Research Article Open Access
Analysis of Right Atrial Function in Obese Pediatric Patients
| José Augusto A Barbosa2, Bruno Morais Damião2, Maria Carmo P3 and Márcia Barbosa1* | |
| 1Ecocenter-Socor Hospital, Avenida do Contorno, 10500. Belo Horizonte, Minas Gerais, Brazil | |
| 2Hospital Julia Kubitscheck- FHEMIG, AV. Cristiano Resende 2745. Belo Horizonte, Mina Gerais, Brazil | |
| 3Department of Pediatrics/ Echocardiography from the Federal University of Minas Gerais, Avenida Alfredo Balena, 460, Belo Horizonte, Minas Gerais, Brazil | |
| Corresponding Author : | Marcia M Barbosa Conde do Rio Pardo 288 – Vila do Conde 3400000 Nova Lima, MG - Brazil Tel: +553192781727 Fax: +55 3135812606 E-mail: marciambarbosa@terra.com.br |
| Received October 30, 2013; Accepted January 03, 2014; Published January 06, 2014 | |
| Citation:Barbosa M , Barbosa JAA , Damião BM, Maria Carmo P, (2014) Analysis of Right Atrial Function in Obese Pediatric Patients. J Obes Weight Loss Ther 4:204. doi:10.4172/2165-7904.1000204 | |
| Copyright: © 2014 Barbosa M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Background : Left atrial enlargement and right and left ventricular dysfunction have been described in obese Patients. A number of studies have also described atrial dysfunction in obese children and adolescents. Objective: The aim of the present study was to investigate right atrial dysfunction in obese pediatric patients and Compare echocardiography findings between these patients and non-obese controls. Methods : Doppler echocardiography was performed on 50 obese pediatric patients (mean BMI=29.8 kg/m2) and 46 lean healthy controls. Systolic and diastolic function in both ventricles was investigated through conventional Doppler echocardiography. Right atrial function was evaluated using Color Doppler Myocardial Imaging (CDMI). Results: No differences were detected between groups with regard to left ventricular ejection fraction. The S wave of the free Wall of the right ventricle was similar in both groups (13.8 ± 1.7 vs. 13.7 ± 1.6, p=0.655). The e’/A’ ratio in the right Ventricle was significantly lower in the obese patients (0.9 ± 0.4 vs.1.2 ± 0.3, p=0.007). CDMI analysis of the right atrium and inter-atrial septum showed significantly lower, strain and strain rate in obese patients (82.6 ± 29.8 vs. 98.6 ± 38.7, p=0.020; 3.9 ± 1.0 vs. 4.4 ± 1.2, p<0.001; 50.9 ± 25.0 vs. 81.1 ± 21.6, p<0.001; and 2.2 ± 1.0 vs. 3.3 ± 0.8, p<0.001, respectively). Conclusion: The findings of the present study suggest incipient right atrial dysfunction, which may be secondary to an incipient impairment of myocardial relaxation in the right ventricle in obese children (BMI above 95th percentile).
| Keywords |
| Atrial function; Obesity; Pediatrics |
| Introduction |
| Obesity has become an epidemic in both developed and developing countries. Statistics from the United States of America reveal a 32.2% rate of obesity among adult men and 25.5% among adult women [1]. It is estimated that Five to 10 million adult individuals in the United States alone have severe obesity (body mass index ≥ 40 kg/m2) [2]. In developing countries, the prevalence of obesity has reached more than 20% of the population. Reports on the pediatric population (children and adolescents aged two to 19 years) reveal that 11.9% are at or above the 97th percentile of the body mass index (BMI) for age, 16.9% are at or above the 95th percentile and 31.7% are at or above the 85th percentile [3]. Ten percent of children starting school in the United Kingdom are already obese [4]. Cardiovascular complications associated with obesity contribute to high rates of morbidity and mortality. Structural and functional alterations in the heart, such as left ventricular hypertrophy, diastolic/systolic dysfunction and atrial enlargement, are well established in adult and pediatric patients with obesity [5-10]. Left atrial dysfunction with left ventricular diastolic dysfunction in subjects with preserved systolic function is well established in patients with hypertension [11,12]. There is strong evidence that left atrial enlargement and dysfunction are associated with an increase in morbidity and mortality rates in patients with cardiovascular disease and present clinical relevance with respect to the rate of long-term events, survival and the risk of developing atrial fibrillation [13]. Using Doppler-derived strain and strain rate (SR) in the evaluation of hypertensive patients, Guan et al. found that left atrial myocardial dysfunction and the E/e’ ratio in the left ventricle correlated negatively with left atrial SR [11]. However, conflicting results are reported for obese patients. Di Salvo et al. studied nonhypertensive children using strain and SR and found reduced left and right atrial function in the obese group [14]. On the other hand, Gulel et al. compared left atrial function using tissue Doppler imaging in adults with BMI ≥ 30 Kg/ m2 versus those with a BMI < 30 Kg/m2 and found no difference in atrial function between groups [15]. The aim of the present study was to compare right atrial function in obese pediatric patients (BMI > 95th percentile) with no comorbidities and lean controls (BMI < 85th percentile) using strain and SR data derived from color Doppler myocardial imaging. |
| Methods |
| Obese pediatric patients six to 18 years of age with a BMI above the 95th percentile were prospectively recruited from the nutrition clinic of a university hospital (Universidade Federal de Minas Gerais) in Belo Horizonte, Brazil. The control group was formed by children aged six to 18 years with a BMI below the 85th percentile recruited from the general pediatrics clinic of the same institution. Patients with a history of hypertension, diabetes mellitus, endocrinological disorders, hereditary or inflammatory systemic diseases, sleep apnea (according to parents’ information) and athletes were excluded in both groups. This study received approval from the Human Research Ethics Committee of the institution and written informed consent was obtained from all participants and/or parents. The participants were weighed in light clothing without shoes using a Welmy® scale with a capacity of 300 Kg and accuracy of 100 g. Height was measured with a stadiometer (accuracy of 0.5 cm). BMI was calculated using the conventional formula of weight in kilograms divided by the square of height in meters. Obesity was defined when BMI exceeded the 95th percentile for gender and age based on reference values [16]. Blood pressure was determined using standard methods with an appropriate cuff size on more than three different occasions. Only patients with systolic and diastolic blood pressure values below the 90th percentile for gender and height were included in the study [17]. |
| A comprehensive Doppler echocardiogram with color flow mapping and tissue Doppler imaging were carried out for all patients using commercially available hardware and software (Vivid 7; GE Vingmed Ultrasound AS, Horten, Norway) and an electronic high-resolution multi-frequency transducer. A single experienced certified cardiologist performed all measurements. The mean values of three consecutive cardiac cycles were obtained for all echocardiographic parameters. Left ventricle (LV), end-systolic left ventricular diameter, end-diastolic left ventricular diameter, left ventricle free wall and septum thickness were determined based on the recommendations of the American Society of Echocardiography [18]. LV ejection fraction (EF) was calculated using the Teichhollz method [12]. Left atrial volume was evaluated using the biplane area-length method from apical 4-chamber and 2 chamber views and indexed to body surface area [19]. For patients in whom an adequate tricuspid regurgitation (TR) spectral Doppler profile could be obtained, peak TR velocity was measured to calculate the right ventricle-right atrium gradient using the modified Bernoulli equation [(TR jet velocity)2 × 4] [20]. |
| Right ventricular (RV) systolic and diastolic function was assessed using pulsed-wave tissue Doppler imaging (PW-TDI) at the tricuspid annulus. The velocity of the S, A’ and e’ waves was determined. The e’/A’ ratio of the right ventricle (RV) was also calculated [21]. All measurements were the mean of three consecutive heartbeats. Color Doppler-derived strain and SR were obtained by placing a 10-mm sample volume in the medial part of free wall of the right atrium and inter-atrial septum from the apical 4-chamber view [22]. The image sector was narrowed to allow the highest frame rate (>150 frames/sec) and the imaging angle to the wall was kept as low as possible to allow better parallel alignment to the wall of interest. Peak systolic strain and SR were measured (Figure 1). |
| Statistical Analysis |
| The primary outcome was the comparison of strain and SR images of the right atrium and inter-atrial septum in the two groups. The sample size was calculated using the indexed LV mass from a previous study [23]. A sample of 45 patients in each group was calculated to provide a 90% power to detect a clinical effect (increase equal or greater than 30%) in LV mass, with a significance level (alpha) of 0.05 (two-tailed) [24]. The secondary outcomes were clinical data, Doppler echocardiographic parameters and PW-TDI values for the assessment of right ventricular systolic and diastolic function. |
| The normality of the data was tested to choose parametric vs. nonparametric tests. To characterize the sample, frequency distributions were used for qualitative variables and descriptive measures (mean, median, standard deviation) were used for quantitative variables. The Student’s t-test was employed for comparisons between groups when variables followed normal distribution and the Mann-Whitney test was employed for data with non-Gaussian distribution. A significance level of 5% was considered on all statistical tests [24]. Intra-observer variability regarding strain and SR values was calculated in a sample of 20 randomly selected obese patients. Analyses were performed using the Statistical Package for Social Sciences version 18.0 (SPSS Inc., Chicago, IL, USA). |
| Results |
| Ninety-six patients were recruited - 50 in the obese group (OG) and 46 lean individuals in the control group (CG). Table 1 displays the clinical, demographic and standard echocardiography data in both groups. Age was similar in both groups. In the OG, 50% of the patients were male and in the CG, 48%. Heart rate was higher in the OG, but remained in the normal range. All patients were situated below the 90th percentile for systolic and diastolic blood pressure. However, mean systolic pressure and diastolic pressure were higher in the OG. |
| Standard echocardiography and PW-TDI |
| M mode LV diameter and LV mass corrected for height2.7 were higher in the OG. The left atrium diameter was also significantly larger in the obese patients in comparison to the lean controls. No statistically significant difference in EF was detected between groups. The RV e’/A’ ratio was significantly lower in the OG (Table 2). Although within the normal range, the RV-right atrial gradient (measured by TR jet velocity) was slightly higher in the OG. |
| Strain and SR derived from color Doppler myocardial imaging |
| Systolic strain and SR of the basal segment of the free wall of the right atrium and the interatrial septum were significantly lower in the obese patients. |
| Reproducibility |
| Intraclass correlation coefficients for intra-observer variability regarding strain and SR for the RA and inter-atrial septum were 0.94c, 0.93c, 0.90c and 0.97c respectively. |
| Discussion |
| Standard echocardiography of obese pediatric patients with no comorbidities revealed a larger left atrial diameter, increased LV mass and the absence of systolic left ventricular dysfunction (Table 1), which is in agreement with previous studies [10,23], Data reported by Di Salvo et al. show left and right atrial dysfunction in obese pediatric patients. Moreover, the present study demonstrates a reduction in right atrial strain and SR in obese children and adolescents in comparison to lean controls [14]. |
| Tissue Doppler image revealed no difference between groups regarding systolic right ventricular function (Table 2). In a previous study analyzing right ventricular function, our research group found an increase in strain and SR in obese pediatric patients and speculated that the hyperdynamic state found in obesity due to an increase in preload may influence RV strain and SR [10]. It is possible that decreased RV strain and SR is only detected later on in the obesity process, when the incipient RV systolic dysfunction overcomes the increase in preload and after load [6]. In the present study, the RV e’/A’ ratio was significantly lower in the obese group (Table 2), which suggests an incipient impairment of myocardial relaxation of the right ventricle in these children and adolescents that may explain the decreased strain and SR in the RA in this type of patient. |
| Limitations of the Study |
| The obese children in the present study did not undergo polysomnography, which is the gold standard for the detection of sleep apnea and cause of pulmonary hypertension. However, since these children exhibited no clinical evidence of sleep apnea, it was not considered appropriate to submit them to this exam. |
| Conclusion |
| The present study demonstrates that obesity in children, even in the absence of comorbidities, is associated with right atrial deformation and incipient RV diastolic dysfunction. These findings underscore the importance of the early prevention of obesity in the pediatric population. |
References
- Flegal KM, Carroll MD, Ogden CL, Curtin LR (2010) Prevalence and trends in obesity among US adults, 1999-2008. JAMA 303: 235-241.
- James WP (2008) The epidemiology of obesity: the size of the problem. J Intern Med 263: 336-352.
- Ogden CL, Carroll MD, Curtin LR, Lamb MM, Flegal KM (2010) Prevalence of high body mass index in US children and adolescents, 2007-2008. JAMA 303: 242-249.
- Rudolf M (2011) Predicting babies' risk of obesity. Arch Dis Child 96: 995-997.
- Tumuklu MM, Etikan I, Kisacik B, Kayikcioglu M (2007) Effect of obesity on left ventricular structure and myocardial systolic function: assessment by tissue Doppler imaging and strain/strain rate imaging. Echocardiography 24: 802-809.
- Abel ED, Litwin SE, Sweeney G (2008) Cardiac remodeling in obesity. Physiol Rev 88: 389-419.
- Dhuper S, Abdullah RA, Weichbrod L, Mahdi E, Cohen HW (2011) Association of obesity and hypertension with left ventricular geometry and function in children and adolescents. Obesity (Silver Spring) 19: 128-133.
- Russo C, Jin Z, Homma S, Rundek T, Elkind MS, et al. (2011) Effect of obesity and overweight on left ventricular diastolic function: a community-based study in an elderly cohort. J Am Coll Cardiol 57: 1368-1374.
- Barbosa MM, Beleigoli AM, de Fatima Diniz M, Freire CV, Ribeiro AL, et al. (2011) Strain imaging in morbid obesity: insights into subclinical ventricular dysfunction. Clin Cardiol 34: 288-293.
- Barbosa JA, Mota CC, Simões E Silva AC, Nunes Mdo C, Barbosa MM (2013) Assessing pre-clinical ventricular dysfunction in obese children and adolescents: the value of speckle tracking imaging. Eur Heart J Cardiovasc Imaging 14: 882-889.
- Guan Z, Zhang D, Huang R, Zhang F, Wang Q, et al. (2010) Association of left atrial myocardial function with left ventricular diastolic dysfunction in subjects with preserved systolic function: a strain rate imaging study. Clin Cardiol 33: 643-649.
- Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, et al. (2005) Recommendations for chamber quantification: a report from the American Society of Echocardiography's Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr 18:1440-1463.
- Kizer JR, Bella JN, Palmieri V, Liu JE, Best LG, et al. (2006) Left atrial diameter as an independent predictor of first clinical cardiovascular events in middle-aged and elderly adults: the Strong Heart Study (SHS). Am Heart J 151: 412-418.
- Di Salvo G, Pacileo G, Del Giudice EM, Natale F, Limongelli G, et al. (2008) Atrial myocardial deformation properties in obese nonhypertensive children. J Am Soc Echocardiogr 21: 151-156.
- Gulel O, Yuksel S, Soylu K, Kaplan O, Yilmaz O, et al. (2009) Evaluation of left atrial functions by color tissue Doppler imaging in adults with body mass indexes >or=30 kg/m(2) versus those <30 kg/m (2). Int J Cardiovasc Imaging 25: 371-377.
- Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320: 1240-1243.
- National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents (2004) The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114: 555-576.
- Schiller NB, Shah PM, Crawford M, DeMaria A, Devereux R, et al. (1989) Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. American Society of Echocardiography Committee on Standards, Subcommittee on Quantitation of Two-Dimensional Echocardiograms. J Am Soc Echocardiogr 2: 358-367.
- Lester SJ, Ryan EW, Schiller NB, Foster E (1999) Best method in clinical practice and in research studies to determine left atrial size. Am J Cardiol 84: 829-832.
- McQuillan BM, Picard MH, Leavitt M, Weyman AE (2001) Clinical correlates and reference intervals for pulmonary artery systolic pressure among echocardiographically normal subjects. Circulation 104: 2797-2802.
- Haddad F, Doyle R, Murphy DJ, Hunt SA (2008) Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation 117: 1717-1731.
- Marwick TH (2006) Measurement of strain and strain rate by echocardiography: ready for prime time? J Am Coll Cardiol 47: 1313-1327.
- Di Salvo G, Pacileo G, Del Giudice EM, Natale F, Limongelli G, et al. (2006) Abnormal myocardial deformation properties in obese, non-hypertensive children: an ambulatory blood pressure monitoring, standard echocardiographic, and strain rate imaging study. Eur Heart J 27: 2689-2695.
- Portney LG, Watkins MP (2009) Review of: Foundations of Clinical Research Applications to Practice (3rd edn) Pearson/Prentice Hall 8: 4.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
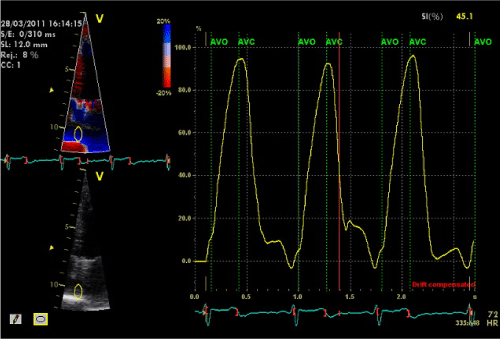 |
| Figure 1 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 13354
- [From(publication date):
February-2014 - Aug 19, 2025] - Breakdown by view type
- HTML page views : 8817
- PDF downloads : 4537
