Case Report Open Access
Ultra-sound Guided Intercostal Neurolysis for Intractable Pain Arising out of Rib Fracture
| Arif Ahmed*, Divesh Arora, Amit Kochar and Niti Gulati | |
| Department of Anesthesia and Pain Management, Asian Institute of Medical Sciences, Sector 21A, Faridabad, Haryana-121001, India | |
| Corresponding Author : | Arif Ahmed Department of Anesthesia and Pain Management Asian Institute of Medical Sciences, Sector 21A Faridabad, Haryana-121001, India Tel: +919717379370 E-mail: arifahmed1978@gmail.com |
| Received: January 07, 2016; Accepted: January 25, 2016; Published: January 31, 2016 | |
| Citation: Ahmed A, Arora D, Kochar A, Gulati N (2016) Cardiac Ultra-sound Guided Intercostal Neurolysis for Intractable Pain Arising out of Rib Fracture. J Pain Relief 5:228. doi:10.4172/2187-0846.1000228 | |
| Copyright: © 2016 Ahmed A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Introduction: Rib fracture from blunt chest trauma leads to considerable morbidity, which increases with each rib fracture. There are multiple methods of pain relief from rib fracture, but most of them are effective for short duration and in acute pain setting. In a few patients, whom the pain becomes chronic, the treatment could be difficult. In this case report, we are describing a patient with severe chest pain arising out of 1st to 11th rib fracture, whose pain was not controlled even after multiple interventions and was on multiple medications.
Case presentation: We had done ultrasound guided intercostal neurolysis of 1st to 11th intercostal nerve with 2 ml of 50% alcohol, after having more than 80% relief from the ultrasound guided diagnostic intercostal block at all the levels. After the neurolysis, there was good pain relief of chest pain, and the patient was able to take deep breaths and do chest physiotherapy. The pain relief from the neurolysis lasted for more than 6 months .There was no immediate and delayed complications after the procedure.
Conclusion: The Ultrasound guided intercostal neurolysis can be a good long lasting alternative for the patients with uncontrolled severe pain from rib fracture.
| Keywords |
| Ultrasound guided; Intercostal neurolysis; Rib fracture |
| Introduction |
| The morbidity and mortality associated with blunt chest trauma is very high [1]. The rib fracture is one of the major part of blunt trauma and the complications increases with each additional rib fracture [2,3]. Rib fractures lead to splinting of chest due to pain and mechanical instability, which finally causes inadequate ventilation, which finally leads to decrease in lung volumes, atelectasis, progressing to respiratory failure and even death [4,5]. If the treatment of rib fracture is not initiated in a timely manner, the complications lead to longterm pulmonary impairment, prolonged hospital stay and increased utilization of health-care resources [1]. |
| There are various effective modalities for the pain relief from the rib fractures, which are non-steroidal anti-inflammatory drugs, patient controlled intravenous analgesia, epidural analgesia, paravertebral analgesia, intercostal blocks and ligocaine patches, etc. [5-10]. But in a few patients, the pain continues and most of these modalities are effective for few days only. In those groups of patients, whom the pain becomes chronic, the main stay of the treatment is opioids and adjuvant medications. In our case, the situation was more difficult as the patient was not able to tolerate opioids due to its adverse effects. |
| Case Presentation |
| We are discussing a patient with fracture of 1st to 11th ribs on left side with severe uncontrolled pain. |
| Our patient is a 52 year old male with no co-morbid illness, who had suffered road traffic accident leading to fracture of ribs, clavicle, vertebrae and pelvis. His Computerized tomography scan showed fracture of 1st to 11th ribs on left side, mild left hemothorax and atelectetic underlying lung, fracture left clavicle, fracture of left transverse process of L1 vertebrae, undisplaced fracture left iliac crest. He complained of severe pain (numerical rating scale, NRS=10/10) over chest on movement, was not able to do deep breathing, coughing and physiotherapy, which resulted in shallow breathing. He was managed conservatively for rib fracture as there was no evidence of flail chest. He was first offered epidural catheter placement at T10-11 level and infusion with local anesthetic (bupivacaine) and opioid (fentanyl), that resulted in excellent pain relief, was able to move, take deep breaths and able to participate in chest physiotherapy. But after 5 days, the epidural catheter was removed and the patient again started to have pain of the same intensity as before and at the same site, and so he was started on intravenous patient controlled analgesia with morphine, but it helped in relieving pain only partially with adverse effects like nausea, vomiting and sedation. So, he was then given continuous paravertebral infusion, which lead to good relief for next 1 week. After the removal of paravertebral catheter and the patient had only slight relief with the patient controlled analgesia with morphine. In the subsequent days, lignocaine infusion and ketamine infusion was tried, but with only minimal benefit. So, finally other options like repeat paravertebral and epidural or intercostal blocks were discussed with the patient, but he was not willing to try an intervention which was temporary in nature. So, the option of diagnostic inter-costal block, and the subsequent therapeutic neurolysis was discussed with him and he agreed to try it. |
| Procedure |
| The diagnostic inter-costal nerve block was performed from 1st to 10th inter-costal space with the patient in sitting position under ultrasound (USG) guidance. The patient was kept in sitting position and the back and left lateral aspect of the chest wall was cleaned with antiseptic solution and covered with sterile drapes. The ribs and inter-costal were identified by using high frequency (6-13 Hz) linear ultrasound (USG) probe (M-Turbo® ultrasound system, Sonosite international, Washington, USA). The site of injection was at the posterior inter-costal line and probe was placed along the short axis to the ribs. The point of entry was anesthetized with 0.5 ml of 1% lignocaine. Under in-plane approach, a 5 cm SonoPlex Stim Cannula (Pajunk Medical Systems L.P., Norcross, GA 30071 USA) was directed into the inter-costal space. The point of entry of the needle was at the upper border of the lower rib, and directed towards the lower and innermost margin of upper rib. Small amount of the saline solution is injected as the needle was advanced in the inter-costal space to prevent pleural puncture, and final position was at 2-3 mm above the pleurae (which was seen as a shining moving structure between the ribs), between internal and innermost intercostal muscle. After negative aspiration for both air and blood, 1 ml of 1% lignocaine was injected under USG guidance at each level. The patient was then observed in the recovery area and physical evaluation of the patient was done to evaluate the effectiveness of the block. After one hour, the NRS score at rest and on deep breathing and coughing were noted. The NRS score had decreased from 10/10 to 1/10 at rest, 2/10 on coughing and deep inspiration and 4/10 over the clavicle area. He was able to move three balls of the spirometer after the block as compared to his inability to move even a single ball of the spirometer before the procedure (Figure 1). |
| After the diagnostic inter-costal block, the risks and benefits of the therapeutic inter-costal neurolysis was discussed with the patient. |
| Therapeutic inter-costal neurolysis was performed on subsequent day at 1st to 10th inter-costal space under USG guidance. The inter-costal neurolysis was done in a similar manner like diagnostic intercostal block till the final positioning of the needle. After negative aspiration for both blood and air, 2 ml of 50% alcohol plus 0.25% bupivacaine was injected at each inter-costal space under USG guidance. In two occasions, patient complained of severe burning pain after the alcohol injection at the injection site only without any radiation which resolved after further injection of 0.5 to 1 ml of 2% preservative free lignocaine. |
| After the neurolysis, the patient was comfortable, able to take deep breaths, cough deeply and participate in the physiotherapy. He was discharged after 2 days and participating in the physiotherapy at home and as an outpatient. He was weaned off to tramadol, etoricoxib and paracetamol. At 3 and 6 months, he was having only minimal pain over the clavicle, which occurs from the active movement of shoulder. The NRS at 3 and 6 month was 1/10 over the ribs on rest and on coughing or deep inspirations. He was able to do the spirometry and deep breathing exercises well without any discomfort till 3 months. Whereas at 3 month NRS was 3/10 over the clavicle on active movement of shoulder, which decreased to 1-2/10 at 6 months. At 3 months, there was mild tenderness (NRS=3/10) over the fracture site of 5th and 7th rib, but it is not causing any discomfort or physical limitation, which disappeared at 6 months. |
| Case Discussion |
| Blunt chest trauma leads to considerable mortality and morbidity, and rib fracture is the major component of blunt chest trauma with complications increasing with each additional rib fracture [1-3]. With rib fracture there is splinting of chest due to pain and mechanical instability leading to hypoventilation, finally leading to loss of lung volumes, atelectesis, progressive respiratory failure and even death [4,5]. But in spite of substantial contribution to morbidity and poor quality of life, the current treatment is only supportive in majority of patients [11]. Chronic pain after rib fracture is very common up to 64% and prolonged disability was found in up to 66 % patients [12,13]. With rib fracture there is detoriation of the quality of life, which does not return to normal even after 2 years [14]. |
| There are various modalities of pain relief for rib fracture. Out of them epidural analgesia is considered best analgesic technique, whereas the continuous para-vertebral block provides effective analgesia for unilateral rib fracture [8,15,16]. Both were effective managing the pain well, but for the time period the catheter is in place, i.e., for a week only. |
| Continuous intercostal block provides better pain control, improves pulmonary function and also decreases the length of hospital stay [8]. Continuous intrapleural analgesia with local anesthetics is also useful for patients with unilateral multiple rib fractures, provided that there is no pulmonary contusions or concomitant injuries [17]. In our patient, we could not use it as there was underlying atelectesis and hemothorax. |
| Lignocaine patches are also useful in reducing pain from rib fractures, but in our patient we could not use as it is not available and the number of ribs fractures are high, requiring more patches leading to toxicity [18]. The transdermal fentanyl patch has also been found to be effective in the management of pain from multiple rib fractures, but in our patient we did not try as there was partial relief with morphine PCA [19]. Intercostal nerve radiofrequency ablation has also been used to treat the chronic pain arising out of rib fracture [20]. Intercostal neurolysis has been used for pain arising out of involvement of ribs by metastasis and intra-operatively to prevent post-thoractomy pain [21-25]. |
| The intercostal nerve block was also found to provide excellent pain relief, but the effects were found to be short lived only [26]. |
| To prevent the toxicity from local anesthetics, we have used 1 ml of 1% lignocaine for the diagnostic block at each level, up to a total of 10 ml plus 5 ml for local infiltration. The final dose of local anesthetic was 157.5 mg, which is much less than the maximum dose of 300 mg or (4.5 mg/kg body weight for a 65 kg patient) 292.5 mg. Also taken into the consideration that the intercostal nerve block leads to a very high plasma concentration, the dose is still acceptable [27]. For the therapeutic block, we have used 22.5 ml of 0.25% bupivacaine (1.5 ml of 50% alcohol in 0.25% bupivacaine) plus 5 ml of lignocaine 1% solution for skin infiltration and another 6 ml of 1% lignocaine which was given to control the severe pain arising out of intercostal neurolysis at some levels, which lower than the maximum recommended dose [27]. |
| Another issue that we faced that while doing a procedure at multiple levels, the chances of failure and incidences of complications are high at one or two levels. But in our patient, both the diagnostic block and the therapeutic neurolysis were successful, and there were no immediate and delayed complications. The high success rate and no complication may be attributed to the use of USG for the procedure as Bhatia et al. also found that with the use of USG, the intercostal blocks are more accurate and requires less medications as compared to landmark technique [28]. USG has been showed to improve the performance of upper and lower extremity blocks by decreasing the time required for block, the number of needle punctures, local anesthetic requirement, onset time of sensory block and finally improving the quality of block and overall success [29,30]. Also the use of USG has improved the efficacy of nerve blocks as compared to neurostimulation technique [31]. Finally, and most importantly the use of color Doppler feature in USG has helped us to prevent the possible intra-vascular injection [32]. |
| In the literature, a few complications of the intercostal nerve block have been reported, of which pneumothorax had occurred in 14 patients out of 161 patients undergoing intercostal nerve block in a study by Shanti et al. [33]. |
| But interestingly, there was a recent case report, in which a spinal cord injury had occurred with USG guided ICN with alcohol, but this patient had also received a epidural steroid injection at the same time, so the injury may not be due to ICN injection [21]. Also in this case the concentration of alcohol was 99.9% and the volume was 2 ml, and in our case we have used less volume and less concentrated alcohol (2 ml of 50% alcohol), and in our case the procedure was done in awake state and with the patient communicating with the anaesthesiologist throughout the procedure, and the epidural and paravertebral spread was also prevented by the real time visualisation of the spread of drug by the use of USG. |
| In earlier times, when the ICN was given under landmark technique, there may be chances that it may spread to the epidural or paravertebral spaces. However with the use of fluoroscopy and USG, the spread of the drug can be visualised, thereby avoiding complications. However, it proves that spinal cord injury can be decreased with fluoroscopy and USG, but cannot be eliminated. |
| There had been three case reports of spinal cord injury after phenol neurolysis of intercostal nerve. In all the three patients, the fluoroscopy was used and the amount of solution injected was 3, 6 and >6.5 ml respectively. In two cases it was 6 cm lateral to midline and in one patient; it was 3-4 cm lateral to midline [22-24]. In our case, we used only 2 ml of the neurolytic solution and have given the intercostal block more lateral to the spine. |
| There was spread of drugs into the paravertebral space in 90% of cases with USG guided ICN injection was done near to spine [34-36]. So, it was advised be done away from the spine along the midaxillary line to prevent the spread [35,36]. In our patient, we did it along the posterior axillary line to prevent this spread, but in the upper intercostal spaces we had to do it near the spine due to presence of scapulae, but the spread of medications was well observed by the USG and no paravertebral spread was observed at any of the levels in both the diagnostic and therapeutic block. |
| The effect of the block was long lasting till 6 months, with no pain over the ribs till 6 months even on active movement. |
| Conclusion |
| This case report highlights the importance of intercostal neurolysis for providing the long term relief of severe uncontrolled pain arising out of rib fracture, and the utility of ultrasonography in improving the performance of the block and eliminating the complications. |
References
- Bulger EM, Arneson MA, Mock CN, Jurkovich GJ (2000) Rib fractures in the elderly. J Trauma 48: 1040-1046.
- Lee RB, Bass SM, Morris Jr JA, MacKenzie EJ (1990) Three or more rib fractures as an indicator for transfer to a Level I trauma center: a population-based study. J Trauma-Injury Infect Crit Care 30:689-694
- Yeh DD, Kutcher ME, Knudson MM, Tang JF (2012) Epidural analgesia for blunt thoracic injury--which patients benefit most? Injury 43: 1667-1671.
- Easter A (2001) Management of patients with multiple rib fractures. Am J Crit Care 10: 320-327.
- Bayouth L, Safcsak K, Cheatham ML, Smith CP, Birrer KL, et al. (2013) Early intravenous ibuprofen decreases narcotic requirement and length of stay after traumatic rib fracture. Am Surg 79: 1207-1212.
- Gage A, Rivara F, Wang J, Jurkovich GJ, Arbabi S (2014) The effect of epidural placement in patients after blunt thoracic trauma. J Trauma Acute Care Surg 76: 39-45.
- Wisner DH (1990) A stepwise logistic regression analysis of factors affecting morbidity and mortality after thoracic trauma: effect of epidural analgesia. J Trauma. 30: 799-804.
- Truitt MS, Murry J, Amos J, Lorenzo M, Mangram A, et al. (2011) Continuous intercostal nerve blockade for rib fractures: ready for primetime? J Trauma 71: 1548-1552.
- Karmakar MK, Critchley LA, Ho AM, Gin T, Lee TW, et al. (2003) Continuous thoracic paravertebral infusion of bupivacaine for pain management in patients with multiple fractured ribs. Chest 123: 424-431.
- Mohta M, Verma P, Saxena AK, Sethi AK, Tyagi A, Girotra G (2009) Prospective, randomized comparison of continuous thoracic epidural and thoracic paravertebral infusion in patients with unilateral multiple fractured ribs–a pilot study. J Trauma 66: 1096-1101.
- Nirula R, Mayberry JC (2010) Rib fracture fixation: controversies and technical challenges. Am Surg 76: 793-802.
- Gordy S, Fabricant L, Ham B, Mullins R, Mayberry J (2014) The contribution of rib fractures to chronic pain and disability. Am J Surg 207: 659-662.
- Fabricant L, Ham B, Mullins R, Mayberry J (2013) Prolonged pain and disability are common after rib fractures. Am J Surg 205: 511-515.
- Marasco S, Lee G, Summerhayes R, Fitzgerald M, Bailey M (2015) Quality of life after major trauma with multiple rib fractures. Injury 46: 61-65.
- Carrier FM, Turgeon AF, Nicole PC, Trépanier CA, Fergusson DA, et al. (2009) Effect of epidural analgesia in patients with traumatic rib fractures: a systematic review and meta-analysis of randomized controlled trials. Can J Anaesth 56: 230-242.
- Duch P, Møller MH (2015) Epidural analgesia in patients with traumatic rib fractures: a systematic review of randomised controlled trials. Acta Anaesthesiol Scand 59: 698-709.
- Wulf H, Jeckström W, Maier C, Winckler K (1991) [Intrapleural catheter analgesia in patients with multiple rib fractures]. Anaesthesist 40: 19-24.
- Zink KA, Mayberry JC, Peck EG, Schreiber MA (2011) Lidocaine patches reduce pain in trauma patients with rib fractures. Am Surg 77: 438-442.
- Solak O, Oz G, Kokulu S, Solak O, Dogan G, et al. (2013) The effectiveness of transdermal opioid in the management multiple rib fractures: randomized clinical trial. Balkan Med J 30: 277-281.
- Engel AJ (2012) Utility of Intercostal Nerve Conventional Thermal Radiofrequency Ablations in the Injured Worker after Blunt Trauma. Pain Physician 15:E711-78.
- Kim BH, No MY, Han SJ, Park CH, Kim JH (2015) Paraplegia following intercostal nerve neurolysis with alcohol and thoracic epidural injection in lung cancer patient. Korean J Pain 28: 148-152.
- Gollapalli L, Muppuri R (2014) Paraplegia after intercostal neurolysis with phenol. J Pain Res 7: 665-668.
- Kissoon NR, Graff-Radford J, Watson JC, Laughin RS (2014) Spinal cord injury from fluoroscopically guided intercostal blocks with phenol. Pain Physician 17: E219-224.
- Kowalewski R, Schurch B, Hodler J, Borgeat A (2002) Persistent paraplegia after an aqueous 7.5% phenol solution to the anterior motor root for intercostal neurolysis: a case report. Arch Phys Med Rehabil 83: 283-285.
- Miliauskas P, Cicenas S, Tikuisis R, Zurauskas A, Piscikas D, et al. (2004) [Intercostal nerve blockade with alcohol during operation for postthoracotomy pain]. Medicina (Kaunas) 40 Suppl 1: 127-130.
- Hwang EG, Lee Y (2014) Effectiveness of intercostal nerve block for management of pain in rib fracture patients. J Exerc Rehabil 10: 241-244.
- Amazon, TextbookRegionalAnesthesiaAcuteManagement
- Bhatia A, Gofeld M, Ganapathy S, Hanlon J, Johnson M (2013) Comparison of anatomic landmarks and ultrasound guidance for intercostal nerve injections in cadavers. Reg Anesth Pain Med 38: 503-507.
- Choi S, McCartney CJ (2014) Evidence Base for the Use of Ultrasound for Upper Extremity Blocks: 2014 Update. Reg Anesth Pain Med.
- Salinas FV (2010) Ultrasound and review of evidence for lower extremity peripheral nerve blocks. Reg Anesth Pain Med 35: S16-25.
- Abrahams MS, Aziz MF, Fu RF, Horn JL (2009) Ultrasound guidance compared with electrical neurostimulation for peripheral nerve block: a systematic review and meta-analysis of randomized controlled trials. Br J Anaesth 102:408-417.
- Hahn C, Nagdev A (2014) Color Doppler ultrasound-guided supraclavicular brachial plexus block to prevent vascular injection. West J Emerg Med 15: 703-705.
- Shanti CM, Carlin AM, Tyburski JG (2001) Incidence of pneumothorax from intercostal nerve block for analgesia in rib fractures. J Trauma 51: 536-539.
- Paraskeuopoulos T, Saranteas T, Kouladouros K, Krepi H, Nakou M, et al. (2010) Thoracic paravertebral spread using two different ultrasound-guided intercostal injection techniques in human cadavers. Clin Anat 23:840-847.
- Scott DB (1995) Techniques of Regional Anesthesia. (2ndedn) Norwalk, CT: Appleton and Lange.
- Kreuscher H (1994) Regionale Schmerztherapie. Regionalana¨sthesie, Lokalana¨sthesie, Regionale Schmerztherapie. Stuttgart, Germany: Georg Thieme: 709-761.
Figures at a glance
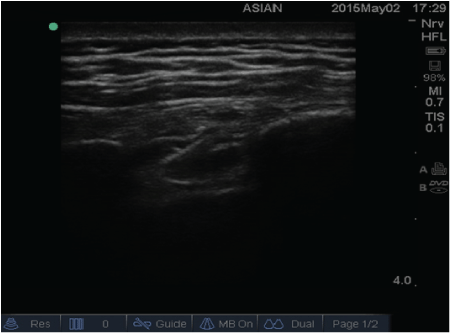 |
| Figure 1 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 13682
- [From(publication date):
January-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 12631
- PDF downloads : 1051
