Research Article Open Access
University Students Sexual Practices- An Insight Overview
Shahkamal Hashmi1, Kelash Rai2, Farzeen Tanwir3*, Vikash4, Imran Ahmed5, Hafiz Muhammad Tayyab6, Nabil Rashid1, Salman Sharif3, Sabihuddin Ahmed3, Manahil Jeoffrey3
1Dow University of Health Sciences, Pakistan
2Director of Post Graduate Studies and Department of Health Government of Sindh, Pakistan
3Department of Periodontology, Ziauddin University, Pakistan
4Department of Infectious Diseases, Tongji Medical College, Huazhong University of Science and Technology, Wuhan, China
5Department of Surgery, Ziauddin University, Karachi, Pakistan
Visit for more related articles at International Journal of Emergency Mental Health and Human Resilience
Abstract
Background: Sexually transmitted infections are an ever growing concern in developing countries. In Pakistan it has been an estimated 97,000 (0.1%) reported cases of HIV alone. Dearth of available information has made it difficult to assess the full extent of the STI problem. A reason for this shortage of data has been attributed to lack of awareness and research. This study aimed to evaluate the sexual practices of students in Karachi.
Methodology: This cross sectional study was conducted at four colleges in Karachi, Pakistan. College students were included without any restriction of age and gender. Ethical approval was obtained from all institutions. Self-administered questionnaire was used to access the knowledge and practices of students regarding Sexually transmitted diseases. Frequencies and percentage were calculated for each variable.
Results: In total 890 university students participated in this study with a response rate of 89%. Overall male participants were 515, while 375 females participated in the study. Almost 30% of the male and 49.6% of the female students knew that there is a vaccine for Human Papillomavirus (HPV) with Male/Female Odds ratio of 0.42( 95% C.I: 1.34-28). However 22.9% of male and 76.5% of female students (M/F OR: 0.29, 95% C.I: 0.34-0.7) believed that the oral sex is as threatening and unsafe as vaginal or anal sex. The most preferred method of contraceptive recognized by the students was condoms (males 14.7 % and females 8.6%, with M/F OR: 1.70, 95% C.I: 0.29-0.67) followed by oral contraceptive pills (males 6.2 %, females 7.7%, M/F OR: 0.80, 95% C.I: 0.72-24.3).
Conclusion: Research needs to be undertaken to employ policies at an administrative level to introduce change in the curriculum and rectify related issues in order to conceive better sexual practices in adolescents.
Keywords
Sexually transmitted diseases, HIV/AIDS, students, college, adolescents
According to research conducted under the auspices of the World Health Organization (WHO), Sexually Transmitted Infections (STIs) have been deemed a “Public health problem of major significance in most parts of the world”. Some of the more important STIs to be concerned about include HIV (Human Immunodeficiency Virus) and Human Papilloma Virus (HPV) (Mascarenhas, Flaxman, Boerma et al., 2012).
HIV is a slowly replicating retrovirus that causes AIDS (Acquired immunodeficiency syndrome), a condition in humans in which continued dysfunction of the immune system makes the body susceptible to attacks by fatal opportunistic infections and cancers. A high relation of the transfer of the disease from person to person has been attributed to sexual intercourse. Globally there are more than 35.3 million people living with HIV, as of 2012 (UNAIDS.org, 2013). There have been reported cases in almost all regions of the world, but the high incidence of the disease has been associated to low- middle income social demographics in low income countries, especially in Sub-Saharan Africa.
As of 2008 there have been more than 2 million AIDs related fatalities worldwide, a high proportion of these fatalities were in the South Asia region (480,000 persons). The prevalence is dominated by the epidemic in India however more locally; Pakistan is facing the challenge of an increased number of reported cases with UN/Pakistan Government estimates of 97,000 people, which makes up 0.1 percent of the population. High drug use and increasing trends of extramarital intercourse have been acknowledged reasons for the rise of the AIDS epidemic locally especially among sex workers, dwellers of squatter colonies and drug users.
HPV is another STI, which is a DNA virus of the papillomavirus family. It infects the keratinocytes of the skin or mucus membrane. Usually asymptomatic, this disease can become symptomatic in some patients and may cause benign papilloma or cancers of the cervix, vulva, vagina, penis, oropharynx and anus. More than 30 types of the virus are transmitted through sexual intercourse and involve the anus and genital area. The global prevalence of infection with HPV (in women without cervical abnormalities) is 11-12% with the highest trends in sub-Saharan Africa, Eastern Europe and Latin America (Forman, de Martel, Lacey et al., 2012). Prevalence in Southsoutheast Asia is also high, with almost 14% of the global infected population residing here (Dawn, 2009). Worldwide screening and treatment campaigns have been proved effective in controlling the rising trend of the disease. It has been estimated by certain studies, that prevalence of HPV is much less in Pakistan, reasons for which include cultural and social taboos surrounding having multiple sexual partners, but as is common for all diseases, without adequate awareness and steps for prevention, spread is highly certain (Dawn, 2009).
Understanding the role of contraceptives in birth control is as important as understanding their role in preventing STIs. Ideally, advantages offered by primary prevention which include abstinence or at least limiting the number of sexual partners preferring long term mutually monogamous relationships are far greater than secondary protection (artificial contraception methods) (National Prevention Information Network, 2014). Reality however is that negligence of the former will continue, hence it is necessary to bring about greater awareness of contraceptive devices as a means to curb the STI epidemic.
The major types of contraceptives include barriers (condoms), oral contraceptives and natural methods. Weighing their pros and cons is imperative when formulating specific target campaigns for disease prevention in developing/ lower socio-economic countries.
Male Condoms
Male condoms are barrier contraceptives which consist of a rubber (latex) sheath worn over the erect penis before copulation. The condom effectively covers that portion of the males anatomy entering the female, and by barring the ejaculate from entering the vagina, it helps prevent the transmission of STIs via exchange of bodily fluids. Hence where barrier contraception is extremely effective in preventing unwanted pregnancy, it is equally effective in preventing the spread of numerous STIs including HIV/AIDs (Skouby, 2010).
There are number of articles where it has been evidenced that condom use does not prevent the transmission of HPV (Baseman, 2005; Skouby, 2010; Thun et al., 2010), however there have been studies conducted in lieu of the role of condoms, in cases of previously acquired cervical cancer, promoting regression of cancer and clearance of the HPV infection, and the results have been favorable (Munk, Gudlaugsson, Ovestad et al., 2012). This just further validates the importance of individuals knowing what contraceptive is best in the pursuit of safe sex.
Oral Contraceptives and Other methods
Oral contraceptives have a high efficacy of pregnancy prevention but since they do not provide mechanical prevention against exchange of body fluids, they are inevitably limited in their use as STI prophylactics. Withdrawal method is a frequently practiced method for contraception, particularly in certain low income countries. This method accompanies much greater chance of failure than using oral contraceptives or condoms (Black, Gupta, Rassi, & Kubba, 2010).
Research conducted in different countries has shown that university students to a large extent are aware of these topics (Agius et al., 2010; Lally et al., 2014). However a dearth of certifiable research conducted in Pakistan has prompted us to conduct a research to get a better understanding of where students in major universities stand. The implications of such a research cannot be overstated. Pakistan, being a low income country, is as yet suffering from a largely privatized healthcare system. Any research conducted to assess the need for better prophylactic care, can only be advantageous towards decreasing the burden on the tertiary care hospitals.
The aim of this study is to gain an insight into the sexual practices of students in Karachi. In the current era of globalization and as sensitive topics are being discussed more frequently (such as sexual practices in adolescent), this study adds and updates the scant existing literature available in the Pakistan.
Method
This cross sectional study was conducted at four colleges located in the city of Karachi. Two of them were public while two were private. The duration of the data collection and analysis was seven months, starting from January 2014 till July 2014. Ethical consent to conduct the study was obtained from all four institution’s ethical board.
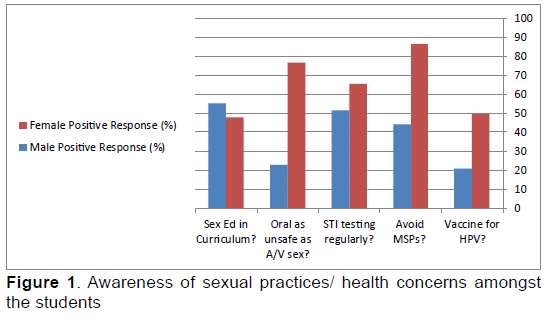
Knowledge and practices of students were evaluated through a self-administered questionnaire. The questionnaire was in English language as the medium of instruction in in all institution was English. Students were told regarding the nature of the study, and written consent was obtained from all the respondents before the filling of the questionnaire. The questionnaire aimed to gather information regarding student’s sexual practices (Figure 1). They were inquired about their preferred method/s of contraception, visits for STIs screening, vaccination status (Figures 2a and 2b). The participants included were college students with no age or gender restrictions. The students were non-medical and studied subjects related to business, economic, social sciences and administration. All students were the citizens of Pakistan; however a few belonged from different cities of Pakistan. Students were randomly selected in the colleges and the confidentiality of their identity was guaranteed. The participants were briefed regarding the mode of transmission, signs and symptoms, complications, prevention, treatment and prognosis of various sexually transmitted diseases by an infectious disease specialist after filling the questionnaire. "Odds ratios with 95% confidence intervals were used to estimate the effects of different independent variables on the practices of the sample population. The study has followed a model of School-linked sexual health services for young people (SSHYP) and further modified according to the local socio-cultural norms in Pakistan. The data was analyzed through Statistical Package of Social Sciences (SPSS) version 17. Frequency and percentages were calculated for each qualitative variable.
Results
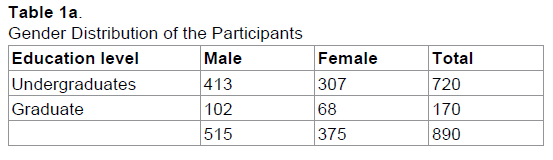
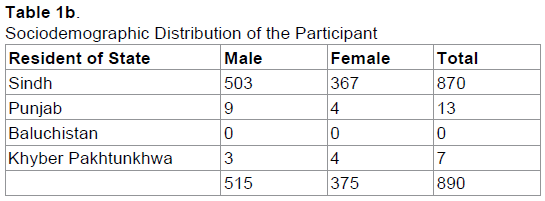
Overall 890 university students participated in this study with a response rate of 89%. The total numbers of male participants were 515 while 375 females participated in the study. Among the respondents, 720 (413 male and 307 female) were undergraduate students and 170 (102 male and 68 female) students were graduate level students (Table 1).
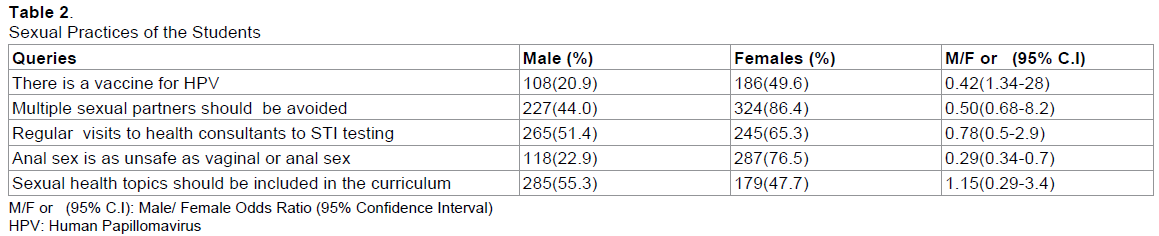
Regarding sexual practices of the students, 20.9% of the male and 49.6% of the female students asserted that there is a vaccine for Human Papillomavirus (HPV) with Male/Female Odds ratio of 0.42 (C.I: 1.34-28). In response to whether multiple sexual partners (MSPs) should be avoided, 44% and 86.4% of the male and female participants respectively believed that they should abstain from MSPs (M/F Odds 0.50 C.I: 0.68-8.2). Majority of males (51.4%) and females (65.3%) participants were in favor of regular visits to the health consultants to test for STIs. Overall, 22.9% of male and 76.5% of female students (M/F OR: 0.29, C.I: 0.34-0.7) thought that the oral sex is as threatening as vaginal or anal sex. Furthermore, 55.3% and 47.7% of males and female participants respectively were in support of introducing sexual health topics in their curriculum (M/F OR: 1.15, C.I: 0.29-3.4) (Table 2).
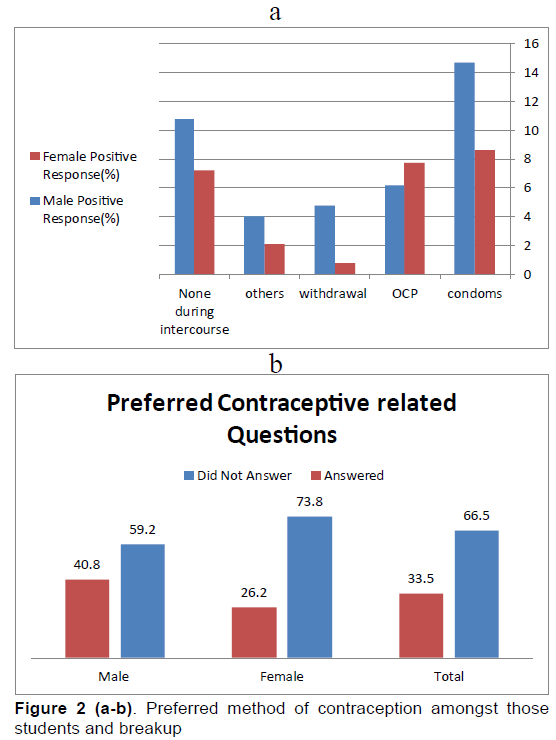
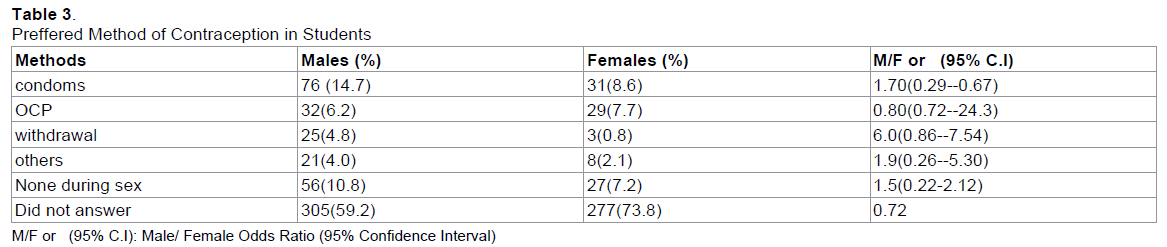
The most preferred method of contraceptive by the students was condoms (males 14.7 % and females 8.6%, with M/F OR: 1.70, C.I: 0.29--0.67) followed by oral contraceptive pills (males 6.2 %, females 7.7%, M/F OR: 0.80, C.I: 0.72--24.3). Majority of the students did not mention their preferred method of contraception (male 59.2% and female 73.8%) (Table 3).
Discussion
Our study demonstrated that non-medical students in Karachi had varying knowledge on different aspects of sexually transmitted disease. Women were found to be more aware regarding healthy sexual practices and STI. At the turn of the twentieth century, WHO released a study on the global prevalence and incidence of selected curable STIs. This study although deficient in the statistics of more grievous infections/ viruses (like HIV and/or HPV) nonetheless paved the way for further research into not just collecting more data on the diseases but also trying to assess the global spread of awareness concerning these diseases and methods of preventing them (Burchell et al., 2006; World Health Organization & UNAIDS; 2008).
A study done on young individuals in Karachi observed that there was a major knowledge gap with respect to STIs and the use of contraceptives (Farid-ul-Hasnain, Johansson, Gulzar, & Krantz, 2013). Results from our study are similar in nature as almost 75 percent of the females and 60 percent of the males failed to answer that whether the contraceptives have been proved useful in preventing STIs and what was the most effective measure to prevent STI. Such a question hoped to elicit two important conclusions. Firstly, whether the students have enough prior knowledge aiding their answers regarding prophylactic management of STDs? And secondly, assuming they do have knowledge to some extent, whether they can correctly identify the best method.
When it comes to knowledge, we were quickly made aware that the students were indeed lacking in awareness. This speaks fairly when compared with major trends in other developing countries facing similar epidemics. Females in a study conducted in Nigeria were largely aware of the association between sexual activities and STDs, however nearly half that proportion was unaware of the advantages contraceptives can have in preventing these infection (Okpani & Okpani, 2000). An important complementary finding of our research was one derived from the question pertaining to the "introduction of Sexual Health Topics in the core Curriculum". Almost 50 percent of both gender populations were averse to this proposal. Many juxtaposed theories can be formulated, regarding this apparent disregard for attainment of health related knowledge in a professionally organized, systematic fashion. Socio-economic concerns, religious ideologies, cultural taboos, and close-knit-family oriented upbringing; are all cited as contributors to such an attitude. Since we are talking about college going students with a much more conservative upbringing than their colleagues from western nations, the only relevant conclusion can be that without experience in the usage and indications of these devices, students cannot make an educated guess towards which one is more effective in preventing STDs.
Now there was a certain percentage of the sample (33.5%) that did answer the questionnaire to the fullest, bringing us to the second postulated question. Majority (12%) of the students voted for condoms as the preferred method of contraception (14.7 percent of males, 8.6 percent of females), followed closely by Oral Contraceptive Pills (6.2 percent of males, 7.7 percent of females), then withdrawal method (4.8 percent of males, 0.8 percent of females) and lastly Other Methods (4 percent of males, 2.1 percent of females). These percentages add up to realize that 75.3 percent of the answering population did believe in some sort of contraception method being responsible for preventing the spread of STD's. This is a positive sign, showing that at least for some individuals, the Word of Mouth, Social Media interactions and Mass Media Propagation of the merits of using contraceptive devices has made an impact in their thinking.
Crosby et al. proposed that condoms could decrease the chances of STD transmission, a proposal that was later validated by The US Centre for Disease and Control (CDC) in 2013 which has advised that "consistent and correct usage of condoms can reduce (not eliminate) the transmission of STDs" (Crosby et al., 2012; Centers for Disease Control and Prevention, 2013). The findings of our study to a certain extent reflect that although some individuals do know about the global attitude towards STD prevention, more awareness is very much needed and the best groups of individuals to target are college going students.
Limitations in our study questionnaire prevented us from eliciting whether or not these individuals have indeed participated in sexual intercourse at any point prior to answering our questions, which could bias the results and this can be the basis for further research into the topic.
Vaccines are currently available with evident efficacy in preventing HPV; however one concern we had was that the general student body would not be aware of these, and the results support our hypothesis. Males were disappointingly negligent with only 20.9 percent affirming to the availability of the vaccine. Females, though higher in proportion at 49.6 percent, were also grossly unaware of the screening and prophylactic protocols surrounding HPV transmission.
This deficiency needs to be addressed in a manner similar to one employed in other developing countries (Cuzick, Arbyn, Sankaranarayanan et al., 2008). The present study may contribute to the existing data and should be used by the concerned authorities (government or non-government organizations) to evaluate and implement interventions that may benefit sexual health in students.
Conclusion
Research must be undertaken to find the feasibility of making PAP smears and vaccines more widely available to sexually active women of reproductive age group. At the same time the subject of cervical cancers and vaccinations/prophylaxis should be broached in colleges and universities where the maximum intermingling of young adults takes place.
References
- Agius, P.A., Pitts, M.K., Smith, A., & Mitchell, A. (2010). Sexual behaviour and related knowledge among a representative sample of secondary school students between 1997 and 2008. Australian and New Zealand journal of public health, 34(5), 476-481
- Baseman, J. G., &Koutsky, L. A. (2005).The epidemiology of human papillomavirus infections.Journal of Clinical Virology, 32, 16-24
- Black, K.I., Gupta, S., Rassi, A., &Kubba, A. (2010). Why do women experience untimed pregnancies? A review of contraceptive failure rates.Best Practice & Research Clinical Obstetrics &Gynaecology, 24(4), 443-455
- Burchell, A.N., Winer, R.L., de Sanjosé, S., & Franco, E.L. (2006). Epidemiology and transmission dynamics of genital HPV infection.Vaccine, 24, S52-S61
- Centers for Disease Control and Prevention (CDC). (2013). Condoms and STDs: Fact sheet for public health personnel. Available from: http://www. cdc. gov/condomeffectiveness/latex. htm
- Crosby, R.A., Charnigo, R.A., Weathers, C., Caliendo, A.M., &Shrier, L.A. (2012). Condom effectiveness against non-viral sexually transmitted infections: a prospective study using electronic daily diaries. Sexually transmitted infections, 88(7), 484-489
- Cuzick, J., Arbyn, M., Sankaranarayanan, R., Tsu, V., Ronco, G., Mayrand, M.H., et al. (2008).Overview of human papillomavirus-based and other novel options for cervical cancer screening in developed and developing countries.Vaccine, 26, 29-41
- Dawn. (2009). HPV prevalence among Karachi women low: study [online] [cited June 2014] Available from: http://www.dawn.com/news/506474/hpv-prevalence-among-karachi-women-low-study
- Fact Sheet.UNAIDS.org. 2013.Retrieved June 1, 2014.Available at http://aids.gov/hiv-aids-basics/hiv-aids-101/global-statistics/
- Farid-ul-Hasnain, S., Johansson, E., Gulzar, S., &Krantz, G. (2013). Need for Multilevel Strategies and Enhanced Acceptance of Contraceptive Use in Order to Combat the Spread of HIV/AIDS in a Muslim Society: A Qualitative Study of Young Adults in Urban Karachi, Pakistan. Global journal of health science, 5(5), 57-66
- Forman, D., de Martel, C., Lacey, C.J., Soerjomataram, I., Lortet-Tieulent, J., Bruni, L et al. (2012).Global burden of human papillomavirus and related diseases.Vaccine, 30, F12-F23.5
- Lally, K., Nathan-V.Y., Dunne, S., McGrath, D., Cullen, W., Meagher, D., et al. (2015).Awareness of sexually transmitted infection and protection methods among university students in Ireland.Irish journal of medical science, 184(1), 135-142
- Mascarenhas, M.N., Flaxman, S.R., Boerma, T., Vanderpoel, S., & Stevens, G.A. (2012). National, regional, and global trends in infertility prevalence since 1990: a systematic analysis of 277 health surveys. PLoS medicine, 9(12), e1001356
- Munk, A.C., Gudlaugsson, E., Ovestad, I.T., Lovslett, K., Fiane, B., van DiermenHidle, B., et al. (2012).Interaction of epithelial biomarkers, local immune response and condom use in cervical intraepithelial neoplasia 2–3 regression.Gynecologic oncology, 127(3), 489-494
- National Prevention Information Network.(2014). ‘STD Prevention Today’. [online] [cited June 2014]. Available from: http://www.cdcnpin.org/scripts/std/prevent.asp
- Okpani, A.O.U., &Okpani, J.U. (2000).Sexual activity and contraceptive use among female adolescents–A report from Port Harcourt, Nigeria.African Journal of Reproductive Health, 4(1), 40-47
- Skouby, S.O. (2010). Contraceptive use and behavior in the 21st century: a comprehensive study across five European countries. The European Journal of Contraception and Reproductive Health Care, 15(S2), S42-S53
- Talha, B. (2008). New government in Pakistan faces old challenges. The Lancet Infectious Diseases, 8(4), 217-218
- Thun, M.J., DeLancey, J.O., Center, M.M., Jemal, A., & Ward, E.M. (2010). The global burden of cancer: priorities for prevention. Carcinogenesis, 31(1), 100-110
- World Health Organization & UNAIDS, U. (2008). Epidemiological fact sheet on HIV and AIDS.Core data on epidemiology and response Uganda.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 18388
- [From(publication date):
June-2015 - Aug 23, 2025] - Breakdown by view type
- HTML page views : 13663
- PDF downloads : 4725