Research Article Open Access
Pulsed Radiofrequency Of Sympathetic Lumbar Plexus Versus Sympathetic Block In The Management Of Lower Limb Complex Regional Pain Syndrome Type 1
| Freitas TS1,2*, Fonoff ET3, Neto ORM1, Deusdará RM1, Waihrich ES1 and Kessler I1 | |
| 1Department of Neurosurgery, University Hospital of Brasília, Distrito Federal, Brazil | |
| 2Functional Neurosurgeon from Brasília Pain Institute, Brasília, Distrito Federal, Brazil | |
| 3Division of Functional Neurosurgery, Department of Neurology of School of Medicine of University of São Paulo, SP, Brazil | |
| Corresponding Author : | Tiago S. Freitas SQS 303 Bloco F Apto. 402 Asa Sul ZIP CODE: 70336-060, Brasília – DF, Brazil Tel: 55 61 84879489 Fax: 55 61 34451840 E-mail: tmosca@gmail.com |
| Received February 18, 2014; Accepted March 10, 2014; Published March 12, 2014 | |
| Citation: Freitas TS, Fonoff ET, Neto ORM, Deusdará RM, Waihrich ES, et al. (2014) Pulsed Radiofrequency of Sympathetic Lumbar Plexus versus Sympathetic Block in the Management of Lower Limb Complex Regional Pain Syndrome Type 1. J Pain Relief 3:138. doi: 10.4172/2167-0846.1000138 | |
| Copyright: © 2014 Freitas TS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Background and Objectives: Complex Regional Pain Syndrome (CRPS) type 1 is a neuropathic syndrome which most patients evolve to the necessity of interventional procedures to treat their pain. Our objective was to compare two safe options (pulsed radiofrequency (PRF) or sympathetic blocks) and their efficiency in the treatment of this neuropathic pain and in the quality of life of patients.
Methods: 40 randomized patients received PRF or sympathetic blocks in lower limb CRPS type 1. They were evaluated with VAS scores, neuropathic pain scale and RAND SF-36 scale in a follow up of 1 day, 7 days, 2-4 and 6 months.
Results: There were similar reductions from the baseline in various pain scores after the procedures. In the PRF group these results were statistically significant superior to the blockade group related to burning pain. The other parameters and RAND SF-36 had similar results.
Conclusions: PRF appears as a technique with similar results in the treatment of lower limb CRPS type 1, compared with the sympathetic block. Only one pain outcome (hot pain) was statistically significant and this difference was insignificant to the final result. Since it is a higher-cost procedure with too few benefits, this difference did not affect the quality of life (RAND SF-36).
| Keywords |
| CRPS type 1; Pulsed radiofrequency; Sympathetic lumbar block |
| Introduction |
| Pain related to complex regional pain syndrome (CRPS) type 1 is frequently resistant to medical, physical, and alternative treatments [1]. Interventional and minimally invasive procedures are often needed to complement the alleviation of persistent pain [2]. Sympathetic blocks are the most commonly used procedures and are performed using local anesthetic agents, and occasionally, clonidine. However, the blocks usually only have a transient effect and repetition of the procedure is often required for a more prolonged effect. Other procedures involving the sympathetic lumbar plexus (e.g., mechanical sympathectomy, radiofrequency, or phenolization) have been tried, but despite their apparent better efficacy, they are associated with a higher risk of dysesthesia, hyperesthesias, and differentiation pain. |
| Pulsed radiofrequency (pRF) has become increasingly popular for the treatment of neuropathic pain because of its minimally destructive nature and possible neuromodulatory mechanism [3,4]. It has been presented in clinical practice as a safer alternative to traditional radiofrequency coagulation [5,6]. pRF exposes a target neural structure to high-frequency electromagnetic oscillations (300–500 kHz) for very brief intervals (20 ms) followed by a silent period (480 ms) to allow for heat dissipation. The electrode tip does not exceed 42°C. This modality of radiofrequency may induce changes in the activity of neural circuits that mediate pain states [7,8]. Changes in C-fos expression at the level of the dorsal horn may result in less central excitation from afferent C fibers. This corroborates the alleviation of pain reported by clinicians over more than a decade after their successful treatment of various neuropathic pain states using such an approach [5,6,9]. |
| The present prospective, randomized study used rigorous inclusion and exclusion criteria to evaluate subjects with lower limb CRPS type 1 with clinical signs/symptoms of sympathetic involvement. The study aimed to determine whether percutaneous pRF applied directly to the sympathetic lumbar plexus was more effective than lumbar sympathetic blocks, and, if so, whether this could be achieved without the risks associated with traditional ablative procedures. |
| Methods |
| Patients who satisfied the diagnostic criteria for CRPS suggested by Bruehl et al. [10] were included in the study. These included symptoms lasting for more than 6 months despite management in a multidisciplinary setting, that is, symptoms that were unresponsive to medications such as oral gabapentin 2400 mg/d, oral amitryptiline 100 mg/d, and oral carbamazepine 1000 mg/d and physiotherapy for more than 6 months (visual analog scale [VAS] score >6 on a scale of 1–10). Exclusion criteria included patients who were not willing to participate, who were allergic to local anesthetic, and those who had bleeding diathesis or local infection. To avoid possible confounding, patients with psychiatric disorders, known drug or alcohol abuse, diabetes mellitus, post-herpetic neuralgia, peripheral neuropathy, pending litigation in any court of law, those who had undergone more than 1 surgical procedure for the same complaint, and those with other known causes of pain (lumbar spondylosis, cord compression) were excluded from the study. |
| Patient selection |
| After providing their written informed consent, 40 patients with lower limb CRPS type 1 who met the above-mentioned criteria were enrolled in the study. The patients were instructed on the use of the VAS score and neuropathic pain scale [11,12]. The study was approved by the local Investigational Review Board. |
| Randomization and blinding |
| Patients were randomized to either pRF or sympathetic lumbar block according to computer-generated random numbers. They were blinded to the procedure as similar scenarios were used for both groups. The investigator involved in data collection was not involved in the performance of the procedures and was unaware of the group to which the patients had been assigned. Baseline VAS, neuropathic pain scale, and SF-36 scale scores were recorded before the procedure. |
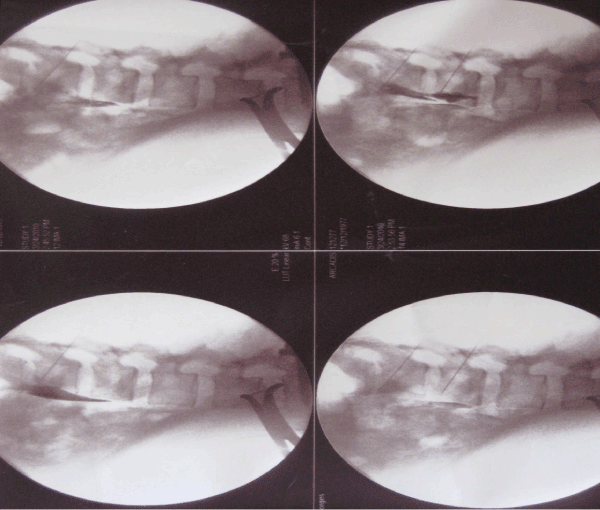
| All patients were reassessed at 24 h; on day 7; and at 2, 4, and 6 months after the procedure. All procedures were performed with the patients in a prone position. pRF was performed using a radiofrequency lesion generator (Smith-Nephew, USA) and aseptic techniques. A sterile, disposable radiofrequency cannula (150-mm long, 10-mm active tip) was introduced 5-cm lateral to the spinous processes of the L2-L3 and L3-L4 vertebral bodies under the guidance of a C-arm with an image intensifier. The position of the needle tip was checked by radiograph using anteroposterior (AP) and lateral views with the needle perpendicular to the sympathetic chain in order to have effect. The location of the needle tip was identified after the injection of 0.5–1 mL of ionic radio contrast media (Urograffin 75%, Schering, Germany) (Figure 1). Negative aspirations for blood and cerebrospinal fluid were noted. Electrical stimulation was performed at 50 Hz and 5 Hz to identify proximity to sensory and motor nerves, respectively. Thereafter, 1 mL of 2% lidocaine was injected at each level before pRF, which was performed over 3 cycles (120 s/cycle at each level at a temperature of 42°C). The generator was set at a target voltage of 45 V with a pulse width (PW) of 20 ms and a pulse rate of 2 Hz; the generator automatically adjusted these parameters to maintain a temperature at or below 42°C. |
| In patients randomized to the sympathetic block, a radiofrequency cannula (150-mm long, 10-mm active tip) was placed approximately 5-cm lateral to the spinous processes of the L2-L3 and L3-L4 vertebral bodies under fluoroscopic guidance (AP and lateral views). The needle position was confirmed in a similar manner to the radiofrequency group with electrical stimulation at 50 Hz and 5 Hz followed by the injection of 15-mL lidocaine 2% plus clonidine 100 mcg at each level. The patients were maintained in a prone position with the needle in situ for 30 min to help decrease the posterior spread of the solutions into the psoas muscles. All patients were admitted to the ward for 24 h of monitoring. |
| Statistical analysis |
| We analyzed 11 pain outcomes (VAS score, pain intensity, sharp pain, hot pain, dull pain, cold pain, sensitive sensation, unpleasant sensation, itchy pain, deep pain, and surface pain), each of which was scored on a scale of 0–10 at baseline and at 24 h; 7 days; and at 2, 4, and 6-monthly follow-ups. In order to compare the 2 groups (blocking and pRF), we calculated the difference between baseline and final pain scores for each patient. After the creation of the new variable, we performed a nonparametric Mann–Whitney test to check for significant differences between the 2 independent groups. Analyses were performed using R software version 2.13.1 (Statistics Department of the University of Auckland, New Zealand). The level of significance was set at 5%. |
| Results |
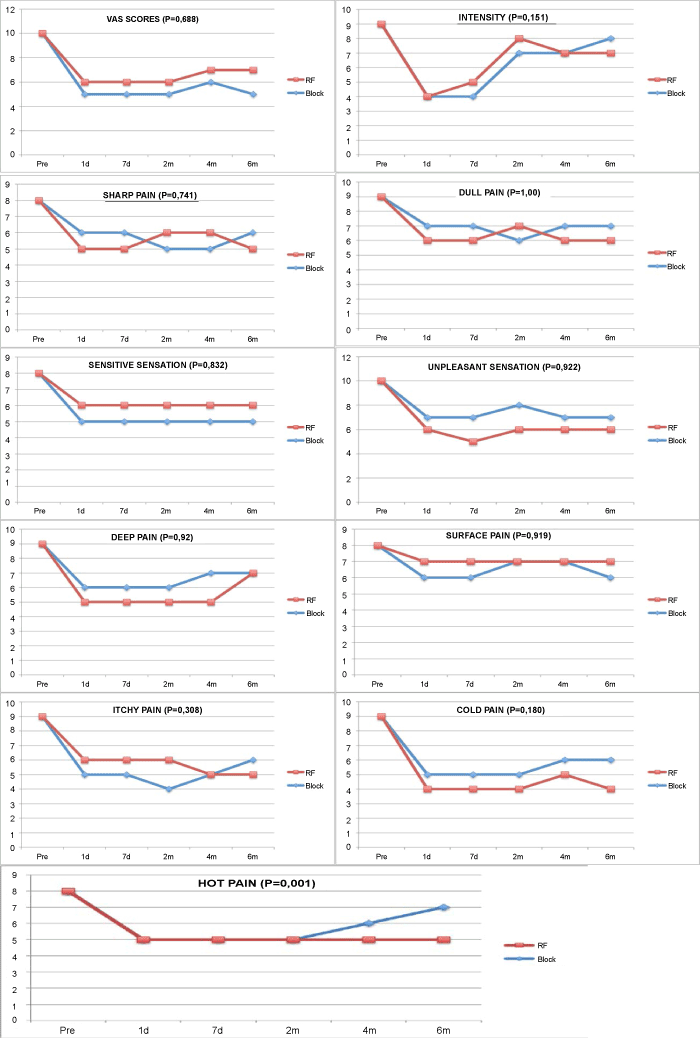
| All patients except for 1 in the radiofrequency group were followed up until the completion of the study (Figure 2). |
| Pain scores in both groups showed similar statistically significantly reductions from baseline after the procedures were performed. In this sense, almost all topics of neuropathic pain scale (pain intensity, sharp pain, dull pain, cold pain, sensitive sensation, unpleasant sensation, itchy pain, deep pain, and surface pain) obtained a reduction that was not statistically significant in both groups of patients. However, in the pRF group, these results were statistically more consistent over the follow-up period for the hot-sensation type of neuropathic pain (P = 0.001) (Figure 2). |
| The Rand-SF 36 did not reveal any statistically significant betweengroup differences for all parameters (Tables 1 and 2). |
| None of the patients had post-sympathectomy neuralgia. Two patients in the radiofrequency group (2 of 10) and 1 in the sympathetic block group (1 of 10) complained of paresthesia during needle positioning. There was no evidence of nerve injury during follow-up in any of the patients. All patients complained of soreness at the site of injection, which lasted for 5–7 days. |
| Discussion |
| CRPS type 1, which was formerly known as “reflex sympathetic dystrophy,” is a pain syndrome that has an unclear pathophysiology and an unpredictable clinical course. Current guidelines recommend interdisciplinary management emphasizing 3 core treatment elements: pain management, rehabilitation, and psychological therapy. Pain management must start immediately in every probable CRPS type 1 case with the aim of treating the pain and restoring function. Pharmacological pain management and physical rehabilitation of limb function are the main pillars of pain therapy. However, if there is no improvement in limb function and persistent severe pain, the following interventional pain management techniques may be considered: nerve blockade, sympathetic block, spinal cord and peripheral nerve stimulation, implantable spinal medication pumps, and sympathectomy [1,2,13]. |
| Radiofrequency procedures are minimally invasive techniques that have demonstrated success in reducing pain in several chronic pain conditions, including chronic cervical pain, lower back pain, and trigeminal neuralgia [14]. However, the use of conventional radiofrequency in the management of neuropathic pain occasionally leads to worsening and even new onset of neuropathic pain. pRF is a minimally/non-destructive procedure that offers a new opportunity and perspective for radiofrequency therapy. In this interventional procedure, short bursts of radiofrequency energy are applied to nervous tissue in a non-neurodestructive procedure that is an alternative to conventional radiofrequency heat lesions [15]. |
| As mentioned above, the mechanism of action of pRF has not been completely elucidated, and laboratory reports suggest a genuine neurobiological phenomenon altering pain signaling [7,8], which some have described as neuromodulatory. In addition, the clinical effect of this technique is not fully proven and thus further research into its clinical and biological effects is justified. |
| This randomized study was performed with the intention of analyzing the clinical efficacy of pRF for this specific type of neuropathic pain (lower limb CRPS type 1). Statistical limitations of the study include the small number of patients enrolled. To detect a difference of 1.0 scale points between groups with 80% power at the 5% significance level a future trial will need to be performed with 80 patients. |
| Conclusion |
| On the basis of this pilot study, pRF appears to have similar efficacy in the treatment of neuropathic pain in patients with lower limb CRPS type 1 as sympathetic blocks. Only 1 pain outcome (hot pain) was statistically significantly different between the 2 procedures, and we consider this difference to not have had a significant effect on the final outcome. Since pRF is a more costly procedure with few benefits, this particular difference regarding hot pain did not affect quality of life as measured by the SF-36. |
References
- Stanton-Hicks MD, Burton AW, Bruehl SP,Carr DB, Harden RN, et al. (2002) An updated interdisciplinary clinical pathway for CRPS: Report of an expert panel. Pain Pract2:1-16.
- Van Eijs F, Stanton-Hicks M, Van Zundert J,Faber CG, Lubenow TR, et al. (2011) Evidence-based interventional pain medicine according to clinical diagnoses. 16. Complex regional pain syndrome.Pain Pract11:70-87.
- Ramanavarapu V, Simopoulos TT (2008) Pulsed radiofrequency of lumbar dorsal root ganglia for chronic post-amputation stump pain. Pain Physician 11:561-566.
- Van Zundert J, Lame IE, de Louw A,Jansen J, Kessels F, at al. (2003) Percutaneous pulsed radiofrequency treatment of the cervical dorsal root ganglion in the treatment of chronic cervical pain syndromes: A clinical audit. Neuromodulation6:6-14.
- Chao SC, Lee HT, Kao TH,Yang MY, Tsuei YS, et al. (2008) Percutaneous pulsed radiofrequency in the treatment of cervical and lumbar radicular pain. SurgNeurol70:59-65.
- Hussain AM, Afshan G (2007) Use of pulsed radiofrequency in failed back surgery syndrome. J Coll Physicians Surg Pak17:353-355.
- Erdine S, Yucel A, Cimen A, Aydin S, Sav A, et al. (2005) Effects of pulsed versus conventional radiofrequency current on rabbit dorsal root ganglion morphology. Eur J Pain9:251-256.
- Van Zundert J, de Louw AJ, Joosten EA, Kessels AG, Honig W, et al. (2005) Pulsed and continuous radiofrequency current adjacent to the cervical dorsal root ganglion of the rat induces late cellular activity in the dorsal horn. Anesthesiology102:125-131.
- Rozen D, Parvez U (2006) Pulsed radiofrequency of lumbar nerve roots for treatment of chronic inguinal herniorraphy pain. Pain Physician9:153-156.
- Bruehl S, Harden RN, Galer BS, Saltz S, Bertram M, et al. (1999) External validation of IASP diagnostic criteria for Complex Regional Pain Syndrome and proposed research diagnostic criteria. International Association for the Study of Pain. Pain 81:147-154.
- Benzon HT (2005)The neuropathic pain scales. RegAnesth Pain Med30:417-421.
- Galer BS, Jensen MP (1997) Development and preliminary validation of a pain measure specific to neuropathic pain: the Neuropathic Pain Scale. Neurology 48:332-338.
- Hsu ES (2009) Practical management of complex regional pain syndrome. Am J Ther16:147-154.
- Racz GB, Ruiz-Lopez R (2006) Radiofrequency procedures. Pain Pract6:46-50.
- Cahana A, Van Zundert J, Macrea L, van Kleef M, Sluijter M (2006) Pulsed radiofrequency: current clinical and biological literature available. Pain Med7:411-423.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 15457
- [From(publication date):
April-2014 - Aug 16, 2025] - Breakdown by view type
- HTML page views : 10799
- PDF downloads : 4658
