Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
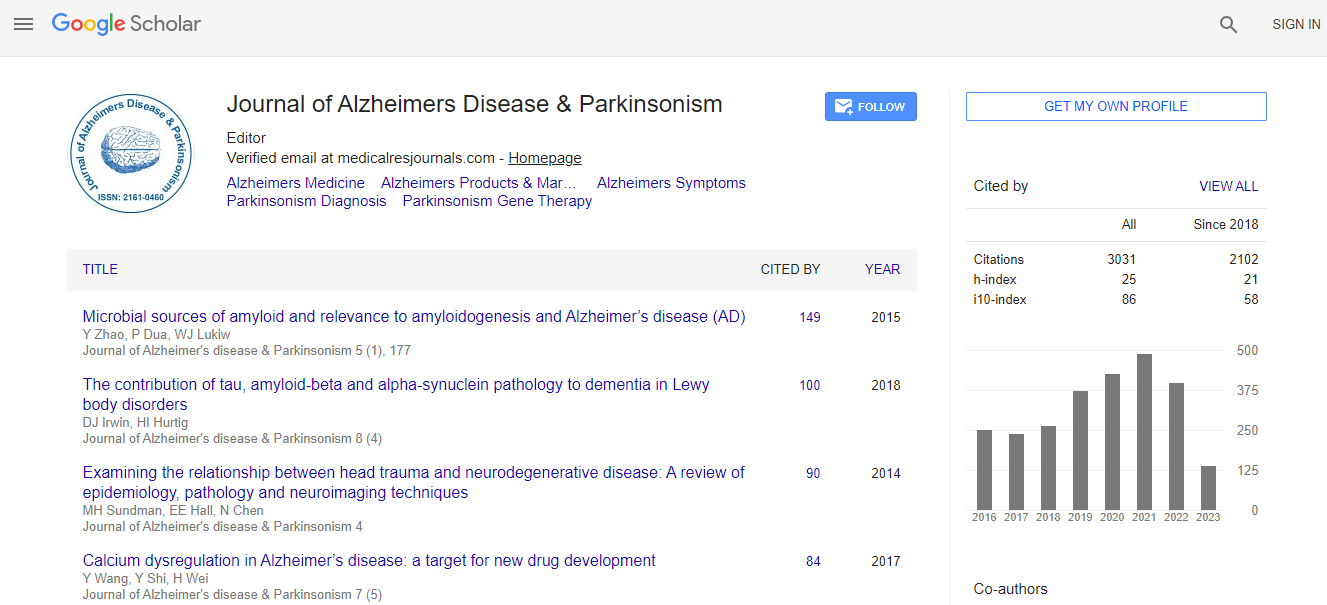
Google Scholar citation report
Citations : 4334
Journal of Alzheimers Disease & Parkinsonism received 4334 citations as per Google Scholar report
Journal of Alzheimers Disease & Parkinsonism peer review process verified at publons
Indexed In
- Index Copernicus
- Google Scholar
- Sherpa Romeo
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- China National Knowledge Infrastructure (CNKI)
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Sleep apnea is a risk factor for cognitive decline of vascular origin
4th International Conference on Vascular Dementia
Antonio Culebras
SUNY Upstate Medical University, USA
Keynote: J Alzheimers Dis Parkinsonism
Abstract
Clinical evidence suggests that moderate to severe obstructive sleep apnea (OSA) is a risk factor for development of vascular cognitive impairment as a result of cerebral subcortical small vessel disease expressed as leukoaraiosis and silent infarctions. A recent study showed that old women with OSA AHI>15 were more likely to develop cognitive impairment (AOR, 1.85; [95% (CI), 1.11-3.08]. Other authors have shown that. OSA AHI>15 is a risk factor for cerebral white matter changes in middle-aged and older patients (OR:2.08 [95% (CI):1.05-4.13]) and for silent cerebral infarction in > 65 y/o patients (OR:2.44 [95% (CI):1.03-5.80]). Intermittent nocturnal hypoxia in patients with moderate to severe OSA contributes to ischemic damage in the cerebral periventricular territory of long penetrating terminal arteries. Blood flow may be already precarious as a result of diabetic vascular autonomic dysregulation and poorly controlled hypertension. Ischemic damage to the cerebral periventricular white matter disturbs the connections of the cortex with the thalamus leading to subcortical dementia characterized by apathy, decreased executive functions, poor memory and in later difficulty walking and urinary incontinence. Treatment of OSA with CPAP may lower cerebrovascular risk by decreasing 24-h urinary catecholamine excretion, improving arterial stiffness, improving baroreflex sensitivity and reducing mean 24-h ambulatory blood pressure. CPAP applications may delay onset of dementia. However, CPAP applications will not modify structural lesions of the brain and therefore early diagnosis and treatment of sleep apnea before structural brain damage ensues is strongly recommended, particularly in patients with several risk factors for stroke.Biography
Antonio Culebras is a Professor of Neurology, SUNY Upstate Medical University, and consultant in the Sleep Center of Upstate Medical University, Syracuse, New York. He is Certified by the American Board of Psychiatry and Neurology and received his Doctorate of Medicine (PhD equivalent) from the University of Alicante, Spain. He is Certified by the American Board of Psychiatry and Neurology, Sleep Medicine. He has lectured in English and Spanish in over 40 countries. He has published 7 books on sleep disorders, co-edited 2 books on cerebrovascular disease, published over 200 articles in professional journals, and has served or serves in the editorial board of 15 national and international neurological publications.
Email: aculebras@aol.com

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi