Case Report Open Access
Isolated Fallopian Tube Torsion: A Case Report and Review of Literature
| Kevin S Baker1*, Ammar A Chaudhry1 and Rajarsi Gupta2 | |
| 1Department of Radiology, Stony Brook University Medical Center, NY, USA | |
| 2Department of Pathology, Stony Brook University Medical Center, NY, USA | |
| Corresponding Author : | Kevin S Baker Department of Radiology Stony Brook University Medical Center Stony Brook, NY 11794, USA E-mail: Kevin.Baker@sbumed.org |
| Received February 27, 2013; Accepted March 08, 2013; Published March 12, 2013 | |
| Citation: Baker KS, Chaudhry AA, Gupta R (2013) Isolated Fallopian Tube Torsion: A Case Report and Review of Literature. OMICS J Radiology. 2:113. doi: 10.4172/2167-7964.1000113 | |
| Copyright: © 2013 Baker KS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Radiology
Abstract
Isolated fallopian tube torsion is a rare cause of pelvic pain in female patients. We present the case of a 10 year old female without significant past medical history who presented with acute left lower quadrant abdominal pain. A CT scan of the abdomen/pelvis showed a dilated, tortuous, fluid-filled structure in the left adnexal region which was ultimately diagnosed as a torsed fallopian tube. Subsequent trans abdominal ultrasound examination documented the fallopian tube’s lack of vascularity with color Doppler and demonstrated thickened, edematous walls and longitudinal folds. The ipsilateral ovary maintained normal vascularity and was unremarkable. The patient underwent laparoscopic salpingectomy, and pathologic examination of the specimen confirmed hemorrhagic fallopian tube necrosis. The patient recovered without complication, and has not experienced any pain recurrence since the procedure.
| Keywords |
| Fallopian tube torsion; Fallopian tube; Torsion; Computed tomography; Ultrasound |
| Abbreviations |
| WBC: White Blood Cell; μl-microliter; CT: Computed Tomography; HU-Hounsfield Units; MRI: Magnetic Resonance Imaging |
| Introduction |
| Isolated fallopian tube torsion is a rare cause of pelvic pain in female patients, and its diagnosis may be elusive when presented with intact ovarian arterial flow on a sonographic examination. We present the case of a 10 year old female who experienced fallopian tube torsion, with documented intact ovarian arterial flow on color and spectral Doppler. A necrotic left fallopian tube was confirmed at surgery. We believe that the presentation of such a case is important, as it provides introduction and concise review of a potential source of acute pelvic pain which the reader may have been unfamiliar with. |
| Case Report |
| A 10 year old female presented to our institution’s emergency department with a 7 hour history of severe left lower quadrant abdominal pain. The patient and her family denied any significant past medical history or hospital admissions. Vital signs were unremarkable at presentation. Laboratory analysis showed a mild leukocytosis (WBC count of 11,200/μl, normal being 4,800-10,800/μl) with a neutrophilic shift (82.0%, normal being 45-70%). Serum chemistry and urinalysis were within normal limits. |
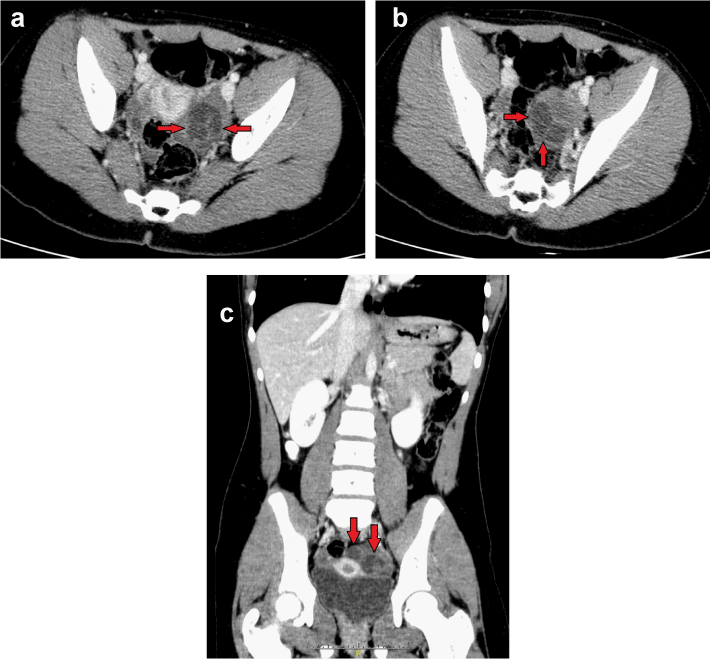
| The patient’s presentation raised clinical suspicion of gastrointestinal pathology, and thus a CT scan of the abdomen/pelvis with oral and intravenous contrast was obtained. The scan showed a tortuous 2.6 (transverse)×2.4 (anteroposterior)×2.1 (craniocaudad) cm hypodensity in the region of the left adnexa (Figures 1a-1c), prompting the recommendation of a pelvic ultrasound. A small amount of pelvic free fluid (with simple fluid attenuation) was also seen in the pelvic cul-de-sac, which was overall physiologic in amount. The right ovary was unremarkable. |
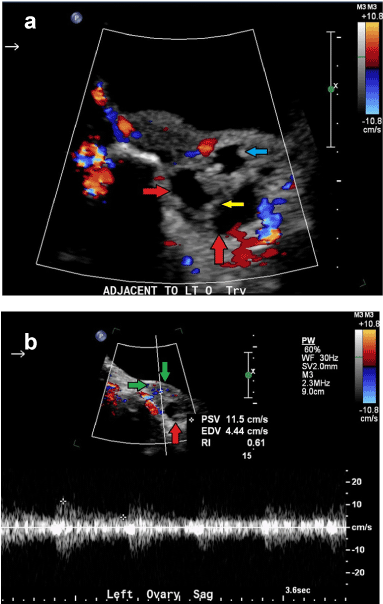
| A transabdominal pelvic ultrasound was then performed for further evaluation of the left adnexa (Figures 2a-2b). An ovoid, heterogeneous structure was seen adjacent to the left ovary with a lack of central vascularity noted upon application of color flow (Figure 2a). The left ovary itself appeared unremarkable and had a normal spectral Doppler arterial waveform (Figure 2b). Given the location of the a vascular, hypoechoic tortuous structure immediately adjacent to the left ovary and the acuity/severity of the patient’s pain, a tentative diagnosis of hydrosalpinx with fallopian tube torsion was made. |
| The patient was taken to the operating room where general anesthesia was administered and orotracheal intubation was performed. The patient then underwent laparoscopy with incisions made at the umbilicus (where a 12 mm trocar was introduced) and bilateral lower quadrants (where 5 mm tro cars were placed). Upon entering the pelvis, a torsed, necrotic, and dilated left fallopian tube was visualized. The fallopian tube was untwisted and subsequently resected. The left ovary appeared normal and was left in place without any fixation measures taken. The right fallopian tube and ovary were unremarkable. The left fallopian tube was sent for pathologic analysis, where microscopic examination confirmed hemorrhagic necrosis. |
| The patient recovered from the surgery well without complication, and was discharged home the next day. She has not experienced any significant pain recurrence or medical problems since the procedure. |
| Discussion |
| Isolated fallopian tube torsion primarily affects adolescents, but can also be seen in older ovulating women, and very rarely in postmenopausal patients. The process was first described in 1890, and is estimated to have an incidence of about one in 1.5 million females [1,2]. Known risk factors include adhesions/endometriosis, hydrosalpinx, pelvic inflammatory disease, trauma, tubal ligation and neoplasm, nearby pelvis masses, and adnexal venous congestion [1]. However, isolated fallopian tube torsion may occur in adolescent females without past medical history or known risk factors (similar to our pre-adolescent patient). Patients will often present with acute lower abdominal/pelvic pain, nausea/vomiting, peritoneal signs, and a possible adnexal mass [1,2]. |
| A proposed mechanism for fallopian tube torsion involves adnexal venous and lymphatic obstruction, causing pelvic congestion and edema with resultant enlargement of the fimbrial end of the fallopian tube, prompting torsion [1,3]. The fallopian tubes and ovaries receive their vascular supply from the ovarian and uterine arteries, and thus it is possible for the fallopian tube to undergo torsion while the ipsilateral ovary maintains normal arterial blood flow. Right sided involvement has been more frequently reported in medical literature, which may due to an increased propensity for surgical exploration in patients with acute right lower quadrant abdominal pain and clinical concern for appendicitis. Others have proposed that the left fallopian tube may be partially immobilized by its proximity to the sigmoid mesentery [1,4]. |
| On ultrasound, a patient with isolated fallopian tube torsion will typically have a dilated, tubular/serpiginous structure with thickened walls and possible internal debris. The torsed fallopian tube itself may mimic a cystic, convoluted adnexal mass with high impedance, reversal, or absence of vascular flow (as in our patient) [1,5-6]. A “beaked” appearance at the site of torsion has also been described [1]. The fallopian tube walls will often be edematous, with prominence and nodularity seen in the longitudinal folds [7]. If the fallopian tube torsion is in fact isolated, then the patient should have an unremarkable appearance of the uterus and bilateral ovaries with normal arterial blood flow. Free fluid may be seen in the pelvis. |
| On CT the torsed fallopian tube may be seen as a twisted, serpiginous adnexal mass. The tube should be dilated, and its wall may be thickened and enhance following intravenous contrast administration. Hemorrhagic luminal contents with attenuation around 50 HU may also be seen if hemorrhagic necrosis has occurred. Secondary inflammatory signs such as pelvic free fluid, broad ligament stranding/thickening, focal ileus, and pelvic free fluid may be present [1,5]. However, the diagnosis can be made on ultrasound alone, and thus in many cases (particularly for pediatric/adolescent patients), the patient may go to laparoscopy without a CT scan being performed. |
| Fallopian tube torsion will be encountered in conjunction with ipsilateral ovarian torsion (“tubo-ovarian torsion”) the majority of the time. The rare nature and nonspecific imaging of isolated fallopian tube torsion make its diagnosis difficult, but the entity should be considered in a patient with a dilated, tubular, hypovascular/avascular adnexal structure, acute lower abdominal/pelvic pain, and normal appearing ovaries on ultrasound. |
| Treatment of isolated ovarian torsion varies on a case by case basis, and depends on the patient’s overall health, the estimated time lapse since onset, and the possible presence of complications. Surgical treatment options include salpingotomy, salpingectomy, and surgical detorsion. A laparoscopic approach is usually preferred [8]. If treatment is delayed, the fallopian tube will likely undergo necrosis and may extend locally, damaging the ipsilateral ovary and resulting in loss of fertility on the affected side. The torsed tube may also become gangrenous and lead to peritonitis if left untreated [8]. Therefore, urgent treatment of these patients is of the utmost importance in order to maximize the chance of salvaging the torsed fallopian tube. |
<References |
|
--
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Relevant Topics
- Abdominal Radiology
- AI in Radiology
- Breast Imaging
- Cardiovascular Radiology
- Chest Radiology
- Clinical Radiology
- CT Imaging
- Diagnostic Radiology
- Emergency Radiology
- Fluoroscopy Radiology
- General Radiology
- Genitourinary Radiology
- Interventional Radiology Techniques
- Mammography
- Minimal Invasive surgery
- Musculoskeletal Radiology
- Neuroradiology
- Neuroradiology Advances
- Oral and Maxillofacial Radiology
- Radiography
- Radiology Imaging
- Surgical Radiology
- Tele Radiology
- Therapeutic Radiology
Recommended Journals
Article Tools
Article Usage
- Total views: 14778
- [From(publication date):
April-2013 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 10191
- PDF downloads : 4587
