Research Article Open Access
Overweight and Obesity in the Reproductive-Age Population of the Central Pennsylvania Women's Health Study
| Geyer N* | |
| Research Technologist III, Department of Public Health Sciences, Division of Epidemiology, Penn State University, Pennsylvania, USA | |
| Corresponding Author : | Nathaniel Geyer, MS Research Technologist III Department of Public Health Sciences Division of Epidemiology Penn State University Pennsylvania, USA Tel: 717-531-0003 ext 281213 E-mail: nrg139@psu.edu |
| Received December 12, 2012; Accepted January 04, 2013; Published January 07, 2013 | |
| Citation: Geyer N (2013) Overweight and Obesity in the Reproductive-Age Population of the Central Pennsylvania Women’s Health Study. J Obes Wt Loss Ther 3:158. doi:10.4172/2165-7904.1000158 | |
| Copyright: © 2013 Geyer N. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Over 54% of currently non-pregnant women aged 18-45 in Central Pennsylvania are overweight or obese. To examine the overall health effects in women, the Central Pennsylvania Women’s Health Study (CePAWHS) had 2,002 women aged 18-45 complete a Random Digit Dial (RDD) general population telephone interview on their health status and health risk indicators for adverse pregnancy outcomes. This study of the CePAWHS population examined the correlates of overweight and obesity in a unique sample of reproductive-age women. The survey measured a large number of health-related variables including pregnancy history. This study also considered whether the definition of obesity affects the identification of correlates. Telephone interview participants were categorized as normal overweight or obese according to the BMI index and analyzed as BMI continuous. ANOVA and Chi-square tests were used to examine differences between BMI continuous and categorical variables. Odds ratios from logistic regression models and linear regression from ANCOVA were used to examine cross-sectional associations of the BMI continuous and categorical. Of the population, 27% were overweight and 25% obese using the BMI index and had a mean BMI of 26.99 ± 6.95. Other variables analyzed included environmental factors, pregnancy outcomes, and health habits and conditions. This research found that obesity in reproductive-age women is associated with a variety of environmental and health-related factors.
| Keywords |
| Body Mass Index (BMI); Obesity; Overweight; Reproductive-age women; Pregnancy outcomes |
| Abbreviations |
| BMI: Body Mass Index; RDD: Random Digit Dial; CePAWHS: Central Pennsylvania Women’s Health Study; SCT: Social Cognitive Theory |
| Introduction |
| Obesity is an epidemic that adversely affects health in women of childbearing age, putting them at risk for cardiovascular disease, type II diabetes, hypertension, and many other chronic disorders [1-3]. Stigma attached to obesity in some cultures can lead to depression and anxiety [2,3], and is often associated with poor levels of health status [4]. Obesity and its associated health effects are more prevalent in women than in men: with the female to male difference in obesity was +4.6% [5]. Some reasons are that people are now consuming more calories and participating less in physical activity [1,6,7]. It also appears that cultural practices, economic growth, and modernization of food markets are also contributing factors to the obesity epidemic [1,7]. The goal of this study is to examine the behavioral, environmental, and personal factors of obesity in women using social cognitive theory. |
| Social cognitive theory provides a framework for understanding health-related variables such as behavioral, environmental, and personal factors. It has been applied to healthy eating behaviors in women and children [8,9]. In a population looking at Asian Americans immigrants found that environmental influences influenced health perceptions of obesity [8]. In addition, how mothers view providing healthy foods and limiting unhealthy foods are effective in prevention of obesity in their children [9]. There also was a strong connection of TV viewing and self-control as prevention of obesity [8,9]. In addition, a study using the Nurses’ Health Study found a connection in women with prolonged TV watching and obesity [10]. Other studies applying a similar theoretical framework found that as physical activity and sleep decrease, hours sitting per day increases causing BMI to increase [11- 14]. In addition, one factor influencing weight during the childbearing years is pregnancy history, since weight gain during pregnancy can carry over into post-pregnancy weight–other health-related and environmental factors also play a role. This study integrates behavior indicators, health indictors, and demographic variables into the model. |
| This study examines the correlates of overweight and obesity in a unique sample of reproductive-age women from a survey that measured a large number of health-related variables including pregnancy history (according to SCT). The study also considers whether the definition of obesity affects the identification of correlates. The main hypothesis is obesity is dependent on different health-related, behavioral, and environmental variables. Another hypothesis was that there was no difference between using BMI as a continuous and categorical outcome of interest. |
| Materials and Methods |
| The Central Pennsylvania Women’s Health Study (CePAWHS) included a population-based survey of women of reproductive age residing in a predominately rural 28-county region in central Pennsylvania. The original purpose of the survey was to estimate the prevalence of multiple risk factors for preterm birth and Low Birth Weight (LBW), identify subpopulations at greatest risk, and provide a baseline for a prospective cohort study to link pre-pregnancy health with pregnancy outcomes. The study was reviewed and approved by the Institutional Review Board of the Penn State College of Medicine and a certificate of confidentiality from NIH (CC-HD-04024) was obtained. |
| Sample and data collection |
| A Random-Digit Dial (RDD) telephone survey was conducted between September 2004 and March 2005. Inclusion criteria were female gender, age 18-45 years, residence in the 28-county target region, and English or Spanish speaking. The study sample was obtained using a disproportionately stratified RDD design, oversampling rural counties and areas with high minority populations. The final sample of 2,002 women represented a cooperation rate of 63% (Cronbach α=0.83), and the sample was highly representative of the target population with regard to age, race/ethnicity, educational level, and poverty status. Further details of the sampling design, response rate, and representativeness have been previously published [15]. |
| For purposes of this analysis, the following exclusion was imposed: currently pregnant (n=77). Currently pregnant women were excluded because it is expected that they would inflate average BMI and impact the number of overweight and obese cases. In addition, there were 44 individuals who had missing data for BMI calculation, which was computed using self-reported weight and height. Thus, the analytic sample for this paper is 1,881 women. |
| Measures |
| Obesity was operationalized by one definition based on the Body Mass Index (BMI) scale. For purposes of analysis, we also created a three-category variable that defined normal weight as a BMI of less than 24.99; overweight as a BMI of equal to or greater than 25, but less than 30 kg/m2 and obesity (including Morbid Obesity) as a BMI of greater than 30 kg/m2. Due to the small sample of morbid obesity women (n=7) the cohort was collapsed into obese category. |
| Health-related variables (i.e. personal and behavioral) included number of prior pregnancies, fruit and vegetable consumption, smoking, binge drinking, hours of sleep, physical activity, and hours sitting per day. Pregnancy history was measured as number of prior pregnancies, which are expected to be associated with the woman’s current weight. The research team created a variable that categorized previous pregnancies into four groups: no pregnancies, one pregnancy, two pregnancies, and three or more pregnancies. For fruit and vegetable consumption, we categorized the data into a yes/no variable that asked, “Do you eat fruits or vegetable at least once per day?” Physical activity was also categorized as yes/no depending on whether or not respondents reported getting 30+ minutes of physical activity on 4+ days per week. Binge drinking was grouped into those who drank fewer than five drinks on one occasion during the past month and those who drank five or more drinks on one occasion, defined as binge drinking, during the past month. Hours of sleep was categorized as less than six hours of sleep, six hours, seven hours, and greater than seven hours of sleep per night. The sedentary hour’s variable was defined as less than or equal to one hour, two hours, three hours, and greater than or equal to four hours daily. |
| Socio-demographic (i.e. environmental) variables included: age group, educational level, race/ethnicity, poverty level, and urban versus rural residence. Age was defined as 18-35 and 36-45. Educational level was defined as high school graduate or less and some college or more. Poverty level was defined as poverty, near poverty, and not poverty. Based on the Rural-Urban Commuting Area (RUCA) codes [16], the effects of urban verses rural residence were examined. |
| Analyses |
| Analyses were conducted using SAS software for Windows, Version 9.3 (SAS Institute Inc., Cary, NC). Analyses used to examine the differences in the BMI continuous variable using ANOVA and multivariable, ANCOVA, linear regression. Also a three category BMI variable of normal, overweight, obese used chi square tests and multivariable proportional odds logistic regression. For the chi square test and ANOVA, the variable output was reported as p-values and correlations. For linear regression, the output was reported with F values and p-values (<0.05). Post-hoc tests using Bonferroni corrections methods were also performed for the ANCOVA model. For logistic regression, the output was reported with odds ratios and 95% confidence intervals. Finally, geospatial representation of the population of interest was performed using ArcGIS 10. |
| Results |
| The mean and standard deviation of the BMI continuous variable was 26.99 ± 6.95, which show the study population as slightly overweight. The percentages of women were underweight (2.13%), normal (46.04%), overweight (26.58%) and obesity, including morbid obesity (25.25%). For purposes of analyzes, the underweight and normal BMI categories were grouped together. These numbers show that the percentage of women who were either overweight or obese was close to 52%. |
| The statistical analysis using the chi square test and ANOVA are found in table 1. It was found that the number of prior pregnancies health-related variable was significant, using the BMI categorical model. The consumed vegetables at least daily variable was not significant using the BMI categorical model, but was significant for the BMI variable. A related variable, consumes fruit at least daily, was significant using both the BMI categorical model and the BMI variable. This finding reflects the direct relationship between nutrition and BMI. The healthrelated variables of physical activity meeting current recommended levels and hours sitting per day were significant for both BMI variables. This reinforces the previously documented adverse effect of sedentary behavior on BMI. The socio-demographic variables showed no difference in significance between the BMI and BMI categorical variables. Either both the BMI and BMI categorical variables showed significance, such as in the case of the poverty level variable, or, as in the case of the urban versus rural residence variable, neither the BMI or BMI categorical variable were significant (as depicted by the map of dot-density of cases by BMI in figure 1). The significance of the poverty level variable and non-significance of the urban versus rural residence variable with regard to the BMI and BMI categorical variables could suggest an environmental effect as a cause of obesity [17]. |
| The multivariable analyses of obesity using linear regression and logistic regression analyses are shown in table 2. The basic findings for the two outcome variables are similar. Physical activity meeting the current recommended level was associated with lower BMI and lower categorized BMI. Sleeping less than the recommended amount of 7-8 hours per night was associated with higher BMI and higher categorized BMI. More hours sitting per day was associated with higher BMI and higher categorized BMI. Cigarette smoking is associated with lower BMI and lower categorized BMI. The age group of women ages 36-45 as compared to women ages 18-35 is associated with higher BMI and higher categorized BMI. A higher education level of some college or more as compared to high school or less is associated with lower BMI. Also of interest is that the number of prior pregnancies, which was significant at the bivariate level, was not significant in the multivariate models. Controlling for age and other adjusters probably accounts for these discrepancies. A similar effect was found for poverty level and eating fruits at least daily. Binge drinking in the past month appeared to have no effect on obesity in the bivariate or multivariate model analyses; this may be due to sample size. Rurality was found not to have a significant effect on obesity based on the dichotomized variable urban versus rural residence. In addition, after correcting the ANCOVA BMI model using post hoc Bonferroni corrections the variables physical activity, smoking, age group, and number of hours sitting were significant at the <0.05 level. Additional analysis of co-morbidities, hypertension, high cholesterol, and diabetes, were found to be significant with BMI continuous and categorical (data not shown). |
| Discussion |
| This study looked at obesity in the context of preconceptiual health in reproductive-age women. Data from this study show that living in isolated, rural towns has a slight non-significant effect on obesity. Household income near poverty is another factor in pre-pregnancy obesity in this study. It was also found that a relationship exists between decreased sleep and obesity. Finally, specific to the target population of this study, there appeared to be a relationship between pre-pregnancy obesity and several co-morbidities that can lead to adverse pregnancy and birth outcomes. Therefore the hypothesis which suggested various variables was supported. |
| BMI can be defined using cutoffs and as a continuous variable without losing important information. This study showed that the results of the two models are comparable in women of childbearing age and supports the continued use of BMI for women. This allowed testing the hypothesis of no difference between the two statistical approaches. Meaning that in the population of women of childbearing age, BMI does not matter if it is continuous or categorical. |
| This relationship between poverty level and BMI adverse effects are documented in the literature [10-14]. Geographic location and residence can create its own unique set of health issues, including obesity [11]. There is an effect between rurality and obesity, as found in this study, as well as in previous studies [11,12]. One study found that living in rural areas is a risk factor for being overweight or obese in childhood, which may lead to being overweight or obese in adulthood [12]. In another study, an obesogenic environment exists in rural communities that encourage low physical activity and unhealthy food choices, which contributes to obesity in residents [11]. |
| The effect between obesity and rurality can be attributed to several environmental factors similar for children and adults. This may impede the ability for regular, sustained physical activity and energy expenditure. As regular physical activity decreases, sedentary behaviors, such as watching television or using a computer recreationally, increases contributing to overweight and obesity in rural localities [5,10]. In fact, rural overweight children over the age of five years in the United States were more likely than those in urban communities to use a computer for non-school related activities for more than three hours a day and watch television for more than three hours a day [5]. This study found a similar relationship between watching television, number of hours sitting daily, and obesity in the target population. Although our study was mostly conducted in rural residences, another study found that environmental factors and physical activities in women aged 18-45 did not vary according to urban or rural area of residence [18]. |
| An interesting positive relationship is seen between obesity in women with household incomes near poverty versus those at or above poverty. Food insecurity could be one explanation for this relationship [14,19]. Concern regarding availability of their next meal can lead women to be overweight or consume high-fat food. An example of this cycle can be seen in the results from a study of overweight food stamp recipients. One study found that food was abundant during the first three weeks of the month followed by a one week period of limited income and food stamps resulting in limited food [14]. Once food is restored, these individuals will be more likely to purchase highfat, energy-dense foods and, also, overeat leading to obesity-related chronic diseases [19]. Food insecurity without hunger was associated with obesity in whites, non-Hispanics; food insecurity with hunger was associated with obesity in Asians, Blacks, and Hispanics [19]. |
| Heavy alcohol drinking may also impact obesity. In a study it was found that consumption of at least one drink per month is common in the United States [20]. Additionally, it was found that those who report consuming four or more drinks per day have a 30% increased risk of being overweight and a 46% increased risk of being obese [20]. The study found further that the odds of obesity were twice as likely among women binge drinkers; however, another study found the risk of obesity among binge drinkers to be similar for both genders [21]. There are several reasons for the link between binge alcohol consumption behavior and obesity [20-22]. These include that alcohol is energy dense and often consumed along with food; also, alcohol can inhibit fat from being oxidized leading to obesity [22]. |
| There is a negative effect between obesity and sleep. The relationship between reduced sleep and obesity has been noted in several previous studies [13,23]. A study involving women of Greek descent between the ages of 30 and 60 years found that for every one hour decrease in sleep to less than seven hours, body fat increased [23]. Similar results were reported in a recent study of women aged 30-55 years indicating that sleeping less than seven hours per night greatly increased the incidence of obesity [13]. Obesity in relation to short sleep duration could be the effect of biological controls. One thought is that shorter sleep duration could alter appetite regulating hormones and/or fat metabolism resulting in increased hunger during wake periods and consumption of high energy dense food [13,23]. It could also be that less sleep time leads to greater levels of tiredness throughout the day. This could reduce the level of energy expenditure through physical activity resulting in weight gain [13]. |
| Social cognitive theory helped explain the relationship between various behaviors, environmental, and personal factors. In addition, perceived social support and use of self-regulatory behaviors were strong predictors of nutritional and physical activity behavior [9,23]. Self-efficacy was a good predictor of healthier levels of physical activity but not of fruits and vegetables [24]. The data suggest that obese women have low self-efficacy since that have significant negative results for physical activity but not fruits and vegetables. |
| The limitations of this study should be considered when interpretation of the cross-sectional study precludes conclusions about the causal and temporal nature of associations. The reliance on selfreport data may have resulted in bias. The variables that were examined were based on results from the literature and theoretical framework. Also, data collection was limited to one geographic region. However, we have no reason to believe that women in other largely rural areas would be significantly different with respect to overall health status and health risks. The use of BMI also has its limitations because it does not distinguish between muscle and fat weight and is height dependent. Future work needs to focus on attitude change procedure within the context of physical activity and diet. |
| Some of the strengths of this study are that it comprised of a large population-based study of women in a rural area, an important target group for obesity health promotion interventions. Strength was that obesity in reproductive-age women is associated with a variety of different environmental and health-related factors. These include rurality, poverty, and getting the recommended amount of sleep of 7 to 8 hours daily. It also supports previous findings of an association between pre-pregnancy obesity and adverse pregnancy outcomes [15]. This forms a basis of an outcome of interest for a prospective clinical trial on women. The future study will look at outcomes including: infertility, pregnancy complications, gestational diabetes, cardiovascular disease, preeclampsia, fetal large gestational size, and morbid postpartum outcomes [25-27]. |
| Conclusion |
| This study demonstrated that obesity is an epidemic affecting women of child bearing years. The survey dataset provides a unique regional dataset that combines multidimensional health information on obesity with reproductive outcomes, allowing classification with health correlates. The range of variables measured in the survey is not generally available in ongoing state or national surveys and is not captured in health surveillance. The data presented here provide a profile of the health status and health risks of women of reproductive age in a defined population, which is a representative sample of the Pennsylvania population. In addition, the data provide insights to guide interventions and policies to improve the health of women. |
| Acknowledgements |
| Our late colleague, Gary A. Chase, PhD, is gratefully acknowledged for his role in conceiving the idea for this manuscript as the first author’s faculty advisor. This project is funded, in part, under grant number 4100020719 with the Pennsylvania Department of Health. The Department specifically disclaims responsibility for any analyses, interpretations, or conclusions. |
References
- World Health Organization (2012) Obesity and overweight.
- Puhl RM, Heuer CA (2010) Obesity stigma: Important considerations for public health American Journal of Public Health 100: 1019-1028.
- Patterson RE, Frank LL, Kristal AR, White E (2004) A comprehensive examination of health conditions associated with obesity in older adults. Am J Preventive Medicine 27: 385-390.
- Byers T, Sedjo R (2007) Public health response to the obesity epidemic: Too soon or too late? The Journal of Nutrition137: 488-492.
- Mascie-Taylor CG, Goto R (2007) Human variation and body mass index: A review of the universality of BMI cut-offs, gender, and urban-rural differences, and secular changes. J Physiol Anthropol 26: 109-112.
- Cohen DA, Farley TA (2008) Eating as an automatic behavior. Preventing Chronic Disease 5: A23.
- Doll HA, Petersen SE, Stewart-Brown SL (2000) Obesity and physical and emotional well-being: associations between body mass index, chronic illness, and the physical and mental components of the SF-36 questionnaire. Obes Res 8: 160-170.
- Mulasi-Pokhriyal U, Smith C (2011) Investigating health and diabetes perceptions among Hmong American children, 9-18 years of age. J Immigr Minor Health13: 470-477.
- Byrd-Bredbenner C, Abbot JM, Cussler E (2011) Relationship of social cognitive theory concepts to mothers' dietary intake and BMI. Matern Child Nutr7: 241-252.
- Hu FB, Li TY, Colditz GA, Willet WC, Manson JE (2003) Television watching and other sedentary behaviors in relation to risk of obesity and type 2 diabetes mellitus in women. JAMA 289: 1785-1791.
- Boehmner TK, Lovegreen SL, Haire-Joshu D, Brownson RC (2006) What constitutes an obesogenic environment in rural communities? Am J Health Promot 20: 411-421.
- Lutifiyya MN, Lipsky MS, Wisdom-Behaunek J, Inpandutr-Martinkus M (2007) Is rural residency a risk factor for overweight and obesity for US children. Obesity 15: 2348-2356.
- Patel SR, Malhotra A, White DP, Gottlieb DJ, Hu FB (2006) Association between reduced sleep and weight gain in women. Am J Epidemiol 164: 947-954.
- Townsend MS, Peerson J, Love B, Achterbeg C, Murphy SP (2001) Food insecurity is positively related to overweight women. J Nutr 131: 1738-1745.
- Weisman CS, Hillemeier MM, Chase GA, Dyer AM, Baker SA, et al. (2006) Preconceptional health: Risks of adverse pregnancy outcomes by reproductive life stage in the Central Pennsylvania Women’s Health Study (CePAWHS). Womens Health Issues 16: 216-224.
- Morrill R, Cromartie J, Hart L (1999) Metropolitan, Urban, and Rural Commuting Areas: Toward a Better Depiction of the United States Settlement System. Urban Geography 20: 727–748.
- Pennsylvania Department of Health (2009) 2007 Behavior health risks of Pennsylvania adults. Harrisburg, PA: Bureau of Health Statistics and Research.
- Cleland VL, Ball K, King AC, Crawford D (2012) Do the individual, social, and environmental correlates of physical activity differ between urban and rural women?. Environment and Behavior 4: 350-373
- Adams EJ, Gummer-Strawn L, Chavez G (2003) Food insecurity is associated with increased risk of obesity in California women. J Nutr 133: 1070-1074.
- Arif AA, Rohrer JE (2005) Patterns of alcohol drinking and its association with obesity: data from the third national health and nutrition examination survey, 1988-1994. BMC Public Health 5: 126.
- Janssens J, Bruckers L, Joossens JV, Molenberghs G, Vinck J, et al. (2001) Overweight, obesity and beer consumption: Alcohol drinking habits in Belgium and body mass index. Archives of Public Health 59: 223-238.
- Tolstrup JS, Halkjaer J, Heitmann BL, Tjonneland AM, Overvad K, et al. (2008) Alcohol drinking frequency in relation to subsequent changes in waist circumference. Am J Clin Nutr 87: 957-963.
- Rontoyanni VG, Baic S, Cooper AR (2007) Association between nocturnal sleep duration, body fatness, and dietary intake in Greek women. Nutrition 23: 773-777.
- Anderson ES, Winett RA, Wojcik JR (2007) Self-regulation, self-efficacy, outcome expectations, and social support: social cognitive theory and nutrition behavior. Ann Behav Med 34: 304-312.
- Steinfeld JD, Valentine S, Lerer T, Ingardia CJ, Wax JR, et al. (2000) Obesity-related complications of pregnancy vary by race. J Matern Fetal Med 9:238-241.
- Samuels-Kalow ME, Funai EF, Buhimschi C, Norwitz E, Perrin M, et al. (2007) Prepregnancy body mass index, hypertensive disorders of pregnancy, and long-term maternal mortality. Am J Obstet Gynecol 197: 490.e1- 490.e6.
- Guelinckx I, Devlieger R, Beckers K, Vansant G (2008) Maternal obesity: Pregnancy complications, gestational weight gain and nutrition. Obes Rev 9: 140-150.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
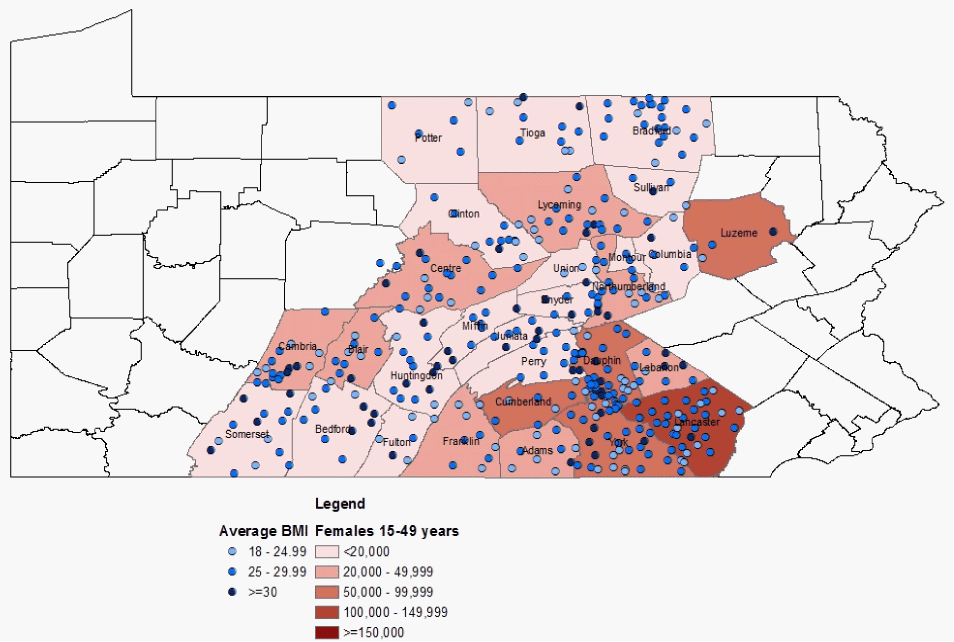 |
| Figure 1 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 14218
- [From(publication date):
January-2013 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 9617
- PDF downloads : 4601
