Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
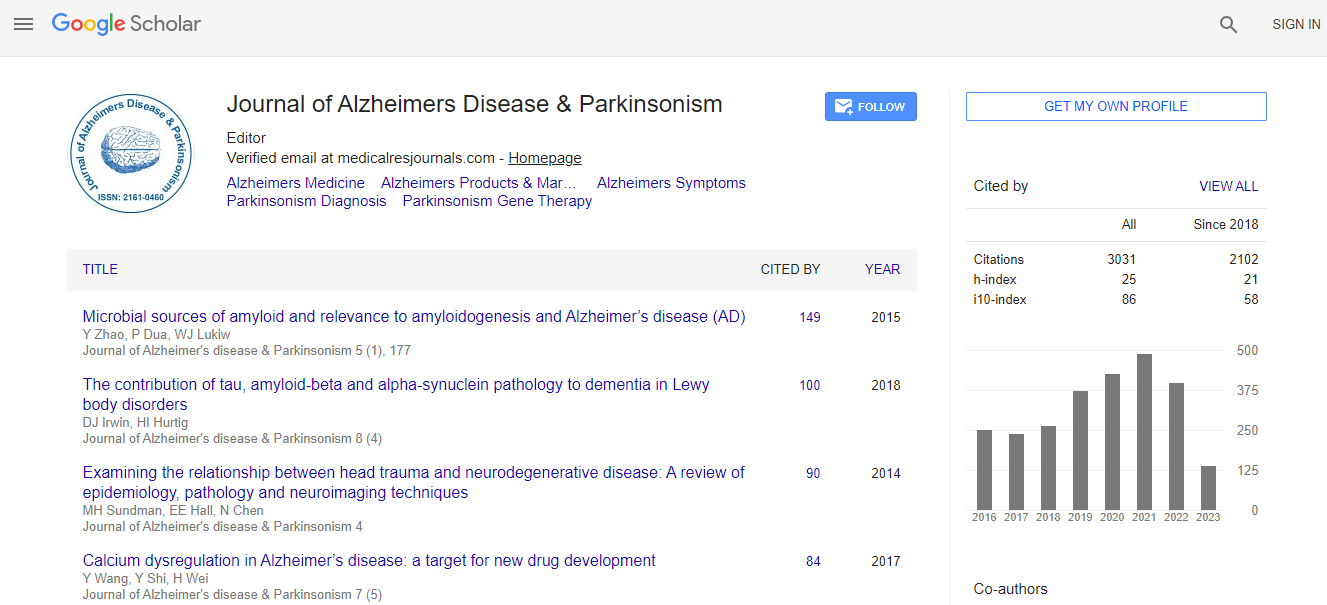
Google Scholar citation report
Citations : 4334
Journal of Alzheimers Disease & Parkinsonism received 4334 citations as per Google Scholar report
Journal of Alzheimers Disease & Parkinsonism peer review process verified at publons
Indexed In
- Index Copernicus
- Google Scholar
- Sherpa Romeo
- Open J Gate
- Genamics JournalSeek
- Academic Keys
- JournalTOCs
- China National Knowledge Infrastructure (CNKI)
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- SWB online catalog
- Virtual Library of Biology (vifabio)
- Publons
- Geneva Foundation for Medical Education and Research
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
The development of a multicellular three dimensional neurovascular unit model with a functional blood- brain barrier
5th International Conference on Parkinson’s disease and Movement Disorders
Goodwell Nzou
Wake Forest School of Medicine, USA
ScientificTracks Abstracts: J Alzheimers Dis Parkinsonism
Abstract
Increased cerebrovascular permeability due to the blood-brain barrier (BBB) disruption is known for destabilizing brain homeostasis, neuronal function and nutritional distribution in brain tissue. The BBB controls these functions through a dynamic structure of tight junctions and adherent junctions formed mainly between endothelial cells. The integral selectivity characteristic of the BBB limits therapeutic options for many neurologic diseases and disorders. Currently, very little is known about the mechanisms that govern the dynamic nature of BBB. To date, most in vitro models only utilize endothelial cells, pericytes, and astrocytes. These models neglect the role of other cell types in the brain cortex such as the neurons, microglia, and oligodendrocytes. Thus, we seek to create a 3D spheroid model of the blood-brain barrier consisting of all major cell types that closely recapitulate normal human brain tissue. Spheroids containing 6 cell types were maintained in static culture with growth media exchange every other day and were fixed in 4% formaldehyde and Immunohistochemistry was performed for TJ, AJ and cell-specific markers. Our data demonstrate the expression of TJs and AJs. Furthermore, our data on BBB functionality assessment using MPTP, MPP+ and mercury chloride in our spheroids indicate charge selectivity through the barrier. Our spheroid model would have applications in drug discovery and neurotoxicity and cytotoxicity testing. This model can serve as a tool for individualized, patient-specific blood-brain barrier disease models through the use of representative cell types derived from induced pluripotent stem cells (iPSCs).Biography
Goodwell Nzou, born and raised in a small, remote village in Zimbabwe near the Mozambique border, Goodwell jokingly credits the snakebite to which he lost his right leg and led him to “escape the crude village life” and to move to the city where he continued school with much bigger goals that he would have ever imagined in the village. With a Bachelor of Science in Chemistry from Nazareth College and now studying molecular medicine, he has an unwavering commitment to playing a role in improving health standards in underserved communities after he completes doctoral studies at Wake Forest University.
E-mail: gnzou@wakehealth.edu

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi