Lower or Upper Approach; Catheter Ablation of Supraventricular Arrhythmia in a Patient with Azygos Continuation of Inferior Vena Cava
Received: 15-Jul-2017 / Accepted Date: 08-Aug-2017 / Published Date: 11-Aug-2017
Abstract
The catheter ablation of supraventricular arrhythmias is generically performed via using a trans femoral venous approach through the inferior vena cava (IVC). However, this procedure becomes a subtle issue if there is a congenital or an acquired obstruction of the IVC. Here, we report a very particular case of slow pathway ablation for atrioventricular nodal reentrant tachycardia in a patient with an interrupted vena cava by virtue of the lower approach.
Keywords: Azygos continuation of interrupted IVC; Polysplenia; Catheter ablation; Atrioventricular nodal reentrant tachycardia (AVNRT)
24221Introduction
The success of catheter ablation for treatment of cardiac arrhythmias has led to the extensive use of this therapy. Recall that the catheter ablation is usually performed via the femoral vein. But, the interruption of IVC with azygos continuation which is resulted from either the congenital or acquired causes can occasionally prevent catheter access to the right atrium (RA). The prevalence of interrupted IVC with azygos continuation is 0.1-0.3% in patients without congenital heart disease [1]. In this case, we will introduce a successful ablation of slow pathway through the femoral vein in a patient with the azygos continuation of interrupted IVC and polysplenia.
Case Presentation
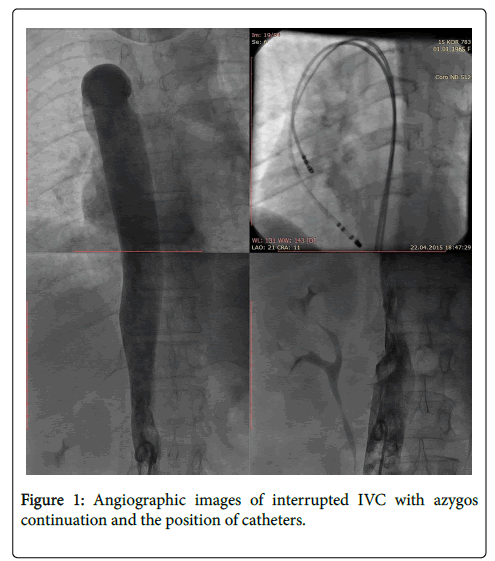
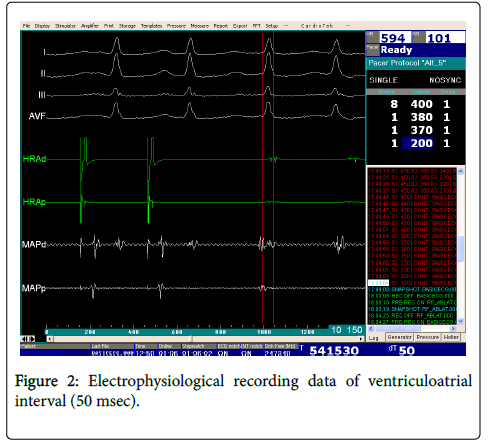
A 53-year-old female patient was admitted to the hospital with the symptoms of palpitation and dizziness which lasted one hour with a frequency of 3-4 times in a month even if she was using various antiarrhythmic drugs. Physical examination and laboratory findings were normal. A 12-lead electrocardiogram (ECG) during sinus rhythm confirmed the absence of ventricular pre-excitation and other abnormality. In the patient’s previous ECG, we saw the existence of regular narrow QRS tachycardia with the rate 180−200 bpm which led us to the atrioventricular nodal reentrant tachycardia (AVNRT). Echocardiographic examination showed us that the hepatic veins were draining directly into the right atrium. Abdominal computed tomography revealed the polysplenia and interrupted IVC with dilated azygos continuation. After the informed consent, the patient was taken to the electrophysiology laboratory. In the venography, the interrupted IVC with dilated azygos continuation and drainage to the right atrium were seen (Figure 1). Thereafter, two venous sheaths were placed into the right femoral vein. Subsequently, a diagnostic quadripolar catheter (Soloist, Medtronic, MN, USA) and a 4 mm curve RF ablation catheter (Marinr, Medtronic, MN, USA) were advanced from the right femoral vein through the superior vena cava via the azygos continuation and finally to the right atrium (see the right upper of Figure 1). Since the azygos vein was so dilated, there was no difficulty as we passed through it. After that, the programmed stimulation from the RA induced slow-fast atrioventricular nodal reentrant tachycardia (AVNRT) with a cycle length of 330 msec (Figure 2). Here, the use of tachycardia entrainment via ventricular pacing was useful in differential diagnosis of supraventricular tachycardias. The difference in the AH interval between atrial pacing and the tachycardia could also allow differentiation of atypical AVNRT from other types of long RP tachycardias. The ventriculoatrial (VA) interval and tachycardia cycle length (TCL) were measured during tachycardia, and entrainment of the tachycardia was accomplished with RV apical pacing. The intervals between the last ventricular pacing stimulus and entrained atrial depolarization during tachycardia (SA) as well as the post-pacing interval (PPI) were considered. In this case, we saw that the SA-VA and PPI-TCL intervals were 95 and 130 msec, respectively. Thereafter, radiofrequency energy was delivered to the posterior aspect of Koch’s triangle where slow pathway potentials were observed. After the ablation, no tachycardia was induced and also no dual AV node conduction properties were detected. Without any antiarrhythmic medication, the patient was discharged in the next day. After three months, it was observed that the patient was still asymptomatic and remained in sinus rhythm.
Discussion
The most common anomaly involving IVC is the absence of infrahepatic segment and connection to the superior vena cava (SVC) through the azygos vein [2]. In this respect, the IVC is interrupted above the level of renal veins and thus the systemic venous drainage which is below the interruption runs into the SVC via an enlarged azygos vein. Additionally, the hepatic veins typically drain through the residual orifice of IVC into the RA. Our case has demonstrated an angiography of azygos continuation IVC with polysplenia. Recall that the IVC with azygos continuation frequently associated with complex congenital malformations as a polysplenia syndrome [3]. Although anomalies of the venous system may complicate catheter ablation strategies in different types of arrhythmias, successful radiofrequency ablation (RFA) of AVNRT, pulmonary vein isolation to treat atrial fibrillation have been previously reported [4,5]. As is known, the positioning and manipulation of the catheters for recording and mapping are more difficult due to the longer course and sharp angulation of azygos vein entering the SVC. In the literature, some of authors have used the lower venous approach in order to access into the right atrium while the others have preferred the superior venous approach for ablation of different arrhythmias. The most common access to the heart is from the femoral approach and this technique is highly effective and safe. Conversely, the upper approach has been recommended to improve catheter stability and achieve higher temperature in the tip-tissue interface by Schluter M et al. Due to its common practice, we have used the long sheath and lower approach and left the upper approach for more complex ablation that needs more stability of catheter. Furthermore, the interruption of IVC may be technically challenging, but it does not preclude RFA as one of therapeutic modalities.
Conflict of Interest
All authors have no declare
References
- Minniti S, Visenti S, Procacci C (2002) Congetinal anomalies of te venae cavae:embryological origin, imaging features and report of three new variants. Eur Radiol 12: 2040-2055.
- Mayo J, Gray R, St Louis E (1983) Anomalies of the inferior vena cava. Am J Roentgenol 140: 339-345.
- Sharma S, Devine W, Anderson RH, Zuberbuhler JR (1987) Identification and analysis of left atrial isomerism. Am J Cardiol 60: 1157-1160.
- Miranda R, Simpson CS, Nolan RL, Diez JC, Michael KA, et al. (2010Superior approach for radiofrequency ablation of atrioventricular nodal reentrant tachycardia in a patient with anomalous inferior vena cava with azygos continuation. Europace 12: 908-909.
- Lim HE, Pak HN, Tse HF, Lau CP, Hwang C, et al. (2009) Catheter ablation of atrial fibrillation via superior approach in patinets with interruption of inferior vena cava. Heart Rhythm 6:174-179.
Citation: Baysal E, Burak C, Alyan O (2017) Lower or Upper Approach; Catheter Ablation of Supraventricular Arrhythmia in a Patient with Azygos Continuation of Inferior Vena Cava. J Card Pulm Rehabil 1: 112.
Copyright: © 2017 Baysal E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 4787
- [From(publication date): 0-2017 - Aug 23, 2025]
- Breakdown by view type
- HTML page views: 3899
- PDF downloads: 888