Case Report Open Access
Case of Cerebral Hydatid Cyst, Rare Parasitic Brain Infection Presenting as Refractory Epilepsy
| Arif Hussain Sarmast*, Humam Nisar Tank, Nayil Khursheed Malik, Basharat Mujtaba and Abrar Ahad Wani | |
| Department of Neurosurgery, Sher I Kashmir Institute of Medical Sciences, Srinagar, India | |
| Corresponding Author : | Arif Hussain Sarmast Dalipora kawadara, Srinagar Kashmir, 190002, India Tel: 91 9906859742 E-mail: arifhsarmast@gmail.com |
| Received: July 18, 2015 Accepted: July 18, 2015 Published: July 22, 2015 | |
| Citation: Sarmast AH, Tank HN, Malik NK, Mujtaba B, Ahad Wani A (2015) Case of Cerebral Hydatid Cyst, Rare Parasitic Brain Infection Presenting as Refractory Epilepsy. J Neuroinfect Dis 6:180. doi:10.4172/2314-7326.1000180 | |
| Copyright: © 2015 Sarmast AH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Cystic hydatidosis is a rare disease which mainly involves the liver and lungs, and rarely the brain. Cysts may be single or multiple. Usually neurohydatidosis with features of raised intracranial pressure such as headache and nausea vomiting or focal neuro-deficits but rarely as refractory epilepsy. We had a 10 year old boy presenting with refractory epilepsy without any focal localizing neurological signs. Brain imaging revealed a huge cystic structure involving the left side of the brain. A diagnosis of brain hydatid cyst was made and the patient was operated on. A large cyst was successfully delivered without rupture. Antihelminthic medication was started and the patient was discharged with no new seizure episodes during 6 month follow up. Hydatid cysts must not be overlooked as a differential diagnosis in children with cystic brain lesions. Surgery is the standard method of treatment, and it is vital to recover the cyst without rupture to avoid severe complications and recurrence.
| Keywords |
| Hydatid cyst brain; Refractory epilepsy; Anti-helmenthic drugs |
| Introduction |
| Hydatid disease is caused by the infestation of the larvae of taenia Echinococcus granulosus. Although it is an uncommon parasitic infestation but in our part of world it is not that rare as most of the population is concentrated in rural areas and people are fond of rearing sheep and canines which form important links in life cycle of echinoccous. They are usually (about 50-75%) seen in children and young adults [1-3]. The liver is the most common organ involved (77%), followed by the lungs (43%) [4-7]. 2% cases of Hydatid cysts have been reported in the brain [1,2,8]. Surgical excision of cyst is the treatment of choice, combined with antihelminthic drugs [2,5]. Careful removal of the lesion without spillage is very important; otherwise fatal complications like anaphylactic shock are inevitable [9]. |
| We describe the case of a 10 year old boy who came to our department with refractory epilepsy. However he was neglected and poorly evaluated previously and was empirically treated with combinations of antiepileptics but was never seizure free before definitive surgery. The main purpose of this study is to demonstrate the unusual symptoms of the patient and the terrible nature of the operated cyst, which was fully resected without rupture. |
| Case Illustration |
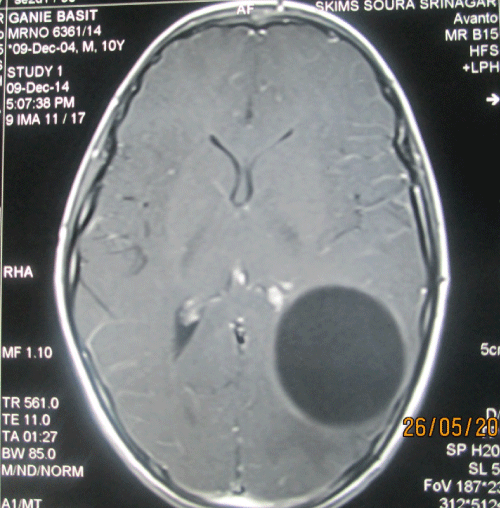
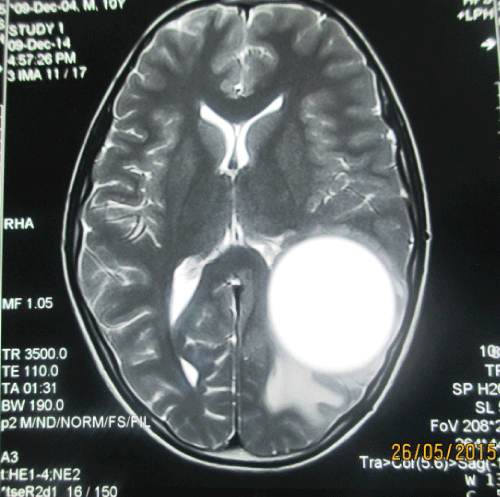
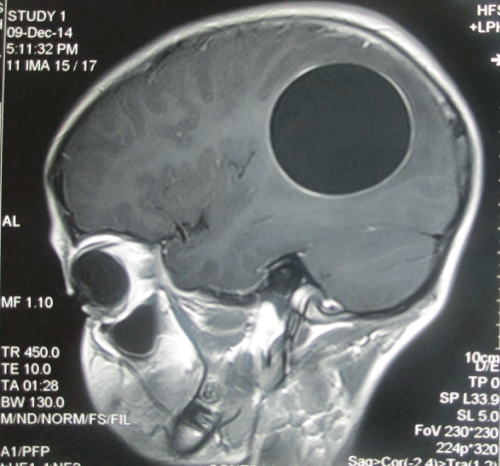
| A young 10 year old boy, from the family of nomadic shepherds presented to neurosurgery OPD with history of seizure disorder. The seizures were initially focal followed by generalized, no EEG records were however available. He was treated with different combinations of anti epileptics over the period of two years but was not responding to treatment and had frequent seizure episodes. However he did not have any history of headaches, nausea/vomiting, or any focal neurodeficit. His vital signs were normal and his Glasgow Coma Scale (GCS) was 15. Neurological examination was grossly normal. Laboratory data showed mild leucocytosis with rise in eosinophils. The enzyme-linked immunosorbent assay (ELISA) for hydatid cysts was negative. Plain chest X-ray and ultrasound scan of the abdomen and pelvis were also normal. Brain MRI of the patient demonstrated a single large, spherical, well-defined, thin-walled homogenous cyst in left posterior parietal area, with signal intensity similar to that of cerebrospinal fluid (CSF), and a wall which did not show enhancement and no edema (Figures 1-3). After summation of all the above data, the diagnosis of a hydatid cyst was made and a right temporoparietal craniotomy was performed. A large cystic structure (10×10×8 cm) was delivered with utmost care to avoid rupture and spillage. The cyst appeared creamy and smooth. A hydatid cyst was confirmed by pathology reports. A post-operative CT scan showed a large space without any residual matter (Figure 4) Postoperatively, albendazole 15 mg/kg/day was started in and continued for 8 weeks. The patient had uneventful post-operative period and was put on oral phenytoin sodium (5 mg/kg/day in divided doses) and was discharged after one week with close follow-up. Upto 6 months of follow up patient showed no signs of recurrence and no new seizure episodes. |
| Discussion |
| Intracranial hydatid disease is rare, with reported incidence of 1-2% of all cases with hydatid disease [10-12]. Hydatid disease is endemic in the middle east, Mediterranean countries, South America, North Africa and Australia [12]. In India it is seen in Andhra Pradesh, Tamil Nadu, Punjab and Jammu & Kashmir [13]. Cerebral hydatid disease is more common in paediatric population [13,14] as in our case also the patient as a young 10 year old boy. |
| The definite hosts of echinococcus are various carnivores, the common being the dog. All mammals (commonly sheep and cattle) are intermittent hosts. Humans are accidental hosts and get infected through the faeco-oral route by ingestion of food or milk contaminated by dog faeces containing ova of the parasite or by direct contact with dogs. After ingestion of eggs by man the eggs loose their enveloping layer in the stomach and release the embryos. The embryos pass through the wall of the gut into the portal system and are carried to the liver where most larvae get entrapped and encysted. Some may reach the lungs and occasionally, some may pass through the capillary filter of the liver and lungs and get entry into the systemic circulation. Through hematogenous root they may get lodged at various sites like brain throughout the body. The wall of the cyst consists of an inner endocyst (germinal layer) and outer ectocyst (laminated layer). The host reacts to the cyst forming a pericyst (fibrous capsule), which provides nutrients to the parasite. In the brain, due to minimal reaction, the pericyst is very thin. The endocyst produce scolices which bud into the cyst cavity and may sediment within the hydatid cavity, commonly known as hydatid sand [8,15]. |
| Hydatid cysts have been reported in the brain (2%) [1,2,4,5,8] heart (2%) [5,7] kidneys (2%) [6,7] orbit (1%) [16,17] spinal cord (1%) [8,18] spleen, 1 spine [5,8] spermatic cord [19] and soft tissues [5]. In our case the child belonged to the nomadic tribe of gujjar-bakarwals in whom hydatid cyst disease has highest prevalence. The reason being that they are a tribe of nomadic shepherds who rear sheep and cattle along with dogs in almost every family. Hence all the risk factors for catching the infection were present in the patient. |
| Brain hydatid cysts can be primary (single) or secondary (multiple) [1,2,4,8,20]. Secondaries are thought to arise from the multiple scolices released from the left side of the heart following cyst rupture in the heart [2,14,20] or due to spontaneous, traumatic or surgical rupture of a solitary cranial cyst [2,8]. Cysts are usually found in supratentorial region, middle cerebral artery [1,4] territory being common, similarly in our case also it was a large cyst in temporo-parietal area Other intracranial regions like intraventricular, posterior fossa and the orbit have also been reported [16,17]. |
| Cysts develop insidiously, usually being asymptomatic initially, and present with inconsistent clinical and imaging features [2,3,8]. In most studies the most common presenting symptoms were headache and vomiting [1,2,4,21]. During review of literature, we saw patients reported ataxia, diplopia, hemiparesis, abducens nerve palsy and even coma [2,4,21]. Surprisingly our case also had uncommon presentation of refractory seizure no other symptomatolgy of raised intracranial pressure, headache, nausea, vomiting and diplopia. He was treated with different combinations of antiepileptics namely, phenytoin, phenobarbitone, leviterasetam, clobazam but all the combinations failed to control seizures. It was during evaluation for cause of seizure disorder that patient was detected having hydatid cyst brain. |
| The Casoni and Weinberg tests, indirect haemagglutination, eosinophilia and ELISA are recommended for diagnosis, but as brain tissue evokes minimal response results often tend to be false negatives [2,5,20]. In our case also, serology for hydatid cyst was negative. CT scan and MRI are used frequently in diagnosing the cystic lesions [5,8]. On CT scan, a solitary cyst appears as well-defined, spherical, smooth, thin-walled and homogeneous, with an inner density similar to CSF, and non-enhancing walls [22]. The wall may appear iso-dense to hyperdense on CT scan [5,8], and rarely, may become calcified [22]. There is usually no surrounding brain parenchymal oedema, which if exists along with ring enhancement, indicates inflammation and infection [4,22]. Ring enhancement and peri-lesional oedema are typical features of brain abscesses and cystic neoplasms but not seen in uncomplicated hydatid cysts [5,8]. MRI is superior in demonstrating the cyst rim [2,5,22]. The cyst shows low signal intensity on T1-weighted, and high signal intensity on T2-weighted MRI [20]. MRI is superior in posterior fossa lesions, presence of super-added infections and cystic contents, and also in surgical planning and ruling out other diagnostic possibilities [23]. We also strongly recommend MRI for better evaluation of cystic brain lesions. When only the endocyst ruptures, cyst contents are held by the outer pericyst giving a peculiar water lily sign, which is pathognomic of hydatid disease [5,8]. |
| Treatment of hydatid cyst is primarily based on medical, antihelminthics and surgical excision. Albendazole alone or in combination with other compounds, such as praziquantel, has been reported with favourable results as an adjunct to surgery or as the primary mode of treatment for very small deep seated cysts [20]. It is reported that albendazole results in the disappearance of up to 48% of cysts and reduction in size in 28% [20]. The recommended dose is 10 mg/kg body weight three times a day and duration of the treatment ranges from four weeks or six to eight weeks in some series even upto four months. Surgery is the mainstay for treating intracranial hydatid cysts and the aim is to excise the cysts entirely without rupture, which can otherwise lead to catastrophic events such as anaphylactic shock as [8,20]. The Dowling-Orlando technique remains the preferred method, in which the cyst can be delivered by lowering the head of the operating table and instilling warm saline between the cyst and the surrounding brain [24]. Even minimal spillage can cause devastating effects as surprisingly 1 ml of hydatid sand contains 400,000 scolices [25]. The thin cyst wall, periventricular location (risk of intraventricular rupture and CSF dissemination) and adhesions to the parenchyma are the main difficulties encountered during the surger [26]. The large cavity which remains after the cystic removal can lead to serious complications, such as cortical collapse, hyperpyrexia and brain oedema [2]. Recurrence remains a major concern, which is managed by both antihelminthic chemotherapy and surgery. In a major study 25% of the patients had recurrence, which highlights the need for long term follow up [27]. In present case report, due to the huge size of the cyst and as per our protocol, surgery was performed and post-operatively albendazole was started as an adjunctive therapy for period of 8 weeks along with antiepileptics. Patient was followed for a period of 6 months with clinical evaluations and radiological screening for recurrence but remained asymptomatic, seizure free and had no recurrence till then. Khalatbari et al. [28] have reported a similar case in their institution of a 16-year-old boy with intractable epilepsy for the previous three years despite receiving full doses of three antiepileptic medications. Their patient underwent surgery for calcified left frontal hydatid and on follow up of more than two years required a single antiepileptic drug (phenobarbital). |
| Conclusions |
| Hydatid disease is highly prevalent in nomadic shepherds but due to their lifestyle and poor socio-economic conditions, is often neglected till the lesion assumes an enormous size. We recommend that for treating brain hydatid cyst, the size of the cyst, multiplicity, location and neurological deficit must all be taken into consideration. It is an uncommon but a totally curable disease. |
References
- Erşahin Y, Mutluer S, Güzelbağ E (1993) Intracranialhydatid cysts in children. Neurosurgery 33: 219-224.
- Cavuşoğlu H, Tuncer C, Ozdilmaç A, Aydin Y (2009) Multiple intracranial hydatid cysts in a boy. Turk Neurosurg 19: 203-207.
- Sierra J, Oviedo J, Berthier M, Leiguarda R (1985) Growth rate of secondary hydatid cysts of the brain. Case report. J Neurosurg 62: 781-782.
- Gana R, Skhissi M, Maaqili R, Bellakhdar F (2008) Multiple infected cerebral hydatid cysts. J ClinNeurosci 15: 591-593.
- Andronikou S, Welman CJ, Kader E (2002) Classic and unusual appearances of hydatid disease in children. PediatrRadiol 32: 817-828.
- Afsar H, Yagci N, Aybasti N, Meto S(1994) Hydatid disease of the kidney. Br J Urol 73:17-22.
- Dahniya MH, Hanna RM, Ashebu S, Muhtaseb SA, el-Beltagi A, et al. (2001) The imaging appearances of hydatid disease at some unusual sites. Br J Radiol 74: 283-289.
- Kovoor JM, Thomas RD, Chandrashekhar HS, Jayakumar PN, Pillai S, et al. (2007) Neurohydatidosis. AustralasRadiol 51: 406-411.
- Pearl M, Kotsilimobos DG, Lehrer HZ, Rao AH, Fink H, et al. (1978) Cerebralechinococcosis, a pediatric disease: report of two cases with one successful five-year follow-up. Pediatrics 61: 915-920.
- Sardana VR, Dharker SR, Mittal RS, Nathani R(1991) : Multiple intracranial hydatid cysts. Neurol India 39: 205.
- ErÅŸahin Y, Mutluer S, GüzelbaÄ� E (1993) Intracranialhydatid cysts in children. Neurosurgery 33: 219-224.
- Onal C, Barlas O, Orakdögen M, Hepgül K, Izgi N, et al. (1997) Three unusual cases of intracranial hydatid cyst in the pediatric age group. PediatrNeurosurg 26: 208-213.
- Dharker SR(1996) Hydatid disease. In:Ramamurthi B, Tandon PN (eds.)Text Book of Neurosurgery, Second edition. Churchill Livingstone, New Delhi 535-544.
- Jiménez-Mejías ME, Castillo-Ojeda E, Cuello Contreras JA, García Gutiérrez D, Romero Arce J, et al. (1991) [Cerebral hydatidosis. Analysis of a series of 23 cases]. Med Clin (Barc) 97: 125-132.
- Haliloglu M, Saatci I, Akhan O, Ozmen MN, Besim A (1997) Spectrum of imaging findings in pediatric hydatid disease. AJR Am J Roentgenol 169: 1627-1631.
- Ergün R, Okten AI, Yüksel M, Gül B, Evliyaoğlu C, et al. (1997) Orbital hydatid cysts: report of four cases. Neurosurg Rev 20: 33-37.
- KarakaÅŸ HM, TokoÄŸlu F, Kacar M, Boyacigil S (1997) Retrobulbarhydatid cyst: assessment of two cases. AustralasRadiol 41: 179-180.
- Mazyad MA, Mostafa MM, Morsy TA (1998) Spinal cord hydatid cysts in Egypt. J Egypt SocParasitol 28: 655-658.
- Yurtçu M, Gündüz M, Toy H, Günel E (2007) Spermatic cord hydatid cyst: an unusual localization. J PediatrSurg 42: e15-16.
- Reddy DR (2009) Managing cerebral and cranial hydatid disease. Neurol India 57: 116-118.
- Guzel A, Tatli M, Maciaczyk J, Altinors N (2008) Primary cerebral intraventricularhydatid cyst: a case report and review of the literature. J Child Neurol 23: 585-588.
- Pedrosa I, Saíz A, Arrazola J, Ferreirós J, Pedrosa CS (2000) Hydatid disease: radiologic and pathologic features and complications. Radiographics 20: 795-817.
- El-Shamam O, Amer T, El-Atta MA(2004). Magnetic resonance imaging of simple and infected hydatid cysts of the brain. MagnReson Imaging 22:1339-1340.
- Carrea R, Dowling E Jr, Guevara JA (1975) Surgical treatment of hydatid cysts of the central nervous system in the pediatric age (Dowling's technique). Childs Brain 1: 4-21.
- Anvari M, Amirjamshidi A, Abbassioun K (2009) Gradual and complete delivery of a hydatid cyst of the brain through a single burr hole, a wrong happening! Childs NervSyst 25: 1639-1642.
- Budke CM, Deplazes P, Torgerson PR (2006) Global socioeconomic impact of cystic echinococcosis. Emerg Infect Dis 12: 296-303.
- Ciurea AV, Fountas KN, Coman TC, Machinis TG, Kapsalaki EZ, et al. (2006) Long-term surgical outcome in patients with intracranial hydatid cyst. ActaNeurochir (Wien) 148: 421-426.
- Khalatbari MR, Brunetti E, Shobeiri E, Moharamzad Y (2014) Calcified Mass on Brain CT in a Teenager with Refractory Seizures. Neuroradiol J 27: 691-696.
Figures at a glance
 |
 |
 |
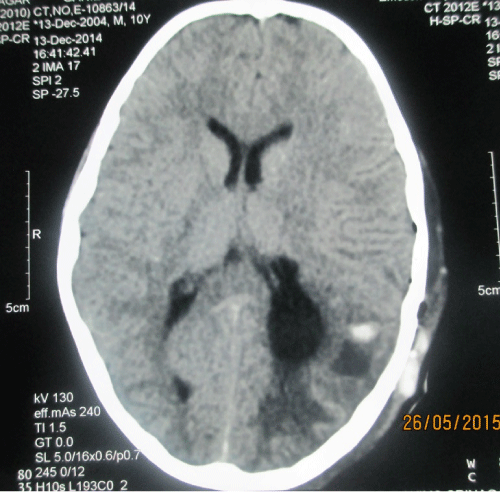 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 15337
- [From(publication date):
August-2015 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 10164
- PDF downloads : 5173
