Research Article Open Access
Patient Strength of Preference for Best Practices in Patient Education
Walsh R*, Aliarzadeh B and Mastrogiacomo CDepartment of Family and Community Medicine, University of Toronto, Toronto, Canada
- *Corresponding Author:
- Rachel Walsh
Family Medicine Teaching Unit, The Scarborough Hospital
3000 Lawrence Ave E, Scarborough, Ontario, M1P 2V5, Canada
Tel: + 416-431-8200
E-mail: rfeld011@gmail.com
Received date: October 21, 2016; Accepted date: November 10, 2016; Published date: November 20, 2015
Citation: Walsh R, Aliarzadeh B, Mastrogiacomo C (2016) Patient Strength of Preference for Best Practices in Patient Education. J Community Med Health Educ 6:484. doi:10.4172/2161-0711.1000484
Copyright: © 2016 Walsh R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Community Medicine & Health Education
Abstract
Background: Patient education is important in healthcare. As such, EULAR, the European League Against Rheumatism, has created and published 8 evidence-based and expert-opinion-based recommendations for patient education. However, the relevance and relative importance of these recommendations to a general patient population are yet to be determined. Our study aimed to determine patients’ strength of preference for the different EULAR recommendations for patient education.
Methods: We performed an adaptive, partial-profile conjoint analysis using a discrete choice survey on a crosssection of patients in a family practice. Results: A total 56.8% of patients approached in clinic agreed to participate. Of those who started the survey, 94.4% completed the survey. The mean time to complete the survey was 10.7 minutes. Mean rankings of the 8 EULAR recommendations, where 1 is the most preferred and 8 the least preferred, were 3.4 for content of education, 3.9 for training of education providers, 4.1 for who delivers the education, 4.5 for education methods offered, 4.6 for how often the education should be offered, 4.9 for accessibility of education, 5.3 for level of personalization, and 5.4 for monitoring of education.
Conclusion: Participants felt that the most important features were content, training of education providers, and who delivered the education. The level of personalization and the monitoring of the education were deemed less important. In addition, we determined that it is feasible to measure patient preferences using a discrete choice survey in a family practice setting.
Keywords
Patient education; Patient preference; Family practice; Conjoint analysis; Discrete choice
Introduction
Patient education (PE) is an important part of providing good quality healthcare. A number of studies have shown that when patients know more about their illnesses and treatments, there is a great potential for improved health outcomes. Lorig et al. found that a health education program for self-management in patients with chronic arthritis resulted in a decline in pain, physician visits, and costs [1]. Sari & Osman found that health education and greater access to spirometry resulted in increased medication use in COPD and asthma patients [2]. A systematic review (Cochrane review) looking at interventions aiming to improve medication adherence showed that patient education interventions improve medication adherence, decrease emergency department (ED) visits, and hospital admissions [3]. Specifically, studies included in the Cochrane review showed that a variety of educational interventions resulted in a decrease in HbA1c in diabetics [4], an increase in medication adherence in schizophrenic and schizoaffective patients [5], an improvement in blood pressure and medication adherence in hypertensive patients [6], as well as an overall improvement in medication adherence in a general pharmacy setting [7]. Another systematic review, from Ghisi et al. found 10 of 11 included studies showed that education significantly increased knowledge in cardiac patients and that educational interventions were significantly and positively related to physical activity, dietary habits, and smoking cessation [8]. Additionally, the 2003 National Assessment of Adult Literacy (NAAL) in the United States (US) reported that higher health literacy was associated with a higher self-reported level of overall health [9].
While the potential benefits are apparent, patient education has been inconsistently done in the past, with variable results on health outcomes. The Cochrane review looking at interventions to improve medication adherence overall showed inconsistent results for educational and other interventions for improving medication adherence. Even the most effective interventions did not lead to large improvements [3]. A systematic review on educational needs of patients with irritable bowel syndrome (IBS) found that 65% of patients were ‘unhappy’ with their level of knowledge or felt poorly informed [10]. Additionally, an international survey done by Aliot et al. showed that cardiologists felt that the level and quality of information about atrial fibrillation given to patients compared poorly with levels of information provided on other cardiovascular diseases [11]. In the same study, the majority of physicians felt that there was an important need for more and improved information given to patients about atrial fibrillation.
Knowing patient preferences for patient education may increase the effectiveness of patient education. In a randomized controlled trial by Giuse et al. tailoring health information according to learning style (i.e. visual, aural, read/write, kinesthetic, multimodal) and health literacy resulted in greater gains in knowledge about hypertension than information customized for health literacy level only [12]. Additionally, Rumpold et al. found that eliciting information preferences in advanced lung cancer patients resulted in high patient satisfaction with end-of-life communication [13].
In 2015, a task force from the European League Against Rheumatism (EULAR) created and published 8 evidence-based and expert-opinion-based recommendations for patient education for people with inflammatory arthritis [14]. The recommendations are presented in Table 1.
| Overarching principles | ||
| Patient education is a planned interactive learning process designed to support and enable people to manage their life with inflammatory arthritis and optimise their health and well-being | ||
| Communication and shared decision making between people with inflammatory arthritis and their healthcare professionals are essential for effective patient education | ||
| Recommendations | Category of evidence | Strength of recommendation |
| Patient education should be provided for people with inflammatory arthritis as an integral part of standard care in order to increase patient involvement in disease management and health promotion | 1A-2B | A-C |
| All people with inflammatory arthritis should have access to and be offered patient education throughout the course of their disease including as a minimum; at diagnosis, at pharmacological treatment change and when required by the patient’s physical or psychological condition | 3-4 | C-D |
| The content and delivery of patient education should be individually tailored and needs-based for people with inflammatory arthritis | 1B | A |
| Patient education in inflammatory arthritis should include individual and/or group session, which can be provided through face-to-face or online interactions, and supplemented by phone calls, written or multimedia material | 1A-B | A |
| Patient education programmes in inflammatory arthritis should have a theoretical framework and be evidence-based, such as self-management, cognitive behavioural therapy or stress management | 1A-B | A |
| The effectiveness of patient education in inflammatory arthritis should be evaluated and outcomes used must reflect the objectives of the patient education programme | 4 | D |
| Patient education in inflammatory arthritis should be delivered by competent health professionals and/or by trained patients, if appropriate, in a multidisciplinary team | 3 | C |
| Providers of patient education in inflammatory arthritis should have access to and undertake specific training in order to obtain and maintain knowledge and skills | 3-4 | C-D |
Table 1: EULAR Recommendations for patient education for people with inflammatory arthritis.
While these recommendations were developed for people with inflammatory arthritis, they appear to be easily generalizable to a more diverse patient population. As such, these recommendations could provide a strong framework for developing patient education in a general patient population, such as in a family doctor’s office. However, the relevance and relative importance of these recommendations to a more general patient population are yet to be determined.
Discrete choice experiments are used to elicit strength of preference when multiple attributes and levels need to be considered [15]. Discrete choice experiments determine preferences by having respondents choose between differing combinations of components (attributes). This method allows an assessment of compromise between a product’s attributes and its effect on choice. As such, discrete choice experiments can be used to assess relative preferences for multiple components of a patient education intervention.
This study aims to determine patients’ strength of preference (partworth utility) for different attributes of patient education strategies as determined by the EULAR recommendations. We also looked at the feasibility of performing a discrete choice survey in a family practice setting.
Methods
We conducted an adaptive, partial-profile conjoint analysis, using a discrete choice experiment, on a cross-section of patients. This study was approved by the Scarborough General Hospital research ethics board (Appendix A).
Patients were consecutively approached in a family medicine community clinic solo practice from Nov 23, 2015 to Jan 29, 2016 during regular clinic hours (i.e. not during after-hours or weekend clinics).
Subjects were included if they were fluent in English and had an adequate literacy level to be able to answer the questionnaire. Literacy level was determined with the Rapid Estimate of Adult Literacy in Medicine–Short Form (REALM-SF) questionnaire prior to the administration of the discrete choice experiment (Appendix B). The REALM-SF questionnaire is a brief, validated tool used to assess adult literacy in medicine [16]. Patients were included in the study if they scored 4 or greater on the REALM-SF literacy screen, indicating a grade 7-8 literacy level.
Appendix B: REALM-SF literacy questionnaire [16].
Subjects were excluded if they were less than 18 years old, if they had difficulty reading and understanding the English language, or if they had cognitive impairment that limited their ability to respond to the questionnaire, i.e. a diagnosis of dementia or significant developmental delay.
Characteristics of the overall population of the study clinic were taken from the clinic’s electronic medical records.
For our feasibility aims, we collected data on the proportion of patients that were approached in the clinic, the proportion that agreed to participate, the proportion that passed the literacy requirements, and the proportion of patients that completed the questionnaire. Data collected also included the number of tasks required for participants to complete the discrete choice experiment, as well as the time required to complete the overall survey.
After completing a brief questionnaire indicating the participant’s age, sex, first language, and education level, participants were asked to complete the discrete choice experiment using the 1000minds online survey platform [17]. Potentially eligible patients were consecutively approached in the clinic either before or after their appointment with the physician, regardless of the reason for visit. They were told involvement in the study would take up to 15 minutes. Participants were then handed a hard-copy questionnaire containing demographic information and the REALM-SF tool to be completed. If participants passed the REALM-SF literacy screen they were asked to complete the online discrete choice experiment on a provided tablet in the waiting room.
The discrete choice task presented to participants was a partial profile, adaptive questionnaire. As such, the participants were individually presented with two choices that each included two different attributes at different levels (Table 2 for a list of attributes and levels). The participants were then asked to select the choice that best reflected their preference, or opt-out by selecting the option “they are equal” or by skipping the question (Appendix C). Total 136 potential tasks using different pairings were included in the survey. However, due to the adaptive nature of the questionnaire, participants completed only as many tasks as necessary until their preference profile was fully determined. Therefore, the number of tasks that each participant was asked to complete varied with each participant. As a feature of the 1000minds survey platform, the order of presented attributes was varied and the order of discrete choice tasks was randomized. Participants had access to members of the research staff at any point for assistance.
| Attribute | Levels |
|---|---|
| Accessibility of education | Available to few patients Available to some but not all patients Available to all patients |
| How often the education should be offered | Only at diagnosis Both at diagnosis, and at treatment change At diagnosis, at treatment change, and with any changes in condition |
| Level of personalization | Not individualized – the same education for everyone Individually tailored and needs-based |
| Education methods offered | Online sessions only Group counselling ± online sessions One-on-one counselling ± group counselling ± online sessions |
| Content of education | Not based on theory or evidence Based on theory but not evidence Based on theory and evidence |
| Monitoring of education | Education program not evaluated for effectiveness Education program evaluated for effectiveness |
| Who delivers the education | Persons from a non-health background Health professionals (e.g. doctors, nurses, therapists etc.) and/or patients |
| Training of education providers | No specific training Training to maintain knowledge and skills Training to maintain knowledge and skills + training for delivering education |
Table 2: Attributes and levels included in the discrete choice survey.
Appendix C: A sample question in the discrete choice survey from the 1000minds online survey platform [17].
Attributes and levels included in the discrete choice experiment were chosen based on the 8 EULAR criteria. The 8 attributes included in the discrete choice experiment were taken directly from the EULAR recommendations. 2-3 levels for each attribute were selected based on recommendations within the EULAR paper and ranked from least desired to most desired (Table 2).
We used the chi-square goodness of fit test to determine if our study population was similar to the base population from which the study population was drawn.
There is no clear consensus on calculating a sample size or performing a power analysis for an adaptive conjoint analysis study. However, there are general statements that suggest a sample size of >200 is adequate for an exploratory study intended to assess main effects of group-level preferences [18].
Analysis of the discrete choice experiment was done using the PAPRIKA method (Potentially All Pairwise Rankings of all possible Alternatives). PAPRIKA uses pairwise ranking (choosing one alternative from two) through an adaptive, partial-profile conjoint analysis survey. PAPRIKA then identifies all other hypothetical alternatives that can be pairwise ranked and eliminates them by applying the logical property of transitivity. Transitivity allows an overall ranking of all possible alternatives to be produced based on pairwise rankings of the individual alternatives. Preference values, or part-worth utilities, are then calculated using linear models. These part-worth utilities represent the relative importance of each attribute [19]. This analysis was performed using the 1000minds software. No specific validity checks were performed.
Results
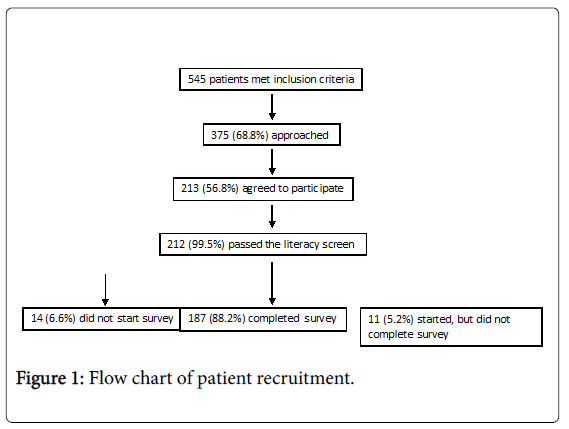
A flow chart of patient recruitment is shown in Figure 1. 545 patients presenting to clinic during the recruitment period met inclusion criteria. Of these, 187 participants completed the discrete choice experiment. Table 3 shows the characteristics of the population included in the study compared to the overall population of the study clinic.
| Study population | All clinic patients | ||
|---|---|---|---|
| N*(%) | N (%) | ||
| Total | 213 | 1481 | p value |
| Age (years) | 0.0003 | ||
| 18-24 | 10 (4.7%) | 146 (9.9%) | |
| 25-34 | 22 (10.3%) | 184 (12.4%) | |
| 35-44 | 52 (24.4%) | 290 (19.6%) | |
| 45-54 | 44 (20.7%) | 290 (19.6%) | |
| 55-64 | 54 (25.4%) | 245 (16.5%) | |
| 65-74 | 18 (8.5%) | 133 (9.0%) | |
| 75-84 | 7 (3.3%) | 123 (8.3%) | |
| 85+ | 6 (2.8%) | 70 (4.7%) | |
| Gender | <0.0001 | ||
| Female | 183 (86.7%) | 1098 (74.1%) | |
| Male | 28 (13.3%) | 383 (25.9%) | |
| First Language | |||
| English | 169 (79.3%) | ||
| French | 5 (2.3%) | ||
| Italian | 20 (9.4%) | ||
| Other | 17 (8.0%) | ||
| Education Level | |||
| Did not complete primary (grade) school | 2 (0.9%) | ||
| Completed at least grade school (grade 6 or equivalent) | 11 (5.2%) | ||
| Completed at least secondary (high) school | 52 (24.5%) | ||
| Completed college/university | 125 (59.0%) | ||
| Completed graduate or professional degree | 22 (10.4%) | ||
| REALM-SF literacy score | |||
| <4 (<7th grade) | 1 (0.5%) | ||
| 4-6 (7-8th grade) | 10 (4.7%) | ||
| 7 (high school) | 202 (94.8%) |
*In cases where total does not add to 213, this is due to missingness.
Table 3: Characteristics of the study population and the overall population of the study clinic.
A maximum 136 discrete choice tasks could be undertaken. The mean number of tasks completed was 31.6 (median 32, range 14-58). The mean time to complete the survey was 10.7 minutes (median 9, range 3-35 minutes).
The relative preferences (part-worth utilities) of each attribute are shown in Table 4 and Figure 2. The mean attribute rankings are shown in Table 5, where 1 is the highest ranked or most preferred and 8 is the lowest ranked or least preferred.
| Utility Values | Mean | 95% Confidence Interval |
|---|---|---|
| Accessibility of education | ||
| Available to few patients | 0.0% | |
| Available to some but not all patients | 5.0% | (4.4%-5.6%) |
| Available to all patients | 12.4% | (11.4%-13.4%) |
| How often the education should be offered | ||
| Only at diagnosis | 0.0% | |
| Both at diagnosis, and at treatment change | 7.8% | (7.1%-8.4%) |
| At diagnosis, at treatment change, and with any changes in condition | 12.5% | (11.8-13.3%) |
| Level of personalization | ||
| Not individualized - the same education for everyone | 0.0% | |
| Individually tailored and needs-based | 9.8% | (8.9%-10.6%) |
| Education methods offered | ||
| Online sessions only | 0.0% | |
| Group counseling ± online sessions | 6.7% | (6.0%-7.3%) |
| One-on-one counselling ± group counselling ± online sessions | 12.6% | (11.8%-13.5%) |
| Content of education | ||
| Not based on theory or evidence | 0.0% | |
| Based on theory but not evidence | 6.8% | (6.2%-7.4%) |
| Based on theory and evidence | 16.1% | (15.2%-17.1%) |
| Monitoring of education | ||
| Education program not evaluated for effectiveness | 0.0% | |
| Educations program evaluated for effectiveness | 9.5% | (8.8%-10.2%) |
| Who delivers the education | ||
| Persons from a non-health background | 0.0% | |
| Health professionals (e.g. doctors, nurses, therapists etc.) and/or patients | 13.1% | (12.2%-13.9%) |
| Training of education providers | ||
| No specific training | 0.0% | |
| Training to maintain knowledge and skills | 9.2% | (8.5%-9.9%) |
| Training to maintain knowledge and skills and training for delivering education | 14.0% | (13.2%-14.9%) |
Table 4: Mean utility values.
| Attributes | Mean Ranking |
|---|---|
| Content of education | 3.4 |
| Training of education providers | 3.9 |
| Who delivers the education | 4.1 |
| Education methods offered | 4.5 |
| How often the education should be offered | 4.6 |
| Accessibility of education | 4.9 |
| Level of personalization | 5.3 |
| Monitoring of education | 5.4 |
Table 5: Mean attribute rankings.
Discussion
Our study found that all of the 8 EULAR recommendations for PE were considered relatively important. Overall, the content of patient education was considered the most important aspect, followed by the training of education providers, and who delivered the education.
Additionally, the study found that it is feasible to determine patient preferences using a discrete choice online questionnaire in a family practice setting.
A total 375 patients (68.8% of the patients presenting to clinic) were approached to participate in the study. The remainder of patients were not approached mostly due to clinic constraints (e.g. running behind schedule), but also included patient visit factors (e.g. patient too distraught or too sick). This might be overcome in a future study by allowing patients to complete the online questionnaire at home, outside of clinic time and at their own leisure.
A total 213 patients (56.8%) agreed to participate. Most patients reported “I don’t have time” as the reason for refusing participation in the study. However, other reasons for refusal included not feeling comfortable using a computer. This may have affected recruitment of elderly or lower literacy populations such that these population may be underrepresented in our study population.
A total 212 participants (99.5%) passed the REALM-SF literacy screen. This high pass rate for the literacy screen was perhaps due to the high literacy level in the clinic population. Another explanation could be that lower-literacy patients were self-screening and declining participation in the study prior to completing the literacy screen due to a perceived inability to understand or read the questions included in the experiment.
A total 187 out of the 212 participants (88.2%) completed the discrete choice experiment. 11 participants (5.2%) started but were unable to complete the experiment. The remainder (6.6%) did not start the experiment in the first place. This was usually due to not being able to wait for another participant to finish the experiment on the provided tablet.
There was a statistically significant difference in age distribution and gender between the study population and the base clinic population. Participants were more likely to be between 35-64 years old compared to the base clinic population. This could be explained by fewer patients outside of that age group presenting for assessment at the family practice during the recruitment period. This is likely the case for patients under 35 years old. The more elderly population over 65 years old may be underrepresented due to a higher number of participants either not meeting eligibility criteria due to cognitive ailments such as dementia, or refusing to participate in the study, perhaps due to unfamiliarity using a computer or tablet. Participants in the study were also more likely to be female compared to the base clinic population. This is most likely due to females presenting more for assessment during the recruitment period. As such, males may be underrepresented in our study population.
The overall level of education was quite high in study participants, with 69.4% having completed a college/university degree or higher. This could be due to a high education level in the base clinic population. Alternatively, this could be explained by more highly educated patients being more likely to agree to participate in the study.
Mean number of tasks completed was 31.6 (range 14-58) with a mean time to complete the experiment of 10.7 minutes (median 9, range 3-35 minutes). The ISPOR (International Society for Pharmacoeconomics and Outcomes Research) Task Force report on good research practices for conjoint analysis suggests that, although there is some debate, it is good practice to include 8-16 conjointanalysis tasks, but that some conjoint analysis practitioners advocate that respondents can complete up to 32 tasks [20]. As such, the cognitive burden of the discrete choice experiment may be considered high in this study.
Attributes had mean utility values ranging from 9.5 to 16.1% indicating that they all have similar levels of importance, with some deemed slightly more important than others.
Developing patient education materials according to the relative patient preferences shown in this study may help improve patient education and patient outcomes. Project Leonardo, a disease and care management model studied by Ciccone et al. showed that patient empowerment interventions, including patient education, can lead to improved health outcomes in chronic disease management [21]. By developing education materials according to patient preference, patients may be more satisfied and more invested in their patient education, leading to higher patient empowerment and improved health outcomes.
Limitations
Our study results need to be interpreted in light of several possible limitations. Due to convenience/consecutive sampling, the study population may not be fully representative of the base clinic population and may be more representative of patients who present to clinic more frequently. It is also possible that the base clinic population may not be fully representative of base population in the area. The population was from the practice of a solo female family practitioner. The patients, based on the demographics collected, were more likely to be female, and may be more highly educated than the base (local) population. Participants were primarily English speaking and the survey was only offered in English. The results of the study are therefore more applicable to a more middle-aged, female, educated, English-speaking population. This could be improved in future studies by offering the survey in several languages and offering the survey at a variety of clinics in different locations. The experiment itself may also have presented a high cognitive burden to participants. In future studies, linking demographic data to the survey results may allow us to determine if education level had an impact on the participant’s ability to complete the survey. However, in our current study, since the demographic data were not linked to the anonymous survey results, we could not examine the effects of demographic factors on patient preference. The final sample size included fewer than 200 participants (212 eligible participants and 187 completed experiments). Due to the relatively low sample size, the results may not be as precise in showing the relative preferences of the base population.
While conducting a discrete choice experiment allowed us to quantify the patient strength of preference for different aspects of patient education, alternative study designs could complement our findings. For example, conducting focus groups would allow for an indepth analysis of patients’ reasons for expressing particular preferences. Further studies in this direction may help clarify the reasoning behind the strengths of preference found in this study.
Conclusion
In conclusion, participants in the study felt that all 8 of the EULAR recommendations were important for patient education, with the content of patient education, the training of education providers, and who delivered the education being the most important of the 8 recommendations on patient education. In addition, while clinic and patient factors, such as time constraints, made it somewhat difficult to recruit participants from a busy family practice office, once patients agreed to participate in the survey, most were able to complete the discrete choice questionnaire without difficulty. Therefore it is feasible to administer a discrete choice online survey in a family practice setting in order to determine relative patient preferences for different aspects of patient education.
Acknowledgements
We would like to acknowledge Dr. Brian Feldman at The Hospital for Sick Children in Toronto for his help with this study.
Authorship
RW and BA were involved in the conception and design of the study. RW and CM were involved in the acquisition of data. RW was involved in the analysis and interpretation of data, as well as drafting the article. BA was involved in critical revision of the article. All authors gave final approval of the version to be submitted.
References
- Lorig KR, Mazonson PD, Holman HR (1993) Evidence suggesting that health education for self-management in patients with chronic arthritis has sustained health benefits while reducing health care costs. Arthritis Rheum 36: 439-446.
- Sari N, Osman M (2015) The effects of patient education programs on medication use among asthma and COPD patients: a propensity score matching with a difference-in-difference regression approach. BMC Health Serv Res 15: 332-341.
- Nieuwlaat R, Wilczynski N, Navarro T, Hobson N, Jeffery R, et al. (2014) Interventions for enhancing medication adherence. Cochrane Database Syst Rev 1: 1-730.
- Ellis DA, Naar-King S, Chen X, Moltz K, Cunningham PB, et al. (2011) Multisystemic therapy compared to telephone support for youth with poorly controlled diabetes: findings from a randomized controlled trial. Ann Behav Med 44: 205-215.
- Farooq S, Nazar Z, Irfan M, Akhter J, Gul E, et al. (2011) Schizophrenia medication adherence in a resource-poor setting: randomised controlled trial of supervised treatment in out-patients for schizophrenia (STOPS). Br J Psychiatry 199: 467-472.
- Morgado M, Rolo S, Castelo-Branco M (2011) Pharmacist intervention program to enhance hypertension control: a randomised controlled trial. Int J Clin Pharm 33: 132-140.
- Wu JY, Leung WY, Chang S, Lee B, Zee B, et al. (2006) Effectiveness of telephone counselling by a pharmacist in reducing mortality in patients receiving polypharmacy: randomised controlled trial. Brit Med J 333: 522.
- Ghisi GLdM, Abdallah F, Grace SL, Thomas S, Oh P (2014) A systematic review of patient education in cardiac patients: Do they increase knowledge and promote health behavior change? Patient Educ Couns 95: 160-174.
- Kutner M, Greenberg E, Jin Y, Paulsen C (2006) The Health Literacy of America's Adults: Results from the 2003 National Assessment of Adult Literacy. U.S. Department of Education, Washington DC.
- Flik CE, van Rood YR, de Wit NJ (2015) Systematic review: knowledge and educational needs of patients with irritable bowel syndrome. Eur J Gastroenterol Hepatol 27: 367-371.
- Aliot E, Breithardt G, Brugada J, Camm J, Lip GY, et al. (2010) An international survey of physician and patient understanding, perception, and attitudes to atrial fibrillation and its contribution to cardiovascular disease morbidity and mortality. Europace 12: 626-633.
- Giuse NB, Koonce TY, Storrow AB, Kusnoor SV, Ye F (2012) Using health literacy and learning style preferences to optimize the delivery of health information. J Health Commun 17: 122-140.
- Rumpold T, Lutgendorf-Caucig C, Jagsch R, Dieckmann K, Watzke H, et al. (2015) Information preferences regarding cure rates and prognosis of Austrian patients with advanced lung cancer. Strahlenther Onkol 191: 549-556.
- Zangi HA, Mwidimi N, Adams J, Andersen L, Bode C, et al. (2015) EULAR recommendations for patient education for people with inflammatory arthritis. Ann Rheum Dis 74: 954-962.
- Orme BK (2010) Getting Started with Conjoint Analysis: Strategies for Product Design and Pricing Research. Research Publishers LLC, Madison.
- Arozullah AM, Yarnold PR, Bennett CL, Soltysik RC, Wolf MS, et al. (2007) Development and validation of a short-form, rapid estimate of adult literacy in medicine. Med Care 45: 1026-1033.
- Hansen P, Ombler F (2008) 1000Minds software.
- Sawtooth Software, Inc. (2010) ACA Technical Paper: Sample size issues for conjoint analysis. Research Publishers LLC.
- Hansen P, Ombler F (2008) A new method for scoring additive multi-attribute value models using pairwise rankings of alternatives. J Multi-Crit Decis Anal 15: 87-107.
- Bridges JF, Hauber AB, Marshall D, Lloyd A, Prosser LA, et al. (2011) Conjoint analysis applications in health—a checklist: a report of the ISPOR good research practices for conjoint analysis task force. Value Health 14: 403-413.
- Ciccone MM, Aquilino A, Cortese F, Scicchitano P, Sassara M, et al. (2010) Feasibility and effectiveness of a disease and care management model in the primary health care system for patients with heart failure and diabetes (Project Leonardo). Vasc Health Risk Manag 6: 297-305.
Relevant Topics
- Addiction
- Adolescence
- Children Care
- Communicable Diseases
- Community Occupational Medicine
- Disorders and Treatments
- Education
- Infections
- Mental Health Education
- Mortality Rate
- Nutrition Education
- Occupational Therapy Education
- Population Health
- Prevalence
- Sexual Violence
- Social & Preventive Medicine
- Women's Healthcare
Recommended Journals
Article Tools
Article Usage
- Total views: 6804
- [From(publication date):
December-2016 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 5819
- PDF downloads : 985