Case Report Open Access
Primary Bone Lymphoma Mimicking as Osteomyelitis: An Unusual Presentation
Tarun Kumar Badam*, Sathish Devadoss, Muthukumar Balaji, Annamalai Devadoss and Rajasekharan PN
Institute of Orthopedic Research and Accident Surgery (IORAS), Madurai – 625007, Tamilnadu, India
- *Corresponding Author:
- Tarun Kumar Badam
Junior Resident (DNB Ortho), Institute of Orthopedic Research and Accident Surgery (IORAS)
Devadoss Multi-speciality Hospital, 75/1, Alagarkovil Main Road, Surveyor Colony
Madurai – 625007, Tamilnadu, India
Tel: +917799607409
E-mail: btk_2075@yahoo.com
Received Date: February 19, 2016; Accepted Date: May 07, 2016; Published Date: May 14, 2016
Citation: Badam TK, Devadoss S, Balaji M, Devadoss A, Rajasekharan PN (2016) Primary Bone Lymphoma – Mimicking as Osteomyelitis: An Unusual Presentation. J Orthop Oncol 2:111. doi:10.4172/2472-016X.1000111
Copyright: © 2016 Badam TK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Orthopedic Oncology
Abstract
Primary Bone Lymphoma is a rare disorder, even though secondary involvement of bone marrow in systemic Lymphoma is common. Most of Primary Bone Lymphomas are Primary Bone Diffuse Large B-cell Lymphomas. We describe a case of Primary Bone Lymphoma, initially treated as Osteomyelitis of unknown etiology. This case shows the difficulties that can occur while diagnosing this entity. We provide an overview of Clinical, Radiological, Pathological characteristics of these rare tumours along with review of Literature.
Keywords
Primary bone lymphoma; Primary bone diffuse large b-cell lymphoma; Mimickers of osteomyelitis
Introduction
The clinical presentation of Primary Bone Lymphoma (PBL), a sub-type of NHL can be a challenging diagnosis. Chronic, intermittent pain of a dull aching nature may be the only presenting complaint. In current case, following detailed history, clinical examination, radiological and laboratory studies, patient was presumptively diagnosed with Osteomyelitis. Considering relative and absolute rarity of PBL, the possibility of such a rare occurrence was considered quite low on the list of differential diagnosis.
Lymphoma commonly occurs in the lymph nodes, and extranodal origin is less frequent. Primary Bone Lymphomas (PBL) is rare, even though secondary involvement of bone marrow in systemic lymphoma is common. Primary Bone Lymphoma was first described by Oberling in 1928 [1]. Parker and Jackson reported a PBL series in 1939 [2] under designation reticulum cell sarcoma of bone, establishing PBL as a distinct entity. The lymphoid and B-cell origin was subsequently proved by Immunohistochemistry [3,4].
Primary Bone Lymphomas account for 7% malignant tumours, 4 to 5% of extra-nodal lymphomas and less than 1% of all malignant lymphomas [5,6]. Most PBLs are Primary Bone Diffuse Large B-cell Lymphomas (PBDLBCL) with a rare occurrence of follicular, marginal zone, anaplastic large cell, Hodgkin and T-cell Lymphoma [5].
Case Report
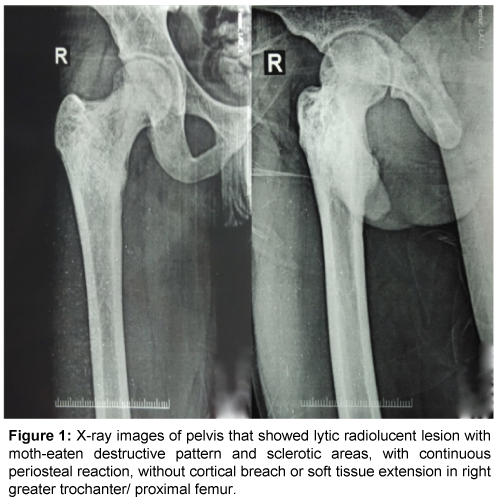
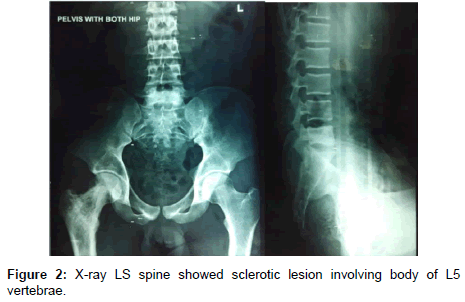
A 18 yr old man complained of progressive pain in the right hip and low back on and off since January 2015. Had episodes of fever on and off. He was treated at various other hospitals with NSAIDS. This treatment relieved some, but not all, of the symptoms. Six months later, the patient presented to the clinic in our department complaining of pain in right hip and low back on weight bearing activities. He had X-ray images of pelvis that showed lytic radiolucent lesion with moth-eaten destructive pattern and sclerotic areas, with continuos periosteal reaction, without cortical breach or soft tissue extension in right greater trochanter/ proximal femur (Figure 1). X-ray LS spine showed sclerotic lesion involving body of L5 vertebrae (Figure 2).
Figure 1: X-ray images of pelvis that showed lytic radiolucent lesion with moth-eaten destructive pattern and sclerotic areas, with continuous periosteal reaction, without cortical breach or soft tissue extension in right greater trochanter/ proximal femur.
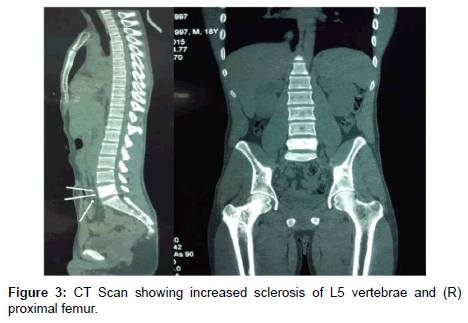
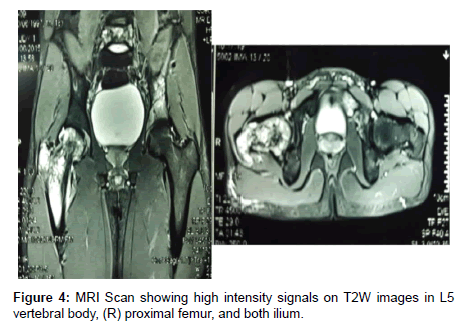
The physical examination at this time revealed some pain on palpation of right greater trochanter and L5 vertebrae. Internal rotation of right hip was restricted and without any other signs of inflammation. Significant laboratory studies included: TWBC 10×103/μl (normal 4.5 -11×103/μl), CRP 2.2 mg/dl (normal 0-1.0 mg/dl), ESR 52/84 mm (normal 1-13 mm/hr), serum Alkaline phosphatase 94 U/L (normal 60- 170 U/L). CT Scan confirmed the X ray findings. MRI Scan was done which showed high intensity signals on T2W images in L5 Vertebral body, (R) Proximal femur, and both Ilium. Due to history, morphology on X-ray, CT scan (Figure 3) and MRI Scan (Figure 4), and Laboratory investigations, Multi-focal Osteomyelitis was suspected. Empirically, patient was started on Antibiotics. No micro-organisms were isolated from cultures of the blood. Patient couldn’t get relief from pain with antibiotics and analgesics.
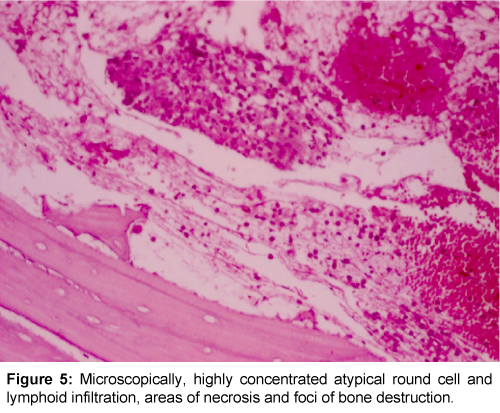
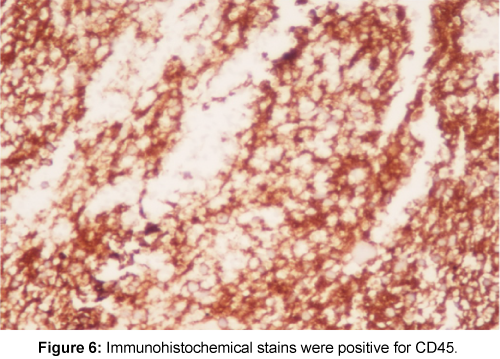
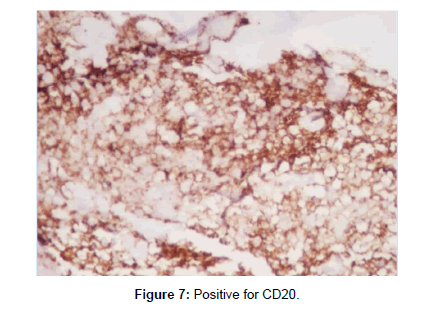
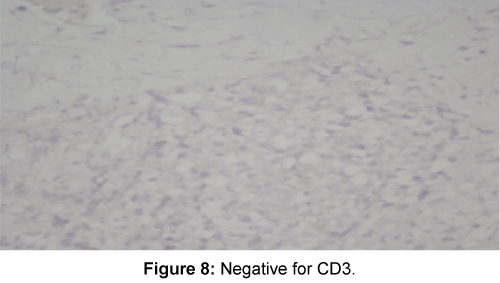
To confirm the diagnosis, Open biopsy of right greater trochanter was done. Grossly, the material consisted of haemorrhagic and highly sclerotic bone specimen. Microscopically, highly concentrated atypical round cell and lymphoid infiltration, areas of necrosis and foci of bone destruction was seen (Figure 5). Immunohistochemical stains were positive for CD45 (Figure 6), CD20 (Figure 7) and negative for CD3 (Figure 8), CD99 and Desmin. Based on these results, the diagnosis of Non-Hogdkins Lymphoma (Diffuse Large B-cell Lymphoma) was made. Ultrasonography of Neck, CT of chest, abdomen and pelvis were done to exclude nodal origin and distant spread, which were negative. Bone marrow aspiration was done and sent for analysis which was negative. Immunohistochemical staining for Ki 67 was done to know the mitotic activity, which was Immunoreactive (75%). Then, a Final diagnosis of Primary Bone Lymphoma – Primary Bone Diffuse Large B-cell Lymphoma (PBDLBCL) was made.
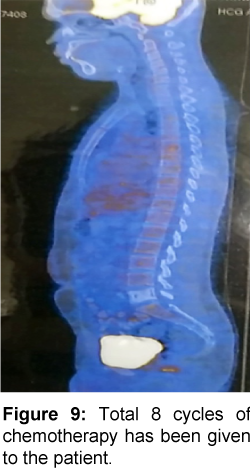
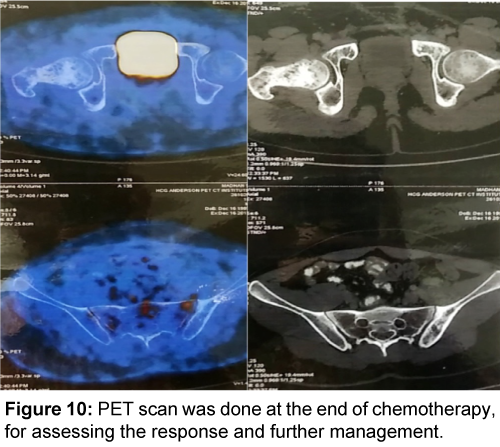
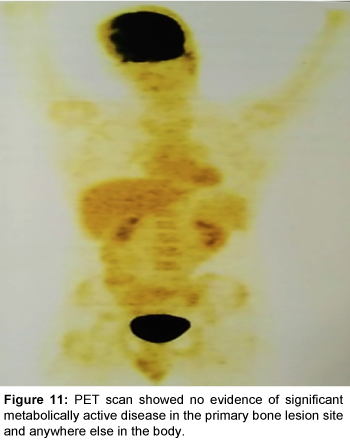
Patient was started on chemotherapy with CHOP-R regimen for 8 cycles. Patient had responded well with 4 cycles of chemotherapy and been pain free after that. Total 8 cycles of chemotherapy has been given to the patient. PET scan was done at the end of chemotherapy, for assessing the response and further management. PET scan showed no evidence of significant metabolically active disease in the primary bone lesion site and anywhere else in the body (Figures 9-11). Patient was given local radiotherapy with a RT dose of 40 Gy for 3 cycles to prevent local recurrence. Patient is on follow-up 4 months post-chemotherapy with 3 more cycles of radiotherapy to undergo. There is no evidence of recurrence to date.
Discussion
The criteria for a diagnosis of Primary Bone Lymphoma was established by Giudici et al. [7] in 1992, (a) on presentation, the patient demonstrates a primary focus in a single bone; (b) histological proof should be obtained from skeletal focus; and (c) the onset of symptoms of primary skeletal lesion should precede the distant metastasis by atleast six months. In 2005, [8] states that following criteria should be met, (a) solitary bone lesion or multiple skeletal lesion with no prior involvement of lymph nodes or other lymphoid tissue; (b) Histological documentation of Lymphoma in the bone; (c) no lymph node involvement or involvement of regional lymph nodes. All of the above criteria were fulfilled in our case.
There are other case reports in literature where Primary bone lymphoma has been misdiagnosed as infection. [9] Published a case series of three lymphomas masquerading as infection, [10] reported three cases of anaplastic large cell bone lymphoma in children of which two appeared as primary tumour, [11] published three cases of PBL treated as Osteomyelitis.
Due to non-specificity of clinical and radiological features, diagnosing this entity is very difficult, without high level of suspicion, the differential diagnosis include Chronic Osteomyelitis, small round cell tumours, Primary bone tumours, Eosinophilic granuloma. Here we reviewed the clinical features, radiological features, gross and microscopic findings, IHC findings, prognosis and treatment of PBDLBCL.
Clinical features
Most commonly affects the middle aged to elderly population. However, it has been described in paediatric patients as well [10,12]. There is male predominance with Male: Female ratio of 1.5:1. The most common presentation of patients with PBDLBCL is bone pain and less frequently by palpable mass and pathological fracture. Very rarely, neurological symptoms such as paraplegia can occur due to cord compression. Systemic symptoms (B-symptoms) such as weight loss, fever, and night sweats are very rare. Rarely, lethargy, constipation, and somnolence can occur due to hypercalcemia [6].
Anatomic location
According to Beal et al. [13], the frequency of different bone involvement was femur (27%), pelvis (15%), tibia/fibula (13%), humerus (12%), spine (9%), other (5%). According to reference [14], femur (34%), humerus (21%), pelvis (17%) and tibia/fibula (17%). In the long bone, preferred site is meta-diaphyseal region. Rarely, small bones of hand and feet are involved.
Radiological features
On X-rays, primary lymphoma of bone have a variable radiographic appearance and lack specificity [15]. Some are lytic and some are sclerotic lesion. But, most of them are lytic radiolucent lesions with moth-eaten or permeative destructive pattern. This may be associated with sclerotic areas. Cortical erosion and soft tissue extension is frequently seen. Periosteal reaction (continuous or interrupted) can be present. In some cases, tumour may evoke a sclerotic response and present as Osteoblastic lesion, which can be mistaken for Pagets disease or Osteoblastic metastasis [16].
Pathological features
Grossly, Soft fleshy gray-white or haemorrhagic appearance with sclerotic bone specimen [5]. Microscopically, diffuse growth pattern with tumour cells permeating between bony trabeculae and invading haversian canals. There is often a sclerotic stroma and tumour cells can invade in nests, cords or solid sheets. PBDLBCL shows a polymorphous appearance. Tumour cells show marked variation in size and shape with multilobulation, that are accompanied with reactive B and T cells. Occasionally, lymphoma shows immunoblastic morphology with round nuclei, prominent nucleoli and abundant amphophilic crystals [17]. Tumour cells may be crushed during biopsy procedure, which may lead to difficulty in diagnosis. Prolonged decalcification may affect cytological features and Immunohistochemical staining [16].
Immuno-histochemical staining
The tumour cells in PBDLBCL are positive for CD45, CD20, CD79a, PAX5 (B cell markers) and negative for CD3 and CD5 (T cell markers). PBDLBCL can be further divided into germinal centre type and non-germinal centre type by using CD10, BCL6, MUM1 antibodies [18] Germinal centre B-cell type has a better prognosis than non-germinal centre B-cell type, even with addition of rituximab [19].
Treatment
Most PBDLBCL are treated with combined radiotherapy and chemotherapy, with good outcome [20]. The radiotherapy dose ranges from 2000-6150 centigrays (cGy) with a median dose of 4400 cGy. Chemotherapy usually consists of CHOP-R (cyclophosphamide, doxorubicin, vincristine, prednisolone with or without rituximab). According to [21], combined chemotherapy is vital in the treatment of PBL. Chemotherapy followed by Radiotherapy is superior in improving overall survival rate. Although chemotherapy was superior to radiotherapy alone, radiotherapy plays a role in local control. Radiotherapy is better in preventing local recurrence when compared to surgical curettage. An RT dose of >40 Gy for 6 cycles and more than 6 chemotherapy cycles are associated with a good outcome.
Prognosis
A study by Beal et al. [13] in 81 patients, 46 patients (56%) received combined therapy, 24 patients (29%) received chemotherapy and 11 patients (13%) received radiotherapy. The 5 yr overall survival rate was 88%. In a study by Cai et al. [22] 3 yr progression free survival in patients who received CHOP-R was 88% compared with 52% for those who received only CHOP. The 5 yr overall survival ranges between 56% and 61%.
Conclusion
Primary Bone Lymphoma is a very rare entity with morphological and radiological heterogenecity. The histological and immunohistochemical similarities, ranging from benign conditions such as Osteomyelitis to small round cell tumours, should be borne in mind while assessing these neoplasms to avoid misdiagnosis and inappropriate treatment. Delays in diagnosis can have serious effects on the prognosis of the disease, in which the stage is considered as most important prognostic indicator [23]. Therefore it is essential to diagnose a lesion prior to leukaemic spread or metastasis. Thus in patients with osteomyelitis like symptoms and bone pain refractory to medical treatment, a thorough diagnostic work-up should be undertaken, and unusual neoplasms such as this haematopoetic malignancy should be considered in differential diagnosis [24].
By reviewing our case and other literature, we have come to the same conclusions as [9]: Surgeons should return to the basics of culturing all suspected tumours and obtaining a biopsy specimen of all presumed infections, even in instances of positive cultures or negative biopsy specimens. Significant worsening of symptoms in chronic osteomyelitis requires thorough work up with appropriate imaging studies, and excision of an additional biopsy specimen.
References
- Oberling C (1928) The reticulum and reticuloendothelio sarcomes bone ( sarcoma D™ Ewing). Bull AssocFr Etude Cancer 17: 259-296.
- Parker F, Jackson H (1939) Primary reticulum cell sarcoma of bone. Surg Gynecol Obstet 68: 45-53.
- Pileri S, Montanari M, Falini B (1990) Malignant lymphoma involving the mandible. Clinical, morphologic and immunohistochemical study of 17 cases. Am J SurgPathol 14: 652-659
- Falini B, Binazzi R, Pileri S, Mori A, Bertoni F, et al. (1988) Large cell lymphoma of bone. A report of three cases of B-cell origin. Histopathology 12: 177-190.
- Unni KK, Hogendoorn PCW, Fletcher CDM, Unni KK, Mertens F (2002) Malignant lymphoma. In Pathology and Genetics of Tumours of Soft Tissue and Bone. Lyon, France: IARC Press; World Health Organization Classification of Tumours 23: 13-27.
- Desai S, Jambhekar NA, Soman CS, Advani SH (1991) Primary lymphoma of bone: a clinicopathologic study of 25 cases reported over 10 years. J SurgOncol 46: 265-269.
- Giudici MA, Eggli KD, Moser RP Jr, Roloff JS, Frauenhoffer EE, et al. (1992) Case report 730. Malignant large cell lymphoma of tibial epiphysis. Skeletal Radiol 21: 260-265.
- Mathur S, Damron T (2002): Malignant Lymphoma.
- Blum YC, Esterhai JL, Esmail AN, Lackman RD, Donthineni-Rao R (2005) Lymphoma masquerading as infection. ClinOrthopRelatRes : 267-271.
- Bakshi NA1 Ross CW, Finn WG, Valdez R, Ruiz R, et al. (2006) ALK-positive anaplastic large cell lymphoma with primary bone involvement in children. Am J ClinPathol 125: 57-63.
- Mika J, Schleicher I, Gerlach U, Adler C (2012) Primary Bone Lymphomas Thought to be Osteomyelitis Urgently demand a Rapid Diagnosis in Bone pathology. Anticancer Research 32: 4905-4912.
- Zhao XF, Young KH, Frank D (2007) Pediatric primary bone lymphomas- diffuse large B-cell lymphoma: morphologic and immunohistochemicalcharac- teristics of 10 cases. Am J ClinPathol127:47-54
- Beal K, Allen L, Yahalom J (2006) Primary bone lymphoma: treatment results and prognostic factors with long-term follow-up of 82 patients. Cancer 106: 2652-2656.
- Demircay E, Hornicek FJ Jr, Mankin HJ, Degroot H 3rd (2013) Malignant lymphoma of bone: a review of 119 patients. ClinOrthopRelat Res 471: 2684-2690.
- Jamie T, Caracciolo, Rose T, Bui MM (2013) Primary Lymphoma of Bone: Imaging Imaging Findings to Improve Diagnosis of a Rarely Considered Disease Prior to Biopsy. Open Journal of Clinical Diagnostics 5: 97-106.
- Unni KK, Inwards CY, Bridge JA, Kindblom L, Wold LE (2005) Tumors of the Bones and Joints Washington. DC: Armed Forces Institute of Pathology 2: 231-240.
- Huebner-Chan D, Fernandes B, Yang G, Lim MS (2001) Animmunophenotypic and molecular study of primary large B-cell lymphoma of bone. Mod Pathol 14: 1000-1007.
- Hans CP, Weisenburger DD, Greiner TC, Gascoyne RD, Delabie J, et al. (2004) Confirmation of the molecular classification of diffuse large B-cell lymphoma by immunohistochemistry using a tissue microarray. Blood 103: 275-282.
- Fu K, Weisenburger DD, Choi WW (2008) Addition of rituximab to standard chemotherapy improves the survival of both the germinal center B-cell-like and non-germinal center B-cell-like subtypes of diffuse large B-cell lymphoma. J Clin Oncol 26:4587-4589.
- Ford DR, Wilson D, Sothi S, Grimer R, Spooner D (2007) Primary bone lymphoma--treatment and outcome. ClinOncol (R CollRadiol) 19: 50-55.
- Cai L, Stauder MC, Zhang YJ, Poortmans P, Li YX, et al. (2012) Early-stage primary bone lymphoma: a retrospective, multicenter Rare Cancer Network (RCN) Study. Int J RadiatOncol Biol Phys 83: 284-291.
- Ramadan KM, Shenkier T, Sehn LH, Gascoyne RD, Connores JM (2007) A clinicopathological retrospective study of 131 patients with primary bone lymphoma: a population-based study of successively treated cohorts from the British Colum- bia Cancer Agency. Ann Oncol18: 129-135.
- Ostrowski ML, Unni KK, Banks PM, Shives TC, Evans RG, et al. (1986) Malignant lymphoma of bone. Cancer 58: 2646-2655.
Relevant Topics
- 3D Printing in Limb-Sparing Surgery
- Adamantinoma
- Aneurysmal Bone Cysts
- Chondrosarcoma
- Chordomas
- Cryosurgery
- Enchondroma
- Ewing’s Sarcoma
- Fibrous Dysplasia
- Giant Cell Tumor of Bone
- Immunotherapy for Osteosarcoma
- Liquid Biopsy in Orthopedic Oncology
- Malignant Osteoid
- Metastatic Bone Cancer
- Molecular Profiling of Bone Tumors
- Multilobular Tumour of Bone
- Orthopaedic Oncology
- Osteocartilaginous Exostosis
- Osteochondrodysplasia
- Osteoma
- Osteonecrosis
- Osteosarcoma
- Primary Bone Tumors
- Sarcoma
- Secondary Bone Tumours
- Targeted Therapy in Bone Sarcomas
- Tumours of Bone
Recommended Journals
Article Tools
Article Usage
- Total views: 18923
- [From(publication date):
June-2016 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 17721
- PDF downloads : 1202