Research Article Open Access
Better Results in Weight Loss after the Second Gastrectomy in Re-Sleeve Gastrectomy
| Jean-Marc Catheline1*, Marinos Fysekidis2, Hélène Bihan2, Arianna Boschetto1, Rami Dbouk1 and Régis Cohen2 | |
| 1Department of Digestive Surgery, Centre Hospitalier de Saint-Denis, F-93205 Saint-Denis, France | |
| 2Department of Endocrinology, Hôpital Avicenne «Assistance Publique – Hôpitaux de Paris », F-93000 Bobigny, France | |
| Corresponding Author : | Jean-Marc Catheline Department of Digestive Surgery Centre Hospitalier de Saint-Denis 2, rue du Docteur Delafontaine F-93205 Saint-Denis Cedex, France Tel: 33 1 42 35 60 46 Fax: 33 1 42 35 62 32 E-mail: jmcatheline@orange.fr |
| Received December 06, 2011; Accepted December 12, 2011; Published December 23, 2011 | |
| Citation: Catheline JM, Fysekidis M, Bihan H, Boschetto A, Dbouk R, et al. (2011) Better Results in Weight Loss after the Second Gastrectomy in Re-Sleeve Gastrectomy. J Obes Weig los Ther 1:107. doi:10.4172/2165-7904.1000107 | |
| Copyright: © 2011 Catheline JM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Background: Sleeve gastrectomy (SG) has been rapidly accepted as a valuable bariatric procedure before its effectiveness on weight loss in the long-term is clearly demonstrated. Re-sleeve gastrectomy (RSG) has been shown to provide promising results for patients with insufficient weight loss after SG.
Methods: Seven patients underwent a re-sleeve gastrectomy procedure for insufficient weight loss after a mean 30±10 month follow-up associated with a dilated gastric pouch seen in upper gastro-intestinal contrast study.
Results:Before SG, mean initial weight was 151 41 kg, mean Body Mass Index (BMI) was 55.4±12.5 kg/m2, 4 had a BMI more than 60 kg/m2 and 3 had a gastric banding before their SG. At follow-up of 12 months after SG, mean weight was 131 ±31 Kg, mean BMI was 48±9 kg/m2, mean %Excess Weight Loss (EWL) was 30 5%, and mean %Excess BMI Loss (EBL) 23 ±3%. At a follow-up of 12 months after RSG, final mean weight was 92 ±10 Kg, final mean BMI was 34±4 kg/m2, and mean %EBL since the second operation (RSG) was 58±17% (mean %EBL since the first operation (SG) was 6618%), and mean %EWL since the second operation (RSG) was 4217%(mean %EWL since the first operation (SG) was 6618%). The RSG resulted in significant mean %EBL (p<0,001) and in significant mean %EWL (p=0,029), compared to the initial SG results.
Conclusion:In patients with insufficient weight loss after SG, RSG resulted in successful extra weight loss.
| Keywords |
| Sleeve gastrectomy; Re-sleeve gastrectomy; Revisional surgery; Obesity; Laparoscopy |
| Introduction |
| Sleeve gastrectomy (SG) presents many advantages in comparison with other procedures used in the surgical treatment of morbid obesity [1,2]. This procedure has been documented to be more effective than gastric banding [2] and has been associated with fewer complications than Roux-en-Y gastric bypass especially in super superobesity [1,3]. However the presence of limited weight loss, especially in super superobese patients, second-stage operations such as gastric bypass or duodenal switch have been suggested [1,3-5]. Additionally due to concerns about the secondary dilation of the gastric pouch associated to weight regain, the re-sleeve gastrectomy (RSG) has been recently proposed [6]. Baltasar reported the first RSG in 2006 for two patients (BMI of 58 and 65 kg/m2) [1]. Iannelli et al. [6] reported the results of 13 obese patients, with mean body mass index (BMI) of 44.58 kg/m2, operated for a second SG after insufficient weight loss following the first SG. Results were impressive with a final BMI of 27.5 kg/m2, 71.4% excess weight loss (%EWL), and 82.8% excess BMI loss (%EBL) at 12 months follow-up, with no associated morbidity [6]. |
| In the present study we confirmed the safeness of this procedure and we underlined the higher effectiveness of the second surgery. |
| Patients and Methods |
| Patients were considered for SG revision when weight loss was estimated as insufficient 18 months since their first operation by using the following criteria: loss of less than 50% of excess weight, progressive weight regain, persistence of comorbidities supposed to improve with further weight loss, and if there were a dilated gastric pouch seen in upper gastro-intestinal contrast studies. Dilated gastric pouch was defined by the persistence of a large part of the gastric fundus and/or the body and/or the upper part of the antrum. All patients gave their written informed consent prior to surgery, and had at least a 12 month follow up after their RSG. Comorbidities were assessed in each patient. |
| Surgical technique |
| All RSG's were completed laparoscopically. At first, any liver adhesions to the anterior surface of the stomach were removed. Then, we released the left border of the gastric tube and the posterior side of the gastric tube until the visualization of the left crura of the diaphragm and we have performed the RSG after the introduction of a 34 French boogie. The section of the gastric tube was started at 4 cm from the pylorus in case of dilation of the antrum. In the case of isolated dilatation of the fundus, only the expanded portion was resected. In all cases the section of the gastric tube was performed parallel to a 34 French boogie using laparoscopic linear staplers (EndoGIA®-Covidien®, Mansfield, MA, USA) and using staple line reinforcement with running sutures. A drain was routinely left in place. A liquid diet was started gradually until the third day and then semi liquid for a three-week period. An upper gastrointestinal contrast study was performed at the third day after surgery to diagnose any leak. |
| Data |
| Data were entered into a prospectively held data base that included age, gender, BMI, %EWL, %EBL, before SG, at the time of RSG, and at follow-up visits (1,3,6,and 12 months and every 6 months thereafter). All RSG patients were operated after a follow up from SG in order to have a minimum of 18 month evaluation for insufficient weight loss since the first operation. BMI, %EWL, and %BML were calculated for a 12 month period [7] following the first SG and for the same time interval after RSG. Also, we have evaluated duration of surgery and hospital stay, postoperative complications, and comorbidities evolution. |
| Results |
| We report, here, a study of 7 patients (5 females, 2 males) with a mean age of 46 (19-60) years old who underwent SG plus RSG. Before SG, mean initial weight was 151 ± 41 kg, mean BMI was 55.4 ± 12.5 kg/ m2, 4 had a BMI more than 60 kg/m2 and 3 had a gastric banding before their SG. Patients presented the following comorbidities: hypertension in two patients, sleep apnea syndrome in two patients, knee joint disease in two patients and dyslipidemia in one patient. |
| At follow-up of 12 months after SG, mean weight was 131 ± 31 Kg, mean BMI was 48 ± 9 kg/m2, mean %EWL (since the first operation) was 30 ± 5%, and mean %EBL 23 ± 3%. The comorbidities that remained were: hypertension in one patient, sleep apnea syndrome in one patient, knee joint disease in two patients, dyslipidemia in one patient. |
| All RSG patients were operated after a mean 30 ± 10 month (range 20 to 49) follow up from SG. RSG was completed laparoscopically in all cases. No operative or postoperative complications were recorded. The mean operative time was 83 (43-153) minutes. The mean hospital stay was 6 (4-9) days. |
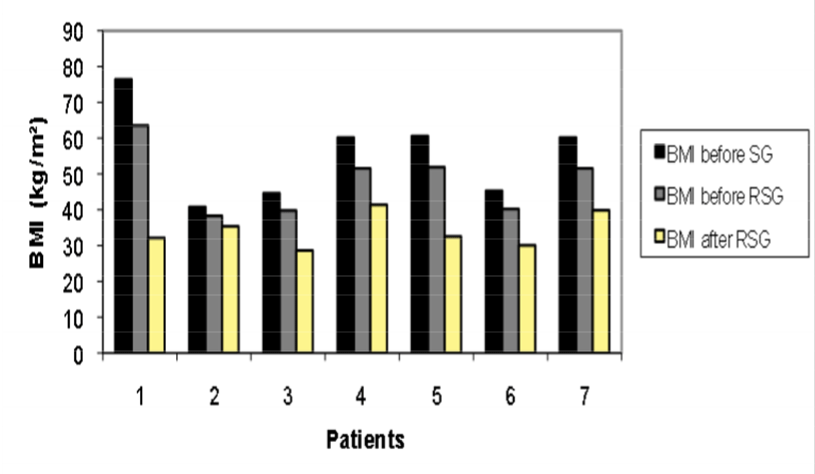
| At a follow-up of 12 months after RSG, final mean weight was 92 ± 10 Kg, final mean BMI (Figure 1) was 34 ± 4 kg/m2, and mean %EBL since the second operation (RSG) was 58±17% (mean %EBL since the first operation (SG) was 6618%), and mean %EWL since the second operation (RSG) was 4217% (mean %EWL since the first operation (SG) was 6618%). Knee joint disease remained in two patients. The RSG resulted in significant mean %EBL (p<0,001) and in significant mean %EWL (p=0,029), compared to the initial SG results (Figure 2). |
| Discussion |
| In this study we demonstrated that RSG was safe, effective with no technical difficulties. We have observed better results in weight loss after the second gastrectomy. |
| RSG was performed after upper gastro-intestinal contrast studies, in order to select patients that have developed a secondary dilated gastric pouch. SG failure can result from other causes like disorders of eating behaviour or high energy intake with liquids and even though existing literature is rather poor. The presence of dilated gastric pouch is an essential criterion in order to ensure additional RSG good results. This is also an element that could explain insufficient weight loss. SG is known to produce weight loss by at least two distinct mechanisms including reduction of ghrelin levels and gastric volume restriction [8]. The proximal fundus is known to be the main secretory site for ghrelin [9,10]. The results of a preliminary study did not show significant mean ghrelin level variation after RSG compared with the SG [11]. The restriction mechanism seems to be a more likely explanation for good results of RSG [6]. |
| Although this is a relatively small study, the benefit/risk ratio of this procedure in our opinion and personal experience is encouraging for the treatment of super obese patients. In a preliminary study with RSG procedure [11], we have noted that obesity was reduced to a BMI of less than 30kg/m2 in one super-superobese patient after a 24 month post RSG follow up. One of the major criticisms of SG is the insufficient weight loss in comparison to gastric bypass [12]. Concerning the morbidity and mortality rates for superobese patients, SG probably provides an advantage in comparison with other procedures like gastric bypass or biliopancreatic diversion frequently associated with higher mortality and morbidity rates [13] as well with a lifetime vitamin supplementation. However, it should be noted that we do not currently have very long-term follow up study. |
| In conclusion, we have observed better results in weight loss after the second gastrectomy. RSG after SG should be considered for treatment of obesity if a secondary dilated gastric pouch has been developed following SG. Long term studies with a greater number of patients are necessary in order to confirm our results. |
| Acknowledgements |
| Mrs Vasiliki Fissekidou for the correction of this article. |
References
- Baltasar A, Serra C, Pérez N, Bou R, Bengochea M (2006) Re-sleeve gastrectomy. Obes Surg 16: 1535-1538.
- Himpens J, Dapri G, Cadière GB (2006) A prospective randomized study between laparoscopic gastric banding and laparoscopic isolated sleeve gastrectomy: results after 1 and 3 years. Obes Surg 16: 1450-1456.
- Regan JP, Inabnet WB, Gagner M, Pomp A (2003) Early experience with twostage laparoscopic Roux-en-Y gastric bypass as an alternative in the superobese patients. Obes Surg 13: 861-864.
- Milone M, Strong V, Gagner M (2005) Laparoscopic sleeve gastrectomy is superior to endoscopic intragastric ballon as a first stage procédure for the super-obese patients (BMI> or = 50). Obes Surg 15: 612-617.
- Almogy G, Crookes PF, Anthone GJ (2004) Longitudinal gastrectomy as a treatment for the high-risk super-obese patient. Obes Surg 14: 492-497.
- Iannelli A, Schneck AS, Noel P, Ben Amor I, Krawczykowski D, et al. (2011) Re-sleeve gastrectomy for failed laparoscopic sleeve gastrectomy: A feasibility study. Obes Surg 21: 832-835.
- Deitel M, Greenstein RJ (2003) Recommendations for reporting weight loss. Obes Surg 13: 159-160.
- Delgado-Aros S, Cremonini F, Castillo JE, Chial HJ, Burton DD, et al. (2004) Independent influences of body mass and gastric volumes on satiation in humans. Gastroenterology 126: 432-440.
- Langer FB, Reza Hoda MA, Bohdjalian A, Felberbauer FX, Zacherl, J et al. (2005) Sleeve gastrectomy and gastric banding: effects on plasma ghrelin levels. Obes Surg 15: 1024-1029.
- Uzzan B, Bihan H, Catheline JM, Cohen R, Reach G, et al. (2005) Ghrelin levels and sleeve gastrectomy in super-super-obesity. Obes Surg 15: 1501-1502.
- Catheline JM, Dbouk R, Helmy N, Ruzeykin I, Cohen R, et al. (2011) Re-sleeve gastrectomie. Obésite 6: 123-125.
- Himpens J, Dobbeleir J, Peeters G (2010) Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg 252: 319-324.
- Fazylov RM, Savel RH, Horovitz JH, Pagala MK, Coppa GF, et al. (2005) Association of super-super-obesity and male gender with elevated mortality in patients undergoing the duodenal switch procedure. Obes Surg 15: 618-623.
Figures at a glance
 |
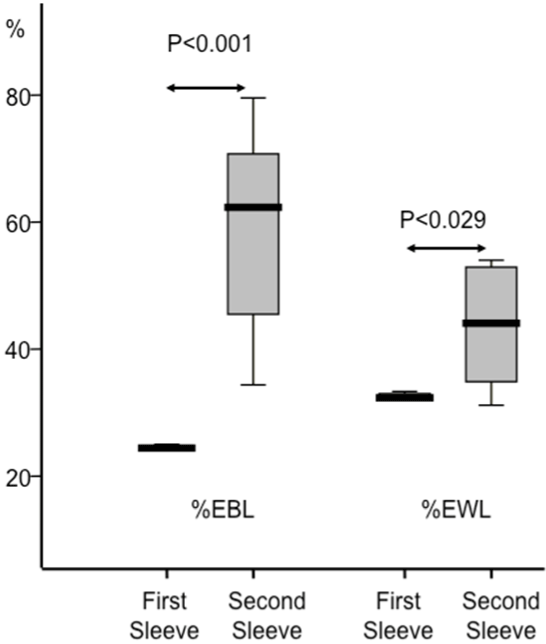 |
| Figure 1 | Figure 2 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 17089
- [From(publication date):
December-2011 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 12504
- PDF downloads : 4585
