Research Article Open Access
Relationships of Kindergarten Childrens BMI amongst Parental Body Dissatisfaction and Dietary Restraint: A Case Study in Hong Kong
Mok WK1*, Ip TT1, Cheuk R2 and Lau K21Department of Applied Science, Hong Kong Institute of Vocational Education, Vocational Training Council, Hong Kong, China
2Healthy Living Department, Hong Kong Council of Early Childhood Education and Services, Hong Kong, China
- Corresponding Author:
- Dr Mok WK
Lecturer Department of Applied Science
Hong Kong Institute of Vocational Education
Vocational Training Council
20 Hing Shing Road, Kwai Chung
N.T., Hong Kong, China
Tel: +852-261-23855
E-mail: vicmok@vtc.edu.hk
Received Date: July 08, 2015; Accepted Date: August 19, 2015; Published Date: August 23, 2015
Citation: Mok WK, Ip TT, Cheuk R, Lau K (2015) Relationships of Kindergarten Children’s BMI amongst Parental Body Dissatisfaction and Dietary Restraint: A Case Study in Hong Kong. J Community Med Health Educ 5:364. doi:10.4172/2161-0711.1000364
Copyright: © 2015 Mok WK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Community Medicine & Health Education
Abstract
Objective: In this study, the aim was to explore the relationships of kindergarten children’s BMI amongst parental factors such as parental BMI, body dissatisfaction, parental dietary restraint, child weight concern and child weight-focused restrictive feeding.
Method: 466 kindergarten students’ parents were participated in this study. A self-administrated questionnaire was distributed to parents. Independent t-test, one way ANOVA and Pearson’s correlation were performed to analyze the relationships amongst different factors contributing to children’s BMI.
Results: 30% parents and 37% children were found either overweight or obese. The six pathways in the proposed model were all significantly correlated. It was found that parental BMI significantly correlated with body dissatisfaction [r (466)=0.282, p<0.001], which was then associated strongly with parental dietary restraint [r (466)=0.715, p<0.001] and weakly with child weight concern [r (466)=0.146, p=0.002]. The child weight-focused restrictive feeding practice was moderately correlated with both parental dietary restraint [r (466)=0.360, p<0.001] and child weight concern [r (466)=0.320, p<0.001], and then significantly correlated with child BMI [r (466)=0.121, p=0.009].
Conclusion: The results of this study confirmed the presence of upward trend of childhood obesity in Hong Kong. In addition, parental body dissatisfaction was found to be a significant factor to determine parental dietary restraint, which was associated with child weight-focused restrictive feeding and finally affected child BMI.
Keywords
Biochemistry; OSPE; Teaching; Lecturer
Introduction
According to World Health Organization [1], childhood obesity has become a crucial public health challenge in the 21st century, as it is associated with the risk factors for cardiovascular diseases, like high blood pressure or high cholesterol level. Over 60% overweight children aged between 5 and 17 had at least one risk factor for cardiovascular diseases and over 25% had 2 or more [2]. Obese child is found 80% likely to remain obese in adulthood, together with increased risk of morbidity and all-cause mortality, including chronic diseases like coronary heart disease, hypertension, type II diabetes and certain types of cancer [3]. The worldwide prevalence of childhood overweight and obesity had dramatically increased from 4.2% in 1990 to 6.7% in 2010. There were over 43 millions of children estimated to be overweight and obese, as well as over 92 millions of children were at risk of overweight in 2010. In Hong Kong, the prevalence of overweight and obesity in primary school students had significantly increased as well, from 16.4% in 1997 to 21.4% in 2010 [4]. It is foreseeable that the trend will keep increasing and reach 9.1% or 60 million worldwide in 2020 [5]. Regarding the causes of obesity, increased adaption of sedentary lifestyle and insufficient physical activities are the major factors [6]; however, parental influence may also take a vital role to childhood obesity.
Parental influence on child weight change
An early parent child interaction, like parenting and feeding styles are found to be the crucial factors contributing to child weight problems [7]. As parents are the one providing the child’s contextual environment, it is believed that parents influence dietary practices of child by controlling the availability and accessibility of food, as well as the meal structure and eating pattern [8].
Parenting style
Parenting style is defined as the way of interaction with children, in which would alter the effectiveness of parental child feeding practices [9]. There are 4 types of parenting style, differing in the degree of parental responsiveness and parental demandingness. Parental responsiveness means the extent to which parents intentionally foster individuality, self-regulation and self-assertion, while parental demandingness is the demands and willingness of maturity, disciplinary efforts and supervision on children [8]. Among these types, Authoritative Parenting Style is characterized with high level of both parental control and responsiveness to the child’s needs, while Permissive Parenting Style and Neglectful Parenting Style are characterized with low level demand and expectations on the children. It is found that children under Authoritative Parenting Style has lower risk of obesity, probably due to the demand of more healthy dietary practice on children compared to Permissive and Neglectful parents [10].
Child feeding practice
Child feeding practice aims to moderate children’s eating behaviors by a number of behavior strategies, for example, modeling eating behavior for both health and unhealthy food; determining the availability and accessibility of both healthy and unhealthy food; pressuring children for specific food choices; concerning about child’s weight; restricting food intake; rewarding behavior, etc. [9]. Parents are the buffer and filter for the child eating environments, it is believed that child feeding practice may associate with the child weight status [11].
Model linking maternal BMI and child BMI
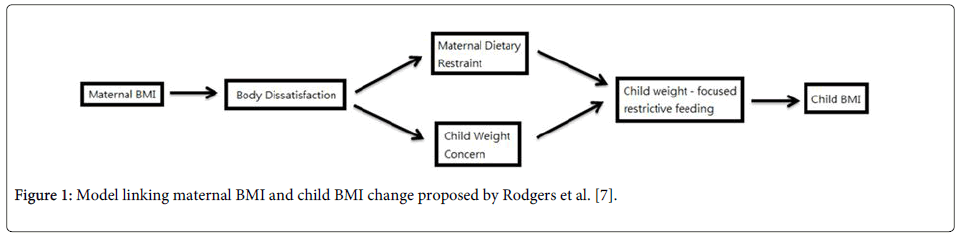
According to the research conducted by Rodgers et al. [7], a model has been proposed to determine the mechanism to predict the child weight gain as shown in Figure 1. In this model, there were six pathways being proposed in total, beginning with the relationship between maternal BMI and body dissatisfaction, then body dissatisfaction to both maternal dietary restraint and child weight concern, followed with child weight-focused restrictive feeding and child BMI change at last. Indirect relationships were obtained amongst maternal BMI, body dissatisfaction and child weight concern, however, the correlation between child weights-focused restrictive feeding practice and child weight concern was found insignificant [7].
Pathway: BMI – body dissatisfaction
Body dissatisfaction is the negative thought of one’s own body, which is developed with a kind of social comparison of body between an ideal body and a current body size [8], including the judgment of appearance, size, shape, weight etc. The association of body mass index and body dissatisfaction had been consistently demonstrated in researches [12-14], in which recent studies had also shown that the increase in BMI can significantly predict the increase in body dissatisfaction in the same period of time [7,13,15].
Pathway: Body dissatisfaction – dietary restraint
Body dissatisfaction was consistently found significantly associated with dieting behaviors [16-18]. Unhealthy dieting behaviors, such as fasting, purging, bingeing might even be developed, resulting in the buildup of eating disorder. In several studies, it was found that body dissatisfaction was consistently correlated with eating disorder in both male and female [19-21]. Dietary Restraint is a type of dieting aiming at weight reduction, as well as maintenance, by restriction of the types and amount of food choice [22]. Correlation between body dissatisfaction and dietary restraint was also found in some researches [7,23].
Pathway: Body dissatisfaction – child weight concern
Apart from dietary restraint, parents with different degrees of body dissatisfaction were found concerning child weight in a different extent [24]. It was found that the concern of child weight increased with the parental BMI, and hence the desire to control child weight. It was believed that parents might implant their own attitude and experience of eating during the feeding interaction with child, as well as the preoccupation of weight and the feeling of body dissatisfaction [25,26]. However, the relationship has not yet well understood as there were some inconsistencies in researches, in which no significant association was obtained with parental weight status [27].
Pathway: Maternal dietary restraint – Child Weight-Focused Restrictive Feeding
Child weight-focused restrictive feeding is a feeding practice, in which parents restrict the types and amount of food eaten by their children for the purpose of weight reduction and maintenance of health [28], in particular the snack food which is high in sugar, salt and fat [24]. Parents, who were dissatisfied with their own body image and might carry dietary restraint, were found associated with a higher usage of child weight-focused restrictive feeding practice [24].
Pathway: Child weight concern – child weight-focused restrictive feeding
Despite maternal dietary restraint, the usage of child weight-focused restrictive feeding was found to be contributed by the concern of child weight. There were some researches showing that the concern of child weight leaded to the desire to control child weight, therefore positively associated with the use of child weight-focused restrictive feeding practice [26,29]. In addition to the relationship, some of the researches have proposed that the concern of child weight mentioned in the association with child weight-focused restrictive feeding practice was not the concern of the child actual BMI weight status, but instead it was suggested to be the concern of the child becoming overweight or obese [30,31].
Pathway: Child weight-focused restrictive feeding – child BMI change
Child weight-focused restrictive feeding practice is supposed to aim at maintaining healthy eating habits and hence controlling child weight. Some researches proposed the association of restrictive feed practice with decreased BMI, in particular in younger children aged 2 to 6 [32,33]. However, the effectiveness of restrictive feeding practice is still in question due to the inconsistent findings.
In contrast to the above hypothesis, there were studies indicating that child weight focused restrictive feeding practice not only failed to control child weight, but also associated with the increase in their BMI [28,34]. Consistent studies were found that the restriction would in turn increase the child’s prevalence and consumption of restricted food [28,35]. It was also proposed that the higher the level of restrictive feeding, the higher is the tendency of overeating by child [36]. It was found that restrictive feeding practice would promote the child’s habit of eating due to desire, but not hunger.
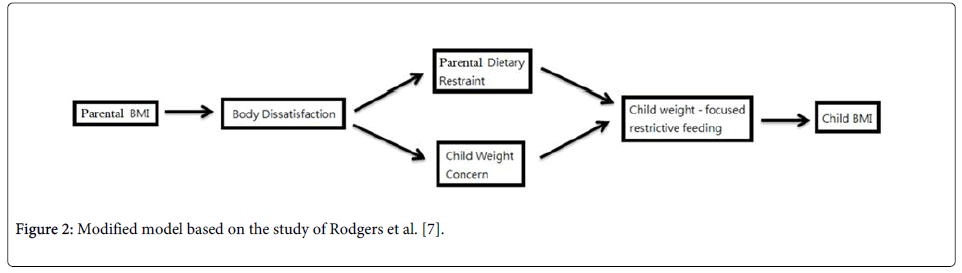
The aim of this study was to explore the factors affecting kindergarten child’s BMI in Hong Kong by application of the model proposed by Rodgers et al. [7], such as the influence of parents own body image perception, eating behavior on children weight concern and type of feeding practice. In this study, the model [7] was slightly modified by replacing the maternal BMI and maternal dietary restraint by parental BMI and parental dietary restraint respectively as shown in Figure 2. The major difference was that the target group shifted from mothers to parents of child.
Materials and Methods
Participants
The current research was carried out during the 2013-2014 academic year. 11 kindergartens in Hong Kong were accepted our invitation to participate in this study. 1860 questionnaires were distributed with 609 questionnaires returned. The response rate was around 33%. Finally, there were 466 questionnaires valid in total.
Procedures
All subjects participated voluntarily. Approval to conduct this study was obtained from Hong Kong Council of Early Childhood Education & Services. Ethical requirements for the collection of personal data of the Institute of Vocational Education were strictly followed. Questionnaires were distributed to parents of kindergarten students in self-administered format through class teachers in February 2014.
Instruments
Questionnaire, consisting of 2 parts, was employed as a mean to measure the behaviors of parents and students. The basic demographic information of parents and child, like gender, age, height, weight, educational level were asked in the first part; and the parental behavior information was questioned in the second part. A pilot test was conducted before the beginning of survey in Feb 2014 to ensure the reliability and accuracy of questionnaire. The pilot test results were fine and acceptable.
Components of the modified model
There were mainly 6 components in the model, consisting parental BMI, body dissatisfaction, parental dietary restraint (PDR), child weight concern (CWC), child weight focused–restrictive feeding (CWFRF) and child BMI.
Parental BMI
Parental BMI was calculated with the self-reported height and weight.
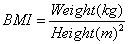
Body dissatisfaction
The five-item Weight Concern subscale of the Eating Disorders Examination Questionnaire [37] had been found valid for assessing body dissatisfaction [7]. Five items including importance of weight, reaction to prescribed weighing, preoccupation with shape or weight, dissatisfaction with weight and desire to lose weight were used to assess the frequency of participants experiencing weight concern in the past 28 days. An example item is “How dissatisfied have you been with your weight?” All the items were answered in frequency scale from +1 (Never) to +7 (Always). The mean of body dissatisfaction was taken for further analysis. In this part, the Cronbach’s α was 0.878.
Parents dietary restraint (PDR)
The frequency of parents engaging dietary restraint in the past 28 days was assessed with the five-item Restraint subscale of the Eating Disorders Examination Questionnaire [37]. Five items including restraint over eating, avoidance of eating, food avoidance, dietary rules and empty stomach were assessed in the frequency scale from +1 (Never) to +7 (Always). An example item is “Have you had a definite desire to have an empty stomach with the aim of influencing your shape or weight?” The mean of dietary restraint was taken for further analysis. The Cronbach’s α was 0.837 for this part.
Child weight concern (CWC)
Parental concern regarding the child weight was determined with the three-item Concern Over Child Weight subscale of the Child Feeding Questionnaire [38] using likert scale ranging from +1 (Not at all concerned) to +7 (Always concerned). The subscale has been demonstrated with good validity and consistency [7,34]. An example item is “How concerned are you about your child having to diet to maintain a desirable weight?” The mean of child weight concern was taken for further analysis. The Cronbach’s α was 0.656 for this section.
Child weight-focused restrictive feeding (CWFRF)
A seven-item Restriction for Weight Control subscale was used to figure out the degree of parents restriction on children to control child weight from Comprehensive Feeding Practices Questionnaire [39], with the likert scale ranging from +1 (Strongly disagree) to +7 (Strongly agree). Restriction subscale from the Comprehensive Feeding Practices Questionnaire was chosen to use instead of the Child Feeding Questionnaire Restriction subscale, not only because of a higher level of internal reliability [7], but also the comprehensiveness and ability to assess the restriction of all types of food. The subscale has been shown to possess good internal reliability and convergent validity in sample of children aged 2-8 years old [39]. An example item is “I often put my child on a diet to control his/her weight.” The mean of child weight-focused restrictive feeding was taken for further analysis. The Cronbach’s α was 0.922 in this section.
Child BMI
The BMI obtained from child would be converted into groups with the adjustment of age and gender according to the population growth reference [40].
Statistical analysis
Statistical software, IBM SPSS Statistics 20, was used for conducting statistical analysis, in which the components of the model were presented with the mean score.
Results
Demographic results
A total of 466 subjects (parents of kindergarten students aged 3 to 6 years old) were investigated, in which 18.9% was male and 81.1% was female. On average, mothers were 33 years old (SD=5.61) and fathers were 39 years old (SD=10.28). Regarding education level, 27.8% and 44.7% of subjects were university graduates and high school graduates respectively as shown in Table 1.
| Frequency (Valid Percentage) | ||
| Gender | Male | 84 (18.9%) |
| Female | 360 (81.1%) | |
| Education Level | ≤Form 3 | 127 (27.5%) |
| Form 4-7 | 206 (44.7%) | |
| Undergraduate | 117 (25.4%) | |
| Postgraduate | 11 (2.4%) |
Table 1: Gender and education level of parents.
Parental weight status
As given in Table 2 in this study, about half (54.7%) of the parents were classified as “Normal”, 16.1% as “overweight”, 9.9% as “obese” and 4.1% as “Severely obese”, while the remaining 15.2% were classified as “underweight”. In comparison with parents as in Table 3 it was found that mothers have better weight control over fathers, as the rate of male being classified as overweight was a double of female, and even 4 times more in the category of obese.
| Count | Cumulative count | |
|---|---|---|
| (Valid Percentage) | (Cumulative percentage) | |
| Underweight | 71 (15.2%) | 71 (15.2%) |
| Normal weight | 255 (54.7%) | 326 (70%) |
| Overweight | 75 (16.1%) | 401 (86.1%) |
| Obese | 46 (9.9%) | 447 (95.9%) |
| Severely obese | 19 (4.1%) | 466 (100%) |
Table 2: Weight status of parents.
| Count(Valid Percentage) | Cumulative count (Cumulative percentage) | |||
|---|---|---|---|---|
| Male | Female | Male | Female | |
| Underweight | 1 (1.2%) | 68 (18.9%) | 1 (1.2%) | 68 (18.9%) |
| Normal weight | 33 (39.3%) | 209 (58.1%) | 34 (40.5%) | 277 (76.9%) |
| Overweight | 24 (28.6%) | 47 (13.1%) | 58 (69%) | 324 (90%) |
| Obese | 22 (26.2%) | 23 (6.4%) | 80 (95.2%) | 347 (96.4%) |
| Severely obese | 4 (4.8%) | 13 (3.6%) | 84 (100%) | 360 (100%) |
Table 3: Comparison of parental weight status among male and female.
Child weight status
About half (56.9%) of the children were classified as “Normal”, 11% as “overweight”, 25.9% as “obese”, while the remaining 6.3% were classified as “underweight” in this study in Table 4. It was found that the weight status shown in Table 5 among boys and girls were similar.
| Count (Valid ercentage) | Cumulative count (Cumulative percentage) | |
|---|---|---|
| Underweight | 27 (6.3%) | 27 (6.3%) |
| Normal weight | 244 (56.9%) | 371 (63.2%) |
| Overweight | 47 (11.0%) | 418 (74.1%) |
| Obese | 111 (25.9%) | 529 (100%) |
Table 4: Weight status of children.
| Count (Percentage) | Cumulative count (Cumulative percentage) | |||
|---|---|---|---|---|
| Boy | Girl | Boy | Girl | |
| Underweight | 19 (8.2%) | 8 (4.1%) | 19 (8.2%) | 8 (4.1%) |
| Normal weight | 123 (52.8%) | 121 (61.7%) | 142 (60.9%) | 129 (65.8%) |
| Overweight | 27 (11.6%) | 20 (10.2%) | 169 (72.5%) | 149 (76%) |
| Obese | 64 (27.5%) | 47 (24%) | 233 (100%) | 196 (100%) |
Table 5: Children’s Weight Status among Boys and Girls.
Gender effect of modified model components’ score
An independent sample t-test was conducted to determine the model component scores against gender. As stated in Table 6, significant difference was found between fathers and mothers for the component parental BMI, and CWC. First of all, the fathers’ BMI (M=24.205, SD=3.86) was significantly higher than mothers’ BMI (M=21.663, SD=5.42); p<0.001, 95% CI [1.31, 3.77]. For CWC, the mean scores in mothers (M=4.693, SD=1.34) was also significantly found to be higher than that in fathers (M=4.282, SD=1.30); p=0.011, 95% CI [0.09, 0.73].
| Male | Female | p-Value | |
|---|---|---|---|
| Mean (SD) | Mean (SD) | ||
| Parental BMI | 24.205 (±3.86) | 21.663(±5.42) | <0.001 |
| Child Weight Concern | 4.282 (±1.30) | 4.693 (±1.34) | 0.011 |
Table 6: Independent t-test of parental BMI and CWC by gender.
Education level effect of modified model components’ score
The mean score of component CWC was found to be significantly difference due to the parents’ education level. According to Table 7, parents either educated to Form 3 or less (M=4.829, SD=1.33); p=0.002, 95% CI [4.01, 2.59], high school level (Form 4 to 7) (M=4.619, SD=1.30); p=0.010, 95% CI [0.21, 2.37], or undergraduate degree (M=4.539, SD=1.25); p=0.023, 95% CI [0.11,2.30] were significantly more concerned about child weight when compared to those postgraduate parents (M=5.333, SD=1.37).
| Child Weight Concern | Form 3 or under | Postgraduate |
|---|---|---|
| 4.829 (±1.33) | 3.33 (±1.91) | 0.002 |
| Form 4 - 7 | Postgraduate | 0.010 |
| 4.619 (±1.30) | 3.33 (±1.91) | |
| Undergraduate | Postgraduate | 0.023 |
| 4.539 (±1.25) | 3.33 (±1.91) |
Table 7: One way ANOVA test of CWC in education level.
Weight status effect of modified model components’ score
One way ANOVA test was conducted to investigate the difference by weight statuses among model variables as stated in Table 8. For Body Dissatisfaction, it was found that the underweight group (M=1.896, SD=1.07) was significantly less dissatisfied with their body when compared to the overweight group (M=2.853, SD=1.36); p<0.001, 95% CI [-0.84, 0.05], the obese group (M=2.817, SD=1.27); p<0.001, 95% CI [-1.50, -0.41], as well as the severely obese group (M=3.17, SD=1.71); p<0.001, 95% CI [-2.12, -0.42]. Moreover, it was also found that the normal weight group (M=2.291, SD=1.05) was significantly less dissatisfied with their body when compared with the overweight group (M=2.853, SD=1.36); p=0.003, 95% CI [-0.99, -0.13], the obese group (M=2.817, SD=1.27); p=0.05, 95% CI [-1.05, 0.0004], as well as the severely obese group (M=3.17, SD=1.71); p=0.017, 95% CI [-1.66, -0.10].
| Body Dissatisfaction | Underweight | Overweight | p-value |
|---|---|---|---|
| 1.896 (±1.07) | 2.853 (±1.36) | <0.001 | |
| Underweight | Obese | <0.001 | |
| 1.896 (±1.07) | 2.817 (±1.27) | ||
| Underweight | Severely obese | <0.001 | |
| 1.896 (±1.07) | 3.168 (±1.71) | ||
| Normal weight | Overweight | 0.003 | |
| 2.291 (±1.05) | 2.853 (±1.36) | ||
| Normal weight | Obese | 0.05 | |
| 2.291 (±1.05) | 2.817 (±1.27) | ||
| Normal weight | Severely obese | 0.017 | |
| 2.291 (±1.05) | 3.168 (±1.71) | ||
| Dietary Restraint | Underweight | Overweight | <0.001 |
| 1.696 (± 0.95) | 2.488 (± 1.09) | ||
| Underweight | Obese | <0.001 | |
| 1.696 (± 0.95) | 2.570 (±1.18) | ||
| Underweight | Severely obese | 0.021 | |
| 1.696 (± 0.95) | 2.495 (±0.96) | ||
| Normal weight | Overweight | 0.01 | |
| 2.055 (±0.95) | 2.488 (± 1.09) | ||
| Normal weight | Obese | 0.014 | |
| 2.055 (±0.95) | 2.570 (±1.18) |
Table 8: One way ANOVA test of BD, PDR in parental weight status.
Similar relationship was obtained in model component PDR as well, in which, the extent of PDR in underweight group (M=1.696, SD=0.95) was significantly lower than that in the overweight group (M=2.488, SD=1.09); p<0.001, 95% CI [-1.26, -0.33], the obese group (M=2.570, SD=1.18); p<0.001, 95% CI [-1.41, -0.34], as well as the severely obese group (M=2.495, SD=0.96); p=0.021, 95% CI [-1.53, -0.07]. Moreover, the extent of PDR in the normal weight group (M=2.055, SD=0.95) was significantly lower than that of the overweight group (M=2.488, SD=1.09); p=0.10, 95% CI [-0.80, -0.06], and the obese group (M=2.570, SD=1.18); p=0.14, 95% CI [-0.97,-0.07].
Descriptive statistics of the modified model
Descriptive statistics and bivariate correlations for the variables of interest are shown in Table 9.
| CBMI | PBMI | BD | PDR | CWC | CWFRF | |
|---|---|---|---|---|---|---|
| CBMI | 1.00 | -.002 | .054 | .100* | .085 | .121** |
| PBMI | 1.00 | .282*** | .304*** | -.096* | .152** | |
| BD | 1.00 | .715*** | .146** | 263*** | ||
| PDR | 1.00 | .152** | .360*** | |||
| CWC | 1.00 | .320*** | ||||
| CWFRF | 1.00 |
*p<0.05, **p<0.01, ***p<0.001
CBMI: Child BMI, PBMI: Parental BMI, BD: Body Dissatisfaction, PDR: Parental Dietary Restraint, CWC: Child Weight Concern, CWFRF: Child Weight-focused restrictive feeding.
Table 9: Pearson’s correlation coefficient of model components.
Standardized path coefficients (β) and explained variance for the modified model
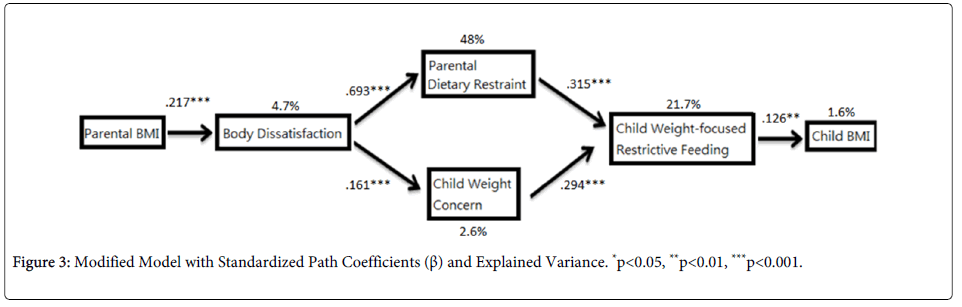
The model explained 4.7% of the variance body dissatisfaction (r2=0.217, p<0.001), 48% of the variance in PDR (r2=0.693, p<0.001), 2.6% of the variance in CWC (r2=0.161, p<0.001), 21.7% of the variance in CWFRF (PDR: r2=0.315, p<0.001; CWC: r2=0.294, p<0.001), and 1.6% of the variance in child BMI (r2=0.126, p=0.006). The six pathways indicated in the modified model were all found significant as shown in Figure 3.
Discussion
With the increased public concern of child obesity, early parent child interaction was believed to be one of the crucial factors contributing to child weight problems [7]. It had been investigated with numerous studies to examine the relationships between parental eating behaviors, body image perception and the transmission of eating-related attitudes and behaviors to children [7,25,27]. As influence of body image perception from parents, eating behavior on children weight concern and feeding practice, and in turn on child BMI has not been examined in Hong Kong, the model proposed by Rodgers et al. [7] was adopted with some modifications in this study.
The association of parent-child interaction on child weight problems among kindergarten period was investigated in this study as it was believed that the younger the children, the stronger the effect of parent child interaction would be associated. 466 participants (parents) were studied in total with 18.9% male and 81.1% female, in which 54.7% was found with normal weight, while 16.1% and 14% were found to be overweight and obese. The rates of male being overweight and obesity were found 2 and 4 times more than female respectively. The result obtained was found similar to the prevalence stated in the Health Facts of Hong Kong 2013, in which the percentage of overweight and obesity of persons aged between 18 and 64 was 36.6% in total [41].
Besides, 11% and 25% kindergarten children were found to be overweight and obese respectively. The percentages were found similar in girls and boys. The total prevalence of overweight and obesity obtained was found to be 36%, which was much higher than the figure obtained in 2010 (21.4%) [4], indicating the presence of upward trend of childhood obesity.
With reference to Table 7, parents who were well educated to postgraduate level were found with lower degree of child weight concern. It was assumed that people with a higher education level would prefer contributing to the society more, therefore the high workload would reduce their focus or concern on child.
Moreover, as expected, parents with a higher BMI would have a higher level of body dissatisfaction as stated in Table 8, which was consistent with previous researches showing the positive association between BMI and body dissatisfaction [7,13,15]. Similar phenomena were also observed in PDR. Parents categorized as overweight and obese had a higher level of parental dietary restraint, probably due to the increase in body dissatisfaction, leading to the development of unhealthy eating behaviors, like fasting, food restraint, aiming at weight reduction [17,18].
According to Table 9 and Figure 3, significant correlations were identified in the six pathways of the modified model. To begin with, parental BMI was found positively correlated with body dissatisfaction [r (466)=0.282, p<0.001], which was consistent to previous research [42]. However, the correlation obtained was comparatively weaker. It was believed that parents, in particular female, had already adapted and accepted the changes of body weight and body image caused by pregnancy. Therefore, the expected stronger body dissatisfaction might not be resulted due to limited postpartum period associating with social thin-ideal body [42].
Regarding body dissatisfaction, a strong correlation was found with dietary restraint [r (466)=0.715, p<0.001], indicating that people who were dissatisfied with their own body were likely to achieve weight loss in order to maintain healthy weight. Apart from PDR, a weak correlation was obtained between body dissatisfaction and CWC [r (466)=0.146, p=0.002] and consistency were found in line with previous researches [25,26].
For the child-weight focused feed practice, moderate correlations were resulted with PDR [r (466)=0.360, p<0.001] and CWC [r (466)=0.320, p<0.001]. It was believed that during parent child interaction, parents would choose the type of feeding practice depending their own eating behavior and attitude. Therefore, those with dietary restraint had a higher preference to use restrictive feeding practice, in order to restrict their children from the food choice which they were also restrained [24,28]. Moreover, as concerning about child weight was not only a thought, it usually came with an action aiming at weight control [26,29]. As a result, child weight-focused restrictive feeding practice was used for purpose.
For the pathway between CWFRF practice and child BMI, a positive correlation [r (466) = 0.121, p=0.009] was found to be in line with pervious researches [28,34]. Some studies supported that the increase in restrictive feeding might trigger child’s preference towards restrictive food. It was revealed that the restriction of food enhanced the child’s approach to those restrictive foods and the trend of child emotional eating and eating in the absence of hunger [36]. Therefore, overconsumption of food would be resulted and hence, calories intake could not be controlled, or even increased with the restrictive feeding practice [28].
Last but not least, our findings also suggested a new significant pathway from PDR to child BMI [r (466)=0.100, p=0.031], which is in line with certain studies [7,43]. It was revealed that individuals with higher dietary restrained were more pleasant and desired to consume restricted food due to the hyper-responsibility in reward-related brain regions [44]. Therefore, it was believed that parents with behavior of dietary restraint would use those restricted food, such as high calories, high fat, high sugar food as rewards to children. As some studies showing the association of increased risk of overweight with food rewards [45], it was thought that child BMI would associate with parental dietary restraint through food rewarding.
Conclusion
The results of this study further confirmed the presence of upward trend of childhood obesity in Hong Kong. In addition, the mechanism amongst parental BMI, body dissatisfaction, parental dietary restrain, child weight concern on child feeding practice and in turn child BMI has been examined by application of the model proposed by Rodgers et al. [7]. As the model only explained 1.6% of the variance in child BMI, it was weak in prediction of the BMI of kindergarten students in Hong Kong. When considering the correlations amongst variables, it was interesting to find a link between child BMI and parental body dissatisfaction. Parental body dissatisfaction was found to be a significant factor to determine parental dietary restraint, which was associated with child weight-focused restrictive feeding and finally affected child BMI. This link might be the result of increase of dietary restraint leading to food rewards. Therefore, it is suggested that programs should be given to parents to help addressing body dissatisfaction and promoting healthy eating behaviors, together with guidance regarding healthy feeding practice to help achieving the children weight management.
Some limitations in the present study should be acknowledged. First, the invitation list of kindergarten for this research does not cover all kindergartens in Hong Kong, the results may be somewhat bias. Second, all data were from self-report, which is subject to both random and systematic bias.
References
- World Health Organization (2014) Childhood Overweight and Obesity.
- American Heart Association (2013) BMI in Children.
- Poirier P, Giles T, Bray G, Hong Y, Stern J, et al. (2006) Obesity and Cardiovascular Disease: Pathophysiology, Evaluation, and Effect of Weight Loss an Update of the 1997 American Heart Association Scientific Statement on Obesity and Heart Disease from the Obesity Committee of the Council on Nutrition, Physical Activity, and Metabolism, Circulation 113: 898-918
- Student Health Service (2012) Feature Article: Childhood Overweight and Obesity.
- DeOnis M,Blossner M, Borghi E (2010) Global Prevalence and Trends of Overweight and Obesity among Preschool Children, The American journal of clinical nutrition 92: 1257-1264
- Mok WK, Lee AYK (2013) A Case Study on Application of the Theory of Planned Behavior: Predicting Physical Activity of Adolescents in Hong Kong, J Community Med Health Educ 3:231
- Rodgers R, Paxton S, McLean S, Campbell K, Wertheim E, et al. (2013) Do Maternal Body Dissatisfaction and Dietary Restraint Predict Weight Gain in Young Pre-School Children? A 1-Year Follow-Up Study, Appetite 67: 30-36
- Golan M, Crow S (2004) Parents Are Key Players in the Prevention and Treatment of Weight-Related Problems, Nutrition reviews 62: 39-50
- Stang J, Loth K (2011) Parenting Style and Child Feeding Practices: Potential Mitigating Factors in the Etiology of Childhood Obesity, Journal of the American Dietetic Association 111: 1301-1305.
- Berge J, Wall M, Loth K, Neumark-Sztainer D (2010) Parenting Style as a Predictor of Adolescent Weight and Weight-Related Behaviors, Journal of Adolescent Health 46: 331-338
- Birch L (2006) Child Feeding Practices and the Etiology of Obesity, Obesity 14: 343-344
- Huon G,Gunewardene A, Hayne A,SankeyM, Lim J, et al. (2002) Empirical Support for a Model of Dieting: Findings from Structural Equations Modeling, International Journal of Eating Disorders 31: 210-219
- Lynch W,Heil D, Wagner E, Havens M (2008) Body Dissatisfaction Mediates the Association between Body Mass Index and Risky Weight Control Behaviors among White and Native American Adolescent Girls, Appetite 51: 210-213
- Neumark-Sztainer, D, Wall M, Story M, Perry C (2003) Correlates of Unhealthy Weight-Control Behaviors among Adolescents: Implications for Prevention Programs, Health Psychology 22: 88
- Presnell K,Bearman S, SticeE (2004) Risk Factors for Body Dissatisfaction in Adolescent Boys and Girls: A Prospective Study, International Journal of Eating Disorders 36: 389-401
- Markey C, Markey P (2005) Relations between Body Image and Dieting Behaviors: An Examination of Gender Differences, Sex Roles 53: 519-530
- Compeau A, AmbwaniS (2013) The Effects of Fat Talk on Body Dissatisfaction and Eating Behavior: The Moderating Role of Dietary Restraint, Body image 10: 451-461
- Heatherton T (1993) Body Dissatisfaction, Self-Focus, and Dieting Status among Women, Psychology of Addictive Behaviors 7: 225
- Jonstang I (2009) The Effect of Body Dissatisfaction on Eating Disorder Symptomatology: Mediating Effects of Depression and Low Self-Esteem: A Partial Test of the Dual-Pathway Model, Department of psychology, University in Oslo
- McCabe M, Ricciardelli L (2004) Body Image Dissatisfaction among Males across the Lifespan: A Review of Past Literature, Journal of psychosomatic research 56: 675-685.
- Troisi A, Di Lorenzo G,Alcini S,Nanni R, Di Pasquale C, et al. (2006) Body Dissatisfaction in Women with Eating Disorders: Relationship to Early Separation Anxiety and Insecure Attachment, Psychosomatic Medicine 68: 449-453
- Gianini L, Smith J (2008) Body Dissatisfaction Mediates the Relationship between Self-Esteem and Restrained Eating in Female Undergraduates, International Journal of Behavioral Consultation & Therapy 4
- Kong F, Zhang Y, You Z, Fan C,Tian Y, et al. (2013) Body Dissatisfaction and Restrained Eating: Mediating Effects of Self-esteem, Social Behavior & Personality: An International Journal 41
- Francis L, Hofer S, Birch L (2001) Predictors of Maternal Child-Feeding Style: Maternal and Child Characteristics, Appetite 37: 231-243
- Francis L, Birch L (2005) Maternal Influences on Daughters' Restrained Eating Behavior, Health Psychology 24: 548
- Gray W,Janicke D,Wistedt K, Dumont-Driscoll M (2010) Factors Associated with Parental Use of Restrictive Feeding Practices to Control Their Children's Food Intake, Appetite 55: 332-337.
- Francis L, Birch L (2005) Maternal Weight Status Modulates the Effects of Restriction on Daughters' Eating and Weight, International Journal of Obesity 29 (8): 942-949
- Rodgers R, Paxton S, Massey R, Campbell K, Wertheim E, et al. (2013) Maternal Feeding Practices Predict Weight Gain and Obesogenic Eating Behaviors in Young Children: A Prospective Study, International Journal of Behavioral Nutrition and Physical Activity 10: 24
- Payne L, Galloway A, Webb R (2011) Parental Use of Differential Restrictive Feeding Practices with Siblings, International Journal of Pediatric Obesity 6 (2-2): 540-546
- May A, Donohue M, Scanlon K, Sherry B,Dalenius K, et al. (2007) Child-Feeding Strategies Are Associated with Maternal Concern about Children Becoming Overweight, but Not Children’s Weight Status, Journal of the American Dietetic Association 107: 1167-1174
- Webber L, Hill C, Cooke L, Carnell S, Wardle J (2010) Associations between Child Weight and Maternal Feeding Styles Are Mediated by Maternal Perceptions and Concerns, European journal of clinical nutrition 64: 259-265
- Farrow C, Blissett J (2008) Controlling Feeding Practices: Cause or Consequence of Early Child Weight?, Pediatrics 121: 164-169
- Campbell K,Andrianopoulos N,Hesketh K, Ball K, Crawford D, et al. (2010) Parental Use of Restrictive Feeding Practices and Child BMI Z-Score. A 3-Year Prospective Cohort Study, Appetite 55: 84-88
- Faith, M, Berkowitz, R, Stallings, V, Kerns, J,Storey M,Stunkard A (2004) Parental Feeding Attitudes and Styles and Child Body Mass Index: Prospective Analysis of a Gene-Environment Interaction, Pediatrics 114 (4): 429-436
- Faith M, Kerns J (2005) Infant and Child Feeding Practices and Childhood Overweight: The Role of Restriction, Maternal & child nutrition 1: 164-168
- Birch L, Fisher J, Davison K (2003) Learning to Overeat: Maternal Use of Restrictive Feeding Practices Promotes Girls’ Eating in the Absence of Hunger, The American Journal of Clinical Nutrition 78: 215-220
- Fairburn C, Beglin S (1994) Assessment of Eating Disorders: Interview or Self-Report Questionnaire?, International Journal of Eating Disorders 16 (4): 363-370.
- Birch L, Fisher J, Grimm-Thomas K, Markey C, Sawyer R, et al. (2001) Confirmatory Factor Analysis of the Child Feeding Questionnaire: A Measure of Parental Attitudes, Beliefs and Practices about Child Feeding and Obesity Proneness, Appetite 36: 201-210
- Musher-Eizenman D, Holub S (2007) Comprehensive Feeding Practices Questionnaire: Validation of a New Measure of Parental Feeding Practices, Journal of Pediatric Psychology 32: 960-972
- World Health Organization (2014) Weight-For-Age
- Health Facts of Hong Kong (2013)
- Rallis S,Skouteris H, Wertheim E, Paxton S (2007) Predictors of Body Image During the First Year Postpartum: A Prospective Study, Women & health 45: 87-104
- Birch L, Fisher J (2000) Mothers' Child-Feeding Practices Influence Daughters' Eating and Weight, The American journal of clinical nutrition 71: 1054-1061
- Burger K, Stice E (2011) Relation of Dietary Restraint Scores to Activation of Reward-Related Brain Regions in Response to Food Intake, Anticipated Intake, and Food Pictures, Neuroimage 55: 233-239
- Bandini L, Curtin C, Anderson S, Philips S, Must A (2013) Food as a Reward and Weight Status in Children with Autism, The FASEB Journal 27: 1063-11.
Relevant Topics
- Addiction
- Adolescence
- Children Care
- Communicable Diseases
- Community Occupational Medicine
- Disorders and Treatments
- Education
- Infections
- Mental Health Education
- Mortality Rate
- Nutrition Education
- Occupational Therapy Education
- Population Health
- Prevalence
- Sexual Violence
- Social & Preventive Medicine
- Women's Healthcare
Recommended Journals
Article Tools
Article Usage
- Total views: 14649
- [From(publication date):
August-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 10035
- PDF downloads : 4614