Research Article Open Access
The Normal Acromioclavicular Joint: An In Vivo Multidetector CT (MDCT) Morphometric and Biometric Cross Sectional Feasibility Study
Nouh MR1*, Doweidar AA2, El-Aziz Amr HA2, El-Refae DI3, Ashry MH4 and Al-Kandri SR21Department of Radiology, Alexandria University, Alexandria, Egypt
2Department of Radiology, Al-Razi Hospital, Sulibikhate 13001, Kuwait
3Department of Radiology, Al-Farwaniya Hospital, Alardhiah, 18373, Kuwait
4Department of Public Health and Community Medicine, Alexandria University, Alexandria, Egypt
- *Corresponding Author:
- Mohamed Ragab Nouh
Department of Radiology and Clinical Imaging
Faculty of Medicine
Alexandria University
Alexandria 21599, Egypt
Tel: +201116590365
Fax: +2034869754
E-mail: mragab73@yahoo.com
Received Date: March 27, 2017; Accepted Date: April 17, 2017; Published Date: April 24, 2017
Citation: Nouh MR, Doweidar AA, El-Aziz Amr HA, El-Refae DI, Ashry MH, et al. (2017) The Normal Acromioclavicular Joint: An In Vivo Multidetector CT (MDCT) Morphometric and Biometric Cross Sectional Feasibility Study. OMICS J Radiol 6: 260. doi: 10.4172/2167-7964.1000260
Copyright: © 2017 Nouh MR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Radiology
Abstract
Aim: To determine the morphometric and biometric measurements of the normal Acromioclavicular (AC) joint on MDCT. Materials and methods: 33 volunteers (32 males and 1 female) and 17 patients (16 Male and 1 female) with clinical and radiographic evidences of AC separations were enrolled in this study. Two observers, blinded to the clinical data, assessed multiple AC joint morphologic and biometric variables. These were statistically attested for inter-observer variability and differences between the volunteers and diseased subjects. Results: The anterior and posterior axial AC joint distances were the only statistically significant variables measuring 0.59 ± 0.27 cm and 0.26 ± 0.11 cm in volunteers, and 0.88 ± 0.3 cm and 0.49 ± 0.39 cm in the AC separation group. The remaining attested variables were not statistically significant. Conclusion: On MDCT, the normal AC joint articular facet morphology shows great variability. The axial anterior and posterior AC joint distances measures 0.59 ± 0.27 and 0.26 ± 0.11 cm; respectively in supine neutral resting position.
Keywords
Normal; Anatomy; Acromioclavicular (AC); Joint; Acromioclavicular
Core Tip of the Research
�?� MDCT showed variability of AC joint articular facet morphology.
�?� Axial MDCT anterior and posterior AC joint distances are sensitive objective variables to separate normal AC Joints.
�?� MDCT can depict the capsular and peri-capsular AC joint ligaments.
Introduction
Acromioclavicular (AC) joint abnormalities are common and include most frequently traumatic separations in young athletes to degenerative disease in elderly [1,2]. Variations in the appearance of AC joint are frequent in the setting of trauma and in uncooperative patients. Likewise, the infrequency of the examination and inconsistent standardized positions for the axial imaging do [3]. The gross [4], radiographic [5], ultrasound [6,7] and MR [8,9] anatomic descriptions of the AC joint have been described. However, in the setting of trauma, the aforementioned factors confound the utility of these imaging tools in assessing the acromioclavicular axial relationship.
Multi-Detector Computed Tomography (MDCT), with its robust volumetric high resolution images and shortened scan times, proved useful in workup of poly-trauma patients including skeletal trauma [10,11]. Then, knowledge of the AC joint measurements and morphologic variations on MDCT would help to recognize patients with occult AC instability, plane arthroscopic procedures and reconstructive procedures of the AC joint biomechanics.
To our knowledge, there is no available morphometric and/or biometric CT data exist for the acromioclavicular joint in English literature. We sought to determine the morphometric and biometric measurements of the normal AC joints on MDCT.
Materials and Methods
Study design and research ethics
Our local institutional review board approved this prospective cohort study between September 2012 and December 2013. The current study included two cohorts: a group of volunteers and another group of patients with clinically suspected AC separations. All subjects participating in this study signed an institutionally approved informed consent.
Study population inclusion and exclusion criteria
Volunteers: Thirty-three volunteers (32 males and 1 female) were recruited in the current study. All volunteers achieved the following criteria [a] age above 18, [b] No previous history of shoulder girdle problems and/or complaints, [c] No history of connective tissue disease, and [d] No deforming musculoskeletal or neurologic disorders involving the shoulder girdle.
Patients with AC dislocation: This cohort included seventeen patients (16 males and 1 female) composed of two groups: [a] A group of five patients referred to our radiology department, from shoulder outpatients’ clinic with clinical diagnosis of AC dislocation and radiographic evidence of separations, for pre-operative imaging work-up of their AC joint. [b] Another group of twelve patients whom were refereed for MRI evaluation of their shoulders due to chronic shoulder-related complaints. These patients showed AC joint effusion and/or edema around AC joint suspecting its sprain [9] with no other remarkable findings of their shoulders. This latter group was re-evaluated clinically by our shoulder outpatients’ clinic consultants and underwent radiographic evaluation of their affected AC joints to confirm AC separation. All MRI studies were interpreted by one of the two MSK-trained radiologists (MRN and AAD) sharing in the study.
Exclusion criteria: Patients with a primary clinical diagnosis of shoulder instability, associated shoulder girdle fractures, acromioclavicular joint degeneration, and history of connective tissue diseases, os acromiale and previous AC joint surgery were excluded from the study.
CT examinations
All studies were conducted on a 16-slice MDCT scanner (GE Light- Speed, GE Healthcare, and Milwaukee, WI, USA). All patients were supine with the upper arm in neutral position close to the body, with slight forward flexion and medial rotation. A helical volumetric acquisition of the examined shoulder was carried out starting cranially above the AC joint down to the scapular mid-body; in both bone and soft tissue settings. The parameters for image acquisition were as follows: Slice thickness of 1.25 mm, 0.625 mm interval, pitch 0.938:1, 120 kV, 200 mA and total exposure time of 11 s, FOV 28 cm, imaging matrix 512 × 512 pixels.
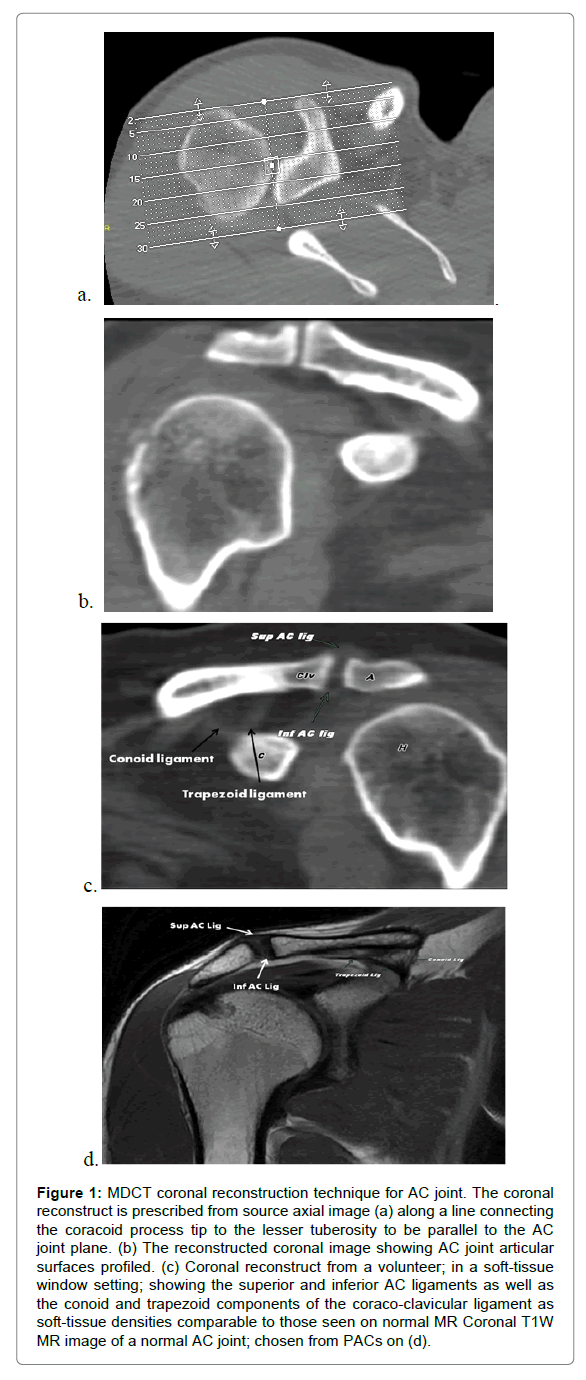
Axial source images, from both bony and soft-tissue algorithm, were reconstructed in coronal oblique plane, centered on the acromioclavicular joint (Figure 1) in a manner similar to previously described in MR literature [8,9]. All source and reconstructed images of all studies were pushed to a digital workstation (Centricity PACS IW 3.7.3.9 SP1, GE healthcare, Milwaukee, WI, USA) for interpretation.
Figure 1: MDCT coronal reconstruction technique for AC joint. The coronal reconstruct is prescribed from source axial image (a) along a line connecting the coracoid process tip to the lesser tuberosity to be parallel to the AC joint plane. (b) The reconstructed coronal image showing AC joint articular surfaces profiled. (c) Coronal reconstruct from a volunteer; in a soft-tissue window setting; showing the superior and inferior AC ligaments as well as the conoid and trapezoid components of the coraco-clavicular ligament as soft-tissue densities comparable to those seen on normal MR Coronal T1W MR image of a normal AC joint; chosen from PACs on (d).
Two readers; a general radiologist with 20 years of experience [observer-I (DIE)] and a musculoskeletal (MSK) radiologist with 18 years of experience [(observer-II (HAA)], independently evaluated all studies. The readers were blinded to both patient’s demographics and referral data. The following variables were assessed on both axial source images and coronal reconstructions.
Morphometric data
The acromioclavicular joints were evaluated for: (a) Orientation of the articular surfaces in both source axial and reconstructed coronal images as determined according to the recognized anatomic planes; (b) The visibility of relevant ligamentous structures (appearing as linear soft-tissue densities on both soft-tissue and bone window settings in proper anatomic location; and using prior MR descriptions [8,9]; including: [i] acromioclavicular [superior and inferior portions] ligaments, [ii] coracoclavicular [conoid and trapezoid portions] ligaments, and [iii] coracoacromial ligament. (c) The trapezoid and deltoid muscles were evaluated for presence or absence of injury.
All AC separation subjects were classified according to the commonly used Rockwood’s [12] classification (Table 1). The rotator cuff was not evaluated in this work.
| Rockwood Class | AC distance | CC distance | Clavicular displacement |
|---|---|---|---|
| Grade-I | Normal | Normal | None |
| Grade-II | Increased | Normal | ≤50% upward |
| Grade-III | Increased | Increased 25-100% | 25-100% upward |
| Grade-IV | Normal or increased | Normal or increased | Posterior on axial radiographs |
| Grade-V | Increased | Increased 100-300% | 100-300% upward |
| Grade-VI | Increased | Normal or decreased | Anterior subacromial or subcoracoid |
Table 1: Rockwood classification of AC joint injuries.
Biometric measurements
Based on prior radiographic work [3,13,14] measurements of the AC joint were obtained to asses both vertical and axial coraco-clavicular translation, including:
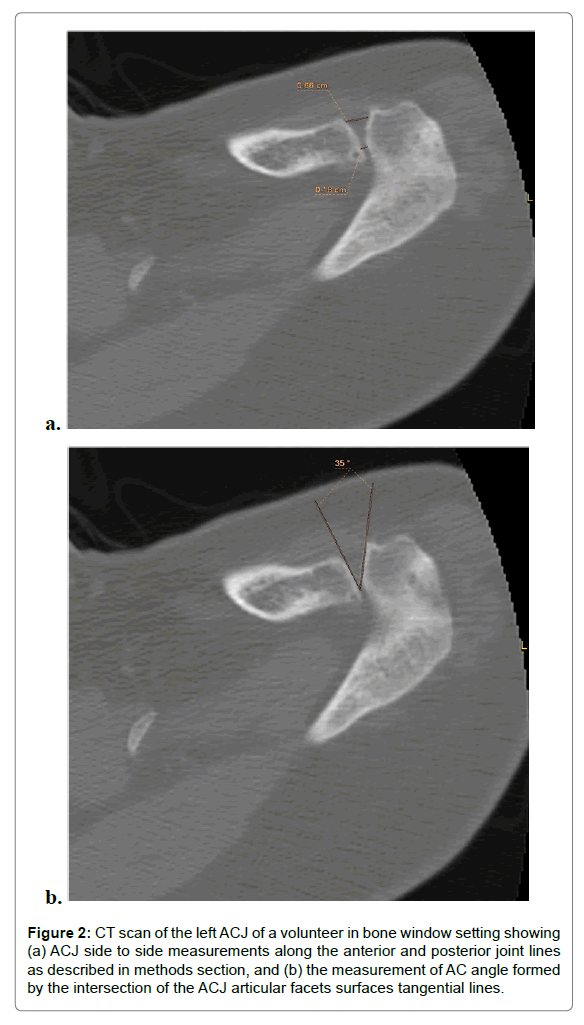
AC joint space distance: On source axial images in the mid joint where the articular facets are well depicted, the acromioclavicular side to side distance was measured at both the most anterior and posterior point on each facet to represent the anterior and posterior joint lines; respectively (Figure 2a).
Figure 2: CT scan of the left ACJ of a volunteer in bone window setting showing (a) ACJ side to side measurements along the anterior and posterior joint lines as described in methods section, and (b) the measurement of AC angle formed by the intersection of the ACJ articular facets surfaces tangential lines.
Axial AC joint space angle: This angle is formed by the intersection of the tangential lines of the acromioclavicular articular facets on source axial images (Figure 2b). This angle aimed to assess subtle axial translation.
The Gleno-Acromioclavicular Angle (GACA): Tauber et al. [3], described the Gleno-Acromioclavicular Angle (GACA) as an objective tool to measure distal clavicular displacement relative to the anterior acromial edge on dynamic radiographic axillary projections. The GACA is formed by the intersection of a line drawn through the glenoid articular surface and the line between the anterior acromial edge and the antero-lateral clavicular edge (i.e., anterior AC joint line).
On axial CT images, the glenoid articular surface and the distal ends of both acromion and clavicle may not appear in the same plane. So, we used the line connecting the coracoids tip and humeral lesser tubercle to express the anterior AC joint line as in previous MR literature [8,9].
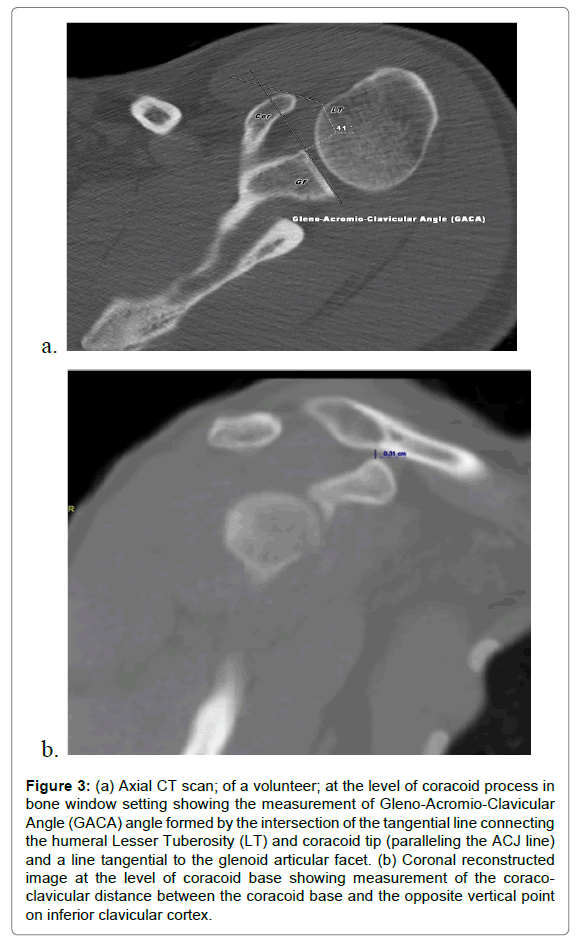
Hence, on true axial CT image in neutral position, the GACA was measured at the intersection of the line drawn through the glenoid articular surface and the anterior AC joint line described before (Figures 3-5). We postulated it as an objective clavicular axial translation indicator.
Figure 3: (a) Axial CT scan; of a volunteer; at the level of coracoid process in bone window setting showing the measurement of Gleno-Acromio-Clavicular Angle (GACA) angle formed by the intersection of the tangential line connecting the humeral Lesser Tuberosity (LT) and coracoid tip (paralleling the ACJ line) and a line tangential to the glenoid articular facet. (b) Coronal reconstructed image at the level of coracoid base showing measurement of the coracoclavicular distance between the coracoid base and the opposite vertical point on inferior clavicular cortex.
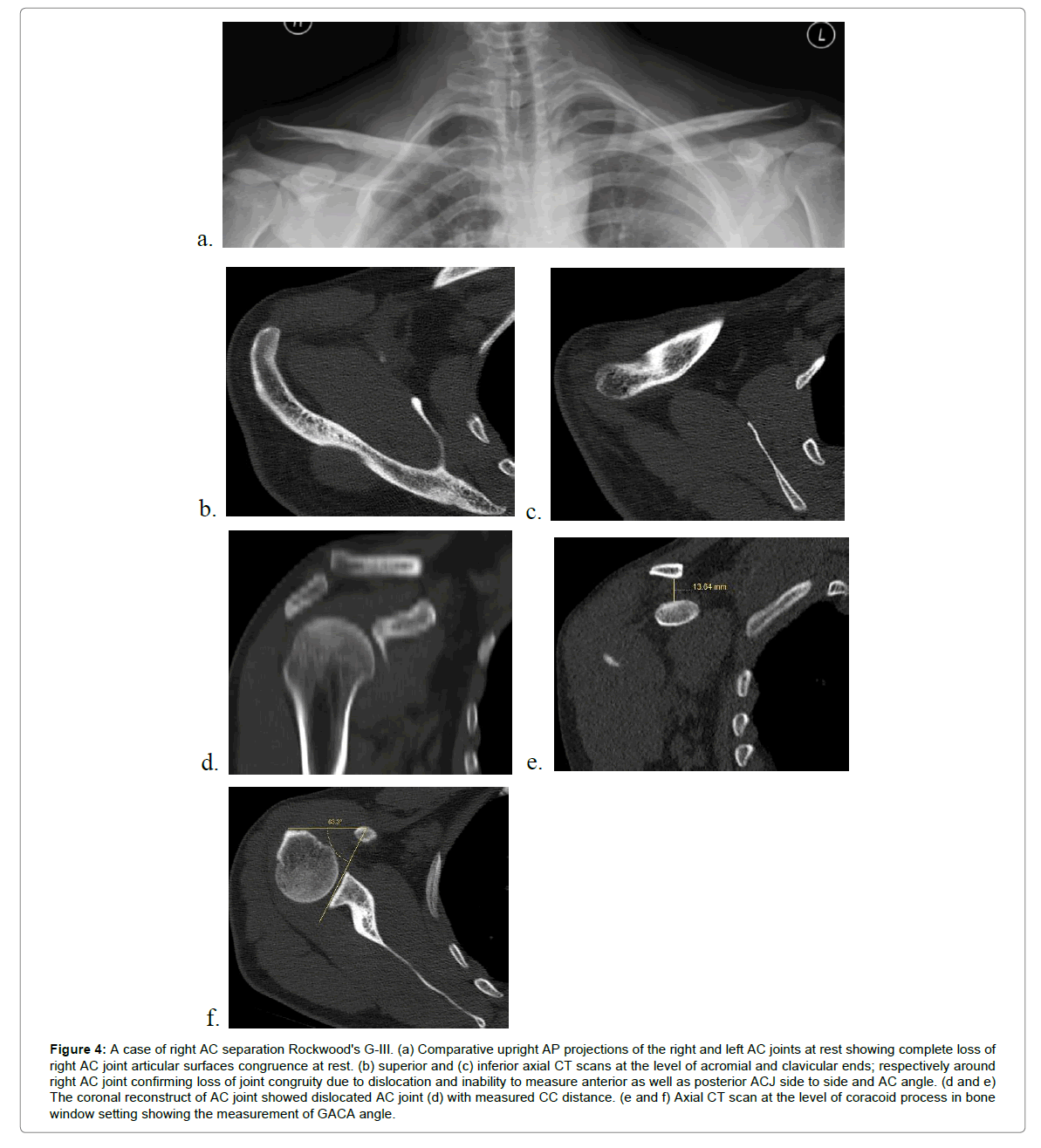
Figure 4: A case of right AC separation Rockwood's G-III. (a) Comparative upright AP projections of the right and left AC joints at rest showing complete loss of right AC joint articular surfaces congruence at rest. (b) superior and (c) inferior axial CT scans at the level of acromial and clavicular ends; respectively around right AC joint confirming loss of joint congruity due to dislocation and inability to measure anterior as well as posterior ACJ side to side and AC angle. (d and e) The coronal reconstruct of AC joint showed dislocated AC joint (d) with measured CC distance. (e and f) Axial CT scan at the level of coracoid process in bone window setting showing the measurement of GACA angle.
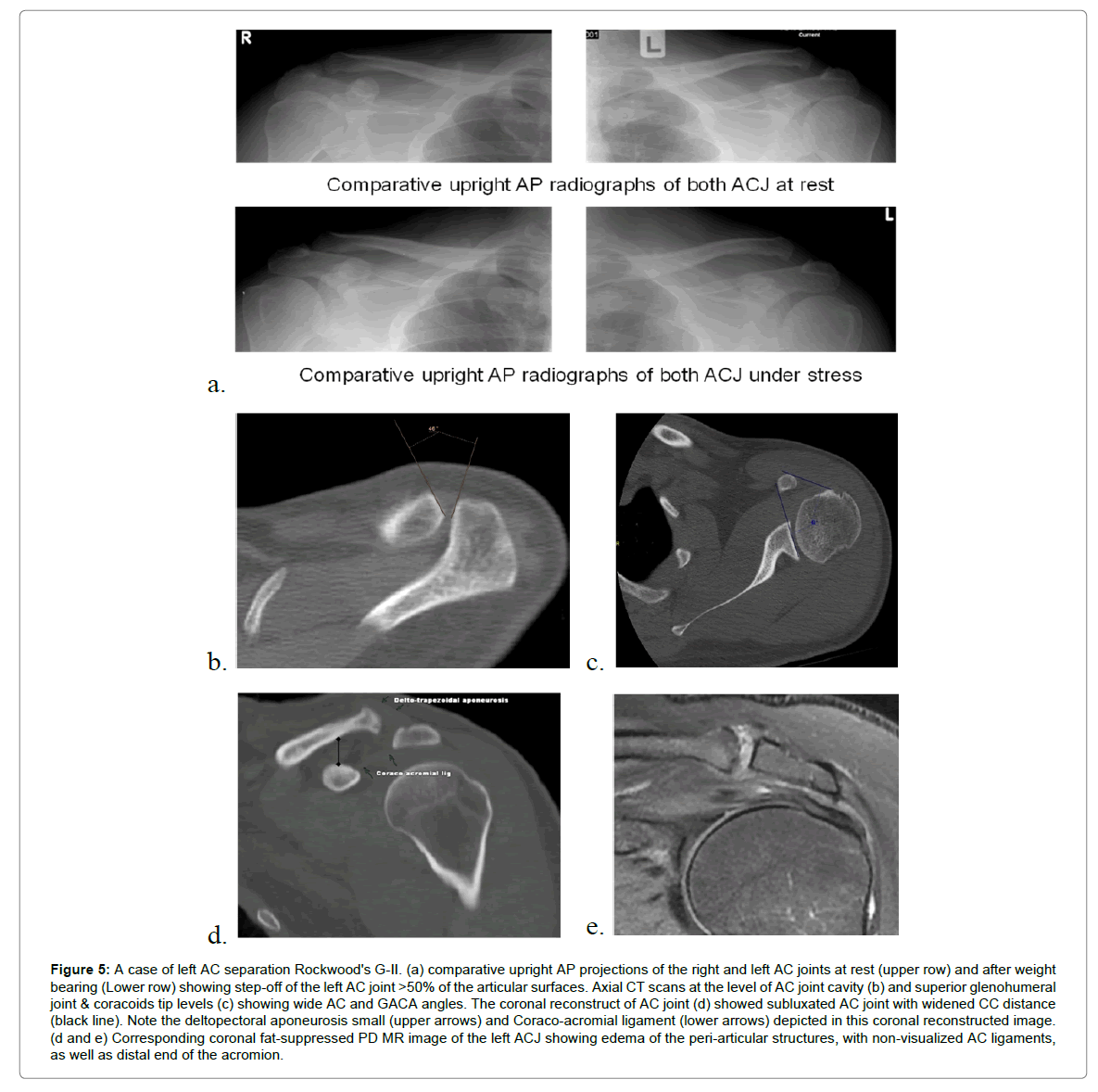
Figure 5: A case of left AC separation Rockwood's G-II. (a) comparative upright AP projections of the right and left AC joints at rest (upper row) and after weight bearing (Lower row) showing step-off of the left AC joint >50% of the articular surfaces. Axial CT scans at the level of AC joint cavity (b) and superior glenohumeral joint & coracoids tip levels (c) showing wide AC and GACA angles. The coronal reconstruct of AC joint (d) showed subluxated AC joint with widened CC distance (black line). Note the deltopectoral aponeurosis small (upper arrows) and Coraco-acromial ligament (lower arrows) depicted in this coronal reconstructed image. (d and e) Corresponding coronal fat-suppressed PD MR image of the left ACJ showing edema of the peri-articular structures, with non-visualized AC ligaments, as well as distal end of the acromion.
Coraco-Clavicular (CC) distance: On the coronal reconstruct images of the mid AC joint mimicking the shoulder AP radiograph, the distance between the coracoid base and 90 degree opposite point on the clavicular surface was measured (Figure 3b). This measurement aimed to assess vertical translation of the AC joint articular surfaces.
Standard of reference: We used the clinical history of all 33 volunteers, emphasizing on clearance of any shoulder problems as our standard of reference. On the other side, as none of our 17 candidates diagnosed with ACJ separation underwent surgical procedure, we used the consensus of all sharing radiologists, provided clinical data and other available imaging studies as the reference standard in agreement with previous research methods [15,16].
Statistical Analysis
Statistical analysis was performed using the Statistical Package for Social Sciences [SPSS version 18]. For qualitative variables, Chi square test; Monte Carlo test and Fisher’s exact test of significance were used. For normally distributed quantitative variables student T-test was used and for skewed quantitative variables non- parametric Mann- Whitney test of significance was used. 5% level of significance was used for interpreting all results. When there was no statistically significant difference between the readings of both observers, the readings of the MSK radiologist (observer-II) were used to assess the presence of any differences between the volunteers and diseased subjects.
Results
Demographic analysis
The study included 33 volunteers [32 males (93.9%) and one female (6.1%)] and 17 candidates with clinical diagnosis of AC separations [16 males (94.1%) and one female (5.9%)]. The mean age of the volunteers and clinical subjects was 32.94 ± 10.74 and 34.94 ± 9 years, respectively. There was no statistically significant difference between the volunteers and patients in age or gender [p=1 and 0.51; respectively].
Patients with AC separations included; one case of Rockwood’s GIII ACJ separation (Figure 4) who refused to do surgery; two cases of Rockwood’s GII with clinical point tenderness over the AC, widened AC distance, and AC articular step off <50% (Figure 5). The remaining fourteen patients were Rockwood’s GI, based on clinical point tenderness, suggestive MR findings and negative radiographs. All of the seventeen subjects with AC injury in our study were conservatively managed.
Inter-observer variations
There was no statistically significant difference between both readers (P value >0.05) as regards the tested CT morphometric and biometric variables of examined AC joints in both volunteers and diseased subjects. This ruled out subjectivity of readings, so the readings of the MSK radiologist were used to analyze the difference between volunteers and diseased (Tables 2 and 3).
| Morphometric variable | Visibility | Volunteer | Test of significance | Diseased | Test of significance | ||
|---|---|---|---|---|---|---|---|
| Observer-I | Observer-II | Observer-I | Observer-II | ||||
| Superior AC ligament | Not seen | 1 (3%) | 3 (9.1%) | P=0.61 | 0 (0.0%) | 4 (23.5%) | P=0.1 |
| Seen | 32 (97%) | 30 (90.9%) | 17 (100%) | 13 (76.5%) | |||
| Inferior AC ligament | Not seen | 1 (3%) | 4 (12.1%) | P=0.36 | 2 (11.8%) | 5 (29.4%) | P=0.4 |
| Seen | 32 (97%) | 29 (87.9%) | 15 (88.2%) | 12(70.6%) | |||
| Trapezoid ligament | Not seen | 2 (6.1%) | 1 (3%) | P=1 | 2 (11.8%) | 1 (5.9%) | P=1 |
| Seen | 31(93.9%) | 32 (97%) | 15 (88.2%) | 16 (94.1%) | |||
| Conoid ligament | Not seen | 2 (6.1%) | 0 (0.0%) | P=0.5 | 1(5.9%) | 1(5.9%) | No difference |
| Seen | 31 (93.9%) | 33 (100%) | 16 (94.1%) | 16 (94.1%) | |||
| Coraco-acromial ligament | Not seen | 7 (21.2%) | 3 (9.1%) | P=0.17 | 1(5.9%) | 2 (11.8%) | P=1 |
| Seen | 26 (78.8%) | 30 (90.9%) | 16 (94.1%) | 15 (88.2%) | |||
| Coraco-humeral ligament | Not seen | 1 (3%) | 2 (6.1%) | P=0.1 | 1 (5.9%) | 2 (11.8%) | P=1 |
| Seen | 32 (97%) | 31(93.9%) | 16 (94.1%) | 15 (88.2%) | |||
| Total | 33 | Fisher’s Exact test | 17 | Fisher’s Exact test | |||
Table 2: Visual assessment of acromioclavicular ligamentous stabilizers visibility among the study population by both observers.
| Biometric variable | Volunteer | Test of significance | Diseased | Test of significance | |||
|---|---|---|---|---|---|---|---|
| Observer-I | Observer-II | Observer-I | Observer-II | ||||
| AC side to side measurements | Anterior | 0.597 ± 0.24 | 0.589 ± 0.27 | P=0.9 | 1.18 ± 0.87* | 0.88 ± 0.3* | P=0.8 |
| - | Posterior | 0.249 ± 0.095 | 0.26 ± 0.111 | P=0.6 | 2.08 ± 4.99* | 0.49 ± 0.39* | P=0.54 |
| Coraco-clavicular distance | - | 0.67 ± 0.34 | 0.72 ± 0.41 | P=0.56 | 0.73 ± .29 | 0.77 ± 0.31 | P=0.73 |
| AC angle | - | 27.13 ± 15.31 | 26.55 ± 14.7 | P=0.88 | 24.65 ± 12.35* | 27.44 ± 12.44* | P=0.52 |
| GACA | - | 52.79 ± 8.18 | 50.82 ± 8.26 | P=0.33 | 48.88 ± 9.28 | 45.94 ± 11.57 | P=0.43 |
*Data derived from 16 AC joint separation cases after exclusion of Rockwood Type-III case due to measurement inapplicability.
Table 3: Objective assessment of both observers for the tested acromio-clavicular biometric data among the study population.
Morphometric variables
The acromial facet antero-medial direction was the commonest orientation in both volunteers (57.6%, n=19) and patients (52.9%, n=9). The lateral direction of clavicular articular facet was commoner in volunteers (48.5%, n=16) compared to the antero-medial direction in patients (47.1%, n=8). However, these differences in both groups were not statistically significant [p=0.8 and 0.7; respectively]. The results of visual assessments of peri-articular ligaments, around AC joints, by both observers are displayed on Table 2. There was no statistically significant variation between both readers, in both groups, as regard visibility of any of the attested ligaments [p-values between 1 and 0.1].
Neither the trapezoid nor the deltoid muscle showed injury in our AC separation group.
Biometric variables
In the single case of Rockwood type-III AC injury; the AC axial side to side and AC angle measurements weren’t applicable thanks to posterosuperior clavicular dislocation with subsequent articular surfaces incongruence (Figure 4). Hence, it was presented as a case report and excluded from statistical analysis of these variances due to its extreme values.
The mean values (± standard deviation) for axial anterior and posterior AC joint lines side to side measurements in patients (0.88 ± 0.3 cm and 0.49 ± 0.39 cm; respectively) was greater than in volunteers (0.59 ± 0.27 cm and 0.26 ± 0.11 cm) and this was statistically significant [p=0.002 and 0.04 for the anterior and posterior joint lines; respectively] (Table 4).
| Biometric variable | Volunteer Mean ± SD |
Diseased Mean ± SD |
Mann-Whitney Test of significance | |
|---|---|---|---|---|
| AC side to side measurements | Anterior | 0.589 ± 0.27 cm | 0.88 ± 0.3 cm* | Z=-3.146 P=0.002* |
| Posterior | 0.262 ± 0.11 cm | 0.49 ± 0.39 cm* | Z=-2.038 P=0.04* |
|
| Coraco-clavicular distance | 0.73 ± .41 cm | 0.77 ± 0.31 cm | Z=-0.799 P=0.42 |
|
| AC angle | 26.55 ± 14.71 | 27.44 ± 12.44* | t=-0.672 P=0.5 |
|
| GACA | 50.82 ± 8.26 | 45.94 ± 11.57 | Z=-1.345 P=0.18 |
|
*Data derived from 16 AC joint separation cases after exclusion of Rockwood Type-III case due to measurement inapplicability
Table 4: Objective assessment of the tested acromio-clavicular biometric data among the study population by observer-II.
The mean values of Coracoclavicular (CC) distance as well as, the Acromioclavicular (AC) and Gleno-acromioclavicular (GAC) angles of both volunteers and patients groups are summarized in Tables 3 and 4. However, there was no significant difference between the volunteers and patients regarding these variables [p- values are=0.42 for the CC distance=0.5 for the AC angle and p=0.18 for the GAC angle].
Discussion
Acromioclavicular joint injuries represent the commonest affliction of this articulation especially in young athletes [1]. Proper grading of the AC injuries relied upon detection of joint widening on conventional radiography [3]. However, inconsistency about imaging planes and debate of applying stress [15-17]; especially in traumatized patients; bias the sensitivity and specificity of this imaging tool. On the other hand, role of Computed Tomography (CT) is well established in skeletal trauma [10,11].
The current study showed no significant statistical differences in the frequency of AC joint articular facet orientations. This is comparable to the results of Colegate-Stone et al. [18] who found no significant difference between the three morphologic shapes of the AC joint in their CT analysis correlated with cadaveric dissections.
Using the previous MR anatomic criteria [9], MDCT depicted the capsular [superior and inferior acromio-clavicular] as well as extra-capsular [coraco-clavicular and coraco-acromial] ligaments in the majority of our study population in both groups.
Previous anatomic descriptions confirmed variable obliquity of the AC joint space from posterior to anterior and from lateral to medial [19] as well as in coronal and sagittal planes [20]. The current study showed that acromial antero-medial and clavicular lateral inclinations are the commonest patterns. Additionally, it assessed the mean AC joint distances at the anterior and posterior joint lines off the articular facets in true axial plane. The derived results showed nearly double measurements at the anterior than the posterior joint lines. Hence, our measurements portray a near conical shape of the AC joint in axial plane with apex directed posteriorly on axial CT images.
A previous report [14] stated that the average AC joint space in normal volunteers measures 3.1 ± 0.8 mm using the integral of side to side measurements between the upper and lower levels of the joint space on frontal radiographs. However, these data lacked standardized views in trauma settings.
Our study showed that axial joint space distances at the anterior and posterior joint lines measured 0.59 ± 0.27 cm and 0.26 ± 0.11 cm; respectively, in volunteers. Moreover, there was statistically significant difference of these measurements from those of the subjects with clinical AC separation; who tolerated the comfortable positioning on CT in trauma settings. We thought this point strengthens the validity and practicality of our measurements.
The normal coraco-clavicular distance is 11-13 mm on plain radiography [1,12-15]. We did not found significant difference between volunteers and subjects with AC separations as regard coraco-clavicular distance on MDCT. This could be explained by absence of gravity dependant effect seen on standing radiographs and elimination of the potential magnification factor in radiography.
We proposed a new angular measurement, the axial Acromioclavicular (AC) angle in a similar way to other skeletal regional measurements [21]. We assessed its ability to detect axial acromioclavicular translation in subjects with AC separation. Its mean value in normal subjects lying supine with neutral arm position was 26.55 ± 14.71. However, no significant difference was found in subjects with Rockwood G-I & G-II AC separations. Unfortunately, this angle is irrelevant in higher grades of AC separations (Rockwood G-III and up) as a result of capsular disruptions with subsequent loss of AC articular surfaces congruence.
Our study evaluated the Gleno-Acromioclavicular Angle (GACA) recently described by Tauber et al. [3] to quantify horizontal instability of the distal clavicle on dynamic radiography in supine patients. We found its mean values are slightly higher in volunteers with no statistically significant difference from the traumatized subjects.
We acknowledge some limitations to the current study. Our volunteer sample size is small as we were concerned with radiation exposure issues. We did not use other CT studies as CT chest to standardize measurements in resting position and assure clearance of any unidentified AC problems. However, most literature reports dealing with the AC injuries cross-sectional imaging and surgeries included limited number of subjects. Further assessment with a larger sample might powerfully validate our results.
In addition, our subjects were scanned in the supine position with the arm resting in neutral position. This eliminated the gravity-assisted displacement classically used in radiographic classification schemes of AC separation. Further studies assessing these measurements while the peri-articular ligaments under stress e.g. in internal rotation may be desired for more validation of clinical applicability of the method. Lack of MR correlation of AC capsular and peri-articular ligaments, in the volunteers, can bias the visibility of articular and peri-articular softtissue ligaments on MDCT. Yet the imaging anatomy of these structures is already well established in imaging, orthopedic and anatomic literatures. In addition, lack of post-operative data, in our cohort of diseased subjects, may bias the CT differentiation of these structures from post-traumatic scars. However, this is still a hot discussion topic for the MR that may necessitate dynamic evaluation [22].
Another limitation is that we could not define a relation between different grades of AC separation and our CT measurements due to our small sample and paucity of variations.
The morphometric parameters and angular measurements may be affected by the bony anatomy, associated dysplasia’s, fractures and/ or concomitant arthritic changes. Also we did not assess the intra-observer variability of these variables.
In spite of these limitations, our study confirms the great variability of AC joint articular facet morphology on MDCT. Additionally, the capsular and peri-capsular AC joint ligaments could be depicted on CT studies. The axial anterior and posterior AC joint distances measures 0.59 ± 0.27 and 0.26 ± 0.11 cm; respectively in supine neutral resting position. This portrays a near conical morphology of the AC joint in axial plane.
Declaration
The authors certify below that they have not received funding for research on which our article is based from any sponsor and/or institution.
Acknowledgment
The authors thank Prof. Mark E. Schweitzer, Chair of the Department of Radiology at Stony Brook Medicine, for his critical revision of the final manuscript.
References
- Mazzocca AD, Arciero RA, Bicos J (2007) Evaluation and treatment of acromioclavicular joint injuries. Am J Sports Med 35: 316-329.
- Pennington RGC, Bottomley NJ, Neen D, Brownlow HC (2008) Radiological features of osteoarthritis of the acromiclavicular joint and its association with clinical symptoms. J Orthop Surg 16: 300-302.
- Tauber M, Koller H, Hitzl W, Resch H (2010) Dynamic radiologic evaluation of horizontal instability in acute acromioclavicular joint dislocations. Am J Sports Med 38: 1188-1195.
- Williams PL, Bannister LH, Warwick R (1995) The anatomical basis of medicine and surgery (38th edn.). Churchill Livingstone, NY, USA.
- Ernberg LA, Potter HG (2003) Radiographic evaluation of the acromioclavicular and sternoclavicular joints. Clin Sports Med 22: 255-275.
- Ferri M, Finlay K, Popowich T, Jurriaans E, Friedman L (2005) Sonographic Examination of the Acromioclavicular and Sternoclavicular Joints. J Clin Ultrasound 33: 345-355.
- Rozin AP (2009) Ultrasound measurement of the acromioclavicular joint. Ann Rheum Dis 68: 445-446.
- Schaefer FK, Schaefer PJ, Brossmann J, Hilgert RE, Heller M, et al. (2006) Experimental and clinical evaluation of acromioclavicular joint structures with new scan orientations in MRI. Eur Radiol 16: 1488-1493.
- Alyas F, Curtis M, Speed C, Saifuddin A, Connell D (2008) MR imaging appearances of acromioclavicular joint dislocation. Radiogr Rev Publ Radiol Soc N Am Inc 28: 463-479.
- Geijer M, El-Khoury GY (2006) MDCT in the evaluation of skeletal trauma: principles, protocols, and clinical applications. Emerg Radiol 13: 7-18.
- Geyer LL, Koerner M, Wirth S, Mueck FG, Reiser MF, et al. (2013) Polytrauma: optimal imaging and evaluation algorithm. Semin Musculoskelet Radiol 17: 371-379.
- Rockwood C, Williams G, Young C (1996) Injuries to the acromioclavicular joint. In: Fractures in adults. Philaderphia: Lippincott-Raven.
- Petersson CJ, Redlund-Johnell I (1983) Radiographic joint space in normal acromioclavicular joints. Acta Orthop Scand 54: 431-433.
- Väätäinen U, Pirinen A, Mäkelä A (1991) Radiological evaluation of the acromioclavicular joint. Skeletal Radiol 20: 115-116.
- Cabarrus MC, Ambekar A, Lu Y, Link TM (2008) MRI and CT of insufficiency fractures of the pelvis and the proximal femur. AJR Am J Roentgenol 191: 995-1001.
- Henes FO, Nüchtern JV, Groth M, Habermann CR, Regier M, et al. (2012) Comparison of diagnostic accuracy of Magnetic Resonance Imaging and Multidetector Computed Tomography in the detection of pelvic fractures. Eur J Radiol 81: 2337-2342.
- Bossart PJ, Joyce SM, Manaster BJ, Packer SM (1988) Lack of efficacy of ‘weighted’ radiographs in diagnosing acute acromioclavicular separation. Ann Emerg Med 17: 20-24.
- Colegate-Stone T, Allom R, Singh R, Elias DA, Standring S, et al. (2010) Classification of the morphology of the acromioclavicular joint using cadaveric and radiological analysis. J Bone Joint Surg Br 92: 743-746.
- Duparc P (1994) Les disjonctions acromio-claviculaires. Montpellier, Sauramps.
- Bosworth BM (1949) Complete acromioclavicular dislocation. N Engl J Med 241: 221-225.
- Isaacs JD, Baba M, Huang P, Symes M, Guzman M, et al. (2013) The diagnostic accuracy of Böhler’s angle in fractures of the calcaneus. J Emerg Med 45: 879-884.
- Izadpanah K, Winterer J, Vicari M, Jaeger M, Maier D, et al. (2013) A stress MRI of the shoulder for evaluation of ligamentous stabilizers in acute and chronic acromioclavicular joint instabilities. J Magn Reson Imaging JMRI 37: 1486-1492.
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 7502
- [From(publication date):
April-2017 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 6528
- PDF downloads : 974