Research Article Open Access
Supplemental Nutrition Assistance Program (SNAP) Participant’s Proximity to Healthy Food Availability within Convenience Stores and the Association with Dietary Intake, Fayette County, Ky 2010-2011
Kelly J Sorge* and Alison A Gustafson
Department of Dietetics and Human Nutrition, University of Kentucky, Lexington, KY 40506, USA
- *Corresponding Author:
- Kelly Sorge
Department of Dietetics and Human Nutrition
University of Kentucky 524 Angliana Ave Apt 4217
Lexington, KY 40508, USA
Tel: (262) 366-0418
E-mail: Kjsorge12@uky.edu, kjso222@g.uky.edu
Received date: July 16, 2013; Accepted date: October 07, 2013; Published date: October 09, 2013
Citation: Sorge KJ, Gustafson AA (2013) Supplemental Nutrition Assistance Program (SNAP) Participant’s Proximity to Healthy Food Availability within Convenience Stores and the Association with Dietary Intake, Fayette County, Ky 2010-2011. J Community Med Health Educ 3:241. doi:
Copyright: © 2013Sorge KJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Community Medicine & Health Education
Abstract
Background: Food environment has been shown to affect the dietary intake of an individual. It is hypothesized that the type of food available in convenience stores and the proximity of those stores to a consumer may influence the purchasing decisions of those shopping a these food outlets. Methods: A cross-sectional survey was used to assess the dietary intake of SNAP participants in Fayette County, Kentucky, compared to the availability of healthful foods options at convenience stores and gas stations, which were within a close proximity to their homes (ten minute drive time or within 20 miles). Food audits were conducted in 35 gas stations and food marts, a total availability score ranged from 0-16, price was scored based on a similar protocol to NEMS-S. A higher scores will indicate better availability and price of healthy foods. 24-hour dietary recalls were then collected from 147 participants to obtain Healthy Eating Index scores. Results: On average, SNAP participants did not meet the daily dietary recommendations for consuming fruits and vegetables. Stores with more healthful options were an average of nine miles and produced an average HES score for participants of 1.03. Where as stores with low availability of healthful options were only located an average of two miles away and produced an average HES score for participants of 1.06. Among those who live close to gas stations with low availability of healthy food items was associated with lower odds of consuming at least one serving of fruit (OR 0.84 95% CI [0.60, 0.95]), and lower odds of consuming one serving of milk (OR 0.88 95% CI [0.72, 0.96]) compared to those who live farther away. Proximity to convenience stores and pharmacies with low availability of healthy food had lower odds of consuming more than five servings of grains per day (OR 0.87 95% CI [0.78, 0.95]) compared to those who live farther away. Conclusion: The results indicate that there is a significant association between having healthful food available at convenience stores and the dietary intake of those living within close proximity to those stores. This implies that there is a need for further interventions on the community level to make available more healthy food choices at these stores.
Keywords
Food availability; Convenience store; Snap participants; Dietary intake
Introduction
In recent years many nutritional studies have addressed the issue of food environment and its correlation to an individual’s dietary intake and weight status. More specifically, convenience and corner stores have been highlighted in this research and their relationship with Supplemental Nutrition Assistance Program (SNAP) participants [1-9]. In a broad view of research findings, a conclusion cannot be met or agreed upon on how an individual’s access to healthier options at a convenience store has an effect on dietary intake or weight status [2]. Nevertheless, it is repeatedly seen that food environment is in someway associated with individual’s dietary choices [3,6,9-11]. By method of a cross sectional analysis, results showed that SNAP participants has a positive association with high waist circumference, BMI and other metabolic risk factors [12]. In a longitudinal analysis of participants, it was found that the availability of convenience stores within walking distance (1/4 mile) to a child’s residence was associated with greater risk of overweight or obesity and having an increased BMI [11]. Further research resulted in the findings that the greater the perceived time to a food outlet, such as a convenience store, was associated with less frequent purchasing of sugar sweetened beverages and energy dense foods [9]. Store classification has also shown to be a factor of food availability. An in-store survey of small food stores produced the information that stores classified as a convenience store carried fewer nutritious and fresh food items then those categorized as small grocery stores [13]. Another study explains that stocking more healthful foods in a convenience store would hurt profits because of the larger demand for the energy dense foods and sweetened beverages and not fruits or vegetables [10]. On the contrary, findings from other reputable research have concluded that food environment and availability cannot be directly linked to higher BMI or weight status [6]. An alternative conclusion that has been met, is that store type is not linked to dietary intake or weight status of it’s consumers, but it is the food that is offered in a store that indicates the health of those who are shopping in them [7,8]. Yet, opposing findings produce no evidence of a definite correlation to what convenience stores offer for sale and its consumer’s dietary intake [14]. In knowing whether food environment is a contributor to obesity and other chronic diseases would help give a starting point to major interventions and prevention methods.
Methods
Study region and design
The spatial area under analysis was Fayette County, KY (population=295,803). Fayette County is 283 square miles with approximately 1,000 people per square mile, with a small urban center as the county seat. The racial and ethnic composition of Fayette County is 76% White, 15% Black, 7% Hispanic or Latino, and 2% Asian based on the United States Census Bureau 2010 [15]. The study was reviewed and determined exempt from the University of Kentucky Internal Review Board. Before collection of data began, as it was a secondary data analysis. The study design was a cross-sectional survey assessing dietary intake and the consumer food environment among gas stations and convenience stores in Fayette County. The study took place January 2010-January 2011. This study was approved by IRB and a letter describing the study and sampling was given to each store manager.
Study sample
Limited resource families were identified and eligible based on participating in either a Nutrition Education Program or SNAP-Ed program in Kentucky during the years of 2010-2011. Individuals were excluded from analysis if baseline line data were missing (n=2).
Recruitment: Limited resource families were recruited through local county agencies, health departments, SNAP benefit offices and commodity distribution programs. Adults age 18 years and over with complete information on all independent, dependent and covariates (complete case) were included for analysis (n=147).
Objective measures of the retail food environment
Identifying food stores around SNAP participants home: A total of n=35 gas stations with food marts, convenience stores, and pharmacies within a ten minute drive time or about 20 miles were identified using ArcMap software, distance was calculated by reported home zip code and street name. Because of the large percentage of calories consumed/purchased from these food venues they were the only types include in the study. Store addresses were purchased from InfoUSA in June 2011 were categorized based on the NAICS codes, convenience stores (446110), gas stations with food marts (447110). Address match rate was 88%. Store’s locations were verified by visiting each food venue.
Food availability within convenience stores
Food store audits of corner stores assessed if the availability and price of the following food items; high fiber cereal with at least 7 grams of fiber, fruit (canned, whole, or frozen), vegetable (canned, whole, or frozen), muffin with at less than 5 grams of sugar, baked chips (4oz bag), water (12oz bottle), soda (12oz bottle or can), whole grain bread, milk (skim, 1%, 2%, and whole). This list was adapted from previous corner store audits conducted in Philadelphia [16] but also with consideration for food that SNAP participants could purchase with EBT cards [17]. The store audits were conducted Monday-Friday between 9-5pm by graduate students trained in store audit collection. Availability and price were collected for all food items with price being recorded as per unit or ounce for each food item. A total availability score ranged from 0-16, price was scored based on a similar protocol to NEMS-S [18] with a possible range in scores from 0-16. Higher scores indicated stores with better availability and price of healthy foods. The total NEMS-S score range from all stores was 6-20 and total score retained a linear shape.
Fieldwork and inter-rater reliability
Two trained college students conducted all the audits for all 35 convenience stores and gas stations with food marts. All venues listed were located and open. All researchers reviewed audit sheets for completeness and accuracy. One student conducted the food store audits in week one while the second student conducted the audit in the same stores at week two. A kappa coefficient was calculated for each food venue to test inter-rater reliability. The kappa threshold, k ≥ 0.60, was used to determine if re-audits were necessary. If a kappa coefficient was lower than 0.60, the establishment was re-audited. Kappa coefficients ranged from 0.90-0.95
Diet quality-healthy eating index score
A 24-hour dietary recall was obtained, in person, from every participant by a Cooperative Extension agent trained in data collection. The type and amount of foods consumed were recalled using aids such as abstract food models, special charts, measuring cups, and rulers to help in quantifying the amounts consumed. Special probes were used to help the recall of commonly forgotten items such as condiments, accompaniments, and fast food. At this time baseline data was also collected and recorded (gender, etc). Based on these data, dietary habits as well as the dietary intake of proteins, carbohydrates, fat, and total calories were quantified using the Nutrition Software (“NutWin”) [19].
Dietary intake data, as assessed by the 24-h recall, were used to calculate Healthy Eating Index (HEI) scores. HEI comprises 10 components (saturated fat, total fat, cholesterol, sodium, grain, fruit, dairy, meat, and vegetable intakes, plus a measure of dietary variety), each contributing 10 points to the maximum possible score of 100 [20]. Food serving amounts were computed from food consumption data using factors derived from the serving-size assumptions given in the Food Guide Pyramid (USDA). Ten points were scored if saturated fat ≤ 10% of energy, total fat ≤ 30% of energy, cholesterol ≤ 300 mg, and sodium ≤ 2.4 mg. A zero score reflected ≥ 15% of energy for saturated fat, ≥ 45% of energy for total fat, cholesterol ≥ 450 mg, and sodium ≥ 4.8 mg; between these two cutoff points, scores were scaled proportionately. A similar process was used for food groups (grains, fruits, vegetables, dairy, and meat): consumption of the recommended number of servings for the individual’s age and sex resulted in a score of 10, with a score of 0 if no servings were consumed. A variety component was also used with a scoring method of ≥8 food items=10 pts and 8 or fewer =0.The maximum overall score for the 10 components combined was 100.
Statistical analyses
Descriptive statistics were conducted for means, proportions, and standard deviations. To test for differences between group means t-test were used. To test the association between proximity to stores with low or high availability of healthy food in each store and the dietary outcomes, multivariate logistic regression was used. Likelihood ratio test was used to test for model fit. Type I error rate was set at alpha 0.05. All models were adjusted for age, race, gender, number of children in household, and population density. Type I error rate was set at alpha 0.05. All analyses were conducted with Stata (version 11.0, 2009, College Station, TX) 32.
Results
The final sample of n=147 consisted of 49% female, 67% white, and 65% reported no children in the household (Table 1). On average SNAP participants did not consume the recommended number of fruits and vegetables. Additionally, there were significant differences between proximity to stores with low and high availability of healthy food (p=0.001). Gas stations with low availability of healthy food were on average two miles from SNAP participants home, while gas stations with high availability of healthy food were nine miles from SNAP participants home. Convenience stores and pharmacies with low availability of healthy food were on average 16 miles from SNAP participants home, while convenience stores and pharmacies with high availability were 11 miles from participant’s homes.
| Percent/Mean | SD | ||
|---|---|---|---|
| Gender | |||
| Female | 49% | ||
| Male | 51% | ||
| Race | |||
| White | 67% | ||
| African American | 25% | ||
| Other | 8% | ||
| Number of Children | |||
| No children in HH | 65% | ||
| 1 child in HH | 22% | ||
| 2-3 children in HH | 10% | ||
| 4 or more | 3% | ||
| Household Income | |||
| less than $1 | 85% | ||
| Not reported | 15% | ||
| Age (yrs) | 37 | 13.13 | |
| Dietary Intake (servings/week) | |||
| Fruit | 0.68 | 0.07 | |
| Vegetable | 1.63 | 0.1 | |
| Grain | 5.49 | 0.33 | |
| Milk | 1.38 | 0.11 | |
| Healthy Eating Index Score | |||
| Total | 59.03 | 1.16 | |
| Miles to participants home for each food venue | |||
| Gas stations with low availability of healthy food | 2.4 | 0.09 | 0.001 |
| Gas stations with high availability of healthy food | 9.49 | 0.26 | |
| Convenience stores with low availability of healthy food | 16.22 | 0.2 | 0.001 |
| Convenience stores with high availability of healthy food | 11.37 | 0.34 |
Table 1: Demographics of Fayette County Supplemental Nutrition Assistance Program participants and consumer food environment 2011.
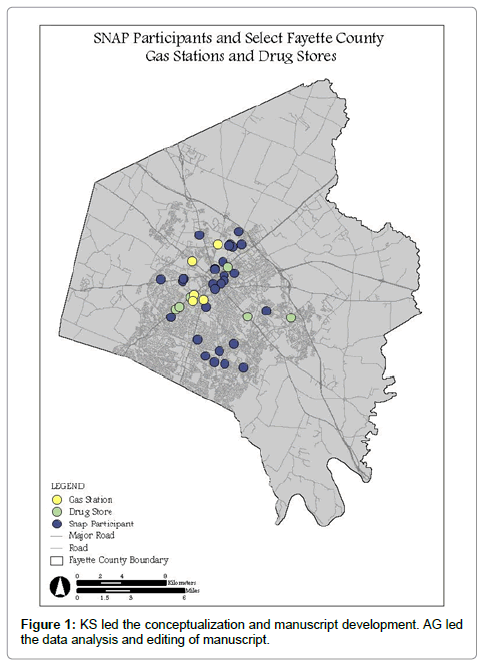
As Figure 1 shows several residents live far from gas stations and convenience stores, but overall there is an abundance of this venue type within less than 10 miles.
As show in Table 2, among those who live close to gas stations with low availability of healthy food items was associated with lower odds of consuming at least one serving of fruit (OR 0.84 95% CI [0.60, 0.95]), and lower odds of consuming one serving of milk (OR 0.88 95% CI [0.72, 0.96]) compared to those who live farther away. Lastly, proximity to convenience stores and pharmacies with low availability of healthy food had lower odds of consuming more than five servings of grains per day (OR 0.87 95% CI [0.78, 0.95]) compared to those who live farther away.
| Gas stations with low nems-s score (n= 12) | Gas stations with high nems-s score (n= 9) | Convenience stores with low nems-s score (n= 6) | Convenience stores with high nems-s score (n= 8) | |
|---|---|---|---|---|
| HEI Score | 1.17 (0.86, 1.61) | 0.96 (0.87, 1.06) | 0.95 (0.87, 1.02) | 1.10 (0.96, 1.26) |
| Fruit | 0.84 (0.60, 0.95) | 1.09 (0.98, 1.21) | 1.06 (0.98, 1.15) | 0.90 (0.78, 1.04) |
| Vegetable | 1.04 (0.75, 1.42) | 1.10 (0.97, 1.25) | 1.06 (0.97, 1.16) | 1.01 (0.88, 1.15) |
| Milk | 0.88 (0.72, 0.96) | 0.96 (0.87, 1.06) | 0.95 (0.87, 1.03) | 1.10 (0.96, 1.26) |
| Grain | 1.11 (0.81, 1.51) | 0.96 (0.87, 1.07) | 0.87 (0.78, 0.95) | 1.07 (0.94, 1.22) |
| References for HEI score is less than 59 | ||||
| Reference is less than 1 serving of fruit, vegetable, and milk | ||||
| Reference is less than 5 servings of grains per day | ||||
| All models adjusted for race, education, gender, no. children in household, and population density | ||||
Table 2: Odds of consuming healthy foods among SNAP participants by proximity to convenience stores and gas stations with low and high availability of healthy foods.
Discussion
In recent years data collection on the association between dietary intake and food environment has begun to rise. The results from this study shows an association of the availability of healthy food options at convenience stores and pharmacies, and the dietary outcomes of those SNAP participants living in a close proximity to these stores. Those who live close to a store with less healthy foods had lower odds of consuming healthy food. Although not surprising, it does suggest that proximity to venues selling less healthy food where an individual is most likely already shopping might make the healthy choice the hard choice. This study is not the first to suggest an association between availability of a healthy food and the intake of those around it. Several studies have found a strong association between fruit and vegetable intake and shopping at convenience stores. The availability of fresh produce at these stores was positively associated with amount of fruit and vegetable intake [21,22].
Conversely, other studies have come up with results that would suggest no association. A study conducted in the metropolitan Minneapolis area found no significant association between the convenience store purchasing and fruit and vegetable intake. This study concluded that many other factors, such as social, cultural and personal preference, are what effects dietary intake [23]. While in another international study, there was no association or pattern found in the subject’s access to a certain store and their dietary intake [24]. However, they most likely came up with different results because the demographic of participants in the studies differed. Different populations may be more or less sensitive to proximity and availability within food venues relative to other sub-groups. Recent systematic reviews have suggested the proximity and availability within food venues may be a determinant in dietary intake depending on the geographic area, such as United States versus Europe or urban versus rural, and within sub-populations [25,26]. Given this low-income population whose mode of travel are limited, proximity to healthy options within stores may have a greater effect on intake relative to other populations where distance and travel accommodations to a store are not a factor.
There are several limitations to the study worth noting. The first limitation is that exact location of where the SNAP participants shop was not collected. However, since we covered all the stores within a tenminute drive time from their home we can estimate that they might choose to shop at one of these stores. Individuals’ most likely shop outside a ten minute drive for food and since this study did not capture daily living patterns, future studies will be addressing daily living patterns as a way to understand how low-income adults daily patterns influence food shopping behaviors and dietary outcomes. Second, dietary intake was self-reported which is subject to misclassification. However, all participants were low-income and had the same agents collecting dietary data. Third, food stores may have closed from the time the survey was conducted and the audits were done. However, verification with the county health department did not indicate any store closings. Lastly, the small sample may have been under powered to detect associations and thus findings need to be repeated in future studies.
Results from this study suggest that if healthier food options were made available at convenience stores, dietary intake of those SNAP participants living within a close proximity might choose the healthier option. Intervention strategies are needed to not only provide access but also place and promotion of healthier options within stores where SNAP participants shop and live. Policy approaches which support price supports might also be one approach to help improve the purchasing power of low-income shoppers at stores close to their homes.
References
- Cummins S (2007) Neighbourhood food environment and diet: time for improved conceptual models? Prev Med 44: 196-197.
- Cummins S, Smith DM, Taylor M, Dawson J, Marshall D, et al. (2009) Variations in fresh fruit and vegetable quality by store type, urban-rural setting and neighbourhood deprivation in Scotland. Public Health Nutr 12: 2044-2050.
- He M, Tucker P, Irwin JD, Gilliland J, Larsen K, et al. (2012) Obesogenic neighbourhoods: the impact of neighbourhood restaurants and convenience stores on adolescents' food consumption behaviours. Public Health Nutr 15: 2331-2339.
- Findholt NE, Michael YL, Jerofke LJ, Brogoitti VW (2011) Environmental influences on children's physical activity and eating habits in a rural Oregon County. Am J Health Promot 26: e74-85.
- Bodor JN, Rice JC, Farley TA, Swalm CM, Rose D (2010) The association between obesity and urban food environments. J Urban Health 87: 771-781.
- Block JP, Christakis NA, O'Malley AJ, Subramanian SV (2011) Proximity to food establishments and body mass index in the Framingham Heart Study offspring cohort over 30 years. Am J Epidemiol 174: 1108-1114.
- Hutchinson PL, Nicholas Bodor J, Swalm CM, Rice JC, Rose D (2012) Neighbourhood food environments and obesity in southeast Louisiana. Health Place 18: 854-860.
- Langellier BA (2012) The food environment and student weight status, Los Angeles County, 2008-2009. Prev Chronic Dis 9: E61.
- Hearst MO, Pasch KE, Laska MN (2012) Urban v. suburban perceptions of the neighbourhood food environment as correlates of adolescent food purchasing. Public Health Nutr 15: 299-306.
- Bodor JN, Ulmer VM, Dunaway LF, Farley TA, Rose D (2010) The rationale behind small food store interventions in low-income urban neighborhoods: insights from New Orleans. J Nutr 140: 1185-1188.
- Leung CW, Laraia BA, Kelly M, Nickleach D, Adler NE, et al. (2011) The influence of neighborhood food stores on change in young girls' body mass index. Am J Prev Med 41: 43-51.
- Leung CW, Willett WC, Ding EL (2012) Low-income Supplemental Nutrition Assistance Program participation is related to adiposity and metabolic risk factors. Am J Clin Nutr 95: 17-24.
- Kersten E, Laraia B, Kelly M, Adler N, Yen IH (2012) Small food stores and availability of nutritious foods: a comparison of database and in-store measures, Northern California, 2009. Prev Chronic Dis 9: E127.
- Harris DE, Blum JW, Bampton M, O'Brien LM, Beaudoin CM, et al. (2011) Location of food stores near schools does not predict the weight status of Maine high school students. J Nutr Educ Behav 43: 274-278.
- Commerce USDo (2010) United States Census Bureau.
- Lucan SC, Karpyn A, Sherman S (2010) Storing empty calories and chronic disease risk: snack-food products, nutritive content, and manufacturers in Philadelphia corner stores. J Urban Health: bulletin of the New York Academy of Medicine 87: 394-409.
- Agriculture USDo (2012) Supplemental Nutrition Assistance Program.
- Glanz K, Sallis JF, Saelens BE, Frank LD (2007) Nutrition Environment Measures Survey in stores (NEMS-S): development and evaluation. Am J Prev Med 32: 282-289.
- Babey S DA, Hastert T, Harvey S, Goldstein H, Flourney R, et al. (2008) S. Designed for Disease: The link between local food environments and obesity and diabetes. UCLA Center for Health Policy Research
- Kennedy ET, Ohls J, Carlson S, Fleming K (1995) The Healthy Eating Index: design and applications. J Am Diet Assoc 95: 1103-1108.
- Lucan SC, Barg FK, Long JA (2010) Promoters and barriers to fruit, vegetable, and fast-food consumption among urban, low-income African Americans--a qualitative approach. Am J Public Health 100: 631-635.
- Zenk SN, Schulz AJ, Israel BA, James SA, Bao S, et al. (2006) Fruit and vegetable access differs by community racial composition and socioeconomic position in Detroit, Michigan. Ethn Dis 16: 275-280.
- Laska MN, Hearst MO, Forsyth A, Pasch KE, Lytle L (2010) Neighbourhood food environments: are they associated with adolescent dietary intake, food purchases and weight status? Public Health Nutr 13: 1757-1763.
- Pearce J, Hiscock R, Blakely T, Witten K (2008) The contextual effects of neighbourhood access to supermarkets and convenience stores on individual fruit and vegetable consumption. J Epidemiol Community Health 62: 198-201.
- Gustafson A, Hankins S, Jilcott S (2012) Measures of the consumer food store environment: a systematic review of the evidence 2000-2011. J Community Health 37: 897-911.
- McKinnon RA, Reedy J, Morrissette MA, Lytle LA, Yaroch AL (2009) Measures of the food environment: a compilation of the literature, 1990-2007. Am J Prev Med 36: S124-133.
Relevant Topics
- Addiction
- Adolescence
- Children Care
- Communicable Diseases
- Community Occupational Medicine
- Disorders and Treatments
- Education
- Infections
- Mental Health Education
- Mortality Rate
- Nutrition Education
- Occupational Therapy Education
- Population Health
- Prevalence
- Sexual Violence
- Social & Preventive Medicine
- Women's Healthcare
Recommended Journals
Article Tools
Article Usage
- Total views: 14932
- [From(publication date):
November-2013 - Nov 22, 2025] - Breakdown by view type
- HTML page views : 10196
- PDF downloads : 4736