Short Communication Open Access
Dry Needling and its Use in Health Care A Treatment Modality and Adjunct for Pain Management
| Woehrle J*, Roman G and Russell BE | |
| Department of Physical Therapy, Midwestern University, USA | |
| Corresponding Author : | Judith Woehrle J Associate Professor Midwestern University 19555 N 59th Avenue Glendale AZ 85308, USA Tel: 623-572- 3921 E-mail: jwoehr@midwestern.edu |
| Received July 16, 2015; Accepted August 06, 2015; Published August 10, 2015 | |
| Citation:Woehrle J, Roman G, Russell BE (2015) Dry Needling and its Use in Health Care – A Treatment Modality and Adjunct for Pain Management. J Pain Relief 4:194. doi:10.4172/21670846.1000194 | |
| Copyright: ©2015 Woehrle J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pain & Relief
Abstract
Dry needling is used by medical professionals throughout the United States to treat pain and to help patients improve quality of life. There are noninvasive mechanisms that are used to treat pain such as heat and cold application, other thermal or electrical modalities, stretching to soft tissue, or manual therapy. Dry needling is a mechanism that is used to treat muscle trigger points that refer pain to areas within the body. Trigger points can cause irritation to skeletal muscle or fascia and affect function. Dry needling is used to reduce pain by achieving a local twitch response to release muscle tension, normalize electrical dysfunction of the motor end plates, and assist with return to activities or rehabilitation. There are many modalities available for pain management and dry needling is one of many used to target soft tissue and manage pain. Using a multimodal approach is an effective method of treatment to consider for many musculoskeletal or neuromuscular conditions.
| Introduction |
| Numerous treatments for pain have been proposed, such as trigger point infiltration, dry needling, acupuncture, manual therapy, stretching of soft tissue, acupressure, and medications. Trigger point dry needling, or intramuscular needling, has become more prevalent and is used by medical professionals throughout the United States. Muscle trigger points (MTrPs) are found to be involved in the pain process whether the pain is in the trunk, neck, arm, or leg. Monofilament needles are used with dry needling and are inserted into MTrPs by touching, tapping or pricking the tip of the needle into the skin. MTrPs are defined as taut bands that are hypersensitive areas in the body and are painful upon palpation.[1] MTrPs are classified as either active or latent. When palpated, active MTrPs could elicit referred pain, reproducing the patient’s symptoms; whereas, latent MTrPs do not cause a pain that will reproduce the patient’s symptoms but could be responsible for tightness of the muscle.[2,3] Dry needling is used for myofascial pain, lower and upper extremity pain, neck pain, back pain, headaches, jaw pain, and migraines, among other conditions. The effects of dry needling in the treatment of knee osteoarthritis has been well documented.[4-6] Dry needling is not used as in traditional Oriental or Chinese medical practice, or to inject solutions into MTrPs. Dry needling is used as an adjunct for the management of pain and dysfunction in numerous neuromusculoskeletal conditions. |
| Effects of dry needling |
| Many schools of thought and approaches to dry needling have been presented as effective ways to treat pain. Various philosophies, theories, rationales, and duration of training programs have been proposed, within health care, addressing the use of dry needling to treat pain and soft tissue irritability. Needling provides a hyperstimulation with an analgesic effect that is similar to heat and cold compress causing changes of the physiological responses within skin.[7] Pain signals are reduced with direct stimulation to the ischemic tight muscle segment allowing it to relax when using needling.[1] Opoids and pain gating have been implicated in pain control. When using imaging, it has been found that changes are noted within the brain after needle treatment.[8,9] Using dry needling under infrared thermovision causes a temperature increase and short-term vasodilatation response that is similar to the pain distribution pattern of the subject.[10] Needle insertion into the MTrPs elicits a localized twitch response that could interrupt the motor end-plate causing analgesia to the area.[11,12] Dry needling disrupts the sensory input to the spinal cord through the mechanical irritation of the needle being inserted into the sensitive loci within the MTrPs, which in turn causes a local twitch response.[13] It has been proposed that with needle insertion there is a disruption of nociceptors which will elicit a local twitch response within the MTrPs causing a disruption of the pain cycle with notable pain relief.[14,15] Pain perceptions and reductions in pain could be due to the number of physiologic mechanisms that contribute to subjective improvements. Some patients may not feel the insertion of the needle while others might note a little electrical impulse in the local tissue. The health care provider should consider these implications when providing dry needling to MTrPs. |
| Dry needling as an intervention |
| Using dry needling in combination with various manual therapy techniques is considered when treating both MTrPs and non-trigger point conditions.[16] Soft tissue interventions such as stretching, manual therapy, and exercises to the deep neck flexors are considered an effective approach to manage neck pain. Dry needling is also used to treat neck pain. Treating neck pain with dry needling to the upper trapezius has had positive results in reducing the pain.[17] Using a single session of dry needling to the specific MTrPs of the upper trapezius, resulted in a decrease of neck pain intensity.[17,18] Treating the effects of whiplash with dry needling and exercise has been shown to produce positive outcomes with significant reduction in pain, pain catastrophizing, and cold hyperalgesia at 6 and 12 months follow-up. [19] The temporomandibular joint has associated myofascial pain dysfunction and is another area that has had successful outcomes with use of dry needling.[20] Treating myofascial pain with dry needling has been shown to be an effective way to manage pain, improve mobility, reduce sensitivity of MTrPs, and improve the quality of life.[21] Being point specific with dry needling seems to produce more effective results than non-point-specific dry needling. Using dry needling on MTrPs of the hamstrings and gluteal muscles did not show significant changes in straight leg raise or hip internal rotation; yet, there were subjective improvements reported in pain and tightness of the muscles following dry needling or sham needling.[3] Using dry needling with a multimodal approach for postoperative repair to a humeral fracture or rotator cuff repair may have assisted with a faster increase in function.[22] The addition of dry needling of the multifidus muscle of the low back in the treatment of low back pain has been shown to increase multifidus muscle contraction and decrease sensitivity to pain in patients who responded to treatment.[23] The use of dry needling has been postulated to be a mechanism for the attainment of early pain relief in order to facilitate a manual therapy technique and a quicker return to function. [24] |
| Other modalities used as an intervention for pain relief |
| Dry needling and other modalities are available to aide in the delivery of pain management. (Figure 1) Thermal modalities change responses in tissue temperature and circulation, altering cell membrane permeability [25], modulate pain via the gate control theory and effect the endogenous opioid system [26]. Modalities are often used in conjunction with or in sequence to one another. Moist heat or cryotherapy are often used with electrical stimulation or inferential current for pain management. For thermal ultrasound, preheating the skin with moist heat prior to an ultrasound treatment is thought to decrease the time necessary to reach moderate to vigorous heating.[25] High volt electrical stimulation with a positive polarity for motor nerve depolarization could be used in combination with thermal ultrasound for localized trigger point release.[25,27] For managing chronic pain, an electrical current is used to depolarize efferent motor nerve fibers through high current amplitude, low pulse frequency, and a long pulse duration.[25,27] Modality selection depends upon the surface area of tissue involvement, the depth of penetration desired and stage of injury healing. Dosing parameters unique to each modality must be carefully considered, in order to foster the best patient outcome. |
| Conclusion |
| In review, it is hypothesized that dry needling is an adjunct to facilitate a quick response to significantly minimize pain so a person could return to function.[24] Practice guidelines have been proposed that provide a rationale to deliver the optimal frequency, intensity, duration and points of insertion when using dry needling for neuromusculoskeletal conditions.[28] Standardization has been explored when treating MTrPs in people who have myofascial pain.[29] There might be a global reduction in pain perception due to the physiological responses to pain mechanisms as proposed when using other modalities for pain relief. In clinical practice, using dry needling as an isolated intervention is atypical. Dry needling combined with conventional therapies such as exercises and other modalities should be considered, especially if long term effects are desired.[19] Dry needling minimizes the pain so that the person is able to focus on performing the exercises, or other interventions, that will help restore movement. When deciding upon the use of dry needling for pain, a multimodal approach should be considered. |
References
- Simons DG, Travell JG, Simons LS (1998) Travell& Simons Myofascial Pain and Dysfunction. (2ndedn) Williams & Wilkins, Baltimore.
- Mejuto-Vázquez MJ, Salom-Moreno J, Ortega-Santiago R, Truyols-Domínguez S, Fernández-de-Las-Peñas C (2014) Short-term changes in neck pain, widespread pressure pain sensitivity, and cervical range of motion after the application of trigger point dry needling in patients with acute mechanical neck pain: a randomized clinical trial.J Orthop Sports PhysTher 44: 252-260.
- Huguenin L, Brukner PD, McCrory P, Smith P, Wajswelner H, et al. (2005) Effect of dry needling of gluteal muscles on straight leg raise: a randomised, placebo controlled, double blind trial.Br J Sports Med 39: 84-90.
- White A, Foster NE, Cummings M, Barlas P (2007) Acupuncture treatment for chronic knee pain: a systematic review.Rheumatology (Oxford) 46: 384-390.
- Whitehurst DG, Bryan S, Hay EM, Thomas E, Young J, et al. (2011) Cost-effectiveness of acupuncture care as an adjunct to exercise-based physical therapy for osteoarthritis of the knee.PhysTher 91: 630-641.
- Witt CM, Jena S, Brinkhaus B, Liecker B, Wegscheider K, et al. (2006) Acupuncture in patients with osteoarthritis of the knee or hip: a randomized, controlled trial with an additional nonrandomized arm.Arthritis Rheum 54: 3485-3493.
- Melzack R (1981) Myofascial trigger points: relation to acupuncture and mechanisms of pain.Arch Phys Med Rehabil 62: 114-117.
- Wu MT, Hsieh JC, Xiong J, Yang CF, Pan HB, et al. (1999) Central nervous pathway for acupuncture stimulation: localization of processing with functional MR imaging of the brain: preliminary experience. Radiology 212: 133-141.
- Bialla G, Solgiu M, Pellegata G, Paulesu E, Castiglioni I, et al. (2001) Acupuncture produces central activations in pain regions. Neuroimage 14: 60-66.
- Skorupska E, Rychlik M, Pawelec W, Samborski W (2015) Dry Needling Related Short-Term Vasodilation in Chronic Sciatica under Infrared Thermovision.Evid Based Complement Alternat Med 2015: 214374.
- Skorupska E, Rychlik M, Samborski W (2015) Intensive vasodilatation in the sciatic pain area after dry needling.BMC Complement Altern Med 15: 72.
- Kietrys DM, Palombaro KM, Azzaretto E, Hubler R, Schaller B, et al. (2013) Effectiveness of dry needling for upper-quarter myofascial pain: a systematic review and meta-analysis.J Orthop Sports PhysTher 43: 620-634.
- Audette JF, Wang F, Smith H (2004) Bilateral activation of motor unit potentials with unilateral needle stimulation of active myofascial trigger points.Am J Phys Med Rehabil 83: 368-374, quiz 375-7, 389.
- Hong CZ (2006) Treatment of myofascial pain syndrome.Curr Pain Headache Rep 10: 345-349.
- Hong CZ, Simons DG (1998) Pathophysiologic and electrophysiologic mechanisms of myofascial trigger points.Arch Phys Med Rehabil 79: 863-872.
- Fernandez-Carnero J, Fernandez-de-las-Penas C, de la Llave-Rincon AI, Ge HY, Arendt-Nielsen L (2007) Prevalence of and referred pain from myofascial trigger points in the forearm muscles in patients with lateral epicondylalgia. Clin J Pain 23: 353-360.
- Mejuto-Vazquez MJ, Salom-Moreno J, Ortega-Santiago R, Truyols-Dominguez S, Fernandez-de-las-Penas C (2014) Short-term changes in neck pain, widespread pressure pain sensitivity, and cervical range of motion after the application of trigger point dry needling in patients with acute mechanical neck pain: a randomized clinical trial. J Orthop Sports PhysTher 44: 252-260.
- Llamas-Ramos R, Pecos-Martin D, Gallego-Izquierdo T, Llamas-Ramos I, Plaza-Manzano G, et al. (2014) Comparison of the short-term outcomes between trigger point dry needling and trigger point manual therapy for the management of chronic mechanical neck pain: a randomized clinical trial. J Orthop Sports PhysTher 44: 852-861.
- Sterling M, Vicenzino B, Souvlis T, Connelly LB (2015) Dry-needling and exercise for chronic whiplash-associated disorders: a randomized single-blind placebo-controlled trial.Pain 156: 635-643.
- Diraçoglu D, Vural M, Karan A, Aksoy C (2012) Effectiveness of dry needling for the treatment of temporomandibularmyofascial pain: a double-blind, randomized, placebo controlled study.J Back MusculoskeletRehabil 25: 285-290.
- Unverzagt C, Berglund K, Thomas JJ (2015) Dry Needling for Myofascial Trigger Point Pain: A Clinical Commentary.Int J Sports PhysTher 10: 402-418.
- Arias-Buria JL, Valero-Alcaide R, Cleland JA, Salom-Moreno J, Ortega-Santiago R, et al. (2015) Inclusion of trigger point dry needling in a multimodal physical therapy program for postoperative shoulder pain: a randomized clinical trial. J Manipulative PhysiolTher 38: 179-187.
- Koppenhaver SL, Walker MJ, Su J, McGowen JM, Umlauf L, et al. (2015) Changes in lumbar multifidus muscle function and nociceptive sensitivity in low back pain patient responders versus non-responders after dry needling treatment. Man Ther 8.
- Dommerholt J (2011) Dry needling - peripheral and central considerations.J Man ManipTher 19: 223-227.
- Alain-Yvan B (2015) Therapeutic Electrophysical Agents. Evidence Behind Practice. (3rdedn) Philadelphia, PA: Lippincott Williams & Wilkins.
- Michelle C (2009) Physical Agents in Rehabilitation. From Research to Practice. (3rdedn) St. Louis, MO: Saunders Elsevier.
- Susan M, James B, Thomas N (2012) Modalities for Therapeutic Intervention. (5thedn) Philadelphia, PA: F.A. Davis Company.
- Dunning J, Butts R, Mourad F, Young I, Flannagan S, et al. (2014) Dry needling: a literature review with implications for clinical practice guidelines. PhysTher Rev 19: 252-265.
- Gerber LH, Shah J, Rosenberger W, Armstrong K, Turo D, et al. (in press) Dry needling alters trigger points in the upper trapezius muscle and reduces pain in subjects with chronic myofascial pain. PMR 7: 711-18.
Figures at a glance
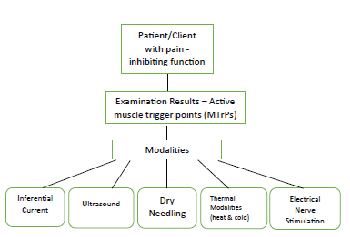 |
| Figure 1 |
Relevant Topics
- Acupuncture
- Acute Pain
- Analgesics
- Anesthesia
- Arthroscopy
- Chronic Back Pain
- Chronic Pain
- Hypnosis
- Low Back Pain
- Meditation
- Musculoskeletal pain
- Natural Pain Relievers
- Nociceptive Pain
- Opioid
- Orthopedics
- Pain and Mental Health
- Pain killer drugs
- Pain Mechanisms and Pathophysiology
- Pain Medication
- Pain Medicine
- Pain Relief and Traditional Medicine
- Pain Sensation
- Pain Tolerance
- Post-Operative Pain
- Reaction to Pain
Recommended Journals
Article Tools
Article Usage
- Total views: 15446
- [From(publication date):
September-2015 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 10718
- PDF downloads : 4728
