Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
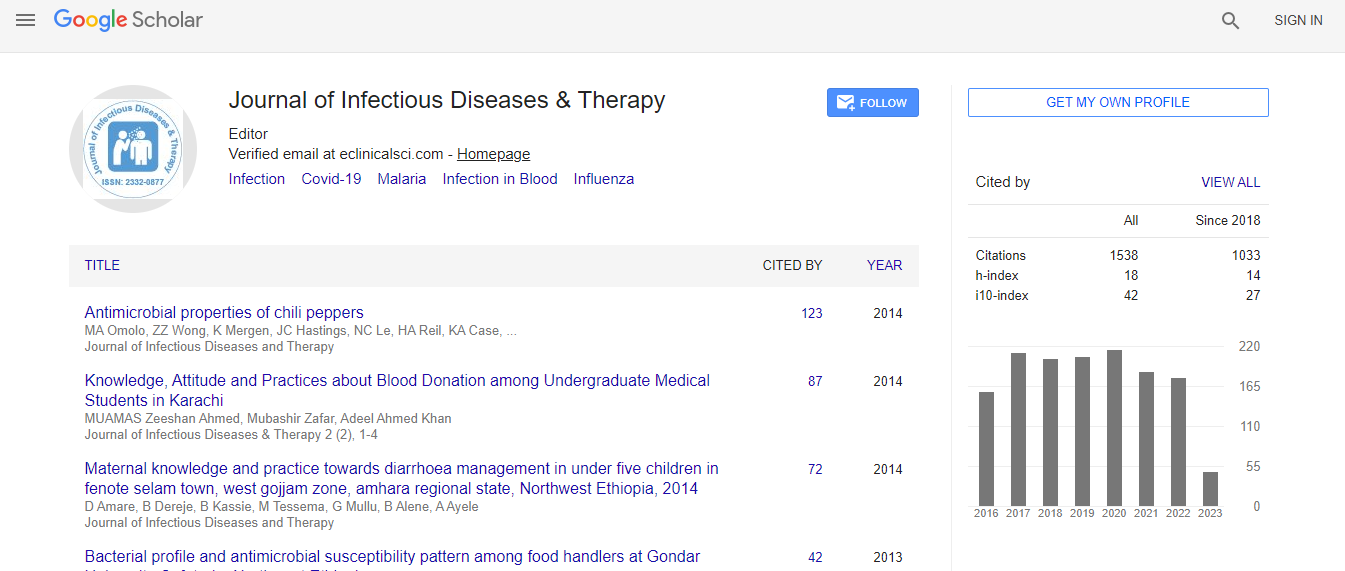
Google Scholar citation report
Citations : 1529
Journal of Infectious Diseases & Therapy received 1529 citations as per Google Scholar report
Indexed In
- Index Copernicus
- Google Scholar
- Open J Gate
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- Publons
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
Significance of polymerase chain reaction (PCR) analysis of vitreous humor in an immunocompromised patient with necrotizing retinochoroiditis
Joint Event on 2nd World Congress on Infectious Diseases & International Conference on Pediatric Care & Pediatric Infectious Diseases
Gabriela Sanchez Petitto, Astrid Serauto, Min Ji Kwak and Gabriel Aisenberg
University of Texas Health Science Center at Houston, USA
Posters & Accepted Abstracts: J Infect Dis Ther
Abstract
A 36-year-old woman with newly diagnosed nephrotic syndrome presented with a 10-day history of progressive vision loss. On ophthalmological exam, visual acuity was 20/800 in both eyes. The left eye showed grade 4 disc edema and both retina had vitreous and intraretinal hemorrhages. HIV serology was positive, CD4 count of 17/ul and viral load of 375000 copies/ml, newly diagnosed. CT head was normal. Cerebrospinal fluid analysis is unremarkable. Serum and CSF immunoglobulins against Toxoplasma spp., PCR for herpes simplex virus 1 and 2, varicella-zoster (VZV) and Cytomegalovirus (CMV) were negative. Empirical ganciclovir, trimethoprim-sulfamethoxazole and prednisolone were started. Vitreal fluid extracted by paracentesis was positive for toxoplasma antigen and negative for CMV and VZV in both eyes. The diagnosis of toxoplasma retinochoroiditis was confirmed. The patient continued a 6-week course of antibiotics with clinical improvement at 4 weeks. In immunocompromised patients is difficult to establish a diagnosis of ocular toxoplasmosis based upon the lesions��? appearance, since atypical lesions are common and obtaining reliable results for immunodiagnostic assays is more difficult. The best clue to diagnosis is recognition of the clinical presentation and the detection of the agent in ocular samples by molecular biology. Confirmation of diagnosis is higher for PCR of vitreous samples compared to aqueous humor; this due to the fact that, anatomically the vitreous humor is closest to the necrotic lesions, leading to a better sampling of the parasitic DNA. In summary, a positive PCR study for T. gondii became a dependable alternative to diagnose retinochoroiditis in an immunocompromised patient.Biography
Gabriela Sanchez Petitto has completed her MD from the Universidad Central de Venezuela, School of Medicine. She is currently a Postgraduate student of Internal Medicine at the University of Texas Health Science Center at Houston. She has worked in several projects with hematological malignancies and in the upcoming future with antibiotic resistance projects.

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi