Review Article Open Access
Overview of Palliative Surgery: Principles and Priorities
Jennifer Hanna1, Dan G Blazer1,2 and Paul J Mosca1,2*
1Department of Surgery, Duke University Medical Center, Durham, North Carolina, USA
2Division of Surgical Oncology, Department of Surgery, Duke University Medical Center, Durham, North Carolina, USA
- *Corresponding Author:
- Paul J Mosca, M.D, Ph.D, MBA
3116 North, Duke Street
Durham, NC 27704, USA
Tel: (919) 660-2244
Fax: (919) 660-2255
E-mail: paul.mosca@duke.edu
Received date: October 16, 2012; Accepted date: October 25, 2012; Published date: October 28, 2012
Citation: Hanna J, Blazer DG, Mosca PJ (2012) Overview of Palliative Surgery: Principles and Priorities. J Palliative Care Med 2:132. doi:10.4172/2165-7386.1000132
Copyright: © 2012 Hanna J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Palliative Care & Medicine
Keywords
Palliative surgery; Palliative care; Intent; Symptom management; End-of-life; Quality; Education; Training; Research; Policy
Principles of Palliative Surgery
Challenges to progress in palliative surgery begin with an understanding of the term itself. While there are variations on the definition of “palliative surgery”, it generally refers to surgery performed with the intent of improving quality of life or relieving symptoms caused by advanced disease. Palliative surgery is frequently confused with or used interchangeably with noncurative surgery, as demonstrated by a Society of Surgical Oncology survey published in 2002, which revealed that 95% of respondents considered gross residual tumor remaining upon conclusion of an oncologic procedure as synonymous with palliative surgery [1]. In fact, the key difference between palliative and noncurative surgery lies in the intent of surgery, namely the intent to provide asymptomatic patients with an oncologic cure in noncurative surgery versus the intent to relieve symptoms without consideration of oncologic benefit in palliative surgery [2]. As such, the effectiveness of palliative surgery is judged by the presence and durability of patient-acknowledged symptom resolution rather than classic oncologic metrics of negative margins and freedom from residual disease. This emerging definition of palliative surgery is consistent with the established principles of nonsurgical palliative care and forms the basis of the discussion in this special issue of Journal of Palliative Care & Medicine.
Palliative surgery is common in surgical oncology practice, consisting of 10 to 20 percent of all surgery performed [3]. However, while palliative surgery is usually taken to imply that malignancy is the underlying disease process, it is used appropriately as an adjunct to the treatment of a variety of disease processes. And when one considers the palliative nature of numerous vascular, plastic, orthopedic, and ophthalmologic procedures performed for the management nonneoplastic, progressive, life-limiting diseases (such as chronic renal failure), the percentage of surgical procedures performed across all specialties that are palliative in nature may be much higher. Palliative surgery plays a role in both adult and pediatric surgery and spans essentially the entire spectrum of surgical specialties. Though it is often associated with end-of-life care, it may be performed in patients with anticipated long-term survival. As such, many patients undergoing palliative surgical procedures may have a longer predicted survival than some patients undergoing procedures that are not classically viewed as “palliative,” such as hemodialysis access procedures for the management of end-stage renal disease or major amputation for complications of peripheral vascular disease.
In contrast to “palliative surgery”, “surgical palliative care” refers to the application of palliative medicine principles to patients under the care of a surgeon [3]. Examples include symptom control, particularly the management of pain and nausea and communication about goals of care. Certainly, while some surgeons who are experienced in performing palliative surgeries typically have expertise in surgical palliative care, that is not universally the case.
Except for the degree of risk, the moral and ethical questions about palliative surgery are no different from those posed by any other medical treatment for this vulnerable population. The primary ethical challenge inherent in palliative surgery is the balancing of the moral duty to help with the ethical imperatives of nonmaleficence and beneficence. Unchallenged benevolence can undermine autonomy if it masks paternalism and the use of power- a risk for surgeons, who have traditionally been seen as authoritarian and powerful. Other threats to patient autonomy that apply when contemplating any invasive palliative treatment include the paucity of scientific outcomes data for many palliative procedures, patients’ heightened physical, psychological, and social vulnerability, and lack of knowledge by both patients and care providers about less invasive but equally effective alternative treatments. However, the increasing availability of palliative care teams provides the opportunity for an interdisciplinary approach to mitigating these pressures on patients, families, and surgeons to “do something”.
Cytoreductive/Aggressive palliative surgery
Extensive partial or grossly complete tumor extirpation is generically termed cytoreductive or “debulking” surgery. Typically performed in the setting of advanced malignancy, cytoreduction may have two potential benefits. One potential benefit of debulking is symptom control. Another is the potential to enhance disease control and possibly augment disease-free or overall survival. Though one or both of these goals may be achieved, in some cases, neither is achieved. Unfortunately, in the latter scenario, the procedure may have done more harm than good, worsening quality of life and/or shortening life while imparting no benefit.
A classic example of palliative debulking surgery is seen in the treatment or advanced ovarian cancer. Such a patient may have abdominal pain and distension associated with malignant ascites and peritoneal carcinomatosis, and, not uncommonly, may have a bowel obstruction. Optimal cytoreduction not only has the potential to eliminate or alleviate these symptoms, but it may also increase survival [4].
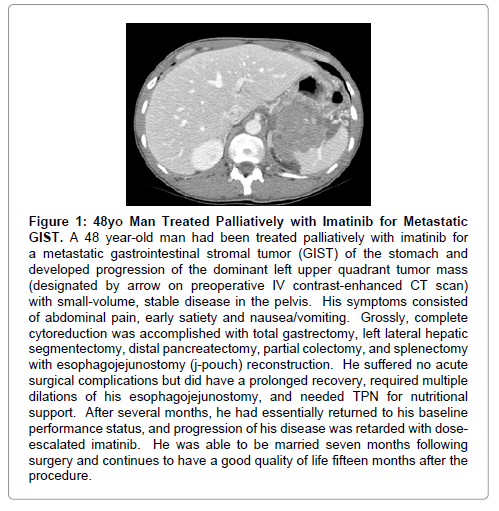
In many cases, however, the potential value of cytoreductive surgery is not so straightforward, such as in the setting of aggressive GI cancers. A vital component of clinical judgment in this area of palliative surgery is thoughtful consideration of technical feasibility and meticulous patient selection with careful attention to patient age, medical co-morbidities and performance status, as well as the patient’s value system, and motivation to undergo major surgery and endure the subsequent recovery period. It is also critically important to compare the risks and potential benefits of major and potentially hazardous interventions with other palliative alternatives, such as minor invasive procedures, medical options, and supportive care alone. In some cases, the only realistic alternative to aggressive surgery may be supportive care or hospice, in which case major surgery would be a more attractive option in a favorable and motivated candidate (Figure 1).
Figure 1: 48yo Man Treated Palliatively with Imatinib for Metastatic GIST. A 48 year-old man had been treated palliatively with imatinib for a metastatic gastrointestinal stromal tumor (GIST) of the stomach and developed progression of the dominant left upper quadrant tumor mass (designated by arrow on preoperative IV contrast-enhanced CT scan) with small-volume, stable disease in the pelvis. His symptoms consisted of abdominal pain, early satiety and nausea/vomiting. Grossly, complete cytoreduction was accomplished with total gastrectomy, left lateral hepatic segmentectomy, distal pancreatectomy, partial colectomy, and splenectomy with esophagojejunostomy (j-pouch) reconstruction. He suffered no acute surgical complications but did have a prolonged recovery, required multiple dilations of his esophagojejunostomy, and needed TPN for nutritional support. After several months, he had essentially returned to his baseline performance status, and progression of his disease was retarded with doseescalated imatinib. He was able to be married seven months following surgery and continues to have a good quality of life fifteen months after the procedure.
A more controversial example of cytoreductive surgery is the noncurative resection of tumor in the asymptomatic patient when there may be no evidence in the literature demonstrating an associated survival benefit. As an example, consider the patient with recurrent retroperitoneal/intra-abdominal sarcoma. In such cases redo surgical resection may be incomplete and may be intended to target specific tumor masses that have exhibited disproportionate growth relative to other sites of disease. One argument given for this type of noncurative resection is that the practice could prevent or delay the onset of future symptoms (e.g., pain or obstruction) and, as such, represents a manner of proactively achieving palliation. Whether surgeries such as this should be performed is uncertain and likely to remain a highly individualized practice, as benefits with respect to symptom control, improved quality of life, or increased survival are uncertain. Moreover, whether such a practice truly constitutes a form of “palliative” surgery, as opposed to simply “noncurative” surgery, is also debatable as interventions are done in advance of patient symptomatology, though preventing these symptoms rather than a true oncologic benefit is the motivation driving resection. The uncertainty surrounding this type of procedure accounts for its frequent incorporation into the spectrum of palliative surgery.
“Curative” resection of primary tumors with short anticipated survival
A variety of difficult oncologic cases are approached with the intent of curative resection, but secondary to the low likelihood of cure and associated short anticipated survival, these procedures can sometimes be thought of as palliative. Patients who undergo palliative orthopedic surgery to stabilize a pathologic fracture from metastatic breast carcinoma have a similar expected median survival as those who undergo a pancreaticoduodenectomy for carcinoma of the pancreatic head [5,6]. Given the expectation that the vast majority of patients undergoing a pancreaticoduodenectomy forpancreatic cancerwill not be cured by the procedure, one might argue that the procedure is palliative in nature. In fact, although this and other types of “potentially curative” resections (e.g., resection of a glioma) are not typically thought of as palliative surgeries, many of the topics discussed in this special issue are as relevant to patients undergoing these procedures as they are to patients undergoing those more traditionally thought of as palliative in nature. It is important to take into account that despite the short survival associated with the majority of these challenging oncologic cases, the primary difference between these “curative” resections and palliative surgery is the intent of surgery from the point of view of both the patient and the surgeon. When these patients are deemed resectable preoperatively, surgery is undertaken regardless of patient symptomatology, with the goal being curative despite the unlikely possibility of achieving such an outcome. However, because of the aggressive nature of these cancers and short associated survival, it forces patients to evaluate their values and motivations for pursuing surgery much in the same way patients considering palliative surgery do.
End-of-life palliative surgery
A common misconception is that palliative surgery is the same as end-of-life surgery. Although palliative care includes hospice care and care near the time of death, it also embraces the management of pain and suffering in medical and surgical conditions throughout life. If palliation is taken to apply solely to care near the time of death, or “comfort measures only,” it fails to include the life-affirming quality of active efforts to relieve the pain and suffering of individuals with chronic illness and injury. In this respect, palliative care is required in the management of a broad range of surgical patients and is not restricted to those at the end of life.
However, end-of-life surgery indeed comprises an important and sizeable component of palliative surgery [7], but there are important distinctions that must be considered. First, while hospice care should be discussed at earlier points in the disease process than is typically the case, certainly in the end-of-life setting, serious consideration should be given to home hospice or even inpatient hospice under appropriate circumstances. Second, the dominant concern in these patients is symptom control and quality of life rather than length of life, which may or may not be the case for patients undergoing palliative surgery with longer anticipated survival. Third, because of the importance of symptom control relative to other priorities, some treatments (for example, anticoagulation for a deep vein thrombosis) may be withheld, particularly if they could adversely impact quality of life. Finally, the potential impact of perioperative morbidity to a patient in the end-oflife setting may be even greater relative to patients with a longer life expectancy. For example, a serious complication following a major procedure, such as a gastrointestinal anastomotic leak, could eliminate a patient’s opportunity to travel, leave their home, or in some cases leave the hospital or hospice setting for the remainder of his or her life.
It is important to understand how end-of-life surgery fits into the spectrum of palliative surgery not only from a purely clinical standpoint, but also from the perspective of research aimed at improving quality and outcomes in the palliative setting. Because some facets of end-oflife surgery are unique, studies that do not distinguish these patients from other palliative surgery patients may be difficult to interpret due the heterogeneity. Furthermore, studies that do not include end-of-life patients may not be generalizable to this group.
The spectrum of palliative procedures
It is important to appreciate the wide array of specialties encompassing essentially of the entire spectrum of surgical expertise that play vital roles in palliative surgery. From gastrointestinal diversion or resection for bowel obstruction to stabilization of pathologic fractures to neurosurgical procedures for unremitting pain to thoracic procedures for drainage of malignant pleural effusions, the key role that the surgeon plays in achieving optimal palliation cannot be overstated. Moreover, studies have estimated that palliative interventions accounted for 6% to 12% of all surgical procedures performed, further emphasizing the importance of the role of the surgeon in this field [8,9]. This multidisciplinary approach demonstrates consideration of the fact that comparable symptoms may demand different responses based upon the biology of each primary disease, and that these, often subtle, distinctions, must be appreciated to provide the finest care. Factors such as symptom severity, the degree of symptom resolution, the timing and choice of procedure, the durability of the intervention, associated complication and patient preferences all play major roles in determining the overall benefit of the palliative operation and the role of the surgeon. In fact, Miner et al. [9] demonstrated that when “experienced clinicians” across a spectrum of surgical fields selected patients for palliative procedures, it resulted in improvement or resolution of specific symptoms 80% of the time [9]. These practices affirm the tradition and heritage of surgery, emphasizing that the control of suffering is of equal importance to the cure of disease.
Priorities
Over the next decade, there likely will be several largely interrelated drivers of advancement in the area of palliative surgery and surgical palliative care. One major factor that will impact this area is increasingly limited financial resources associated with the unsustainable escalation of health care costs and efforts to control those costs through health reform and other measures. A second and intimately related influence is the increasing emphasis on evidence-based medicine and justification of risky and/or costly treatments through outcomes and comparative effectiveness studies. A third driver of progress is the rapid growth of palliative medicine programs over recent years, which fosters a more open discourse regarding goals of care and focuses efforts towards empowering the patient and family in making palliative care decisions and formulating realistic and attainable quality of life goals after consideration of their own values [10]. An additional force is the increasing demand for quality metrics in all aspects of health care. Although this has been increasingly highlighted in the context of health reform, it is fundamentally an extension of basic market principles to the business of health care. Surgeons will play a key role in advancing palliative care in surgical patients.
Education and training
The foundation for progress towards better palliative care management in surgery is formal education and training. Ideally this should begin during medical school and continue through residency and fellowship training and beyond. The primary goal should be to establish a level of comfort and competency in addressing and communicating about palliative care issues. A number of articles have been published regarding communication in the context of advanced and chronic illness and serve as an excellent introduction to its complexities and challenges [11-17]. Though it is clear that education regarding palliative care, including the role of surgery, should begin in medical school, according to a recent survey, only 30% of medical schools required students to take a course on palliative and hospice care [18]. However, this percentage can be expected to grow rapidly over time. Opportunities for further education and training are increasingly becoming available to surgical trainees and practicing surgeons, and the American Board of Surgery now offers a subspecialty certificate in hospice and palliative medicine [19-23].
Surgeons are frequently the people to whom patients and their families look for ultimate answers and guidance. It is important that surgical residents learn to be comfortable with that responsibility and that they care deeply about staying with their patients near the end of life. Moreover, education and training in palliative care is necessary because when one looks at studies of what patients with life-threatening illnesses say they want and compares them to what patients actually experience, the gap is huge. Patients with late-stage illness say they want, in order of prominence (1) pain and symptom control, (2) to avoid inappropriate prolongation of the dying process, (3) to achieve a sense of control, (4) to relieve burdens on their families, and (5) to strengthen relationships with loved ones [24]. For patients and physicians, the irony is that for patients in their final year, more medical care, meaning more procedures and prolonged ICU stays, leads to lower satisfaction with care. Family members of decedents in high-intensity hospital service areas report lower quality of: emotional support, shared decision-making, information about what to expect, and respectful treatment [25]. Therefore, it is of utmost importance for physicians to master the basic knowledge and techniques of palliative care in order to learn how to be clear with patients, their families, colleagues, and ourselves regarding the realities of a patient’s disease picture and what our judgment and skill in the art of surgery can provide for their comfort, function, and longevity.
Engagement
As palliative care gains increasing traction as a specialty and becomes increasingly pervasive among health care institutions, surgeons have an opportunity, and arguably, an obligation to be engaged in shaping palliative care in surgery. This engagement must occur at multiple levels. First and foremost, surgeons must engage patients and their families. When confronted with palliative care matters, surgeons should remain a guiding force even if the discourse regarding specific palliative care clinical recommendations is directed by another practitioner. When appropriate, surgeons should also engage colleagues, such as palliative medicine teams, and should do so in a proactive fashion in order to be most helpful to the patient. Additionally, the surgeon’s perspective is vital to establishing the direction of education and training in palliative care topics germane to the field of surgery, as there are many aspects of surgery that are not only difficult and complex, but unique to this field.
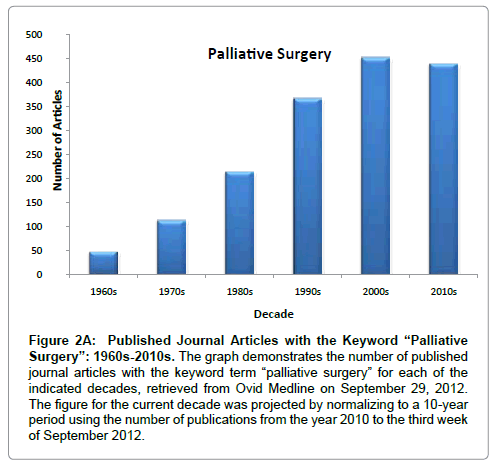
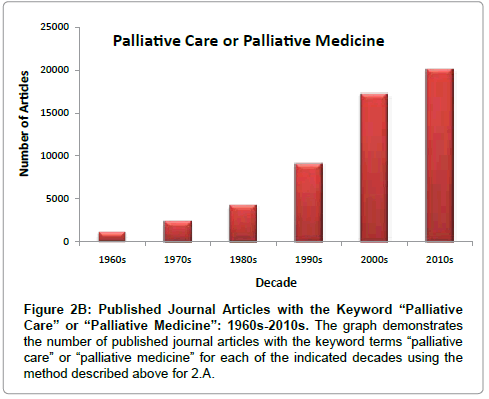
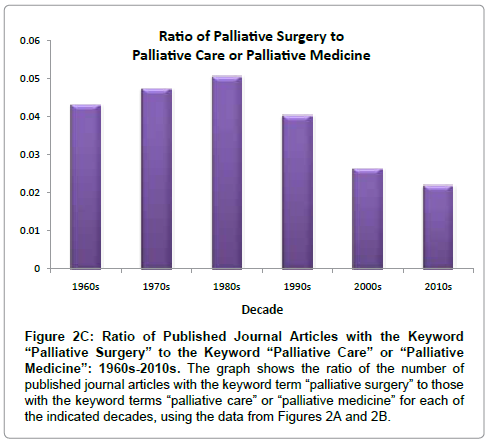
The trend in the overall level of interest of the medical community in palliative surgery should be reflected, in part, by the number of published articles pertaining to this topic. In order to examine this trend, the Ovid Medline database was searched for articles containing the keyword term “palliative surgery” from 1946 to week 3 of September 2012, and the results were grouped by decade for all decades with more than a dozen published articles (Figure 2A). The value for the current decade was projected by normalizing to a 10-year period using the number of publications from the year 2010 to the third week of September 2012. This analysis reveals that the number of articles on the topic of palliative surgery has begun to plateau since the 1990s. In contrast, if the keyword terms “palliative medicine” and “palliative care” are combined, it is evident that the number of published articles has increased at a faster rate since the 1990s relative to articles on “palliative surgery” (Figure 2B). Consequently, the ratio of “palliative surgery” articles to those on “palliative medicine”/“palliative care” has dropped during this time period (Figure 2C). A similar relationship is seen when the keyword “palliative” is used in place of the terms “palliative care” and “palliative medicine”. While such an assessment has obvious limitations and represents only a single dimension of the overall interest in palliative surgery, it could reflect a lag in the degree of engagement and commitment to the advancement of palliative surgery relative to palliative care as a whole and may likewise reflect a need to more actively involve surgeons in palliative care initiatives.
Figure 2a: Published Journal Articles with the Keyword “Palliative Surgery”: 1960s-2010s. The graph demonstrates the number of published journal articles with the keyword term “palliative surgery” for each of the indicated decades, retrieved from Ovid Medline on September 29, 2012. The figure for the current decade was projected by normalizing to a 10-year period using the number of publications from the year 2010 to the third week of September 2012.
Figure 2b: Published Journal Articles with the Keyword “Palliative Care” or “Palliative Medicine”: 1960s-2010s. The graph demonstrates the number of published journal articles with the keyword terms “palliative care” or “palliative medicine” for each of the indicated decades using the method described above for 2.A.
Figure 2c: Ratio of Published Journal Articles with the Keyword “Palliative Surgery” to the Keyword “Palliative Care” or “Palliative Medicine”: 1960s-2010s. The graph shows the ratio of the number of published journal articles with the keyword term “palliative surgery” to those with the keyword terms “palliative care” or “palliative medicine” for each of the indicated decades, using the data from Figures 2A and 2B.
Integration
Some areas of surgery, such as oncologic surgery, inherently require, and are conducive to, multidisciplinary care. Indeed, this is typically an index of quality of care. Palliative care, whether or not in the context of oncology, is similar in this regard. Surgery so frequently comprises a component of palliative care that the degree of integration of the surgeon into the palliative care team is often a reflection of the quality of care. However, not all surgeons have both the time and interest to actively participate in the palliative care process.
Integration of palliative surgery into the palliative care of a patient is often interpreted as integration of the surgeon alone, though this is not really the case [26]. In reality, the nursing staff, surgical trainees, students and other allied health professionals should all be galvanized into a coordinated team in order to provide the best-rounded care for the patient. In practice, this is extraordinarily difficult to achieve without vertical and horizontal investment across the institution. And while integrating the surgeon alone into palliative care management is inadequate, clearly the surgeon must be a leader in championing coordinated, patient-centered, multi-disciplinary palliative care.
Quality metrics
In discussing the topic of quality metrics, it is important to recognize that quality metrics are not the same as quality. Quality metrics represent a surrogate of quality, a measurable parameter that affords the ability to evaluate quality relative to peers and relative to past performance. Fundamentally, quality metrics represent a practical way to guide improvements in and maintenance of quality care. In addition, payers and policy-makers have collectively determined that paying for performance may be an effective way to improve quality.
At present, it appears that quality indicators are here to stay. However, because a particular metric seems like a logical choice does not mean that it is an acceptable measure of a particular aspect of quality, especially if those selected indicators are based on an inadequate knowledge and understanding of what is being measured. Therefore, in addition to supporting relevant research questions, surgeons should feel obligated to not only be involved in but take leadership roles in determining the optimal quality metrics in monitoring are ability to provide quality palliative surgery.
Research
Another area in which surgeons must remain invested is palliative surgery research. There is a paucity of high level evidence supporting the optimal role of most palliative surgical procedures. Concurrently, the stakes are usually quite high in terms of the potential risk of worsening rather than improving quality of life. The procedures also tend to be resource-intensive, not only in terms of the cost of the procedures themselves, but also in terms of the postoperative recovery. Foremost among the important questions regarding palliative surgery are whether specific palliative procedures are superior in terms of outcome measures such as quality of life and cost-effectiveness compared with non-operative alternatives. For those procedures that are superior to medical management alone, a critical research question relates to defining the optimal patient population for that procedure. Additionally, there are important questions related to defining quality using reliable quality metrics, optimizing the outcomes of palliative surgical procedures, and enhancing communication and collaboration with other members of the palliative care team.
Policy
Surgery is not unlike other medical specialties in that it has layers of complexity that can only be fully appreciated by surgeons themselves. Unfortunately, health policies do not always seem to consider the surgeon’s perspective, an assertion that can arguably be applied to virtually any medical specialty. In a recent article, we cautioned that an increasing focus on limiting healthcare expenditures toward the end-of-life could adversely impact resource-intensive, but much needed, surgical procedures aimed at symptom management [27]. On a practical level, most such policies would be expected to incur financial penalties in the form of decreased or no reimbursement for services. The reality, however, is that appropriate implementation of a palliative care approach for patients with serious or life-threatening illnesses can not only provide better symptom management, but may also be associated with cost savings [28]. Nonetheless, there is a very real threat that policy, financial, and medical legal concerns could increasingly prevent access to effective palliative surgeries by creating a progressively more risk-averse culture surrounding these procedures.
Surgeons would likely have a greater opportunity to shape policies that impact the future role of palliative surgeries if they are proactive in leading the dialogue and educating the public as well as hospital policy-makers regarding the role of surgery in palliative management. One area of concern is the adoption of policies that have an unintended adverse “collateral” impact on palliative surgery. For example, if a policy were designed to prevent routine elective orthopedic procedures in the end-of-life setting, such as a knee arthroplasty for advanced osteoarthritis, might it also prevent some patients from receiving a palliative procedure for a painful pathologic fracture? This would seem to be inevitability rather than just a possibility if the wide spectrum of surgeons involved in administering palliative procedures is not involved in the discussion regarding the development of policies that impact their use.
Discussion
Surgeons play a key role in multidisciplinary palliative patient care and have recently begun to take the lead in defining the important clinical, educational, research and policy agendas. However, universal investment among surgeons is lacking, and there are misconceptions and diverging opinions about the best strategy for moving the field forward and even the very meaning of “palliative surgery” itself.
Fortunately, steps have been taken to align surgeons and other palliative care team members around common goals. What palliative surgery clinical programs should look like, their optimal role, and how best to integrate them into the palliative care system is unclear at this point. However, efforts to formalize palliative care education for surgeons and to be more inclusive of surgeons in the clinical decision-making process should provide insight into viable models of integration. It is also important to involve surgeons from a broad array of specialties with an interest and commitment to multidisciplinary palliative care research in order to create a shared responsibility toward the goal of advancing the field of palliative care. In this special issue, a broad range of topics in palliative surgery will be addressed in an effort to stimulate interest in solidifying our collective commitment to palliative care and in addressing some of the most pressing clinical, research, educational, and policy questions.
References
- McCahill LE, Krouse R, Chu D, Juarez G, Uman GC, et al. (2002) Indications and use of palliative surgery-results of Society of Surgical Oncology survey. Ann Surg Oncol 9: 104-112.
- Sallnow L, Feuer D (2010) The role of surgery in the palliation of malignancy. Clin Oncol (R Coll Radiol) 22: 713-718.
- Geoffrey P. Dunn, David E. Weissman (2009) Surgical Palliative Care: A Residents Guide. American College of Surgeons/Cunniff-Dixon Foundation: Essex, CT, USA.
- Eisenkop SM, Spirtos NM, Lin WC (2006) "Optimal" cytoreduction for advanced epithelial ovarian cancer: a commentary. Gynecol Oncol 103: 329-335.
- Niikura N, Liu J, Hayashi N, Palla SL, Tokuda Y, et al. (2011) Treatment outcome and prognostic factors for patients with bone-only metastases of breast cancer: a single-institution retrospective analysis. Oncologist 16: 155-164.
- Hsu CC, Herman JM, Corsini MM, Winter JM, Callister MD, et al. (2010) Adjuvant chemoradiation for pancreatic adenocarcinoma: the Johns Hopkins Hospital-Mayo Clinic collaborative study. Ann Surg Oncol 17: 981-990.
- McCahill LE, Krouse RS, Chu DZ, Juarez G, Uman GC, et al. (2002) Decision making in palliative surgery. J Am Coll of Surg 195: 411-422.
- Krouse RS, Nelson RA, Farell BR, Grube B, Juarez G, et al. (2001) Surgical palliation at a cancer center: incidence and outcomes. Ach Surg 136: 773-778.
- Miner TJ, Brennan MF, Jaques DP (2004) A prospective, symptom related, outcomes analysis of 1022 palliative procedures for advanced cancer. Ann Surg 240: 719-726.
- Miner TJ, Cohen J, Charpentier K, McPhillips J, Marvell L, et al. (2011) The palliative triangle: improved patient selection and outcomes associated with palliative operations. Arch Surg 146: 517-522.
- Miner TJ (2011) Communication skills in palliative surgery: skill and effort are key. Surg Clin North Am 91: 355-366.
- Rialon KL, Blazer DG, Abernethy AP, Mosca PJ (2012) Surgery and the D-Word: Approaching the Topic of Death and Dying with Surgical Patients. J Palliat Care Med.
- Long CO (2011) Ten best practices to enhance culturally competent communication in palliative care. J Pediatr Hematol Oncol 33: S136-S139.
- Sharma RK, Dy SM (2011) Cross-cultural communication and use of the family meeting in palliative care. Am J Hosp Palliat Care 28: 437-444.
- Slort W, Schweitzer BP, Blankenstein AH, Abarshi EA,Riphagen II, et al. (2011) Perceived barriers and facilitators for general practitioner-patient communication in palliative care: a systematic review. Palliat Med 25: 613-629.
- Turner M, Payne S, O'Brien T (2011) Mandatory communication skills training for cancer and palliative care staff: does one size fit all? Eur J Oncol Nurs15: 398-403.
- Villarreal D, Restrepo MI, Healy J, Howard B, Tidwell J, et al. (2011) A model for increasing palliative care in the intensive care unit: enhancing interprofessional consultation rates and communication. J Pain Symptom Manage 42: 676-679.
- Van Aalst-Cohen ES, Riggs R, Byock IR (2008) Palliative care in medical school curricula: a survey of United States medical schools. J Palliat Med 11: 1200-1202.
- Hanna NN, Bellavance E, Keay T (2011) Palliative surgical oncology. Surg Clin North Am 91: 343-53.
- Pernar LI, Peyre SE, Smink DS, Block SD, Cooper ZR (2012) Feasibility and impact of a case-based palliative care workshop for general surgery residents. J Am Coll Surg 214: 231-236.
- Bradley CT, Webb TP, Schmitz CC, Chipman JG, Brasel KJ (2010) Structured teaching versus experiential learning of palliative care for surgical residents. Am J Surg 200: 542-547.
- Klaristenfeld DD, Harrington DT, Miner TJ (2007) Teaching palliative care and end-of-life issues: a core curriculum for surgical residents. Ann Surg Oncol 14: 1801-1806.
- Minor S, Schroder C, Heyland D (2009) Using the intensive care unit to teach end-of-life skills to rotating junior residents. Am J Surg 197: 814-819.
- Singer PA, Martin DK, Kelner M (1999) Quality end-of-life care: patient's perspectives. JAMA 281: 163-168.
- Teno JM, Mor V, Ward N, Roy J, Clarridge B, et al. (2005) Bereaved family member perceptions of quality of end-of-life care in U.S. regions with high and low usage of intensive care unit care. J Am Geriatr Soc 53: 1905-1911.
- Rialon KL, Abernethy AP, Mosca PJ (2012) Integration of Palliative Surgery into the Palliative Care Delivery Team. J Palliative care med 2: 1-2.
- Mosca PJ, Blazer DG 3rd, Wheeler JL, Abernethy AP (2011) When a chance to cut is not a chance to cure: a future for palliative surgery? Ann Surg Oncol 18: 3235-3239.
- Morrison RS, Dietrich J, Ladwig S, Quill T, Sacco J, et al. (2011) Palliative care consultation teams cut hospital costs for Medicaid beneficiaries. Health Aff (Millwood) 30: 454-463.
Relevant Topics
- Caregiver Support Programs
- End of Life Care
- End-of-Life Communication
- Ethics in Palliative
- Euthanasia
- Family Caregiver
- Geriatric Care
- Holistic Care
- Home Care
- Hospice Care
- Hospice Palliative Care
- Old Age Care
- Palliative Care
- Palliative Care and Euthanasia
- Palliative Care Drugs
- Palliative Care in Oncology
- Palliative Care Medications
- Palliative Care Nursing
- Palliative Medicare
- Palliative Neurology
- Palliative Oncology
- Palliative Psychology
- Palliative Sedation
- Palliative Surgery
- Palliative Treatment
- Pediatric Palliative Care
- Volunteer Palliative Care
Recommended Journals
- Journal of Cardiac and Pulmonary Rehabilitation
- Journal of Community & Public Health Nursing
- Journal of Community & Public Health Nursing
- Journal of Health Care and Prevention
- Journal of Health Care and Prevention
- Journal of Paediatric Medicine & Surgery
- Journal of Paediatric Medicine & Surgery
- Journal of Pain & Relief
- Palliative Care & Medicine
- Journal of Pain & Relief
- Journal of Pediatric Neurological Disorders
- Neonatal and Pediatric Medicine
- Neonatal and Pediatric Medicine
- Neuroscience and Psychiatry: Open Access
- OMICS Journal of Radiology
- The Psychiatrist: Clinical and Therapeutic Journal
Article Tools
Article Usage
- Total views: 26289
- [From(publication date):
December-2012 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 21239
- PDF downloads : 5050