Research Article Open Access
Exploring the Role of Perceived Stress in a Patient's Experience of Fibromyalgia
| Toussaint LT1, McAllister JS2, Whipple OM2, Aleman K2, Hassett LA4, Oh HT3 and Vincent A2* | |
| 1Department of Psychology, Luther College, 700 College Drive, Decorah, Iowa, USA | |
| 2Department of Medicine Mayo Clinic, Rochester, Minnesota, USA | |
| 3Department of Physical Medicine and Rehabilitation, Mayo Clinic, 200 First Street SW, Rochester, Minnesota, USA | |
| 4Department of Anesthesiology , University of Michigan, 1500 E Medical Center Drive, Ann Arbor, Michigan, USA | |
| Corresponding Author : | Ann Vincent Department of Medicine, Mayo Clinic, 200 First Street SW Rochester, MN 55905, USA Tel: 507-284-8913 E-mail: ann.vincent@mayo.edu |
| Received May 13, 2014; Accepted September 08, 2014; Published September 10, 2014 | |
| Citation: Toussaint LT, McAllister JS, Whipple OM, Aleman K, Hassett LA, et al. (2014) Exploring the Role of Perceived Stress in a Patient’s Experience of Fibromyalgia. J Pain Relief 3: 155. doi: 10.4172/2167-0846.1000155 | |
| Copyright: © 2014 Toussaint TL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
The purpose of this exploratory study was to examine cross-sectional relationships between perceived stress and fibromyalgia impact. Also, we sought to examine the mediating effects of key fibromyalgia symptoms including pain, fatigue, unrefreshing sleep, dyscognition, depressed mood and autonomic symptoms on this relationship. Data from 705 patients meeting Fibromyalgia Research Survey Criteria who completed a battery of self-report measures was used. Bivariate correlations revealed that stress was associated with fibromyalgia impact (r=0.49). Stress was also associated with all symptoms assessed (rs=0.29-0.77) and fibromyalgia impact was also associated with these symptoms (rs=0.33-0.59). Mediation modeling revealed that the total effect of stress on fibromyalgia impact was statistically significant (B=0.35,p<0.001), however, the direct effect was not significant when controlling for all mediators (B=0.03,p<0.05) and the total indirect effect of all mediators (B=0.32,p<0.05) was statistically significant and fully explained the association between stress and fibromyalgia impact. Specifically, pain, fatigue, negative mood, and autonomic dysregulation had significant indirect effects on this relationship. Our results demonstrate that perceived stress is associated with the patient’s experience of exacerbated individual fibromyalgia symptoms. Also, the patient reported symptoms serve to explain the relationship between perceived stress and a patient’s report of overall impact of fibromyalgia on day-to-day living.
The significance of the association of stress with psychological and physical symptoms in patients with fibromyalgia has been exemplified in three recent studies [9-11]. In the two studies by Malin and Littlejohn, perceived stress was reported to be associated with key fibromyalgia symptoms including pain, sleep, fatigue, dyscognition, depression, and anxiety; also, they identified psychological control methods (neuroticism, mastery, and degree of internal control) as a mechanism for the gradient effect of stress on fibromyalgia severity [10,11]. Similarly, in a study by Gonzalez-Ramirez et al., the association of stress and fibromyalgia symptoms was partly explained by an individual’s self-efficacy [9]. Although these three studies provide evidence for the relationship between stress and fibromyalgia symptoms and identify some potential mechanisms between the two, there remains little explanation about how perceived stress impacts a patient’s experience of fibromyalgia and how it interferes with their ability to accomplish day to day goals.
We sought to provide insight into this relationship by utilizing the overall impact subscale of the Fibromyalgia Impact Questionnaire (FIQ-R), the most widely utilized measure of fibromyalgia [12,13]. The impact subscale provides a quantitative measure of how overwhelmed a patient feels as a result of fibromyalgia and how the patient perceives fibromyalgia has interfered with their ability to accomplish day to day goals. Our objective in this exploratory study was to examine cross-sectional associations between perceived stress and fibromyalgia impact and examine the mediating effects of pain, fatigue, unrefreshing sleep, dyscognition, depressed mood and autonomic symptoms on this relationship. We hypothesized that perceived stress and fibromyalgia impact would be significantly related and this association would be mediated by these key fibromyalgia symptoms.
The PSS is a validated 10-item self-report questionnaire which asks individuals to indicate how often they have found their lives unpredictable, uncontrollable, and overloaded in the last month [15]. The PSS is a brief and easily administered measure of the degree to which situations in one's life are appraised as stressful and is an excellent tool to examine issues about the role of appraised stress levels in the etiology of disease and behavioral disorders. Total scores range from 0-40, with higher scores indicating greater perceived stress. It has been reported to have an internal consistency (Cronbach’s Alpha) of 0.78 and has demonstrated construct validity [16]. For this analysis, we utilized the total score of the PSS to represent perceived stress.
The Revised Fibromyalgia Impact Questionnaire (FIQ-R)
The FIQ-R is a 21-item validated self-report questionnaire that assesses three domains in fibromyalgia, namely: function, overall impact and symptoms [12]. Scores on the FIQ-R total range from 0-100, and on the subscale range from 0-20, with higher scores indicating greater symptom severity/impact. Internal consistency, as reported by Bennett et al. was 0.95, with item-total correlations ranging from 0.56 to 0.93 [13]. For this analysis we utilized the FIQ-R overall impact subscale to quantify fibromyalgia impact i.e. a patient’s experience of how overwhelmed they were by fibromyalgia and how having fibromyalgia has influenced their ability to accomplish goals.
Brief Pain Inventory (BPI)
The BPI is a 14-item validated self-report questionnaire that has two subscales which assess pain severity (the intensity of pain) and pain interference (the degree to which pain interferes with function) [17]. Scores on the subscales range from 0-10, with higher scores indicating greater pain severity and pain interference. Internal consistencies for the Pain Severity Subscale and the Pain Interference subscale have been reported as being 0.85 and 0.88 [18-21]. For this analysis, we utilized the Pain Severity subscale to represent pain.
Multidimensional Fatigue Inventory (MFI-20)
The MFI-20 is a 20-item validated self-report instrument that assesses multiple dimensions of fatigue, namely: general fatigue, physical fatigue, mental fatigue, reduced motivation and reduced activity [22]. MFI-total scores range from 0-100, with higher scores indicating worse fatigue. Internal consistency for the total score has been reported to be 0.93 [23,24]. For this analysis, we utilized the total score of the MFI-20 to represent the symptom of fatigue.
Profile of Mood States (POMS)
The POMS is a 30-item validated self-report measure of mood [25]. It yields 6 factors: 1) tension-anxiety, 2) depression-dejection, 3) anger-hostility, 4) fatigue-inertia, 5) confusion-bewilderment, and 6) vigor-activity. Scores range from 0-120 with higher scores indicating worse mood. A total mood score is computed by summing the first 5 factors and subtracting the vigor-activity factor. It has been reported to have an internal consistency of 76-.95 [26]. For this analysis, the total POMS score was used to represent mood.
Medical Outcomes Sleep Scale (MOS-Sleep)
The MOS- Sleep scale is a 12-item, validated, self-report measure that assesses 6 dimensions of sleep: 1) sleep disturbance, 2) sleep adequacy, 3) sleep quantity, 4) somnolence, 5) snoring, and 6) awakening with shortness of breath or headache [27,28]. It yields two summary indices: the Sleep Problems Index I (6 items) and Sleep Problems Index II (9 items). Scores on dimensions and summary indices range from 0-100, with higher scores indicating poorer sleep. The MOS-sleep scale has an internal consistency of 0.7 in patients with FM [29]. For this analysis, we utilized the sleep problems index II subscale to represent sleep disturbance.
Multiple Ability Self Report Questionnaire (MASQ)
The MASQ is a 38-item validated self-report measure of cognition and has five cognitive domains: language, visual perception, verbal memory, visual spatial memory, and attention concentration [30]. Scores on the cognitive domains range from 0-30 or 0-40; and the maximum total score is 190. Higher scores indicate greater perceived difficulties with cognition. It has been reported to have an internal consistency of 0.92 for the total score and greater than 0.70 for each individual scale [31]. For this analysis, we utilized the total score of the MASQ to represent the symptom of cognitive difficulties referred to as dyscognition in the fibromyalgia literature.
Composite Autonomic Symptom Score (COMPASS 31)
COMPASS 31 is a 31-item validated self-report measure that assesses autonomic symptom severity across multiple autonomic domains [32]. The autonomic domains are: 1) orthostatic intolerance, 2) vasomotor, 3) secretomotor, 4) gastrointestinal, 5) bladder, and 6) pupillomotor. For each of the seven domains the internal consistency was reported to range between 0.71 and 0.93; it has been reported to be a valid and reliable measure of autonomic symptom severity [32]. For this analysis, we utilized the total score of COMPASS 31 to represent autonomic symptoms.
Analyses
Analyses involved Pearson correlation and the PROCESS macro developed by Andrew Hayes for examining mediation models in SPSS 19 [33]. The PROCESS macro allows for examination of several effects: 1) total (reported in parentheses on all figures), 2) direct (reported on all paths in figures), and 3) indirect (reported in text). Statistical significance testing and confidence intervals are provided through bootstrapped standard errors which offer a powerful and robust estimation method that is less influenced by violations of standard assumptions. Unless otherwise stated, data were acceptable for significance testing procedures, and the statistical significance cutoff was set at p<0.05.
Pearson correlation analysis for the study variables showed expected associations and all associations were statistically significant at p<0.001. Stress was positively correlated with increased fibromyalgia impact (r=0 .49), as well as increased pain (r=0.29), fatigue (r=0.54), negative mood (r=0.77), sleep problems (r=0.37), cognitive impairment (r=0.47), and self-reported symptoms of autonomic dys-regulation (r=0.30). In turn, pain (r=0.48), fatigue (r=0.56), negative mood (r=0.59), sleep problems (r=0.37), cognitive impairment (r=0.44), and autonomic dys-regulation (r=0.33) were positively correlated with increased fibromyalgia impact. Associations between mediators were moderate in size (rs=0 .29-0.62).
Bivariate correlations revealed that stress was associated with fibromyalgia impact. Stress was also associated with all mediators, and in turn, all mediators were associated with fibromyalgia impact. Given this pattern of bivariate associations, it was prudent to inspect not only the total (bivariate) effects but also the pattern of direct and indirect effects. To better understand the role of each mediator it can be useful to examine the mediators separately in individual mediation models while also examining a multiple mediation model that includes all mediators simultaneously.
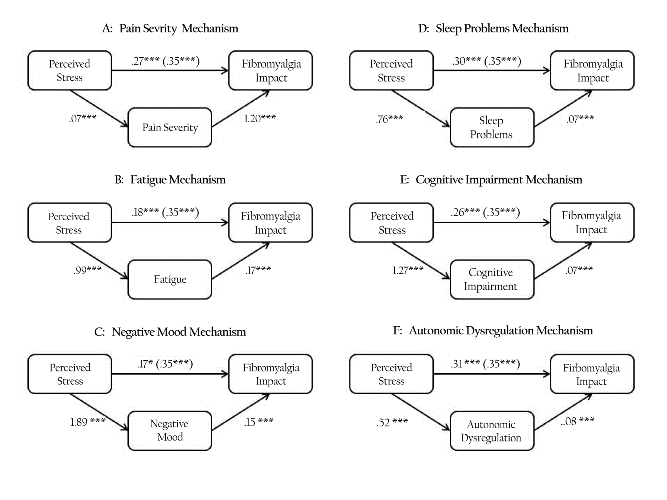
Individual mediation models are presented in Figure 1 and show that the association between stress and fibromyalgia is mediated by pain (B=0.08, p<0.05; Figure 1A), fatigue (B=0.17, p<0.05; Figure 1B), negative mood (B=0.28, p<0.05; Figure 1C), sleep disturbance (B=0.05, p<0.05; Figure 1D), cognitive impairment (B=0.09, p<0.05; Figure 1E), and autonomic dysregulation (B=0.04, p<0.05; Figure 1F). However, in each case mediation is partial and the direct effect of stress on fibromyalgia impact (Bs=0.07–0.31, ps<0.01) remains statistically significant after controlling for the individual mediator.
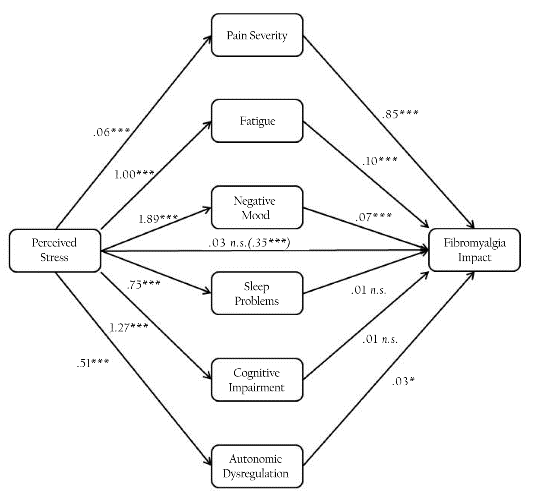
The total effect of stress on fibromyalgia impact was statistically significant (B=0.35, p<0.001; Figure 2), however, the direct effect of stress on fibromyalgia impact was not significant after controlling for all the mediating variables simultaneously (B=0 .03, p >0.05; Figure 2). That is to say, the total indirect effect of all mediators (B=0.32, p<0.05) was statistically significant and fully explained the association between stress and fibromyalgia impact. However, not all mediators conveyed statistically significant indirect effects from perceived stress to fibromyalgia impact in this model. When simultaneously adjusting for all possible mediators in the multiple mediator model it was pain (B=0.05, p<0.05), fatigue (B=0.10, p<0.05), negative mood (B=0.13, p<0.05), and autonomic dysregulation (B=0.01, p<0.05) that showed statistically significant indirect effects (Figure 2). The indirect effects of sleep problems and cognitive impairment were no longer significant in the multiple mediator models.
The exploratory nature of our study, limits our ability to comment on potential clinical implications of these findings. However, if the mechanisms of the relationship between perceived stress and fibromyalgia impact were confirmed in longitudinal and intervention studies, then perceived stress would be a potential target through which to decrease fibromyalgia symptom burden and improve patient quality of life. This is especially important in an illness such as fibromyalgia for which the etiology is unknown and management focuses primarily on symptom reduction.
There are a several limitations to our study. First, our study is cross-sectional, which precludes us from understanding causal relationships. Second, as our sample was comprised of patients who presented to a tertiary care center, our results may not be generalizable to all patients with fibromyalgia, particularly patients with fibromyalgia in the community. This model should be validated in other clinical and community samples. Third, as this was a survey study, we did not have any biomarkers for stress or an objective measure for pain and other symptoms. This could be a consideration for future studies.
Study data were collected and managed using REDCap electronic data capture tools hosted at Mayo Clinic. REDCap (Research Electronic Data Capture) is a secure, web-based application designed to support data capture for research studies, providing: 1) an intuitive interface for validated data entry; 2) audit trails for tracking data manipulation and export procedures; 3) automated export procedures for seamless data downloads to common statistical packages; and 4) procedures for importing data from external sources.
References
- Goldberg RT, Pachas WN, Keith D (1999) Relationship between traumatic events in childhood and chronic pain. Disability and Rehabilitation; 21: 23-30.
- Hallberg LR, Carlsson SG (1998) Psychosocial vulnerability and maintaining forces related to fibromyalgia. In-depth interviews with twenty-two female patients. Scandinavian Journal of Caring Sciences; 12: 95-103.
- Kivimaki M, Leino-Arja P, Virtanen M, Elovaino M, Keltikangas-Jarvinen L, et al. (2004) Work stress and incidence of newly diagnosed fibromyalgia: prospective cohort study. Journal of Psychosomatic Research; 57: 417-422.
- Macfarlane GJ, Norrie G, Atherton K, Power C, Jones GT (2009) The influence of socioeconomic status on the reporting of regional and widespread musculoskeletal pain: results from the 1958 British Birth Cohort Study. Annals of the Rheumatic Diseases; 68: 1591-1595.
- McLean SA, Williams DA, Stein PK, Harris RE, Lyden AK, et al. (2006) Cerebrospinal fluid corticotropin-releasing factor concentration is associated with pain but not fatigue symptoms in patients with fibromyalgia. Neuropsychopharmacology; 31: 2776-2782.
- Paras ML, Murad MH, Chen LP, Goranson EN, Sattler AL (2009) Sexual abuse and lifetime diagnosis of somatic disorders: a systematic review and meta-analysis. JAMA : the Journal of the American Medical Association; 302: 550-561.
- Weissbecker I, Floyd A, Dedert E, Salmon P, Sephton S (2006) Childhood trauma and diurnal cortisol disruption in fibromyalgia syndrome. Psychoneuroendocrinology;31: 312-324.
- Low LA, Schweinhardt P (2012) Early life adversity as a risk factor for fibromyalgia in later life. Pain Research and Treatment 2012: 140-832.
- Gonzalez-Ramirez MT, Garcia-Campayo J, Landero-Hernandez R (2011) The role of stress transactional theory on the development of fibromyalgia: a structural equation model. ActasEspanolas de Psiquiatria; 39: 81-87.
- Malin K, Littlejohn GO (2012) Psychological control is a key modulator of fibromyalgia symptoms and comorbidities. Journal of Pain Research 5: 463-471.
- Malin K, Littlejohn GO (2013) Stress modulates key psychological processes and characteristic symptoms in females with fibromyalgia. Clinical and Experimental Rheumatology 31(6 Suppl 79): S64-S71.
- Bennett RM, Friend R, Jones KD, Ward R, Han BK, et al. (2009) The Revised Fibromyalgia Impact Questionnaire (FIQR): validation and psychometric properties. Arthritis Research & Therapy; 11: R120.
- Williams DA, Arnold LM (2011) Measures of fibromyalgia: Fibromyalgia Impact Questionnaire (FIQ), Brief Pain Inventory (BPI), Multidimensional Fatigue Inventory (MFI-20), Medical Outcomes Study (MOS) Sleep Scale, and Multiple Ability Self-Report Questionnaire (MASQ). Arthritis Care & Research 63 Suppl 11: S86-S97.
- Whipple M, McAllister SJ, Oh TH, Luedtke CA, Toussain LL (2013) Construction of a US Fibromyalgia Registry Using the Fibromyalgia Research Survey Criteria. Clinical and Translational Science; 6: 398-399.
- Cohen S, Kamarck T, Mermelstein R (1983) A global measure of perceived stress. Journal of Health & Social Behavior; 24: 385-396.
- Cohen S (1988) Perceived stress in a probability sample of the United States, in The Social Psychology of Health, Sage Publications, Inc, Thousand Oaks, CA: 31-67.
- 17.Cleeland CS, Ryan KM (1994) Pain assessment: global use of the Brief Pain Inventory. Annals of the Academy of Medicine, Singapore; 23: 129-138.
- Cleeland CS, Ryan KM (1994) Pain assessment: global use of the Brief Pain Inventory. Annals of the Academy of Medicine, Singapore; 23: 129-138.
- Cleeland CS (1985) Measurement and prevalence of pain in cancer. Seminars in Oncology Nursing; 1: 87-92.
- Keller S, Bann CM, Dodd SL, Schein J, Mendoza TR (2004) Validity of the brief pain inventory for use in documenting the outcomes of patients with noncancer pain. The Clinical Journal of Pain; 20: 309-318.
- Radbruch L, Loick G, Kiencke P, Lindena G, Sabatowski R (1999) Validation of the German version of the Brief Pain Inventory. Journal of Pain and Symptom Management; 18: 180-187.
- Tan G, Jensen MP, Thornby JI, Shanti BF (2004) Validation of the Brief Pain Inventory for chronic nonmalignant pain. The journal of pain : official journal of the American Pain Society; 5: 133-137.
- Smets EM, Garssen B, Boke B, De Haes JC (1995) The Multidimensional Fatigue Inventory (MFI) psychometric qualities of an instrument to assess fatigue. Journal of Psychosomatic Research; 39: 315-325.
- Ericsson A, Mannerkorpi K (2007) Assessment of fatigue in patients with fibromyalgia and chronic widespread pain. Reliability and validity of the Swedish version of the MFI-20. Disability & Rehabilitation; 29: 1665-1670.
- Lin, J-MS, Brimmer DJ, Maloney EM, Nyarko E, BeLue R, et al. (2009) Further validation of the Multidimensional Fatigue Inventory in a US adult population sample. Population Health Metrics 7(18).
- Shacham S (1983) A shortened version of the Profile of Mood States. Journal of Personality Assessment; 47: 305-306.
- Bourgeois A, LeUnes A, Meyers M (2010) Full-scale and short-form of the Profile of Mood States: A factor analytic comparison. Journal of Sport Behavior; 33: 355-376.
- Hays RD Martin SA, Sesti AM, Spritser KL (2005) Psychometric properties of the Medical Outcomes Study Sleep measure. Sleep Medicine; 6: 41-44.
- Hays RD, Stewart A (1992) Sleep Measures, in Measuring functioning and well-being: the medical outcomes study approach, A. Stewart and J.E. Ware, Jr., Editors. Duke University Press: Durham: 235-259.
- Cappelleri JC, Bushmakin AG, McDermott AM, Dukes E, Sadosky A, et al. (2009) Measurement properties of the Medical Outcomes Study Sleep Scale in patients with fibromyalgia. Sleep Medicine; 10: 766-770.
- Seidenberg M, Haltiner A, Taylor MA, Hermann BB, Wyler A (1994) Development and validation of a Multiple Ability Self-Report Questionnaire. Journal of Clinical Experimental Neuropsychology; 16: 93-104.
- 32.Sletten DM, Suarez GA, Low PA, Mandrekar J, Singer W (2012) COMPASS 31: a refined and abbreviated Composite Autonomic Symptom Score. Mayo Clinic Proceedings ; 87: 1196-1201.
- Williams DA, Clauw DJ, Glass JM (2011) Perceived cognitive dysfunction in fibromyalgia syndrome. Journal of Musculoskeletal Pain; 19: 66-75.
- Sletten DM, Suarez GA, Low PA, Mandrekar J, Singer W (2012) COMPASS 31: a refined and abbreviated Composite Autonomic Symptom Score. Mayo Clinic Proceedings ; 87: 1196-1201.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 14548
- [From(publication date):
September-2014 - Sep 02, 2025] - Breakdown by view type
- HTML page views : 9905
- PDF downloads : 4643
