for patient radiation dose management. J Vas Inter Rad 20: 263-273.
- Pantos I, Patatoukas G, Katritsis DG,Efstathopoulos E (2009) Patient radiation doses in interventional cardiology procedures. CurrCardiol Rev 5: 1-11.
- Bogaert E, Bacher K, Thierens H (2008) A large-scale multicentre study in Belgium of dose area product values and effective doses in interventional cardiology using contemporary X-ray equipment. RadiatProtDosim 128: 312-323.
- International Electrotechnical Commission Report 60601 (2000) Medical Electrical Equipment–Part 2-43: Particular requirements for the safety of X-ray equipment for interventional procedures.Geneva, Switzerland.
- Miller DL, Balter S, Cole PE, Lu HT, Berenstein A, et al. (2003) Radiation doses in interventional radiology procedures: the RAD-IR Study Part II: skin dose. J VascIntervRadiol 14: 977-990.
- International Commission on Radiological Protection (2000) ICRP Publication 85: Avoidance of radiation injuries from medical interventional procedures. Ann ICRP 30.
- European Union (1997) Council Directive 97/43 Euratom, on health protection of individuals against the dangers ionizing radiation in relation to medical exposure, and repealing. Directive 84/466 Euratom. Off J Eur Communities 180: 22-27.
- Neofotistou V, Vano E, Padovani R, Kotre J, Dowling A, et al. (2003) Preliminary reference levels in interventional cardiology. EurRadiol 13: 2259-2263.
- Bogaert E, Bacher K, Lemmens K, Carlier M, Desmet W, et al. (2009)A large-scale multicentre study of patient skin doses in interventional cardiology: dose-area product action levels and dose reference levels. Br J Radiol 82: 303-312.
- International Commission on Radiological Protection (1991) 1990 recommendations of the International Commission on Radiological Protection. Ann ICRP 21: 1-3.
- International Commission on Radiological Protection (1996) Radiological protection and safety in medicine. Ann ICRP.
- Bogaert E, Bacher K, Thierens H (2008) Interventional cardiovascular procedures in Belgium: effective dose and conversion factors. RadiatProtDosim 129: 77-82.
- https://eeae.gr/en/legislation
- https://www.gov.uk/government/publications/diagnostic-radiology-national-protocol-for-patient-dose-measurements
- Verdun Francis R, Abbas A, Eleni S, Francois B, Jean-Francois S (2011) Protection of the patient and the staff from radiation exposure during fluoroscopy-guided procedu res in cardiology.AdvDiaCoronary Atherosclerosis, pp: 367-379.
- Stratis AI, Anthopoulos PL, Gavaliatsis IP, Ifantis GP, Salahas AI,et al. (2009) Patient dose in cardiac radiology. Hellenic J Cardiol 50: 17-25.
- Tsapaki V,Kottou S, Vano E, Faulkner K, Giannouleas J, et al. (2002) Patient dose values in a dedicated Greek cardiac centre. Br J Radiol 76: 726-730.
- Betsou S, Efstathopoulos EP, Katritsis D, Faulkner K, Panayiotakis G (1998) Patient radiation doses during cardiac catheterization procedures. Br J Radiol 71: 634-639.
- Katritsis D, Efstathopoulos E, Betsou S, Korovesis S, Faulkner K, et al. (2000) Radiation exposure of patients and coronary arteries in the stent era: a prospective study. Catheter CardiovascInterv 51: 259-264.
- Toossi MTB, Zare H, Bayani S,Esmaili S (2008) Organ and effective doses of patients arising from coronary angiography and percutaneous transluminal coronary angioplasty at two hospitals in Mashhad-Iran. RadiatProtDosim 128: 363-366.
- Ying CK,Kandaiya S (2010) Patient skin dose measurements during coronary interventional procedures using Gafchromic film. J RadiolProt 30: 585-596.
- Hansson B, Karambatsakidou A (2000) Relationships between entrance skin dose, effective dose and dose area product for patients in diagnostic and interventional cardiac procedures. RadProtDosim 90: 141-144.
- Trianni A, Chizzola G, Toh H, Quai E, Cragnolini E, et al. (2006) Patient skin dosimetry in haemodynamic and electrophysiology interventional cardiology. RadiatProtDosim 117: 241-246.
- Giordano C, D’Ercole L, Gobbi R, Bocchiola M, Passerini F (2010) Coronary angiography and percutaneous transluminal coronary angioplasty procedures: evaluation of patients’ maximum skin dose using Gafchromic films and a comparison of local levels with reference levels proposed in the literature. Phys Med 26: 224-232.
- Silva MO, Rodrigues BD,Canevaro LV (2011) Evaluation of patients skin dose undergoing interventional cardiology procedure using radiochromic film. Rev Bras Fis Med 5: 79-84.
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 4091
- [From(publication date):
February-2017 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 3160
- PDF downloads : 931