Research Article Open Access
The Effectiveness of Instrument-assisted Soft Tissue Mobilization Technique (Ergon�?© Technique), Cupping and Ischaemic Pressure Techniques in the Treatment of Amateur Athletes�?�? Myofascial Trigger Points
Konstantinos Fousekis1*, Eleni Kounavi1, Symeon Doriadis1, Konstantinos Mylonas2, Elias Kallistratos3 and Elias Tsepis11Human Assesment and Rehabilitation Lab, Department of Physiotherapy, Technological Educational Institute of Western Greece, Greece
2Department of Physiotherapy, IASO General Hospital, Athens
3Clinical Practice Lab, Department of Physiotherapy, Alexander Technological Educational Institute of Thessaloniki, Greece
- *Corresponding Author:
- Dr. Konstantinos Fousekis
Technological Educational Institute of Western Greece
Psaron 6, Egio 25100, Greece
Tel: +302810229000
Email: konfousekis@gmail.com
Received date: May 25, 2016; Accepted date: July 04, 2016; Published date: July 16, 2016
Citation: Fousekis K, Kounavi E, Doriadis S, Mylonas K, Kallistratos E, et al. (2016) The Effectiveness of Instrument-assisted Soft Tissue Mobilization Technique (Ergon© Technique), Cupping and Ischaemic Pressure Techniques in the Treatment of Amateur Athletes΄ Myofascial Trigger Points . J Nov Physiother S3:009. doi:10.4172/2165-7025.S3-009
Copyright: © 2016 Fousekis K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Objective: To compare the effectiveness of a novel Instrument-assisted soft tissue mobilization technique (Ergon© Technique), cupping therapy, and ischaemic pressure technique in the treatment of active myofascial Trigger-points (MTrPs) at the low-back region of amateur soccer players. Design: Randomised controlled clinical trial. Methods: Seventy (70) amateur soccer players (age=24.76 ± 4.39; height=174.98 ± 8.31 cm; weight=73.26 ± 11.21 kg) were evaluated for the presence of active MTrPs in their low-back region and were randomly allocated to three subgroups. The first group (N=20) was treated with Εrgon-IASTM Technique©, the second (N=20) with a static application of cupping therapy and the third group (N=20) with ischaemic pressure. Ten (10) players received no treatment and served as controlsgroup. All athletes received one (1) therapeutic intervention per week for three (3) weeks. Outcome measures were MTrPs pain pressure threshold (PPT) and pain sensitivity (VAS). Results: All three therapeutic interventions led to a significant (p<0.05) reduction in MTrPs pain sensitivity and an increase in PPT at the end of the treatment compared with controls. The Εrgon©-IASTM Technique produced a significantly larger effect (p<0.05) in the reduction of pain and PPT during compression of MtrPs compared with cupping and ischaemic pressure technique. These therapeutic adaptations after Εrgon©-IASTM Technique application were evident even from the first treatment (p<0.05) and reinforced by the end of the third treatment (p<0.001). No significant difference (p>0.05) was observed between cupping and ischaemic pressure techniques for their impact on MTrPs. Conclusions: The Ergon©-IASTM technique can serve as a first treatment options for sports physiotherapists when they manage Low-back MTrPs in amateur athletes. More research is needed in order definite conclusion to be drawn regarding the effects of this novel therapeutic intervention on MTrPs.
Keywords
Myofascial trigger points; Ergon instrumment assisted soft-tissue mobilization technique; Cupping; Ischaemic compression technique
Introduction
Myofascial pain syndrome is defined as sensory, motor, and autonomic symptoms resulting from painful spots in the fascia surrounding skeletal muscle known as myofascial trigger points (MTrPs) [1,2]. MTrPs are associated with palpable nodules in taut bands of muscle fibers. Compression of these points may elicit a) motor dysfunction, b) local and referred tenderness, b) pain perceived at a different spot than the site of the painful stimulus (referred pain), c) transient contraction of the muscle (local twitch response) and d) autonomic phenomena. Diagnostic findings of MTrPs include severe ROM limitation, a palpable taut band with exquisitely tender nodule and familiar to patient pain elicited from pressure on painful Spots (jump sign) [3,4].
Etiology of myofascial pain is multifactorial including poor ergonomy and body biomechanics, acute or repetitive trauma, excessive or no exercise and vitamin deficiency [5,6]. Οther factors contributing to the development of MTrPs include psychosocial factors, such as high job pressure, psychological stress and anxiety [7,8]. MTrPs are thought to be involved in pain in tension headaches, low back pain syndromes; pelvic pain; and musculoskeletal pathologies such as bursitis, tendinopathies, and muscle strains [9,10].
MTrPs can be seen in the setting or athletic injury due to muscle asymmetries and imbalances, postural deficiencies, or secondary to repetitive injury and training overloading. Evidence to date reinforces the theory that MTrPs develop after muscular overuse and especially after eccentric overloading and submaximal-maximal concentric contractions [11,12]. A key factor is a localized ischemia, leading to the subsequent release of several inflammatory mediators in muscle tissue through a pH reduction [7]. Examples of the latter include MTrPs in quadratus lumbar in association with lumbar pathologies or gluteal trigger points in the presence of hip and pelvis overloading. More specifically, myofascial pain arising from trigger points in the low-back and gluteal region is a typical presentation in athletes who overload the hip area with shear forces like soccer players [13]. This type of myofascial pain may be local or referred and in the majority of the cases, is reproduced by the application of digital pressure to gluteal muscle trigger points [14].
Treatment of myofascial trigger points in non-athletic populations during the past has been based on invasive and noninvasive techniques. Invasive therapies include acupuncture, dry needling and injections [15]. Non-invasive techniques are osteopathic manual techniques, massage, stretching, application of heat and ice, TENS, ethyl chloride Spray and Stretch technique, ischemic pressure, cupping therapy, instrument-assisted soft tissue techniques (ΙΑSΤΜ) and a combination of them [16,17]. Nevertheless, the efficacy of the above methods is not clear since several researchers reported that many myofascial treatment techniques are poorly validated and not necessarily more effective than placebo [5,18]. It seems that the application of a noxious stimulus may be the key to obtaining improvements in pain sensation perception. Likewise, ischaemic pressure and dry needling, have shown benefits in releasing myofascial induced muscle spasm and aches [19,20].
Ischaemic compression using local application of sustained pressure over the MTrPs has been reported that reduces muscle spasm and therefore deactivates the MTrPs [21,22]. The benefits of ischemic compression that were described by several investigators have been attributed to several adaptations like a) separation of the actin-myosin cross fiber links, b) reflex vasodilation and subsequent flushing away of metabolites and substances that maintain muscle contraction and c) temporary suspension of the involuntary motor neuron activity. Lastly, it is also thought that the deep pressure also results in the release of endorphins which mask the perception of pain [21,22].
Instrument-assisted soft tissue mobilization techniques (IASTM) and cupping therapy techniques are procedures rapidly growing in popularity amongst athletes due to their effectiveness and efficiency in treating soft tissue restrictions while remaining non-invasive. IASTM techniques use special stainless steel instruments that enable clinicians to locate efficiently and treat soft tissue dysfunctions, such as fibrosis, adhesions, chronic inflammation, or degeneration [23,24]. Benefits from IASTM use include increased fibroblast proliferation, reduction in scar tissue and adhesions, increased vascular response, and remodeling of disorganized collagen fiber matrix [25]. IASTM technique also has been found that it results in clinical benefits such as improvements in range of motion, strength and pain perception following treatment [26,27]. Despite extensive use of IASTM techniques research regarding its effect on myofascial pain reduction, is limited. Gulick reported that IASTM (Graston Technique) does not differ regarding effectiveness on upper back MTrPs release compared to the control group [28].
Cupping is a therapeutic method that utilizes a glass or plastic cup to create negative pressure on the skin over a painful area for muscle spasm and pain reduction. The mechanism of cupping therapy is not clear, but some researchers suggest that placement of cups on the skin produces hyperemia, fascial release, and local stretching. Nevertheless, its therapeutic effect has not been proven through valid randomized control studies [29].
Although myofascial pain arising from MTrPs is a common problem in athletes, effective treatment strategies still elude us. Only one study in 59 male runners from Huguenin et al. [30] showed that dry needling and placebo needling of the gluteal trigger points resulted in subjective improvement in activity related muscle pain and tightness but not in straight leg raise or hip internal rotation range of motion. Unfortunately, we have no data comparing results between effective techniques like ischaemic pressure and novel therapeutic techniques like IASTM and cupping techniques from which to draw clinical conclusions about their effectiveness in athletic populations.
The purpose of the present study was two-fold to examine the presence of MTrPs in the low back and gluteal region of amateur athletes, and to compare the effectiveness of IASTM, cupping and ischaemic pressure techniques in MTrPs treatment. The following null hypothesis was tested: no difference exists among groups of amateur athletes�? receiving ischemic pressure, IASTM and cupping therapy versus control treatment in reducing MTrPs pain pressure sensitivity and pain intensity.
Methods
The study took place during the three-month period from June to August 2015. Following approval from Research Ethical Committee of the School of Health Sciences of Technological Educational Institute of Western Greece, seventy (70) male amateur soccer athletes (Age=24.76 ± 4,39; height=174.98 ± 8.31 cm; weight=73.26 ± 11.21 kg) recruited from local soccer clubs, advertisements, and referral from private medical clinics. The eligibility criteria were: a) amateur soccer players, b) aged 18 to 30; c) approximately same training regime (2-3 training sessions per week), d) presence of active MTrPs identifiable by spot tenderness in a taut, muscular band of quadratus lumborum and gluteal muscles (Maximus-medius) of the dominant side.
Exclusion criteria were: a) injury to the low back and lower extremities over the last six months; (b) skin lesion, (c) infection or inflammatory edema at MTrPs site. All athletes were given a full musculoskeletal physiotherapy assessment by KF, an experienced sports physiotherapist with training in MTrPs identification. After this first assessment seventy (70) soccer players met inclusion criteria and included in the study.
All subjects informed about the goals of the survey and agreed to participate. Patients gave written informed consent and randomly allocated to four experimental subgroups: a) the ischaemic compression (IC-TrPs, N=20) group, which received sustained ischaemic pressure on the MTrPs, b) the IASTM group that received Ergon© IASTM therapy to trigger points (IASTM-TrP, N=20), c) the group that received cupping therapy (C-TrP, N=20) or d) the control group (N=10). The three groups received three treatments over a three week period in total.
MTrPs evaluation
MTrPs were identified by palpation of taut muscle bands in the low back and gluteal region with the presence of a “jump sign” and referred pain when a firm pressure was applied. This task was performed by KF a licensed clinical physiotherapist with almost 20 years of clinical experience. Pressure sensitivity (in kg) of the MTrPs was assessed by a mechanical Algometer (Wagner Pain Test™ instrument - Model FPK/ FPN-Greenwich-USA) with a 1-cm diameter tip. Test-retest reliability of such equipment in assessing muscle function is reported to be relative high [31].
Interventions
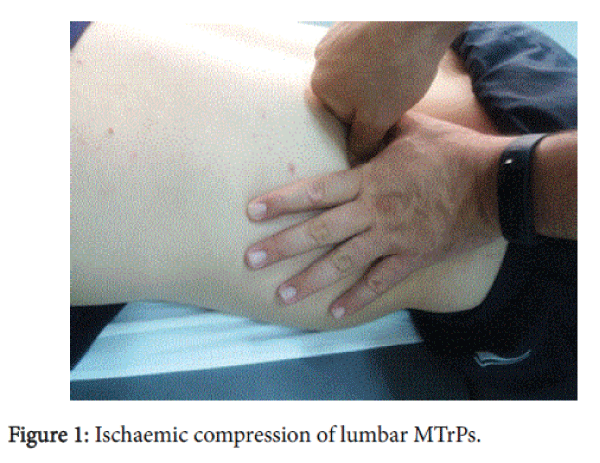
Iscaemic pressure: The IP-TrPs group received ischemic compression treatment at the three MTrPs of the gluteal and low-bak region. For this therapeutic procedure, the athlete was lying prone with the cervical spine in a neutral position. The therapist (KF) applied gradually increasing pressure to the MTrPs with the tip of his thumb until the sensation of pressure became one of pressure and pain (Figure 1). At that moment, the pressure was maintained until the discomfort perceived by the patient eased by around 50%, at which time pressure was increased until pain appeared again. This process was repeated for 90’’ [3].
Instrumment-assisted soft tissue mobilization techniques (Ergon© Technique)
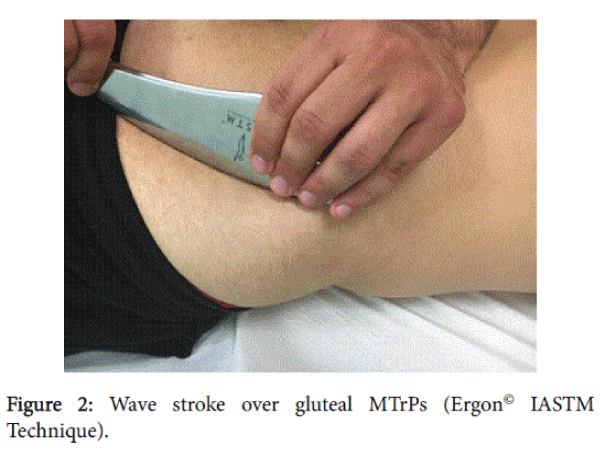
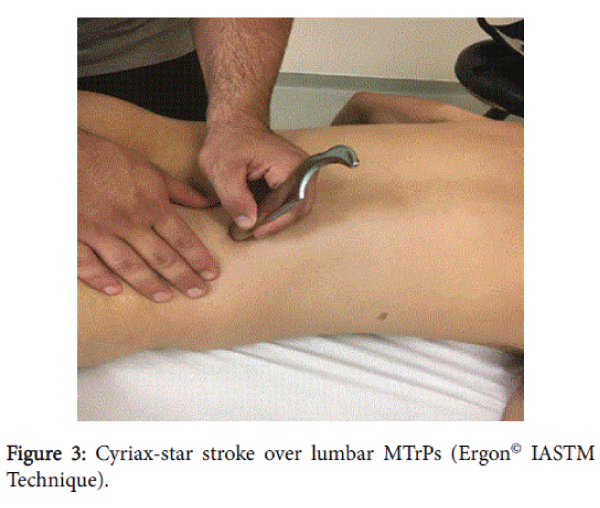
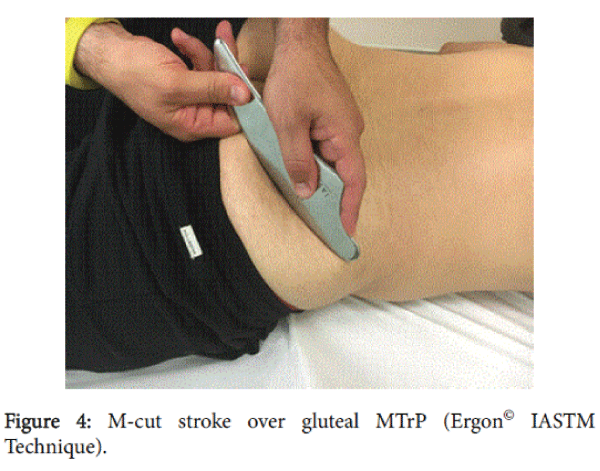
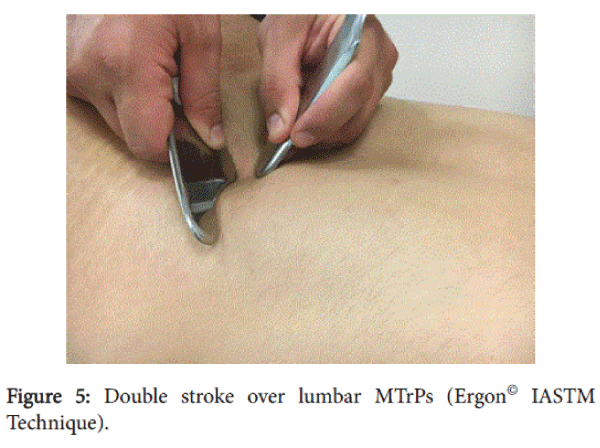
The IASTM-TrPS group received particular instrument-assisted soft tissue technique called Ergon© Iastm Technique on MTrPs [32]. Ergon© Technique is an innovative therapeutic approach that combines static and dynamic manipulation of soft tissues with specific clinical tools (Ergon© tools) aimed at treatment of myofascial dysfunctions. These techniques, when applied to specific areas of myofascial restrictions, can improve facial mobility and decrease muscle spasm and pain. For the application of Ergon© Technique, the patient was lying prone on the couch [32]. The therapist applied four (4) Ergon© strokes for two (2) minute on each MTrP with specific Ergon© IASTM Tools. Ergon© strokes used were a) the wave (Figure 2) b) the cyriax in star type of application (Figure 3) c) the m-cut stroke (Figure 4) d) the double stroke (Figure 5). The wave stroke involves linear facial applications, respectively, performed in all directions above and around the MtrPs. Cyriax-Star stroke is a therapeutic intervention applied just above the trigger point pain spot and with direction from the center to the periphery with the purpose of localized release and tissue stretching. M-cut stroke refers to a saw motion of IASTM tools which covers the entire area combining linear and vertical tools applications on soft tissue. The double-stroke technique involves the simultaneous use of two tools (Ergon© tools I and II) in a procedure where one tool stabilizes the anatomical spot to allow the “compression” and “lifting” of the MTrPs from the other tool. Ergon©IASTM techniques were applied by two researchers (KF and KM) which are Ergon© Technique certified trainers.
Cupping
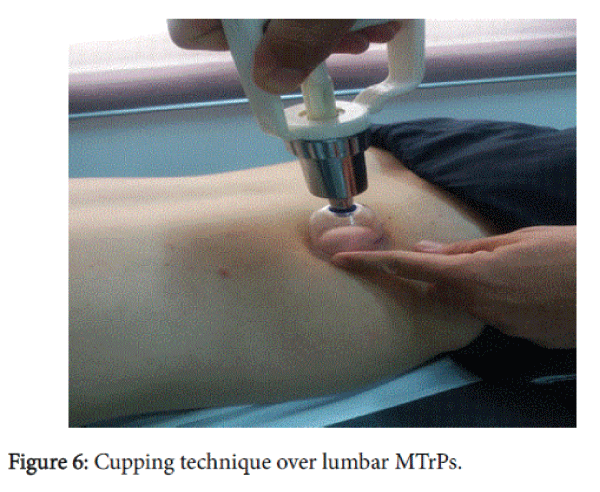
Cupping was performed by the study researcher (SD), who is trained in cupping and regularly performed cupping in his clinical practice. For cupping procedure patients were asked to lay prone on the massage couch. The cupping technique involved the static application of high-quality polycarbonate cupping jars (meridian cupping set, Durham-USA) on the three tTrPs for 5 minutes. Negative pressure inside cups was produced through a rubber pump which sucked the air out of the cups (Figure 6).
Evaluation
Ischaemic pressure technique: Primary outcome measures of the study were PPT and pain sensitivity. PPT of the primary MTrPs was measured in kg/cm2, using a mechanical Algometer (Wagner Pain Test™ instrument-Model FPK/FPN-Greenwich-USA) with a 1-cm diameter tip. Pain intensity over the active MTrP evoked by a second application of 2.5 kg/cm2 of pressure on the MTrP was measured on a visual analogue scale (VAS), where 0 (cm) was ‘least pain imaginable and 10 (cm) was ‘worst pain imaginable’, 'as proposed by Fernándezde- las-Peñas et al. [33]. These outcomes were assessed pre-and post treatment by an examiner blinded to a) the treatment allocation of the subject and b) the body side treated. Each athlete received three treatments (1/week) and six evaluations in total (pre and post each intervention).
Statistical method
Data were analyzed with SPSS version 11.5 (SPSS Inc., Chicago, Ill, USA) and ensured for their normal distribution using numerical (Shapiro-Wilk Test) and graphical methods (Normal Q-Q Plots). Comparison of treatment effects of tested techniques was achieved using one-way analysis of variance (ANOVA) after Bonferonni corrections. Statistical significances were tested at α=0.05 probability level.
Results
Pain Pressure Threshold (PPT) and Visual Analogue Scale (VAS) data before and after the implication of Cupping, Ergon© IASTM and Ischaemic pressure technique for the treatment of MTrPs in athletes are presented in Table 1. Descriptive data showed that although there was no differentiation in the control group [1st Measurement=7.94/3rd measurement=7.66], PPT scores for both three treatment techniques increased from the 1st till the 3rd evaluation.
| Variables | Techniques | 1st Intervention | 2nd Intervention | 3rd Intervention | |||
|---|---|---|---|---|---|---|---|
| Pre | Post | Pre | Post | Pre | Post | ||
| Mean±SD | Mean±SD | Mean±SD | Mean±SD | Mean±SD | Mean±SD | ||
| PTA | Cupping | 7,63±1.68 | 7.75±1.65 | 7.93±1.66 | 8.23±1.78 | 8.56±1.68 | 8.83±1.71 |
| Ergon© IASTM | 7.35±1.61 | 7.59±1.73 | 8.58±1.74 | 9.05±1.86 | 10±1.75 | 11.26±1.83 | |
| Ischaemic Pressure | 7.49±1.41 | 7.40±1.52 | 7.7±1.42 | 8.06±1.68 | 8.57±1.66 | 8.88±1.65 | |
| Controls | 7.94±1.55 | 8.14±1.59 | 7,6±1.56 | 7.6±1.63 | 7.66±1.41 | 7.66±1.21 | |
| VAS | Cupping | 6.25±1.57 | 6.56±1.28 | 5.7±1.38 | 5.57±1.62 | 4.74±1.45 | 4.20±1.73 |
| Ergon© IASTM | 5.77±1.62 | 5.71±1.54 | 4.93±1.38 | 4.44±1.47 | 3.36±1.53 | 2.17±1.72 | |
| Ischaemic Pressure | 6.2±1.58 | 6.12±1.58 | 5.74±1.25 | 5.22±1.70 | 4.37±1.61 | 3.89±1.80 | |
| Controls | 5.92±1.66 | 6.29±1.51 | 6.18±1,33 | 6.29±1.56 | 6.22±1.59 | 6.22±1.20 | |
Table 1: Pain pressure threshold (PPT) and visual analogue scale (VAS) descriptive data before and after the implication of cupping, Ergon© IASTM and Ischaemic pressure technique for the treatment of MTrPs in athletes.
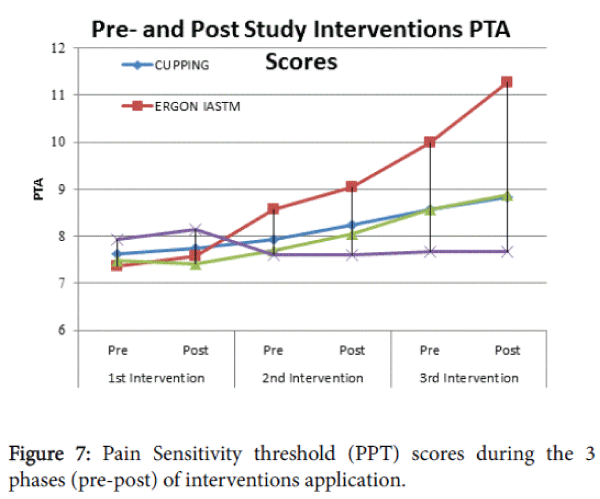
One-way ANOVA testing revealed statistically significant differences (p <0.05) between the effects of treatments tested. More precisely, post-hoc comparisons showed a statistical significant PPT rise in the athletes received IASTM-ERGON treatment compared with those received cupping (Pre 2nd evaluation: p=0.030, Post second evaluation: p=0.015), iscaemic pressure (Pre 2nd evaluation: p=0.003, Post 2nd evaluation: p=0.003) and controls (Pre 2nd evaluation: p= 0.007 , Post 2nd evaluation p=0.000 ) at the time pre ( p=0.009) and post (p=0.002) 2nd application of techniques (Figure 7).
This superiority of athletes receiving ERGON© IASTM in PPT scores in comparison with athletes receiving Cupping and Iscaemic pressure was further reinforced pre (p<0.001) and post (p<0.001) the 3rd application of therapeutic techniques.
PPT scores of athletes received cupping and ischemic pressure as a treatment of their MTrPs were almost identical (p>0.05) from the start till the end of the study. Nevertheless both of these techniques led to a significant increase in PPT scores after the 2nd and 3rd interventions compared with the control group (p<0.05).
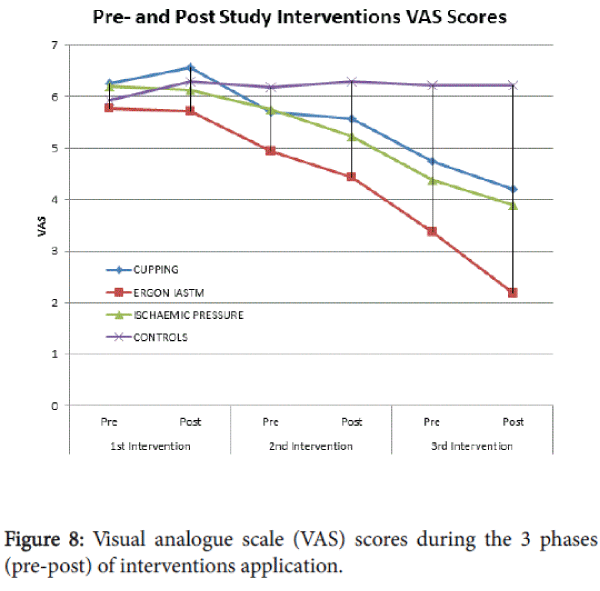
The application of Ergon© IASTM technique led to better results compared with other treatment methods in terms of pain sensitivity (VAS, Figure 8). Even after the 1st treatment Ergon© IASTM technique resulted in significant decrease in pain sensitivity compared with cupping technique (p=0.014).
As for PPT scores, the pain sensitivity of MTrPs in athletes receiving Ergon© IASTM was significant lower than those receiving the other two techniques (iscaemic/cupping) and controls at the evaluation pre- (p=0.001) and post(p=0.001) 2nd application of the techniqes.
No significant differences (p>0.05) was observed for the effects of cupping compared with those of iscaemic pressure during the 3 phases of the study. Neverthelles, both of three therapeutic interventions (Ergon© IASTM, Cupping, Ischaemic pressre) led to significant decrease (p<0.005) in MTrPs pain sensitivity compared with control group at the 2nd and 3nd evaluation.
Discussion
Myofascial pain syndrome (MPS) is presented with motor, sensory, and autonomic manifestations. Motor aspects of MTrPs may include disturbed muscle functional capacity regarding muscular weakness due to motor inhibition and restricted ROM due to muscular stiffness [34].
Sensory adaptations may include local tenderness and referral of pain to a distant anatomical site. MTrPs also are associated with peripheral sensitization and an increase in responsiveness of nociceptors. Signs of peripheral awareness are allodynia and hyperalgesia [34].
Several possible aetiological factors and mechanisms can lead to the development of MTrPs, including amongst others: a) myofascial overload with maximal/submaximal concentric or eccentric contractions, b) direct trauma c) low-level muscle contractions and d) uneven intramuscular pressure distribution.
Concentric and eccentric contractions inevitably lead to capillary constrictions, impaired blood flow, ischemia, and hypoxia. Hypoxia, which appears to be one of the most important precursors for the development of MTrPs in athletes contributes to the development of more muscle damage (a local acidic milieu) and sensitization of muscle nociceptors [7].
The findings of the present study reinforce previous theories about etiology of MTrPs as the vast majority of amateur athletes evaluated in the present study had active MTrPS in areas particularly strained with concentric and eccentric contractions as the lower back and gluteal regions. More precisely 88% of athletes evaluated for inclusion in the study had active quadratus lumborum MTrPs and 99% of them had gluteal MTrPs and included in the survey.
Al three therapeutical techniques (Ergon© IASTM, Cupping, and ischaemic pressure technique) evaluated in the study increased pain pressure threshold (PPT) and decreased pain sensitivity (VAS) of myofascial TrPs at the low back and hip region of amateur soccer players compared with controls. These positive adaptations were evident even at the time of one week after the initial application of techniques implicating that a single bout of therapy is by far better than doing nothing for MTrPS. These findings were in agreement with those reported from several studies evaluating the effect of ischaemic pressure as a treatment of MTrPs [35-37]. The positive effect of Ischaemic pressure in alleviating symptoms of TrPs can be attributed to ischemia and hyperemia that follows. Local ischemia is connected to a lowered pH and a subsequent release of several inflammatory mediators in muscle tissue while hyperemia can contribute to clearance of the muscle from the derivatives of inflammation and pain metabolites and thus desensitize nerve endings [36,37]. Cupping therapy, although not studied efficiently, seems that it also has a critical impact on myofascial MTrPs treatment that can also be attributed to tissue stretching and hyperemia provoked by their application on the body [38].
The Ergon© IASTM technique used in this study was proved superior in decreasing myofascial pain originated from lumbar and gluteal MTrPs in amateur athletes comparatively with ischaemic pressure and cupping therapy. The athletes reported better results even after the 1st application of Ergon© IASTM technique in comparison with the other methods and this gain in pain sensitivity and PPT was reinforced after the next two applications. Disabling myofascial pain after IASTM application can be theoretically attributed to three main mechanisms that have been reported in the literature: a) local temperature and blood flow increase, b) localized tissue manipulation and stretch and c) reduction of fascial adhesions and restrictions. IASTM techniques have been reported that effectively affects the fascial system of the human body treating fascial adhesions and constraints. These “adhesions” can affect the muscular functions, reduce blood flow and nutrition of tissues, and can lead to the development of myofascial MTrPs. The blood-flow theory is lately supported by the findings of Portillo-Soto et al. [39] in a study aiming at evaluating the effects of the IASTM (Graston © Technique) and massage therapy on calf blood flow, using skin temperature measures. The researchers reported that massage and IASTM techniques increased skin temperature and thus local circulation significantly in twenty-eight participants. Furthermore, the researchers showed that the peak temperature was achieved at 25 minutes after treatment indicating that the therapeutic effects of IASTM therapy remain in the place for several minutes after the end of the treatment. Findings of the present study are in disagreement with those of Gulick [28] reporting no effect of Graston IASTM technique in the therapy of upper-back MTrPS compared with control group. These differences can be explained by the types of IASTM techniques applied as well from methodological issues (type and time of application). The Ergon© IASTM technique used in this study is a more aggressive technique and with different application strokes than Graston© Technique. Furthermore, the selected Ergon© IASTM strokes were applied directly over the each MTrPS unlike Graston IASTM maneuvers chosen by Gulick [28] which were implemented in a more general fashion. The time of application also was different as each Ergon© IASTM stroke was applied for 3 minutes continuously on the MTrPS while the Graston© IASTM strokes were applied consistently for one minute in the study of Gullic [28].
The main limitations of the present study include deficits in participants selection technique as well as methodological issues. All study participants were athletes of local amateur soccer clubs, and their selection was not based on random sampling. Also, the evaluation of the effect of therapeutic techniques in the treatment of MTrPs was based only on the assessment of the sense of pain and pressure pain threshold. Other possible critical adjustments to the functional capacity of athletes from the existence of trigger points as negative adaptations in joint range of motion, strength and neuromuscular control were not evaluated in this study. Moreover, the evaluation of the impact of therapeutic applications had short-term character and was limited to three (3) weeks that lasted the research. Another significant methodological issue that has been recognized as a possible source of measurement errors is the amount of pressure exerted through algometer as maintaining a constant pressure rate reported as the most challenging aspect of algometer [40,41].
An ideal study evaluating the effect of various techniques on the reduction of adverse effects of MTrPs should assess the therapeutic effect of applied techniques in all the aspects of the functional capacity of athletes and must have long-term evaluation and re-evaluation planning. However, the present study is innovative as it assessed comparatively the effect of two novel therapeutic applications such as the Ergon© IASTM and cupping technique alongside with ischemic pressure method for which there is moderate evidence that positively contributes to MTrPs symptoms reduce. Moreover, the present study also assessed MTrPs in lumbar and hip region, which are areas that have been poorly studied.
Conclusions
MTrPs evaluation and treatment is a challenging condition for both the sports physical therapists and athletes. Ergon© IASTM, cupping, and ischemic pressure techniques are effective, but not comparable, in reducing tenderness of myofascial trigger points (MTrPs). Ergon© IASTM technique seem to has significantly better results in reducing the adverse effects of MTrPs than both other two techniques as its application resulted in a meaningful statistical improvement of pain symptoms. The findings of the present study should be confirmed by future trials with better methodological designs so as to draw definitive conclusions.
References
- Baldry PE (1989) Acupuncture, trigger points, and musculoskeletal pain. Churchill Livingstone, Edinburgh, London, UK.
- Malanga GA, Cruz Colon EJ (2010) Myofascial low back pain: a review. Phys Med RehabilClin N Am 21: 711-724.
- Simons DG, Travell JG, Simons LS (1999) Travell& Simons' myofascial pain and dysfunction: upper half of body. Lippincott Williams & Wilkins, Philadelphia, Pennsylvania, United States.
- Alvarez DJ, Rockwell PG (2002) Trigger points: diagnosis and management. Am Fam Physician 65: 653-660.
- Dommerholt J, Bron C, Franssen J (2006) Myofascial trigger points: an evidence-informed review. Journal of Manual & Manipulative Therapy 14: 203-221.
- Gerwin RD (2010) Myofascial pain syndrome. In Muscle pain: Diagnosis and Treatment. Springer Berlin, Heidelberg, Germany.
- Bron C, Dommerholt JD (2012) Etiology of myofascial trigger points.Curr Pain Headache Rep 16: 439-444.
- Gerwin RD (2005) A review of myofascial pain and fibromyalgia--factors that promote their persistence.Acupunct Med 23: 121-134.
- Gerwin RD (2001) Classification, epidemiology, and natural history of myofascial pain syndrome.Curr Pain Headache Rep 5: 412-420.
- Travell JG, Simons DG (1992) Myofascial pain and dysfunction. Williams & Wilkins, Philadelphia, Pennsylvania, United States.
- Slobounov SM (2008) Injuries in athletics: Causes and consequences. Springer Science & Business Media, Berlin, Germany.
- Itoh K, Okada K, Kawakita K (2004) A proposed experimental model of myofascial trigger points in human muscle after slow eccentric exercise.Acupunct Med 22: 2-12.
- Simons DG, Travell JG (1983) Myofascial origins of low back pain. 3. Pelvic and lower extremity muscles.Postgrad Med 73: 99-105, 108.
- Mense S, Simons DG, Russell IJ (2001) Muscle pain: understanding its nature, diagnosis, and treatment. Lippincott Williams & Wilkins, Philadelphia, Pennsylvania, United States.
- Lavelle ED, Lavelle W, Smith HS (2007) Myofascial trigger points.AnesthesiolClin 25: 841-851.
- Gam AN, Warming S, Larsen LH, Jensen B, Høydalsmo O, et al. (1998) Treatment of myofascial trigger-points with ultrasound combined with massage and exercise--a randomised controlled trial.Pain 77: 73-79.
- Simons DG (2002) Understanding effective treatments of myofascial trigger points. Journal of Bodywork and movement Therapies 6: 81-88.
- Huguenin LK (2004) Myofascial trigger points: the current evidence. Physical therapy in Sport 5: 2-12.
- Hanten WP, Olson SL, Butts NL, Nowicki AL (2000) Effectiveness of a home program of ischemic pressure followed by sustained stretch for treatment of myofascial trigger points. Physical therapy 80: 997-1003.
- Edwards J, Knowles N (2003) Superficial dry needling and active stretching in the treatment of myofascial pain--a randomised controlled trial.Acupunct Med 21: 80-86.
- Iqbal A, Khan SA, Miraj M (2010) Efficacy of ischaemic compression technique in combination with strain counterstrain technique in managing upper trapezius myofascial trigger point pain. Indian Journal of Physiotherapy and Occupational Therapy 4: 10-15.
- Grieve R, Barnett S, Coghill N, Cramp F (2013) Myofascial trigger point therapy for triceps surae dysfunction: a case series.Man Ther 18: 519-525.
- Southerst D (2011) Myofascial trigger points: pathophysiology and evidence-informed diagnosis and management. Churchill Livingstone, London, UK.
- Laudner K, Compton BD, McLoda TA, Walters CM (2014) Acute effects of instrument assisted soft tissue mobilization for improving posterior shoulder range of motion in collegiate baseball players. Int J Sports PhysTher 9: 1-7.
- Hammer W, Pfefer M (1998) Treatment of a case of subacute lumbar compartment syndrome using the Graston Technique. J Manipulative PhysiolTher 28: 199-204.
- Melham TJ, Sevier TL, Malnofski MJ, Wilson JK, Helfst RH Jr (1998) Chronic ankle pain and fibrosis successfully treated with a new noninvasive augmented soft tissue mobilization technique (ASTM): a case report.Med Sci Sports Exerc 30: 801-804.
- Wilson J, Sevier T, Helfst R, Honing E, Thomann A (2000) Comparison of rehabilitation methods in the treatment of patellar tendinitis. J Sports Rehabil 9: 304-314.
- Gulick DT (2014) Influence of instrument assisted soft tissue treatment techniques on myofascial trigger points.J BodywMovTher 18: 602-607.
- Kim JI, Lee MS, Lee DH, Boddy K, Ernst E (2011) Cupping for treating pain: a systematic review.Evid Based Complement Alternat Med 2011: 467014.
- Huguenin L, Brukner PD, McCrory P, Smith P, Wajswelner H, et al. (2005) Effect of dry needling of gluteal muscles on straight leg raise: a randomised, placebo controlled, double blind trial. Br J Sports Med 39: 84-90.
- Gulick DT, Palombaro K, Lattanzi JB (2011) Effect of ischemic pressure using a Backnobber II device on discomfort associated with myofascial trigger points.J BodywMovTher 15: 319-325.
- www.ergontechnique.com
- Fernández-de-las-Peñas C, Alonso-Blanco C, Fernández-Carnero J, Miangolarra-Page JC (2006) The immediate effect of ischemic compression technique and transverse friction massage on tenderness of active and latent myofascial trigger points: a pilot study. J Bodywork MovTher 10: 3-9.
- Lucas KR, Polus BI, Rich PS (2004) Latent myofascial trigger points: Their effect on muscle activation and movement efficiency. J Bodywork MovTher 8: 160-166.
- Kostopoulos D, Nelson Jr AJ, Ingber RS, Larkin RW (2008) Reduction of spontaneous electrical activity and pain perception of trigger points in the upper trapezius muscle through trigger point compression and passive stretching. Journal of Musculoskeletal Pain 16: 266-278.
- Gemmell H, Miller P, Nordstrom H (2008) Immediate effect of ischaemic compression and trigger point pressure release on neck pain and upper trapezius trigger points: A randomised controlled trial. Clinical Chiropractic 11: 30-36.
- Aguilera FJM, Martín DP, Masanet RA, Botella AC, Soler LB, et al. (2009) Immediate effect of ultrasound and ischemic compression techniques for the treatment of trapezius latent myofascial trigger points in healthy subjects: a randomized controlled study. J Manipulative PhysiolTher 32: 515-520.
- Lauche R, Cramer H, Hohmann C, Choi KE, Rampp T, et al. (2011) The effect of traditional cupping on pain and mechanical thresholds in patients with chronic nonspecific neck pain: a randomised controlled pilot study. Evid Based Complement Alternat Med 2012: 429718.
- Portillo-Soto A, Eberman LE, Demchak TJ, Peebles C (2014) Comparison of blood flow changes with soft tissue mobilization and massage therapy.J Altern Complement Med 20: 932-936.
- Hakgüder A, Birtane M, Gürcan S, Kokino S, Turan FN (2003) Efficacy of low level laser therapy in myofascial pain syndrome: an algometric and thermographic evaluation.Lasers Surg Med 33: 339-343.
- Chesterton LS, Sim J, Wright CC, Foster NE (2007) Interrater reliability of algometry in measuring pressure pain thresholds in healthy humans, using multiple raters. Clin J Pain 23: 760-766.
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 21803
- [From(publication date):
specialissue-2016 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 20327
- PDF downloads : 1476