Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
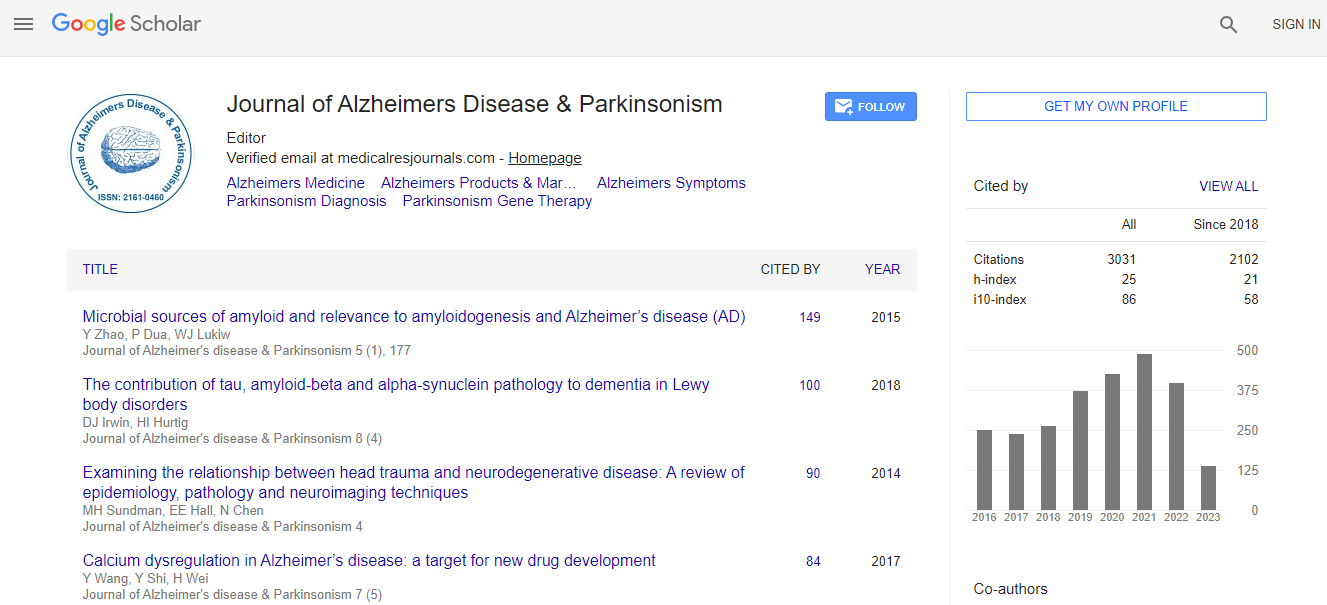
Google Scholar citation report
Citations : 4334
Journal of Alzheimers Disease & Parkinsonism received 4334 citations as per Google Scholar report
Journal of Alzheimers Disease & Parkinsonism peer review process verified at publons
Indexed In
- Index Copernicus
- Google Scholar
- Sherpa Romeo
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- China National Knowledge Infrastructure (CNKI)
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Alzheimer disease biomarkers: Facing the complexity
8th International Conference on Dementia and Dementia Care
Panteleimon Giannakopoulos
University of Geneva, Switzerland
Keynote: J Alzheimers Dis Parkinsonism
Abstract
Early clinic-pathological studies demonstrated that the two cardinal lesions associated with Alzheimer disease (AD), neurofibrillary tangles (NFT) and amyloid deposits, have a differential impact on cognition both at early and late stages of the neurodegenerative process. In contrast to �?�?-amyloid (A�?�?) deposition that occurs diffusely in the human brain over 60 years of age, NFT formation follows hierarchical schemes of regional and cellular vulnerability affecting first the entorhinal cortex and parahippocampal formation before moving in adjacent neocortical association areas. Long before the emergence of novel imaging techniques, it was clear that A�?�? deposits correlate very weekly with cognition and downstream neurodegenerative biomarkers. In contrast, NFT and associated synaptic loss is strictly related to the loss of cognitive functions not only at late but also at early stages of AD. The last decade was characterized by the exponential increase of knowledge in the field of AD predictive biomarkers and, most importantly, characterization of tracers for �?�?-amyloid (A�?�?). It is now widely acknowledged that amyloid deposits in positron emission tomography (PET) with Pittsburg compound B (PiB; a marker of A�?�? fibrillar deposits) precede dementia by 5-10 years, and PiB burden inversely correlates with concentration of A�?�?42 in the cerebro-spinal fluid. However, increased PiB burden was reported in nearly 20% to 30% of controls in the general population pointing to the fact that A�?�? deposition is not sufficient to cause cognitive decline in AD. Moreover, the rate of A�?�? accumulation is not related to neurodegeneration at baseline and only 8% of controls display both decreased hippocampal volume and increased PiB signal. According to Jack��?s model, all of the aforementioned markers become positive well before dementia onset, and the ones related to amyloid pathology already reach their plateau at the time of first cognitive deficits. More recently, selective tau tracers became available for clinical research. Although a PiB equivalent is not yet ready for tau imaging, the recent development of tau tracers with higher selectivity, reduced non-specific binding and improved tracer kinetics compared to the first molecules raise increasing expectations among the scientific community. Given the tight association between tau deposition, cognition and neurodegeneration, and unlike A�?�? imaging, tau imaging will be essential for assessing disease progression. Furthermore, they may help to resolve the controversy about the temporal sequence of tau pathology in AD. The new diagnostic criteria by Dubois and collaborators consider that the development of tau pathology, at least under its fibrillar forms, is a late phenomenon in AD dependent, at least partly, on the A�?�? deposition in prodromal states. Recent contributions showed that tau-related markers (but also structural MRI changes) might become positive in the absence of PiB deposits mainly in preclinical cases. Ultimately, tau imaging will provide the tool to change the landscape and explore whether or not presymptomatic administration of anti-A�?�? therapy impacts on the progression of tau pathology that determines the clinical expression of AD.Biography
Panteleimon Giannakopoulos was born in 1965 in Greece. He obtained his MD degree in the University of Athens in 1989 before completing a full training on psychiatry and psychotherapy in London (Maudsley Hospital and Geneva) as well as postdoc training in Paris (La Pitié-Sâlpetrière Hospital, Federation of Neurology). In 1998, aged 33 years, he has been appointed as associate professor and medical head of the Division of Geriatric Psychiatry of the University Hospitals of Geneva. Later on (2004) he obtained the position of full tenured professor of Psychiatry in the University of Geneva. From 2003 to 2011, he also assumed a parallel position of full professor of Old Age Psychiatry in the University of Lausanne in order to promote the academic careers of junior staff locally. He has been Chairman of the Department of Mental Health and Psychiatry in Geneva for ten years (2005-2015) and vice dean of the Faculty of Medicine in the University of Geneva in charge of postgraduate and continuous education (2003-2011). From December 1st 2015, he is the medical head of the forensic psychiatry development in Geneva country. Specialist of Alzheimer disease research, he published more than 240 peer-reviewed articles in the field of neurobiology of aging with particular focus on predictive biomarkers of cognitive decline.

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi