Research Article Open Access
Relationship among Analgesic Effects, Radiating Pain, and Radiological Contrast Material Distribution in Lumbosacral Selective Nerve Root Block
| Satoko Chiba*, Sayako Tsutsui, Tomofumi Chiba, Hidekazu Watanabe, Noriko Takiguchi, Yuhei Ishikawa, Tomoko Kitamura and Hisashi Date | |
| Sendai Pain Clinic Center, Sendai, Miyagi, Japan | |
| Corresponding Author : | Satoko Chiba Sendai Pain Clinic Center 3-4-11,Shindenhigashi Miyagino-ku Sendai Miyagi, 983-0039, Japan Tel: +81-22-236-1310 Fax: +81-22-236-1315 E-mail: sato33150@ktj.biglobe.ne.jp |
| ReceivedJuly 04, 2014; Accepted October 07, 2014; Published October 10,2014 | |
| Citation: Chiba S, Tsutsui S, Chiba T, Watanabe H, Takiguchi N, et al. (2014) Relationship among Analgesic Effects, Radiating Pain, and Radiological Contrast Material Distribution in Lumbosacral Selective Nerve Root Block. J Pain Relief 3:157. doi: 10.4172/2167-0846.1000157 | |
| Copyright: 2014 Chiba S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Objectives: We aimed to determine the correlation of radiographic contrast material distribution with selective lumbosacral nerve root block (SLNRB)-induced radiating pain and pain reduction obtained 3 ± 1 hours after SLNRB.
Patients were stratified according to the distribution of contrast material: those in whom nerve fibres were visualised (type 1), those in whom the nerve sheath was visualised (type 2), and those in whom contrast material was distributed around the nerves (type 3).
Materials and methods: The study population comprised 111 patients who had undergonefluoroscopic SLNRB for pain presumed to be arising from lumbar intervertebral disc displacement. Using a numerical rating scale (the scale is an 11 point scale 0=no pain, 10=worst pain possible), patients evaluated pain intensity before and immediately after SLNRB, 3 ± 1 hours after SLNRB, and SLNRB-induced radiating pain.
Results: Median pain score decreased by 2.5, 3.0, and 3.0 in types 1, 2, and 3, respectively, at 3 ± 1 hours after SLNRB, showing no significant intergroup differences. Median radiating pain scores at the time of SLNRB were 9.5, 9.0, and 6.0 in types 1, 2, and 3, respectively, with significant intergroup differences. Most notably, the radiating pain score was significantly greater in types 1 and 2 than in type 3 (P=0.002 and P=0.01, respectively), though there was no significant difference between types 1 and 2.
Discussion: The analgesic effect of SLNRB was similar regardless of radiographic findings and radiating pain intensity, suggesting that severe radiating pain at the time of SLNRB, or contrast distribution types 1 and 2, is not required for SLNRB.
| Keywords |
| Contrast media, Intervertebral disc displacement, Spinal nerve root, Nerve block, Pain |
| Introduction |
| Selective lumbar nerve root blocks (SLNRBs) were reported to be useful in the diagnosis of radiculopathy by Macnab and colleagues (1971) [1]. Furthermore, SLNRB has been found to be effective for the treatment of spinal pain and radiculopathy, and is commonly employed both in the diagnosis and treatment of spinal pain and radiculopathy [2-4]. However, an understanding of the mechanism by which SLNRB achieves analgesia in spinal pain and radiculopathy remains largely unclear. Pfirrmann and colleagues (2001) previously reported that there was no relationship among needle-tip positions, radiating pain, and analgesic effect after comparing the fluoroscopic contrast material distribution, radiating pain, and analgesic effect of SLNRB in combination with steroids. The authors proposed a “safe triangle,” composed of the inferior border of the pedicle, the lateral border of the vertebral body, and the superior border of the nerve root, as the best site for maximising the analgesic effect of SLNRB for the treatment of lumbosacral radicular pain. According to them, SLNRB at this site elicits sufficient analgesia without eliciting radiating pain [5]. This suggests that there is no relationship between the occurrence of radiating pain and the analgesic effect after SLNRB, and that it is not necessary to inject the local anaesthetic agent into the nerve fibres. However, in their study, it is questionable whether the analgesic effect is mainly due to the action of the SLNRB, because of inadequate time to measure the analgesia at 15 minutes and 2 weeks after the SLNRBs. The analgesic effects at 15 minutes and 2 weeks seem to be mainly due to a direct effect of the local anaesthetic agent and to an anti-inflammatory effect of the steroid administered concomitantly, respectively. |
| In the present study, we chose to measure analgesia at 3 ± 1 hours after SLNRB to exclude the possibility of a direct anaesthetic effect and/or anti-inflammatory effect. We sought to focus on the existence of any causative relationships among needle-tip position, radiating pain, and analgesic effect by comparing fluoroscopic contrast material distribution, radiating pain, and the analgesic effect of SLNRB during treatment for pain presumed to be arising from lumbar intervertebral displacement. |
| Materials and Methods |
| Consent to ethical guidelines and license |
| The protocol of this study was approved by the ethical review committee of our hospital and registered in the UMIN Clinical Trials Registry (Registration No. UMIN000010558). Written informed consent was obtained from all patients prior to participation in the study. |
| Materials |
| The study population consisted of adult patients who were diagnosed with lumbar intervertebral disc displacement on the basis of physical findings, symptoms, and imaging findings such as magnetic resonance imaging data during the period from February 2011 to October 2012, and underwent SLNRB. The present study was restricted to subjects with intervertebral disc displacement, because the therapeutic efficacy of SLNRB varies by disease included [6-10]. Patients in whom the nerve root causing pain was not clarified and patients of multiple radiculopathy were also included. Skin sensory perception was measured on the area supplied by each nerve root before and immediately after SLNRB. Patients with decreased skin sensation after SLNRB were selected as those in whom SLNRB was performed successfully. Patients in whom pain reduced immediately after SLNRB were selected as those in whom the SNLRB had been applied to the nerve root causing pain. From among the selected patients, only those who had received a 0.5 ml injection of the contrast material were selected. Finally 111 adult cases were selected for this study. |
| We excluded patients undergoing spinal surgery and those with communication difficulties, cauda equina syndrome, hypersensitivity to local anesthetic agents or steroids, and comorbidities such as systemic inflammatory disease, blood coagulation disorders, poorly controlled diabetes mellitus, psychiatric disorders, malignant disease, heart disease, and skin problems at the puncture site. |
| Study implementation |
| All SLNRBs were performed on an in-hospital basis by anesthesiologists and orthopedic surgeons (in total, 7) at the Sendai Pain Clinic Center. All the procedures were performed under X-ray fluoroscopic guidance, with the patient in an oblique or prone position. After skin disinfection, a local anesthetic agent (1% mepivacaine) was injected with a 25-gauge needle. |
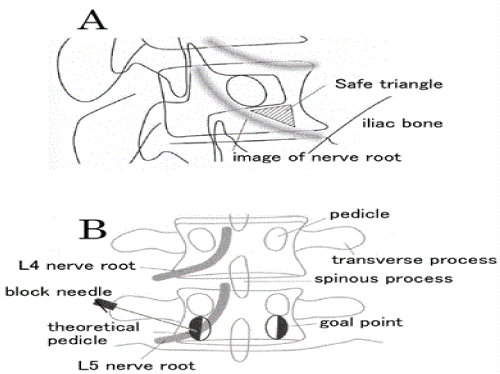
| Oblique position: The end plate of the target vertebral body was aligned under X-ray fluoroscopy in a completely prone position. In the lumbar spine, the positional relation between the superior articular process of the caudal vertebral body and the target vertebral body was aligned while rotating an X-ray tube to obtain the fluoroscopic image (Figure 1a). The dorsal sacral foramen was localized in the sacral spine. A 12-cm, 22-gauge block needle was advanced incrementally anterior to the caudal superior articular process, caudal to the pedicle of the vertebral arch, cranial to the inferior border of the vertebral body in the lumbar spine, and toward the dorsal sacral foramen in the sacral spine. |
| Prone position: The patient was placed in a completely prone position, so that the spinous processes would be at the centre of the superior vertebral body on the X-ray fluoroscopic image. The X-ray tube was rotated toward the cranial direction, so that the target end plate would be on the straight line joining the end plate (Figure 1b). A block needle was inserted in the direction of the transverse process base in the lumbar spine and in the direction of the inferior border of the dorsal sacral foramen in the sacral spine. Then, the block needle was slightly retracted and then advanced as if it was sliding along the inferior border of the transverse process in the lumbar spine. Assuming that there was another virtual pedicle of vertebral arch caudal to the actual pedicle of vertebral arch, the needle was inserted to the lateral half (Figure 1b). In the sacral spine, the needle was advanced to the central side of the dorsal sacral foramen. |
| In both techniques, insertion of the needle was stopped when radiating pain was induced, a non-ionic contrast material (iohexol for the spinal cord) was injected at a dose of 0.5 ml, and the contrastenhanced nerve root was identified. |
| Thereafter, 1 ml of 2% mepivacaine and 1 ml of dexamethasone 3.3 mg (in total, 2 ml) were injected. In general, ≤0.5 ml of anaesthetic agent is injected for diagnostic SLNRB,6 11 and 1.5–2.5 ml is injected for therapeutic SLNRB.12 13 In the present study, we used a total of 2 ml of anaesthetic agents (1 ml of 2% mepivacaine and 1 ml of dexamethasone 3.3 mg). |
| The distribution of radiographic contrast material was classified into one of three types according to Pfirrmann’s classification.5 |
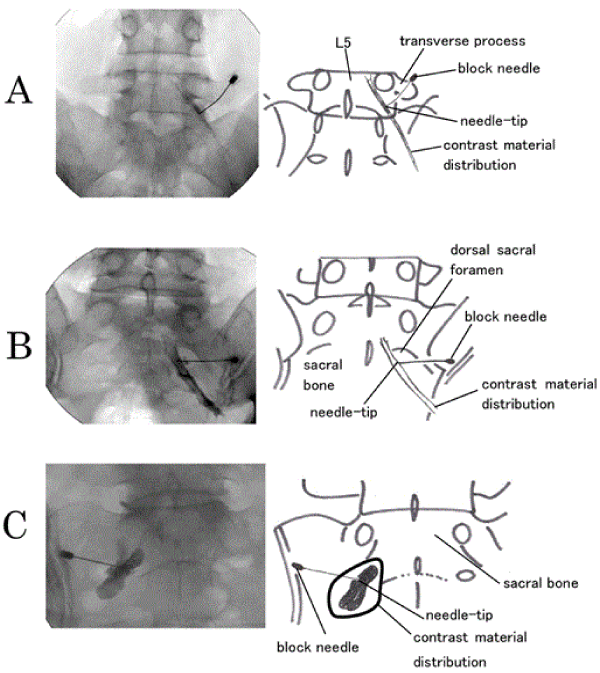
| 1) Type 1, intraneural pattern: The outer border of the nerve root was visualised in a tube form and the inner nerve fibres were visualised in a feather-like pattern. (Figure 2a, Right L5 nerve root) |
| 2) Type 2, extraneural pattern: The nerve root was visualised as a filling defect. There was a clear border between the nerve root and the contrast material. (Figure 2b, Right S1 nerve root) |
| 3) Type 3, paraneural pattern: The contrast material was distributed around the nerve root in a cloud-like appearance. The border between the nerve root and the contrast material was not clearly visualised. (Figure 2c, Left S1 nerve root) |
| Using 0.5 ml or more contrast agent, the contrast agent will leak out of a nerve sheath, to become the imaging findings type 3 all, so the amount of contrast agent was adopted 0.5 ml. |
| Pain intensity was reported by patients using an 11-point numerical rating scale (NRS; 0 = no pain to 10 = worst possible pain). Pain was evaluated three times, namely, before and immediately after SLNRB and at 3 ± 1 hours after SLNRB. The degree of pain reduction was calculated by subtracting the NRS score at the time of 3 ± 1 hours after SLNRB from the baseline NRS score obtained before SLNRB. The intensity of radiating pain at the time of the SLNRB was also determined using an 11-point NRS |
| To account for individual differences in dermatome distribution, 14 skin sensory perception was measured on the area innervated by each nerve root immediately before and after SLNRB. Sensitivity was quantified using an 11-point NRS (0 = no sense of touch to 10 = normal sense of touch). |
| Statistical analysis |
| Background values were compared among groups by using the Kruskal-Wallis test. Pre-SLNRB and post-SLNRB pain intensity in all subjects were compared by using the Mann-Whitney U test. The intensity of radiating pain and the degree of pain reduction were compared among groups by using the Kruskal-Wallis test. A P value less than 0.05 was considered significant. When the Kruskal-Wallis test showed significant differences among the groups, Mann-Whitney U test was employed for comparison |
| Results |
| Background |
| Among 111 cases in total, according to the pattern of radiographic contrast material distribution, 39 patients (17 women, 22 men) were classified as type 1, 37 (19 women, 18 men) as type 2, and 35 (16 women, 19 men) as type 3. Table 1 provides the background characteristics for this study population. There were no significant differences in age or sex distribution among the groups. |
| The effect |
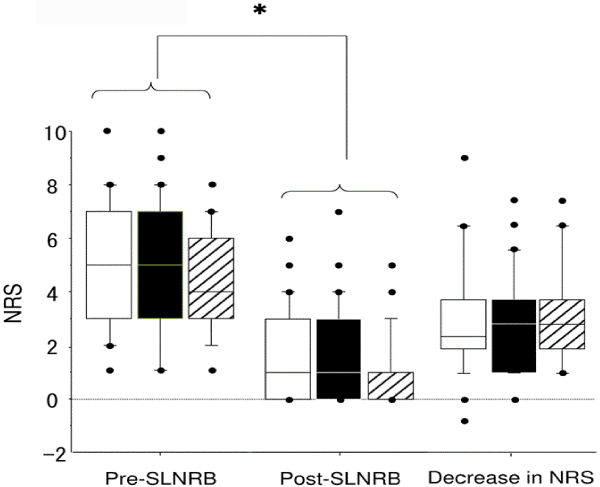
| The effect of SLNRB was evaluated differently based on the radiographic contrast material distribution pattern by classifying the patients as type 1, 2, or 3. The degree of pain reduction was determined 3 ± 1 hours after SLNRB. Overall, median NRS scores decreased from 5 before SLNRB to 1 after SLNRB, showing a significant reduction in pain after SLNRB (Figure 3). When examined according to the distribution of radiographic contrast material, median NRS scores decreased from 5 to 1 for type 1, 5 to 1 for type 2, and 4 to 0 for type 3, showing no significant intergroup differences before or after SLNRB. That is, pain associated with types 1, 2, and 3 decreased by 2.5, 3.0, and 3.0, respectively, after SLNRB, showing no significant intergroup differences (H value=0.144, P = 0.45, degrees of freedom=2) (Figure 3). |
| Radiating pain |
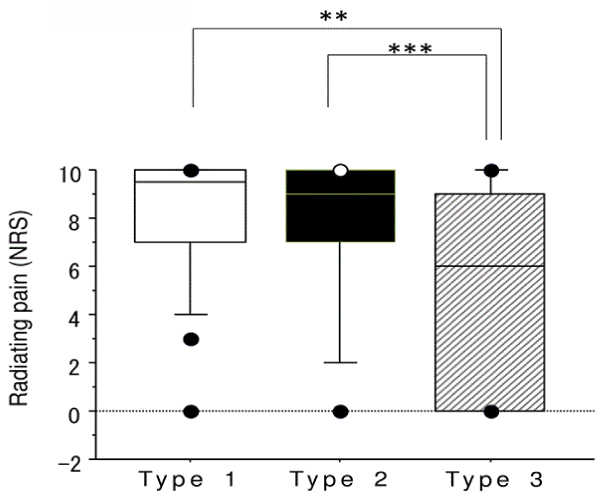
| The intensity of SLNRB-induced radiating pain was also compared among the three groups. The median intensity of radiating pain in types 1, 2, and 3 was 9.5, 9.0, and 6.0, respectively, showing a significant intergroup difference (H value=10.65, P = 0.005, degrees of freedom=2). Radiating pain was significantly more severe in types 1 and 2 as compared with type 3 (U value=407.0, P = 0.002 and U value=433.0, P = 0.01, respectively) (Figure 4), though pain intensity did not differ between types 1 and 2 (U value=658.5, P = 0.5). |
| Discussion |
| Pfirrmann et al. performed SLNRB in combination with steroids [5] We utilise this approach at our clinic because steroids with SLNRB has been reported to be useful in medium term [11-19] As for the analgesic mechanism of SLNRB in combination with steroids, local anaesthetic agents improve blood flow19 and steroids have an antiinflammatory effect [20-22]. In general, the duration of action of local anaesthetic agents is short. The duration of action of conduction anesthesia with mepivacaine to the little finger has been reported to be 46.6 minutes [23] Furthermore, the duration of action of the epidural anesthesia with mepivacaine reported to be 149 minutes even though in the presence of epinephrine, [24] which is well known for extent the duration of action of the epiduralanesthesia. Therefore, the effect of mepivacaine used to SLNRB would disappear within about 2 hours in the absence of epinephrine. On the other hand, the clinical effect of steroids appears to be 1–7 days after administration [25] It is well known that steroid exerts anti-inflammatory effects regardless of the route of administration [18,22,26]. As Pfirrmann et al. evaluated the analgesic effect at 15 minutes and 2 weeks after SLNRB,5 it is highly likely that a direct analgesic effect of a local anesthetic agent may have been maintained until 15 minutes after SLNRB, while the antiinflammatory action of steroids may have appeared in 2 weeks after SLNRB. Moreover, 2 weeks may have been sufficient time for patients to have responded well to other treatment modalities such as oral medications and physical therapy. The analgesic effect of SLNRB itself should be elucidated by evaluating the reduction in pain during the period when neither local anesthetic agents nor steroids, regardless of the route of administration, [18,22,26] are effective. The analgesic effect at 3 ± 1 hours after SLNRB, appears to be independent of the direct analgesic effect of the anaesthetic agent mepivacaine and the anti-inflammatory effects of steroids. Therefore, we estimated the pain 3 ± 1 hours after SLNRB. |
| As shown in Figure 3, the reduction in pain obtained by SLNRB did not differ among the three groups, that is, it did not vary depending on the distribution of radiographic contrast material. However, radiating pain was significantly more severe in types 1 and 2 than in type 3 (Figure 4). Nerve fibres were visualised in type 1 (Figure 2a), the pattern considered to be closest to the nerve root. The inner side of the nerve sheath was visualised in type 2 (Figure 2b), suggesting distance to the nerve root just greater than that of type 1. In type 3, the outer side of the nerve sheath was visualised (Figure 2c), which did not allow for conclusions regarding distance to the nerve root. Notably, radiating pain grows more severe as distance to the nerve root decreases. In the type 1 distribution, as well as in the type 2, intensity of radiating pain was significantly more severe than in the type 3. Remarkably, the degree of pain reduction was similar regardless of contrast material distribution, suggesting that therapeutic SLNRB can be performed without intense radiating pain. |
| SLNRB can be effective without inducing radiating pain, when performed by advancing the needle-tip to the region of the safe triangle (Figure 1a) [27,28] , because a SLNRB pointed toward the region of the safe triangle induces no radiating pain, the burden imposed on patients is reduced. However, it is difficult to confirm whether the needle-tip has been advanced to the target site; in addition, radiating pain can occur even when the needle-tip has been advanced toward the region of the safe triangle. In the present study, the SLNRB was not targeted toward the safe triangle, but rather demarcated by inducing conventional radiating pain. When radiating pain is induced by SLNRB, complications such as nerve damage may occur in very low case [29]. Recently, paraplegia and other problems have been reported to result from SLNRB targeted toward the region of the safe triangle [30-32] A new site has recently been proposed for needle-tip insertion, so as to replace the safe triangle without inducing radiating pain [33,34 ]The ability to achieve SLNRB without inducing radiating pain would offer great benefits to patients. Further studies are necessary to identify alternative injection sites to replace the use of the safe triangle. |
| This study has several limitations. First, there was no threshold of NRS scores before SLNRB. Lower NRS scores before SLNRB were associated with less pain reduction; this may have led to data bias and discrepancies. In the present study, however, median NRS values before SLNRB did not differ significantly among the three groups; we therefore consider that the analysis was not affected. Second, the duration of intervertebral disk herniation was not investigated. When patients suffer over longer periods of time, physiopathologic changes can occur, which in turn affects the manifestation of SLNRB [35]. In the present study, there were no significant differences in the degree of pain reduction among the three groups. This may imply that the duration of disease did not vary among the groups. Further research is required to determine the relationship between disease duration and the therapeutic effect of SLNRB. Third, SLNRB was performed with the patient in either an oblique or prone position. There are minimal differences in needle-tip position and needle angle on X-ray frontal and lateral views between the two patient positions. Thus, the analgesic effect of SLNRB is likely to be independent of patient position. |
| In conclusion, the results of this study verified the analgesic effect of SLNRB for three typical patterns of radiographic contrast material distribution. There was no significant difference in analgesia among the three groups, but the intensity of radiating pain at the time of SLNRB was more severe in types 1 and 2 than in type 3. It is presumed that the analgesic effect of therapeutic SLNRB would be similar regardless of contrast material distribution type and the intensity of radiating pain, indicating that neither severe radiating pain, nor contrast material distribution type 1 or 2, is required for the implementation of therapeutic SLNRB. |
| Acknowledgements |
| H. Date, H. Watanabe and T. Chiba conceived the idea for the present study. S. Tsutsui, S. Chiba, H. Watanabe, T. Chiba and H. Date contributed the experimental study design. All authors including N. Takiguchi, Y. Ishikawa and T. Kitamura examined the patients and collected the data serving for the present study. H. Date and S. Chiba wrote the manuscript after analyzing the data from all authors. |
| This work was supported only by institutional funding. |
References
- Macnab I (1971) Negative disc exploration. An analysis of the causes of nerve-root involvement in sixty-eight patients. J Bone Joint Surg Am 53: 891-903.
- Nocom G, Ho KY, Perumal M (2009) Interventional management of chronic pain. Ann Acad Med Singapore 38: 150-155.
- DePalmaMJ ,Bhargava A, Slipman CW (2005) A critical appraisal of the evidence for selective nerve root injection in the treatment of lumbosacral radiculopathy. Arch Phys Med Rehabil 86: 1477-1483.
- Galloway HR (2003) Image-guided spinal injection for diagnosis and therapy. AustralasRadiol 47: 219-225.
- Pfirrmann CW, Oberholzer PA, Zanetti M, Boos N, Trudell DJ (2001) Selective nerve root blocks for the treatment of sciatica: evaluation of injection site and effectiveness--a study with patients and cadavers. Radiology 221: 704-711.
- Manchikanti L, Buenaventura RM, Manchikanti KN, Ruan X, Gupta S (2012) Effectiveness of therapeutic lumbar transforaminal epidural steroid injections in managing lumbar spinal pain. Pain Physician 15: E199-245.
- Manchikanti L, Boswell MV, Datta S, Fellows B, Abdi S (2009) Comprehensive review of therapeutic interventions in managing chronic spinal pain. Pain Physician 12: 123-198.
- Slipman CW, Chow DW (2002) Therapeutic spinal corticosteroid injections for the management of radiculopathies. Phys Med RehabilClin N Am 13: 697-711.
- Peterson C, Hodler J (2010) Evidence-based radiology (part 1): Is there sufficient research to support the use of therapeutic injections for the spine and sacroiliac joints? Skeletal Radiol 39: 5-9.
- Narozny M, Zanetti M, Boos N (2001) Therapeutic efficacy of selective nerve root blocks in the treatment of lumbar radicular leg pain. Swiss Med Wkly 131: 75-80.
- Castro WH, Grönemeyer D, Jerosch J, Seibel R, Lorenz G, et al. (1994) How reliable is lumbar nerve root sheath infiltration? Eur Spine J 3: 255-257.
- Blankenbaker DG , Davis KW, Choi JJ (2004) Selective nerve root blocks. SeminRoentgenol 39: 24-36.
- Wagner AL, Murtagh FR (2002) Selective nerve root blocks. Tech VascIntervRadiol 5: 194-200.
- Wolff AP, Groen GJ, Crul BJ (2001) Diagnostic lumbosacral segmental nerve blocks with local anesthetics: a prospective double-blind study on the variability and interpretation of segmental effects. RegAnesth Pain Med 26: 147-155.
- Gharibo CG, Varlotta GP, Rhame EE, Liu EC, Bendo JA (2011) Interlaminar versus transforaminal epidural steroids for the treatment of subacute lumbar radicular pain: A randomized, blinded, prospective outcome study. Pain Physician 14: 499-511
- Rados I, Sakic K, Fingler M, Kapural L (2011) Efficacy of interlaminarvstransforaminal epidural steroid injection for the treatment of chronic unilateral radicular pain: prospective, randomized study. Pain Med 12: 1316-1321.
- Benny B, Azari P (2011) The efficacy of lumbosacral transforaminal epidural steroid injections: a comprehensive literature review. J Back MusculoskeletRehabil 24: 67-76.
- Ghahreman A, Ferch R, Bogduk N (2010) The efficacy of transforaminal injection of steroids for the treatment of lumbar radicular pain. Pain Med 11: 1149-1168.
- Yabuki S, Kikuchi S (1995) Nerve root infiltration and sympathetic block. An experimental study of intraradicular blood flow. Spine (Phila Pa 1976) 20: 901-906.
- Quraishi NA (2012) Transforaminal injection of corticosteroids for lumbar radiculopathy: systematic review and meta-analysis. Eur Spine J 21: 214-219.
- Manchikanti L (2002) Role of neuraxial steroids in interventional pain management. Pain Physician 5: 182-199.
- Park JW, Nam HS, Park Y (2011) Usefulness of posterolateraltransforaminal approach in lumbar radicular pain. Ann Rehabil Med 35: 395-404.
- Ulfendahl HR (1957) Some pharmacological and toxicological properties of a new local anaesthetic, CARBOCAIN®. ActaAnaesthScand 1: 81-86.
- Covino BG (1971) Comparative clinical pharmacology of local anesthetic agents. Anesthesiology 35: 158-167.
- Derby R, Kine G, Saal JA, Reynolds J, Goldthwaite N, et al. (1992) Response to steroid and duration of radicular pain as predictors of surgical outcome. Spine (Phila Pa 1976) 17: S176-183.
- Green LN (1975) Dexamethasone in the management of symptoms due to herniated lumbar disc. J NeurolNeurosurg Psychiatry 38: 1211-1217.
- Manchikanti L, Cash KA, Pampati V, Damron KS, McManus CD (2004) Evaluation of lumbar transforaminal epidural injections with needle placement and contrast flow patterns: a prospective, descriptive report. Pain Physician 7: 217-223.
- Nam HS, Park YB (2011) Effects of transforaminal injection for degenerative lumbar scoliosis combined with spinal stenosis. Ann Rehabil Med 35: 514-523.
- Huston CW, Slipman CW, Garvin C (2005) Complications and side effects of cervical and lumbosacral selective nerve root injections. Arch Phys Med Rehabil 86: 277-283.
- Glaser SE, Falco F (2005) Paraplegia following a thoracolumbar transforaminal epidural steroid injection. Pain Physician 8: 309-314.
- Glaser SE, Shah RV (2010) Root cause analysis of paraplegia following transforaminal epidural steroid injections: the 'unsafe' triangle. Pain Physician 13: 237-244.
- Atluri S, Sudarshan G, Yerramsetty P (2011) Time to understand "safe triangle technique" for transforaminal epidural steroid injections. Pain Physician 14: E459-460.
- Zhu J1, Falco FJ, Formoso F, Onyewu O, Irwin FL (2011) Alternative approach for lumbar transforaminal epidural steroid injections. Pain Physician 14: 331-341.
- Park JW, Nam HS, Cho SK, Jung HJ, Lee BJ, et al. (2011) Kambin's Triangle Approach of Lumbar Transforaminal Epidural Injection with Spinal Stenosis. Ann Rehabil Med 35: 833-843.
- Roberts ST, Willick SE, Rho ME, Rittenberg JD (2009) Efficacy of lumbosacral transforaminal epidural steroid injections: a systematic review. PM R 1: 657-668.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 14763
- [From(publication date):
November-2014 - Aug 19, 2025] - Breakdown by view type
- HTML page views : 10177
- PDF downloads : 4586
