Case Report Open Access
Stomatitis Medicamentosa: A Case Report with Review
Pravda C1*, Raghu Ganesh2 and Koteeswaran2
1Department of Oral Medicine and Radiology, Sathyabama University Dental College & Hospital, Chennai, India
2Department of Oral Medicine & Radiology, Meenakshi Ammal Dental College, Chennai, India
- *Corresponding Author:
- Pravda C
Department of Oral Medicine and Radiology
Sathyabama University Dental College & Hospital
Jeppiaar nagar, Old Mamallapuram Road
Chennai- 600 119, India
Tel: 044-23782566
Fax: 044–23781631
E-mail: prabhakaranramachandran@yahoo.co.in
Received Date: October 08, 2013; Accepted Date: March 30, 2014; Published Date: April 05, 2014
Citation: Pravda C, Ganesh R, Koteeswaran (2014) Stomatitis Medicamentosa: A Case Report with Review. J Oral Hyg Health 2:128. doi: 10.4172/2332-0702.1000128
Copyright: © 2014 Pravda C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Oral Hygiene & Health
Abstract
A great variety of drugs are implicated in oral mucosal lesions. Allergic inflammatory reactions of oral mucosa due to intake of drug are rare and non-specific. These reactions are found to be associated with drug or medicament used locally or systemically. An allergic reaction from topical medications is referred as Stomatitis venenata. Stomatitis medicamentosa is a less common oral lesion that is produced with systemic administration of drugs. The lesion may vary from diffused distribution of erythema to extensive areas of ulcerations with or without vesicle or bulla formation. The lesions are seen commonly involving gingiva, palate, lips and tongue.
This article includes a case of Stomatitis medicamatosa in a patient who presented with multiple oral ulcerations on oral administration of Carbamazepine used for the treatment of Trigeminal Neuralgia. The article also includes a review of other oral reactions that are associated with systemic administration of various other drugs.
Keywords
Drugs; Stomatitis venenata; Stomatitis medicamentosa; Allergic reactions; Ulcerations; Erosions
Introduction
Drugs are often double edged sword. A drug that is absolutely safe in one person can be life threatening to others because of its adverse reactions. The adverse drug reactions form a spectrum that ranges from mild erythema, rashes to more life threatening anaphylacticreactions like bronchospasm or bronchial asthma [1].
The oral reactions to systemic administration of drugs can be broadly classified as non-immunogenic reactions such as gingival hyperplasia due to Dialantin sodium, Heavy metal poisoning, oral ulcerations due to Chemotherpeutic drugs and immunogenic reactions, also referred as Stomatitis medicamentosa [2]. Table 1 shows various patterns of oral drug reactions [3].
| Reaction | Drug |
|---|---|
| Gingival hyperplasia | Phenytoin, Nifedipine |
| Lichenoid reaction | Gold, D-penicillamine |
| Black hairy tongue | Antibiotics, griseofulvin |
| Thrush | Antibiotics, corticosteroids |
| Oral ulcerations | Aspirin, NSAIDS, antimetabolites |
| Enamel staining | Iron, fluoride, tetracycline |
| Metallic taste | Metronidazole, griseofulvin |
| Xerostomia | Antihistamines, anticholinergics, tranquilizers, antidepressants |
Table 1: Various patterns of oral drug reactions [3].
Stomatitis medicamentosa is a variety of sensitivity reactions following systemic intake of great many drugs and chemicals at normal dose, but not related to any pharmacological activity or toxicityof these drugs. These reactions are rare and more coincidental [4]. This is a case of a 60 year old patient who developed multiple oral ulcerations and facial swelling on taking systemic carbamazepine for Trigeminal neuralgia.
Case Report
A 60 year old female patient reported with a complaint of swelling of the face and lips and multiple ulcerations throughout the mouth associated with pain and discomfort for past one week. History reveals that the patient had visited a local dentist for severe lancinating pain on the right side of the face that was present for one month. The dentist has extraction of his right lower back tooth, but he pain did not subside. Then she was prescribed Tegretol (Carbamazepine) 200 mg twice daily. On taking this drug, the patient developed rashes all over the body and swelling in the face, lips and multiple ulcerations all over the mouth with which she reported to our hospital.
The patient is a known diabeticfor past ten years was under medication.
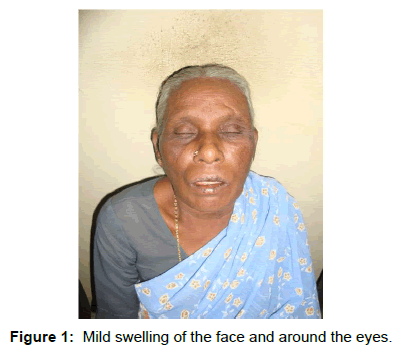
Extra oral examination of the patient revealed a mild periorbital edema with areas of hyperpigmentation was seen around the eyes and the skin over the cheek (Figure 1). Diffused swelling of the upper lip and philtrum was present. Ulceration with crestations was seen in both upper and lower lips.
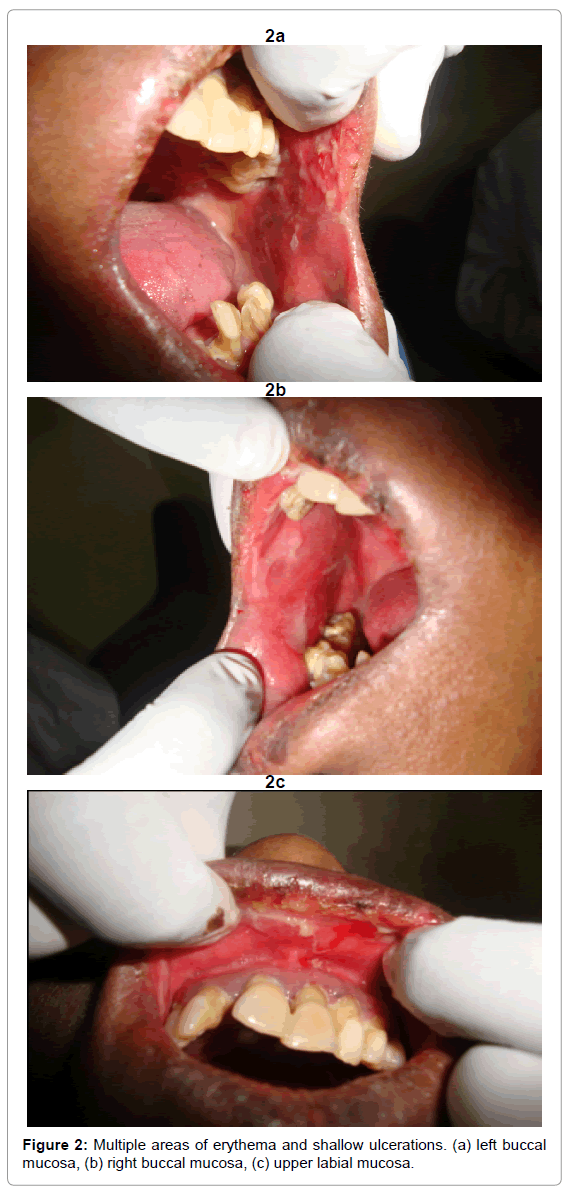
Mouth opening was slightly restricted and painful. Periodontal health was poor with multiple mobile teeth. Multiple areas of erosions and shallow ulcerations were seen in labial mucosa, buccal mucosa and soft palate that was associated with pain and discomfort (Figures 2a-2c).
Correlating the features such as development of rashes, multiple ulcerations of the oral mucosa and swelling of the face and lips on taking Tegritol, the case was diagnosed as stomatitis medicamentosa, an allergic drug reaction to systemic administration of drugs. The patient was immediately asked to stop taking Tegritol. Oral antihistamines (Tab CETZIN) were prescribed. Because of the severity of the lesion, oral Prednisolone (Tab WYSOLONE) 10 mg twice daily was prescribed for one week.
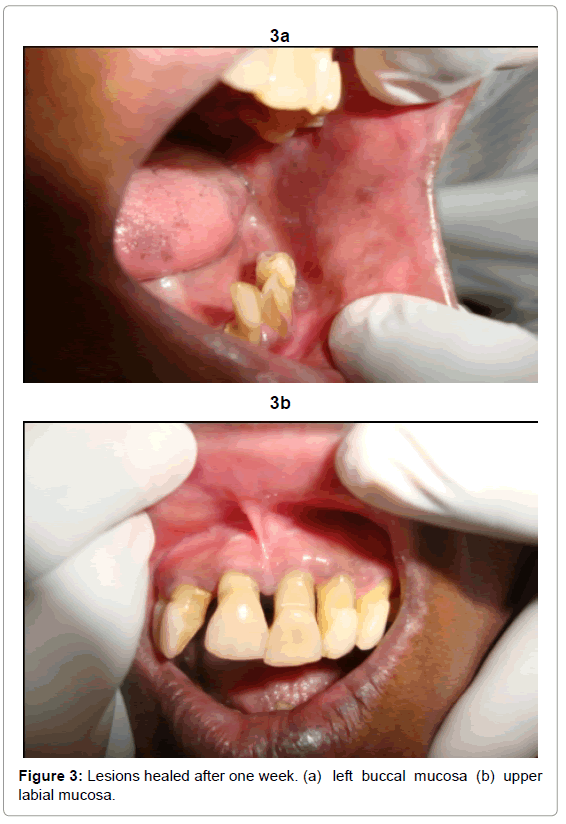
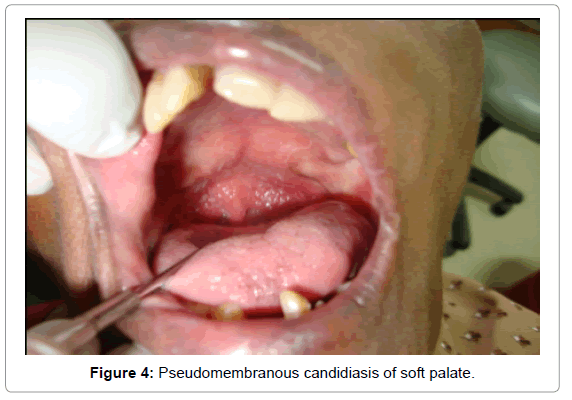
After one week the lesion almost healed (Figures 3a and 3b), but the patient developed pseudomembranous candidiasis in the soft palate (Figure 4).
Prednisolone was stopped and topical antifungal agent (CANDID MOUTH PAINT) was prescribed for candidiasis.
The patient had episodic, severe lancinating pain that was unilateral involving the right side of the lower part of the face and it was not associated with any teeth. So she was diagnosed clinically as Trigeminal Neuralgia. Instead of Tegritol, Baclofen 5 mg twice daily was prescribed.
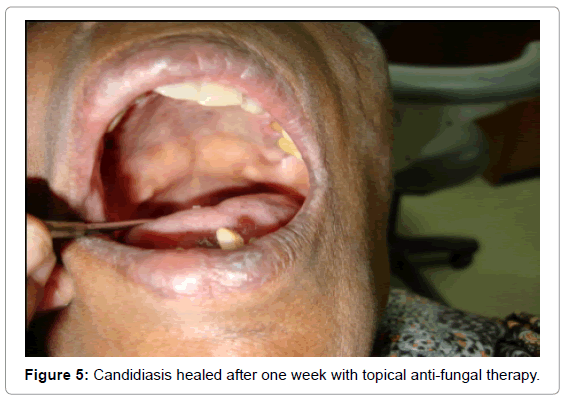
Patient was reviewed after one week and the lesion had healed completely (Figure 5) and the pain was also controlled.
Discussion
Adverse drug reactions are common iatrogenic illness complicating 5-15% of therapeutic drug courses [5]. An estimated 2-4% of hospital admissions are related to these reactions. Every drug has been recognized at one time or the other, capable of producing allergic reaction in sensitive person. Some drugs has greater tendency and some patients has greater susceptibility to drugs especially those with asthma or hay fever.
Epidemiological data supports the existence of specific factors that increases the risk of developing adverse drug reactions like female gender, asthma, polypharmacy, Systemic Lupus Erythematosis, infections with herpes or HIV [6]. Multiple medications are found to be most likely to escalate the allergic reactions. Use of two medications is associated with 6% risk. With the use of 5 drugs, the frequency increases to 50%. When more than 8 drugs are taken simultaneously, there is 100% risk of developing adverse drug reactions [7].
The drug related risk factors includes its chemical properties, molecular weight and route of administration. Larger drugs with greater structural complexity like non-human proteins are more immunogenic. Topical, intramuscular, intravenous administration of drugs are more likely to cause allergic reactions due to the antigen present in the skin and high concentration of circulating drug antigen that is rapidly achieved with iv therapy [8].
The pathogenesis of these reactions is mostly immunological where the immune response is triggered by the antigenic component on the drug molecule leading to hyper immune response. The reactions depends on several factors like immunogenicity of the drug, frequency of exposure, route of administration and innate reactivity of the patient’s immune system. Sometimes these reactions occur through non immunological mechanism where there is no participation of immune response and the drugs directly affect the mast cells and release chemical mediators [9].
The various allergic reactions to systemic drugs occur several hours or days after the administration of the drug or as immediate reaction [10]. The adverse drug reaction may involve any part of the body or organ system. Skin is the commonest site. The various cutaneous manifestations include morbilliform rashes, urticaria, bullous skin lesions like erythema multiforme, Steven-Johnson syndrome and toxic epidermal necrolysis which are associated with significant morbidity and mortality.
Angioedema is an acute condition characterized by sudden and rapid tissue swelling. The two major chategories are Hereditary and Acquired. Most common type is acquired angioedema which is an IgE mediated hypersensitivity reaction characterized by mast cell degranulation and associated histamine release [2]. Mild cases respond well to oral antihistamines. In case of pharyngeal or laryngeal involvement obstructing the airway, the condition becomes more life threatening, a parenteral epinephrine or intravenous corticosteroids are indicated.
Oral mucosa may occasionally be the target or sometimes the sole site of involvement.
The common allergic reactions of the oral mucosa are erythema multiformae characterized by multiple ulcerations all over the oral cavity. It ranges from erythema to life threatening and fulminant diseases like Steven Johnson Syndrome & Toxic Epidermal Necrolysis. The drugs most frequently associated with it are antibiotics like penicillin, sulphanamides, tetracycline, NSAIDS, sulphanomides, carbamazepines, barbiturates, etc.
Anaphylactic stomatitis occurs once the drug enters the blood and binds with the IgE mast cells [7]. Signs and symptoms of anaphylaxis like horseness, respiratory distress, vomiting exhibiting multiple zones of erythema or erosion of the affected mucosa. This is more common with antibiotics such as penicillin and sulpha groups of drugs.
Intraoral fixed drug eruption is a localized hypersensitivity reaction where the lesion appears on the same site each time a particular drug is administered [2]. The lesions are characterized by localized areas of erythema, edema in the labial mucosa. The drugs implicated with this are Barbiturates, sulphanamides, phenazone, salisalates, and tetracycline.
Allergic mucosal reactions may also resemble lichen planus, lupus erythematosis, and pemphigus. These lesions mimic their namesakes clinically, histopathologically and immunologically and involve any part of the oral mucosa.
Histopathology of these lesions reveals non-specific features demonstrating stratified squamous epithelium with necrosis of keratinocyte, edema, basal cell destruction and spongiosis. Infiltration of lymphocytes and eosinophils in connective tissue stroma with mononuclear and polymorphonuclear cell adjacent to epithelium are seen [7].
Diagnosis of adverse drug reactions is highly challenging because of its multiple clinical manifestations, multiple mechanisms of host drug interactions and relative paucity in the laboratory investigations available for drug allergy. Diagnosis requires a high index of suspicion and a careful history taking. Initial history should include recording all the prescription and non-prescription drugs that the patient has been taking for past one month. History of any previous drug reactions should be asked. Physical examination includes evaluation of signs and symptoms like rashes, fever, mucosal lesions and lymphadenopathy. Withdrawal of the drug should result in improvement of the signs and symptoms. Reinstitution of the drugs worsens the patient’s condition. Laboratory investigations help to evaluate biochemical and immunological markers responsible for adverse drug reactions. Skin testing is standardized for penicillin, local anesthesia and muscle relaxants [6].
Genomic research has led to the identification of genes that confer susceptibility to severe drug reactions. The genes appear to be specific to the drug, phenotype and ethnicity. A genetic association of HLA-B 1502 and HLA-B 5801 was found in all the patients with cutaneous reactions to carbamazepine and allopurinol respectively, among people of various ethnicities [11].
Once the diagnosis of adverse drug reactions has been established, appropriate documentation should be done in the case sheet specifying the causative drug and the nature of the adverse effect because, an immune mediated drug hypersensitivity reaction pose a more serious health risk with re exposure of the drug.
The key for the successful management of the drug induced hypersensitive reaction is early identification of the lesion and prompt withdrawal of the offending drug. The drug can be replaced by another drug with same efficacy. Acute signs are relieved by administration of antihistamines. For local reactions, topical steroids are helpful. A severe reaction with systemic involvement requires hospital admission and parenteral administration of epinephrine, corticosteroids or antihistamines.
Conclusion
Adverse drug reactions can result in high morbidity and mortality. This can be minimized if an oral clinician follows these steps. Before writing a prescription, the patient should be asked for allergy to any drug or food. If the patient is allergic to any drug, avoid prescribing all the drugs of that group and those with structural similarities to avoid cross interactions. If a patient presents with acute onset of ulcerations with facial edema with a recent use of a drug, the drug should be immediately withdrawn. The patient should be informed about the drug allergy and familiarize the common brand names of the drug that the patient is allergic to. The patient must also be instructed strictly to inform his drug allergy whenever he visits a physician or an oral clinician.
References
- Bankowski Z, Bruppach er R, Crusius I, Gallagher J, Kremer G, et al. (2000) Reporting adverse drug reactions, CIOMS 88.
- Rajendran, B. Sivapathasundram (2009) Shafer’s Textbook of Oral Pathology, (6thedn), Elseveir, India.
- Alan Tack D, Roy S (2002) Oral drug reactions, Dermatological Therapy 15: 236-250.
- Binnie WH, Burett AW, James Wright. Oral Diseases, (3rdedn), Cawson, 13-3
- Ditto AM (2002) Drug allergy. In: Grammer LC, Greenberger PA (Eds.), Patterson’s Allergic disease (6th Edn.), Philadelphia: Lippincott Williams & Wilkins: 295
- Riedl MA, CasillasAM (2003) Adverse drug reactions: types and treatment options. AmFam Physician 68: 1781-1790.
- Neville, Danm, Allen, Bouquol (2009) Oral and Maxillofacial Pathology, (3rdedn), pp: 347-58.
- Adkinson NF Jr (1984) Risk factors for drug allergy. J Allergy ClinImmunol 74: 567-572.
- Sanjay Saraf Textbook of Oral Pathology 156-58
- Regezi JA, Sciubba JJ.Oral Pathology-Clinical pathologic Correlation (3rdedn), 61-63.
- Fernando SL, Broadfoot AJ (2010) Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening. CMAJ 182: 476-480.
Relevant Topics
- Advanced Bleeding Gums
- Advanced Receeding Gums
- Bleeding Gums
- Children’s Oral Health
- Coronal Fracture
- Dental Anestheia and Sedation
- Dental Plaque
- Dental Radiology
- Dentistry and Diabetes
- Fluoride Treatments
- Gum Cancer
- Gum Infection
- Occlusal Splint
- Oral and Maxillofacial Pathology
- Oral Hygiene
- Oral Hygiene Blogs
- Oral Hygiene Case Reports
- Oral Hygiene Practice
- Oral Leukoplakia
- Oral Microbiome
- Oral Rehydration
- Oral Surgery Special Issue
- Orthodontistry
- Periodontal Disease Management
- Periodontistry
- Root Canal Treatment
- Tele-Dentistry
Recommended Journals
Article Tools
Article Usage
- Total views: 25783
- [From(publication date):
May-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 19676
- PDF downloads : 6107