Case Report Open Access
Posttraumatic Stress Disorder after Hurricane Sandy among Persons Exposed to the 9/11 Disaster
Kimberly Caramanica MPH1*, Robert M. Brackbill Ph D, MPH1, Steven D. Stellman Ph D, MPH1,2, Mark R. Farfel ScD1
1New York City Department of Health and Mental Hygiene, USA
2Department of Epidemiology, Mailman School of Public Health, Columbia University, New York, USA
Visit for more related articles at International Journal of Emergency Mental Health and Human Resilience
Abstract
Background: Traumatic exposure during a hurricane is associated with adverse mental health conditions post-event. The World Trade Center Health Registry provided a sampling pool for a rapid survey of persons directly affected by Hurricane Sandy in the New York City (NYC) metropolitan area in late October 2012. This study evaluated the relationship between Sandy experiences and Sandy-related posttraumatic stress disorder (PTSD) among individuals previously exposed to the September 11, 2001 (9/11) disaster. Methods: A total of 4,558 surveys were completed from April 10-November 7, 2013. After exclusions for missing data, the final sample included 2,214 (53.5%) respondents from FEMA-defined inundation zones and 1,923 (46.5%) from non-inundation zones. Sandy exposures included witnessing terrible events, Sandy-related injury, fearing for own life or safety of others, evacuation, living in a home that was flooded or damaged, property loss, and financial loss. Sandy-related PTSD was defined as a score of ≥44 on a Sandy-specific PTSD Checklist. Results: PTSD prevalence was higher in the inundation zones (11.3%) and lower in the non-inundation zones (4.4%). The highest prevalence of Sandy-related PTSD was among individuals in the inundation zone who sustained an injury (31.2%), reported a history of 9/11-related PTSD (28.8%), or had low social support prior to the event (28.6%). In the inundation zones, significantly elevated adjusted odds of Sandy-related PTSD were observed among persons with a prior history of 9/11-related PTSD, low social support, and those who experienced a greater number of Sandy traumatic events. Conclusions: Sandy-related stress symptoms indicative of PTSD affected a significant proportion of persons who lived in flooded areas of the NYC metropolitan area. Prior 9/11-related PTSD increased the likelihood of Sandy-related PTSD, while social support was protective. Public health preparation for events similar to Sandy should incorporate outreach and linkages to care for persons with prior disaster-related trauma.
Keywords
9/11, posttraumatic stress disorder (PTSD), hurricanes, disasters, World Trade Center Health Registry, social support
Introduction
Traumatic exposure during a hurricane, such as disaster-related displacement, relocation, injury, and personal and financial loss, has been associated with adverse post-event mental health conditions including posttraumatic stress disorder (PTSD) (Neria, Nandi, & Galea, 2008; Norris et al., 2002). Several studies have documented levels of PTSD 5-9 months following hurricanes; one study found a PTSD prevalence of 30.3% among residents of New Orleans impacted by Hurricane Katrina (Galea et al., 2007). Another study among inhabitants of large areas of Florida impacted by four hurricanes (Charley, Frances, Ivan, & Jeanne) in 2004 found a prevalence of 3.6% (Acierno et al., 2007).
On October 29, 2012 Hurricane Sandy made landfall in the New York metropolitan area, resulting in numerous deaths, hundreds of thousands of damaged or destroyed homes and businesses, extensive and long-lasting power and transportation outages, and billions of dollars in structural damage (Abramson & Redlener, 2012). Recent studies suggest that prevalence of hurricane-related PTSD is high among those impacted by Sandy. For instance, an online survey of 1,000 participants conducted one month post-Sandy found PTSD symptoms in 23.6% of persons from Sandy affected areas (Palgi et al., 2014), and PTSD symptoms were positively related to degree of Sandy exposure (Shrira, Palgi, Hamama-Raz, Goodwin, & Ben- Ezra, 2014). Another cross-sectional telephone survey of 200 adults conducted 6-8 months post-Sandy among individuals residing in communities along New Jersey’s coastline found that 14.5% of residents screened positive for PTSD; high Sandy exposure strongly predicted adverse mental health status (Boscarino et al., 2013).
In addition, prior studies have found that retrospective reports of low social support (Acierno et al., 2007; Boscarino et al., 2013) and recollections of prior disasters including earlier hurricanes or the September 11, 2001 (9/11) disaster (Palgi et al., 2014; Shrira et al., 2014) significantly increase the likelihood of hurricanerelated PTSD. However, these studies do not provide a temporal relationship between exposure and subsequent PTSD or account for the longitudinal influence of social support. The World Trade Center (WTC) Health Registry (Registry) provided a sampling pool for a survey of the experiences and physical and mental health of persons directly affected by Hurricane Sandy in the New York City (NYC) metropolitan area in late October 2012. This study evaluated the relationship between Sandy experiences and Sandy-related posttraumatic stress disorder (PTSD) among individuals previously exposed to the 9/11 disaster.
Materials and Methods
Sample Selection and Data Collection
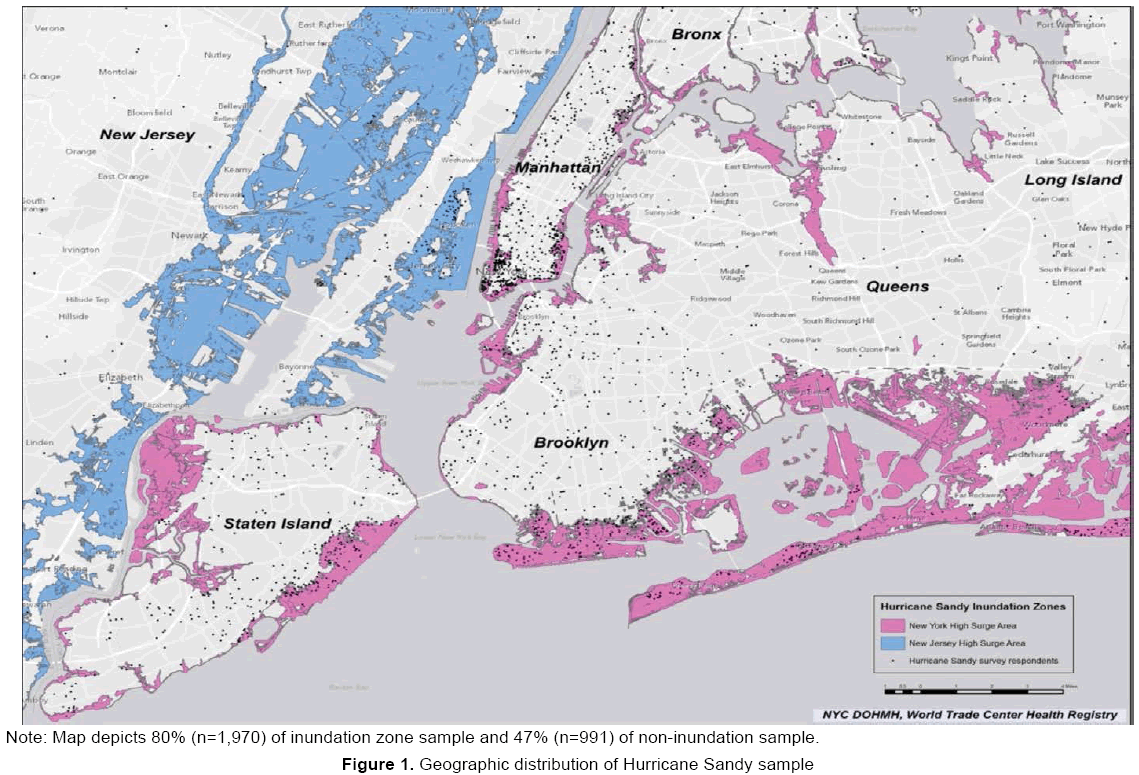
The World Trade Center Health Registry (Registry), a longitudinal cohort study (Wave 1 2003-2004; Wave 2 2006-2007; Wave 3 2011-2012) of 71,431 persons exposed to the events of 9/11 in NYC, provided the sampling pool for this study (Brackbill et al., 2009; Farfel et al., 2008). Since Hurricane Sandy occurred shortly after completion of the third wave of Registry data collection (June 2011-March 2012), 43,134 enrollees who completed the Wave 3 survey formed the sampling pool for the Sandy sub-study. Two study groups were defined based on the location of their residences within the NYC tri-state metropolitan area (including NYC, Long Island, and parts of Connecticut and New Jersey). The first group consisted of enrollees who lived in the hurricane inundation zone, defined by the FEMA Modeling Task Force (n=4,435), while a comparison group of the same size consisted of a randomly selected subset of enrollees with a current tri-state area address outside the inundation zone (n=4,435) (Figure 1).
Approximately five months post-Sandy (March 28, 2013), the selected enrollees were sent lead letters via email and/or mail which described the study and invited their participation. Shortly afterward, sample subjects with valid email addresses were invited to participate in an Internet survey (n=7,367). Internet surveys were utilized to better reach persons displaced by Sandy. Over the next two months, seven email reminders were sent to Internet survey nonrespondents. Beginning three weeks after the launch of the Internet survey, up to three rounds of paper surveys were mailed to study subjects who did not complete the Internet survey or did not have a valid email address (n=6,353). At the close of data collection (November 7, 2013) 4,558 surveys were completed (51.4% response rate). The study protocol was approved by the NYC Department of Health and Mental Hygiene’s Institutional Review Board.
Study Variables
The Sandy survey included questions on knowledge of evacuation zone status, home evacuation, storm and subsequent environmental exposures, loss of services, flood damage, costs of home repairs, activities related to storm response such as rescue, clean-up and repair, and physical and mental health assessments. This analysis also incorporates information from each participant obtained from Waves 1, 2, and 3 of the Registry surveys, including gender, age, race/ethnicity, household income in 2010, marital status, and education.
Probable PTSD was assessed in the Registry Wave 1, 2, and 3 surveys using a 9/11-specific PTSD Checklist-Civilian Version (PCL-17). The PCL-17 is a self-reported, 17-item scale that corresponds to the three PTSD symptom clusters (re-experiencing, avoidance, hyper-arousal) as outlined in the DSM-IV (Blanchard, Jones-Alexander, Buckley, & Forneris, 1996; Ruggiero, Del Ben, Scotti, & Rabalais, 2003; Ventureyra, Yao, Cottraux, Note, & De Mey-Guillard, 2002). Respondents rated symptom severity (within the last 30 days) on a five point Likert scale from not at all (1) to extremely (5). Any 9/11-related PTSD was defined as a PCL-17 score of ≥44 at Registry survey Waves 1, 2, or 3.
Exposure to 9/11 was defined with a 12-item summary measure used in previous Registry reports (Brackbill, Stellman, Perlman, Walker, & Farfel, 2013) and categorized as none (0-1 exposures) or any (≥2). Traumatic life event score at Wave 3 was based on a sum of endorsement of up to eight events or situations other than the 9/11 disaster and expressed categorically as none, 1, or >1 traumatic life event post-9/11.
A composite measure of psychosocial resources was created from a social integration index (Brissete, 2000) and the Medical Outcomes Study Modified Social Support Survey (MOS-MSSS) (Ritvo, 1997) 5-item version at Wave 3. These two measures have a nearly orthogonal relationship (Schwarzer & Leppin, 1991). The social integration index consisted of four items that referred to contact with friends or relatives and attendance at religious services or volunteer activities. Social support was assessed using a five point Likert scale from none (0) to all (4) of the time. This scale covered multiple dimensions, including emotional/information support (e.g., someone who understands your problems), tangible support (e.g., someone to take you to the doctor), and positive social interaction (e.g., someone to have a good time with); responses were summed for a total score range of 0-20 (Ghuman, Brackbill, Stellman et al., 2014). The responses to the two scales were dichotomized (social integration: none/1 source vs. >1 source; social support: <16 (median score) vs. ≥16) and combined to create a three level social support index categorized as high (>1 source and social support ≥16), intermediate (>1 source and social support 0-15 or none/1 source and social support ≥16), and low (none/1 source and social support 0-15).
Hurricane Sandy-related probable PTSD was assessed in the Sandy survey using a version of the PCL-17 that was identical to that used to assess 9/11-related PTSD, except the eight questions referring to 9/11 were re-worded to refer to Sandy. Sandy-related PTSD was defined as a PCL-17 score of ≥44 at the Sandy survey.
A Sandy traumatic experiences measure consisted of nine individual trauma items derived from questions used after Hurricane Katrina (Galea et al., 2007): stranded during or after the storm; feared for life or safety; unsure about safety or whereabouts of others; family or friends injured or killed; witnessed terrible events; personally threatened/robbed/assaulted; family or friends threatened/ robbed/assaulted; home broken into/robbed; unable to communicate with others. Affirmative responses to these items were summed to create categorical levels of traumatic experiences including none/ low (0-1 exposures), medium (2-3), and high Sandy trauma (4-9). Other Sandy exposures included home evacuation, property damage (e.g., living in a home flooded with ≥3 feet of water), degree of home damage, property loss, financial cost of damage to home or possessions due to Sandy, and sustaining a Sandy-related injury in the first week after the storm.
A separate composite Hurricane Sandy exposure scale comprised of individual Hurricane Sandy trauma items as well as financial and other Sandy impacts was created by combining the following seven yes/no measures: high Sandy trauma, evacuated home ≥7 days, flooded living area with ≥3 feet of water, damaged (inhabitable and uninhabitable) home, loss of >1 possessions (e.g., important documents, items of sentimental or financial value, vehicle, other possessions), financial cost of damage ≥$25,000, and any injury sustained in the first week after Sandy. The number of yes responses was used to create a four-level Sandy exposure scale (no exposure, 1-2, 3-4, and 5-7).
Study Sample
The study sample includes 4,558 surveys completed from April 10-November 7, 2013. Persons with incomplete information on Sandy-related PTSD were excluded (n=421). This resulted in a final sample size of 4,137; 2,214 surveys (53.5%) were from inundation zone residents and 1,923 (46.5%) were from non-inundation zone residents.
Statistical Analysis
Chi-square tests were used to test for significant associations between Sandy-related PTSD and selected sociodemographic characteristics, 9/11 exposures, and Sandy exposures and experiences. Adjusted odds ratios (AOR) were calculated using logistic regression to estimate the strength of the association between selected covariates (see footnote in Table 4) and Sandy-related PTSD among persons who resided in an inundation zone. All analyses were conducted using SAS Version 9.2.
Results
Enrollees who resided in a Hurricane Sandy inundation zone were more likely to be female, divorced/separated or never married, and have lower income and education compared to those who resided in a non-inundation zone (Table 1). Persons who resided in the inundation and non-inundation zones had similar levels of social support 1-2 years prior to Sandy. However, Sandy-related PTSD prevalence 5-12 months post-Sandy was higher among residents of the inundation zone (11.3%) compared to the non-inundation zone (4.4%).
| OverallSample | Inundation Zone | Non-Inundation Zone | |
|---|---|---|---|
| N (%) | N (%) | N (%) | |
| Total | 4,137 (100.0) | 2,214 (100.0) | 1,923 (100.0) |
| Sociodemographic Characteristics | |||
| Gender | |||
| Male | 2,328 (56.3) | 1,172 (52.9) | 1,156 (60.1) |
| Female | 1,809 (43.7) | 1,042 (47.1) | 767 (39.9) |
| Age Group at W3 (years) | |||
| 18-29 | 100 (2.4) | 63 (2.8) | 37 (1.9) |
| 30-44 | 786 (19.0) | 374 (16.9) | 412 (21.4) |
| 45-64 | 2,642 (63.9) | 1,430 (64.6) | 1,212 (63.0) |
| ≥65 | 609 (14.7) | 347 (15.7) | 262 (13.6) |
| Race/Ethnicity | |||
| Non-Hispanic White | 3,009 (72.7) | 1,621 (73.2) | 1,388 (72.2) |
| Non-Hispanic Black | 382 (9.2) | 176 (7.9) | 206 (10.7) |
| Hispanic or Latino | 447 (10.8) | 251 (11.3) | 196 (10.2) |
| Asian | 198 (4.8) | 110 (5.0) | 88 (4.6) |
| Multiracial/Other | 101 (2.4) | 56 (2.5) | 45 (2.3) |
| Household Income in 2010 | |||
| ≤$25,000 | 396 (10.0) | 264 (12.5) | 132 (7.1) |
| $25,001-50,000 | 552 (13.9) | 317 (15.0) | 235 (12.7) |
| $50,001-75,000 | 664 (16.8) | 342 (16.2) | 322 (17.4) |
| $75,001-150,000 | 1,497 (37.8) | 740 (35.1) | 757 (40.9) |
| >$150,000 | 849 (21.5) | 444 (21.1) | 405 (21.9) |
| Marital Status at Wave 3 | |||
| Married/living with partner | 2,569 (62.6) | 1,287 (58.6) | 1,282 (67.1) |
| Divorced/separated | 591 (14.4) | 349 (15.9) | 242 (12.7) |
| Widowed | 169 (4.1) | 105 (4.8) | 64 (3.3) |
| Never married | 778 (18.9) | 455 (20.7) | 323 (16.9) |
| Education at Wave 1 | |||
| Less than high school | 159 (3.9) | 108 (4.9) | 51 (2.7) |
| High school graduate/GED | 767 (18.6) | 412 (18.6) | 355 (18.5) |
| Some college | 964 (23.3) | 500 (22.6) | 464 (24.2) |
| College/post-graduate | 2,239 (54.2) | 1,190 (53.8) | 1,049 (54.7) |
| Hurricane Sandy-relatedPTSD | |||
| Yes | 335 (8.1) | 251 (11.3) | 84 (4.4) |
| No | 3,802 (91.9) | 1,963 (88.7) | 1,839 (95.6) |
| Low | 181 (4.5) | 105 (4.9) | 76 (4.1) |
| Intermediate | 2,117 (52.9) | 1,179 (55.1) | 938 (50.4) |
| High | 1,703 (42.6) | 856 (40.0) | 847 (45.5) |
| a Assessed via Sandy-specific PCL-17, 5-12 months after Sandy; defined as a PCL-17 score ≥44 at Hurricane Sandy survey. | |||
Table 1: Sociodemographic Characteristics and Hurricane Sandy-related PTSD status a among Adult Registry Enrollees by Inundation Zone Residence (n=4,137)
As shown in Table 2, the percent of persons with 9/11 exposure and traumatic life events post-9/11 was similar for enrollees in the inundation and non-inundation zones; however, individuals in the inundation zone had a somewhat higher proportion of any 9/11-related PTSD (33.5% and 29.7%, respectively). In the inundation zone, the prevalence of Sandy-related PTSD was higher among individuals who had a history of any 9/11-related PTSD (28.8%), low social support (28.6%), >1 traumatic life event post-9/11 (19.7%), and ≥2 9/11 exposures (12.9%).
| Inundation Zone | Non-Inundation Zone | |||
|---|---|---|---|---|
| Total | Hurricane Sandy-related PTSDa,b | Total | Hurricane Sandy-related PTSDa,b | |
| N (%) | % | N (%) | % | |
| 9/11-related PTSD c | ||||
| Yes | 646 (33.5) | 28.8 | 516 (29.7) | 14.3 |
| No | 1,281 (66.5) | 4.1 | 1,221 (70.3) | 0.7 |
| 9/11 Exposure | ||||
| Yes | 1,619 (73.1) | 12.9 | 1,416 (73.6) | 4.9 |
| No | 595 (26.9) | 7.2 | 507 (26.4) | 2.8 |
| Traumatic Life Events Post-9/11 d | ||||
| 0 | 1,518 (69.0) | 8.7 | 1,258 (66.0) | 3.7 |
| 1 | 351 (16.0) | 14.5 | 378 (19.8) | 4.2 |
| >1 | 330 (15.0) | 19.7 | 270 (14.2) | 7.8 |
| Social Integration/Social Support Index | ||||
| Low | 105 (4.9) | 28.6 | 76 (4.1) | 11.8 |
| Intermediate | 1,179 (55.1) | 13.2 | 938 (50.4) | 5.3 |
| High | 856 (40.0) | 6.8 | 847 (45.5) | 2.6 |
| a Assessed via Sandy-specific PCL-17, 5-12 months after Sandy; defined as a PCL-17 score ≥44 at Hurricane Sandy survey. b Expressed as row percents. c Assessed via 9/11-specific PCL-17; defined as a PCL-17 score ≥44 at Registry Wave 1, 2, or 3. d Assessed through Wave 3 (2011-12); excludes Hurricane Sandy. |
||||
Table 2: The prevalence of Hurricane Sandy-related PTSD a in Relation to 9/11 Exposures and Experiences among Adult Registry Enrollees by Inundation Zone Residence (n=4,137)
Among enrollees residing in the inundation zone, more than onequarter evacuated their home for ≥7 days (25.7%), sustained damage to their home (40.4%), lost >1 possession (28.1%), or experienced a financial cost of damage ≥$25,000 (25.3%) (Table 3). The highest prevalence of Sandy-related PTSD was among those who reported an injury one week after Sandy (31.2%), followed by those whose home living area was flooded with ≥3 feet of water (25.1%), home was damaged and uninhabitable/destroyed (25.1%), and experienced high Sandy trauma (23.2%).
| Inundation Zone | ||
|---|---|---|
| Total | Hurricane Sandy- related PTSDa,b |
|
| N (%) | % | |
| Total | 2,214 (100.0) | 11.3 |
| Hurricane Sandy Traumatic Experiences | ||
| High (4-9) c | 664 (30.0) | 23.2 |
| Medium (2-3) | 1,071 (48.4) | 7.0 |
| None/Low (0-1) | 479 (21.6) | 4.6 |
| Evacuated Home | ||
| Evacuated ≥7 days c | 555 (25.7) | 20.4 |
| Evacuated <7 days | 478 (22.1) | 7.3 |
| Did not evacuate | 1,128 (52.2) | 8.2 |
| Flooded Living Area with ≥3 Feet of Water | ||
| Yes, flooded c | 334 (15.1) | 25.1 |
| No | 1,880 (84.9) | 8.9 |
| Home Damage | ||
| Damaged and uninhabitable/destroyed c | 435 (19.9) | 25.1 |
| Damaged but habitable c | 449 (20.5) | 15.1 |
| None/minimal | 1,303 (59.6) | 5.3 |
| Property Loss | ||
| >1 possession c | 621 (28.1) | 22.4 |
| 1 possession | 267 (12.1) | 15.4 |
| None | 1,319 (59.8) | 5.3 |
| Financial Cost of Damage (Q43) | ||
| ≥$25,000 c | 528 (25.3) | 23.5 |
| <$25,000 | 1,560 (74.7) | 7.3 |
| Any Injury (Q55) | ||
| Yes, injury c | 221 (10.5) | 31.2 |
| No | 1,874 (89.5) | 8.2 |
| a Assessed via Sandy-specific PCL-17, 5-12 months after Sandy; defined as a PCL-17 score ≥44 at Hurricane Sandy survey. b Expressed as row percents. c These elements were used to generate the composite Hurricane Sandy exposure scale in Table 4. |
||
Table 3: Hurricane Sandy-related PTSD a in Relation to Hurricane Sandy-Exposures and Experiences among Adult Registry Enrollees Residing in an Inundation Zone by (n=2,214)
We observed a dose-response relationship between Sandy exposures and Sandy-related PTSD, with the odds of Sandy-related PTSD increasing from 1-2 exposures (AOR=2.7, 95% CI: 1.6- 4.5) to 5-7 exposures (AOR=16.8, 95% CI: 9.7-29.0) (Table 4). The likelihood of Sandy-related PTSD was nearly 7 times greater for persons with a prior history of 9/11-related PTSD (AOR=6.6, 95% CI: 4.6-9.6) and 3 times greater for those who previously reported indicators of low social support (AOR=2.7, 95% CI: 1.4- 5.1). An intermediate level of social support was also significantly associated with Sandy-related PTSD (AOR=1.6, 95% CI: 1.1-2.4) when compared to those with high social support. Interestingly, 9/11 exposure was not associated with Sandy-related PTSD.
| Crude OR(95% CI) | Adjusted OR a(95% CI) | |
|---|---|---|
| 9/11 Exposure | ||
| Yes | 1.9 (1.3-2.7) | 1.3 (0.8-2.0) |
| No | 1.0 | 1.0 |
| 9/11-relatedPTSD | ||
| Yes | 9.6 (6.9-13.2) | 6.6 (4.6-9.6) |
| No | 1.0 | 1.0 |
| Traumatic Life Events Post-9/11 b | ||
| 0 | 1.0 | 1.0 |
| 1 | 1.8 (1.3-2.5) | 1.5 (1.0-2.3) |
| >1 | 2.6 (1.9-3.6) | 1.4 (0.9-2.1) |
| Social Integration/Social Support Index | ||
| Low | 5.5 (3.3-9.1) | 2.7 (1.4-5.1) |
| Intermediate | 2.1 (1.5-2.9) | 1.6 (1.1-2.4) |
| High | 1.0 | 1.0 |
| Composite Hurricane Sandy Exposure Scale | ||
| 5-7 exposures | 13.9 (8.8-21.8) | 16.8 (9.7-29.0) |
| 3-4 exposures | 7.0 (4.4-11.0) | 7.6 (4.5-13.0) |
| 1-2 exposures | 3.6 (2.3-5.7) | 2.7 (1.6-4.5) |
| No exposure | 1.0 | 1.0 |
| a Adjusted for gender, age group at Wave 3, race/ethnicity, and household income in 2010. b Assessed through Wave 3 (2011-12); excludes Hurricane Sandy. |
||
Table 4: Association between Hurricane Sandy experiences and Hurricane Sandy-Related PTSD among Hurricane Sandy Survey Participants Residing in an Inundation Zone (n=2,214)
Discussion
Hurricane Sandy placed individuals in grave danger, destroyed homes and neighborhoods, and for many who lived in flooded areas, resulted in months of being displaced or living in homes requiring extensive repairs. As expected, having experienced Sandy traumatic events greatly increased the likelihood of symptoms indicative of Sandy-related PTSD, in addition to the independent effects of prior history of 9/11-related PTSD and low social support (Gray, Maguen, & Litz, 2004). This study confirms the relatively high prevalence of Sandy-related PTSD previously reported and extends the understanding of Sandy-related PTSD by accounting for prior PTSD history (Boscarino et al., 2013; Palgi et al., 2014).
The prevalence of PTSD in the present study 5-12 months post- Sandy among persons who lived in the inundation zone (11.3%) was similar to that observed 6-8 months post-Sandy by Boscarino et al. (2013) among New Jersey shore residents (14.5%), even though they used a different tool to measure PTSD (the four-item Primary Care PTSD Screener). It is important to note that 4.4% of persons in the present study who lived in the non-inundation zone had symptoms indicative of Sandy-related PTSD. This may be expected, as persons outside the flooded areas also experienced the impact of Sandy through electrical power outages, heat loss, and transportation issues.
Our study measured 9/11 exposure, 9/11-related PTSD symptomatology, and social support prior to Sandy, in contrast to two other cross-sectional studies that measured these factors concurrent with assessing the impact of Sandy trauma on the development of PTSD (Boscarino et al., 2013; Palgi et al., 2014). Similar to both studies, we found that high storm exposure and low social support were associated with Sandy-related PTSD. As an established risk for 9/11-related PTSD, exposure to the 9/11 disaster (e.g., being injured, witnessing horrible events) (Brackbill et al., 2009; Liu et al., 2014) was not associated with Sandy-related PTSD in our study; this is in contrast to Palgi et al. (2014) who reported that recollection of prior disaster experiences, including the WTC disaster, was significantly associated with Sandy-related PTSD symptoms. Palgi et al. (2014) hypothesized that the memory of prior disasters and related trauma sensitized people to the negative impact of Sandy-related trauma resulting in Sandy-related PTSD symptoms. However, in the current study 9/11-related PTSD symptomatology was a strong risk factor for Sandy-related PTSD. This is consistent with Breslau et al. (2008) who found that persons who had a prior trauma and PTSD were significantly more likely to have subsequent PTSD following a new trauma than persons who had prior trauma and no PTSD.
After adjusting for the association between Sandy-related trauma and 9/11-related PTSD symptomatology, low levels of social support reported prior to Sandy were significantly associated with Sandy-related PTSD. Specifically, we found a strong dose-response association between a composite social integration/social support measure and Sandy-related PTSD. A number of other disaster-related studies, including hurricanes and 9/11, have reported a buffering effect of social support to stress reactions resulting from disaster events (Acierno et al., 2007; Boscarino et al., 2013; Brackbill et al., 2009; Galea et al., 2002; Schwarzer et al., 2014). These studies have generally measured social support retrospectively, with the exception of Schwarzer et al. (2014). Using a pre-Sandy measure of social support, we observed a significant dose-response relationship between level of social support and Sandy-related PTSD; individuals with a low or intermediate level of social support had an increased likelihood of Sandy-related PTSD.
From a public health perspective, the identification of persons who have a history of PTSD symptoms is important so that health practitioners can monitor the development of new symptoms if a major trauma event occurs, such as a damaging storm or earthquake. Typically, after major disasters brief mental health counseling is made available for persons directly affected by the physical consequences of the event. Beginning in November 2012, Project HOPE provided no-cost individual and group counseling, education, and referrals for persons impacted by Sandy in NYC. It is important that counseling protocols take into account PTSD symptom history resulting from prior disasters.
The major strength of this study is the large and diverse prospective cohort of persons exposed to WTC disaster on 9/11, among which there was a substantial group who were directly affected by Hurricane Sandy. It is fortuitous that we completed a follow-up of this cohort 1-2 years before the hurricane occurred in October 2012, providing timely pre-storm health status and other contextual information such as income and marital status. It is noteworthy that we used event specific measures of probable PTSD for both the 9/11 disaster and Sandy using a standard scale anchored to either 9/11 or Sandy.
There are several limitations to this study. First, we achieved a moderate response rate of 53.5% among persons who lived in inundated zones. Although Sandy survey participants were slightly more likely than non-participants to be female, older, non-Hispanic white, lower Manhattan area workers/passersby, and have higher levels of education and 9/11 exposure, they did not differ from nonparticipants on household income, marital status, or 9/11-related PTSD status. Second, our findings are not generalizable to the general population, given that the source of the sample was defined as persons with potential exposure to 9/11. However, our data are somewhat unique and offer insight into the consequences of natural disasters. Moreover, because this was a WTC disaster cohort we were able to address the scientific issue of prior trauma in the induction of PTSD among Sandy exposed persons. Third, there may have been response bias in the measurement of Sandy-related PTSD because of multiple prior 9/11-related PTSD assessments. It would be difficult to determine if multiple measurements of PTSD created a priming effect on subsequent responses, although repeated monitoring of health is a common practice.
Conclusion
Public health preparation for events similar to Hurricane Sandy should incorporate outreach and linkages to care for persons who had prior disaster-related trauma. Further studies using these data will assess the association between storm-related experiences and environmental exposures on both physical and mental health.
Acknowledgements
Conflicts of Interest
Ms. Caramanica and Drs. Brackbill, Stellman, and Farfel report no conflicts of interest.
Funding/Support
This study was supported by Cooperative Agreement U50/ OH009739 from the National Institute for Occupational Safety and Health; Cooperative Agreement U50/ATU272750 from the Agency for Toxic Substances and Disease Registry of the Centers for Disease Control and Prevention, which included support from the National Center for Environmental Health (NCEH); and the NYC Department of Health and Mental Hygiene (NYCDOHMH). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of CDC.
Role of the Funder/Sponsor
The sponsor provided advice on the design of the study, reviewed the manuscript, and had a minor role in the collection, management, analysis, and interpretation of the data and the preparation of the manuscript apart from approval of the manuscript.
Additional Contributions
We gratefully acknowledge the participation of all Registry enrollees, particularly the 4,558 who completed the Hurricane Sandy survey. We thank all staff from the NYCDOHMH who collected the data. We also acknowledge the following NYCDOHMH employees for their consultation in study design, data analysis, or critical review of the manuscript: Drs. Charon Gwynn, James Hadler, and Sukhminder Osahan.
References
- Abramson, D.M., & Redlener, I. (2012). Hurricane sandy: lessons learned, again. Disaster Medicine and Public Health Preparedness, 6(4), 328-329
- Acierno, R., Ruggiero, K.J., Galea, S., Resnick, H.S., Koenen, K., Roitzsch, J., et al. (2007). Psychological sequelae resulting from the 2004 Florida hurricanes: implications for postdisaster intervention. American Journal of Public Health, 97 (Suppl 1), S103-108
- Blanchard, E.B., Jones-Alexander, J., Buckley, T.C., & Forneris, C.A. (1996). Psychometric properties of the PTSD Checklist (PCL). Behaviour Research and Therapy, 34(8), 669-673
- Boscarino, J.A., Hoffman, S.N., Kirchner, H.L., Erlich, P.M., Adams, R.E., Figley, C.R., et al. (2013). Mental health outcomes at the Jersey Shore after Hurricane Sandy. International Journal of Emergency Mental Health, 15(3), 147-158
- Brackbill, R.M., Hadler, J.L., DiGrande, L., Ekenga, C.C., Farfel, M.R., Friedman, S., et al. (2009). Asthma and posttraumatic stress symptoms 5 to 6 years following exposure to the World Trade Center terrorist attack. Journal of American Medical Association, 302(5), 502-516
- Brackbill, R.M., Stellman, S.D., Perlman, S.E., Walker, D.J., & Farfel, M.R. (2013). Mental health of those directly exposed to the World Trade Center disaster: unmet mental health care need, mental health treatment service use, and quality of life. Social Science and Medicine, 81, 110-114
- Breslau, N., Peterson, E.L., & Schultz, L.R. (2008). A second look at prior trauma and the posttraumatic stress disorder effects of subsequent trauma: a prospective epidemiological study. Archives of General Psychiatry, 65(4), 431-437
- Brissete, I., Cohen, S., Seeman, T.E. (2000). Measuring social integration and social networks. In S. Cohen, Underwood, L.G., Gottlieb, B.H. (ed.), Social Support Measurement and Intervention: A Guide for Health and Social Scientists,New York: Oxford University Press
- Farfel, M., DiGrande, L., Brackbill, R., Prann, A., Cone, J., Friedman, S., et al. (2008). An overview of 9/11 experiences and respiratory and mental health conditions among World Trade Center Health Registry enrollees. Journal of Urban Health, 85(6), 880-909
- Galea, S., Ahern, J., Resnick, H., Kilpatrick, D., Bucuvalas, M., Gold, J., et al. (2002). Psychological sequelae of the September 11 terrorist attacks in New York City. New England Journal of Medicine, 346(13), 982-987
- Galea, S., Brewin, C.R., Gruber, M., Jones, R.T., King, D.W., King, L.A., et al. (2007). Exposure to hurricane-related stressors and mental illness after Hurricane Katrina. Archives of General Psychiatry, 64(12), 1427-1434
- Ghuman, S.J., Brackbill, R.M., Stellman, S.D., Farfel, M.R., & Cone, J.E. (2014). Unmet mental health care need 10-11 years after the 9/11 terrorist attacks: 2011-2012 results from the World Trade Center Health Registry. BMC Public Health, 14, 491
- Gray, M.J., Maguen, S., & Litz, B.T. (2004). Acute psychological impact of disaster and large-scale tauma: limitations of traditional interventions and future practice recommendations. Prehospital and Disaster Medicine, 19(1), 64-72
- Liu, B., Tarigan, L.H., Bromet, E.J., & Kim, H. (2014). World Trade Center disaster exposure-related probable posttraumatic stress disorder among responders and civilians: a meta-analysis. PLoS One, 9(7), e101491
- Neria, Y., Nandi, A., & Galea, S. (2008). Post-traumatic stress disorder following disasters: a systematic review. Psychological Medicine, 38(4), 467-480
- Norris, F.H., Friedman, M.J., Watson, P.J., Byrne, C.M., Diaz, E., & Kaniasty, K. (2002). 60,000 disaster victims speak: Part I. An empirical review of the empirical literature, 1981-2001. Psychiatry, 65(3), 207-239
- Palgi, Y., Shrira, A., Hamama-Raz, Y., Palgi, S., Goodwin, R., & Ben-Ezra, M. (2014). Not so close but still extremely loud: recollection of the world trade center terror attack and previous hurricanes moderates the association between exposure to hurricane sandy and posttraumatic stress symptoms. Comprehensive Psychiatry, 55(4), 807-812
- Ritvo, P.G., Fischer, J.S., Miller, D.M., Andrews, H., Paty, D.W., & LaRocca, N.G. (1997). Multiple Sclerosis Quality of Life Inventory: A User's Manual Retrieved October 6, 2014, from http://www.nationalmssociety.org/NationalMSSociety/media/MSNationalFiles/Brochures/MSQLI_-A-User-s-Manual.pdf
- Ruggiero, K.J., Del Ben, K., Scotti, J.R., & Rabalais, A.E. (2003). Psychometric properties of the PTSD Checklist-Civilian Version. Journal of Traumatic Stress, 16(5), 495-502
- Schwarzer, R., Bowler, R.M., & Cone, J.E. (2014). Social integration buffers stress in New York police after the 9/11 terrorist attack. Anxiety Stress and Coping, 27(1), 18-26
- Schwarzer, R., &Leppin, A. (1991). Social Support and Health: A theoretical and empirical overview. Journal of Social and Personal Relationships 8(1), 99-127
- Shrira, A., Palgi, Y., Hamama-Raz, Y., Goodwin, R., & Ben-Ezra, M. (2014). Previous exposure to the world trade center terrorist attack and posttraumatic symptoms among older adults following hurricane sandy. Psychiatry, 77(4), 374-385
- Ventureyra, V.A., Yao, S.N., Cottraux, J., Note, I., & De Mey-Guillard, C. (2002). The validation of the Posttraumatic Stress Disorder Checklist Scale in posttraumatic stress disorder and nonclinical subjects. Psychotherapy and Psychosomatics, 71(1), 47-53.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 14719
- [From(publication date):
specialissue-2015 - Jul 31, 2025] - Breakdown by view type
- HTML page views : 10044
- PDF downloads : 4675