Research Article Open Access
Coaxial Needle Technique for Percutaneous Nephrostomy
| Nishi Mehta1 and Clifford R Weiss2* | |
| 1New York Medical College, School of Medicine, USA | |
| 2Johns Hopkins University, School of Medicine, Department of Radiology, Division of Vascular and Interventional Radiology, USA | |
| Corresponding Author : | Clifford R Weiss The Johns Hopkins University School of Medicine 600 North Wolfe Street/Blalock 544 Baltimore, MD 21287-4010, USA Tel: 410-614-0601 Fax: 410-955-0233 E-mail: cweiss@jhmi.edu |
| Received March 26, 2014; Accepted May 19, 2014; Published May 26, 2014 | |
| Citation: Mehta N, Weiss CR (2014) Coaxial Needle Technique for Percutaneous Nephrostomy. OMICS J Radiol 3:163. doi:10.4172/2167-7964.1000163 | |
| Copyright: © 2014 Mehta N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Purpose: To describe a new coaxial needle technique for percutaneous nephrostomy.
Materials and methods: The technique was performed in six patients where standard ultrasound guidance techniques had failed. A 15 cm, 18 gauge trocar needle was placed adjacent to the renal capsule under ultrasound guidance and a 20 cm, 22 gauge Chiba needle was then placed through the 18-gauge needle to access the renal collecting system.
Results: Successful access into the renal collecting system was achieved in all patients with no complications.
Conclusions: The coaxial needle technique can be used to successfully access the renal collecting system in a manner that is safe and effective.
| Keywords |
| Percutaneous nephrostomy; Coaxial technique; Ultrasound guidance; Hydronephrosis |
| Introduction |
| Renal access for urinary diversion is typically achieved by means of percutaneous nephrostomy. Other indications for percutaneous nephrostomy include treatment of nephrolithiasis and complex urinary tract infections, ureteral intervention, and nephroscopy and ureteroscopy. Typically the kidney is accessed in the avascular plane of Brodel to prevent bleeding complications [1]. Visualization of the collecting system is imperative for successful needle placement and can be performed either using a blind-stick approach with contrast opacification, using intravenous pyelography (IVP) and triangulation, or more commonly using direct ultrasound guidance. Currently, ultrasound guidance is the preferred method because it allows for visualization of both the needle and the targeted collecting system throughout the initial needle placement, without the need for contrast, resulting in more accurate guidance of the needle towards its target and avoidance of critical structures both inside and outside of the kidney [2]. After localization using ultrasound, either an 18- or a 21/22 gauge needle is typically guided into the posterior pole calyx of the kidney. Once the collecting system is accessed, dilation from an 0.018” system to an 0.035” system is performed before the catheter is finally placed [3]. There are times when visualization using ultrasound guidance may fail and reverting back to the blind-stick or IVP method for percutaneous nephrostomy is necessary. Typically this occurs when a patient is obese, edematous, generally echo-unfriendly, or when the ultrasound equipment used provides adequate, but low image quality. |
| The use of either an 18- or a 21/22 gauge needle has its limitations. While an 18 gauge needle is both more easily visualized using ultrasound and is more rigid and controllable, its size also makes it more traumatic to the kidney, and using it for access into the collecting system can cause injury to the kidney or surrounding structures. To prevent these complications many choose a smaller needle (either 21 gauge or 22 guage) for initial access into the collecting system. These smaller, less traumatic needles are safer alternatives to the 18 gauge needle. However, they can be more difficult to control due to their greater flexibility, and they can often be very difficult to visualize using ultrasound, particularly in echo-unfriendly patients or when using older ultrasound machines. This can result in multiple needle passes into or around the kidney before successful entry into the targeted renal collecting system is achieved. This increases both procedure time and risk to the patient [4]. Ultimately, it would be preferable to use a needle-system that is not only safe and controllable, but that is also easily visualized under ultrasound guidance, even when performing percutaneous nephrostomy on echo-unfriendly patients or when using older ultrasound machines that may produce poorer quality images. Therefore, the purpose of this study is to describe and to demonstrate the technique and effectiveness of using a coaxial needle technique for percutaneous nephrostomy. |
| Materials and Methods |
| A coaxial needle technique for percutaneous nephrostomy involves advancing a 15 cm, 18 gauge trocar needle (Cook Medical, Bloomington, IN) using ultrasound guidance, IU22- with a C5-1 Transducer (Philips Healthcare, Bothell, WA), to the desired pole of the kidney and directing it at a calyx without puncturing the kidney capsule. After removing the inner stylet, a 20 cm, 22 gauge Chiba (Cook Medical, Bloomington, IN) needle is then passed coaxially though the 18 gauge trocar and is advanced into the preferred calyx using ultrasound guidance. Urine is then aspirated to confirm entry into the renal collecting system followed by a confirmatory nephrostogram. Following this, standard techniques can then be used for placement of a nephrostomy tube. This coaxial needle technique was performed on six patients undergoing percutaneous nephrostomy after initial attempts using the standard 21/22 gauge needles had failed due to poor visualization under real-time sonographic guidance: |
| Patient 1 was a 69 year-old male with history of bladder cancer with radical cystectomy and neobladder creation. He presented with slight pelviectasis and rising creatinine, as well as urinary tract infection. Multiple initial attempts using a 22 gauge Chiba needle failed because of needle displacement due to significant respiratory motion, however by using a coaxial needle technique, we were able to gain access to the renal collecting system. |
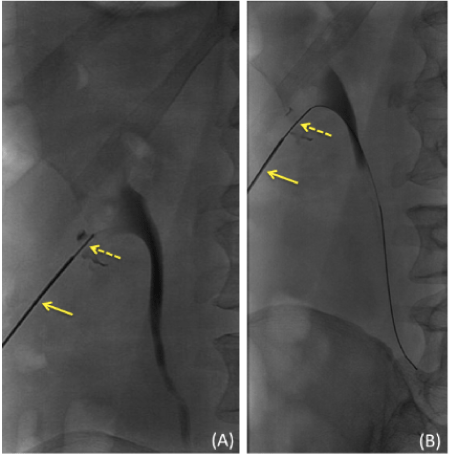
| Patient 2 was a 63 year-old male with history of bladder cancer status post neobladder reconstruction. The patient developed flank pain on the left and underwent nuclear renography read as equivocal for obstruction. The patient’s recent CT demonstrated very miminally dilated central collecting system. Initial attempts at gaining access into the renal collecting system had failed due to poor visualization provided by an older ultrasound machine and therefore a coaxial needle technique was used (Figure 1). |
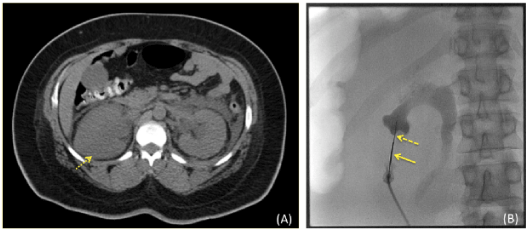
| Patient 3 was a moderately obese 36 year-old female with stage IV cervical cancer and bilateral ureteral obstruction. A coaxial needle technique was used (Figure 2) after multiple initial attempts to gain access into the renal collecting system had failed using a 21 gauge trocar needle. |
| Patient 4 was a 51 year-old female with cervical cancer, status post neoadjuvant chemotherapy and modified radical hysterectomy with bilateral salpingo-oophorectomy, pelvic and para-aortic lymphadenectomy. The patient presented with recurrence and right-sided hydronephrosis. The patient had significant respiratory movement, which led to failed attempts at gaining access using the standard 21-gauge trocar needle under ultrasound guidance. |
| Patient 5 was a 73 year-old male with history of prostate cancer, status post radiation, chronic renal insufficiency, human immunodeficiency virus/acquired immune deficiency syndrome, and diabetes. Patient presented with new moderate left hydronephrosis and mild left hydroureter with UVJ obstruction. |
| Patient 6 was a 51-year-old female with history of cervical cancer status post a modified radical hysterectomy, bilateral salpingooophorectomy, pelvic lymphadenectomy with recurrence and extensive tumor involvement of the bladder. She presented with new onset fever, leukocytosis and new minimal right hydronephrosis. |
| In addition, all of the above patients were echo-unfriendly, therefore necessitating the use of a coaxial needle technique (Figure 3). |
| After a coaxial needle technique was used to gain access into the collecting system of the kidney, a 0.018” Microvena wire (ev3, Plymouth, MN) was advanced through the 22 gauge Chiba needle into the renal collecting system. After removing both needles, dilation from a 0.018” system to a 0.035” system was performed using a Neff or Jeffrey set (Cook Medical, Bloomington, IN) by advancing a sheath over the 0.018” Microvena wire. The 0.018” Microvena wire was then exchanged for a 0.035” Rosen wire. Finally, an 8Fr percutaneous nephrostomy catheter was advanced over the 0.035” Rosen wire into the ureter, and the wire was removed. All four patients successfully recovered from their percutaneous nephrostomy procedure using a coaxial needle technique with no complications. |
| Results |
| In all six patients, a coaxial needle technique was successfully used to gain access into the renal collecting system with subsequent successful percuatenous nephrostomy catheter placement. There were no post-procedural complications. |
| Discussion |
| In this brief report we describe a coaxial needle technique that was successfully used on six patients undergoing percutaneous nephrostomy procedures. A 15 cm, 18 gauge trocar needle and a 20 cm, 22 gauge Chiba needle were used to successfully gain access to the renal collecting system after multiple attempts using the standard 21/22 gauge needle had failed. This technique combines the safety of a 22 gauge needle with the visibility and controllability of an 18 gauge needle in a manner that is safe, with no complications, controllable, and easily visible even under limited ultrasound guidance. This coaxial needle technique is especially useful in teaching situations, allowing the use of an 18 gauge needle without the associated risk of damaging the kidney. It is also useful when performing percutaneous nephrostomy on echo-unfriendly patients or when using older ultrasound machines that may produce poorer visualization. In an effort to better measure the technical success of a coaxial needle technique for percutaneous nephrostomy, a larger patient population should be studied in the future. |
References |
|
Figures at a glance
 |
 |
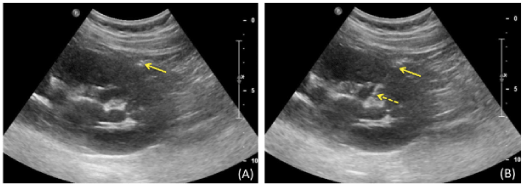 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 18110
- [From(publication date):
September-2014 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 13455
- PDF downloads : 4655
