Case Report Open Access
Metastatic Urothelial Cancer of the Bladder Cancer Presented for the First Time in its Final Stage: Case Report and Literature Review
Lorenzo-Gómez MF1*, Padilla-Fernández B1, Arcila-Piedrahita A2, Antúnez-Plaza P3, Valverde-Martínez S1 and Silva-Abuín JM11Department of Urology, Universitary Hospital of Salamanca University of Salamanca, Spain
2School of Medicine of CES University of Medellín, Colombia
3Department of Pathology, Universitary Hospital of Salamanca University of Salamanca, Spain
- Corresponding Author:
- MF Lorenzo-Gomez
Department of Urology
Universitary Hospital of Salamanca University of Salamanca, Spain
E-mail: mflorenzogo@yahoo.es
Received Date: January 11, 2012; Accepted Date: June 22, 2012; Published Date: June 25, 2012
Citation: Lorenzo-Gómez MF, Padilla-Fernández B, Arcila-Piedrahita A, Antúnez- Plaza P, Valverde-Martínez S, et al. (2012) Metastatic Urothelial Cancer of the Bladder Cancer Presented for the First Time in its Final Stage: Case Report and Literature Review. J Palliative Care Med 2:122. doi:10.4172/2165-7386.1000122
Copyright: © 2012 Lorenzo-Gómez MF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Palliative Care & Medicine
Abstract
Introduction: According to the European Urologic Guidelines up to 85% of urothelial cancer of the bladder (UCa) is diagnosed at the non-metastatic stage, being gross haematuria the most common symptom in 70-80% of the cases. This report introduces the case of a T4 G3 metastatic UCa proved to be asymptomatic until its final stage, when an effective treatment is unavailable.
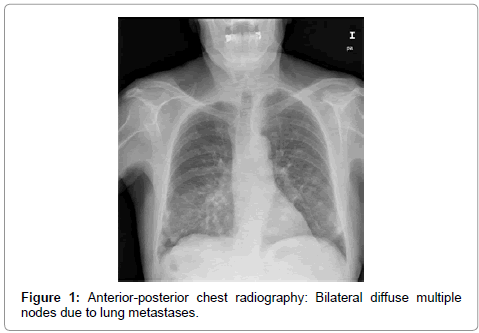
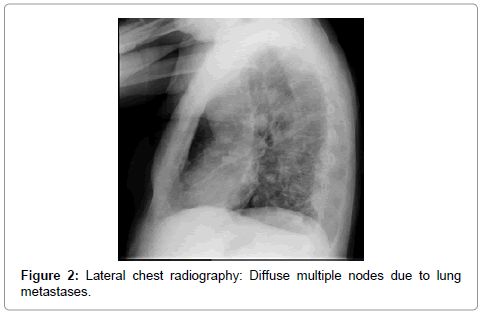
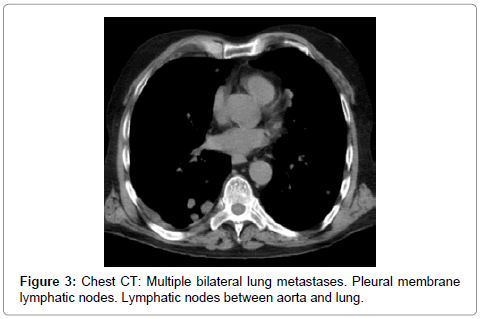
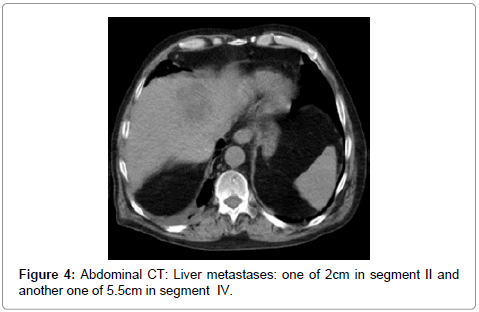
Case report: A 68-year-old male has been presenting dizziness and mild haematuriafor fourteen days before arranging a doctor’s appointment. Physical examination goes as follows: Apyretic, lightly painful, abdomen. Serum creatinine 1.3 mg/dl, Hemoglobin 11.7 gr/dl. Abdominal ultrasound: Both kidneys were standard, bladder contained a heterogeneous mass. History: He remembers a single gross haematuria monosymptomatic episode 12 years before. Three months after the aforementioned episode, a pituitary macroadenoma 7 cm is size was diagnosed and surgically dissected; for this reason, the haematuria drew no attention. The patient had no spouse or close relatives. He had never had other gross haematuria episodes or other urologic symptoms before. Urine cytology: UCa grade 3. Chest radiography: Multiple metastases. Computed Tomography (CT) of thorax-abdomen-pelvis showed pulmonary, pleural, liver, mesenteric and bone metastases; positive lymphatic nodes in pleural membrane and between aorta and lung. Both kidneys were normal. The urinary bladder appeared to be filled with mass. Due to both clinical and personal circumstances, the patient, in agreement with his family, signed up for palliative care only. He passed away out of acute respiratory failure 41 days after the first consult.
Conclusions: Metastatic UCa at diagnosis shows a very poor survival rate. Chemotherapy with methotrexate + vinblastine + adriamicyn + cisplatin can have a success rate of 30%, improving survival to 11-14 months with high toxicity.
Keywords
Advanced bladder cancer; Belated diagnosis; Palliative care
Case Report
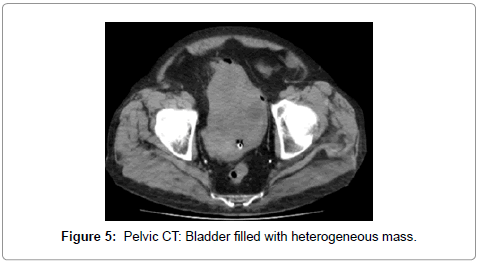
A 68-year-old male presented dizziness and mild haematuria for fourteen days before arranging a doctor’s appointment. Physical examination: Apyretic, lightly painful abdomen. Serum creatinine 1.3 mg/dl, Hemoglobin 11.7 gr/dl. Abdominal ultrasound: Both kidneys were standard, bladder was filled with a heterogeneous mass. History: He remembers a single gross haematuria monosymptomatic episode 12 years before. Three months after the aforementioned episode, a pituitary macroadenoma 7 cm is size was diagnosed and surgically dissected; for this reason, the haematuria drew no attention. The patient had no spouse or close relatives. He had never had other gross haematuria episodes or other urologic symptoms before. Urine cytology: Transitional cancer grade 3. Chest radiography: Multiple metastases (Figure 1 and 2). Computed Tomography (CT) of thoraxabdomen- pelvis showed pulmonary, pleural (Figure 3), liver (Figure 4), mesenteric and bone metastases; and positive lymphatic nodes in pleural membrane and between aorta and lung. Both kidneys were normal. The urinary bladder appeared to be filled with mass (Figure 5). Due to both clinical and personal circumstances, the patient, in agreement with his family, signed up for palliative care only. He passed away out of acute respiratory failure 41 days after the first consult.
Literature Review
Bladder cancer is the ninth most common carcinoma in the world. There are up to 330,000 new diagnoses every year and it is the cause of death of up to 130,000 people per year [1].
Bladder cancer is the most common UCa, the most common urologic tumour in women and the second most common in men. The men/women ratio is of 3:1, at an average of 70 years of age. It appears more frequently in Caucasians. UCa makes up for 95% of bladder cancers. These tumours are considered superficial or nonmuscle- invasive (70%), infiltrative (20%) or metastatic (10-15%). 80% of muscle-invasive transitional cell carcinoma is diagnosed de novo. 15-20% of the patients initially diagnosed with a superficial UCa will develop an invasive tumour [1-3]. 10-15% of patients with muscleinvasive UCa have a metastatic disease at the time of diagnosis [1,4,5]. 50% of patients with infiltrative UCa will develop metastases, most commonly located in liver, lung and bone [1,2,5,6].
Main prognostic factors are treatment timing, concomitant diseases, tumour types, previous treatments, renal and/or hepatic insufficiency, obesity, visceral metastases, functional status of the patient (Karnofsky performance status <80%). These last two factors play the most important role when deciding which treatment a patient is going to undergo [5]. Patients with metastatic UCa who are asymptomatic and have only positive lymph node or single metastases have the best prognosis [1,2,4]. Despite the importance of comorbidity during clinical practice, it is still yet to acquire a significant role in clinical essays or medical statistics [7]. Comorbidities are an important predictor of clinical results [8].
Muscle-invasive UCa has a highly systemic dissemination rate. Combining therapy and surgery, chemotherapy and radiotherapy are the only option of treatment for the patient. Histological studies and prior knowledge of positive lymphatic nodes can help the physician decide whether the patient can benefit from an adjuvant or a neoadjuvant type of chemotherapy [9].
Advanced UCa is chemo-sensitive, but a little number of patients shows a positive response to this treatment, and just for a short time span; drugs with the highest activity rate are cisplatin and methotrexate, showing a 30% response. Survival rate for patients with supportive chemotherapy only lies within a 4 to 6 months ratio. However, this span can be doubled by administering a polychemotherapeutic protocol with the aforementioned drugs [4].
Prior to the introduction of chemotherapy development for UCa, patients with metastases would not survive for more than 3 to 6 months. Prognostic factors should provide a guide to the selection of proper treatment [1].
In non-treatable or metastatic bladder cancer, quality of life is reduced because of associated voiding problems, bleeding and pain, with subsequent social and sexual disruptions [10]. There is little literature available which describes what the quality of life in patients with bladder cancer undergoing palliative care is like, but there are reports of symptoms related to metastatic bladder cancer relieved by means of palliative surgery, radiotherapy and/or chemotherapy [11- 13].
Discussion
We believe the best treatment possible for any given patient is that which provides said patient with the highest level of quality of life and health. When the patient’s health cannot be improved through medical procedures, we believe that choosing the treatment that reduces the patient’s quality of life in the least is the best course of action.
Within the medical literature consulted it is more frequent to find invasive treatment that were successful than to find real data from cases where this was not the case.
There are in existence several publications that feature diverse chemotherapy protocols for patients with UCa Metastases [1,14] but we have not been able to find studies where a comparison between quality of life and survival results among patients who underwent these trial protocols of new lines and therapeutic combinations and palliative care. Fortunately, we do not have a series of oligo-paucisymptomatic that debut at a terminal stage with UCa, therefore we want to make our experience with a unique case widely available.
The case we are reporting on is very rare case in our field. By introducing a patient like the one described, we want to contribute with an unpublished or less often reported type of case. We wish to also bring to light common mistakes that can be made within a health system where the social problems associated with certain patients, and the fact that some pathologies may not be closely monitored by the physician, are matters to be debated. It is certain that we have people in our offices with relevant comorbidities that are not taking into account the proper attention in the case of asymptomatic tumours.
In the case at hand, the absence of close relatives who could have closely followed the course of the disease and the presence of fear, ignorance and disinterest on the patient’s part turned an already dire situation into a much worse one.
The slow progression of the disease has lead us to believe that, in this case, it all began as a superficial and/or low grade tumour, and that it was one of the 15-20% of cases that progress to increasingly aggressive stages.
Comorbidity in patients with advanced UCa is a controversial issue since, as a risk factor, comorbidity is commonly associated with poor outcomes in this kind of patients. In this particular case, the absence of symptoms and the attention given to a different problem (macroadenoma of the pituitary gland) lead to a surprisingly lengthy tumour evolution.
Considering that we have an advanced health system, with modern diagnosis and therapeutic resources, it is very rare for us to find a UCa at its stage without any prior sanitary intervention. Currently, only 4-11% of individuals at advanced ages that present muscle-invasive cancer undergo radical dissecting surgery, with a rate of complications of 24-60%, and a 90-day mortality rate of 10% [15].
Being at the final stage at the time of diagnosis, chemotherapy, radiotherapy or quality-of-life improving surgery could not be prescribed.
For some patients, as it was in this case, clinical and personal circumstances make Palliative Care the best possible choice, provided there is a patient/relatives consensus is reached.
Conclusion
Urothelial cancer of the bladder, metastatic at diagnosis, has a poor survival rate. Chemotherapy with methotrexate + vinblastine + adriamicyn + cisplatin has a response rate of 30%, improving survival 11-14 months with high toxicity.
For some patients, as in the case at hand, clinical and/or personal circumstances make palliative care the best choice possible, provided there is patient-family consensus.
References
- Stenzl A, Cowan NC, De Santis M, Kuczyk MA, Merseburger AS, et al. (2011) Treatment of muscle-invasive and metastatic bladder cancer: update of the EAU Guidelines. Eur Urol 59: 1009-1018.
- Lerner SP (2007) Bladder Cancer in The American Urological Association Educational Review Manual in Urology. CCGPM 405-431.
- Iborra I (2006) Tratamiento de los tumores vesicales superficiales in Tratado de Urología. J Jiménez Cruz, Prous Science Barcelona 1909-1941.
- Albiol S, Bellmunt J (2004) Advanced bladder cancer: new therapeutic stratagies. Med Clin (Barc) 120: 68-77.
- Kurian A, Lee J, Born A (2011) Urothelial bladder cancer with cavitary lung metastases. Can Respir J 18: e46-47.
- Pak K, Kim CJ, Ishida A, Shirasu A, Tomoyoshi T (1987) Statistical survey of metastasis of bladder tumors-from the annual of pathological autopsy cases in Japan. Hinyokika Kiyo 33: 1835-1839.
- Feinstein AR (1970) The pre-therapeutic classification of co-morbidity in chronic disease. Journal of Chronic Diseases 23: 455-468
- Pal SK, Hurria A (2010) Impact of age, sex, and comorbidity on cancer therapy and disease progression. J Clin Oncol 28: 4086-4093.
- Vishnu P, Mathew J, Tan WW (2011) Current therapeutic strategies for invasive and metastatic bladder cancer. Onco Targets Ther 4: 97-113
- Fosså SD, Aaronson N, Calais da Silva F, Denis L, Newling D et al. (1989) Quality of life in patients with muscle-infiltrating bladder cancer and hormone-resistant prostatic cancer. Eur Urol 16: 335-339.
- Rödel C, Weiss C, Sauer R (2005) Organ preservation by combined modality treatment in bladder cancer: The European perspective. Semin Radiat Oncol 15: 28-35.
- Nagele U, Anastasiadis AG, Merseburger AS, Corvin S, Hennenlotter J, et al. (2007) The rationale for radical cystectomy as primary therapy for T4 bladder cancer. World J Urol 25: 401-405.
- Fokdal L, Høyer M, von der Maase H (2006) Radical radiotherapy for urinary bladder cancer: treatment outcomes. Expert Rev Anticancer Ther 6: 269-279.
- Solsona E, Iborra I, Collado A, Rubio-Briones J, Casanova J, et al. (2010) Feasibility of radical transurethral resection as monotherapy for selected patients with muscle invasive bladder cancer. J Urol 184: 475-480.
- Pycha A, Comploj E (2011) The dilemma of cystectomy in old-old and oldest-old patients. Expert Rev Anticancer Ther 11: 1863-1870.
- Sengeløv L, Kamby C, von der Maase H (2001) Metastatic urothelial cancer: evaluation of prognostic factors and change in prognosis during the last twenty years. Eur Urol 39: 634-642.
- Bellmunt J, Albanell J, Paz-Ares L, Climent MA, González-Larriba JL, et al. (2002) Pretreatment prognostic factors for survival in patients with advanced urothelial tumors treated in a phase I/II trial with paclitaxel, cisplatin, and gemcitabine. Cancer 95: 751-757
Relevant Topics
- Caregiver Support Programs
- End of Life Care
- End-of-Life Communication
- Ethics in Palliative
- Euthanasia
- Family Caregiver
- Geriatric Care
- Holistic Care
- Home Care
- Hospice Care
- Hospice Palliative Care
- Old Age Care
- Palliative Care
- Palliative Care and Euthanasia
- Palliative Care Drugs
- Palliative Care in Oncology
- Palliative Care Medications
- Palliative Care Nursing
- Palliative Medicare
- Palliative Neurology
- Palliative Oncology
- Palliative Psychology
- Palliative Sedation
- Palliative Surgery
- Palliative Treatment
- Pediatric Palliative Care
- Volunteer Palliative Care
Recommended Journals
- Journal of Cardiac and Pulmonary Rehabilitation
- Journal of Community & Public Health Nursing
- Journal of Community & Public Health Nursing
- Journal of Health Care and Prevention
- Journal of Health Care and Prevention
- Journal of Paediatric Medicine & Surgery
- Journal of Paediatric Medicine & Surgery
- Journal of Pain & Relief
- Palliative Care & Medicine
- Journal of Pain & Relief
- Journal of Pediatric Neurological Disorders
- Neonatal and Pediatric Medicine
- Neonatal and Pediatric Medicine
- Neuroscience and Psychiatry: Open Access
- OMICS Journal of Radiology
- The Psychiatrist: Clinical and Therapeutic Journal
Article Tools
Article Usage
- Total views: 7895
- [From(publication date):
September-2012 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 3319
- PDF downloads : 4576