Our Group organises 3000+ Global Conferenceseries Events every year across USA, Europe & Asia with support from 1000 more scientific Societies and Publishes 700+ Open Access Journals which contains over 50000 eminent personalities, reputed scientists as editorial board members.
Open Access Journals gaining more Readers and Citations
700 Journals and 15,000,000 Readers Each Journal is getting 25,000+ Readers
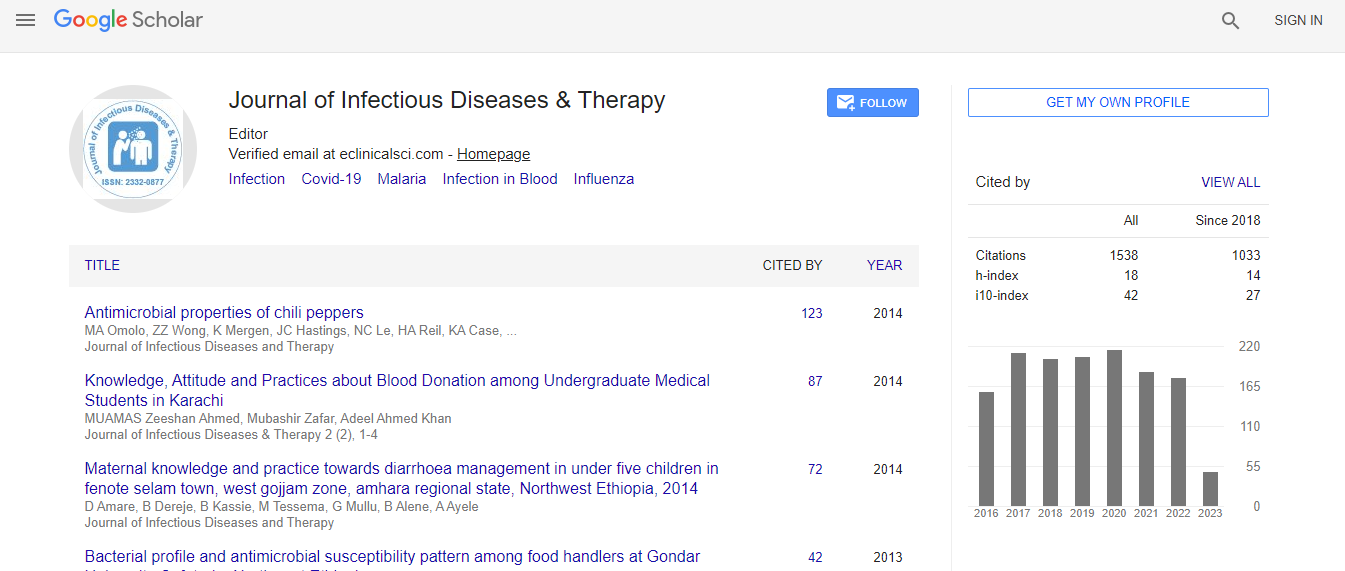
Google Scholar citation report
Citations : 1529
Journal of Infectious Diseases & Therapy received 1529 citations as per Google Scholar report
Indexed In
- Index Copernicus
- Google Scholar
- Open J Gate
- RefSeek
- Hamdard University
- EBSCO A-Z
- OCLC- WorldCat
- Publons
- Euro Pub
- ICMJE
Useful Links
Recommended Journals
Related Subjects
Share This Page
The need for surveillance-A snapshot of antimicrobial resistance of gram-negative isolates in Australian children with culture-proven bloodstream infections
4th International Congress on Infectious Diseases
Shakif Mohammad Shakur, John Whitehall and Poonam Mudgil
Western Sydney University, Australia
Posters & Accepted Abstracts: J Infect Dis Ther
Abstract
Gram-negative bloodstream infections cause significant morbidity and mortality of children worldwide. Rising rates of bacterial resistance emphasizes the need for monitoring of causative organisms and their susceptibility patterns, to guide appropriate antibiotic therapy. Antimicrobial resistance is an important public health issue and thus, monitoring of local populations is warranted. We investigated cases of proven bacteraemia from infected children from a socio-economically disadvantage population. We retrospectively reviewed the cohort of children aged 0 to 16 years who were admitted to a metropolitan hospital in Sydney, Australia, from January 1, 2010 to August 31, 2014 inclusive, and whose blood cultures isolated gram-negative organisms. Data was collected regarding patient demographics, species of bacteria isolated, antimicrobial susceptibility of these isolates, and clinical outcomes. We identified a total of 35 isolates from 33 patients, of whom 45% were aged <12 months. The most common gram-negative isolate was Escherichia coli (42%), followed by Salmonella spp. (12%) and Neisseria meningitidis (12%). The most common primary site of infection was the urinary tract, accounting for 33% of patients. Escherichia coli showed high rates of resistance to ampicillin (43%), trimethoprim (36%) and co-trimoxazole (41%). The majority of Escherichia coli isolates were susceptible to amoxicillin/clavulanate (81%) and all isolates tested against ceftriaxone and gentamicin was susceptible. Most other isolates showed >90% susceptibility to common antimicrobial agents. In this single-centre study, we have drawn attention to a high rate of resistance of Escherichia coli bacteria to common antimicrobial agents. This highlights the importance of ongoing surveillance of local populations, and may warrant changes to empirical antibiotic treatment in the near future.Biography
Shakif Mohammad Shakur has completed his Bachelor of Medicine/Bachelor of Surgery at Western Sydney University, Australia. Currently, he is a Junior Medical Officer at Campbelltown Hospital, a 300 bed hospital located at South Western Sydney, New South Wales, Australia.
Email: shakif_shakur@live.com

 Spanish
Spanish  Chinese
Chinese  Russian
Russian  German
German  French
French  Japanese
Japanese  Portuguese
Portuguese  Hindi
Hindi