Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
A 20-Year-Old Woman with Stenosis and Dilations of the Biliary Tree
| Irene Franceschet1, Nora Cazzagon1, Raffaella Motta2 and Annarosa Floreani1* | |
| 1Department of Surgery, Oncology and Gastroenterology, University of Padova, Padova, Italy | |
| 2Department of Medicine, University of Padova, Padova, Italy | |
| *Corresponding Author : | Annarosa Floreani Department of Surgery Oncology and Gastroenterology Padova, Italy Tel: 390498212894 Fax: 390498760820 E-mail: annarosa.floreani@unipd.it |
| Received October 01, 2015; Accepted January 02, 2016; Published January 07, 2016 | |
| Citation: Franceschet I, Cazzagon N, Motta R, Floreani A (2016) A 20-Year-Old Woman with Stenosis and Dilations of the Biliary Tree. J Neuroinfect Dis 7:196.doi:10.4172/2314-7326.1000196 | |
| Copyright: © 2016 Franceschet I, et al. This is an open-access article distributed nder the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Neuroinfectious Diseases
| Keywords |
| Primary sclerosing cholangitis; Magnetic resonance imaging |
| Case Report |
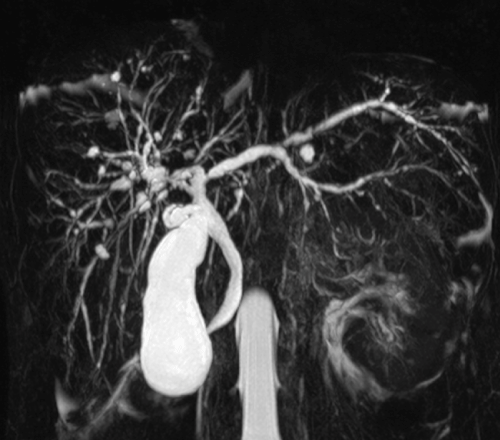
| A 20-year-old woman presented with epigastric pain and jaundice. Physical examination revealed mild icteric sclera and normal liver and spleen. Biochemical tests were as follows: normal blood count, alanine aminotransferase 191 U/l, gamma-glutamyltransferase 149 U/l, alkaline phosphatase 252 U/l, total bilirubin 5.6 mg/dl (5.0 conjugated), normal renal function tests. Viral markers for hepatitis A, B, C, Epstein Barr, HIV, CMV were negative, and the immunological profile was normal. She reported occasional alcohol consumption and sporadic cigarette smoking habits. She was not taking medication, but reported an assumption of Levonorgestrel (750 mcg) after a sexual intercourse 2 weeks before. Abdominal ultrasound showed dilatation of intrahepatic biliary ducts; a nuclear magnetic resonance cholangiography (MRC) showed enlarged liver with focal inflammatory areas, splenomegaly, intrahepatic biliary tree enlargement with irregular profiles and marked stenosis alternated to dilatations and cystis; the common hepatic duct was mild dilated without stenosis, compatible with primary sclerosing cholangitis (PSC) (Figure 1). An inflammatory bowel disease was ruled out by a colonoscopy. The patient was treated with standard dose of ursodeoxycholic acid, followed by a gradual normalization of liver function tests. A MRC performed after 2 months revealed a normal biliary tree with disappearance of the biliary changes (Figure 2). |
| The total disappearance of the cholangiographic abnormalities suggests a secondary form of sclerosing cholangitis (SSC). SSC is a rare condition determined by a variety of causes including post-traumatic or surgery conditions, ischemia, cholelithiasis/choledocolithiasis, haematologic conditions (eosinophilic and mast-cell abnormalities), hepatic inflammatory pseudotumor, AIDS, infectious conditions (recurrent pyogenic cholangitis), infiltrative disorders, metastasis, congenital hepatic diseases [1]. Among the SSC only the eosinophilic cholangitis has been reported to have a complete regression of the biliary abnormalities, particularly after steroid treatment [2]. |
| The unique risk factor for hepatic damage in the patient was the consumption of Levonorgestrel. Drug-induced liver injury may be characterized by a cholestatic pattern with biochemical alterations in absence of morphological abnormalities of the biliary tree. Recently, 8 cases of drug-induced liver disease with biliary abnormalities at the MRC have been reported [3]. |
| Anecdotal cases of low dose levonorgestrel/ethinylestradiol hepatotoxicity have been reported in young females taking pill as anti-contraceptive [4,5]. In these cases liver biopsy showed sinusoidal dilatation or focal necrosis in peri- and centrolobular area, and liver damage resolved after pill discontinuation. In 2 cases endoscopic retrograde cholangiogram showed normal biliary tree. |
| These evidences suggest a possible role of emergency contraception with Levonorgestrel in cholestatic liver injury. Usually a cholestatic toxicity due to a drug-induced liver injury is characterized by biochemical alterations in absence of morphological abnormalities. Our case report is relevant because for the first time we pinpointed the link between Levonorgestrel and biliary tree alterations which had a complete regression after the drug discontinuation. |
References
- Abdalian R, Heathcote EJ (2006) Sclerosing cholangitis: a focus on secondary causes. Hepatology 44:1063-1074.
- Miura F, Asano T, Amano H, Yoshida M, Toyota N, et al. (2009) Resected case of eosinophiliccholangiopathy presenting with secondary sclerosing cholangitis. World J Gastroenterol 15:1394-1397.
- Gudnason H, Björnsson HK, Gardarsdottir M, Olafsson S, Bergmann O, et al. (2015) Secondary sclerosing cholangitis in patients with drug induced liver injury. Dig Liver Dis 47: 502-507.
- Elouni B, Ben Salem C, Zamy M,Ganne N, Beaugrand M, et al.(2010) Cytolytic hepatitis possibly related to levonorgestrel/ethinylestradiol oral contraceptive use: 2 case reports. Ann Pharmacother 44:2035-2037.
- Tierney S, Nakeeb A, Wong O, Lipsett PA, Sostre S, et al. (1999) Progesterone alters biliary flow dynamics. Ann Surg 229:205-209.
Figures at a glance
 |
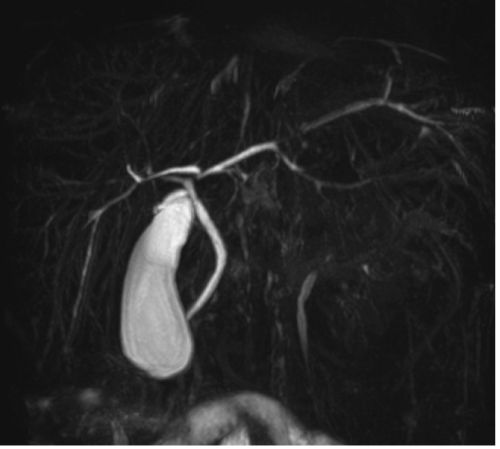 |
| Figure 1 | Figure 2 |
Post your comment
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 10539
- [From(publication date):
March-2016 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 9546
- PDF downloads : 993
