Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
The Erroneous Diagnosis of Prune Belly Syndrome in a Case of Posterior Urethral Valve
| Hong R*, Whalen M, Casale P and Ruzal-Shapiro C | |
| Department of Radiology, Children’s Hospital of New York, New York Presbyterian–Columbia 3959 Broadway, New York, NY, USA | |
| Corresponding Author : | Richard Hong Department of Radiology, Children’s Hospital of New York New York Presbyterian–Columbia 3959 Broadway, New York, NY, USA Tel: (212) 305–9665 E-mail: reh27@columbia.edu |
| Received March 08, 2013; Accepted June 25, 2013; Published June 28, 2013 | |
| Citation: Hong R, Whalen M, Casale P, Ruzal-Shapiro C (2013) The Erroneous Diagnosis of Prune Belly Syndrome in a Case of Posterior Urethral Valve. OMICS J Radiology 2:132 doi: 10.4172/2167-7964.1000132 | |
| Copyright: © 2013 Hong R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
We report a diagnostically challenging case of a full term baby boy with a prenatal diagnosis of a posterior urethral valve. While postnatal imaging was felt to be more consistent with Prune Belly Syndrome, cystoscopy confirmed the diagnosis of the valve. A review of the literature has shown an interesting similarity in imaging and physical exam findings and perhaps an explanation for the misdiagnosis.
| Keywords |
| Neuroblastoma; Thoracic tumors; MRI; CT; MIBG; Adult; Mediastinum; Metastasis; Lymphoma |
| Introduction |
| Posterior urethral valve is the most common congenital cause of bilateral urinary obstruction [1]. Distinction from other congenital abnormalities of the genitourinary tract, such as Prune Belly Syndrome, is important as the clinical management differs [1,2]. Our case is an example of an atypical presentation of posterior urethral valve that was confused with Prune Belly Syndrome based on imaging findings. |
| Case Report |
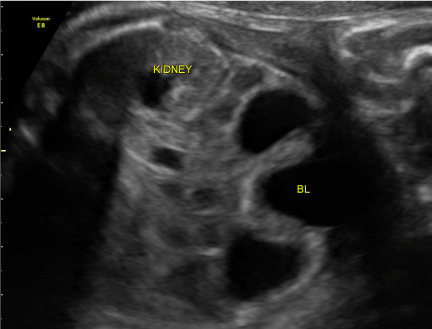
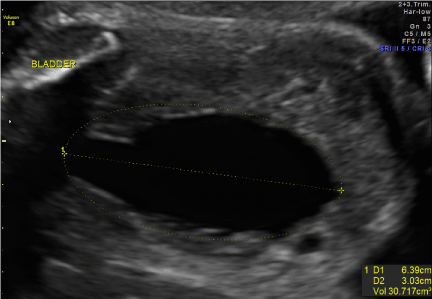
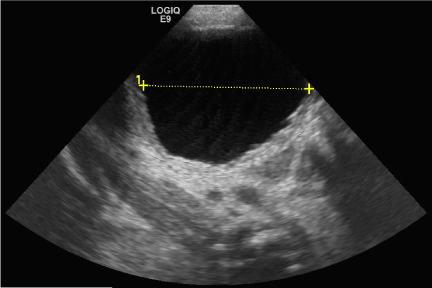
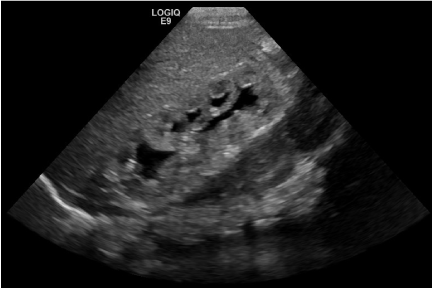
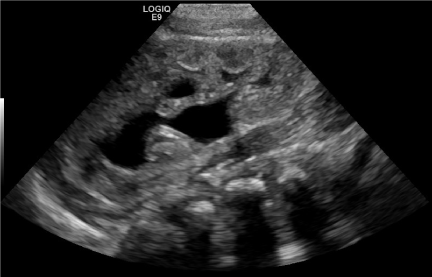
| Our patient was born to a 26 y/o G1P0. Prenatal anatomic survey performed at 18 weeks gestation was normal. At 19 2/7 weeks, US revealed bilateral hydronephrosis with an enlarged ‘keyhole’ bladder (Figures 1 and 2). Two large round sonolucent structures seen adjacent to the bladder were felt to be either urinomas or enlarged ureters (Figure 1). Amniotic fluid volume at this time was normal. Subsequent ultrasound examinations were similar until 36 weeks when oligohydramnios was first seen; with an AFI of 3.2 cm. Birth was at 36 5/7 weeks. Apgars were 8/8 and patient voided in the delivery room. Physical exam was remarkable for abdominal distension and undescended testes. Abdominal wall musculature was intact. A foley catheter was placed. |
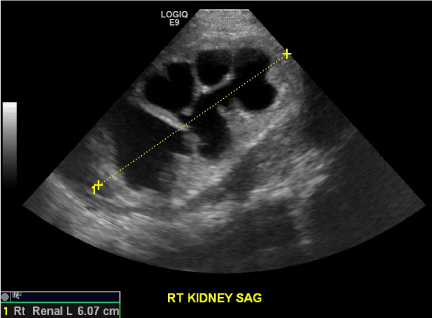
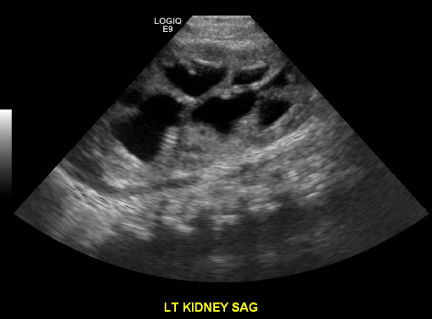
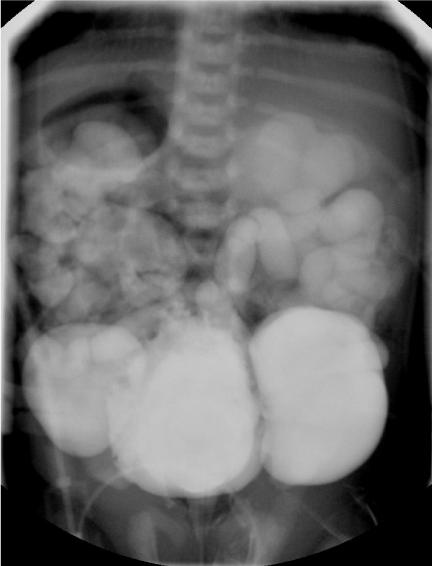
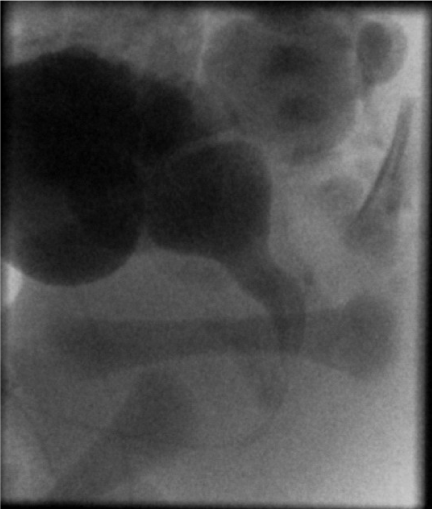
| Ultrasound performed on the first day of life demonstrated bilateral hydronephrosis with a distended mildly trabeculated bladder (Figures 3-5). Both testicles were found in the inguinal canals. VCUG performed on day of life one revealed massive bilateral vesicoureteral reflux with intrarenal reflux. There were bilateral giant bladder diverticula, corresponding to the sonolucent structures adjacent to the bladder felt to be urinomas or enlarged ureters on prenatal examination (Figure 6). The posterior urethra was only mildly dilated with a gaping patulous bladder neck (Figure 7). There was also filling of a normal appearing prostatic utricle (Figure 7). |
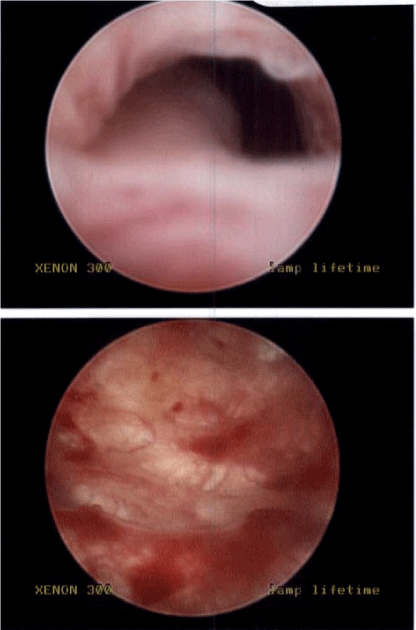
| Removal of the foley catheter was attempted on day of life three, however, the patient was unable to void. The patient was brought to the operating room the same day for cystoscopy that revealed the presence of a posterior urethral valve, a markedly trabeculated bladder, and large bilateral bladder diverticula (Figure 8). Valve fulguration and circumcision were performed. |
| Ultrasound on POD # 2 revealed improved bilateral hydronephrosis, bladder diverticula and a trabeculated bladder (Figures 9 and 10). |
| Discussion |
| Our case is an example of an atypical presentation of a posterior urethral valve that was misinterpreted as Prune Belly Syndrome after postnatal imaging. A review of the literature has shown that the imaging characteristics and clinical findings seen in Prune Belly Syndrome and posterior urethral valves often overlap [2]. As such, atypical presentations make for a confusing diagnostic picture. |
| On prenatal sonography, some key elements of Prune Belly Syndrome include a large thin walled bladder and dilation of the entire urethra, neither of which were seen in our case [2,3]. The hydronephrosis and hydroureter, which was seen in our case, is common to both entities. Posterior urethral valves will manifest signs of urinary tract obstruction on prenatal imaging such as a dilated thick walled bladder and dilated posterior urethra i.e. the ‘keyhole sign’ [4,5]. |
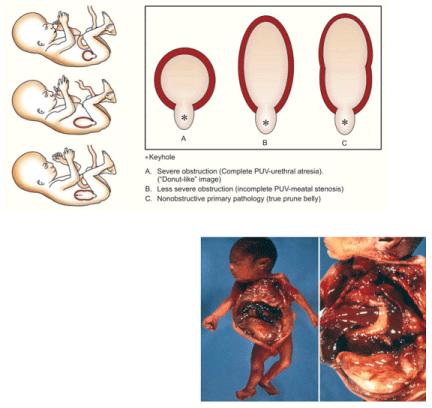
| The ‘keyhole sign’ depicting a dilated bladder and posterior urethra has been described as a classic prenatal finding in the presence of an obstructing posterior urethral valve. It was this notion that informed the prenatal diagnosis made in our case. A recent review of 42 fetuses suspected to have posterior urethral valves on prenatal examination performed by Bernardes et al. found that this sign while highly sensitive, holds very low specificity. They report that the best diagnostic indicators were bladder dilation and bladder wall thickening [6]. Furthermore, in a review by Bonilla-Musoles et al. a distinction is made between the particular configuration of the keyhole as a distinguishing feature between posterior urethral valve and Prune Belly Syndrome [4] (Figure 11). Although this notion was unknown to us during the work-up of our case, in retrospective review of the ‘keyhole’ sign seen in our case, its configuration would point more towards a diagnosis of Prune Belly Syndrome. |
| A distinguishing feature of Prune Belly Syndrome is a gaping patulous bladder neck as opposed to the hypertrophied closed bladder neck typically seen in posterior urethral valves [7,8]. Posterior urethral valves demonstrate bladder trabeculation and a dilated posterior urethra [1]. The findings of a wide bladder neck and only mildly dilated posterior urethra seen on our voiding cystourethrogram, were felt to be more consistent with Prune Belly Syndrome than posterior urethral valves. Visualization of a normal caliber prostatic utricle, as in our case, is felt to be more consistent with Prune Belly Syndrome than the dilated prostatic utricle more often seen in posterior urethral valves [4,9]. The presence of bladder diverticula was not found to be a distinguishing feature by Blane et al. which found them common to both entities [10]. |
| There are several hypotheses regarding the etiology of Prune Belly Syndrome. One of the leading theories includes urethral obstruction. It seems reasonable then that an obstructing posterior urethral valve would present with similar imaging and physical exam findings as Prune Belly Syndrome. Underlying posterior urethral valves have been found in cases of Prune Belly Syndrome [11]. Furthermore, a review of 192 patients with posterior urethral valves performed by Heikkila et al. found that 16% had cryptorchidism. This incidence was 16 fold higher than that in the comparative normal population. They also found that patients with cryptorchidism tended to have a more severe form of PUV [12]. |
| The overlap in the diagnoses has also been shown at the histological level. Workman et al. report that fetuses with posterior urethral valves generally showed increased-detrusor muscle thickness and those with Prune Belly Syndrome generally showed thin bladders with increased ratio of connective tissue. Interestingly, however, three of the Prune Belly cases demonstrated bladder histology more consistent with that seen in posterior urethral valves [13]. |
| Weber et al report an interesting case of a family with five male descendants with posterior urethral valves. Two of these cases demonstrate the full spectrum of Prune Belly Syndrome. This case underlines the hypothesis that Prune Belly Syndrome may in some cases be a secondary manifestation of posterior urethral valve [14]. |
| In our review of the literature, we have only found one other report of a case of posterior urethral valve being mistakenly diagnosed as Prune Belly Syndrome [15]. In this particular case, the diagnosis was made based on the presence of cryptorchidism and abnormal abdominal musculature, rather than any imaging work-up. It was the finding of a markedly trabeculated bladder and a dilated posterior urethra that finally led to the correct diagnosis. Given the considerable overlap in imaging and physical exam findings it is reasonable to assume that this diagnostic dilemma is not uncommon. We hope our case serves to shed some light on these confusing evaluations. |
References |
|
--
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
 |
 |
 |
 |
| Figure 5 | Figure 6 | Figure 7 | Figure 8 |
 |
 |
 |
|
| Figure 9 | Figure 10 | Figure 11 |
Post your comment
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 16269
- [From(publication date):
September-2013 - Aug 20, 2025] - Breakdown by view type
- HTML page views : 11606
- PDF downloads : 4663
