Case Report Open Access
Malignant Squamous Changes in Unicystic Ameloblastoma:A Case Report and Review of Literature
AnkitaTandon*Faculty of Dentistry, Jamia MilliaI slamia, New Delhi, India
- Corresponding Author:
- AnkitaTandon
Faculty of Dentistry, Jamia Millia Islamia
New Delhi, India
Tel: 9891987040
E-mail: drankitatandon7@gmail.com
Received date: March 20, 2014; Accepted date: June 30, 2014; Published date: July 7, 2014
Citation: Tandon A (2014) Malignant Squamous Changes in Unicystic Ameloblastoma: A Case Report and Review of Literature. J Interdiscipl Med Dent Sci 2:132. doi:10.4172/2376-032X.1000132
Copyright: © 2014 Tandon A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use,distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
Unicystic ameloblastoma, a variant of solid or multicystic ameloblastoma is commonly reported to occur in third decade and encountered in the posterior mandible with a biologically low-grade course and with limited recurrence potential. Clinically, it frequently manifests as a painless swelling, which can be accompanied by facialde formity, malocclusion and paresthesia of the affected area. Histologically, the minimum criterion for diagnosing a lesion as unicystic ameloblastoma is the demonstration of a single cystic sac lined by odontogenic (ameloblastomatous) epithelium often seen only in focal areas whereas radiographically they represent a unilocular radiolucency. This report however, is first to show malignant squamous conversion of unicystic ameloblastoma lining in a 35 year old female patient.
Keywords:
Unicysticameloblastoma; Carcinoma; Enucleation
Introduction
The concept of unicysticameloblastoma was first introduced by Robinson and Martinez in 1977 [1]and later this was variously termed as mural, monocystic, intracystic, cystogenic, or cystic ameloblastoma [1].It occurs at a mean age of 22 years and is located commonly in the mandible (mandible to maxilla=3 to 13:1) with female: male preponderance of approximately1:1.3 [2].It is a unilocular, cystic lesion whose clinical features are similar to a non-neoplastic cyst [3].The unicysticameloblastoma deserves special consideration on the basis of its clinical & radiologic appearance, its histopathology, and its response to treatment.The importance of the unicysticameloblastoma is that it possesses a much better prognosis after enucleation or curettage than does the classic intraosseousameloblastoma [1].
Our case, on the contrary highlights a more aggressive counterpart of unicysticameloblastoma in which the lesion shows dysplastic features (carcinomatous changes) to a great extent. This case represents first among the category of malignant transformation of unicysticameloblastoma lining; which however, is reported on and often among classical ameloblastomas. Also,a brief review of malignant changes within ameloblastomas of maxillofacial region is presented herewith.
Case Report
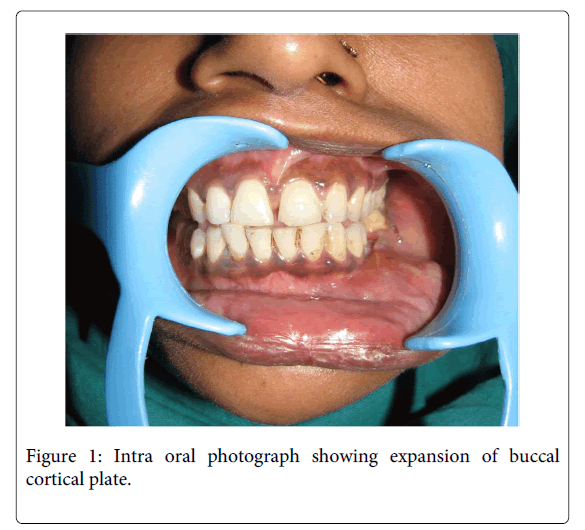
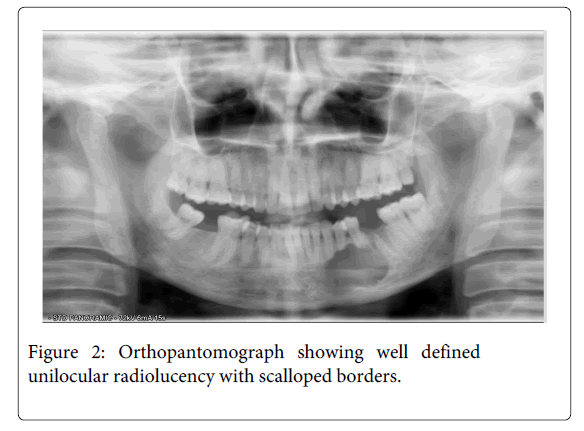
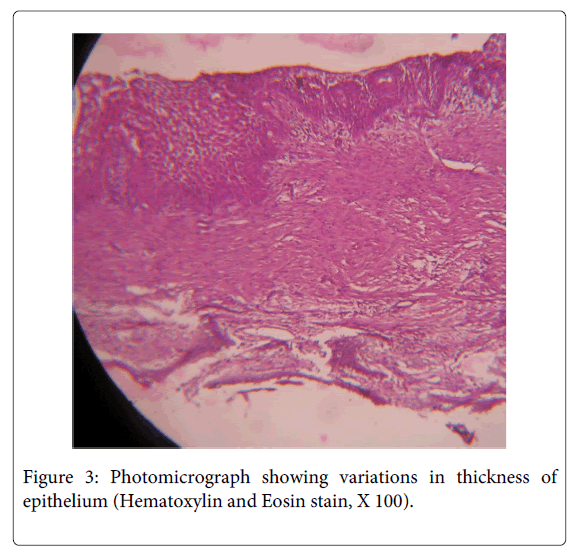
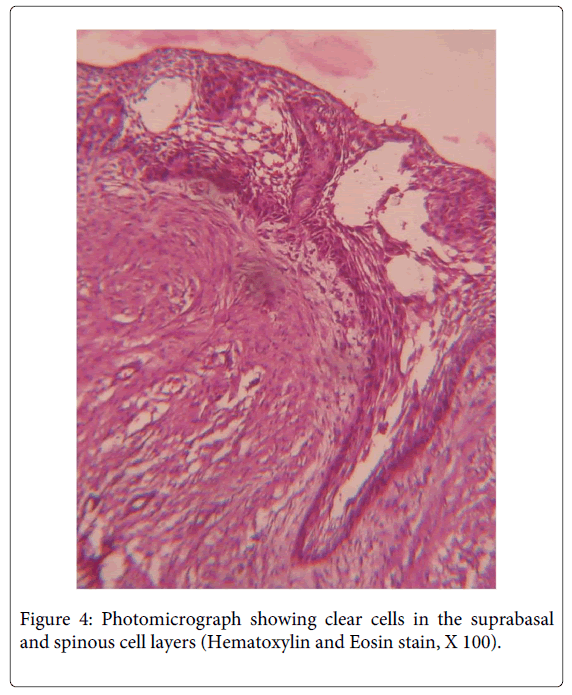
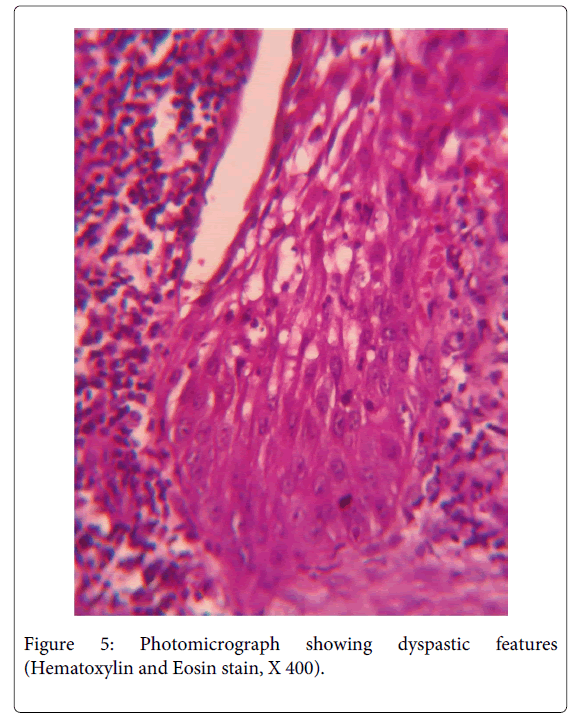
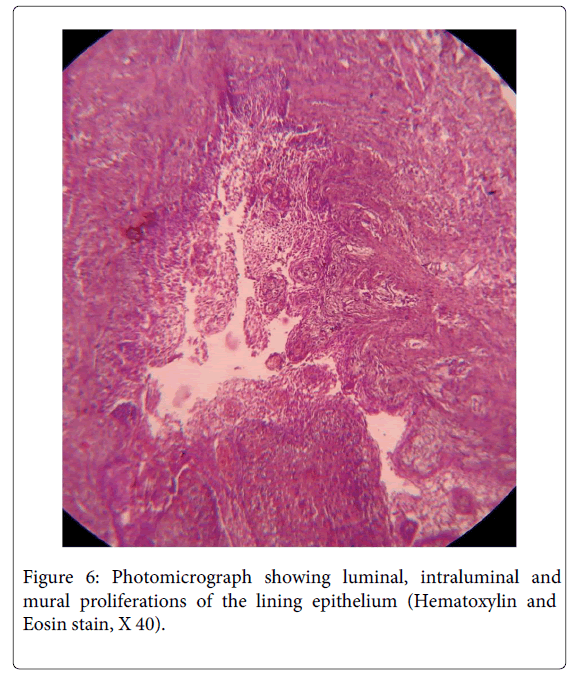
A 35 year old female patient visited the Department of Oral Pathology, with the chief complaint of pain andswelling in the left lower back teeth region since 5 months. On examination, extraorally, a smooth and diffuse swelling was located in left lower cheek region causing facial asymmetry, measured approximately 4x5 cm in dimensions and extended from angle of mouth to mid body region antero- posteriorly. This was associated with dull pain and was tender on palpation. Intra orally, the swelling was present in 33 to 36 region, measured approximately 4x6 cm, was smooth surfaced and had an open socket in relation to 36 (Figure 1). The lesion also presented expansion of left buccal cortical plate and obliteration of the left buccal vestibule. An orthopantomographic evaluation revealed a well-definedunilocular radiolucency with scalloped borders extending from 31 to 36 region anteroposteriorly (Figure 2). Based on the above mentioned findings, a differential diagnosis of odontogenickeratocyst, radicular cyst and unicysticameloblastoma were made. The aspirate was drawn and micro protein estimation value was found to be 9.8 gm% which ruled out the possibility of odontogenickeratocyst. Following this, enucleation was performed with application of Carnoy’s solution at the margins. The histopathology of the sections stained with H & E revealed the presence of stratified squamous epithelium overlying inflamed fibrocellular connective tissue stroma. The epithelial lining facing the lumen was variable in thickness from 4-5 layers to extensive proliferations of upto 15 layers at places (Figure 3). The basal layer appeared to be well defined columnar to cuboidal with polarization of nuclei along with heaping up of superficial cells and suspension of a few clear cells in the suprabasal and spinous cell layers (Figure 4).The epithelial lining at places significantly revealed dysplastic features with hyperchromatism, increased nucleo cytoplasmic ratio, increased mitotic figures, cellular and nuclear pleomorphism (Figure 5) along with massive epithelial proliferations both towards the lumen (luminal/intraluminal) as well as towards the connective tissue wall (mural) (Figure 6). The underlying connective tissue stroma had collagen fibre bundles with fibroblasts, chronic inflammatory cell infiltration chiefly of lymphocytes, endothelium lined blood vessels with few extravasated RBCs and irregular trabeculae of bone with osteocytes and osteoblastic rimming.
Correlation of histopathological, radiographic and clinical features supported a diagnosis of UnicysticAmeloblastoma (UA 1.2.3) with early carcinomatous change. The postoperative course was uneventful and at the one-year follow-up, there was no evidence of recurrence.
Discussion
Leider et al. [2] has proposed three pathogenic mechanisms for the evolution of unicysticameloblastoma : (1) the reduced enamel epithelium associated with a developing tooth undergoes ameloblastic transformation with subsequent cystic development; (2) ameloblastomas may arise in a dentigerous or other type of dental cyst in which the neoplastic ameloblastic epithelium is preceded temporarily by a non-neoplastic stratified squamous epithelial lining; (3) a solid ameloblastoma undergoes cystic degeneration of ameloblastic islands with subsequent fusion of multiple microcysts to develop a unicystic lesion.
Unicysticameloblastoma most commonly manifest facial disfigurement with noticeable swelling which coincides with the clinical presentation of the lesion in our case. The most common site for the occurrence of unicysticameloblastoma in the mandible is the third molar area but mandibular body region is not an uncommon site for its occurrence as was also reported in our case.Unicysticameloblastoma represents a cyst that is lined by Ameloblastomatous epithelium [2]. This epithelium may grow exophytically in the cyst lumen forming intraluminal nodules, or it may invade the fibrous cyst wall [1].
Yavagal et al. [4] revealed that although cystic ameloblastomas follow a biologically low-grade course, recent evidence suggests that they may often behave as biologically aggressive tumors. This is supported by the high incidence of cortical perforation, tooth resorption, lesion size, bone destruction, and a high rate of recurrence after simple enucleation. Epithelial-mesenchymal interactions are essential in pathogenesis of these type of lesions which is brought about through modification of the extracellular matrix/stroma.Fibroblasts, the cells that synthesize collagen undergo changes in response to tumorigenesis in adjacent epithelial cells. These changes in fibroblasts bring about alteration of collagen fibres, affecting their quality and organization [5]. This aggressive biological behaviour is also strongly supported by numerous immunohistochemical studies which confirm the presence of proliferation and aggressiveness markers in unicysticameloblastoma (Table 1).
| Reference | Markers | Expression |
|---|---|---|
| Altini M et al. [6],(1987) | Stromal myofibroblasts (MF) | Marked expression |
| Li TJ [7], (1995) | PCNA & Ki-67 | Marked expression in invading islands |
| el-Sissy NA[8] , (1999) | p53 | Marked expression |
| E-cadherin | Weak positive expression | |
| ß catenin | Marked expression | |
| Piatelli A et al. [10], (2003) | Calretinin | Marked expression |
| Hande AH [11], (2011) | CD105 | Marked expression |
Table 1: Expression of immunohistochemical markers in unicysticameloblastoma
Review of malignant changes arising from ameloblastomas in existing English literature could reveal only a few cases which have been summarised in Table 2. To the best of our knowledge, the case presented here is first to showmalignant squamous conversion of ameloblastomatous epithelium in unicysticameloblastoma. Unicystic-type ameloblastoma are generally removed as a dentigerous cyst without preoperative biopsy, and all of the tissue must be included for a proper diagnosis [12]. Hence, the treatment performed was surgical enucleation with mechanical curettage following application of Carnoy’s solution on the margins to remove the residual tissue bits, if any. After 1 year of follow-up no recurrence was detected [18].
| S. no | Reference | Location | Diagnosis |
|---|---|---|---|
| 1 | VILLA VG [13] (1952) | Intraosseous mandibular ameloblastoma | Ameloblastoma developing into epidermoid carcinoma. |
| 2 | Baden E et al. [14] (1993) | Peripheral maxillary ameloblastoma | Malignant transformation of peripheral ameloblastoma |
| 3 | Ueta E et al. [15] (1996) | Intraosseous mandibular ameloblastoma | Intraosseous carcinoma arising from mandibular ameloblastoma with progressive invasion and pulmonary metastasis. |
| 4 | Nthumba PM [16](2011) | Intraosseous mandibular ameloblastoma | Squamous cell carcinoma in an orocutaneous fistula of a large mandibular ameloblastoma |
| 5 | Ahuja A et al. [17] (2012) | Intraosseous mandibular ameloblastoma | Acanthomatous ameloblastoma masquerading as a squamous cell carcinoma. |
| 6 | Present case | Intraosseous mandibular unicystic ameloblastoma | Unicystic Ameloblastoma (UA 1.2.3) with squamous malignant change |
Table 2: Review of malignant squamous changes in ameloblastoma
To conclude, it is important to keep in mind that, in general, unicysticameloblastomas are solitary lesions with less aggressive behaviour in comparison to classical ameloblastomas. However, the clinicians should be aware of the possibility malignantsquamous changes in unicysticameloblastoma lining manifested as early carcinomatous change. These types should be treated carefully and a follow up phase is mandatory as they may be associated with recurrences.
References
- Gardner DG (1996) Some current concepts on the pathology of ameloblastomas. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 82: 660-669.
- Philipsen HP, Reichart PA (1998) Unicystic ameloblastoma. A review of 193 cases from the literature. Oral Oncol 34: 317-325.
- Rajendran R (2006) Cysts and tumors of odontogenic origin. (5th edn), Shafer’s textbook of Oral Pathology.
- Yavagal C, Anegundi RT, Shetty S (2009) Unicystic plexiform ameloblastoma: an insight for pediatric dentists. J Indian Soc Pedod Prev Dent 27: 70-74.
- Bergers G, Coussens LM (2000) Extrinsic regulators of epithelial tumor progression: metalloproteinases. Curr Opin Genet Dev 10: 120-127.
- Altini M, Cohen M (1987) Experimental extra-follicular histogenesis of follicular cysts. J Oral Pathol 16: 49-52.
- Li TJ, Browne RM, Matthews JB (1995) Expression of proliferating cell nuclear antigen (PCNA) and Ki-67 in unicystic ameloblastoma. Histopathology 26: 219-228.
- el-Sissy NA (1999) Immunohistochemical detection of p53 protein in ameloblastoma types. East Mediterr Health J 5: 478-489.
- Toshihiko A, Motohiko N, Hiroshi T (2001) Clinicopathological and immunohistochemical studies of unicystic ameloblastoma. Journal of Gifu Dental Society 28:7-31.
- Piattelli A, Fioroni M, Iezzi G, Rubini C (2003) Calretinin expression in odontogenic cysts. J Endod 29: 394-396.
- Hande AH, Gadbail AR, Sonone AM, Chaudhary MS, Wadhwan V, et al. (2011) Comparative analysis of tumour angiogenesis in solid multicystic and unicystic ameloblastoma by using CD 105 (endoglin). Arch Oral Biol 56: 1635-1640.
- Jivan V, Altini M, Meer S, Mahomed F (2007) Adenomatoid odontogenic tumor (AOT) originating in a unicystic ameloblastoma: a case report. Head Neck Pathol 1: 146-149.
- VILLA VG (1952) Ameloblastoma developing into epidermoid carcinoma. Acta Med Philipp 9: 137-145.
- Baden E, Doyle JL, Petriella V (1993) Malignant transformation of peripheral ameloblastoma. Oral Surg Oral Med Oral Pathol 75: 214-219.
- Ueta E, Yoneda K, Ohno A, Osaki T (1996) Intraosseous carcinoma arising from mandibular ameloblastoma with progressive invasion and pulmonary metastasis. Int J Oral Maxillofac Surg 25: 370-372.
- Nthumba PM (2011) Squamous cell carcinoma (Marjolin's ulcer) in an orocutaneous fistula of a large mandibular ameloblastoma: a case report. J Med Case Rep 5: 396.
- Ahuja A, Mathur S, Iyer VK (2013) Acanthomatous ameloblastoma masquerading as a squamous cell carcinoma. Cytopathology 24: 344-345.
- Kamath VV, Satelur K, Yerlagudda K (2012) Spindle cell variant of ameloblastic carcinoma arising from an unicystic amelobastoma: Report of a rare case. Dent Res J (Isfahan) 9: 328-333.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 15367
- [From(publication date):
August-2014 - Aug 28, 2025] - Breakdown by view type
- HTML page views : 10585
- PDF downloads : 4782