Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
Myofascial Pain Syndrome - A Surgical Perspective
| Pianta WR and Burkhead WZ Jr* | |
| WB Carrell Memorial Clinic, North Central Expressway, Dallas, USA | |
| Corresponding Author : | Wayne Zealous Burkhead WB Carrell Memorial Clinic 9301 North Central Expressway, Dallas TX, 75231, USA Tel: (214) 720 9339 Fax: (214) 397 1539 E-mail: wburkheadj@gmail.com |
| Received: February 16, 2015 Accepted: November 18, 2015 Published: November 25, 2015 | |
| Citation: Pianta WR, Burkhead WZ Jr (2015) Myofascial Pain Syndrome – A Surgical Perspective. J Pain Relief 4:215. doi:10.4172/2167-0846.1000215 | |
| Copyright: © 2015 Pianta WR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pain & Relief
Abstract
In this article we discuss the evaluation of a typical patient referred to our clinic with myofascial pain syndrome. With an understanding of the underlying pathoanatomy and pathophysiology we discuss the rationale and potential benefits of surgery for some patients.
| Case Report |
| Our understanding of myofascial pain syndrome (MPS) has progressed a great deal in the past decade. However, our review reveals no published data regarding surgical management. The senior author was introduced to trigger point denervation fasciectomy by Dr.Harry Ornstein, of the Plastic Surgery Department, University of Texas, Southwestern Medical School. Over the past 20 years the senior author has used this technique to help patients with recalcitrant MPS. The purpose of this paper is to introduce the reader to the pathophysiology of this condition and a novel operative procedure, which can alleviate pain in patients who have previously been considered beyond help. We discuss our surgical management of this disease, as highlighted by presentation of a typical patient. |
| A 59 year old Caucasian right-hand dominant woman was referred to our clinic with right shoulder pain. Her pain was periscapular and it had been present for many years. She rated the pain 8/10 on the visual analogue scale (VAS). There was no inciting trauma she could recall. Otherwise she had medicated hypertension and hypercholesterolemia, and a short history of treatment for Parkinson’s disease. |
| Clinically there was no wasting of the shoulder girdle. Point tenderness was elicited and reproducible in two foci within the midportion of the infraspinatus fossa. She had symmetrical range of movement of her shoulders and no pain or weakness on testing of rotator cuff musculature. Her acromio-clavicular joint and long head of biceps tendon were non-tender. Cervical spine range of motion was unrestricted and did not initiate any girdle/limb pain. No neurological abnormalities we present. |
| Plain radiography of the shoulder was normal. MRI revealed supraspinatus tendinopathy and acromio-clavicular joint degeneration. |
| Exhaustive non-operative treatment is the authors’ preferred management of MPS. Simple analgesics (acetaminophen, 1000 mg, orally, qid regularly) and anti-inflammatory medications (diclofenac, 50 mg, orally, tds regularly) are prescribed, as well as muscle relaxants at night (cyclobenzaprine, 2.5 mg to 10 mg, orally, two hours before bed, regularly). Other modalities, including moist heat, massage and phonophoresis are utilized, along with physical therapy focusing on scapula stabilizing and shoulder rebalancing exercises. We perform dual purpose, diagnostic and therapeutic, injections into the trigger points and anticipate total pain relief. Initially, the trigger points are localized with 5/8th inch, 25 gauge needles with a syringe containing lidocaine 1%, 2 cc - this is used to infiltrate the trigger points and overlying subcutaneous tissues and skin. The needles remain in-situ as the lidocaine takes effect. Subsequently, a syringe with a mixture of triamcinolone, 2 cc with bupivocaine 0.75%, 4 cc, is attached to the hub of the needles, injected and evenly distributed between the trigger points. We perform three injections at three-weekly intervals. |
| We feel it judicious to consider in the differential diagnosis cervical radicular pain, thoracic outlet syndrome, primary shoulder girdle pathology such as rotator cuff disease, acromio-clavicular joint arthrosis and snapping scapula syndrome, as well as fibromyalgia. In regards to fibromyalgia, we follow the American College of Rheumatology 1990 Criteria of chronic, widespread pain in combination with tenderness at 11 or more specific tender points [1]. We recognize the issues inherent in diagnosing fibromyalgia [2]. In contrast to these patients, candidates for this surgery have isolated pain to the periscapular region of their shoulder girdle, either unilaterally or bilaterally. |
| Our patient’s pain was relieved temporarily with each of her injections but persisted despite all non-operative treatments. She returned to discuss further management. It is our experience that this type of patient can have a dramatic improvement in pain after surgical intervention and is a good candidate for surgery. |
| On the day of surgery, prior to any analgesics and anesthetics, the surgeon identifies the trigger points and marks them with an indelible pen. Each trigger point is approached through a 5 cm longitudinal incision overlying the point. Sharp dissection proceeds to the deep fascia. Subcutaneous flaps are elevated until a 5 cm by 5 cm area of fascia is exposed. Utilizing sharp dissection and cautery this 5 cm by 5 cm area is excised. The epimysium is teased off the muscle belly fibers and excised as well. Subjectively, the fascia and subcutaneous tissue in these patients is thickened, however the specimens are not routinely sent to pathology for microscopic examination. See Figure 1, below, for macroscopic appearance of specimen. Care is taken to achieve meticulous hemostasis. The wound is thoroughly lavaged with normal saline and multi-modal local anesthetic is generously infiltrated in the region. The wound is closed in layers and a pressure dressing applied. Frequently a drain is placed given the large dead space as a result of the development of subcutaneous soft tissue flaps. |
| Post-operatively, there is no need for immobilization in an arm sling, however it can be used for comfort. Gentle range of movement exercises are commenced immediately. Loading through the limb is permitted once wounds are healed. This lady recovered without complication and by the post-operative review at three weeks, she had no pain (VAS 0/10) and was using her arm as needed. |
| MPS is a condition manifested by a characteristic pattern of referred pain with reproducible generation of this pain on palpation of a consistent focus overlying a muscle belly. At this point a taut band can be palpated. This is a highly receptive structure and cell depolarization occurs on stimulation/triggering of the taut band, hence this condition is also known as myofascial trigger point pain syndrome, coined by American physician Janet Travell [3-6]. |
| The etiology of MPS is not proven [7]. Trauma, ranging from indirect injury to repetitive use, for example lifting, is suspected as a factor in periscapular MPS [8]. A number of alternate factors have been proposed [4,9]. |
| In search of the pathological structure researchers’ attention has turned to the deep fascia and epimysium. |
| The epimysium is intimately related to its underlying muscle fibers and is separated from the deep fascia by loose connective tissue [7,10]. The loose connective tissue, containing hyaluronic acid, has an important role in allowing normal gliding on one another [11]. Microscopically, the epimysium has connections with muscle spindles [12,13]. These are highly sensitive receptors within the muscle belly, which infer a central role in movement control [7]. This proprioceptive function is reinforced by the presence of free nerve endings rather than Pacinian or Ruffini corpuscles within the epimysium [7,14]. |
| On a histological level, the deep fascia undergoes fibrous change in response to damage to its underlying epimysium in pigs [11]. A change in structure of the deep fascia can reduce the motion between tissue planes [15]. The epimysium transmits a significant proportion of the force generated by a muscle, however when diseased, this is impaired [16]. |
| The above describes Partanen’s muscle spindle hypothesis for development of MPS [8]. It is our opinion surgical treatment of this condition, based on this hypothesis, has merit as it excises the pathological tissue. |
| Given the basic science underpinning this condition, as well as the lack of awareness on the part of physicians and surgeons, we are attempting a review of a much larger series of patients who have undergone this procedure. Obviously, a level 1 or level 2 study would be the optimum way of confirming the efficacy of this procedure. |
References
- Wolfe F, Smythe HA, Yunus MB, Bennett RM, Bombardier C, et al. (1990) The American College of Rheumatology 1990 Criteria for the Classification of Fibromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum 33: 160-172.
- Katz RS, Wolfe F, Michaud K (2006) Fibromyalgia diagnosis: a comparison of clinical, survey, and American College of Rheumatology criteria. Arthritis Rheum 54: 169-176.
- Ge HY, Fernández-de-Las-Peñas C, Madeleine P, Arendt-Nielsen L (2008) Topographical mapping and mechanical pain sensitivity of myofascial trigger points in the infraspinatus muscle. Eur J Pain 12: 859-865.
- Cummings M, Baldry P (2007) Regional myofascial pain: diagnosis and management. Best Pract Res ClinRheumatol 21: 367-387.
- Ge HY, Fernández-de-las-Peñas C, Arendt-Nielsen L (2006) Sympathetic facilitation of hyperalgesia evoked from myofascial tender and trigger points in patients with unilateral shoulder pain. ClinNeurophysiol 117: 1545-1550.
- Hocking MJ (2013) Exploring the central modulation hypothesis: do ancient memory mechanisms underlie the pathophysiology of trigger points? Curr Pain Headache Rep 17: 347.
- Stecco A, Gesi M, Stecco C, Stern R (2013) Fascial components of the myofascial pain syndrome. Curr Pain Headache Rep 17: 352.
- Partanen JV, Ojala TA, Arokoski JP (2010) Myofascial syndrome and pain: A neurophysiological approach. Pathophysiology 17: 19-28.
- Henriksson KG, Backman E, Henriksson C, de Laval JH (1996) Chronic regional muscular pain in women with precise manipulation work. A study of pain characteristics, muscle function, and impact on daily activities. Scandanavian Journal of Rheumatology. 25: 213-223.
- Findley T, Chaudhry H, Stecco A, Roman M (2012) Fascia research--a narrative review. J BodywMovTher 16: 67-75.
- McCombe D, Brown T, Slavin J, Morrison WA (2001) The histochemical structure of the deep fascia and its structural response to surgery. J Hand Surg Br 26: 89-97.
- Boyd-Clark LC, Briggs CA, Galea MP (2002) Muscle spindle distribution, morphology, and density in longuscolli and multifidus muscles of the cervical spine. Spine (Phila Pa 1976) 27: 694-701.
- Maier A (1999) Proportions of slow myosin heavy chain-positive fibers in muscle spindles and adjoining extrafusal fascicles, and the positioning of spindles relative to these fascicles. Journal of Morphology 242: 157–65.
- Klingler W, Velders M, Hoppe K, Pedro M, Schleip R (2014) Clinical relevance of fascial tissue and dysfunctions. Curr Pain Headache Rep 18: 439.
- Langevin HM, Fox JR, Koptiuch C, Badger GJ, Greenan-Naumann AC, et al. (2011) Reduced thoracolumbar fascia shear strain in human chronic low back pain. BMC MusculoskeletDisord 12: 203.
- Purslow PP (2010) Muscle fascia and force transmission. J BodywMovTher 14: 411-417.
Figures at a glance
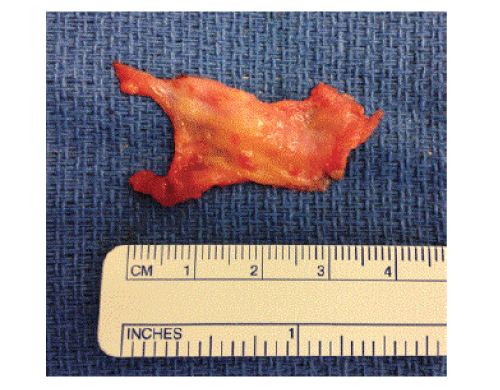 |
| Figure 1 |
Post your comment
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 20123
- [From(publication date):
November-2015 - Aug 01, 2025] - Breakdown by view type
- HTML page views : 19054
- PDF downloads : 1069
