Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
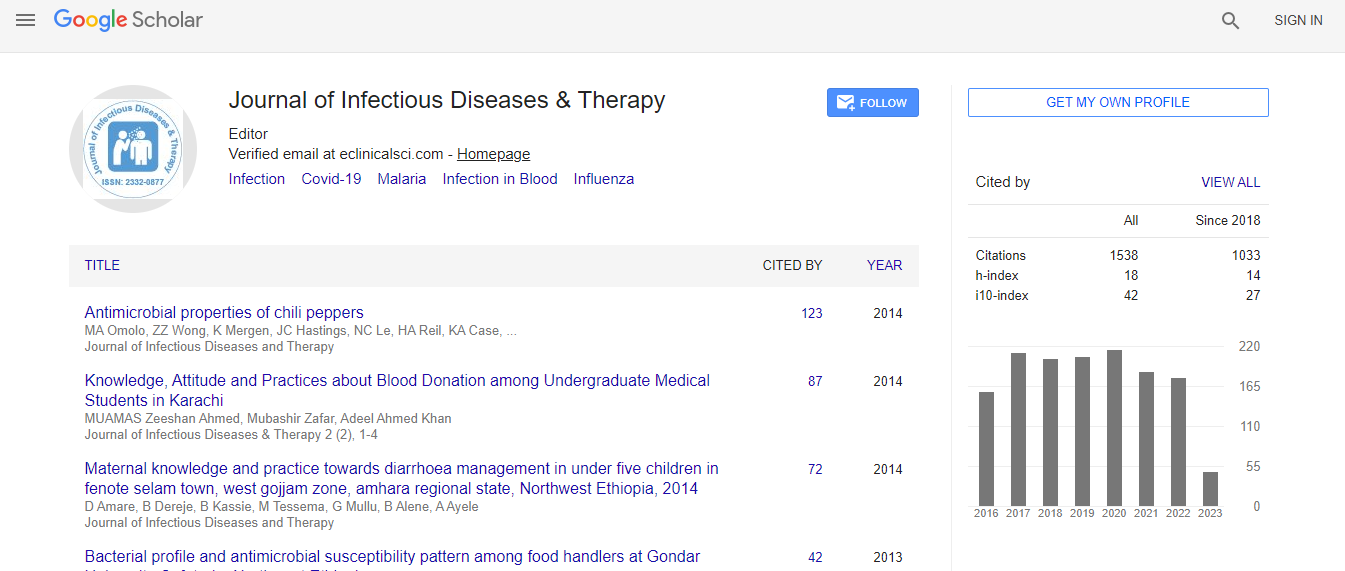
Google Scholar citation report
Citations : 1529
Journal of Infectious Diseases & Therapy received 1529 citations as per Google Scholar report
Indexed In
- Index Copernicus
- Google Scholar
- Open J Gate
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- Publons
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Digestive tract diseases and infections
3rd Annual Congress on Infectious Diseases
Eugenie Bergogne Berezin
Bichat-Claude Bernard Hospital-Paris University, France
Keynote: J Infect Dis Ther
Abstract
Human digestive tract (DT) is one of the most vulnerable organs to microbial aggressions. A natural bacterial flora in the DT is a source of maturation of immune systems: Lactobacilli, Bifidobacterium lactis contribute to children growth. Normal adult intestinal flora includes Enterobacteriaceae, Escherichia coli, Proteus spp., and anaerobes, as contributors to digestive tract functions. In adults who suffered of recurrent gastric pain, the discovery of Helicobacter pylori, Gram negative micro-aerophilic, helix-shaped organism, has been shown as responsible for gastric ulcer, Malt lymphoma, adeno-carcinoma: living in acidic areas, (upper digestive tract, 50% of elderly), treatment omeprazole+ clarithromycin has proven efficacy. Lower intestinal tract can be invaded by species responsible for diarrhea, contagious, of variable severity: Shigella, Salmonella spp, Vibrio cholerae: in countries with poor hygiene, cholera epidemics often occur. Yersinia enterocolitica, Y.pseudotuberculosis carried by pigs and contaminant to humans, determine sporadic acute gastro-enteritis, (contact with animals, contaminated food). Intestinal infections should not be treated with antibiotics systematically, as in some cases they result in aggravation, emergence of Clostridium difficile. The presence in intestinal flora of Escherichia coli resistant to �?²-lactams is a threat for treatment failure. E. coli resistant to �?²-lactams and carriage of genes of resistance became international problems. In ICU patients, disorganized flora occurs whatever treatment used: pathogenic MDR are often isolated. To re-establish equilibrium with a â�?�?normal â�?�?floraâ�?, the development of â�?�?Fecal Microbiota Transplantâ�? becomes extensively used ( in pills or tablets). Another option has been successful using living organisms (â�?�?probioticsâ�?) such as fungi (Saccharomyces spp., S.boulardii sp.) can control ICU diarrhea.Biography
Eugénie Bergogne-Bérézin is Professor of Clinical Microbiology at the University Paris 7. She is Doctor in Medicine (MD and PhD), specialized in Microbiology- Infectious Diseases. She has developed.several fields of Research: 1-Acinetobacter spp as a nosocomial pathogen (epidemiology, resistance, infections); 2-Pharmacology of antibiotics tissue and body fluid distribution Pharmacodynamics of Antibiotics -3 Intestinal microbial Ecology, jejunal flora, bacterial adhesion to intestinal mucosa, impact of antibiotic therapy on intestinal flora. .She has published ~200 International Articles, 6 Medical Books, she contributed to Chapters in recent International Books of Infectious Diseases (Mosby), Pneumology (Respiratory Infection, James Pennington Ed, Raven Press), Antimicrobial Therapy (Victor Yu). She continues to work on Acinetobacter at an International level.

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi