Research Article Open Access
Ultrasound Guidance in Paravertebral Injections of Oxygen-Ozone: Treatment of Low Back Pain
| Araimo Morselli FSM*, Zuccarini F, Scarpa I, Imperiale C, Guzzo F, Toro F and Tordiglione P | |
| Department of Anaesthesiology and Critical Care Medicine, Sapienza University of Rome, Italy | |
| Corresponding Author : | Fabio Silvio Mario Araimo Morselli Department of Anaesthesiology and Critical Care Medicine Sapienza University of Rome Viale del Policlinico 155, 00186, Rome, Italy Tel: +39 333 508 3507 Fax: +39 06 499 791 91 E-mail: f.araimo@policlinicoumberto1.it |
| Received: September 09, 2015 Accepted: December 02, 2015 Published: December 08, 2015 | |
| Citation: Araimo Morselli FSM, Zuccarini F, Scarpa I, Imperiale C, Guzzo F, et al. (2015) Ultrasound Guidance in Paravertebral Injections of Oxygen-Ozone: Treatment of Low Back Pain. J Pain Relief 4:220. doi:10.4172/2187-0846.1000220 | |
| Copyright: © 2015 Araimo Morselli FSM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Background: Paravertebral injection of ozone is an established clinical practice for the treatment of Low Back Pain (LBP). The role of Ultrasound Guidance (USG) in mini invasive procedures has become important in many clinical practice thanks to the greater precision this technique can add. As matter of fact, a large volume of ozone in a single administration may have some adverse or side effects. In this study we wanted to verify if the use of USG in Oxygen/ Ozone (O2/O3) infiltrations could allow the administration of a smaller volume of gas mixture, increasing the safety and the comfort of the procedure itself, obtaining however similar or better results in pain decrease.
Methods: We compared two groups of 25 patients affected by LBP, undergoing 10 infiltrations of O2/O3, by using USG (group U) or only anatomical landmarks (group AL). Pain intensity, by calculating Visual Analogical Scale (VAS) difference before and after the treatment, and the discomfort were evaluated in both groups.
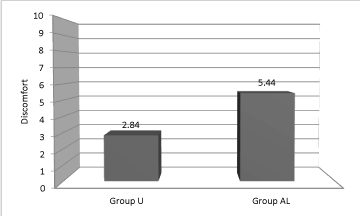
Results: The mean of the VAS before the treatment was 6.44 in group U and 6.48 in group AL. The mean of the VAS after the treatment was 2.22 in group U and 3.04 in group AL. The mean of discomfort rate was 2.84 in group U and 5.44 in group AL. The number of patients with unbearable discomfort was 0 in group U and 7 in group AL.
Conclusions: As many other treatment, also paravertebral injections of O2/O3 benefits of the advantages of the US device which makes this treatment safer and more accurate.
| Keywords |
| Ozone; Low back pain; Paravertebral injections; Ultrasound guidance |
| Abbreviations |
| USG: Ultrasound Guidance; O2/O3: Oxygen-Ozone; LBP: Low Back Pain; Group U: USG Procedure; Group AL: Anatomical Landmarks; BMI: Body Mass Index; SD: Standard Deviation; SEM: Standard Error of the Mean; CI: Confidence Interval |
| Introduction |
| Low Back Pain (LBP) is a frequent and economically relevant disease with a cumulative life incidence of 70%. It is one of the most causative for long-lasting disability and the most common cause of invalidity in the population with an age >45 years [1-3]. Many studies demonstrated how patients affected by LBP have positive analgesic effects when treated by Oxygen/Ozone (O2/O3) infiltrations [4-6]. The administration of O2/O3 by paravertebral injections increases the threshold of pain through the nociceptive stimulation thanks to the engagement of the descending control of spinal nociception [7]. |
| The efficacy of ozone in the treatment of LBP is very well stated by Megalhães’ analysis [4] but, as all mini invasive procedures, it may have side effects caused by the procedure itself as well as gas infiltration [7]. As a matter of fact, large volume of ozone in a single administration may have the following adverse or side effects [7-9]: acute muscular pain and deep visceral pain with high incidence of symptoms and exacerbation of the functio laesa, fatal air embolism due to erroneous injection of a big volume of gas in a blood vessel, burning and heaviness sensation, various complications caused by improper use of gas mixture (dosage and administration). The aim of our study was to evaluate the use of Ultrasound Guidance (USG) to practice O2/O3 infiltrations in order to enhance better identification of the anatomical landmarks and therefore the need for a smaller volume of O2/O3. |
| Materials and Methods |
| The study was conducted at Pain Center of Policlinico Umberto I, University of Rome Sapienza, upon approval by the Institutional Ethical Committee: protocol number 718/12. |
| Sample size calculation was performed by calculator GraphPad InStat 3. We enrolled, from January 2014 to March 2015, 50 patients: 26 males and 24 females affected by LBP, not responsive to classical pharmacology, aged between 39 and 77 years, having a BMI range of 18.5-24.9. |
| Each patient was asked to sign an informed consent before starting the treatment. Patients were included in two groups: group U (n=25) and group AL (n=25). Randomization process was programmed by an online program (www.randomization.com) and statistical unit, in sealed envelope, was sent to the investigators for randomization purpose. |
| Exclusion criteria were: favism, pregnancy, severe cardiovascular diseases, hematological and respiratory failure, cancer and thyreopaties. |
| The treatment consisted in 10 administrations, once a week. Needle’s caliber used for the treatment was 25 G * 90 mm in both groups. |
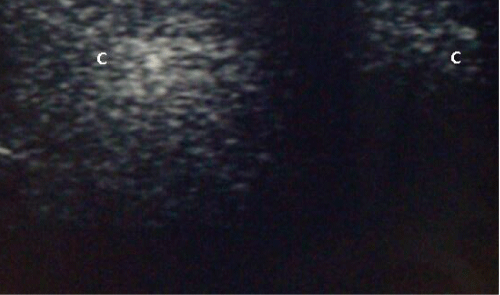
| Group U underwent a single administration per side of 5 ml of O2/O3 [O3 20 mcg/ml], practiced under USG (MicroMaxx Ultrasound System 38 mm, SonoSite, Via della Moscova, 3, 20121, Milano, Italy).After located the trigger area by manual palpation, we proceeded to the injection of O2/O3 under USG at a distance of 2 cm from the spinal apophysis. The needle was inserted at 35-45° to the sagittal plane of the body. The correct position of the needle was confirmed by its identification near the articular facets thanks to the USG. After the injection, ozone should reveal as a hyperecogen area (Figure 1). The ozone administration was performed after negative aspiration test, in order to avoid blood vessels’ involving. |
| Group AL underwent a single administration per side of 10 ml of O2/O3 [O3 20 mcg/ml]. The identification of the anatomical landmarks was only based on manual palpation. After located the trigger area, we proceeded to the injection of O2/O3 at a distance of 2 cm from the spinal apophysis. The needle was inserted at 35-45° to the sagittal plane of the body. The ozone administration was performed after negative aspiration test, in order to avoid blood vessels’ involving. |
| Pain assessment was performed as follows: |
| - Pain intensity by VAS, before and after each treatment cycle (10 injections). |
| - Discomfort by a numeric scale from 0 to 10. |
| A binary variable was defined with discomfort. A discomfort ≥7 was classified as unbearable and a discomfort ≤ 6 as bearable. We defined as unbearable a discomfort which caused such a great burning and heaviness sensation that could threaten the continuity of the treatment and patient’s confidence in the procedure. |
| A Medica-srl machine, model E100, was used to generate medical ozone (Ozonline International, Medica S.r.l., Via Sante Vincenzi, 48 – 40138, Bologna, Italy) from oxygen and electricity. The machine converts medical oxygen into a mixture of O3 (0.05%) and O2 (99.95%) through an electrochemical process. It is equipped with a photometer, calibrated according to the classic iodometric titration of ozone, and a voltage system which regulates the concentration within a range from 5 to 100 μg/ml. |
| Results |
| In group U, before the treatment, the mean of the VAS was 6.44, SD was 1.294, SEM was 0.2587, CI95%=[5.906-6.974]; the minimum was 4, the maximum was 9; normality test p value was 0,0236. After the treatment, the mean of the VAS, was 2.22, SD was 1.958, SEM was 0.3916, CI95%=[1.392-3.008]; the minimum was 0, the maximum was 6 normality test p value was <0.0001 (Table 1). |
| The mean of the discomfort was 2.84, SD was 1.028, SEM was 0.256, CI95%=[2.416-3.264]; the minimum was 0, the maximum was 4; the median (50th percentile) was 3.000; normality test p value was <0.0001. |
| In group AL, before the treatment, the mean of the VAS was 6.48, SD was 1.584, SEM was 0.3169, CI95%=[5.826-7.134]; the minimum was 4, the maximum was 10; normality test p value was 0.0032. After the treatment, the mean of the VAS was 3.04, SD was 2.508, SEM was 0.5016, CI95%=[2.005- 4.075]; the minimum was 0, the maximum was 7; normality test p value was 0.0251 (Figure 2). |
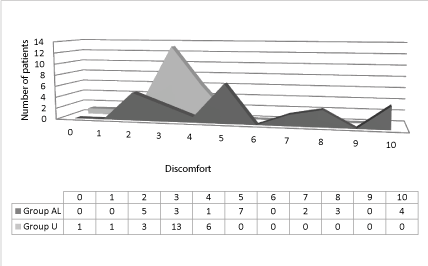
| The mean of the discomfort was 5.44, SD was 2.800, SEM was 0.560, CI95%=[4.284-6.596]; the minimum was 2, the maximum was 10; the median (50th percentile) was 5.000; normality test p value was <0.0096 (Figure 3). |
| The medians of VAS in group U and AL do not differ significantly. The two tailed p value is 0.1316 (Mann-Whitney Test). |
| The medians of discomfort rate of group U was 2.60 points less than group AL. Patients with unbearable discomfort is significantly different between the two groups: 0 in group U and 7 in group AL, tested by Fisher exact test (p<0.01) (Figure 4). |
| The medians of discomfort in group U and AL differ significantly. The two tailed p value is 0.0008 (Mann-Whitney Test). |
| Discussion |
| Even if it’s always more affirmed in many clinical practice with indisputable advantages in terms of efficacy and safety, international guidelines concerning paravertebral injections of O2/O3 do not provide for USG. Our study demonstrates that also this kind of procedure takes advantages from the support of this device. |
| At the present state, many studies demonstrate the efficacy of ozone therapy in the treatment of LBP [4,6,8-13]. |
| As showed by Megãlhaels’ analysis, O2/O3 therapy appears to yield positive results and low morbidity rates when applied percutaneously for the treatment of LBP [4]. |
| Melchionda also reports positive effects of O2/O3 therapy in terms of rapidity, simplicity and safety of the procedure in treating lumbar radiculopathies secondary to disc herniation [9]. |
| Our clinical practice allowed us to understand that, when the anatomical landmarks were identified by palpation, patients underwent to 10 ml O2/O3 [20 mcg] injections had better results in terms of VAS decrease than those underwent to 5 ml O2/O3 [20 mcg] injections. Anyway they also had a greater discomfort caused by the big volume injection and some of them referred such a great burning and heaviness sensation that could have threaten the continuity of the treatment and patient’s confidence in the procedure. |
| That is why we decided to investigate if the use of USG in paravertebral injection of 5 ml O2/O3 could help to reach the same results of 10 ml injections in terms of VAS decrease obtaining however the benefits of safety and low discomfort of 5 ml injection. For this purpose, this study allowed us to reconfirm the minimal volume, efficacious and with less discomfort, for USG injections. |
| The results showed that the discomfort caused by the procedure is significantly lower in group U than in group AL (p=0.0008) and the number of patients with unbearable discomfort is significantly lower in group U (p<0.01). A big volume injection is perceived as a heaviness and burning sensation by patients. Moreover, the reduced use of O2/O3 volume increased the safety of this technique [7-9]. |
| Both procedures were equal in term of VAS decrease. The medians of VAS in group U and AL do not differ significantly. The two tailed p value is 0.1316. |
| In order to benefit of the therapeutic effect of this gas mixture, O2/O3 injection should be as closest as possible to the articular facet. But how to be certain of where we are injecting without the aid of USG? |
| In conclusion, we support the need for more investigations about USG paravertebral injections in the treatment of LBP to implement our preliminary results. In our opinion, the opportunity of a better precision and therefore, the use of a smaller volume of O2/O3 makes this technique more accurate and safer. |
| References |
References
- Andersson GB (1999) Epidemiological features of chronic low-back pain.Lancet 354: 581-585.
- Murray CJ, Atkinson C, Bhalla K, Birbeck G, Burstein R, et al. (2013) The state of US health, 1990-2010: burden of diseases, injuries, and risk factors.JAMA 310: 591-608.
- Werner CM, Hoch A, Gautier L, König MA, Simmen HP, et al. (2013) Distraction test of the posterior superior iliac spine (PSIS) in the diagnosis of sacroiliac joint arthropathy.BMC Surg 13: 52.
- Magalhaes FN, Dotta L, Sasse A, Teixera MJ, Fonoff ET (2012) Ozone therapy as a treatment for low back pain secondary to herniated disc: a systematic review and meta-analysis of randomized controlled trials.Pain Physician 15: E115-129.
- Borrelli E (2011) Mechanism of action of oxygen ozone therapy in the treatment of disc herniation and low back pain.ActaNeurochirSuppl 108: 123-125.
- Paoloni M, Di Sante L, Cacchio A, Apuzzo D, Marotta S, et al. (2009) Intramuscular oxygen-ozone therapy in the treatment of acute back pain with lumbar disc herniation: a multicenter, randomized, double-blind, clinical trial of active and simulated lumbar paravertebral injection.Spine (Phila Pa 1976) 34: 1337-1344.
- Ceccherelli F, Ricciardi A (1998) Lombalgie e Lombosciatalgie: Criteri di Diagnosi e Cura. Libreria Cortina, Torino.
- Peng J, Xing H, Zhang B, Wu F, Guo J, et al. (2009) Analysis of the efficacy of ozone therapy on lumbar disc herniation. International Journal of Ozone Therapy 8: 206-210.
- Melchionda D, Milillo P, Manente G, Stoppino L, Macarini L (2012) Treatment of radiculopathies: a study of efficacy and tolerability of paravertebral oxygen-ozone injections compared with pharmacological anti-inflammatory treatment. J. Biol. Regul. Homeost. Agents 26: 467-474.
- De Nêuton F, Magalhães O, Soares SC, Torres JM, et al. (2013) Effects of ozone applied by spinal endoscopy in patients with chronic pain related to failed back surgery syndrome: a pilot study. Neuropsychiatr. Dis. Treat. 9: 1759-1766.
- Rahimi-Movaghar V, Eslami V (2012) The major efficient mechanisms of ozone therapy are obtained in intradiscal procedures.Pain Physician 15: E1007-1008.
- Muto M, Ambrosanio G, Guarnieri G, Capobianco E, Piccolo G, et al. (2008) Low back pain and sciatica: treatment with intradiscal-intraforaminal O(2)-O(3) injection. Our experience.Radiol Med 113: 695-706.
- Apuzzo D, Giotti C, Pasqualetti P, Ferrazza P, Soldati P, et al. (2014) An observational retrospective/horizontal study to compare oxygen-ozone therapy and/or global postural re-education in complicated chronic low back pain.FunctNeurol 29: 31-39.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 11444
- [From(publication date):
January-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 10420
- PDF downloads : 1024
