Research Article Open Access
Changes in Knee Pain, Perceived Need for Surgery, Physical Function and Quality of Life after Dietary Weight Loss in Obese Women Diagnosed with Knee Osteoarthritis
| Kamary Coriolano1*, Alice B Aiken1, Mark M Harrison2, Caroline F Pukall3, Brenda J Brouwer4 and Dianne Groll5 | |
| 1School of Rehabilitation Therapy, Queen’s University, ON, Canada | |
| 2School of Medicine, Queen’s University and Department of Surgery, Kingston General Hospital | |
| 3Department of Psychology, Queen’s University, ON, Canada | |
| 4School of Graduate Studies, School of Kinesiology and Health Studies, School of Rehabilitation Therapy, ON, Canada | |
| 5Department of Psychiatry, Kingston General Hospital, ON, Canada | |
| Corresponding Author : | Kamary Coriolano School of Rehabilitation Therapy - (Louise D. Acton Bldg.) Queen’s University, 31 George Street Kingston, ON, Canada K7L 3N6 Tel: 613-5336000(79386) E-mail: 5ldskc@queensu.ca |
| Received April 17, 2013; Accepted May 27, 2013; Published June 01, 2013 | |
| Citation: Coriolano K, Aiken AB, Harrison MM, Pukall CF, Brouwer BJ, et al. (2013) Changes in Knee Pain, Perceived Need for Surgery, Physical Function and Quality of Life after Dietary Weight Loss in Obese Women Diagnosed with Knee Osteoarthritis. J Obes Weight Loss Ther 3:174. doi:10.4172/2165-7904.1000174 | |
| Copyright: © 2013 Coriolano K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Objectives: This pilot study had two main objectives, the first aimed to investigate whether weight loss is associated with a reduction in perceived need for Total Knee Replacement (TKR) surgery due to decrease in knee pain and improvement in function. The second aimed to identify whether change in body weight would directly affect reduction in knee pain to a point where the need for surgery could be prolonged or alleviated. 34 subjects were recruited into the study. Design: Women between 40 and 65 years old with morbid obesity (BMI ≥ 35 kg/m2) and osteoarthritis of he knee were pre-selected. If participants passed study criteria the Western Ontario McMaster University questionnaire (WOMAC), Item -36 Short Form Health Survey (SF-36), 6 Minute Walk Test (6MWT) and Timed Up And Go (TUG) were obtained from baseline and subjects were enrolled into a weight loss program, with no exercises included, for a 6 month period. Results: Repeated measures analysis of variance (ANOVA) revealed that at 6 weeks of diet the mean body weight reduction of 9.5%, was followed by a significant reduction (p=.015) in WOMAC scores and (p=.038) SF-36 sub score of physical function. At 3 months of diet a significant reduction of 16.5% in body weight contributed to a significant decrease of 37% in knee pain and 56% of participants perceived not to have surgery. Conclusions: These results suggest that an initial loss of 16.5% of body weight for obese individuals was significant enough to reduce pain and postpone patient’s intent to have surgery in 56%.
| Keywords |
| Osteoarthritis; Obesity; Pain; Perceived need for surgery |
| Introduction |
| Obesity has become a global health problem of major importance [1]. In Canada, the 2004 Canadian Community Health Survey (CCHS) indicated that the number of obese adults was about 23.1% (over 5.5 million) of the population [2]. This substantial increase in weight has a great effect on the health of Canadians due to related comorbidities associated with obesity [2,3]. Obesity increases the incidence of many chronic conditions, including osteoarthritis (OA) [3,4]. The onset of OA in weight-bearing joints such as knees and hips has been associated with obesity [5,6]. Excessive weight increases the biomechanical load on these joints during weight-bearing activities intensifying a deterioration process of the cartilage inside the joints, causing varying degrees of stiffness, swelling and pain [3,7]. And joint pain is unquestionably one of the most debilitating aspects of OA [8]. |
| Obesity is commonly measured by the individual’s Body Mass Index (BMI). The standard categories for BMI include normal weight (18.5-24.9 kg/m2), overweight (25-29.9 kg/m2) and obese (30 kg/m2 or more) [9]. The obesity category is divided into three subcategories: class I obesity (BMI 30-34.9 kg/m2), class II obesity (BMI 35-39.9 kg/m2) and class III obesity (BMI ≥ 40 kg/m2) [9]. Many morbidly obese individuals with knee OA require a total knee replacement (TKR) surgery to improve their quality of life. However, those with a BMI of 35 kg/m2 or greater have higher chances of poorer post-operative outcomes after a total joint replacement than those within a normal or overweight BMI range [10]. The post-operative outcome for these individuals tends to be affected negatively by their weight [11]. |
| The likelihood of a successful outcome after a total joint replacement surgery in obese individuals is reduced due to increased rates of infection, and the development of complications such as deep vein thromboses, or early failure of the prosthetic [10,12,13]. Therefore, many surgeons refuse to operate on obese patients until they have lost weight. However, after losing considerable amount of weight these individuals show reduced knee pain, increased functional performance and improvements in quality of life [14,15]. Even though these changes might encourage some patients to postpone surgery indefinitely, up to now, weight loss in morbidly obese people with knee OA has not been associated with perceived need for TKR surgery [16]. |
| Therefore, the primary purpose of this pilot study was to investigate whether weight loss is associated with a reduction in perceived need for TKR surgery due to decrease in knee pain and improvement in function. Secondly, this study aimed to identify whether change in body weight would directly affect reduction in knee pain to a point where the need for surgery could be prolonged or alleviated. |
| Methods |
| Patients |
| The study population was a sample of convenience. Women between 40 and 65 years old with morbid obesity (BMI ≥ 35 kg/m2) and severe OA of the knee presenting for an orthopedic consult for TKR were pre-selected. Patients meeting these criteria were recruited between April 2008 and March 2009. Women who had comorbidities that would prevent them from participating in the diet program, such as kidney disease or gallbladder attacks, were excluded. |
| Ethical approval was obtained from General Research Ethics Board (GREB) of Queen’s University before recruiting potential participants for the study. Once approval was endorsed, patients were recruited from the orthopedic surgical case load of four participating orthopedic surgeons. Patients with BMI ≥ 35 kg/m2, who indicated severe knee pain and radiological knee OA, were identified by the surgeons during consultation where weight loss was suggested prior to surgery. These patients were subsequently contacted by a research associate who described and invited them to participate in the study. |
| The patients who agreed to participate self-reported, over the phone, being in a good health and willing to participate in a diet program. The total length of the diet was 6 month however; participants were encouraged to continue the diet until they reached their personal goal. The patients were asked whether they were able to tolerate moderate activity between 60 to 90 minutes. Additionally, all participants were pre-screened to exclude those with a history of: non-knee OA related mobility restrictions (neurological and musculoskeletal), cardiac disease (unstable angina, peripheral vascular disease, congestive heart failure), uncontrolled hypertension (systolic pressure > 140 mmHg, diastolic pressure > 90 mmHg), or cognitive deficits limiting communication. Those who were eligible were booked for an initial assessment conducted in a university laboratory. |
| Upon arrival at the laboratory, subjects were given a letter of information and consent form. If they agreed to participate, their demographic data including height and weight, their perceived need for surgery (PNS), functional tests and questionnaires were obtained. |
| Outcome measures |
| Patients’ weight, PNS and objective and subjective measures of physical function were obtained at baseline before commencing the diet and again at 6 weeks, 3 months and 6 months during the diet program. The objective functional tests performed were the Six Minute Walk Test (6MWT) and the Timed Up and Go test (TUG). The 6MWT is generally conducted in an enclosed, quiet corridor on a 25-meter track delineated by two lines marked on the floors [17]. Patients were instructed to walk from one line to the other, covering as much ground as possible in six minutes. Individuals were told that they could rest if they became too short of breath or tired, but to continue walking when they were able to do so. To calculate the walking distance a metre wheel was used to measure the additional steps of any incomplete lap (in meters). The procedure for the TUG requires documenting the time, in seconds, that an individual takes to rise from a standard armchair, walk 3 meters, turn, walk back to the chair and sit down quickly and safely [18]. In this experiment, the test was initiated with the participant sitting in the chair with their back leaning on the back of the chair, both arms on the arms of the chair, legs lined up and feet flat on the floor. The chair was positioned such that it did not move when the subjects moved from sitting to standing. |
| The subjective measure of physical function was the Western Ontario McMaster University questionnaire (WOMAC). The WOMAC uses 17 items related to the degree of difficulty of performing activities of daily living (e.g., walking or sitting) to assess the individual’s level of physical function. The Likert scale version of WOMAC was the one used in this study. The patients were asked to identify on a scale from 0 (none) to 4 (extreme) the degree of difficulty they have been experiencing in the past 72 hours. The maximal score for this questionnaire section ranges from 0 to 68, with higher scores indicating greater dysfunction. The WOMAC pain section consists of 5 items with a total score ranging from 0 to 20, with higher scores indicating greater levels of pain. Finally, the WOMAC stiffness section corresponds to the degree of stiffness individuals with knee OA are experiencing in the last 72 hours. This section consists of 2 items with a total score of 8 which indicates a high degree of stiffness [19]. |
| The SF-36 is a validated general health related quality of life (QOL) questionnaire. It includes one multi-item scale that measures eight health concepts: general health (GH), vitality (VIT), role physical (RP), physical functioning (PF), emotional health problems (RE), social activities (SOC), mental health (MH) and bodily pain (BP). The SF-36 scale ranges from 0 to 100, with higher scores indicating a better health status [20]. |
| In this study, the PNS was used to measure patients’ level of perceived need for surgery such as total knee replacement surgery. The participants were asked at baseline and at each follow up session whether they still needed surgery and the answer was obtained as a yes or no response. |
| After baseline testing, subjects were referred for a full medical exam and enrolment into a weight loss program at the Bernstein Diet Centres TM at no charge. The program is a low-fat; low calorie and low carbohydrate diet that is medically monitored. Patients can only eat certain food and they must track everything they eat. As part of the diet protocol, patients are not expected to eat more than 900 calories per day and the diet is combined with weekly vitamin B injection. The patients were monitored and weighed three times a week at the clinic, and were seen by a physician every two weeks. Blood work and urine samples were taken regularly to monitor subjects’ health status. There were no physical activities or specific exercises combined with diet. One year of maintenance was provided for all patients who reached their final goal after 6 months of diet. |
| Analysis |
| Data was analyzed using a Statistical Package for Social Science (SPSS 19) and Microsoft Excel 2007. Univariate descriptive statistics (mean, standard deviation, frequency counts and percentages) were calculated for demographic and outcome data. The analysis was conducted with a power level of 0.8 and alpha (α) level of .05. Results were presented as mean ± standard deviation (SD) and/or median range or as counts with proportion as appropriate. |
| In the first set of analyses, an independent t-test was used to compare the participants who were enrolled but dropped out prior to commencing the diet with those who remained in the program. Then we observed whether body weight was associated with knee pain, WOMAC, SF-36 and objective measures of physical function (6MWT and TUG) over time. For that purpose, a Pearson’s correlation analysis was carried out over time. The PNS values were described as the percentage of yes responses, based on the number of respondents at each time point. Furthermore, a Chi-square analysis was used to identify whether the percentage of YES responses, compared to the percentage of NO responses were significantly different based on the number of respondents at each time point. |
| Finally, we observed whether significant changes occurred in body weight, knee pain, WOMAC, SF-36, 6MWT and TUG. A repeated measure ANOVA was generated to identify whether these changes varied significantly over time. Then a Post hoc test analysis, using the Bonferroni method, identified where the changes occurred, and whether these changes were linearly distributed within the group. The Post hoc analysis also obtained the mean difference, at each time point, of each variable in the statistical test. The mean difference of each variable was used to calculate their percentage change over time. For example the mean difference in body weight was used to calculate the percentage of its reduction at each time point. |
| Results |
| Forty subjects were referred for the study, of these, 6 did not meet the inclusion criteria, and thus 34 subjects were recruited into the study. Of those, 8 (23.5%) withdrew before commencing the diet, 17 (50%) completed six months on the program and only 9 continued the diet after 6 months and reached to their personal goal. No significant difference in weight, BMI, pain, WOMAC total score, PNS, 6MWT and TUG was observed between those who withdrew before starting the diet and those who remained in the study. At baseline, mean age was 58.2 ± 5.8 years old. Participants’ characteristics at baseline are summarized in Table 1. |
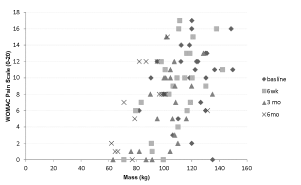
| The correlation analysis over the six month period indicated that knee pain significantly (r=0.511; p=0.048) correlated with body weight (Figure 1). Repeated measures ANOVA showed that knee pain significantly changed over time (Table 2), however it did not significantly change until 3 months of diet (p=0.004; 95% CI 1.37, 7.62) when participants indicated 37% less pain and had lost 16.5% of their body weight (p=.000; 95% CI 16.276, 23.340). Even though at 6 weeks participants had a significant weight loss of 9.5% of body weight (p=.000; 95% CI 9.38, 13.54), no significant change in pain was observed (Table 3). |
| With regard to the PNS, the percentage of individuals who responded yes, at each time point, is shown in Table 4. The total number of responses corresponded to the number of respondents at each time point. For instance, at 6 weeks 25 responses were obtained, indicating that a total of 25 individuals responded whether a TKR surgery was still necessary (Table 4). The Chi-square result X2=4.16, at 6 weeks, indicated a significant difference (p=0.04) between YES and NO responses. No significant difference was observed at 3 months, but at 6 moths a Chi-square result of X2=13.9 also indicated a significant difference (p=0.001) between YES and NO responses (Table 4). |
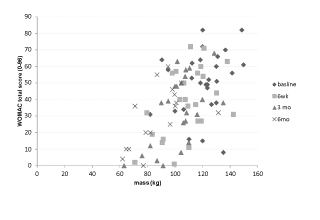
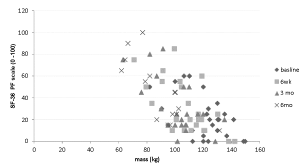
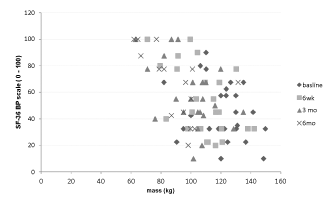
| The WOMAC total score significantly (r=.564; p=0.019) correlated with body weight over time (Figure 2). Repeated measures ANOVA indicated that the WOMAC total score significantly changed over time (Table 2) and a significant decrease of 21.1% was observed at 6 weeks of diet (Table 3). SF-36 sub score of physical function (PF) and body pain (BP) significantly (r=0.667; p=0.00 and r=0.521; p=0.00) correlated with body weight over time (Figure 3a and 3b). Repeated measures ANOVA showed that SF-36 sub scores PF (p=0.000; F3, 14=16.56) and BP (p=.001; F3, 14=8.74) significantly changed over time. However, only the SF-36 (PF) significantly changed at 6 weeks (Table 3). |
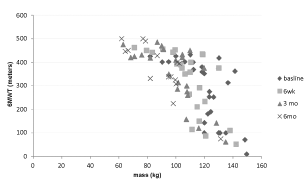
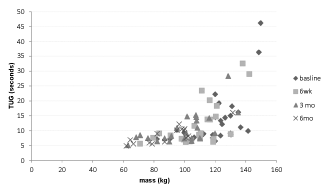
| Both measures of physical function (6MWT and TUG) significantly (r=0.709; p=0.00 and r=0.633; p=0.00) correlated with body weight over time (Figure 4 and 5). Further analysis indicated that both the 6MWT and TUG changed over time (Table 2). There was a significant increase of 28.9% in the 6MWT (p=.000; F3, 11=12.42) at 3 months of diet and a significant increase of 31.2% in the TUG test (p=0.007; F3, 11=6.22) but only at 6 months of diet (Table 3). |
| Discussion |
| Joint pain is one of the major complaints among those with OA [21], and it is unquestionably one of the most debilitating aspects of OA [8]. Therefore, it might influence a patient’s decision to undergo TKR surgery [22]. A review study observed the effect of bariatric surgery on joint pain [23]. Bariatric surgery can be achieved by different procedures performed on obese individuals to reduce body weight [23]. According to the review study, a significant reduction in BMI values contributes to reduce joint pain. In our study, a significant weight loss was followed by significant reduction in knee pain at 3 months of diet (Table 2 and 3). Similar to our findings, a previous study observed significant reduction in knee pain by 3 months after bariatric surgery [24]. Further studies have emphasized that reduction in body weight contributes to reduced knee pain followed by significant improvements in physical function and quality of life in obese and overweight individuals [14,25,26]. Therefore, decrease in body weight, knee pain and improvement in physical function might be important factors in patients’ decisions to not undergo TKR surgery [22]. Based on our findings, after significant reduction of body weight at 6 weeks, 3 months, and 6 months followed by decrease in knee pain, improvements in function and quality of life, only 60%, 44% and 29.4% of the participants, respectively, thought that TKR surgery was still necessary. A significant decrease in PNS was observed at 6 weeks, where 60% of the participants considered surgery, and then at 6 months where only 29.4% of the participants were still considering surgery (Table 4). |
| However, at 3 months no significant difference was observed in PNS between those who perceived surgery and those who did not perceive surgery. It appeared that at 3 months, patient’s’ decision to undergo TKR surgery was shifting, but not significant enough to show any difference. |
| It has been suggested that a reduction of more than 5% of body weight is needed to promote reduction in disability and pain [14]. A meta-analysis of previous weight loss studies suggests that at least 10% of body weight loss in needed to have a considerable clinical effect on pain and physical function [16]. However, to our knowledge no other study has observed the association of obese individuals’ PNS with pain and the amount of weight they need to lose to prolong or alleviate the need for surgery. |
| Two important criteria for TKR surgery are based on the severity level of knee pain and its loss of function due to OA. However, for obese individuals with knee OA, a considerable weight loss can significantly decrease disability and knee pain before TKR surgery takes place [14,16]. Our study observed that knee pain and body weight significantly changed over time (Table 2). Yet, unlike body weight the level of pain did not significantly change until 3 months of diet has been reached. Interestingly, at 3 months of diet participants indicated a higher percentage of pain reduction (37%) compared to pain reduction at 6 months (33%), when great weight loss has been achieved. This could be an indication that after 3 months of diet, the level of pain may have reached a plateau; where, independent of further weight loss, the level of pain after 3 months would not significantly reduce. Given that there was no significant reduction in pain between 3 and 6 months, the percentage of PNS still dropped from 44% at 3 months to 29.4% at 6 months (Table 4). The perception regarding the choice to pursue TKR surgery consistently decreased following weight loss from baseline to 6 months (Table 3 and 4). |
| Extrapolating from another study that observed the perceived disability and functional limitations in obese women [27], the authors suggested that perception of disability depends on how individuals view themselves in terms of disability and whether the individuals have high or low expectations during their daily activities. It seems that after significant weight loss, some participants had a better perception of their abilities regardless of pain. This level of perception may have guided some of these participants to reach a greater weight loss with consequent decrease in PNS for a TKR. For instance, all nine women who reached their personal goal after 6 months of dieting obtained a BMI of 25 kg/m2 ± 1.0 and body weight of 64.04 kg ± 5.27 and indicated that a TKR surgery was no longer necessary. Even though, they showed a significant difference (p=.03) in body weight compared to those who completed 6 months of diet but had not reached their goal weight, no significant difference in knee pain, physical function and quality of life was observed. |
| From a clinical perspective, by knowing the amount of weight obese women need to lose to significantly reduce pain and therefore prolong or alleviate the need for surgery, one could change the PNS for those who require surgery, after losing a significant percentage of body weight. Moreover health care providers could prevent premature knee replacement surgeries and subsequent early prosthetic revision for those who could benefit from conservative interventions. Our statistical analysis indicated that a significant loss of 16.5% of body weight for morbidly obese women (BMI ≥ 35 kg/m2) represented a significant reduction of 37% in knee pain and a decrease in more than 50% of PNS (Table 3 and 4). |
| These results suggest that an initial loss of 16.5% of body weight for obese women was significant enough to reduce by 56% their desire to have surgery. Previous studies have suggested that a weight loss of 10% to 15% of baseline body weight may provide the necessary stimulus to reduce inflammation and knee joint loads to levels that result in less cartilage deterioration and consequent delay of disease progression [14,16]. Moreover, a reduction of only 5% of body weight might contribute to decrease the level of cytokine and adipokine activity [28], which has been related to cartilage breakdown and signs of synovial joint inflammation [29]. Therefore, in concordance with the above mentioned studies, our results suggest that a significant loss of 16.5% of baseline body weight may not only contribute to reducing the excessive mechanical load and biochemical effect on the knee joint, but also it may encourage these individuals to postpone a TKR surgery indefinitely. |
| After 6 months of diet, when an average of 27% of baseline body weight had been lost, only 29.4% of the participants still perceived TKR surgery as an option (Table 3 and 4). Even though these participants still thought surgery was needed after 6 months of diet, it should be taken into consideration that these individuals may still benefit from losing weight. Similar to previous studies [14-15,25] significant improvements in WOMAC total scores and SF-36 sub scores (PF) were continuously observed when participants had lost 9.5%, 16.5% and 27% of body weight (Table 3). The 6MWT significantly improved after 16.5% of body weight loss, while the TUG significantly improved after 27% of body weight loss (Table 3). Therefore, despite significant changes in function and quality of life, those who still perceived need for surgery after losing 27% of baseline body weight would have improved their general health and had additional health benefits from losing the weight. Moreover, they would likely have reduced the chances of post-operative infections and complications such as deep vein thromboses, or early failure of the prosthetic [10,12,13] when they do undergo TKR surgery. |
| Even though a weight loss of 16.5% might influence a patients’ choice to undergo TKR surgery, this finding might not be extended to the general morbidly obese population. Not all obese women with knee OA who lose 16.5% or more of their body weight might be able to avoid surgery. However, based on our results, we expect that a weight loss of 16.5% might provide a major decrease in knee pain and increase in function. These remarkable changes give therapists and medical doctors the opportunity to motivate patients; allowing them to improve their quality of life, and increase their level of physical activity, in a safe, motivating, pleasant and accessible way [30]. Therefore, even if an initial weight loss of 16.5% or a final weight loss of 27% did not change the actual PNS for TKR of some participants, a reduction in pain and increase in function will likely provide patients with the necessary confidence they need to improve their health before surgery takes place. |
| A small sample size was a visible limitation in our pilot study. However with limited resources we were able to successfully provide the same diet program to 34 participants. Unfortunately we lost 50% of our participants who dropped out the study before completing 6 months of diet. As they decided to stop the diet they were automatically excluded from the study. Despite limitations, our pilot study is the first longitudinal study to indicate the amount of body weight obese women with knee OA should lose to prolong or alleviate a TKR surgery by assessing individuals’ PNS. This study indicates that an initial reduction of 16.5% of body weight might change the PNS during diet intervention, which also improves physical function and quality of life of obese women with knee OA. Even though, participants obtained significant results only based on diet intervention, the effective association of exercise with diet has been strongly recommended [14-16,25,28]. |
| Therefore, future studies should combine diet and exercise and possibly integrate health education programs to enhance the use of daily physical activities for obese individuals. In this manner, obese individuals with knee OA might sustain a long term weight loss and better manage their knee OA symptoms. Facilitating regular physical activity in the community might be essential to the maintenance of a better life style and management of knee OA [31]. Previous weight loss studies recruited a higher number of participants with diet interventions varying from 12 to 18 months [16,25] consequently, a larger sample is needed and a strong strategy to improve retention and adherence is critical, particularly if the duration of the diet is to be increased. It is also important to observe physiological measures of physical function such as quadriceps and hamstrings strength as well as oxygen consumption, which are important in determining functional capacity of obese individuals with knee OA. |
| The clinical importance of these findings is the effect of weight lost before surgery. Therefore, future research could also observe at what rate significant functional improvements continue to occur in individuals who end up having surgery even after losing 16.5% or more of their body weight before surgery. However, considering the possible ineffectiveness of surgical intervention in knee OA for obese patients [10,13] our results give strong support to a minimal weight loss of 16.5% as a foundation for the conservative treatment of obese patients with knee OA. |
| Declaration |
| Financial disclosure statements have been obtained, and no conflicts of interest have been reported by the authors or by any individuals in control of the content of this article. |
References
- Sokar-Todd HB, Sharma AM (2004) Obesity research in Canada: literature overview of the last 3 decades. Obes Res 12: 1547-1553.
- Tjepkema M (2006) Adult obesity. Health Rep 17: 9-25.
- Luo W, Morrison H, de Groh M, Waters C, DesMeules M, et al. (2007) The burden of adult obesity in Canada. Chronic Dis Can 27: 135-144.
- Hunter DJ, Felson DT (2006) Osteoarthritis. BMJ 332: 639-642.
- Coggon D, Reading I, Croft P, McLaren M, Barrett D, et al. (2001) Knee osteoarthritis and obesity. Int J Obes Relat Metab Disord 25: 622-627.
- Nevitt MC, Lane N (1999) Body weight and osteoarthritis. Am J Med 107: 632-633.
- Felson DT (2006) Clinical practice. Osteoarthritis of the knee. N Engl J Med 354: 841-848.
- Kelly KD, Voaklander DC, Johnston DW, Newman SC, Suarez-Almazor ME (2001) Change in pain and function while waiting for major joint arthroplasty. J Arthroplasty 16: 351-359.
- Douketis JD, Paradis G, Keller H, Martineau C (2005) Canadian guidelines for body weight classification in adults: application in clinical practice to screen for overweight and obesity and to assess disease risk. CMAJ 172: 995-998.
- Winiarsky R, Barth P, Lotke P (1998) Total knee arthroplasty in morbidly obese patients. J Bone Joint Surg Am 80: 1770-1774.
- Foran JR, Mont MA, Etienne G, Jones LC, Hungerford DS (2004) The outcome of total knee arthroplasty in obese patients. J Bone Joint Surg Am 86-86A: 1609-1615.
- Pritchett JW, Bortel DT (1991) Knee replacement in morbidly obese women. Surg Gynecol Obstet 173: 119-122.
- Mulhall KJ, Ghomrawi HM, Mihalko W, Cui Q, Saleh KJ (2007) Adverse effects of increased body mass index and weight on survivorship of total knee arthroplasty and subsequent outcomes of revision TKA. J Knee Surg 20: 199-204.
- Messier SP (2010) Diet and exercise for obese adults with knee osteoarthritis. Clin Geriatr Med 26: 461-477.
- Messier SP, Legault C, Mihalko S, Miller GD, Loeser RF, et al. (2009) The Intensive Diet and Exercise for Arthritis (IDEA) trial: design and rationale. BMC Musculoskelet Disord 10: 93.
- Christensen R, Bartels EM, Astrup A, Bliddal H (2007) Effect of weight reduction in obese patients diagnosed with knee osteoarthritis: a systematic review and meta-analysis. Ann Rheum Dis 66: 433-439.
- Beriault K, Carpentier AC, Gagnon C, Ménard J, Baillargeon JP, et al. (2009) Reproducibility of the 6-minute walk test in obese adults. Int J Sports Med 30: 725-727.
- Podsiadlo D, Richardson S (1991) The timed "Up & Go": a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc 39: 142-148.
- Maly MR, Costigan PA, Olney SJ (2006) Determinants of self-report outcome measures in people with knee osteoarthritis. Arch Phys Med Rehabil 87: 96-104.
- Brazier JE, Harper R, Jones NM, O'Cathain A, Thomas KJ, et al. (1992) Validating the SF-36 health survey questionnaire: new outcome measure for primary care. BMJ 305: 160-164.
- Woolf AD, Pfleger B (2003) Burden of major musculoskeletal conditions. Bull World Health Organ 81: 646-656.
- Harris WH, Sledge CB (1990) Total hip and total knee replacement (2) N Engl J Med 323: 801-807.
- Vincent HK, Ben-David K, Cendan J, Vincent KR, Lamb KM, et al. (2010) Effects of bariatric surgery on joint pain: a review of emerging evidence. Surg Obes Relat Dis 6: 451-460.
- Korenkov M, Shah S, Sauerland S, Duenschede F, Junginger T (2007) Impact of laparoscopic adjustable gastric banding on obesity co-morbidities in the medium- and long-term. Obes Surg 17: 679-683.
- Messier SP, Loeser RF, Miller GD, Morgan TM, Rejeski WJ, et al. (2004) Exercise and dietary weight loss in overweight and obese older adults with knee osteoarthritis: the Arthritis, Diet, and Activity Promotion Trial. Arthritis Rheum 50: 1501-1510.
- Rejeski WJ, Focht BC, Messier SP, Morgan T, Pahor M, et al. (2002) Obese, older adults with knee osteoarthritis: weight loss, exercise, and quality of life. Health Psychol 21: 419-426.
- Larsson UE, Mattsson E (2001) Perceived disability and observed functional limitations in obese women. Int J Obes Relat Metab Disord 25: 1705-1712.
- Nicklas BJ, Ambrosius W, Messier SP, Miller GD, Penninx BW, et al. (2004) Diet-induced weight loss, exercise, and chronic inflammation in older, obese adults: a randomized controlled clinical trial. Am J Clin Nutr 79: 544-551.
- Teichtahl AJ, Wang Y, Wluka AE, Cicuttini FM (2008) Obesity and knee osteoarthritis: new insights provided by body composition studies. Obesity (Silver Spring) 16: 232-240.
- Stuifbergen AK (2006) Building health promotion interventions for persons with chronic disabling conditions. Fam Community Health 29: 28S-34S.
- Hurley MV (2003) Muscle dysfunction and effective rehabilitation of knee osteoarthritis: what we know and what we need to find out. Arthritis Rheum 49: 444-452.
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3a |
 |
 |
 |
| Figure 3b | Figure 4 | Figure 5 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 13660
- [From(publication date):
May-2013 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 9126
- PDF downloads : 4534
