Case Report Open Access
Unusual Presentation of Metastatic Prostate Cancer: A Case Report
Tawfeeq H* and Ihezue CDepartment of Radiology, Queen Alexandra Hospital, Portsmouth, England
- *Corresponding Author:
- Haseeba Tawfeeq
Department of Radiology, Queen Alexandra Hospital
Portsmouth, England
Tel: 00447743698638
E-mail: haseebatawfeeq@yahoo.com
Received date: July 10, 2017; Accepted date: July 28, 2017; Published date: August 02, 2017
Citation: Tawfeeq H, Ihezue C (2017) Unusual Presentation of Metastatic Prostate Cancer: A Case Report. OMICS J Radiol 6:267. doi: 10.4172/2167-7964.1000267
Copyright: © 2017 Tawfeeq H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Radiology
Abstract
61-year-old male, previously healthy, presented to Primary care with four-month history of non-tender, non-traumatic left lower neck mass. Patient denied any significant urinary or constitutional symptoms or any bone pain. A referral for neck Ultrasound was organized which showed an abnormal rounded hypoechoic left SCF (supraclavicular fossa) node with loss of fat hilum. USS (Ultrasound)-guided biopsy of this node was performed, and while histological results were being awaited, a CT (neck, chest and abdomen) was done. The scan results demonstrated multiple left SCF and upper left retroperitoneal/para-aortic nodes. A working diagnosis of Lymphoma was entertained at this point and whilst the result of the biopsy was being awaited a PET-CT was done which showed the presence of metabolically active left SCF nodes, of which, the most prominent one showing a standardized uptake value (SUVMax=4). In addition, the scan showed a focal activity in the right peripheral zone of the prostate gland (SUVMax=5) along with metabolically active lesions involving the pelvic bones and the neck of the left femur consistent with skeletal metastases (SUVMax=6). Biopsy of the left SCF node showed evidence of prostatic adenocarcinoma. This case report reviews an uncommon presentation of prostate cancer with supraclavicular adenopathy.
Keywords
Prostate cancer; Lymphadenopathy; Metastasis
Introduction
Prostate cancer is one of the leading causes of morbidity and mortality in men. The incidence has increased considerably over the last several decades and as a result led to the development of screening tools, which assisted in early detection and subsequent treatment of the disease [1]. However; a substantial proportion of men with prostate cancer remain asymptomatic and seek medical attention significantly late when they present with disseminated disease. Local lymph nodes are the single most common metastatic site for carcinoma of the prostate with pelvic and retroperitoneal nodes being the most commonly involved [2]. Despite left supraclavicular nodes being reported as a site of non-regional, extra-skeletal metastases, they remain an uncommon presentation of prostate cancer [3].
Case Report
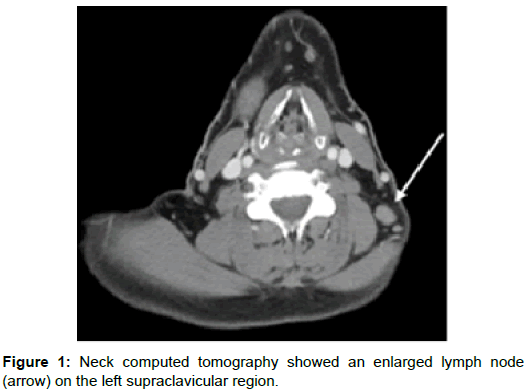
61-year-old man, previously healthy, presented to Primary care with four-month history of non-tender, non-traumatic left lower neck mass. Significant urinary or constitutional symptoms or bone pain were denied at initial presentation. Patient was referred to head and neck surgeons for assessment of lower neck mass. Neck ultrasonography showed abnormal rounded hypoechoic left supraclavicular fossa node with loss of fat hilum. Fine needle biopsy of the Supraclavicular node was performed and further imaging was arranged while waiting for the histological results (Figure 1).
A subsequent torso CT with contrast demonstrated multiple enlarged left supraclavicular and left retroperitoneal lymphnodes (Figures 2 and 3).
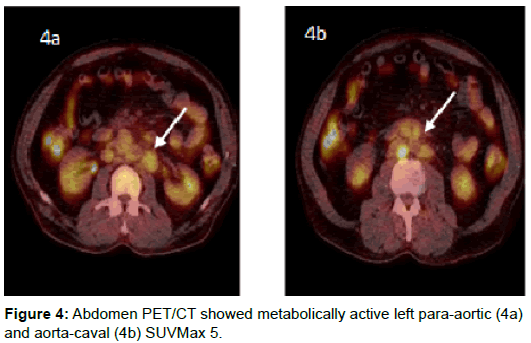
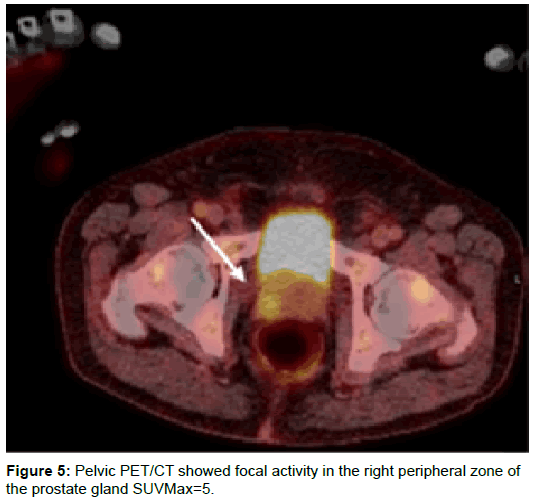
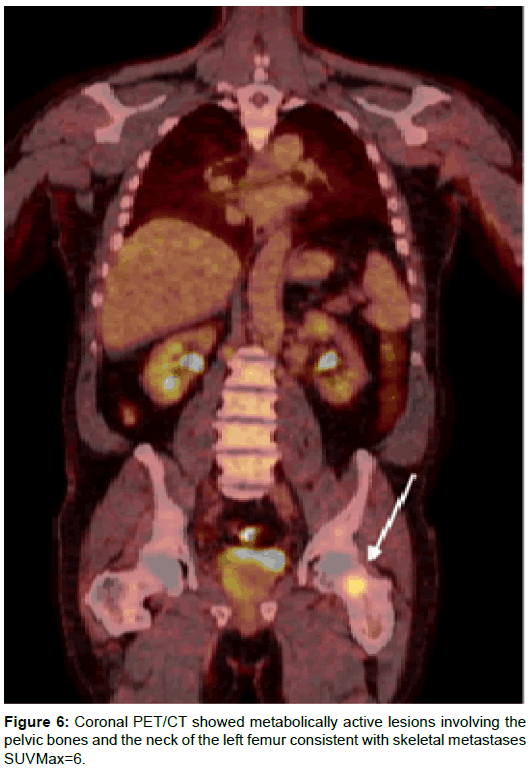
At this point, a diagnosis of Lymphoma was suggested. A PET-CT was performed at the same time as the biopsy results were still pending. Images showed the presence of metabolically active left supraclavicular fossa nodes, of which, the most prominent one showing a standardized uptake value (SUVMax 4) (Figure 3) and metabolically active left para-aortic and aortocaval nodes (SUVMax 5) (Figures 4a and 4b). In addition, the PET-CT scan showed a focal activity in the right peripheral zone of the prostate gland (SUVMax 5) (Figure 5) along with metabolically active lesions involving the pelvic bones and the neck of the left femur consistent with skeletal metastases (SUVMax=6) (Figure 6).
Figure 7 shows the prostatic adenocarcinoma in the biopsy of the left supraclavicular lymph node. A subsequent digital rectal examination revealed enlarged prostate gland with palpable nodularity. Biochemistry blood tests were unremarkable except for a serum Prostate Specific Antigen (PSA) of 18 mg/ml [4].
Discussion
The aggressiveness of prostate cancer varies from low-risk tumours associated with slow progression to high-risk tumours with quick metastasis outside the prostate gland. Most prostate cancers spread locally and regionally to lymph nodes and bones [5]. The vast majority of prostate cancers are detected in the early stages of the disease; thus, the cure rate is very high. Despite that, a considerable percentage does not present until late in the disease course when the cancer spreads distally such as a supraclavicular lymph node [6].
Lymphatic spread is key determinant of Gleason score namely one of the main tools used to calculate the pathological stage of prostate cancer [7]. Migration of the cancerous cells typically follows step-wise progression starting in regional lymph nodes (obturator and pelvic) to the retroperitoneal space then cyterna chyli and lastly the thoracic duct where the lymphatic system enters the systemic circulation via the left subclavian vein. Anatomically, left cervical nodes are closely related to the entry of the thoracic duct into the left subclavian vein which drains to the left jugular trunk. Retrograde lymphatic spread appears to be the likely mechanism of metastases to left supraclavicular nodes [8].
Butler et al. were among the first researchers who studied supraclavicular lymphadenopathy as the initial presentation of previously unrecognized prostate cancer. 18 of the 19 cases they reported had left supraclavicular lymphadenopathy as the initial manifestation of prostate adenocarcinoma. Histological examination of this group was found trivially worse than those presenting at the early non-metastatic stages [9,10]. This makes the current prognostic markers of the disease relatively unreliable.
Neck lymphadenopathies are frequently associated with local invasion from regional primary cancers and occasionally from breast, kidney or lung tumors. Prostate cancer is seldom considered a differential diagnosis when a supraclavicular node involvement is the initial manifestation of the disease. As such, prostate cancer patients presenting with left supraclavicular node (Virchow’s node) or the scarcer presentation of the right supraclavicular node-only one single case has been reported in literature [10] are only recognized when histological evidence is confirmed following a biopsy of those nodes.
As a result, high index of suspicion is key to recognize unusual presentation of prostate cancer like clinical supraclavicular lymphadenopathy. This is particularly crucial when other markers like Prostate-specific-antigen PSA and prostate special staining are relatively inconclusive which renders the systemic spread of the disease unlikely.
Conclusion
A number of case reports studied the atypical presentation of prostate cancer with single or generalized lymphadenopathy with occasional absence of other indicators of prostate cancer [3,4,10]. Surprisingly, it is still a commonly an overlooked picture of the disease, which can potentially lead to a considerable diagnostic and therapeutic delay. Although metastatic prostate carcinoma of the supraclavicular nodes is rare, this case emphasizes the importance of considering prostate carcinoma in the differential diagnosis of men presenting with supraclavicular lymphadenopathy.
References
- Catalona W, Richie J, Ahmann F, Hudson M, Scardino P, et al. (1994) Comparison of digital rectal examination and serum prostate specific antigen in the early detection of prostate cancer: results of a multicenter clinical trial of 6,630 men. J Urol 151: 1283-1290.
- Saitoh H, Yoshida K, Uchijima Y, Kobayashi N, Suwata J, et al. (1990) Two different lymph node metastatic patterns of a prostatic cancer. Cancer 65: 1843-1846.
- Ozgur A, Ilker Y, Turkeri LN (2003) Cervical lymph node enlargement on the right side as the initial manifestation of metastatic prostate cancer. Arch Esp Urol 56: 859-861.
- Hematpour K, Bennett C, Rogers D, Head C (2006) Supraclavicular lymph node: incidence of unsuspected metastatic prostate cancer. Eur Arch Otorhinolaryngol 263: 872-874.
- López F, Rodrigo J, Silver C, Haigentz M, Bishop J, et al. (2015) Cervical lymph node metastases from remote primary tumour sites. Head Neck 38: E2374-E2385.
- Epstein JI (2007) Pathology of prostatic neoplasia. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds.)Campbell-Walsh Urology(9th edn.) Philadelphia. WB Saunders, pp: 2874-2875.
- Montironi R, Mazzuccheli R, Scarpelli M, Lopez-Beltran A, Fellegara G, et al. (2005) Gleason grading of prostate cancer in needle biopsies or radical prostatectomy specimens: contemporary approach, current clinical significance and sources of pathology discrepancies. BJU Int 95: 1146-1152.
- Cellini N1, Luzi S, Mantini G, Mattiucci GC, Morganti AG, et al. (2003) Lymphatic drainage and CTV in carcinoma of the prostate. Rays 28: 337-341.
- Marley J (2007) Campbell-Walsh Urology (9th edn.). In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds.) Int J Urol Nurs 1: 94-95.
- Butler JJ, Howe C, Johnson D (1971) Enlargement of the supraclavicular lymph nodes as the initial sign of prostatic carcinoma. Cancer 27: 1055-1063.
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 4220
- [From(publication date):
August-2017 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 3370
- PDF downloads : 850