Research Article Open Access
Treatment Of Lateral Epicondylitis With Pulsed Radiofrequency: Comparative Study Of Two Procedures
| Bovaira M1*, Calvo A2, Jiménez A2, Jovaní M3, Desçe J2 and March R4 | |
| 1 Head of Pain Unit, Department of Anesthesiology, Critical Care and Pain, Levante Rehabilitation Center, Valencia, Spain | |
| 2 Department of Anesthesiology, Critical Care and pain unit, Centro de Recuperación y Rehabilitación de Levante, Valencia, Spain | |
| 3 Associate Professor of Biostatistics, Valencia University of Medicine and Surgery, Valencia, Spain | |
| 4 Head of Anesthesiology, Department of Anesthesiology, Critical Care and Pain Unit, Levante Rehabilitation Center, Valencia, Spain | |
| Corresponding Author : | Maite Bovaira Forner Head of Pain Unit Department of Anesthesiology Critical Care and Pain Levante Rehabilitation Center Cirilo Amorós 47- 2º- 2ª 46004, Valencia, Spain Tel: +34 649409017 E-mail: bovaira@gmail.com |
| Received January 17, 2014; Accepted February 07, 2014; Published February 09, 2014 | |
| Citation: Bovaira M, Calvo A, Jiménez A, Jovaní M, Desçe J, et al. (2014) Treatment of Lateral Epicondylitis with Pulsed Radiofrequency: Comparative Study of Two Procedures. J Pain Relief 3:132. doi: 10.4172/2167-0846.1000132 | |
| Copyright: © 2014 Bovaira M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Objectives: Lateral epicondylitis (tennis elbow) is a tendinosis of the forearm extensor muscles; it has a clear occupational profile. Epicondylitis usually improves with conservative treatment but some 10% of cases require more invasive therapies, such as shock waves, infiltration with steroids or growth factors. Although its mechanism of action is unknown, pulsed radiofrequency appears to improve the patient’s perception of pain. In recent years, this has been used in peripheral pathologies with promising results. This study evaluates the efficacy of two different patterns of radiofrequency for treating epicondylitis.
Materials and methods: This was a comparative study of 34 patients, divided randomly intotwo groups: Group A received pulsed radiofrequency (PRF) at the lateral epicondyle trigger point with two needles (45 volts, for four minutes), creating a dual field; whenever a trigger point was located at the exit of the posterior interosseous, PRF was applied for two minutes; Group B received PRF at the lateral cutaneous branch of the radial nerve for 4 minutes; whenever a trigger point was located at the exit of the posterior interosseous, PRF was applied for two minutes. All patients were monitored during a six-month follow-up.
Results: In general, there was a tendency for pain to decrease, but the visual analogical scale(VAS) identified significantly higher decreases in Group B than Group A. Group Atreatment was effective (VAS decreased more than 50%) for 23% of patients after one month, for 47% of patients after three months and 58.8% of patients after six months. Group B results were better, with decreases in pain experienced by 65% of patients after one month, and 82.3% of patients after three and six months. The recovery of strength was also greater in Group B (8 out of 10) than Group A (6 out of 12). The average time passed before Group A patients could return to work following treatment was 3.058 ± 2.4, and 1.176 ± 1.24 months for Group B patients.
Conclusions: When epicondylitis fails to respond to conservative treatment, pulsedradiofrequency is a safe, partially effective technique. Its effect is greater when it is applied to peripheral nerves than to trigger points.
| Keywords |
| Lateral epicondylitis; Pulsed radiofrequency; Nerves; Trigger points; Efficacy |
| Introduction |
| Lateral epicondylitis (tennis elbow) is a frequent elbow condition with an incidence of 1-3% among the general population [1]. It consists of a chronic tendinosis produced, in most cases, by the overuse of the forearm extending muscles. It is related to manual work or sport activities, and so has a clear occupational profile [2]. |
| Its diagnosis is mostly clinical and its treatment is initially conservative. It usually has a long duration (6-9 months), is frequently self-limited, and is a common cause of sick leave, incurring considerable expense. |
| Regarding its etiopathogeny, lateral epicondylitis is caused by degenerative changes and non-accute inflammation, which are only present at very early stages of the illness. It is a degenerative tendinopathy, with degeneration of collagen tissue called angiofibroblastic tendinosis of the extensor carpi radialis brevis tendon and, at a lesser rate, of the common extensor of the fingers [3]. |
| Lateral epicondylitis first appears, insidiously and gradually, as pain on the lateral side of the elbow. It is usually associated with weakness and a feeling of loss of strength in the hand. Treatment is normally conservative and has satisfactory results in 90% of cases. But in the remaining 10%, supplementary treatments are recommended, based on physical therapy and ergonomic changes in the work place. Table 1 gives an extensive list of non-steroidal anti-inflammatory treatments (both oral and topical) and conservative therapies that may be applied [4-6] (Table 1). |
| Radiofrequency (RF) has been postulated as an efficient option among a range of peripheral therapies. There are two types of RF lesioning in clinical use: conventional (CRF) and pulsed (PRF). RF consists of the application of high frequency current to target tissues, mainly nerves and ganglions. Conventional radiofrequency, which has been in clinical use for 45 years [7], works by raising temperature resulting in a thermo coagulation of the surrounding tissues and neuroablation; it is the more common of the two RF types. More recently, pulsed RF has been developed, a system of radiofrequency that, rather than raise temperature, aims to work by generating electric fields [8]. |
| Many articles of research have tried to explain the ways in which pulsed radiofrequency might exert its biological effects. Although it is accepted that pulsed RF operates as a neuromodulating method, to date the internal processes of neuromodulation remain unknown [9]. |
| Pulsed radiofrequency is a safe method and recent research suggests it may be useful in the treatment of certain painful peripheral pathologies such as omalgia [10,11], pudendal neuralgia [12], carpal tunnel syndrome [13], meralgiaparesthetica [14] and joint pain [15]. |
| The aim of this study was to test the efficacy of pulsed radiofrequency, comparing two different techniques used to treat lateral epycondilitis. |
| Materials and Methods |
| This was a randomized, prospective study of 34 patients with lateral epicondylitis. The patients had previously received conservative treatment consisting of physiotherapy and anti-inflammatory medication. All patients gave their informed consent to participate in the study, and were divided randomly into two groups: |
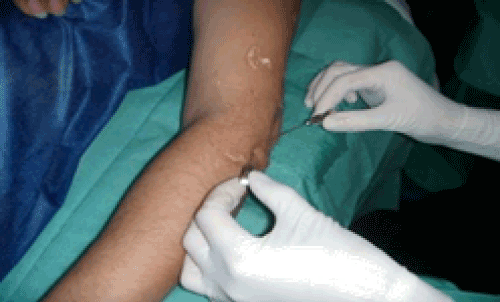
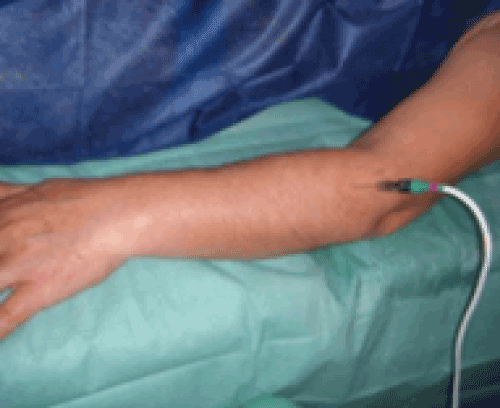
| Group A: The carpi extensor radialisbrevis tendon was approached by means of two needles, applied for four minutes, creating an electric field that would act on the nerve fibers. As postulated by Sluijter in 2008, it is thought that this could have an inmunohistochemical effect on the degenerated tendon [15] (Figure 1). If a trigger point was located at the exit of the posterior interosseous nerve, pulsed radiofrequency was also applied at this point for two minutes (Figure 2). |
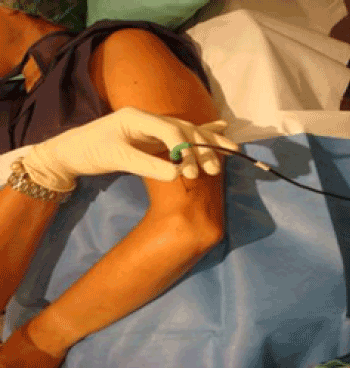
| Group B: Considering elbow innervation, PRF was applied to the cutaneous antebrachial dorsal nerve for two minutes, which is located on the humeral crest and constitutes the most extensive innervation of the epicondyle (Figure 3). If a trigger point was located at the level of the posterior interosseous, PRF was applied for two minutes. |
| PRF parameters were: 45 volts, 42ºC, two cycles per second, of 2 milliseconds each. |
| The following variables were assessed: |
| - Measurement of pain by means of visual analogue scale (VAS) taken at baseline, after 15 days, one, three and six months. |
| - Strength recovery (evaluated as a percentage; strength recovery greater than 30% was considered as positive). |
| - Post-treatment surgery. |
| - Time passed before returning to work. |
| - Possible side effects. |
| Patient follow-up continued for six months.Since the sample size was not very large, statistical analysis of results was performed applying non-parametric procedures, including the Mann-Whitney U test and Student’s T test. Significance was set at p<0.05. |
| Results |
| The two groups of 17 patients were homogeneous, with the exception of gender distribution – eight women in Group A and four in Group B. Average age was similar: 42.7 ± 3.7 years in Group A and 43.23 ± 52 in Group B. In both groups, there was a clear commonality between types of work: most patients were manual workers (electricians, plumbers [16,17]; bricklayers [6] and cleaners [4]), with no differences between groups. |
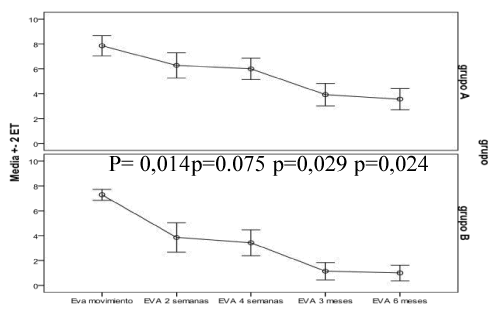
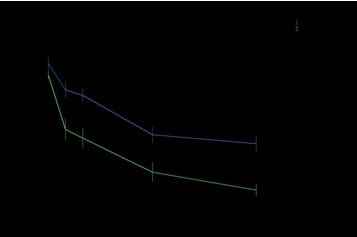
| Pain decreased over time in both Groups A and B, especially at the two-week and three-month follow-ups after treatment. However, it was found that pain reduction was not equal between thegroups; the decline in VAS scores for each variable was significantly higher in Group B than Group A, (p<0.05) (Figures 4 and 5). |
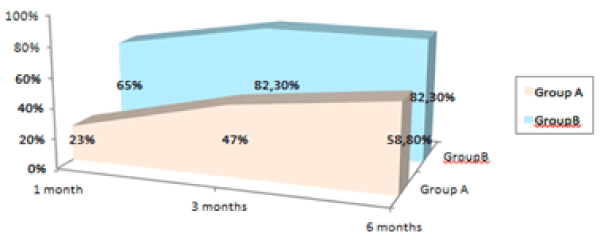
| Considering treatment as effective when VAS scores were reduced by 50% or more, Group A treatment was effective in 23% of the patients alter one month, in 47% of patients after three months, and in 58.8% of patients after six months. Group B results were clearly better with an efficacy of 65% of patients after one month, and 82.3% of patients after three and six months (Figure 6). |
| These are good results compared with the usual evolution of the disease.Regarding the recovery of strength, 12 Group A patients believed they had suffered a loss of strength; six of them recovered after treatment. In Group B, only two patients out of ten showed no sign of recovery. |
| The rate of surgery after treatment was similar in both groups: four patients in Group A and three in Group B. Four patients in Group A had been off work prior to treatment; the mean time needed before they could return to work after PRF had been applied was 3.05 ± 2.4 months. In Group B, six patients were off work; the mean time needed before they could return to work after PRF treatment was 1.176 ± 1.24 months. In this way, the recovery time was significantly longer in Group A patients (p=0.005). |
| Discussion |
| Therapeutic approaches to peripheral pain pathologies – including epicondylitis – remain badly defined in clinical practice. While numerous articles on different conservative treatments proclaim hopeful results, few give scientific evidence of their efficacy. In 2002, Rohof suggested that pulsed radiofrequency might provide an effective treatment for less severe pain arising from lateral epicondylitis. However, no published research has defined what the exact target of PRF treatment should be in cases of epicondylitis. PRF was developed in 1995, and its first clinical application was performed on 1st February 1996 [8]. Its mechanism of action is still unknown but is an ongoing topic of investigation. It has traditionally been considered a neuromodulating technique [9,17] with no side effects. However, Cosman and Cosman Sr. [18] claimed that destructive effects could be expected to occur at microscopic level. The most likely causes of pathology of RF lesions are heat, high electric fields and high current fields, which produce changes in cellstructure,electroporation and the destruction of membranes. This would bring about certain miniablation in the surrounding tissues, but only in a thin surrounding layer of about 0.3 mm. The small area of tissue destruction following PRF may be attributed to heat spikes. |
| One study looked at exposure of the cervical dorsal root ganglion (DRG) to both CRF and PRF [19]. C-Fos expression was found to increase bilaterally in the dorsal horns of rats seven days after intervention with both CRF and PRF. C-Fos is a non-specific immediate early gene marker that is used to detect activated neurons. This supports the concept that C-Fos activation is heat independent and may provide information as to the mechanism of action of PRF in pain relief. Another study looked at cell stress in rats after PRF application by studying activating transcription factor 3, a marker of cell stress [20]. Results showed that PRF seems to act effectively on the finest axons, specifically C and A-δ nociceptive fibers, with an absence of motor or sensitive alterations. It would be logical, therefore, “to assume that cell stress will result in general reduction of cellular activity including down-regulation of excitatory neuromodulators within nociceptors and this may include behavioral analgesia” [20]. |
| Erdine et al. studied PRF applied to the sciatic nerve of rats, while a control sham application was simultaneously applied to the contralateral sciatic nerve [21]. The ultrastructure of the treated axons was examined after ten days by electron microscopy. Evidence was found that PRF produced an alteration in the morphology of mitochondria, and disruption and disorganization of microfilaments and microtubules. The study also reported the way in which PRF acts on the thinnest fibers selectively. |
| Vallejo et al. [22], in a more recent study, examined the modulated expression of pain regulatory genes following the induction of spared sciatic nerve injury pain model in rat, treated with PRF therapy. Many of these genes returned to control values in each of these tissues: sciatic nerve, ipsilateral L5 dorsal root ganglia and spinal cord. |
| In 2008, Sluijter [15] published an article on intra-articular PRF applied to both small and large joints. The author postulated two different mechanisms of action: one acting on the nerves innervating small joints, and the other a possible effect of the electric field on the immune system. In this way, PRF could have an anti-inflammatory effect which would account for its possible efficiency on the largest joints. |
| If the mechanism of action of PRF has not been fully defined, there is even less data regarding its efficacy. In an article criticizing PRF [23], the author claimed that applying PRF instead of CRF means changing a technique whose efficiency has been proved for one with no proven benefit. |
| There are few randomized studies about PRF efficacy. Van Zundert et al. [24] applied PRF to cervical DRG in patients with chronic cervical pain. Of a total sample of 23 patients, PRF was applied to the cervical DRG in 11 patients, while the remaining 12 patients were treated with a needle of similar characteristics containing a placebo. The difference in the results was noticeable after three months: 82% of the group treated with PRF experienced a reduction in pain of over 50%, compared with 25% in the placebo group; after 6 months, those treated with PRF showed a significant reduction in pain medication. No complications were observed. Recently, Gofeld et al. [25] published a randomized double-blind trial of pulsed radiofrequency of supraescapular nerve to treat chronic shoulder pain. Considering limitations of the study design, PRF seems to be more effective than lidocaine injection alone. |
| Numerous works have been published describing clinical cases and clinical case series of PRF applied to different nerves and peripheral ganglions for the treatment of chronic pain [10-15]. None of these cases have reported negative effects. The period during which pain continues to decline seems to range from two to 30 months, with a mean duration of 9.2 months [12]. |
| Other advantages of PRF are that the treatment may be repeated if pain reappears, as the technique is neuromodulating, only minimally destructive [9,20], and selective for nocicetive fibers (C and A-δ). |
| PRF’s most relevant limitation continues to be the incomplete knowledge of its mechanism of action and the lack of randomized studies that support its efficacy. |
| The present study set out to evaluate PRF efficacy in terms of two mechanisms of action: neuromodulation and its possible antiinflammatory effect. The study suffered an important limitation in that the patients sample was not large enough to reach firm conclusions but nevertheless, the results for the efficacy of PRF for the parameters assessed are statistically significant in favor of PRF application to the nerves most seriously affected by lateral epicondylitis. |
| Conclusions |
| Based on the results of the present study with a limited sample size, it may be concluded that the use of pulsed radiofrequency on the nerves innervating the epicondyle is effective in the middle and long term. The reduction in pain helped the recovery of strength, and these improvements contributed to an earlier return to work among patients on sick leave. |
| There was a slight improvement to muscular targets resulting from PRF treatment but these did not reach statistical significance. In no case were negative effects observed. |
References
- Shiri R, Viikari-Juntura E, Varonen H, Heliovaara M (2006) Prevalence and determinants of lateral and medial epicondylitis: a population study. Am J Epidemiol 164: 1065-1074.
- Hortal RM, Salido M, Navarro P, Candelas G (2005) Epicondilitis. Semin Fund Esp Reumatol 6: 79-88.
- Henry M, Stutz C (2006) A unified approach to radial tunnel syndrome and lateral tendinosis. Tech Hand Up Extrem Surg 10: 200-205.
- Nimgade A, Sulllivan M, Goldman R (2005) Physiotherapy, steroid injections, or rest for lateral epicondylosis? What the evidence suggest. Pain Practice 5: 203-215.
- Pettrone FA, McCall BR (2005) Extracorporeal shock wave therapy without local anesthesia in chronic lateral epicondylitis. J Bone Joint Surg Am 87: 1297-1304.
- Galvin R, Callaghan C, Chan WS, Dimitrov BD, Fahey T (2011) Injection of botulinum toxin for treatment or chronic lateral epicondilitis: Systematic review and meta-analysis. Semin Arthritis Rheum 40: 585-587.
- Rosomoff HL, Carroll F, Brown J, Sheptak P (1965) Percutaneous radiofrequency cervical cordotomy technique. J Neurosurg 23: 639-644.
- Sluijter ME, van Kleef M (2007) Pulsed radiofrequency. Pain Medicine 8: 388-389.
- Reig E, Abejón D (2003) Is pulsed radiofrequency a neuromodulation technique? Neuromodulation6:1-3.
- Rohof O (2002) Radiofrequency treatment of Peripherals nerves. Pain Practice 2: 257-260.
- Liliang PC, Lu K, Ling CL, Tsai YD, Hsieh CH, et al. (2009) Pulsed radiofrequency lesioning of the suprascapular nerve for chronic shoulder pain: a preliminary report. Pain Medicine 10: 70-75.
- Rhame EE, Levey KA, Gharibo CG (2009) Succesful treatment of refractory pudendal neuralgia with pulsed radiofrequency. Pain Physician 12: 633-638.
- Haider N, Mekansha D, Chiravuri S, Wasserman R (2007) Pulsed radiofrequency of the median nerve under ultrasound guidance. Pain Physician 10: 765-770.
- Philip CN, Candido KD, Joseph NJ, Crystal GJ (2009) Successful treatment of meralgiaparesthetica with pulsed radiofrequency of the lateral femoral cutaneous nerve. Pain Physician 12: 881-885.
- Sluiter ME, Texeira A, Serra V, Balogh S, Schianchi P (2008) Intraarticularapplicationa of pulsed radioqrequency for arthrogenic pain. Report of six cases. Pain Practice 8: 51-61.
- Wilhem A (2000) Tratamiento de la epicondilitis humeral en resistente al tratamiento fisioterápico mediante denervación. Tec Quir Ortop Traumatol 9: 213-225.
- Cahana A, van Zundert J, Macrea L, van Kleef M, Sluijter M (2006) Pulsed radiofrequency: Current clinical and biological literature available. Pain Medicine 7:411-423.
- Cosman Jr ER, Cosman Sr ER (2005) Electric and thermal fields’ effects in the tissue around radiofrequency electrodes. Pain Medicine 6: 405-424.
- van Zundert J, deLouw AJA, Joosten EAJ, Kessels AGH, Honig W, et al. (2005) Pulsed and continuous radiofrequency current adjacent to the cervical dorsal root ganglion of the rate induces late cellular activity in the dorsal horn. Anesthesiology 102: 125-131.
- Hamann W, Abou-Sherif S, Thompson S, Hall S (2006) Pulsed radiofrequency applied to dorsal root ganglia causes a selective increase in ATF3 in small neurons. Pain 10: 171-176.
- Erdine S, Bilir A, CosmanSr ER, Cosman Jr ER (2009)Ultraestructural changes in axons following exposure to pulsed radiofrequency fields. Pain Practice 9: 407-417.
- Vallejo R, Tilley DM, Williams I, Labak S, Aliaga L, et al. (2013) Pulsed radiofrequency modulates pain regulatory gene expression along the nociceptive pathway. Pain Physician 16: 601-613.
- Bogduk N (2006) Pulsed radiofrequency. Pain Med 7: 396-407.
- van Zundert J, Patijn J, Kessels A, Lame I, van Suijekom H, et al. (2007) Pulsed radiofrequency adjacent to the cervical dorsal root ganglion in chronic cervical radicular pain: A double blind sham controlled randomized clinical trial. Pain 127: 173-182.
- Gofeld M, Restrepo-Garces CE, Theodore BR, Faclier G (2013) Pulsed radiofrequency of supraescapular nerve for chronic shoulder pain: a randomized double-blind placebo-controlled study. Pain Practice 13: 96-103.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
 |
 |
 |
| Figure 4 | Figure 5 | Figure 6 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 17072
- [From(publication date):
February-2014 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 12215
- PDF downloads : 4857
