Research Article Open Access
The Compassion Fatigue and Resilience Connection: A Survey of Resilience, Compassion Fatigue, Burnout, and Compassion Satisfaction among Trauma Responders
Harvey J. Burnett, Jr.1*, Kathleen Wahl2
1Behavioral Sciences Department, Andrews University, Michigan, United States
2Michigan Department of Community Health, Office of Public Health Preparedness United States
Visit for more related articles at International Journal of Emergency Mental Health and Human Resilience
Abstract
Research has shown that compassion fatigue is associated with burnout and compassion satisfaction. Practically no studies have examined how resilience may impact these variables. This study examined how resilience is related to compassion fatigue, burnout, and compassion satisfaction among a convenience sample of disaster behavioral health and emergency preparedness responders (N =139) attending a training conference in Michigan. Measures included the 30-item Professional Quality of Life Scale, the 14-item Resilience Scale, and a demographic questionnaire. Seventy-two percent of the participants were at risk for compassion fatigue, while 19% were at risk for burnout. Only 22% of participants had scores indicative of high resilience. Resilience was found to have a significant negatively correlation with compassion fatigue and with burnout. A significant positive correlation was also found between compassion satisfaction and resilience. Mediation analysis found that resilience moderately mediated the relationship between compassion fatigue and burnout. These findings suggest that resilience plays an important role in mediating the effects between compassion fatigue and burnout. Implications for practice are discussed.
Keywords
Burnout, compassion fatigue, compassion satisfaction, resilience
Disasters and other critical incidents that occur throughout the world today can have an impact on those affected. Unfortunately, professionals who work in the field of disaster response can be affected as well. In fact, the very nature of “helping and caring,” which is embedded within the disaster behavioral health and emergency response professions, practically exposes these populations to the continuous realm of trauma experiences that may impact their ability to cope and provide critical services. Indirect trauma exposure related problems such as compassion fatigue and burnout are possible negative resultant outcomes. On the other hand, factors as resilience and compassion satisfaction may have an important role in ameliorating the dangerous effects of compassion fatigue and burnout among disaster behavioral health and emergency preparedness response providers.
Compassion Fatigue
The phenomenon known as compassion fatigue (CF) was first identified by Joinson (1992) among nurses who exhibited feelings of anger and helplessness or turned off their own emotions in response to watching their patients suffering from major illnesses or trauma. Figley (1995) defined CF as the normal behavioral and emotional responses resulting from an individual “knowing about a traumatizing event experiences by a significant other – the stress resulting from helping or wanting to help a traumatized or suffering person” (p. 7). In other words, CF is the “cost of caring” (Figley, 1995, p. 1) that can impact the trauma service provider cognitively, emotionally, behaviorally, spiritually, interpersonally and physically (Yassen, 1995).
In fact, CF has also been constructually defined as Secondary Traumatic Stress (STS) or secondary trauma within trauma literature (Figley, 1995; Motta, 2008; Cieslak, Shoji, Douglas, Melville, Luszczynska, & Benight, 2013). STS is conceptually similar to Posttraumatic Stress Disorder reactions and its symptomatology parallels those individuals who have been directly exposed to a traumatic event (Figley, 1995; Bride, Robinson, Yegidis, & Figley 2004; Motta, 2008; Cieslak et al., 2013). More specifically, STS was found highly correlated with emotional exhaustion in relation to depersonalization or lack of accomplishment (Cieslak et al., 2013). Hence, the more chronic version of secondary traumatic stress (Secondary Traumatic Stress Disorder, STSD) has three identified symptom clusters that involve re-experiencing the traumatic event, avoidance/numbing of reminders of the event, and persistent physiological arousal (Figley, 1995; Stamm, 2010; Cieslak et al., 2013). STSD symptoms may develop after one month or more among trauma care providers or responders who have had indirect exposure to individuals that have suffered from primary exposure to a trauma event (Figley, 1995; Cieslak et al., 2013).
Another construct that is common within the trauma literature that is synonymous with CF is vicarious traumatization. Vicarious traumatization is considered the negative reactions that can develop among trauma care workers as a result of their “empathetic engagement” with trauma victims (Pearlman & Saakvitne, 1995) and often times is more associated with alteration of core beliefs and cognitive schemas as a result of extensive interactions with trauma victims (McCann & Pearlman, 1990; Motta, 208). Motta (2008) however indicated in his literature review that STS and vicarious traumatization are not entirely distinct concepts. For the purposes of this study CF is considered synonymous with STS, secondary trauma, and vicarious traumatization.
Studies have noted several variables that may predict the development of CF. These variables included: female gender; age; increased exposure to trauma clients; length of time providing sexual abuse treatment; occupational stress; the clinician’s own personal history of trauma exposure; regular access to supervision; lack of supportive social network; and self-efficacy (Wee & Myers, 2002; Baird & Kracen, 2006; Sprang, Clark, & Whitt-Woosley, 2007; Killian, 2008; Pietrantoni & Prati, 2008; Craig & Sprang, 2010). Caseloads with PTSD clients and implementing evidence-based practice (Sprang et al., 2007; Craig & Sprang, 2010), as well as the attachment styles of avoidance and ambivalence (Tosone, Bettmann, Minami, & Jasperson, 2010) were also found to be significant predictors of CF. Figley (1995) further suggested that employing empathy, having experienced some prior traumatic event, the activation of unresolved traumas that are similar in clients, or helping children who have been exposed to traumatic events may contribute to the vulnerability among trauma and emergency workers to develop CF.
Burnout and Compassion Fatigue
An element of CF is burnout. Empirical studies on burnout suggest that it is prevalent in the helping professions (Maslach & Jackson, 1984; Craig & Sprang, 2010; Newell & MacNeil, 2011; Cieslak et al., 2013). Pines and Aronson (1988) conceptually defined burnout as a “state of physical, emotional and mental exhaustion caused by long term involvement in emotionally demanding situations” (as cited in Figley, 1995, p.11). Stamm (2010) associated burnout with feelings of hopelessness and difficulties in dealing with work or in doing one’s job effectively. A more three-dimensional framework regarding job burnout suggests that prolonged exposure to job stressors may result in the responses of exhaustion, cynicism, and inefficacy (Maslach, Schaufeli, & Leiter, 2001).
Figley (1995) posited that the emergence of burnout is a gradual process that results from emotional exhaustion, whereas CF can occur suddenly with little warning. Craig and Sprang (2010) found that age, working in an inpatient setting, having specialized training on trauma assessment and treatment, having a high percentage of PTSD caseloads, and using evidence-based practices were significant predictors of burnout.
A meta-analysis of 41 studies among workers indirectly exposed to trauma suggested a strong association between burnout and CF, especially when both constructs were assessed with the Professional Quality of Life Scale (Cieslak et al, 2013). Other factors, such as female gender, working in an occupation that only involve secondary exposure to trauma victims, employment in North American, and using English-language versions of assessment measures were significant moderators of the relationship between burnout and CF (Cieslak et al., 2013).
Compassion Satisfaction
Trauma research has also focused on the variable of compassion satisfaction (CS). CS refers to the fulfillment that an individual derives from their work and from the act of helping itself (Stamm, 2002; Craig & Sprang, 2010; Stamm, 2010). One important aspect of CS involves training. Research has indicated that professionals who received specialized trauma training had higher levels of CS and decreased levels of CF and burnout (Ortlepp & Friedman, 2002; Linley & Joseph, 2007; Sprang et al., 2007). Other variables that seem linked with CS and tend to buffer the effects of CF include: older age; access to clinical supervision; training for new and experienced mental health workers; perceived coping capability; emotional separation; years of clinical experience; self-care strategies; and social support (Sprang et al., 2007; Craig & Sprang, 2010).
Compassion Fatigue, Burnout and Compassion Satisfaction
A plethora of research literature has indicated that compassion fatigue, burnout and compassion satisfaction are associated with each other (Sprang et al., 2007; Pietrantoni & Prati, 2008; David, 2012; Thomas, 2012; Ray, Wong, White & Heaslip, 2013; Slocum-Gori, Hemsworth, Chan, Carson & Kazanjian, 2013). Stamm (2010) suggested workers with high CS combined with moderate to low CF and burnout levels embodies a more positive behavioral outcome (e.g., receives positive reinforcement from work, no significant inability to be efficacious in their job, and is likely a good influence on their colleagues and organization).
Resilience
Wagnild and Young (1993) have defined resilience as the ability to cope, learn, and grow from difficult experiences. Ahern et al. (2006) categorized resilience as the ability to successfully cope with change or adversity. She also argues that resilience is a characteristic of the personality that handles the effects of negative stress and promotes adaptation. Everyly, Welzant and Jacobson (2008) suggested that resilience is based on a person’s ability to “positively adapt and/or rebound from significant adversity and the distress it often creates” (p. 262). Luther, Cicchetti and Becker (2000) referred to resilience as a “dynamic process encompassing positive adaptation within the context of significant adversity” (p. 543). However, Bonanno (2008) provided a more concise definition of resilience which argues that despite being exposed to trauma and loss, it is an individual’s ability to “maintain relatively stable, healthy levels of psychological and physical functioning across time and possess the ability to generate new experiences and positive emotions” (p. 102).
Resilience is comprised of multiple factors (i.e., hardiness, selfenhancement, repressive coping, positive emotion and laughter) and is derived from various pathways (Bonanno, 2005/2008; Mancini & Bonanno, 2009). Southwick and Charney (2012) reported 10 effective resilience coping mechanisms to manage stress and trauma (i.e., realistic optimism, facing fear, moral compass, religion and spirituality, social support, resilient role models, physical fitness, brain fitness, cognitive and emotional flexibility, and meaning and purpose). Everly and colleagues posited that human resilience is comprised of several core characteristics which include innovative, decisiveness, tenacity, interpersonal connectedness, honesty and integrity, self-control, and optimism (Everly, 2012; Everly & Lating, 2013).
One model that has been touted to provide a more integrative description of the resilience construct which advocate the difference between “protective factors and rebound capability” is the Johns Hopkins Tripartite Model of Resistance (Kaminsky, McCabe, Langlieb & Everly, 2007; Nucifora, Langlieb, Siegal, Everly & Kaminsky, 2007; Everly & Lating, 2013). This model asserts that resilience consists of three components: resistance, resilience and recovery. Furthermore, self-efficacy and self-confidence are important elements of this model and are central features of resilience (Everly, 2012; Everly & Lating, 2013).
Resilience studies have provided a further understanding on predictors of psychological resilience and characteristics of highly resilient people. Bonanno, Galea, Bucciarelli and Vlahov (2007) found that gender, age, race/ethnicity, education, level of trauma exposure, income change, social support, frequency of chronic disease, and recent and past life stressors were unique predictors of resilience. In addition, resilience has been found to correlate with CF, burnout, and CS (David, 2012). For the purposes of this study, resilience is defined as the ability to adapt to change or manage adverse life experiences.
Present Study
Trauma research has examined compassion fatigue, compassion satisfaction, and burnout but has not explored how resilience is related to these variables. The purpose of this study was to: (1) identify the prevalence of compassion fatigue among a sample of disaster behavioral health and emergency preparedness workers in Michigan; (2) examine how compassion fatigue, compassion satisfaction, and burnout are related to resilience; and (3) examine how compassion fatigue is affected by resilience in a way that reduces burnout.
Method
Participants
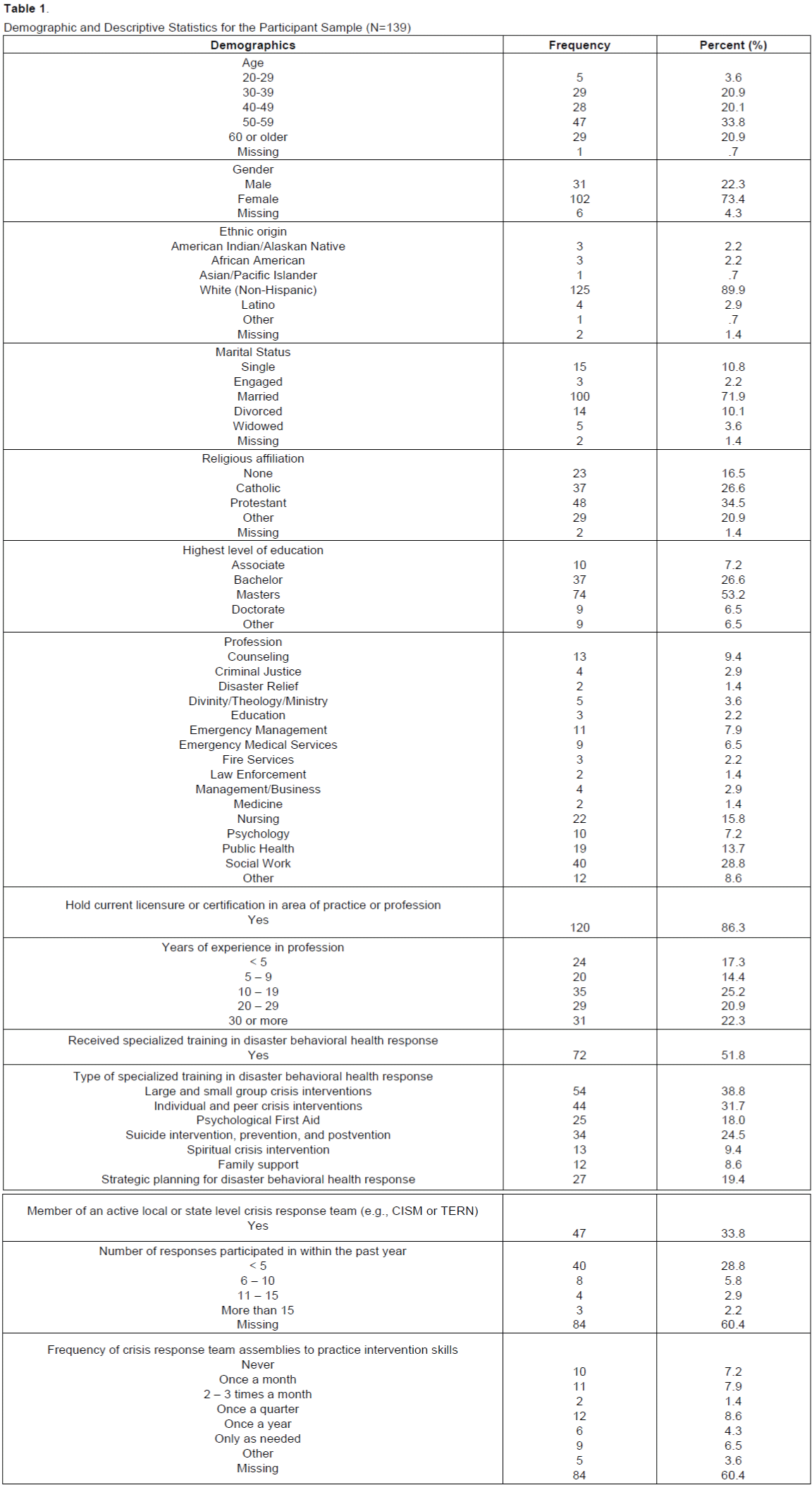
The data for this study was collected from a convenience sample of volunteer participants who attended the Fostering Resilience in the Aftermath: The Art of Delivering Disaster Behavioral Health Services conference held at the Kellogg Hotel and Conference Center in Lansing, Michigan on Thursday, November 7, 2013. After checking for completion, 139 useful surveys were obtained out 339 recorded attendees to the conference (41% participation rate). Of the 139 surveys, 23% were males and 77% were females; 72% were married, 11% were single, 10% were divorced, 4% were widowed, and 2% were engaged; and 53% had a Master’s degree, 27% had a Bachelor’s degree, 7% had an Associate’s degree, 6% had a Doctorate’s degree, and 6% indicated their highest level of education as “Other.” The ethnic distribution was 90% White (non-Hispanic), 3% Latino, 2% American Indian/Alaskan Native, 2% African American, 1% Asian/Pacific Islander, and 1% indicated their ethnic origin as “Other.” The age range was between 20 and older than 60, with 34% between ages 50-59, 21% between ages 30-39, 21% ages 60 or older, 20% between ages 40-49, and 4% between ages 20-29. In regards to years of experience in their profession, 25% had between 10-19 years, 22% had 30 or more years, 21% had between 20-29 years, 14% had between 5-9 years, and 17% had less than 5 years. The most frequent professions that participants indicated that they work in were: Social Work (n =40), Nursing (n =22), and Public Health (n =19). Table 1 provides further descriptive statistics regarding participant demographics.
Measures
The measures used in this study included a demographic questionnaire, the Professional Quality of Life Scale (ProQOL) and the 14-Item Resilience Scale (RS-14).
Professional Quality of Life Scale (ProQOL)
The ProQOL is a self-report measure that was developed by Stamm (2010) to assess compassion fatigue, compassion satisfaction, and burnout. The ProQOL contains 30 items (10 items for each subscale) that are rated on a 5-point Likert scale, ranging from 1 (Never) to 5 (Very Often). The average score on each subscale is 50 (SD =10), with higher scores being indicative of the subscale’s specific measure. Stamm (2010) reported that the ProQOL has demonstrated good construct validity and inter-scale correlations. Cronbach’s alpha reliabilities were 0.88 (compassion satisfaction (CS) subscale), 0.81 (compassion fatigue (CF) subscale), and 0.75 (burnout (BO) subscale).
The 14-item Resilience Scale (RS-14)
The Resilience Scale was originally developed by Wagnild and Young (1993) as a 25-item self-report questionnaire designed to measure five resilience themes using a 7-point Likert scale. Wagnild (2010) developed a shorter 14-item version of the original instrument. The RS-14 contains 14 items that are rated on a 7-point Likert scale, ranging from 1 (Strongly Disagree) to 7 (Strongly Agree). Cronbach’s alpha reliability was reported to be 0.93 and 0.91, respectively between two samples. Higher scores on the RS- 14 are indicative of higher resilience. The Resilience Scale and RS- 14 has demonstrated good construct, convergent, concurrent, and discriminant validity (Wagnild, 2010).
Procedure
Prior to the conference, written permission to use the conference to conduct the study was granted by the Director of the Michigan Office of Public Health Preparedness. The conference was sponsored by the Michigan Department of Community Health, Office of Public Health Preparedness. A research packet containing the informed consent, demographic questionnaire, ProQOL, and RS-14 was provided to all conference attendees in their registration packet. During the welcome/housekeeping phase of the conference, all attendees were informed about the study by the researchers and instructions were provided on how they could participate. The conference allotted time during lunch and at the end of the conference in which attendees who wish to participate could complete and return the documents to a clearly marked collection box designated for the study at the registration table.
Through the informed consent form, all attendees were notified about: the nature of the study; the number of questionnaires and time required to complete them; the risk involved; what they should do if they no longer wanted to participate once started; how confidentiality would be kept; and that all participants included in this study must be 18 years of age or older. After reading the informed consent form, participants detached the informed consent letter for their personnel record and completed all three questionnaires. The completed questionnaires were returned to a collection box marked “Survey” that was located at the registration table. Consent was given through completing and returning the forms which was indicated as a statement at the top of the first instrument which was the demographic questionnaire. Participation in the study was voluntary and anonymous. Both, the Andrews University and the Michigan Department of Community Health respective Institutional Review Boards granted permission to conduct the study.
All missing values on the ProQOL subscales and the RS-14 were imputed from their means in order to provide a complete set of data for analysis. The prevalence of CF, CS, BO and resilience were examined through frequency distributions using cut scores as recommended by the instrument developers. The Pearson’s r was utilized to examine the magnitude and direction of the relationship between participants’ scores on all four variables. Mediation analysis was then conducted using the mediation function in MBESS package version 3.3.3. (Kelley & Lai, 2012) in R 3.1.1 to examine whether any relationship between CF and BO was mediated by more resilience. Mediation analysis allows researchers to investigate whether the relation of an observed effect is due to a mediator or is spurious (MacKinnon, Fairchild, & Fritz, 2007; MacKinnon, Cheong, & Pirlott, 2012). The Preacher and Kelley (2011) κ2 statistic, which represents the proportion of the maximum possible indirect effect accounted for by the actual indirect effect, was used as a measure of mediation effect size. The present study applied the benchmarks of 0.01, 0.09, and 0.25 as small, medium, and large κ2 effect sizes respectively for qualitative interpretation of mediation (Preacher & Kelley, 2011).
Results
For the ProQOL subscales: CF subscale scores ranged from 0 to 3.70 (Mean =1.99, SD =0.52); CS subscale scores ranged from 0 to 5.00 (Mean =4.06, SD =0.60); and BO subscale scores ranged from 0 to 3.80 (Mean =2.04, SD =0.54). RS-14 scores ranged from 3.92 to 7.00 (Mean =5.90, SD =0.67).
Prevalence
The present study examined the prevalence of compassion fatigue among disaster behavioral health and emergency preparedness workers in the State of Michigan who attended the conference. Stamm (2010) established cut scores at the 25th and 75th percentile based on using a standardized score to indicate relative risk or protective factors on the ProQOL measures. CF had a standardized mean score of 49 which was lower than the standardized mean of 50, with 72.2% of participants who attended the conference scoring above the suggested 75th percentile cut score. On the BO subscale, the standardized mean and standardized sample mean were both 50, with 18.9% of participants scoring above the suggested 75th percentile cut score. For CS, the standardized sample mean was 55, compared to the standardized mean of 50, with 40.4% of participants scoring above the 75th percentile cut score.
In regards to resilience, scores below 64 on the RS-14 are considered low (Wagnild, 2010). Wagnild (2010) reported the total sample mean score on the RS-14 as 76.2, compared to our study mean of 82.6, with 4.5% of participants in this study scoring below 64. Approximately 22% of participants scored in the high resilient range, while 73.4% scored between the moderately low to moderately high resilient range.
Pearson’s r Analysis
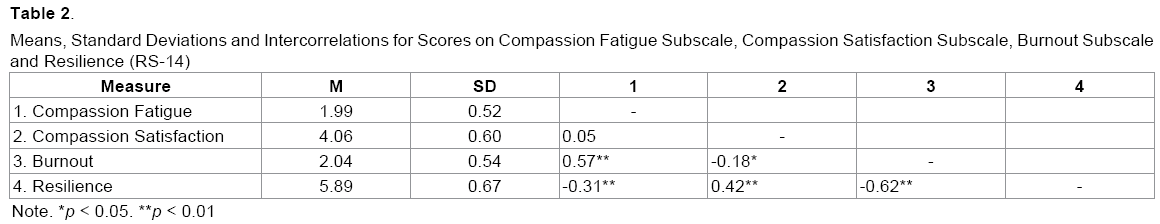
In regards to the magnitude and direction of the relationship between CF, CS, BO, and resilience (see Table 2), results indicated: no significant correlation between CF and CS (r =0.07, p =0.51); a significant positive correlation between CF and BO (r =0.57, p =0.00, r2=0.32); and a significant negative correlation between CF and resilience (r =-0.31, p = 0.00, r2 =0.10). CF accounted for 32% of the variance in BO and 10% of the variance in resilience. These results suggest that: (1) there was no association between compassion fatigue and compassion satisfaction; (2) higher scores of compassion fatigue were strongly associated with higher burnout scores; and (3) higher scores indicative of compassion fatigue were moderately associated with lower resilience scores.
Our analysis further found a significant negative correlation between BO and resilience (r =-0.62, p =0.00, r2 =0.38) and between BO and CS (r =-0.18, p =0.03, r2 =0.03). BO accounted for 38% of the variance in resilience and 3% of the variance in CS. These results suggest that higher burnout scores were strongly associated with lower resilience scores and higher burnout scores were mildly associated with lower compassion satisfaction scores. A significant positive correlation was found between resilience and CS (r =0.42, p =0.00, r2 =0.18), with higher resilience scores being associated with high scores indicative of compassion satisfaction. Resilience accounted for 18% of the variance in CS.
Mediation Analysis
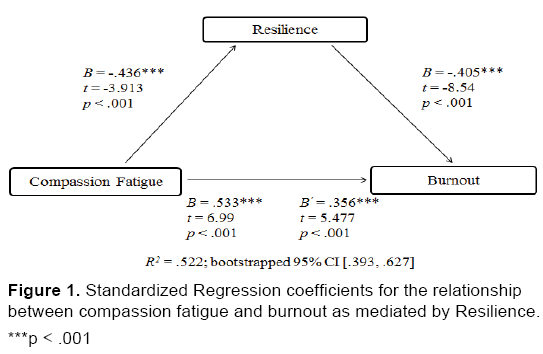
The relationship between CF and BO was mediated by resilience. As Figure 1 illustrates, CF (r =-0.31, p <0.001) and BO (r =-0.62, p <0.001) both correlated with resilience, but only moderately mediated the relationship between CF and BO. In other words, 33% of the total effect of CF on BO goes through resilience. Resilience accounted for about 52% of the variance in BO (R2 =0.522, 95% CI [0.393, 0.626]); however, the mediation effect size (κ2 =0.191; bootstrapping 95% CI [0.092, 0.274]) was medium to large. Hence, our results showed that participants who experience a high level of compassion fatigue, he or she is then more likely to report greater burnout. This relationship can be partially explained by detailing the involvement of resilience. In essence, those who reported lower levels of compassion fatigue reported higher levels of resilience and, in turn, resilient participants reported lower levels of burnout.
Discussion
Our study investigated the relationship between CF, burnout, CS and resilience among a sample of disaster behavioral health and emergency preparedness response professionals in Michigan. The results of this study were consistent with previous research as well as provided further insight about resilience as a mediating variable.
The study examined the incidence of CF, burnout, CS and resilience among its participants. Although participant-mean scores on the CF and burnout subscales were roughly the same as the suggested ProQOL standardized score means, the distribution of these scores among participants begs to tell a more concerning story. Approximately 72% participants had cut scores that were above the 75th percentile which is considered a significant risk indicator for CF. This would suggest that almost two thirds of the disaster behavioral health and emergency response participants may be at risk for developing depression and other problems characteristic of caring for those who have experienced traumatizing events. It has been strongly advocated that professionals exposed to trauma indirectly through their work are more susceptible to elevated symptoms or consequences unique to the disaster behavioral health and emergency preparedness occupational groups, compared to other occupations (Beck, 2011). Newell and MacNeil (2011) would suggest that the significant elevation of CF found among the various professions represented in our study was expected. In essence, working in the field of disaster behavioral health and emergency preparedness response has the inherent potential risk of developing CF.
Prevalence risk for burnout was less concerning, with approximately 20% of participants scoring above the 75th percentile cut score. In other words, the number of participants that may be exhibiting problems associated with burnout, such as having feelings of hopelessness, exhaustion, or believing that one was not performing his or her job effectively was small. The incidences of CF and burnout found in our study were higher than rates reported in other studies (Wee & Myers, 2002; Sprang et al., 2007; Craig & Sprang, 2010). Notably, these studies were conducted primarily on mental health providers compared to our study which included a diversity of disciplines as a combined group that were involved with various aspects of disaster behavioral health and emergency preparedness response. Empirical literature is void of consistent measures of CF and burnout that involve a diversity of trauma response providers as a combined group. These findings underscore the importance of continuing ongoing research to establish incidence rates of CF and burnout that resemble this study’s diverse sample population as a specific trauma-related occupations group.
In regards to CS, less than half of participants had subscale scores indicative of deriving good satisfaction from their job as well as from the act of helping those in their care. This finding was similar to research conducted by Sprang et al. (2007) who found mean CS scores ranging from 36.13 for licensed medical doctors to 40.43 for subjects with licensure as a Clinical Alcohol and Drug Counselor, as well as with Craig and Sprang (2010) who reported that 46% of clinicians that participated in their study had high levels of CS. As mentioned earlier, literature is very sparse regarding empirical support of CS prevalence rates among disaster behavioral health and emergency preparedness response providers as a specific trauma-related occupations group that resemble this study’s sample population. Further research is needed in this area of disaster behavioral health.
The majority of participants had resilience score that were reflective of possessing adequate skills for adapting to change and managing adversity. Unfortunately, there were no empirical studies that may have shed light on how our results compare with other specific trauma-related occupations group populations.
When our study examined the relationship between CF and burnout, a significant strong positive correlation was found between these two variables. As stated earlier, CF accounted for 32% of the variation in burnout subscale scores, which is considered a strong relationship. This finding was consistent with previous research regarding CF and burnout (Cieslak et al., 2013) which would strongly suggest that individuals working in occupations that expose them indirectly to trauma may not only develop CF, but are also more likely to acquire burnout symptoms. A major implication of this finding is that it continues affirm that burnout is a gradual and pervasive process (Figley, 1995) that tends to emerge as a more negative component of cumulative CF (Stamm, 2010). More research is needed to establish a causal link between CF and burnout, beyond the plethora of correlational and regressional analysis literature.
An unexpected finding was that no significant association was found between CF and CS. This is contrary to Slocum-Gori at al. (2013) and Simon, Pryce, Roff and Klemmack (2005) who found a significant inverse relationship between CF and CS among hospice care palliative workers and oncology social workers, respectively. Ray, Wong, White and Heaslip (2013) also determined a significant inverse relationship between these two variables among frontline mental health care professionals. A plausible explanation for our study’s finding centers on the type of sample population used. The present study had a diversity of professions within the broad spectrum of the disaster behavioral health and emergency preparedness response field, whereas the aforementioned studies used specific occupational samples (i.e., hospice care workers, oncology social workers, and mental health care professionals). In fact, this was one of the major limitations of this study. However, using the data that was collected in our study to examine specific occupations reported in this study in the future may provide a relational significance similar to what has been found in the trauma literature.
In regards to CS and burnout, a significant negative relationship was observed between these two variables. Higher CS was associated with lower amounts of burnout. Similar findings were noted by Simon et al. (2005) among oncology social workers and by Slocum- Gori et al. (2013) among hospice palliative care providers. Although this finding was significant in our study, CS only moderately accounted for 3% of the variation in burnout subscale scores. In other words, CS’s association with levels of burnout among our sample is relatively minor; suggesting that another variable is more likely a stronger contributor to the variability found among burnout scores. We suspected that resilience was the stronger contributing variable which was confirmed through mediation analysis. An important implication from this finding is the development of or enhancement of strategies that foster stronger CS behaviors in conjunction with the stronger contributor variable.
One of the more promising results of the present study involved finding significant inverse associations between CF and resilience and between burnout and resilience. These results would indicate that higher levels of resilience is strongly associated with lower amounts of burnout and CF. In fact, this relationship was stronger for burnout than CF (38% of the variance versus 9% of the variance). Previous research has found similar results (David, 2012; Cooke, Doust, & Steele, 2013). A major implication of these findings is the importance of enhancing resilience-focused building strategies among disaster behavioral health and emergency preparedness response workers to help mitigate and reduce the harmful effects of CF and burnout.
We then examined how CF is affected by resilience in a manner that effects burnout through mediation analysis. The intent of conducting a mediation analysis helps the researcher to examine the degree of overlapping variance among three variables that allows a causal statement (Jose, 2013). The results of our analysis indicated that the relationship of CF to burnout was moderately mediated by resilience. In other words, resilience seems to explain a significant part of the relationship between CF and burnout. As mentioned earlier, participants who reported lower levels of CF reported higher levels of resilience and, in turn, resilient participants reported lower levels of burnout. Our study seems to be the first to link resilience as an important mediator between CF and burnout among disaster behavioral health and emergency preparedness response providers. This finding also affirms that resilience is the stronger contributing variable to the observed variability among burnout scores compared to CS. A major implication of this finding is the importance of developing and/or enhancing resilience-building strategies (“best practices”) that are proven to help reduce the negative impact of CF and burnout among disaster behavioral health and emergency preparedness response providers.
There were several limitations with our research. The focus of this study was on those participants who were a part of an organization or team that were involved with being deployed or responding to traumatic/critical incident type events. The main limitation was that our participant sample group used for analysis was comprised of several occupational disciplines relevant to the field of disaster behavioral health and emergency preparedness response. Most studies have focused on a single discipline (i.e., nurses, hospice care providers, social workers, therapists, etc.) in the trauma field. Thus, our results were limited in generalizability. Another limitation was that our results were based on data collected from a convenience sample of participants who attended a disaster behavioral health conference. There was no cross-sectional design method conducted among the participants who attended the conference to ensure a sample representative of key disaster behavioral health and emergency preparedness response occupations (i.e., mental health, nursing, first responders, emergency management, public health, etc.). Thus, our prevalence data in regards to compassion fatigue, burnout, compassion satisfaction, and resilience was not truly representative of those occupations within the State of Michigan. A final limitation involved the imputing of missing values on the ProQOL subscales and the RS-14 from their means in order to provide a complete set of data for analysis. Although this technique can assist researchers to avoid the pitfalls of list wise deletion of cases with missing values (i.e., provide more representativeness of the results), there is still the possibility of bias as it relates to missing completely at random data (see Schafer & Graham, 2002).
Implications for Practice
A primary goal of providing disaster behavioral health and emergency preparedness response services is to mitigate disasterrelated stress reactions and to assist individuals and communities affected by a traumatic event to return as soon as possible to their predisaster level of functioning (Myers & Wee, 2005). Based on the overall results of our study, it is apparent that resilience plays a key role in the well-being of those working in the disaster behavioral health and emergency preparedness response field. As stated earlier, resilience is comprised of multiple factors and pathways that may help a person to adapt to change and manage adverse life experiences. Therefore, our study has implications for practice in the disaster behavioral health and emergency preparedness response field.
The data from our study strongly supports the need for disaster behavioral health and emergency preparedness response agencies, organizations and crisis response teams to implement a “best practices” resiliency program for their workers who may be deployed or respond to assist those affected by traumatic events in order to help them reduce the harmful effects of indirect trauma exposure (Craig & Sprang, 2010). Research literature has provided several key components that should be adopted within the structure of such a program and include: developing and enhancing protective factors and rebound capabilities which promote self-efficacy and self-confidence (Ortlepp & Friedman, 2002; Kaminsky et al., 2007; Nucifora, 2007); nurturing self-care strategies (Inbar & Ganor, 2003; Killian, 2008; Harrison & Westwood, 2009, Lambert 2013; David & Naturale 2012); advocating personal and family emergency preparedness (Myers & Wee, 2005); providing access to supervision and support (Rich, 1997; Myers & Wee, 2005); incorporating a selection process for participation in disaster response work and providing an orientation to the disaster assignment prior to deployment (Myers & Wee, 2005); arranging for post disaster closure activities, debriefing of responders, recognition of responder accomplishments and follow-up support (Myers & Wee, 2005; Potter, Stevens & LaBerteaux, 2006); and providing access to specialized training and opportunities for skill development (Ortlepp & Friedman, 2002; Palm et al., 2004; Myers & Wee, 2005; Sprang et al., 2007; Craig & Sprang, 2010).
Based on the components mentioned in the previous paragraph, there are several resiliency models reviewed in the trauma literature that agencies, organizations and crisis response teams can adopt. Yassen’s (1995) Ecological Model and the Johns Hopkins Tripartite Model of Resistance, Reslience, and Recovery (Kaminsky et al., 2007; Nucifora, 2007) provide an excellent framework for developing balance and establishing a common evidence-based resiliency construct in which to operate. The CODE-C Disaster Mental Health Service Model (Myers, 1992; Myers & Wee, 2005) and the Critical Incident Stress Management (CISM) system (Everly & Mitchell, 1999; Everly & Langlieb, 2003; Everly & Mitchell, 2008) both offer a good strategic approach to help build resiliency. Both approaches have been widely used and incorporate a comprehensive, integrated, multi-component systems approach to deliver crisis intervention and disaster mental health services to those affected directly and indirectly by traumatic events. A major implication and challenge for practice would be incorporating all of these models into one overarching evidence-based “best practices” model. Further research is needed on such a resiliency model to establish its efficacy and feasibility once it has been developed and piloted.
References
- Ahern, R.N., Kiehl, M.E., Sole, L.M., & Byers J. (2006).A review of instruments measuring resilience.Issues in Comprehensive Pediatric Nursing, 29, 103-125
- Baird, K., &Kracen, A.C. (2006). Vicarious traumatization and secondary traumatic stress: A research synthesis. Counselling Psychology Quarterly, 19(2), 181-188
- Beck, C.T. (2011). Secondary traumatic stress in nurses: A systematic review. Archives of Psychiatric Nursing, 25, 1-10
- Bonanno, G.A. (2005). Resilience in the face of potential trauma.Current Directions in Psychological Science, 14(3), 135-138
- Bonanno, G.A. (2008). Loss, trauma, and human resilience: Have we underestimated the human capacity to thrive after extremely aversive events? Psychological Trauma: Theory, Research, Practice, and Policy, S(1), 101-113
- Bonanno, G.A., Galea, S., Buccuarelli, A., &Vlahov, D. (2007). What predicts psychological resilience after disaster? The role of demographics, resources, and life stress.Journal of Consulting and Clinical Psychology, 75(5), 671-682
- Bride, B.E., Robinson, M.M., Yegidis, B., &Figley, C.R. (2004).Development and validation of the Secondary Traumatic Stress Scale, Research on Social Work Practice, 14, 27-35
- Cieslak, R., Shoji, K., Douglas, A., Melville, E.,Luszczynska, A., &Benight, C.C. (2013).A meta-analysis of the relationship between job burnout and secondary traumatic stress among workers with indirect exposure to trauma, Psychological Services, 11(1), 75-86
- Craig, C.D., & Sprang, G. (2010). Compassion satisfaction, compassion fatigue, and burnout in a national sample of trauma treatment therapists.Anxiety, Stress, & Coping, 23(3), 319-339
- Cooke, G., Doust, J.A., & Steele, M.C. (2013).A survey of resilience, burnout, and tolerance of uncertainty in Australian general practice registrars.BMC Medical Education, 13(2), 1-6
- David, D. (2012). Resilience as a protective factor against compassion fatigue in trauma therapist (unpublished doctoral dissertation). Walden University: Minneapolis, MN
- David, J. &Naturale, A. (2012).Self-care for disaster behavioral health responders.Substance Abuse and Mental Health Services Administration.Retrieved, June 30, 2014, from http://beta.samhsa.gov/sites/default/files/podcasts-selfcare-dbhresponders-presentation.pdf
- Everly, G.S. (2012). Fostering human resilience: A primer on resilient leadership, psychological first aid, psychological body armor and critical incident stress management (2nded.). Ellicott City, MD: Chevron Publishing
- Everly, G.S., & Langlieb, A. (2003).Evolving nature of disaster mental health.International Journal of Emergency Mental Health, 5, 113-119
- Everly, G. S., & Lating, J.M. (2013). Resilience: The final frontier. A clinical guide to the treatment of the human stress response (3rded.) (pp. 143-154). New York: Springer
- Everly, G. S., & Mitchell, J.T. (1999).Critical incident stress management (2nded.). Ellicott City, MD: Chevron
- Everly, G.S., & Mitchell, J.T. (2008).Integrative crisis intervention and disaster mental health. Ellicott City, MD: Chevron
- Everly, G.S., Welzant, V., & Jacobson, J.M. (2008). Resistance and resilience: The final frontier in traumatic stress management. International Journal of Emergency Mental Health, 10(4), 261-270
- Figley, C.R. (1995). Compassion fatigue as secondary traumatic stress disorder; an overview.In C.R. Figley (Ed.), Compassion fatigue: Coping with secondary traumatic stress disorder in those who treat the traumatized (pp. 1-20). New York: Routledge
- Harrison, R.L., & Westwood, M.J. (2009).Preventing vicarious traumatization of mental health therapists: Identifying protective practices.Psychotherapy Theory, Research, Practice, Training, 46(2), 203-219
- Inbar, J., &Ganor, M. (2003). Trauma and compassion fatigue: Helping the helpers. Journal of Jewish Communal Service, Winter/Spring, 109-111
- Joinson, C. (1992). Coping with compassion fatigue.Nursing, 22(4), 118-121
- Jose, P.E. (2013). Doing statistical mediation & moderation. New York: The Guilford Press
- Kaminsky, M.J., McCabe, O.L., Langlieb, A., & Everly, G.S. (2007). An evidence-informed model of human resistance, resilience, & recovery: The Johns Hopkins’ outcomes-driven paradigm for disaster mental health services. Brief Therapy and Crisis Intervention, 7, 1-11
- Kelley, K. & Lai, K. (2012).MBESS (Version 3.3.3 or higher) [Computer software and manual]. Retrieved from http://www.cran.r-project.org/
- Killian, K.D. (2008). Helping till it hurts? A multimethod study of compassion fatigue, burnout, and self-care in clinicians working with trauma survivors, Traumatology, 14(2), 32-44
- Linley, P.A., & Joseph, S. (2007). Therapy work and therapists’ positive and negative well-being.Journal of Social and Clinical Psychology, 66, 319-335
- Lambert, S.F.(2013).Resilience of professional counselors following hurricanes Katrina and Rita .Journal of Counseling and Development.doi:http://dx.doi.org/10.1002/j.1556-6676.2013.00094.x
- Luthar, S.S., Cicchetti, D., & Becker, B. (2000). The construct of resilience: A critical evaluation and guidelines for future work. Child Development, 71(3), 543-562
- MacKinnon, D.P., Fairchild, A.J., & Fritz, M.S. (2007).Mediation analysis.Annual Review of Psychology, 58, 593-614
- MacKinnon, D.P., Cheong, J., &Pirlott, A.G. (2012).Statistical mediation analysis.In H. Cooper (Ed.), APA Handbook of Research Methods in Psychology (Vol. 2 Research Designs, pp. 313-331)
- Mancini, A.D., &Bonanno, G.A. (2009). Predictors and parameters of resilience to loss: Toward an individual differences model. Journal of Personality, 77(6), 1805-1831
- Maslach, C., & Jackson, S.E. (1984).Burnout in organizational settings.In S. Oskamp (Ed.), Applied Social Psychology Annual (Vol. 5, pp. 133-153). Beverly Hills, CA: Sage
- Maslach, C., Schaufeli, W.B., &Leiter, M.P. (2001).Job burnout.Annual Review of Psychology, 52, 397-422
- McCann, I.L., & Pearlman, L.A. (1990). Vicarious traumatization: A contextual model for understanding the effects of trauma on helpers. Journal of Traumatic Stress, 3, 131-149
- Motta, R.W. (2008). Secondary trauma.International Journal of Emergency Mental Health, 10(4), 291-298
- Myers, D. (1992). Hurricane Andrew disaster field office stress management program: After action report. Miami, FL: Federal Emergency Management Agency
- Myers, D., & Wee, D.F. (2005). Disaster mental health services. New York: Routledge
- Newell, J.M., &MacNeil, G.A. (2011).A comparative analysis of burnout and professional quality of life in clinical mental health providers and health care administrators.Journal of Workplace Behavioral Health, 26, 25-43
- Nucifora, F., Langlieb, A., Siegal, E., Everly, G.S., &Kaminsky, M.J. (2007).Building resistance, resilience, and recovery in the wake of school and workplace violence.Disaster Medicine and Public Health Preparedness, 1(Supplement 1), 33-37
- Ortlepp, K., & Friedman, M. (2002). Prevalence and correlates of secondary traumatic stress in the workplace lay trauma counselors. Journal of Traumatic Stress, 15(3), 213-222
- Palm, K.M., Polusny, M.A., &Follette, V.M. (2004). Vicarious traumatization: Potential hazards and interventions for disaster and trauma workers. Prehospital and Disaster Medicine, 19(1), 73-78
- Pearlman, L.A., &Saakvitne, K.W. (1995).Treating therapist with vicarious traumatization and secondary traumatic disorders.In C.R. Figley (Ed.), Compassion fatigue: Coping with secondary traumatic stress disorder in those who treat the traumatized (pp. 150-177). New York, NY: Routledge
- Pietrantoni, L. &Prati, G. (2008).Resilience among first responders.African Health Sciences, 8, S14-S20
- Pines, A.M., & Aronson, E. (1988).Career burnout: Causes and cures. New York: Free Press
- Potter, D. Stevens, J.A., &LaBerteaux, P. (2006). Practical concepts and training exercises for crisis intervention teams: Including role-plays and interactive games (2nded.). Ellicott City, MD: Chevron
- Preacher, K.J., & Kelley, K. (2011). Effect size measures for mediation models: Quantitative strategies for communicating indirect effects. Psychological Methods, 16(2), 93-115
- Ray, S.L., Wong, C., White, D., &Heaslip, K. (2013). Compassion satisfaction, compassion fatigue, work life conditions, and burnout among frontline mental health care professionals. Traumatology, 19(4), 255-267
- Rich, K.D. (1997). Vicarious traumatization: A preliminary study. In S. B. Edmunds (Ed.), Impact: Working with sexual abusers (pp. 75-88). Brandon, VT: Safer Society Press
- Schafer, J.L., & Graham, J.W. (2002).Missing data: Our view of the state of the art.Psychological Methods, 7(2), 147-177
- Simon, C.E., Pryce, J.G., Roff, L.L., &Klemmack, D. (2005). Secondary traumatic stress and oncology social work: Protecting compassion from fatigue and compromising the worker’s worldview. Journal of Psychosocial Oncology, 23(4), 1-14
- Slocum-Gori, S., Hemsworth, D., Chan, W.W., Carson, A., &Kazanjian, A. (2013). Understanding compassion satisfaction, compassion fatigue and burnout: A survey of the hospice palliative care workforce. Palliative Medicine, 27(2), 172-178
- Sprang, G., Clark, J.J., & Whitt-Woosley, A. (2007). Compassion fatigue, compassion satisfaction, and burnout: Factors impacting a professional’s quality of life. Journal of Loss and Trauma, 12, 259-280
- Southwick, S.M., &Charney, D.S. (2012).Resilience: The science of mastering life’s greatest challenges. New York: Cambridge University Press
- Stamm, B.H. (2002). Measuring compassion satisfaction as well as fatigue: Developmental history of the compassion satisfaction and fatigue test. In C. R. Figley (Ed.), Treating compassion fatigue. New York, New York: Brunner-Routledge
- Stamm, B.H. (2010). The concise ProQOL manual, 2nd Ed. Pocatello, ID: ProQOL.org
- Thomas, J.T. (2012). Does personal distress mediate the effects of Mindfulness on professional quality of life? Advances in Social Work, 13(3), 561-585
- Tosone, C., Bettmann, J.E., Minami, T., &Jasperson, R.A. (2010). New York City social workers after 9/11: Their attachment, resiliency, and compassion fatigue. International Journal of Emergency Mental Health, 12(2), 103-116
- Wagnild, G.M. (2010). The resilience scale user’s guide.Worden, Montana; Resilience Center
- Wagnild, G., & Young, H. (1993). Development and psychometric evaluation of the resilience scale. Journal of Nursing Measurement, 1(2), 165-178
- Wee, D.F., & Myers, D. (2002). Stress response of mental health workers following disaster: The Oklahoma City bombing. In C.F. Figley (Ed.), Treating compassion fatigue. Psychosocial stress series, no. 24., (pp. 57-83)
- Yaseen, J. (1995). Preventing secondary traumatic stress disorder.In C.R. Figley (Ed.), Compassion fatigue: Coping with secondary traumatic stress disorder in those who treat the traumatized (pp. 150-177). New York, NY: Routledge.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 25323
- [From(publication date):
specialissue-2015 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 19599
- PDF downloads : 5724