Research Article Open Access
Barriers and Facilitators to Chronic Non-cancer Pain Management in Primary Care: A Qualitative Analysis of Primary Care Providers' Experiences and Attitudes
Elizabeth Lincoln L1,2*, Linda Pellico3, Robert Kerns2,4,5 and Daren Anderson61Department of Medicine, Yale University School of Medicine, USA
2VA Connecticut Health Care System, USA
3Yale University School of Nursing, USA
4Department of Psychiatry and Neurology, Yale University School of Medicine, USA
5Department of Psychology, Yale University, USA
6Community Health Center Inc., USA
- *Corresponding Author:
- Elizabeth Lincoln L
Instructor, Department of Medicine
Harvard Medical School
Massachusetts General Hospital 55 Fruit St
Yawkey 4B, Suite 4700 Boston, MA 02114, USA
Tel: 203-752-6168
E-mail: llincoln2@partners.org
Received date: February 25, 2013; Accepted date: March 08, 2013; Published date: March 11, 2013
Citation: Lincoln LE, Pellico L, Kerns R, Anderson D (2013) Barriers and Facilitators to Chronic Non-cancer Pain Management in Primary Care: A Qualitative Analysis of Primary Care Providers’ Experiences and Attitudes. J Palliative Care Med S3:001. doi:10.4172/2165-7386.S3-001
Copyright: © 2013 Lincoln LE, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Palliative Care & Medicine
Keywords
Primary care; Chronic pain; Pain management; Primary care providers; Ambulatory care
Introduction
Pain and effective pain care are among the most critical health issues facing Americans. In 2011, the Institute of Medicine reported that about one-third of all Americans experience persistent pain at an annual cost of as much as $635 billion in medical treatment and lost productivity. The report noted that military veterans are an especially vulnerable group, with data documenting a particularly high prevalence of pain and extraordinary rates of complexity associated with multiple medical and mental health comorbidities [1].
Pain is the most common symptom reported by patients receiving care in primary care, accounting for up to 40% of all visits to primary care providers (PCPs) [2]. More than half of all patients who have Chronic Non-Cancer Pain (CNCP) receive their care primarily from PCPs [3]. Estimates suggest that as many as 50% of male veterans and up to 75% of female veterans seen in Veteran’s Health Administration (VHA) primary care settings report the presence of pain [4-6]. More recent data suggest that the prevalence of CNCP, particularly painful musculoskeletal disorders including chronic low back pain, is increasing annually [7]. Cost effective strategies that improve the management of CNCP in the primary care setting are needed to address the challenges posed by this public health crisis.
The VHA has implemented a Stepped Care Model for Pain Management (SCM-PM) as a national pain care strategy to meet the needs of veterans [8]. The SCM-PM provides for effective assessment and treatment of pain within primary care whenever possible, with the capacity to escalate treatment options to include specialized care and interdisciplinary approaches, if needed. Critical to the success of the SCM-PM is the ability of PCPs and multidisciplinary primary care teams to effectively access and manage most common pain conditions. The SCM-PM is similar to that advocated by the American Academy of Pain Medicine [9], and it was cited by the Institute of Medicine as a potentially important model of care for persons with CNCP [1].
Unfortunately, the literature suggests that PCPs do not feel adequately prepared to take on the role of frontline providers for patients with CNCP. Although several studies have described PCPs’ attitudes and barriers to prescribing opioids for CNCP [10-14], few studies provide a broad overview of CNCP management from a provider’s perspective. Previous surveys have shown that PCPs have concerns about the prescribing of opioids and are fearful of contributing to addiction. In addition, PCPs note the deficiency in primary care education and training in pain management, and question their capacity to provide optimal pain care [15-19]. Limitations of this research include the fact that some of these studies targeted subsets of the broader population of primary care patients with CNCP such as patients having high rates of opioid utilization or addiction, or included providers other than PCPs. More information is particularly needed about the experiences and attitudes of PCPs serving the population of veterans. There are even fewer studies using qualitative analysis [17,19,20]. Qualitative research offers a method of inquiry that values the identification of the human experience related to a phenomenon of interest and may provide a more complete understanding of PCPs’ attitudes and experiences about pain management. Interestingly, to our knowledge, no study has specifically inquired about the positive aspects of pain management. While we know about some of the barriers to pain care, there is relatively little information about factors that providers feel facilitate the care of patients with chronic pain other than opioid agreements and a strong therapeutic doctor-patient alliance [17,20].
Our objective in conducting this study was to further describe the context of CNCP management in primary care by exploring PCPs’ experiences and viewpoints of barriers and facilitators using qualitative analysis. We expected that the findings would highlight important opportunities for improving the quality of chronic pain management in primary care not previously identified. This study was part of a larger research project to improve the care of veterans with chronic pain at the VA Connecticut Healthcare System (VACHS) and its findings will be used to promote knowledge uptake and inform system-wide improvements in pain management across the VHA.
Methods
Setting
The primary care section of the VACHS provides medical care to 46,000 veterans. Primary care is provided by PCPs in two large academic medical centers and six community based practices. Comprehensive specialty care is available to all VACHS patients. Patients have access to pain specialists who perform consultations and procedures, as well as to an interdisciplinary pain center.
Sample
All PCPs (N=60) were invited to participate in the study by completing a three item open response survey and a fifty item knowledge questionnaire. Only results of the open response survey are reported here. Forty-five PCPs participated, for a return rate of 75%. Respondents were 60% female and 40% male, with 40 Attending Physicians, four Advanced Practice Registered Nurses (APRNs), and one Physician Assistant (PA). Academic faculty numbered 26. Average time in practice since graduation from training was 17 years. On average, approximately five percent of each provider’s panel of patients was being treated with prescription opioid medication.
Design
Survey questions were formed based upon current research findings, overall aims of the study, and researchers’ experience treating patients with chronic pain. This study was reviewed and approved by the VACHS Human Studies Subcommittee, and the Yale University School of Medicine Institutional Review Board. A waiver of written informed consent was approved. All PCPs in the VACHS were provided with a study information sheet and a paper copy of the three survey questions. Open-ended questions were selected for this survey because this tactic offers a less biased approach rather than forced participant responses and it facilitates spontaneity from respondents [21]. Participants were recruited at practice meetings, via mailings, and e-mail. Non-respondents were contacted again through e-mail by one of the study staff. Study questions were:
1. Describe some barriers that you feel limit your ability to manage chronic pain.
2. Can you describe some of the positive aspects related to caring for patients with chronic pain?
3. What are some of the negative aspects about caring for patients with chronic pain?
The PCPs’ written comments were typed verbatim into an excel spread sheet and verified as accurate by comparing them to the original survey data. Respondents’ comments totaled nearly 3000 words; individual comments ranged from one word (“time”) to 55 words (average, 11 words). Rather than code responses by each survey question, all data were merged in order to comprehend meaning in its entirety without losing connections between the three survey probes.
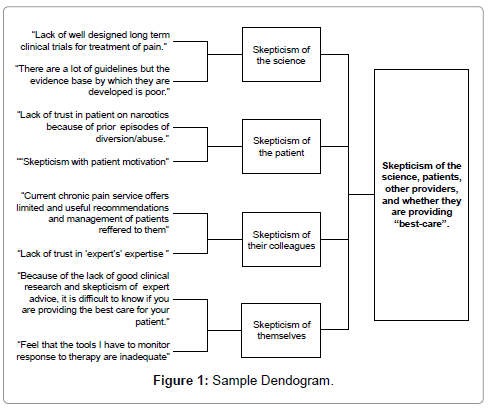
Three of the four authors read the aggregated comments in entirety and inductively coded the comments. An inductive approach was used to analyze the data since there is fragmented knowledge related to the phenomenon of PCPs’ experience with CNCP using qualitative methodology [22]. In inductive coding, the text progresses from specific to general, so that individual instances are discerned and then related into a larger whole that describes the phenomenon of interest. Content analysis using Krippendorff’s method [23] was used to identify repetitive themes. Coding consisted of the authors separately selecting exact words, passages, or sentences, noting unique comments as well as recurrent passages related to the research questions. Data were grouped according to Krippendorff’s analytical technique of clustering to identify phrases and sentences that shared some characteristics. As an example, statements such as “suspicion,” “lack of trust in the experts’ expertise,” and “many comfortable patients state their pain score is 10” were categorized as skepticism. Dendrograms, or tree-like diagrams, were then created to illustrate how data collapsed into clusters. An example of a dendogram is presented in figure 1.
Authors consisted of a multidisciplinary team including a qualitative nurse researcher, two primary care providers, and a pain psychologist. The authors met frequently to discuss selection of passages, text characteristics, and the transcripts were discussed line by line. Coding among the researchers was reconciled to represent consensus about the meaning of participant comments, and the construction of themes was established by group consensus. An audit trail was created to record personal reflections and to provide plausible interpretation and evidence of consistency with the original data set. The audit trail was shared with all authors. In addition, numerous participant quotes were included in the results to enhance the credibility of our findings.
Results
Eleven themes were identified. The themes are artificially organized into three domains as a taxonomy in which the reader can consider the inter-relationships of the themes. They are: System, Personal/ Professional, and Interpersonal domains. Two of the eleven themes interrelate across the three domains and therefore are described separately.
Systems domain
The systems domain consists of two themes: inadequacies in medical education and health care system structure.
Theme One: Inadequacies of training: Studies have shown that PCPs report a lack of knowledge, education, and training in pain management [16,18,19,24] especially in the area of opioid prescribing. Our study describes similar perceptions. In particular, respondents were described to be ill-equipped to manage opioids in complex patients with co-occurring addiction and behavioral health problems.
“Lack of training in difference in efficacy/safety of different pain treatments”
“Limited familiarity with maximum doses of medications and when to switch to LA preparations”
“Managing opioids in many of the patients who have substance abuse and other psychological issues”
Results of our study provide additional insight into specific areas where providers lack competence. These areas include certain physical exam skills and maneuvers, when to order an imaging study, when to refer to specialty care, how to choose between various treatments, and tools to use to monitor response to therapy.
“inadequate training to perform types of physical exams necessary to identify A) cause of pain (which muscle, tendon, etc.), B) rule out malingering, C) correlate physical exam with MRI and other imaging”
(difficulty) “Exploring both surgical (neurosurgical for back), psychological (behavioral), physical therapy options in a rational and responsible manner” “not always clear when surgery/interventional options are appropriate”
Theme two: Health care systems structure: Respondents identified barriers in our organizations that decrease efficiency of practice and result in increased PCP workload. Some structural issues cited by providers are unique to the VA setting, including formulary restrictions, a prohibition against accessing state prescription monitoring programs, the requirement to handwrite opioid prescriptions, and the challenge of communicating with other providers outside the VA [barriers include the] “inability to prescribe pain medications that might be costly without referral to pain management” “incredible time it takes to contact outside providers who are prescribing opioid narcotics in patients who are comanaged”
An additional issue more common to other primary care settings includes the challenge of coordinating opioid refills and urine drug testing, and limited ancillary staff to assist with this process. Other structural barriers refer to “limited access to pain medicine specialists,” restricted pain clinic hours, and lack of convenient location for CNCP patients “not enough ancillary staff for observed urines” “limited availability/convenience because of distance to physical therapy, other adjunctive services for some patients”. Providers’ comments suggest a desire for more administrative and systems assistance both to help them manage patients clinically and for coordinating the care of complex patients.
“Lack of support group to manage patients with chronic pain on narcotics”
“No forum to discuss challenging patients with specialists on a regular basis”
“difficulty in coordinating treatment modalities –e.g. Physical therapy (infrastructure); system is poorly designed for patients with complex chronic pain disorders “Uniform protocols, i.e., “uniform prescribing and follow-up” were viewed as positive system features that facilitate management aspects such as prescribing and monitoring of patients on opioids.
Personal/Professional domain
The personal/professional domain consists of four themes that reflect the daily practice of PCPs managing patients with CNCP, and the impact of this work on them as individuals and clinicians.
Theme three: Clinical quandaries: The clinical quandaries PCPs face daily relate to “diagnostic dilemmas” and difficulties managing patients with CNCP who have multiple co-morbidities, and “so many disease processes to manage.” Their comments note that “many patients have contraindications to most non-opioid pain alternatives (especially the elderly),” which adds to the complexity of care management. As a result, PCPs “fear (they are) missing something.” The PCPs’ comments detail that many of their patients with CNCP have comorbid mental health disorders, which triggers a concern whether patients were using opioids to treat their mental health or substance abuse problems. A “lack of objective findings (unclear the cause of pain in many instances)” only seems to heighten this concern. PCPs also describe quandaries such as “deciphering issues of abuse, misuse, and/or diversion,” “inheriting patients on chronic opiates because (they were) unhappy with previous providers” and “managing patients expectations with pain control.” “High prevalence of substance abuse and psychiatric disease in veterans” “tendency in some patients to ease psychosocial problems (with opioids) and difficulty teasing this out from pain”, “ability to localize nature of pain (especially individuals on chronic opioids without radiographic evidence of pathology or severe pathology).”
Theme four: The challenge: A particularly interesting theme emerged in which the challenges of solving difficult diagnostic or management problems in chronic pain were viewed as intellectually stimulating and satisfying. “Challenges to look further in obtaining a correct diagnosis”, “challenges me to think outside the box”, “ego gratification involved in dealing with or even resolving difficult problems”, others found the challenge of providing holistic care for patients to be gratifying.
“Enjoy the challenge in attempting to meet the needs of the patient, not only his/her physical but psychosocial as well.”
Additionally, clinicians noted that chronic pain care helped them develop keener interpersonal and other communication skills.
“Challenges to communicate effectively a therapeutic plan with patient, it teaches empathy and builds patience and endurance.”
Theme five: The rewards of healing: Many PCPs commented on the emotionally rewarding association of witnessing successful pain care with “improvements in patient function and mood,” “improved quality of life,” and “return to work,” with benefits accrued beyond “the patient, to the family and society” as a whole. Providers felt personally rewarded in “helping (patients) when they are in real discomfort,” “empathizing with a suffering person,” and PCPs “appreciated long term relationships” with patients. The fact that “some patients are very gratified when you provide relief of their pain” was personally “satisfying.” The “avoidance of long term narcotic use (with chronic pain managed)” was also viewed as a positive outcome that left PCPs with a sense of reward.
Theme six: Provider frustrations: Provider frustrations related to the complexity of CNCP management and their inability to control the patient’s pain. Their ineffectiveness ultimately impacts the providers’ sense of efficacy and self-image.
“Frustration and apathy develop over time as well as hopelessness in the provider and resentment toward the patient.”
“Poor long term success with maintaining pain control. Sense can never win-will never fully relieve pain or satisfy patient.”
“Frustration at inability to help patients with pain feel better. Whatever you do is never enough and it makes the MD feel inadequate and mean for not keeping the patient pain- free.”
Interpersonal domain
The interpersonal domain consists of three themes that cluster around the dyad relationships of provider and provider or patient and provider.
Theme seven: Provider-provider relationships: A lack of quality specialty services was identified frequently as a barrier to CNCP management. Issues detailed by PCPs included consults being “rejected” and a lack of collaboration and “ownership” by specialists for patients. Complaints about lack of effective support were especially prevalent for the pain consultants but extended to many disciplines involved in pain management including orthopedics, rheumatology, neurosurgery, and substance abuse. Comments suggest that PCPs believed the onus for caring for patients with chronic pain rested on their shoulders. In this study, the quality of consultations seemed to be more of a concern for PCPs than issues of access as found in other studies [17,25-27].
“…they (pain specialty) spend a lot of time rejecting consults and turfing back to primary care”
“Pain specialists do not take ownership of the patient”
“Current chronic pain service offers limited and useful recommendations and management of patients referred to them”
Interestingly, given that opioids have become among the most prescribed medications in the U.S. [28], some providers commented that a deficiency in consultative services led to a personal overreliance on pharmacologic therapy, particularly opioids.
“I work with female patients who often have complex pain syndromes. Our system is poorly designed to handle these patients. They seem to fall through the cracks-when referred…… my own bag of tricks is limited to counseling and pain medications.”
However, the availability of complementary and alternative medicine resources, such as chiropractic and acupuncture services, and the availability of a “multidisciplinary team approach” were highlighted as facilitators of effective CNCP management which leads to a positive collegial relationship among providers.
Theme eight: Antagonistic patient-provider interactions: Troubling or unpleasant encounters between PCPs and some patients with chronic pain were noted in this study. In such encounters, patients were described as “dishonest”, “manipulative”, “angry”, “aggressive”, “explosive” and “abusive” in the context of opioid use. While similar findings have been previously described [20], our respondents also highlighted the unwillingness of patients to accept non-pharmacologic modes of treatment, particularly behavioral health interventions as an additional dissatisfying element of such interactions. PCPs noted what they perceive to be patients’ unrealistic expectations to be “painfree”. These encounters lead to a sense of exasperation observed in the comments of the PCP and set the stage for antagonistic providerpatient relationships.
“Patients tend to be problematic, ill, demanding, manipulative, and even dishonest”
“Patient resistance to PT/CBT (physical therapy/cognitive behavior therapy) - ‘just want a pill’”
“Difference between patient expectations in pain relief and actual pain relief obtainable with multiple complex pain regimens”
Theme nine: Enjoyable patient-provider interaction: Providers experienced satisfaction in creating long-term relationships with patients who had chronic pain. Their comments describe a shift from an acute model of care and traditional role of primary decision maker to a chronic model of collaborative shared partnership between patient and provider, which is viewed as enjoyable. The chronicity of CNCP allowed for the building of stronger relationships and comments detail that some providers formulate positive attitudes that encourage the effective and compassionate treatment of CNCP.
“Reward of working together with patient, to achieve goals”
“If you can enter a collaborative working relationship it can be positive”
(positive aspect is) “Forming an alliance with patient to meet shared goals”
“I actually enjoy working with chronic pain patients. They are difficult and as such don’t often feel validated by some providers. (particularly specialty clinics, etc.). I find that the patients often benefit from an empathetic ear … and I experience some reward from being able at least to empathize, validate, usually medicate, and counsel.”
Theme ten: Skepticism: The notion of skepticism traversed all three domains (system, personal/professional, and interpersonal). Respondents expressed skepticism towards the science of pain management, the usefulness of consultants’ advice, their personal delivery of “best practice,” and patients’ motivation and participation. PCPs expressed doubt in the quality of evidence in the field of pain management. Comments suggest that participants question the rigor of clinical trials and clinical practice guidelines. Many PCPs felt that many recommended treatment modalities were ineffective in their patient population. In addition, the inability to access the state prescription monitoring database, a VA-specific prohibition, prevented PCPs from investigating their suspicions that some patients were receiving opioids from other community providers. PCPs’ comments also expressed a lack of trust in pain specialists further enhanced by a perception that many recommended treatment plans were ineffective in improving patient outcomes. Respondents also expressed concern about cross covering other providers’ patients, noting that “patients are on strange combinations of multiple short and long pain medications.” An additional factor contributing to the theme of suspicion is what respondents referred to as the “subjective nature of pain” and the lack of objective measures to corroborate complaints of pain. Respondents expressed skepticism about the numeric one to ten scale used to assess pain, noting “many comfortable patients state their pain score is 10.” Finally, PCPs’ comments reveal skepticism of patients’ motivation and commitment to adhere to a plan of care. They were suspicious of patients whom they felt may have secondary gain motives. PCPs expressed mistrust of patients who might be diverting or abusing opioids and those whom they felt were receiving opioids from multiple providers. Providers reported this as a barrier since it led to the loss of a trusting relationship. Refer to the dendrogram (Figure 1) for specific supporting comments.
Theme eleven: Lack of time: Time pressure was a theme that was found in the system, personal/professional, and interpersonal domains. Providers’ describe busy office visits without enough time to address all the issues, limited appointment availability for specialty clinics and resultant long wait times, and burdensome, time-consuming prescription refill activities. They report that patients with chronic pain often required more time than other visits and also needed more frequent visits overall compared with other patients. This perception that CNCP patients on opioids have a higher number of clinic visits is supported by the literature [29,30]. PCPs also noted that patients with pain generate more non-visit work such as coordination of care and frequent medication refills, which result in an increased workload for PCPs and staff. Addressing pain in the context of a primary care visit sometimes resulted in neglecting other non-pain related conditions. As noted by PCPs, “there are so many other disease processes to manage,” that “there is not enough time to really think critically.” They also note that time pressure impacts negatively on their ability to care for other patients as well. Additionally, patients “demanding to be seen between appointments,” and “pestering” the PCP and staff are considered both “time consuming and energy consuming.”
“Time; Office visits are so compressed as it is; it’s difficult to spend appropriate time assessing change in function, emotional aspects which feed into pain, etc.”
“Time; ideally should be seeing these folks more often than we have time for”
“…. large amount of time spent on phone, in person, outside of usual office visit”
“It takes away time from other patients”
“Frequent walk ins and phone calls and interruptions while in clinic seeing other patients, patients can be challenging, demanding, come in between appointments, demand to be seen.”
Discussion
This study provided a rich and descriptive picture of providers’ experiences and viewpoints about chronic pain management in primary care. Through the application of a rigorous and structured qualitative method, Krippendorf’s method, we were able to identify and elaborate three distinct, yet overlapping, domains, namely System, Personal/Professional, and Interpersonal, that may provide an important framework that can be employed to inform the development and enactment of quality improvement efforts. The findings describe the context of pain care in primary care settings and point out the challenges of providing care to persons with CNCP that must be addressed to meet the needs of this vulnerable population. Importantly, we also identified themes that characterize perceived positive aspects of this work that may serve as incentives for engaging in quality improvement efforts.
Across the three domains, multiple barriers of caring for persons with CNCP were identified. System factors included inadequacy of education and deficient competencies to assess and manage even common chronic pain conditions, as well as organizational barriers that impede the enactment of even well- developed comprehensive treatment plans. A second primary domain focused on Personal and Professional factors that are associated with the provision of optimal pain care. Themes highlighted the complexity of managing pain in persons with multiple comorbidities, especially mental health and substance use disorders, and both the clinical quandaries that are commonly confronted and the pervasive experience of frustration that accompanies these challenges. The third domain that was isolated via the analyses relates to the interpersonal aspects of pain care, including challenging issues related to share care among PCPs and specialists as well as difficult aspects of provider – patient interactions. The identification of multiple specific themes within this domain may help to better isolate targets for improvement.
The fact that primary care providers find pain management challenging, is not a new observation. Studies have shown that PCPs harbor significantly negative feelings about pain care [15,20] and feel unable to meet the needs of patients with CNCP [15-19]. Our study, however, provides a rich and more nuanced picture of what primary care providers feel about the topic and adds more detail, with important observations that can help guide future improvement activities. In addition, the significant positive elements about pain care expressed by providers in this study suggest a real opportunity to address the underlying problems and convert pain care into a satisfying aspect of primary care practice.
However, the challenges outlined in this study will need to be addressed. Providers need training and support in opioid management, physical diagnosis, and a broader understanding of the role of nonpharmacologic interventions. Providers need better communication and coordination of care with pain specialists and a stronger collaboration with specialists to ensure that accountability is clarified and consults are appropriate. Improving partnerships with specialists and access to specialty care for primary care patients is part of the Stepped Care Model advocated by the American Academy of Pain Medicine [9] and an important element of a new initiative in VHA called SCAN-ECHO (Specialty Care Access Network- Extension of Community Healthcare Outcomes). In SCAN-ECHO, specialists provide ongoing case based learning and collaborative, consultative care via videoconferencing to PCPs in remote settings in order to support the development of competencies in pain assessment and management. Another support being trialed at the VHA are electronic consults, which provide answers to specific questions posed by PCPs without a visit encounter, by various specialists including pain specialists.
The primary care team including nurses, medical assistants, and receptionists, needs to work together to address the increased work load that patients with pain entail and to develop efficient work flows to manage administrative issues such as opioid agreements, urine toxicology monitoring, and telephone communication. The Patient Centered Medical Home model calls for a collaborative, team-based approach to primary care [31]. Many of the systems issues cited in this study could be improved through more effective use of a health care team. The use of nurse care coordinators to provide support for patients with chronic pain has been shown to improve patient satisfaction and pain scores [32-34]. Opioid renewal clinics can improve pain care by assigning dedicated staff to manage the opioid prescription and monitoring process for high risk patients [35]. Other collaborative and interdisciplinary approaches may help with the management of patients with complex psychosocial and behavioral issues. Chronic pain is prevalent in two-thirds of patients with major depressive illness [36,37]. Optimizing depression in a primary care setting with the assistance of a mental health liaison improves pain levels [38,39]. Efforts to integrate mental health care into primary care as is practiced at the VHA should be expanded.
One particularly frequent theme that appeared in our study and that of Matthias et al. was that of the challenging, antagonistic patient encounter [20]. The physician-patient relationship is predicated on trust, communication, and a patient centered partnership in which the patient and provider work together towards a common aim. Comments from this study suggest that such relationships often are compromised by suspicion and lack of trust and that antagonism, frustration, and even nihilism often pervade the encounter. In pain care, differing expectations between patients and PCPs are common [40,41]. Lack of concordance between patient and physician goals may contribute many of the negative feelings about pain care expressed by study respondents. This aspect of pain care needs to be addressed specifically. Primary care providers need training in how to handle challenging and unpleasant encounters and need to acquire tools, many of which are more commonly employed by behavioral health staff, to manage these negative emotions and better handle difficult encounters to improve the likelihood of a positive outcome.
Our institution has piloted a peer support intervention for PCPs who may be experiencing tension in the relationship with an individual patient with chronic pain. In this model, PCPs can present their experience to a committee that includes PCPs who are knowledgeable in pain care, a behavioral health provider, and an addictions specialist. PCPs are able to share their frustrations, receive emotional support, and are also assisted in developing a specific plan of care. Occasionally, members of the committee will meet with the PCP and patient together, to help facilitate understanding and defuse tension. Preliminary feedback of this process from PCPs has been highly positive.
The positive factors identified in this study that facilitate CNCP care in the primary care setting are of equal interest and have been less described in the literature. They largely encompassed humanistic, altruistic and relational aspects of caring for an individual with chronic pain. Positive relationships can contribute to provider satisfaction in CNCP management [17,20]. Enhancing patient-centered skills in the context of shared decision making may improve the experience of providers and patients. Training providers in empathy, a positive aspect of pain care cited in this study, may be especially helpful in CNCP care [42,43]. Novel approaches to training providers and medical students in shared decision making and affective skills improves provider satisfaction, relationships, and interest in caring for patients with pain [44,45]. Providers described feeling rewarded when they were able to alleviate suffering and provide comfort to patients, and see them regain functionality and have improved well-being.
Additional facilitators to CNCP care included the intellectual satisfaction of solving difficult diagnostic, management, and communication problems. Having universal protocols in place, the availability of complementary and alternative medicine resources, especially chiropractic services, and multidisciplinary care of complex patients were other promoters of successful pain care.
Skepticism among PCPs about the science of pain management is another interesting finding from this study that merits further attention. PCPs suggested that pain management guidelines were not supported by robust clinical evidence noting in particular the lack of strong evidence for the efficacy and safety of opioids for the management of long term CNCP [46]. PCPs may find it beneficial to have access to practice algorithms for specific syndromes and symptom complexes. Such an approach to management may help to resolve some of the uncertainties around the need for imaging tests and in deciding which pharmacologic and non-pharmacologic treatment options to consider for individual patients.
This study had several limitations. The sample size, consisting of PCPs from one VA medical system, was small. However, our high response rate, the varied clinical settings, and the detailed nature of the responses suggest that we were able to capture a broadly representative picture for a VHA health system that includes academic and non-academic sites, and large as well as smaller community based practices. Additionally, 100% of the providers surveyed were primary care providers. Most providers served male veterans, limiting the generalizability to female patients and non-veterans. A distracting factor may have been the increased complexity of primary care patients in the VHA setting. We used written survey data, which limited our capacity to further explore participant responses. Additionally, there is concern that participants with either strong positive or negative opinions may take the time to respond to the survey while participants with neutral positions may not respond. Therefore, valuable observations may not be available for interpretation.
Conclusion
Findings from our study should help to inform efforts to improve the management of CNCP in primary care. Pain care gets limited attention in medical training and in research, despite the fact that the prevalence of chronic pain exceeds that of ischemic heart disease and diabetes combined [47]. Given the high prevalence of pain in primary care, chronic pain management should be considered a primary care competency through accreditation and board requirements. The increasing awareness of the problems posed by prescription opioid abuse and diversion, coupled with the recognition that pain is often undertreated in medicine, leaves primary care providers caught in the middle with limited tools and skills. Current practice may be unsustainable, leaving both patients and providers unsatisfied and leading to an overreliance on opioids and a burgeoning prescription drug abuse crisis. Sustained focus on these critical issues is needed to ensure that primary care can continue to place patients at the center of care and do so in a manner that is rewarding and professionally satisfying for the primary care provider.
Acknowledgements
This material is supported in part by the Department of Veterans Affairs, Veterans Health Administration, Office of Research and Development, Health Services Research and Development Service Research Enhancement Award Program (REAP 08-266); a Program for Research Leadership Award from The Patrick and Catherine Weldon Donaghue Medical Research Foundation and Mayday Fund.
References
- Institute of Medicine Consensus Report (2011) Relieving pain in America: a blueprint for transforming prevention, care, education, and research.
- Kroenke K (2003) Patients presenting with somatic complaints: epidemiology, psychiatric comorbidity and management. Int J Methods Psychiatr Res 12: 34-43.
- Breuer B, Cruciani R, Portenoy RK (2010) Pain management by primary care physicians, pain physicians, chiropractors, and acupuncturists: a national survey. South Med J 103: 738-747.
- Kerns RD, Otis J, Rosenberg R, Reid MC (2003) Veterans’ reports of pain and associations with ratings of health, health-risk behaviors, affective distress, and use of the healthcare system. J Rehabil Res Dev 40: 371-379.
- Haskell SG, Heapy A, Reid MC, Papas RK, Kerns RD (2006) The Prevalence and age-related characteristics of pain in a sample of women veterans receiving primary care. J Womens Health (Larchmit) 15: 862-869.
- Crosby FE, Colestro J, Ventura MR, Graham K (2006) Survey of pain among veterans in Western New York. Pain Manag Nurs 7: 12-22.
- Haskell SG, Ning Y, Krebs E, Goulet J, Mattocks K, et al. (2012) The prevalence of painful musculoskeletal conditions in female and male veterans in 7 years after return from deployment in Operation Enduring Freedom/Operation Iraqi Freedom. Clin J Pain 28: 163-167.
- Veterans Health Administration (2009) VHA Directive 2009-053: Pain Management. Washington, DC: Department of Veterans Affairs.
- Dubois MY, Gallagher RM, Lippe PM (2009) Pain Medicine Position Paper. Pain Med 10: 972-1000.
- Hutchinson K, Moreland AM, de C Williams AC, Weinman J, Horne R (2007) Exploring beliefs and practice of opioid prescribing for persistent non-cancer pain by general practitioners. Eur J Pain 11:93-98.
- Potter M, Schafer S, Gonzalez-Mendez E, Gjeltema K, Lopez A, et al. (2001) Opioids for chronic nonmalignant pain. Attitudes and practices of primary care physicians in the UCSF/Stanford collaborative research network. J Fam Pract 50: 145-151.
- Nwokeji ED, Rascati KL, Brown CM, Eisenberg A (2007) Influences of attitudes on family physicians’ willingness to prescribe long-acting opioid analgesics for patients with chronic nonmalignant pain. Clin Ther: 2589-2602.
- Bhamb B, Brown D, Hariharan J, Anderson J, Balousek S, et al. (2006) Survey of select practice behaviors by primary care physicians on the use of opioids for chronic pain. Curr Med Opin 9: 1859-1865.
- Turk DC, Brody MC, Okifuji EA (1994) Physicians’ attitudes and practices regarding the long-term prescribing of opioids for non-cancer pain. Pain 59: 201-208.
- Dobscha SK, Corson K, Flores JA, Tansill EC, Gerrity MS ( 2008) Veterans Affairs primary care clinicians’ attitudes toward chronic pain and correlates of opioid prescribing rates. Pain Med 9: 564-571.
- Upshur CC, Luckmann RS, Savageau JA (2006) Primary care provider concerns about management of chronic pain in community clinic populations. J Gen Intern Med 21: 652-655.
- Barry DT, Irwin KS, Jones ES, Becker WC, Tetrault JM, et al. (2010) Opioids, chronic pain, and addiction in primary care. J Pain 11: 1442-1445.
- Ponte CD, Johnson-Tribino J ( 2005) Attitudes and knowledge about pain: an assessment of West Virginia family physicians. Fam Med 37: 477-480.
- Leverence RR, Williams RL, Potter M, Fernald D, Unverzagt M, et al. (2011) Chronic non-cancer pain: a siren for primary care--a report from the PRImary Care MultiEthnic Network ( PRIME Net). J Am Board Fam Med 24: 551-561.
- Matthias MS, Parpart AL, Nyland KA, Huffman MA, Stubbs DL, et al. (2010) The patient-provider relationship in chronic pain care: provider’s perspectives. Pain Med 11: 1688-1697.
- Niedomysl T, Malmberg B (2009) Do open-ended survey questions on migration motives create coder variability problems? Population, Space, and Place 15: 79-86.
- Elo S, Kyngas H (2008) The qualitative content analysis process. J Adv Nurs 62: 107-115.
- Krippendorf K (2004) Content analysis: an introduction to its methodology. Sage Publications, Inc, California.
- Corrigan C, Desnick L, Marshall S, Bentov N, Rosenblatt RA (2011) What can we learn from first-year medical students' perceptions of pain in the primary care setting? Pain Medicine 12: 1216-1222.
- Vadivelu N, Kombo N, Hines RL (2009) The urgent need for pain management training. Academic Medicine 84: 408.
- Breuer B, Pappagallo M, Tai JY, Portenoy RK (2007) U.S. board-certified pain physician practices: uniformity and census data of their locations. J Pain 8: 244-250.
- The Mayday Fund Special Committee on Pain and the Practice of medicine (2009) A call to revolutionize chronic pain care in America: an opportunity in health care reform.
- Kuehn BM (2009) Opioid prescriptions soar. JAMA 297: 249-251.
- Blyth FM, March LM, Brnabic AJ, Cousins MJ (2004) Chronic pain and frequent use of health care. Pain 111: 51-58
- Buckley D, Calvert J, Lapidus J, Morris C (2010) Chronic Opioid therapy and preventive services in rural primary care: an Oregon rural practice-based research network study. Ann Fam Med 8: 237-244.
- Joint Principles for the Medical Education of Physicians as Preparation for Practice in the Patient-Centered Medical Home (2010).
- Dobscha SK, Corson K, Perrin NA, Hanson GC, Leibowitz RQ, et al. (2009) Collaborative care for chronic pain in primary care: a cluster randomized trial. JAMA 301: 1242-1252.
- Matthias MS, Bair MJ, Nyland KA, Huffman MA, Stubbs DL, et al. (2010) Self-managment support and communication from nurse care managers compared with primary care physicians: a focus group study of patients with chronic musculoskeletal pain. Pain Manag Nurs 11: 26-34.
- Bair MJ, Matthias MS, Nyland KA, Huffman MA, Stubbs DL, et al. (2009) Barriers and facilitators to chronic pain self-management: a qualitative study of primary care patients with comorbid musculoskeletal pain and depression. Pain Med 10: 1280-1290.
- Wiedemer NL, Harden PS, Arndt IO, Gallagher RM (2007) The opioid renewal clinic: a primary care, managed approach to opioid therapy in chronic pain patients at risk for substance abuse. Pain Med 8: 573-584.
- Bair MJ, Robinson RL, Katon W, Kroenke K (2003) Depression and Pain Comorbidity: A Literature Review. Arch Intern Med 163: 2433-2445.
- Arnow BA, Hunkeler Em, Blasey CM, Lee J, Constantino MJ, et al. (2006) Comorbid depression, chronic pain , and disability in primary care. Psychosom Med 68: 262-268.
- Kroenke K, Bair MJ, Damush TM, Wu J, Hoke S, et al. ( 2009) Optimized antidepressant therapy and pain self-management in primary care patients with depression and musculoskeletal pain: a randomized controlled trial. JAMA 301: 2099-2110.
- Kroenke K, Bair M, Damush T, Hoke S, Nicholas G, et al. (2007) Stepped Care for Affective Disorders and Musculoskeletal Pain (SCAMP) study: design and practical implications of an intervention for comorbid pain and depression. Gen Hosp Psychiat 29: 506-517.
- Frantsve LM, Kerns RD (2007) Patient–provider interactions in the management of chronic pain: current findings within the context of shared medical decision making. Pain Med 8: 25-35.
- Parsons S, Harding G, Breen A, Foster N, Pincus T, et al. (2007) The Influence of patients' and primary care practitioners' beliefs and expectations about chronic musculoskeletal pain on the process of care: a systematic review of qualitative studies. Clinical J Pain 23: 91-98.
- Banja JD (2008) Toward a more empathic relationship in pain medicine. Pain Med 9: 1125-1129.
- Gallagher RM (2006) Empathy: a timeless skill for the pain medicine toolbox. Pain Med 7: 213-214.
- Sullivan MD, Leigh J, Gaster B (2006) Brief report: training internists in shared decision making about chronic opioid treatment for noncancer pain. J Gen Intern Med 21: 360-362.
- Murinson BB, Nenortas E, Mayer RS, Mezei L, Kozachik S, et al. (2011) A new program in pain medicine for medical students: integrating core curriculum knowledge with emotional and reflective development. Pain Med 12: 186-195.
- Martell RD, O’Connor PG, Kerns RD, Becker WC, et al. (2007) Systematic Review: opioid treatment for chronic back pain: prevalence, efficacy, and association with addiction. Ann Internal Med 146: 116-127.
- http://www.painmed.org/patient/facts.html%20
Relevant Topics
- Caregiver Support Programs
- End of Life Care
- End-of-Life Communication
- Ethics in Palliative
- Euthanasia
- Family Caregiver
- Geriatric Care
- Holistic Care
- Home Care
- Hospice Care
- Hospice Palliative Care
- Old Age Care
- Palliative Care
- Palliative Care and Euthanasia
- Palliative Care Drugs
- Palliative Care in Oncology
- Palliative Care Medications
- Palliative Care Nursing
- Palliative Medicare
- Palliative Neurology
- Palliative Oncology
- Palliative Psychology
- Palliative Sedation
- Palliative Surgery
- Palliative Treatment
- Pediatric Palliative Care
- Volunteer Palliative Care
Recommended Journals
- Journal of Cardiac and Pulmonary Rehabilitation
- Journal of Community & Public Health Nursing
- Journal of Community & Public Health Nursing
- Journal of Health Care and Prevention
- Journal of Health Care and Prevention
- Journal of Paediatric Medicine & Surgery
- Journal of Paediatric Medicine & Surgery
- Journal of Pain & Relief
- Palliative Care & Medicine
- Journal of Pain & Relief
- Journal of Pediatric Neurological Disorders
- Neonatal and Pediatric Medicine
- Neonatal and Pediatric Medicine
- Neuroscience and Psychiatry: Open Access
- OMICS Journal of Radiology
- The Psychiatrist: Clinical and Therapeutic Journal
Article Tools
Article Usage
- Total views: 16752
- [From(publication date):
specialissue-2013 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 11939
- PDF downloads : 4813