Review Article Open Access
Left Ventricular Hypertrophy in Obese Children
Rahaf Z Attar1 and Osama Y Safdar2*
1College of Medicine, King Abdulaziz University, Saudi Arabia
2Pediatric Department, Faculty of Medicine, King Abdulaziz University, Saudi Arabia
- *Corresponding Author:
- Osama Safdar
Department of Pediatrics
Faculty of Medicine
King Abdulaziz University P.O. Box 80215
Jeddah 21589, Saudi Arabia
Tel: +996-5056-20849
Fax: +996-2-6655728
E-mail: safderosama@hotmail.com
Received February 16 2016; Accepted April 21, 2016; Published April 24, 2016
Citation: Attar RZ, Safdar OY (2016) Left Ventricular Hypertrophy in Obese Children. J Obes Weight Loss Ther 6:309. doi:10.4172/2165-7904.1000309
Copyright: © 2016 Attar RZ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Childhood obesity is one of the most troubling health conditions worldwide, and it is associated with many diseases that eventually lead to serious morbidities and mortality in adulthood, such as insulin resistance, type 2 diabetes mellitus, high blood pressure, dyslipidemia, obstructive sleep apnea and subsequent renal, and liver and cardiovascular diseases. Cardiovascular disease carries the most risk of all of the long-term outcomes of obesity because it is associated with serious complications in adult life, such as heart failure, acute coronary syndrome, and premature sudden death. This review aims to address childhood obesity as a worldwide health concern and focuses on the cardiovascular risk and adverse outcomes associated with this condition. This review presents details of obesity-related cardiac structural and functional changes, such as left ventricular hypertrophy (LVH) and dysfunction, respectively. A search of multiple medical databases was performed, and the results yielded many studies related to pediatric left ventricular hypertrophy; seventeen studies were found on left ventricular hypertrophy in obese children from 1980 to 2015. Most of these studies demonstrated that obesity and its comorbidities are important predictors for left ventricular hypertrophy in the pediatric age group. Furthermore, weight reduction is an important measure to reverse these structural changes and reduce the associated risks.
Keywords
Obesity; Left ventricular hypertrophy; Obesity; Children
Introduction
Childhood obesity is one of the most troubling health conditions worldwide [1]. The association of this condition with many diseases that eventually lead to serious morbidities and mortality in adulthood makes it a challenging public health concern. Morbidities include insulin resistance, type 2 diabetes mellitus, high blood pressure, dyslipidemia, obstructive sleep apnea and subsequent renal, liver and cardiovascular diseases. Obesity is also a risk factor for multiple cancers in adults [2-4].
The prevalence of childhood obesity has increased significantly in recent years, and it has become an epidemic in certain areas. The recent WHO Global Database on Child Growth and Malnutrition report states “in the year 2013, an estimate of 42 million children under the age of five around the world are either overweight or obese” [5]. In addition to that, the prevalence of obesity is increasing in all childhood ages, including both males and females of different ethnicities, [6]. Obesity is most often caused by a disturbance in energy balance, which occurs when a child embraces a sedentary life style with decreased physical activity, increased caloric intake, or both. Other factors, such as hormonal, psychosocial, medical and genetic factors, also contribute to the development of obesity but to a much lesser extent.
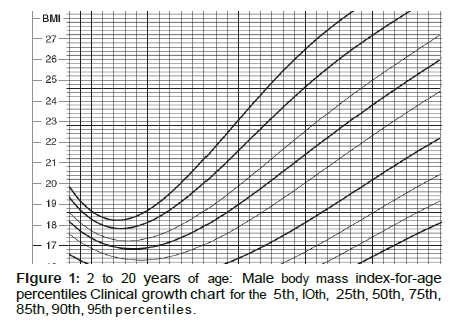
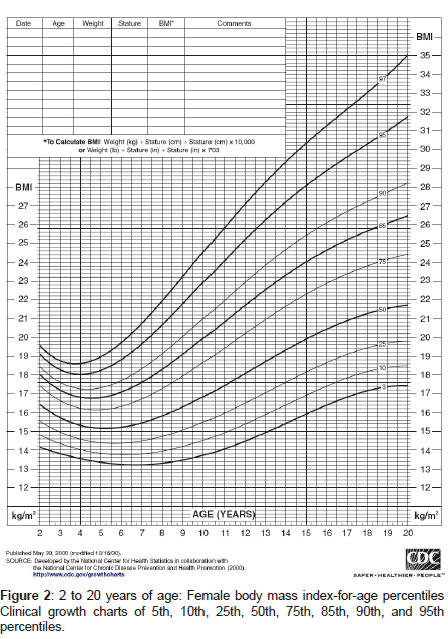
Classification of childhood obesity as “overweight” or “obese” is determined using the body mass index (BMI) of the child compared to the average BMI for children of the same sex and age rather than the fixed parameters used in the adult index. These measurements are plotted on the growth charts displayed in Figures 1 and 2.
The Center of Disease Control and Prevention defines ‘overweight’ as “a BMI at or above the 85th percentile and below the 95th percentile for children and teens of the same age and sex”. ‘Obesity’ is defined as “a BMI at or above the 95th percentile for children and teens of the same age and sex”.
Body mass index is calculated as the child’s weight in kilograms divided by the square of his\her height in meters. Many studies reported that obese children are more likely to turn into obese adults [7]. This observation emphasizes the importance of addressing this problem at an early stage.
Cardiovascular complications carry the greatest risk of all of the long-term complications of obesity because they are associated with serious consequences in adult life, such as heart failure, acute coronary syndrome and premature sudden death [8]. This review addresses childhood obesity and short-term changes related to obesity, including hormonal, metabolic, structural and functional changes, and it focuses on cardiovascular changes and risk. Details address cardiac structural and functional changes, such as left ventricular hypertrophy (LVH) and diastolic dysfunction, respectively.
A literature search of the following databases was performed: PubMed, Medline, CAB direct, and Google scholar. The terms ‘childhood obesity and LVH’, ‘obesity and cardiovascular risk’, ‘hypertension and LVH’ ‘childhood metabolic syndrome’, ‘obesity and cardiomyopathy’, and ‘children’ were used in the search. More than 50 studies are included in this review, and 17 of these studies related to LVH in obese children from 1980 to 2015 (Tables 1 and 2). Summarize these studies at the end of the review. This review does not discuss causes of obesity or the long-term effect of childhood obesity on adults in detail. Very few examples from adult studies are included, primarily for comparisons to emphasize certain points, particularly when data from pediatric studies are lacking.
| Ref. | Sample | Date | Outcome |
|---|---|---|---|
| Dušan et al. [44] | 103 obese subjects aged 9 to 19 years |
2015 | LVH was found in 10 % of subjects |
| Pieruzzi et al. [44] | 526 obese children aged 6 to 15 years |
2015 | Obesity was significantly associated with diastolic dysfunction and correlated with concentric hypertrophy of the left ventricles (P��?<��?0.001) |
| Bonito et al. [58] | 281 obese children aged 6 to 16 years |
2014 | 47 % had abnormal LV geometry, 18.5 % had eccentric LVH, 15.5 % had concentric LVH, and 13 % had concentric LV remodeling. |
| Alp H et al. [37] | 430 obese children aged 6 to 17 years |
2014 | BMI and total fat mass were predictors for abnormal left ventricular geometry. |
| Falkner et al.[51] | 301 African -American adolescents aged f13 to 18 years | 2013 | High left ventricular mass index was found in 24 % obese children compared to 12 % non-obese children. |
| Dhuper et al.[45] | 343 children, 213 obese, 130 non- obese |
2011 | The obese subjects had significantly higher LV mass index (LVMI; 49.6 ± 0.9 vs. 46.0 ± 1.0 g/m2.7, (P = 0.01). Concentric remodeling (CR) was the most prevalent pattern noted in the obese group. |
| Khositseth et al. [54] | 49 obese children aged 3.4 to 15.4 years |
2010 | 47% had LVH, 6% had concentric remodeling, 12% had concentric hypertrophy, and 30% had eccentric hypertrophy. |
| Movahed et al. [33] | 1,500 adolescences between the ages of 12 and 20 years who are actively involved in school sport programs |
2009 | 10.32 % of obese athletes had left ventricular hypertrophy (LVM >215 g) in contrast to 0.2 % of controls. 41.4 % of obese students had relative wall thickness >0.43 vs. 15.7 % of controls. |
| Chinali et al [34] | 460 adolescent participants aged 14 to 20 years Categorized as overweight, obese, or normal BMI |
2006 | Left ventricular hypertrophy was more prevalent in obese (33.5 %) and overweight (12.4 %), compared with normal weight participants (3.5 %); P < (0.001). |
| Kinik et al. [48] | 30 obese children who were matched to a control group |
2006 | Left ventricular hypertrophy was associated with children who had elevated BMI, insulin resistance, and dyslipidemia. |
| Friberg et al [58] | 19 obese and 20 lean adolescents were recruited. | 2004 | Left ventricular mass index was 16 % greater in obese compared to lean adolescents. |
| Urbina et al. [60] | 160 healthy children and young adults, 9 to 22 years old | 1995 | Weight excess is an important predictor for elevated left ventricular mass. |
| Stephen et al [41] | 201 children and adolescents from 6 to 17 years old |
1995 | Lean body mass is a significant predictor for left ventricular mass. |
Table 1: Summary of published studies of LVH in obese children.
| Ref. | Sample | Date | Outcome |
|---|---|---|---|
| Hypertension | |||
| Pieruzzi et al. [44] | 526 obese children aged 6 to 15 years | 2015 | Blood pressure values and hypertension are independently associated with an increase in cardiac mass and the presence of cardiac hypertrophy (P��?<��?0.001 and P��?<��?0.05, respectively). |
| Falkner et al. [51] | 301 African- American adolescents aged 13 to 18 years | 2013 | LVMI was high in hypertensive children (19 %) compared to children with normal blood pressure (12 %), and it was the highest in obese hypertensive children (57 %). |
| Pruette et al. [61] | 141 hypertensive children |
2013 | The prevalence of LVH was 35 % overall, and it is more prevalent in obese African-Americans than non-obese non- African-Americans. |
| Karen et al [50] | 163 adolescents, 44with normal blood pressure, 116 hypertensive | 2004 | The prevalence of LVH in hypertensive children was higher (44.5 %) compared to children with normal blood pressure (9.1 %). |
| Stephen et al. [39] | 201 children and adolescents from 6 to 17 years old |
1995 | The variance of left ventricular mass explained by the model was 77 %. Systolic blood pressure explained only 0.5 % of the variance. |
| Fat mass and distribution | |||
| Pieruzzi et al. [44] | 526 obese children aged 6 to 15 years |
2015 | Waist circumference z-scores were significantly associated diastolic dysfunction. |
| Daniels et al. [49] | 123 children and adolescent aged 9 to 17 years |
1999 | There was a significant correlation between fat percentage and fat distribution with left ventricular mass (r=0.37). |
| Lipid profile | |||
| Kinik et al. [48] | 30 obese children who were matched to a control group |
2006 | There was a slight correlation between insulin and lipid profile with relative wall thickness of the heart, but when these measures were indexed to height, the study failed to show any correlation. |
| Obstructive sleep apnea or nocturnal hypoxemia | |||
| Avelar et al. [57] | 455 severely obese subjects with body mass index 35 to 92 kg/m2 and 59 non- obese reference subjects. | 2007 | 'Low nocturnal oxygen saturation' compared to other factors, such as systolic BP and BMI. showed the strongest probability for predicting LVH (P<0.001). |
Table 2: Summary of published studies of LVH associated with other comorbidities.
The metabolic effect of childhood obesity
Childhood obesity may lead to many metabolic disturbances, including insulin resistance and subsequent type 2 diabetes mellitus, abnormal lipid profiles and fatty infiltration of the liver. This condition may produce a state of hormonal dysregulation and chronic inflammation because of the association of an increased percentage of adipose tissue and elevated inflammatory cells and cytokines. Obesity also contributes to vascular hemostasis irregularities, reproductive abnormalities and unusual immune responses [9,10].
Dyslipidemia
Children with increased body weight tend to exhibit an abnormal lipid profile. Increased body fat directly elevates lipid parameters [11]. Abnormalities that are classically observed in these populations are elevated triglyceride and decreased high- density lipoprotein (HDL) levels [12]. Low-density lipoprotein (LDL) levels may be normal or high.
Insulin resistance and the metabolic syndrome
Weiss et al. [13] defined childhood metabolic syndrome as a cluster of potent risk factors that present during childhood and significantly increase the likelihood of developing type 2 diabetes mellitus, atherosclerosis and subsequent cardiovascular disease in adults. This cluster of risk factors includes hypertension, hyperlipidemia, insulin resistance and obesity. The most significant impact of these factors is shown to be on the adult population, but the sequence of events that lead to the development of the cardiovascular disease begins during childhood.
Many studies demonstrated that obesity is the cornerstone of the development of childhood metabolic syndrome [14,15]. Weiss et al. also reported that the prevalence of metabolic syndrome was directly proportional to the severity of obesity. Metabolic syndrome is observed in up to 50 % of severely obese children and adolescents. The International Diabetes Federation provided more comprehensive criteria to define childhood metabolic syndrome based on the age of the child (table 3).
| The IDF consensus definition of metabolic syndrome in children and adolescents | |||||
|---|---|---|---|---|---|
| Age group (years) |
Obesity* (WC) |
Triglycerides | HDL-C | Blood pressure | Glucose (mmol/L) or Known T2DM |
| 6-<10 | >90° Percentile |
Metabolic syndrome cannot be diagnosed, but further measurement should be made if there is a family history of metabolic syndrome, T2DM, dyslipidemia, cardiovascular disease, hypertension and/or obesity |
|||
| 10-<16 Metabolic syndrome |
>90° percentile or adult cut-off if lower | >1.7 mmol/L (> 150 mg/dL |
<1.03 mmol/L (<40 mg/dL) |
systolic > 130/ diastolic >85mm Hg | >5.6 mmol/L (100mg/dL) (if >5.6mmol/L [or known T2DM] recommend an OGTT) |
| 16+ Metabolic syndrome | Use existing IDF criteria for adults, i.e: Central obesity (defined as waist circumference >94cm for Europid men and > 80cm for Europid women, with ethnicity specific values for other groups*) Plus any two of the following four factors:
|
||||
| WC: waist Circumference; HDL-C: high-density lipoprotein chelostrol; T2DM: type 2 diabetes mellitus; OGTT; oral glucose tolerance test. The IDF Consensus group recognise that these are ethnic, gender and age difference but research is still needed an outcomes to establish risk. |
|||||
Table 3: International Diabetes Federation's definition of metabolic syndrome in children and adolescents
A local hospital-based study was conducted in Saudi Arabia at King Abdulaziz University hospital [16] to determine the prevalence of metabolic syndrome in overweight and obese Saudi children from 2 to 18 years of age. A total of 173 of the 387 participants exhibited hyperinsulinism (44.7 %), 55 children exhibited metabolic syndrome (14.29 %) and 35 children had type 2 diabetes mellitus (9.04 %). This study concluded that metabolic syndrome and type 2 diabetes mellitus were prevalent in overweight and obese children. Early management of obesity, with a hope of prevention, is vital to maintain optimal health and prevent unnecessary complications.
Childhood obesity and blood pressure
Recent studies reported that childhood hypertension was prevalent in overweight and obese children. Some studies stated that childhood obesity was the most relevant risk factor to essential high blood pressure in children [17-19] other risk factors included family history of hypertension and ethnicity. Hypertension in children is categorized based on the normal distribution of blood pressure in children of the same age and sex. Normal blood pressure is defined as “systolic and diastolic blood pressure that is less than the 90th percentile for sex, age, and height on at least three separate occasions”. Stage 1 hypertension is “Systolic and/or diastolic BP between the 95th percentile and 5 mmHg above the 99th percentile or if in adolescents the BP exceeds 140/90 mmHg even <95th percentile”. Stage 2 hypertension is “Systolic and/or diastolic BP ≥ 99th percentile plus 5 mmHg” [20]. High blood pressure is a serious condition that leads to dreadful adverse outcomes, such as cardiovascular accidents, heart failure, renal failure, seizures, and encephalopathy, if left unmanaged.
Weight is strongly associated with blood pressure, which supports the importance of weight loss on reducing elevated blood pressure. Weight loss is one of the most effective measures in the management and prevention of hypertension and its complications. Clarke et al. [21,22] used a 10-year retrospective observational study and reported that any weight change directly affected blood pressure. Weight gain led to elevations in blood pressure, and weight loss helped in reduction of blood pressure.
Childhood obesity and cardiovascular risk
The presence of obesity in children increases the risk of developing cardiovascular disease during adulthood because of the association between obesity and the development of atherosclerosis (which is the main element of the pathogenesis of this disease). Excess adipose tissue in children often leads to physiological, inflammatory and metabolic disturbances. These dysregulations increase the probability of children exhibiting signs of premature cardiac dysfunction and structural abnormalities in subsequent events. Therefore, obese children may exhibit cardiometabolic patterns that are similar to obese adults [23,24].
Wong et al. [25] defined obesity-related cardiomyopathy as “myocardial disease in obese individual that cannot be explained by diabetes mellitus, hypertension, coronary artery disease or other etiologies”.
Recent studies identified obesity as an independent predictor for heart [26,27]. Furthermore, the duration of Obesity is another important predictor for the development of cardiac dysfunction and structural abnormalities, which predisposes children to heart failure in early adulthood [28,29]. Since obese children tend to grow into obese adults, early identification of these cardiovascular changes and weight reduction are important to ensure the reversibility of these changes.
Obesity-related left ventricular hypertrophy (LVH) and cardiac dysfunction
Left ventricular geometry is assessed using echocardiographic measurements. It is classified into the following four groups based on left ventricular mass (LVM) and relative wall thickness (RWT): concentric hypertrophy “increased mass and increased relative wall thickness”, eccentric hypertrophy “increased mass and normal relative wall thickness”, concentric remodeling “normal mass and increased relative wall thickness”, and normal geometry “normal mass and normal relative wall thickness [30] (Figure 3). Left ventricular mass index (LVMI) is calculated by indexing the echocardiographic measurement to height to a 2.7 power. One study of more than 2000 children revealed that “for children above 9 years LVM/height 2.7 values > 40 g/m 2.7 in girls and >45 g/m 2.7 in boys can be considered abnormal because it falls beyond the 95th percentile of the normal LVMI distribution for age and sex” [31]. Cardiac diastolic function is evaluated using a Doppler echocardiography by measuring the mitral E/A ratio.
Obese children, especially children with severe obesity, exhibit a tendency to develop abnormal left ventricular geometry (left ventricular hypertrophy or relative wall thickness) and cardiac dysfunction [32- 34]. The underlying pathogenesis is that obese children have increased metabolic activity due to the presence of excess adipose tissue, which leads to increased heart output and total blood volume to meet the metabolic demands. This compensatory process causes the structural changes and cardiac dysfunction that are occasionally observed in obese children [35].
One study of the relative effect of elevated blood pressure and obesity on left ventricular mass demonstrated statistically significant results, which supports the roles of obesity and elevated blood pressure as independent factors that increase the probability of the occurrence of LVH. Data analysis revealed that “obesity OR = 3.26, p<0.001. In addition, high blood pressure showed an OR = 2.92, p<0.001”. High blood pressure and obesity together exert an additive effect on the development of LHV [36-39].
Relative wall thickness correlates directly to BMI. Other metabolic conditions that are generally associated with obesity, such as waist circumference, insulin resistance, and hyperlipidemia, are also associated with LVH [40].
This is a topic of interest because LVH (among other factors) has been established as an independent risk factor for cardiovascular disease in adults. Multiple data analyses demonstrated that LVMI exhibited the highest independent relative risk for the development of these events in the future [41,42].
Among different left ventricular geometry patterns, concentric hypertrophy is the most prevalent type of LV remodeling observed in obese children, and this pattern in particular is shown to have the worst prognosis. One recent study reported [43] that 40% of obese children had concentric hypertrophy, 40 % had normal geometry, and 20% had eccentric hypertrophy or concentric remodeling. These signs may be present at an early age in obese children, even before 9 years of age. Other studies reported similar results [44,45]. Obesity prevention and early management using weight reduction (conventional or surgical) are important nonpharmacological measures to ameliorate LVM and reverse most cardiac abnormalities that are associated with obesity in children. One study [46] has evaluated morbidly obese adolescents before and after bariatric surgery and demonstrated that the prevalence of concentric LVH improved from 28% pre-operatively to only 3% at follow up. Furthermore, normal LV geometr was more frequently observed from 36% to 79% at follow up, and diastolic function also improved.
Lipid profile and LVH
An abnormal lipid profile is one of the metabolic disturbances caused by obesity and elevated fat mass. Moreover, it is associated with cardiovascular accidents, and plays a role in the pathogenesis of developing atherosclerosis. However, it is not well known whether a significant relationship between dyslipidemia and LVH exists or the relationship is not more than an indirect association because dyslipidemia is a “comorbidity of obesity”. A recent study in Indonesia [47] examined the relationship between lipid profile and LVM in obese adolescents, and the results demonstrated no significant association between lipid profile disturbances with LVM. Another study [48] demonstrated that relative left ventricular wall thickness (intraventricular septum and left ventricular posterior wall thickness) correlated with insulin, very low-density lipoprotein, and triglyceride levels. Data in this area are inconsistent, and further research is needed.
Fat mass and distribution and LVH
In addition to abnormal lipid profile, the percentage of fat and its distribution are also related to LVH. One study demonstrated significant (P<0.05) univariate correlations between fat distribution (central deposition of fat-android pattern) and fat mass with LVM. The correlation coefficient between the android pattern and LVH was equal (r=0.37) [49].
High blood pressure and LVH
Hypertension is an independent predictor for the development of LVH, and LVH is the most prevalent end organ damage in children with hypertension. LVH correlates with the severity of hypertension, and it generally indicates a worse prognosis [50]. Falkner et al. [51] investigated 301 African-American adolescents and reported that “adolescents with higher blood pressure had higher left ventricular mass index (33.2 vs. 38.7 gm/m 2.7, p<0.001) and greater left ventricular hypertrophy”. The effect of blood pressure was independent of obesity.
Obesity and high blood pressure promote concentric LV remolding, but this change is more highly associated with high blood pressure than obesity [52,53].
Obstructive sleep apnea and LVH
Obstructive sleep apnea is defined as a complete cessation of airflow for >10s during sleep. The decrease in airflow leads to a fall in oxygen saturation (i.e., nocturnal hypoxemia). Obstructive sleep apnea is associated with obesity. A strong association between obstructive sleep apnea and LVH was reported previously [54]. LVH was observed in 78-88% of adults [55,56] as well as 40% of children with obstructive sleep apnea. “Low nocturnal oxygen saturation” was the strongest independent predictor for LVH compared to other factors, such as systolic BP and BMI (P<0.001) [57,58].
Conclusion
Obesity is one of the most prevalent public health problems worldwide, and it affects nearly one in five children. Obesity is associated with many short- and long- term complications, and it predisposes children to adult onset obesity, cardiovascular- associated morbidities and premature death.
The process of developing this risk begins during childhood because obesity is an independent risk factor for the development of LVH and cardiac dysfunction. Other factors that are generally associated with obesity, such as dyslipidemia, insulin resistance, fat mass distribution, high blood pressure, and nocturnal hypoxemia, are also related to LVH. These factors, especially high blood pressure and nocturnal hypoxemia, exert a synergetic effect with obesity for the development of LVH, which is more common and prevalent when these two conditions coexist.
Obesity prevention and early management using weight reduction (conventional or surgical) are important nonpharmacological measures to ameliorate left ventricular mass and reverse most cardiac abnormalities that are associated with obesity in children.
Future efforts should focus on parents and the public to recognize the health consequences of obesity in young children and adolescents and spread greater awareness of this condition by encouraging everyone to play an active role in the prevention and early management of obesity in the young. Completion of this goal requires a collaborative effort between the medical profession, government and the public.
Acknowledgment
Special thanks to Abdulrahman Ghoneim and Solafa Ghoneim for their valuable assistance in the reviewing and editing of this article.
References
- [No authors listed] (2000) Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser 894: 1-253.
- Pulgarón ER (2013) Childhood obesity: a review of increased risk for physical and psychological comorbidities. Clin Ther 35: A18-32.
- Ogden CL, Yanovski SZ, Carroll MD, Flegal KM (2007) The epidemiology of obesity. Gastroenterology 132: 2087-2102.
- Biro FM, Wien M (2010) Childhood obesity and adult morbidities. Am J Clin Nutr 91: 1499S-1505S.
- United Nations Children’s Fund, World Health Organization, The World Bank. UNICEFWHO- World Bank (2012) Joint Child Malnutrition Estimates. (UNICEF, New York; WHO, Geneva; The World Bank,Washington
- Ogden CL, Flegal KM, Carroll MD, Johnson CL (2002) Prevalence and trends in overweight among US children and adolescents, 1999-2000. JAMA 288: 1728-1732.
- Serdula MK, Ivery D, Coates RJ, Freedman DS, Williamson DF, et al. (1993) Do obese children become obese adults? A review of the literature. Prev Med 22: 167-177.
- Zalesin KC, Franklin BA, Miller WM, Peterson ED, McCullough PA (2011) Impact of obesity on cardiovascular disease. Med Clin North Am 95: 919-937.
- Saki F, Karamizadeh Z2 (2014) Metabolic syndrome, insulin resistance and Fatty liver in obese Iranian children. Iran Red Crescent Med J 16: e6656.
- Irizarry KA, Brito V, Freemark M (2014) Screening for metabolic and reproductive complications in obese children and adolescents. Pediatr Ann 43: e210-217.
- Williams D, Going S, Lohman T, Harsha D, SrinivasanS, et al. (1992) Body fatness and risk for elevated blood pressure, total cholesterol, and serum lipoprotein ratios in children and adolescents. Am J Public Health 82: 358-363.
- Caprio S, Hyman LD, McCarthy S, Lange R, Bronson M, et al. (1996) Fat distribution and cardiovascular risk factors in obese adolescent girls: importance of the intraabdominal fat depot. Am J ClinNutr 64: 12-17.
- Weiss R (2011) Childhood metabolic syndrome: must we define it to deal with it? Diabetes Care 34: S171-176.
- Weiss R, Bremer AA, Lustig RH (2013) What is metabolic syndrome, and why are children getting it? Ann N Y Acad Sci 1281: 123-140.
- Molnár D (2004) The prevalence of the metabolic syndrome and type 2 diabetes mellitus in children and adolescents. Int J Obes Relat Metab Disord 28 : S70-74.
- Al-Agha A, Ocheltree A, Shata N (2012) Prevalence of hyperinsulinism, type 2 diabetes mellitus and metabolic syndrome among Saudi overweight and obese pediatric patients. Minerva Pediatr 64:623-31
- Urrutia-Rojas X, Egbuchunam CU, Bae S, Menchaca J, Bayona M, et al. (2006) High blood pressure in school children: prevalence and risk factors. BMC Pediatr 6:32.
- Pela I, Modesti PA, Cocchi C, Cecioni I, Gensini GF, et al. (1990) Changes in the ambulatory arterial pressure of normotensive obese children. Pediatr Med Chir 12: 495-497.
- Fixler D, Kautz J, Dana K (1980) Systolic blood pressure differences among pediatric epidemiological studies. Hypertension 2: I3-I7.
- (2004) The Fourth Report on the Diagnosis, Evaluation, and Treatment of High Blood Pressure in Children and Adolescents. PEDIATRICS 114: 555-576.
- Clarke WR, Woolson RF, Lauer RM (1986) Changes in ponderosity and blood pressure in childhood: the Muscatine Study. Am J Epidemiol 124: 195-206.
- Cote AT, Harris KC, Panagiotopoulos C, Sandor GG, Devlin AM (2013) Childhood obesity and cardiovascular dysfunction. J Am Coll Cardiol 62: 1309-1319.
- McCrindle BW (2015) Cardiovascular consequences of childhood obesity. Can J Cardiol 31: 124-130.
- Herouvi D, Karanasios E, Karayianni C, Karavanaki K (2013) Cardiovascular disease in childhood: the role of obesity. Eur J Pediatr 172: 721-732.
- Wong C, Marwick T (2007) Obesity cardiomyopathy: pathogenesis and pathophysiology. Nature Clinical Practice Cardiovascular Medicine 4: 436-443.
- Baena-D´iez JM, Byram AO , MaríaGrau, Fernández GO, Vidal-Solsona M, et al. (2010) Obesity and the risk of heart failure. : Zona Franca Cohort Study Clin Cardiol 12: 760-764
- Hubert HB, Feinleib M, McNamara PM, Castelli WP (1983) Obesity as an independent risk factor for cardiovascular disease: a 26-year follow-up of participants in the Framingham Heart Study. Circulation 67: 968-977.
- Alpert M, Terry B, Mulekar M, Cohen M, Massey C, et al. (1997) Cardiac Morphology and Left Ventricular Function in Normotensive Morbidly Obese Patients With and Without Congestive Heart Failure, and Effect of Weight Loss. The American Journal Of Cardiology 80: 736-740
- Wong CY, O'Moore-Sullivan T, Leano R, Byrne N, Beller E, et al. (2004) Alterations of left ventricular myocardial characteristics associated with obesity. Circulation 110: 3081-3087.
- Krumholz HM, Larson M, Levy D (1995) Prognosis of left ventricular geometric patterns in the Framingham Heart Study. J Am Coll Cardiol 25: 879-884.
- Khoury PR, Mitsnefes M, Daniels SR, Kimball TR (2009) Age-specific reference intervals for indexed left ventricular mass in children. J Am SocEchocardiogr 22: 709-714.
- Khositseth A, Suthutvoravut U, Chongviriyaphan N (2009) Left Ventricular Mass and Geometry in Obese Children. Asian J Of Clinical Nutrition 1: 58-64.
- Movahed MR, Martinez A, Greaves J, Greaves S, Morrell H, et al. (2009) Left ventricular hypertrophy is associated with obesity, male gender, and symptoms in healthy adolescents. Obesity (Silver Spring) 17: 606-610.
- Chinali M, de Simone G, Roman MJ, Lee ET, Best LG, et al. (2006) Impact of obesity on cardiac geometry and function in a population of adolescents: the Strong Heart Study. J Am CollCardiol 47: 2267-2273.
- Alpert MA (2001) Obesity cardiomyopathy: pathophysiology and evolution of the clinical syndrome. Am J Med Sci 321: 225-236.
- Dušan P, Tamara I, Goran V, Gordana ML, Amira PA (2015) Left ventricular mass and diastolic function in obese children and adolescents. Pediatr Nephrol 30: 645-652.
- Alp H, Karaarslan S, EklioÄŸlu BS, Atabek ME, Baysal T (2014) The effect of hypertension and obesity on left ventricular geometry and cardiac functions in children and adolescents. J Hypertens 32: 1283-1292.
- Falkner B, DeLoach S, Keith SW, Gidding SS (2013) High risk blood pressure and obesity increase the risk for left ventricular hypertrophy in African-American adolescents. J Pediatr 162: 94-100.
- Daniels SR, Kimball TR, Morrison JA, Khoury P, Witt S, et al. (1995) Effect of Lean Body Mass, Fat Mass, Blood Pressure, and Sexual Maturation on Left Ventricular Mass in Children and Adolescents : Statistical, Biological, and Clinical Significance. Circulation 92: 3249-3254
- Kinik ST, Varan B, Yildirim SV, Tokel K (2006) The effect of obesity on echocardiographic and metabolic parameters in childhood. J PediatrEndocrinolMetab 19: 1007-1014.
- Casale PN (1986) Value of Echocardiographic Measurement of Left Ventricular Mass in Predicting Cardiovascular Morbid Events in Hypertensive Men. Annals of Internal Medicine Ann Intern Med 105: 173-178
- Levy D, Garrison RJ, Savage DD, Kannel WB, Castelli W P (1990) Prognostic Implications of Echocardiographically Determined Left Ventricular Mass in the Framingham Heart Study. New England Journal of Medicine N Engl J Med 322: 1561-1566.
- Binkley CM, Jing L, Suever JD, Umasankar N, Wehner GJ, et al. (2015) Children with obesity have cardiac remodeling and dysfunction: A cine DENSE magnetic resonance imaging study. Journal of Cardiovascular Magnetic Resonance J CardiovascMagnReson17.
- Pieruzzi F, Antolini L, Salerno FR, Giussani M, Brambilla P, et al. (2015) The role of blood pressure, body weight and fat distribution on left ventricular mass, diastolic function and cardiac geometry in children. J Hypertens 33: 1182-1192.
- Dhuper S, Abdullah RA, Weichbrod L, Mahdi E, Cohen HW (2011) Association of obesity and hypertension with left ventricular geometry and function in children and adolescents. Obesity (Silver Spring) 19: 128-133.
- Ippisch HM, Inge TH, Daniels SR, Wang B, Khoury PR, et al. (2008) Reversibility of cardiac abnormalities in morbidly obese adolescents. J Am CollCardiol 51: 1342-1348.
- Kaunang ED, As’ad S, Sarah M, Warouw A, Kabo P (2014) Relationship between Lipid Profile and Left Ventricular Mass in Obese Adolescents Sch. J App Med Sci 2:3353-3356
- Daniels SR, Morrison JA, Sprecher DL, Khoury P, Kimball TR (1999) Association of body fat distribution and cardiovascular risk factors in children and adolescents. Circulation 99: 541-545.
- Mcniece KL, Gupta-Malhotra M, Samuels J, Bell C, Garcia K, et al. (2007) Left Ventricular Hypertrophy in Hypertensive Adolescents: Analysis of Risk by 2004 National High Blood Pressure Education Program Working Group Staging Criteria. Hypertension 50: 392-395.
- Falkner B, DeLoach S, Keith SW, Gidding SS (2013) High risk blood pressure and obesity increase the risk for left ventricular hypertrophy in African-American adolescents. J Pediatr 162: 94-100.
- Woodiwiss AJ, Libhaber CD, Majane OH, Libhaber E, Maseko M (2008) Obesity Promotes Left Ventricular Concentric Rather Than Eccentric Geometric Remodeling and Hypertrophy Independent of Blood Pressure. American Journal of Hypertension 21: 1144-1151
- Cloward TV, Walker JM, Farney RJ, Anderson JL (2003) Left Ventricular Hypertrophy Is a Common Echocardiographic Abnormality in Severe Obstructive Sleep Apnea and Reverses With Nasal Continuous Positive Airway Pressure. Chest 124: 594-601.
- Amin RS, Kimball TR, Bean JA, Jeffries JL, Willging JP, et al. (2002) Left ventricular hypertrophy and abnormal ventricular geometry in children and adolescents with obstructive sleep apnea. Am J RespirCrit Care Med 165: 1395-1399.
- Avelar E, Cloward TV, Walker JM, Farney RJ, Strong M, et al. (2006) Left Ventricular Hypertrophy in Severe Obesity: Interactions Among Blood Pressure, Nocturnal Hypoxemia, and Body Mass. Hypertension 49: 34-39.
- Di Bonito P, Sanguigno E, Forziato C, Di Fraia T, Moio N, et al. (2014) Glomerular filtration rate and cardiometabolic risk in an outpatient pediatric population with high prevalence of obesity. Obesity (Silver Spring) 22: 585-589.
- Friberg P, Allansdotter-Johnsson A, Ambring A, Ahl R, Arheden H, et al. (2004) Increased left ventricular mass in obese adolescents. Eur Heart J 25: 987-992.
- Urbina EM, Gidding SS, Bao W, Pickoff AS, Berdusis K, et al. (1995) Effect of body size, ponderosity, and blood pressure on left ventricular growth in children and young adults in the Bogalusa Heart Study. Circulation 91: 2400-2406.
- Pruette CS, Fivush BA, Flynn JT, Brady TM (2013) Effects of obesity and race on left ventricular geometry in hypertensive children. Pediatr Nephrol 28: 2015-2022.
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 13789
- [From(publication date):
April-2016 - Aug 28, 2025] - Breakdown by view type
- HTML page views : 12728
- PDF downloads : 1061