Research Article Open Access
Laryngopharyngeal reflux - a randomized controlled trial of voice changes after treatment in Scandinavian adults.
Mette Pedersen*
Mette Pedersen, The Medical Centre, Voice Unit, Østergade 18, 3, 1100 Copenhagen
- *Corresponding Author:
- Mette Pedersen
The Medical Centre, Voice Unit
Østergade 18, 3, 1100 Copenhagen, Denmark
Tel: +4533159600
Fax: +4533137705
E-mail: m.f.pedersen@dadlnet.dk
Received date: October 07, 2014; Accepted date: March 14, 2015; Published date: March 20, 2015
Citation: Pedersen M (2015) Laryngopharyngeal Reflux - A Randomized Controlled Trial of Voice Changes after Treatment in Scandinavian Adults. J Community Med Health Educ 5:336. doi:10.4172/21610711.1000336
Copyright: © 2015 Pedersen M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Community Medicine & Health Education
Abstract
A randomized prospective controlled study was made in order to find out if voice related acoustical measures show usable predictive pathologies in patients with laryngo-pharyngeal reflux (LPR), based on high speed films with 4000 pictures of the larynx per second. The main results of this study were that lifestyle changes (according to the standard literature) did optimize the voice in patients with LPR. The used acoustical program was an advanced MDVP (multi-dimensional voice program) by Laryngograph Ltd. which routinely adjusts to well-defined sustained tones measures as well as reading of a standard text and electroglottography. Three treatment groups for LPR with each 78, 70 and 89 patients respectively were treated with standard advice of lifestyle changes, combined with proton pump inhibitors, and a third group with lifestyle changes, proton pump inhibitors and alginate. The mean age was 42, 42 and 41 years, all three groups with a standard deviation of 15 years. There was no difference of treatments effect between the groups; they were therefore added to each other. A comparison between the first and second consultation after two weeks did show shimmer change from 9.35% to 7.76% after two weeks to 7.96% follow up after three months, comparing the first to the third measurement. In reading of a standard text the frequency and intensity variations were also reduced from 10.73% and 16.23% at the first consultation to 9.43% and 15.26% at the second consultation and after three months the frequency variation was 9.51% and 15.77%. So it can be concluded that especially reading of a standard text is changed after treatment of LPR. No change was found of electroglottography. The acoustical findings were not related to the oedema of the arytenoid region based on high speed films with 4000 pictures per second. The acoustical measures should be refined in the future with online measures on high speed films.
Keywords
Randomized controlled trials; Laryngo-pharyngeal reflux; Oedema of the arytenoid region; MDVP; Jitter; Reading of a standard text; Electroglottography
Introduction
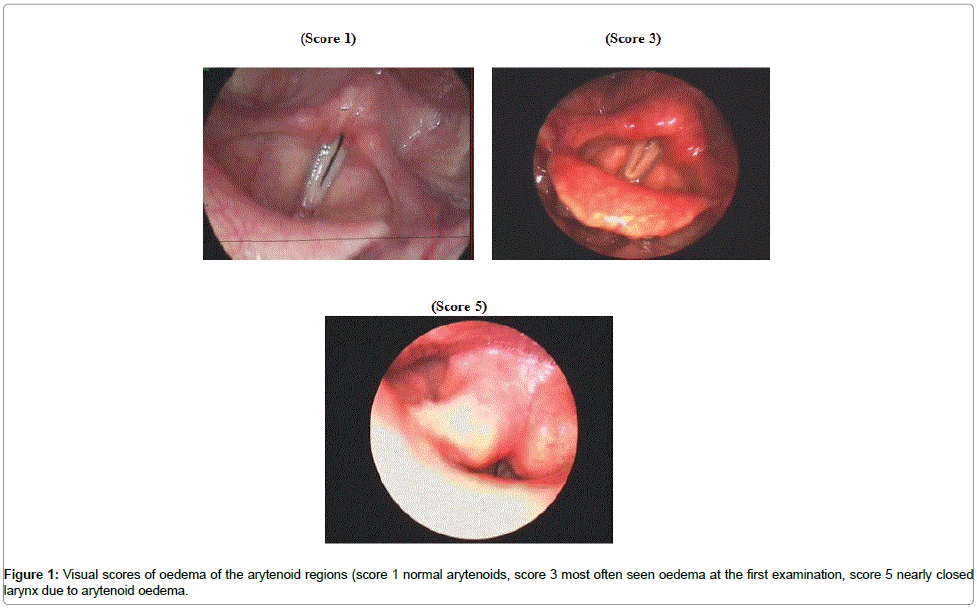
In our Cochrane review on laryngeal reflux (LPR) and hoarseness, studies were insufficient to document specific voice related acoustical relations to the larynx. Mostly, the amounts of patients were too low for statistical evidence [1]. Probably there is one disorder, GERD, which in some cases gives laryngeal complaints due to oedema of the arytenoid region shown in Figure 1 [2-4]. There is a lack of voice related acoustical evidence in randomized controlled trials between gastro oesophageal reflux disease (GERD) and LPR [5-10]. A meta-analysis did not give validated conclusions either [11,12]. With high speed films it is possible to document treatment effect with reduction of oedema of the arytenoid region, in this way we have new objective measures for prognostic evaluation of LPR. The aim of this prospective randomized study was based on an earlier study, to make an acoustical evaluation: that the speaking voice is a parameter of interest in LPR [13,14].
Materials and Methods
Subjective complaints
The required subjective symptom complaints duration of LPR for inclusion was at least 2-4 weeks in adult Scandinavians. The presence of inter-arytenoid oedema with visual score 2-5, documented with high speed films of 4000 frames per second, was also required for the inclusion to the study. This evaluation replaces earlier used videostroboscopy with only 25 frames per second because videostroboscopy gives a “false” picture of the larynx. The LPR complaints with at least three of the following: Clearing your throat/excess throat mucus or postnasal drip, hoarseness, difficulty swallowing food, liquids, or pills (dysphagia), coughing after you ate or after lying down, troublesome or annoying cough, breathing difficulties or chocking episodes (larynx spasms and hick up), sensational of something sticking in your throat or lump in your throat (globules) and/or Heartburn, chest pain, indigestion or stomach acid coming up, pain or burning feeling in the throat.
Reasons for exclusion were: under 18 years of age, no subjective complaints, and lack of the objective evaluation of oedema of the inter-arytenoid region on high speed films. Other reasons were malignancies, pregnancies, and lack of cooperation. The data collection in the database of patients was made during a period of 2½ years in Copenhagen in an ear-nose-throat clinic.
Study protocol
The first examination included registration of complaints, high speed films with 4000 frames per second and randomization and start of treatment. The second examination after two weeks included treatment results and the third examination followed after three months with final collection of results, a follow up and where treatment could stop. All participating patients signed a written consent, which was scanned and stored in the database. Patient treatment was randomized into three groups of treatment:
1. lifestyle correction (avoid the following acid provoking habits and food: Smoking, fatty and smoked food, coffee, chocolate, spices, strong alcohol (alcohols containing a lot of tannins), acidic fruits and juices. No food 2-3 hours before sleep, avoid over eating, sleep with your head high. Singers should avoid eating just before a concert).
2. Life style correction+proton pump inhibitors (esomeprazol) 1 tablet daily 40 mg and a group 3 with supplementary alginate 1 tablet after the evening meal.
High speed films with description of inter arytenoid oedema were recorded with the standard equipment from Richard Wolf GmbH Pforzheimer Straße 32, 75438 Knittlingen, Germany. The Multi- Dimensional Voice Program (MDVP) was used for sustained tones, reading of a standard text and electroglottography (EGG) as developed in England by Fourcin and Abberton and used by Laryngograph Ltd. 78 Manor Road, Wallington, Greater London, SM6 0AB, United Kingdom [15].
Statistical sample size consideration for the prospective randomized controlled study
A total of 49 patients were needed in each group of lifestyle correction, lifestyle correction+proton pump inhibitor in the second group and the third group with supplementary alginate, to obtain a power of 90% in a two-group, one-sided, t-test to detect a difference of 20% under the assumption that the true difference was 5% and that the standard deviation was 25%. Based on this general consideration and taking into account, possible drop out and evaluation of multiple endpoints, a total of 237 patients were randomized in the study.
Each numerical week 2, endpoint was evaluated in an analysis of covariance including baseline value as covariate and treatment group as fixed effect. This included voice related acoustical analysis, subjective complaints, and inter arytenoids oedema scores on high speed films.
For each endpoint the hypotheses were tested
An effect of treatment based on voice related acoustical analysis, subjective complaints and high speed films. A difference between treatment groups of lifestyle correction, and lifestyle correction and added treatment with the proton pump inhibitor esomeprazole 40 mg, one tablet at night against the two sided alternative that there is a difference. A difference between treatment groups of lifestyle correction and lifestyle correction combined with esomeprazole 40 mg and alginate, 1-2 chewing tablets after the evening meal against the two sided alternative that there is a difference. Values were analysed as such and no imputation was made, which means that missing data were not included in the analysis.
The subjective complaints had descriptive statistics for each LPR complaint. Formal statistical analysis was conducted on the derived endpoint: Total number of complaints. The total number of complaints was calculated as the sum of the individual evaluations of each of the complaints. Only patients who had both baseline and week 2 visits were included in the analysis. Missing data for symptoms were imputed to be absent. The total number of complaints was analysed as for the numerical endpoints.
The study comprised a baseline visit with LPR complaints as the subjective inclusion criteria and a visual inter arytenoid oedema score (2-5) on high speed films with 4000 frames per second as the objective findings. The investigator was blinded as to the allocation of the patients in the groups, prior to inclusion where the lowest randomization number was given. At the second examination, the follow up was planned after a period of three months, both with the same analysis, and treatment as randomised and started at the 1st examination.
The symptom evaluation was dichotomized in the way that each subjective symptom was considered maximally present. As for the objective findings, a scaling was made for acoustical analysis, and the interarytenoid oedema of one (normal) to five. Spearman correlation coefficients were calculated on the acoustical parameters.
Results
A description of adult Scandinavian patients included in the study
Since no voice related acoustical differences were found between the three treatment groups which consisted of lifestyle correction, lifestyle correction + proton pump inhibitor, and the third group with supplementary alginate, they were treated together. What can be concluded from this is that life style change is essential in treatment of LPR. The three treatment groups for LPR had each 78 patients (group 1 lifestyle correction regarding diet and behaviour), 70 patients (group 2 Life style correction + proton pump inhibitors (esomeprazol) 1 tablet daily 40 mg) and 89 patients (group 3 with same treatment as group 2 supplementary alginate 1 tablet after the evening meal.)
A summary is presented of percentage variation of fundamental frequency of sustained tones, reading of a standard text and EGG at the first, second and third consultation. The statistical comparison was made between first and second consultation and the first and third consultation respectively as shown in Table 1. Arytenoid region oedema score with high speed films was given at the top of the table. A reduction of reading frequency and intensity variation in percentage was given of 10.73% and 16.23% at the first consultation to 9.43% and 15.26% at the second consultation and after three months was 9.51% and 15.77% respectively. A significant reduction of shimmer percentage of sustained tones was also found at the second (from 9.35% to 7.76%) and the third examination (7.96%). The p-values are presented of all three consultations.
| Parameter | 1st consultation | 2nd consultation | 3rd consultation | ||||||
|---|---|---|---|---|---|---|---|---|---|
| N | Mean (SD) | N | Mean (SD) | Mean change | N | Mean (SD) | Mean change | ||
| (p-value) | (p-value) | ||||||||
| Arytenoids region oedema visual score | 237 | 2.71 (0.69) | 196 | 2.19 (0.70) | -0.52 (<.0001) | 147 | 1.96 (0.72) | -0.77 (<.0001) | |
| Reading | Frequency (%) | 235 | 10.73 (9.20) | 194 | 9.43 (7.64) | -1.18 (0.0251) | 144 | 9.51 (8.29) | -1.92 (0.0062) |
| Intensity (%) | 233 | 16.23 (4.91) | 193 | 15.26 (4.13) | -1.02 (0.0002) | 145 | 15.77 (4.27) | -0.80 (0.0246) | |
| Qx (%) | 235 | 47.68 (6.03) | 193 | 47.81 (5.75) | 0.35 (0.2934) | 145 | 47.51 (5.86) | 0.10 (0.8057) | |
| Tone | Jitter (%) | 234 | 2.81 (8.31) | 192 | 2.02 (5.73) | -0.77 (0.0635) | 143 | 2.55 (6.93) | -0.31 (0.5979) |
| Shimmer (%) | 232 | 9.35 (8.04) | 191 | 7.76 (4.38) | -1.37 (<.0001) | 144 | 7.96 (4.56) | -1.41 (0.0003) | |
| Qx (%) | 234 | 46.39 (8.60) | 191 | 46.45 (7.19) | 0.25 (0.5605) | 143 | 47.08 (7.59) | 0.63 (0.2707) | |
Table 1: A summary is presented of percent variation of fundamental frequency of sustained toned, reading of a standard text and electroglottography (EGG) at the first, second and third consultation, arytenoid region oedema score was given at the top of the table. A reduction of reading intensity % was found at the second as well as third. At the second and third examination a reduction of shimmer % of sustained tones was found.
Spearman correlation for percentage change of the acoustical parameters was compared with oedema of the arytenoids at the second and third consultation on high speed films as shown in Table 2. The better results of jitter at the third consultation were not found in reading. Statistically no change for the other parameters was found after LPR treatment. A comparison was here made of the Spearman correlation quotient between arytenoids swelling changes and MDVP including EGG at the second and third consultation. The jitter measures were due to a few aberrant variables. So the arytenoid oedema and the acoustical parameters did not change in a way that corresponds statistically.
| Parameter | 2nd consultation | 3rd consultation | |||
|---|---|---|---|---|---|
| Spearman | P-value | Spearman | P-value | ||
| Reading | Frequency (%) | 0.17 | 0.0190* | 0.04 | 0.6587 |
| Intensity (%) | -0.02 | 0.8107 | 0.06 | 0.5149 | |
| Qx (%) | -0.11 | 0.1466 | -0.11 | 0.1741 | |
| Tone | Jitter (%) | 0.12 | 0.1065 | 0.22 | 0.0073** |
| Shimmer (%) | 0.15 | 0.0416* | 0.09 | 0.2714 | |
| Qx (%) | 0.05 | 0.4792 | -0.1 | 0.225 | |
Table 2: Spearman correlations for percent change of the acoustical parameters compared with oedema of the arytenoids at the second and third consultation. The results of jitter were not found in reading. A comparison was made of the Spearman correlation quotient between arytenoids swelling changes and MDVP and EEG at the second and third consultation. The jitter measures were due to a few aberrant variables.
Visual scores of oedema of the arytenoid regions (score 1 normal arytenoids, score 3 most often seen oedema at the first examination, score 5 nearly closed larynx due to arytenoid oedema).
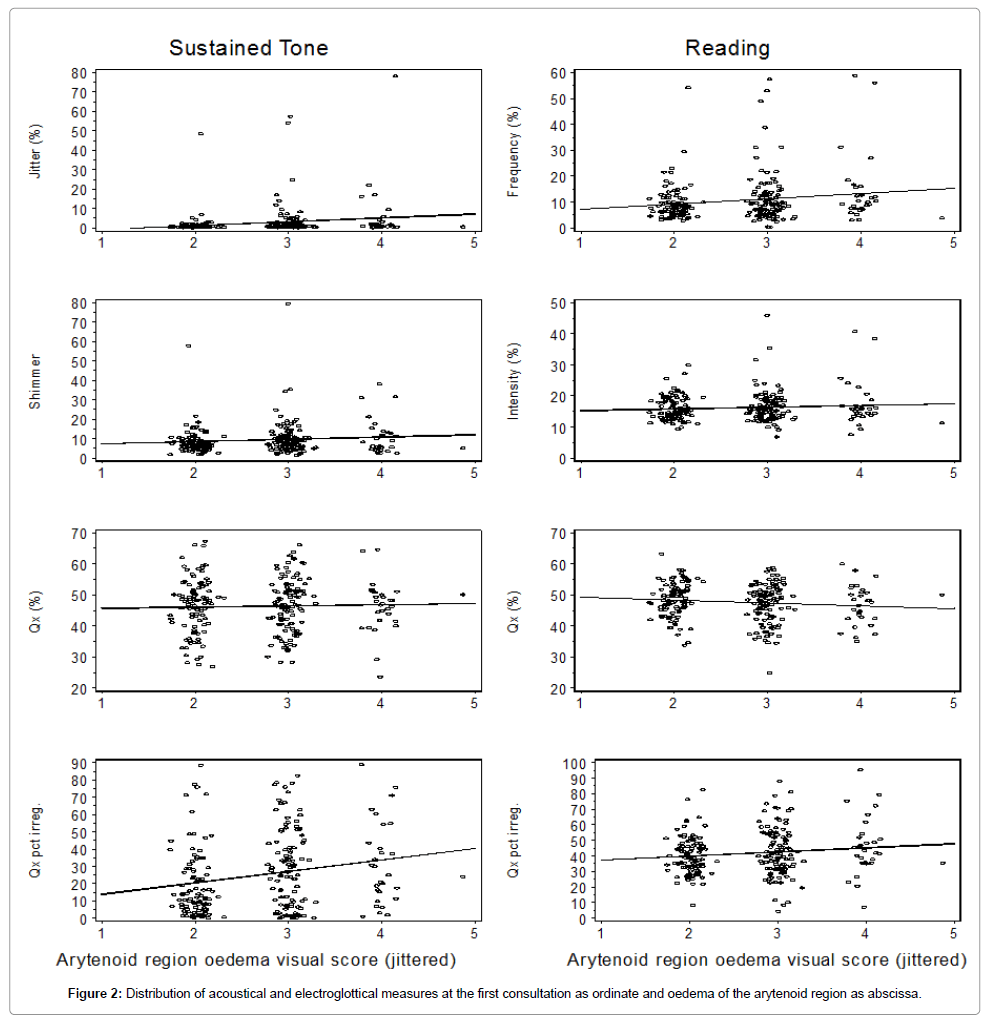
Figure 2 shows the distribution of voice related acoustical and electroglottographical measures in percentage for sustained tones and reading of a standard text at the first consultation as ordinate and oedema of the arytenoid region as abscissa.
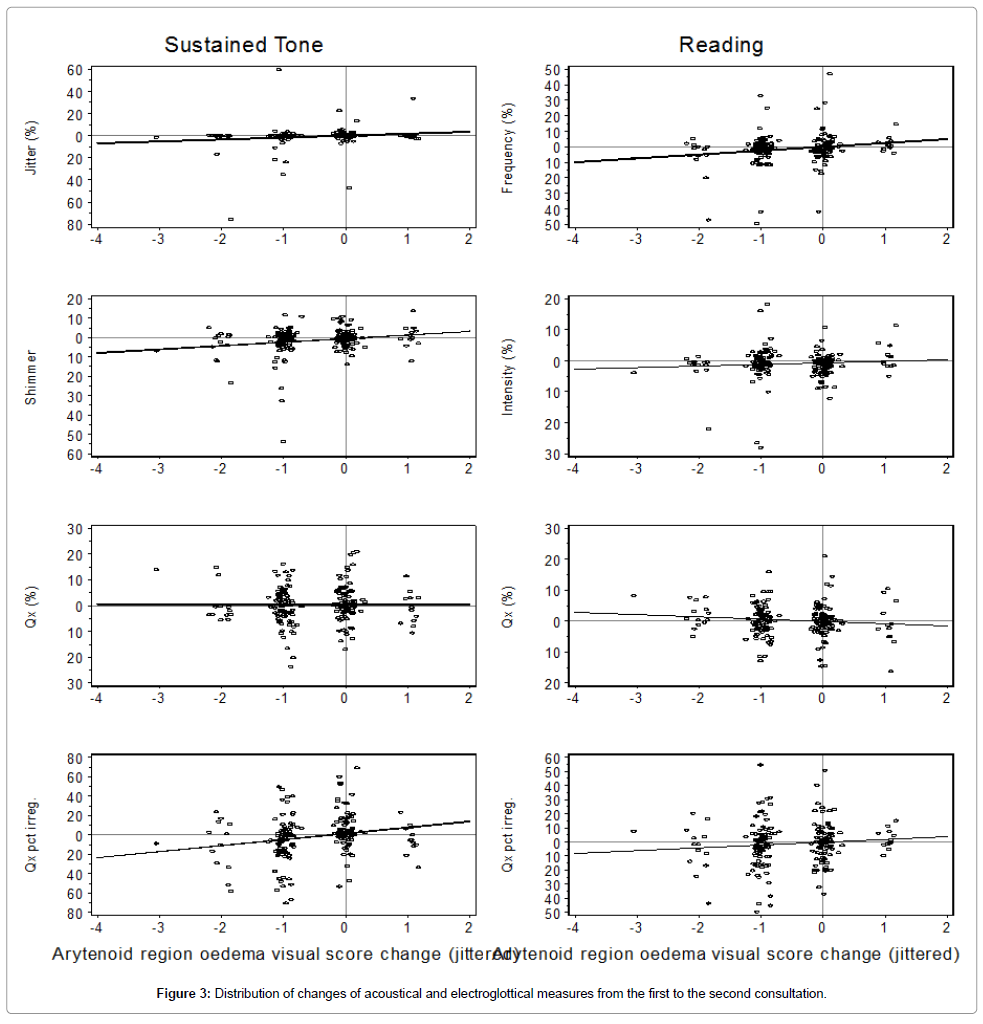
Figure 3 shows the distribution of changes of voice related acoustical and electroglottographical measures in percentage from the first to the second consultation as ordinate and arytenoid oedema as abscissa.
Discussion
We have made a prospective randomized controlled trial of LPR based on subjective complaints treated with lifestyle correction and two added medications, with high speed films as an objective inclusion parameter. No acoustical differences were found between the three groups, therefore we combined them. The voice related acoustical measures were only weakly associated with the swelling of the arytenoid regions based on the used measures, and could therefore not replace the visual inspection of the arytenoid regions at the second examination with high speed films.
There was a significant reduction of the oedema of the arytenoid region at the second examination and a further reduction at the third consultation after 3 months in the study. Since high speed films and acoustical analyses have not been compared before references cannot be given for comparison, And as we have shown, mostly too small materials have been used earlier, for acoustical measures and video stroboscopy and reflux [1].
A statistical significant reduction of frequency and intensity variation in percentage in reading of a standard text was found at the second as well as the third examination. A reduction of shimmer percentage of sustained tones was also found at the second and third examination. Therefore it is suggested that acoustical focus on reflux treatment is made in patients of the two parameters.
The parameter EGG is interesting but without change. The parameter is found optimized in high-speed film and quantitative kymography films. Still no evidence of the value of the parameter in our LPR research study is found.
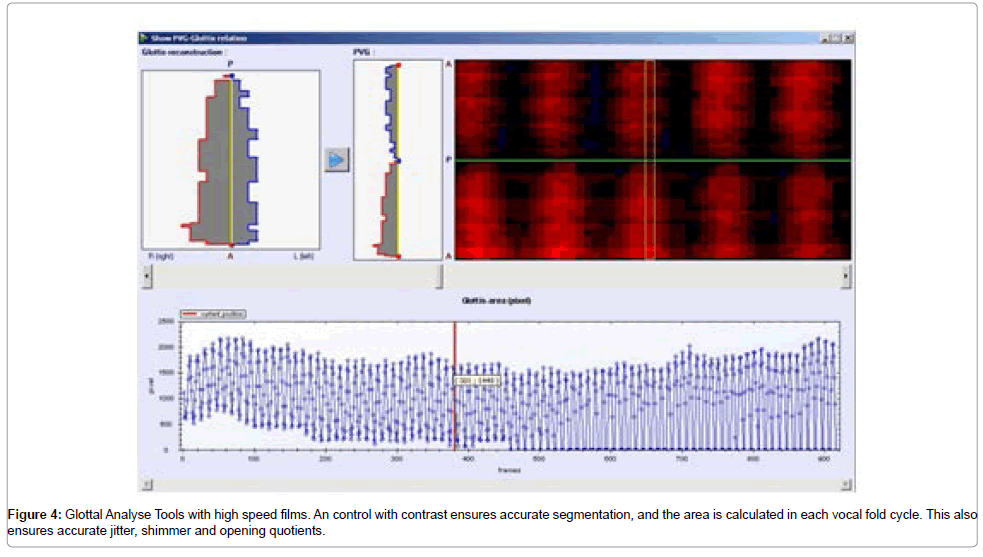
Table 3 presents the Glottis Analyse Tools, online on highspeed films for vocal fold dynamics for each vocal fold with the Phonovibrogram in one of our patients. It can be combined with high speed films for online measures, acoustical parameters and stiffness of vocal cords [16-19]. The principle is better than the presented MDVP, which is not online with the films of the larynx (Figure 4).
| Jitt(%) | 0.542 | ||||
| HNR(dB) | 11.098 | ||||
| Shim (%) | 5.048 | ||||
| Mean | Std | Min | Max | ||
| ClosingQuotient(CQ) | 0.4149 | 0.0602 | 0.2727 | 0.5455 | |
| AsymmetrieQuotient | 0.4872 | 0.0721 | 0.3333 | 0.5833 | |
| Stiffness | Left | 0.4919 | 0.1902 | 0.254 | 0.9897 |
| Stiffness | Right | 0.4769 | 0.1664 | 0.2625 | 0.8411 |
Table 3:A glottal analysis tool to be used in the future, combined with high speed films is shown for online measures, acoustical parameters and stiffness of vocal cords.
The use of arytenoid oedema visual scores 1-5, on high speed films might be a prognostic parameter. In the future it might be possible to evaluate the oedema of arytenoid areas with optical coherence tomography as a supplementary mucosal diagnostic factor in speakers and in singers, once all voice clinics have the high (cheaper) speed films as a clinical basic routine [20].
Conclusion
In our MDVP study based on the advanced acoustical set-up by Laryngograph Ltd. referring to research by Fourcin and Abberton, a randomised prospective study of three different treatment aspects of LPR were made, life style change alone being important. No difference between the three treatment groups was found. There was an acoustical measured reduction in all groups of reading frequency and intensity variation and shimmer. The relations between changes in the MDVP measurements and the changes in arytenoid swelling were found to be weak. In this study oedema of the arytenoid regions oedema seen on high speed films seemed to be a prospective factor for treatment effect as well as acoustical measures with MDVP by Laryngograph Ltd.
Acknowledgements
Anne B. Alexius Agersted (medical student, University of Copenhagen) helped with preparing the manuscript. Anders Overgård Jønsson (medical student, University of Copenhagen). Sanila Mahmood (pharmacy student, University of Copenhagen).
References
- Hopkins C,Yousaf U, Pedersen M(2006) Acid reflux treatment for hoarseness. Cochrane Database Syst Rev CD00505
- Committee for medical products for human use (CHMP) (2009 ) Guideline on the evaluation of drugs for the treatment of gastroesophageal reflux disease. European Medicines Agency, London.
- Karkos PD,Potamianos SP, Apostolidis MT, Kekes G(2006)When gastroenterology met otolaryngology: laryngopharyngeal reflux. Am J Med 119:e19-e20
- Lin CC, Wang YY, Wang KL (2009) Association of heartburn and laryngopharyngeal symptoms with endoscopic reflux esophagitis, smoking and drinking. Otolaryngol Head Neck Surg 14:264-271.
- Cheung TK, Lam PK, Wei WI, Wong WM, Ng ML, et al. (2009) Quality of life in patients with laryngopharyngeal reflux. Digestion 79: 52-57
- Gupta R, Sataloff RT(2009) Laryngopharyngeal reflux, current concepts and questions. CurrOpinOtolaryngol Head Neck Surg17:143-148
- Vaezi MF(2008) Laryngeal manifestations of gastroesophageal reflux disease. CurrGastroenterol Rep 10: 271-277
- Ulis JM, Yanagisawa E (2009)What’s new in differential diagnosis and treatment of hoarseness? CurrOpinOtolaryngol Head Neck Surg 17: 209-215
- Fass R, Noelck N, Wilis MR (2010) The effect of esomeprazole 20 mg twice daily on acoustic and perception parameters of the voice in laryngopharyngeal reflux. NeurogastroenterolMotil 22:134-141.
- Siupsinskiene N, Adamonis K, Toohill RJ(2009) Usefulness of assessment of voice capabilities in female patients with reflux-related dysphonia. Medicina (Kaunas). 45:978-987
- Maryn Y, Roy N, De Bodt M, Van Cauwenberge P, Corthals P(2009) Acoustic measurement of overall voice quality: a meta-analysis. J AcoustSoc Am 126:1619-2634
- Wang X (2012) Auditory and Visual Training on Mandarin Tones: A Pilot Study on Phrases and Sentences. Int J Computer-assisted Learning and Teaching 2:16-29.
- Pedersen M, Munck KA (2007) prospective case-control study of jitty % shimmer% and Qx%, glottis closure cohesion factor (Spead by Laryngograph Ltd.) and long Time Average Spectra. Congress report: Models and analysis of vocal emissions of biomedical applications (MAVEBA); 60-64.
- Pedersen M(2014) Acoustical voice measurements did change after treatments in patients with laryngo-pharyngeal reflux: A prosective randomized study including MDVP (laryngograph Ltd.) Journal of Rhinolaryngo-Otologies 2:67-73.
- Fourcin A, Abberton E, Miller D, Howells D (1995) Laryngograph: speech pattern element tools for therapy, training and assessment. Int J Language Communication Disorders 30:101-115
- OGuz H, Kilic M, Safak M (2011) Comparison of results in two acoustic analysis programs: Praat and MDVP. Turk J Med Sci 41:835-841
- Voigt D, Döllinger M, Yang A, Eysholdt U, LohschellerJ (2010)“Automatic diagnosis of vocal fold paresis by emplyingPhonovibrogramfeautures and machine learning methods”.Comput Methods Programs Biomed 99:275-288.
- Voigt D, Döllinger M, Braunschweig T, Yang A, Eysholdt U, et al. (2010) Classification of functional voice disorders base don Phonovibrograms. ArtifIntell Med 49:51-59.
- Döllinger M, Lohscheller J, McWhorter A, Kunduk M (2009) Variability of normal vocal fold dynamics for different vocal loading investigated by Phonovibrograms. Journal of Voice 23:175-181
- Pedersen M(2014) Future aspects of cellular and molecular research in clinical voice treatment. Advances in cellular and molecular otolaryngology 2:24442
Relevant Topics
- Addiction
- Adolescence
- Children Care
- Communicable Diseases
- Community Occupational Medicine
- Disorders and Treatments
- Education
- Infections
- Mental Health Education
- Mortality Rate
- Nutrition Education
- Occupational Therapy Education
- Population Health
- Prevalence
- Sexual Violence
- Social & Preventive Medicine
- Women's Healthcare
Recommended Journals
Article Tools
Article Usage
- Total views: 15752
- [From(publication date):
April-2015 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 11154
- PDF downloads : 4598