Research Article Open Access
Emerging Role of the Fat Free Mass Preservation during Weight Loss Therapy through a Novel Advanced Bio-Impedance Device (BIA-ACC)
| Nicoletta Canitano1, Paola Paci2 and Flora Ippoliti1* | |
| 1Department of Experimental Medicine, Sapienza University, Rome, Italy | |
| 2Institute of Systems Analysis and Computer Science (IASI) - CNR Rome, Italy | |
| Corresponding Author : | Flora Ippoliti Dipartimento di Medicina Sperimentale Sapienza Università di Roma Viale Regina Elena 324 00161, Rome, Italy E-mail: flora.ippoliti@uniroma1.it |
| Received July 18, 2013; Accepted September 11, 2013; Published September 13, 2013 | |
| Citation: Canitano N, Paci P, Ippoliti F (2013) Emerging Role of the Fat Free Mass Preservation during Weight Loss Therapy through a Novel Advanced Bio-Impedance Device (BIA-ACC). J Obes Weight Loss Ther 3:193. doi:10.4172/2165-7904.1000193 | |
| Copyright: © 2013 Canitano. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Obesity & Weight Loss Therapy
Abstract
Topic: Psychological and stressful social situations, as well as factors of an unhealthy lifestyle (such as insufficient exercise, weight increase and/or social isolation) are potential causes of MUS (Medically Unexplained Symptoms) and obesity, usually overlooked by general practitioners. Obesity is often underestimated using BMI, since it does not reflect the real loss of fat mass after nutritional strategies. Scope: We analyzed the changes in fat mass (FM) and fat-free mass (FFM) in the presence of decreasing BMI, using a novel advanced bio-impedance device, BIA-ACC (Bioelectric Impedance Analyzer for Analisi Composizione Corporea) that measures numerous parameters of body composition. Methods: 109 patients were enrolled at the center for primary care for a routine check-up, all apparently free of disease but with problems of excess weight and MUS to varying degrees. The evaluation of the parameters BIA-ACC was performed at the first visit T0, and at follow-up T1, after about 2 months of a standard nutritional strategy. Results: BMI decreased in all patients. FFM, particularly skeletal muscle, was the 1st principal component (PCA1: 58%) that determines the well-being of the patients and a decrease of MUS. The 2nd component (PCA2: 22%) is the FM. We found 3 different patterns of patient response to BMI reduction: 75.23% showed loss of FM and minimally FFM; 17.43% showed loss of FM with preservation or increase FFM; 7.34% showed loss of FFM alone. Conclusions: Body composition analysis is a valuable non-invasive tool to monitor patients in the early stages of immune-metabolic dysregulation when clinical symptoms are not yet evident. Our results demonstrate the importance of the maintenance of FFM rather than the loss of FM alone during weight loss therapy. Preservation of skeletal muscle is essential to facilitate the stabilization of loss of only fat and thus to eliminate the MUS correlated to chronic stress.
| Keywords |
| Medically unexplained symptoms; BIA-ACC; Body composition; Stress-related obesity; BMI; Weight loss; Immunometabolism |
| Introduction |
| The incidence of obesity has burgeoned to epidemic proportions in the Western world and in Italy: also called “globesity” [1-3]. The etiology of obesity is multifactorial, not only with genetic influences, but also environmental (socio-economic, behavioral or psychological causes) and determines a corresponding increase in both morbidity and mortality [4-6]. |
| Obesity and being overweight are due to excessive amount of body fat leading to a greater health risk [1,6]. The ideal body mass index (BMI) ranges between 18.5 and 25 kg/m2 with values ranging between 25 and 30 kg/m2 considered as overweight while BMI over 30 kg/m2 would be considered as obese. Nevertheless, BMI is not able to evaluate the real loss of fat mass after appropriate nutritional strategies. When an obese or overweight individual attempts without success to lose weight, from a practical point of view, this lack of success often triggers the onset of symptoms known as “vague and non-specific” (or MUS, Medically Unexplained Symptoms), which typically are the first reason for the patient to seek health care, and after clinical assessment do not seem to be explained by a clearly defined cause or diagnosis of a defined medical disease [7]. |
| MUS may be related to a number of factors, including stressful events related particularly to social relationships [8]. Among environmental factors inducing obesity, we can include stress-related disorders [9-11] which then affect energy regulation between the nervous system, the immune system, and the adipose tissue (AT) [12-15]. |
| Weight loss involves alteration of energy regulation and neuroimmuno- endocrine control are the basis of chronic inflammatory processes, which in turn constitute the common denominator of chronic pathological disease and an inflammatory response [16,17]. The role of immuno-endocrine control in obesity has been little investigated [3,4,6,18-22] and this research do not examines variations in body composition during the stress of weight loss to identify forerunners of chronic pathologies. Chronic stress activates the immune system thus consuming energy. In this way many apparently unrelated metabolic diseases arise because other organs receive no energy-rich fuels from storage organs. Changes in metabolic pathways lead to objective symptoms associated with those very conditions: cachectic obesity, insulin resistance and hyperinsulinemia, dyslipidemia, adipose tissue increase in inflamed tissues, hypertension and osteopenia [15-17]. Increasing evidence therefore underlines the pathogenetic relationship between stress, obesity and metabolic disease through neuro-immune activation [6,23,24]. |
| Environmental stressors and eating disorders alter adipose tissue anatomy and physiology, fat distribution and function patterns, though changes in plasticity. Previous work supports the notion that visceral/ abdominal adipose tissue (VAT or AAT) and subcutaneous adipose tissue (SAT) both contain white and brown adipocytes, collectively forming a multi-depot organ called the “adipose organ” [6,25]. VAT and SAT differ in their cellular composition, molecular properties and role in regulating metabolism: whereas increases in VAT contribute to metabolic disease, SAT is considered a weaker risk factor, and in some cases has a protective effect [26]. Only VAT responds to obesity in a manner that is consistent with active inflammation whereas no such changes are detected in micro vessels from subcutaneous fat or skeletal muscle [25,26]. A fraction of VAT deposits can accumulate especially with the continuous intake of fatty and sugary foods (“comfort foods”) [27,28] and this fact is still evaluated with the waist-to-hip ratio (WHR: waist/hip ratio) [26]. Obesity then is the ultimate consequence of a chronic positive energy balance, regulated by a complex network of signals that connects the immuno-endocrine system and the central nervous system [29-33]. |
| Energy-rich foods increase SAT. When SAT saturates and adipocytes can no longer proliferate or expand, impaired adipose tissue expandability may lead to ectopic lipid accumulation in VAT, liver, muscle and pericardial cells [6,34,35]. Energy dysregulation favors insulin resistance and metabolic disease [31,34]. Hence the risk of diabetes and coronary artery disease correlates strongly with relative visceral adiposity, rather than with BMI per se [35]. A clinically important finding is that VAT secretes more pro-inflammatory cytokines than SAT. Therefore waist circumference or waist-to-hip ratio or both diagnostic measurements are better than BMI as a proxy to prevent metabolic disease and CVD but are not yet sufficient. Although the above factors have been studied from a metabolic viewpoint, the widespread incidence of obesity points to an urgent need to consider weight loss measures in MUS and to develop tools to inform nutritionists and general practitioners dealing with MUS patients. |
| Scope of this work |
| Obesity is often underestimated using body mass index and waisthip ratio that are not able to evaluate the real loss of fat mass after appropriate nutritional strategies [36,37]. |
| A large part of the adult population, with stressful social situations and eating disorders, suffers or have suffered on several occasions from MUS symptoms that can be traced back to a wide variety of disorders of various kinds, which only rarely allow a precise diagnosis, keeping frequently within the limits of clinical altered only slightly, not to the point of being pathological [7,8,37]. To the best of our knowledge, there have been few studies into the connection between MUS, inflammation and possible role of the physiological balance of endocrine, metabolic and immune factors. |
| Hence we undertook a study of objective parameters that used a rapid non-invasive analysis of the body composition using the tools of the BIA-ACC project [38-40]. In Italy, “the BIA-ACC project” (Bioelectric Impedance Analyzer - Analisi Composizione Corporea) is a large-scale research project launched in 2004 to redefine the application of bio impedance measurement in the clinical setting. Body composition analysis based on the measurement of bio-impedance is widely used, and has successfully been through several validation processes in nephrology, nutrition, sports and preventive medicine, yet much of the potential of this technique is still unknown because of early compartmentalization of clinical and technical research [38]. |
| Data are furnished to inform the doctor upon the first visit regarding the state of health of the patient with MUS and obesity and guide medical therapy. Thus we analyzed, in presence of decreasing BMI, the changes in Fat Mass (FM) and Fat-free Mass (FFM) in relation to all the other variables provided by a novel advanced bio-impedance device that takes advantage from numerous parameters of body composition. Finally, we attempted to confirm whether repeated body composition analysis may be an effective method to improve the ability of patients with MUS to maintain achieved weight loss over a period of time. |
| Materials and Methods |
| Patients |
| Patients enrolled at the center for primary care for a routine checkup, in collaboration with the Department of Experimental Medicine, all apparently free of disease but with problems of excess weight were administered a self-evaluation form to point out MUS. |
| Inclusion criteria for MUS were: persistent tiredness or fatigue; mood disorders; insomnia for a long time or night-time awakenings; anxiety; apathy; melancholic depression; panic attacks; perceived increases in heart rate at rest; changes in appetite (excessive hunger or lack of appetite); acidity and stomach pain, feeling of fullness, bloating after every meal, nausea; irritable bowel; persistent bouts of constipation; hands and feet always cold; impaired body perspiration during sleep. |
| The evaluation of the parameters BIA-ACC was performed both at the first visit, T0, and after weight loss of at least 5% of initial weight identified as time T1, according to a standard nutritional strategy. Of all the patients with MUS, only those with decreasing BMI were selected for evaluation with BIA-ACC, resulting in the cohort under study: 109 patients 79 females and 30 males aged between 30 and 70 years. The protocol was approved by the locally appointed ethics committees and participants gave written informed consent. |
| Instrumentation |
| Bioelectrical impedance analysis, BIA-ACC was performed by a measurement device by BioTekna, Inc. (Marcon-Venice Italy). This device applies two alternating currents with two different frequencies at 50 kHz and 1.5 kHz (bi-frequency measurement method). The device uses a multi-compartment model for body composition (2C, 3C, 4C, 5C). The BIA-ACC tool is applicable to both adults and children of all ages and both sexes. The patient lies supine on a flat surface that is nonconducting nor in contact with metallic elements. Two electrodes are applied on the dorsal surface of the right hand and two electrodes on the dorsal surface of the right foot. |
| On established healthy nomograms, BIA-ACC clearly is able to distinguish healthy from metabolically diseased subjects at multiple parameters. BIA-ACC consents assessment of potential pathologies such as chronic inflammation, MUS, stress and neuro-immunoregulation, thanks to large clinical data sets collection, which highlight correlations that were not observed previously. The BIA-ACC system is designed for connection to remote telematic services: the web portal DINU (DI NUtrizione) uses a set of mathematical formulation to expand the BIA-ACC output through new analytical processing algorithms which are able to point out the strong relationships between bio impedance-derived parameters and other diagnostics indexes that are generally gathered by other measurement technologies, including invasive or expensive ones [38-42]. |
| The supplied parameters are: |
| BMI (Body Mass Index): It is usually calculated by dividing the weight of an individual in kilograms by his/her height given in meter square. |
| TBW (Total Body Water): Indicates the amount of total body water, expressed in liters and in percentage compared to the total weight of the patient, is the overall percentage of body fluids compared to the total weight of the subject; physiological values are considered those between 60% and 70% (during childhood the value reaches to 77%. |
| ECW (Extracellular Water): Amount of water present in the extracellular environment. |
| ICW (Intracellular Water): Amount of water present in the intracellular environment, expressed in liters and as a percentage of total body water (TBW). The ICW and ECW used to assess the relationship of distribution of body fluids between the intra-and extracellular compartments, the two values are in the physiological relationship when the ICW is 60% to 40% and ECW. |
| FFM (Fat Free Mass): Amount of lean mass present in the body, expressed in kilograms and in percentage compared to the total weight of the patient. |
| FM (Fat Mass): Amount of fat present in the body, expressed in kilograms and in percentage compared to the total weight of the patient. FFM and FM represent the percentage of lean body mass and fat mass compared to the total weight of the subject, in normal conditions the FM should not exceed 25% of body weight, so the value of the FFM should constitute at least 75% of the total weight. |
| BMR (Basal Metabolic Rate): Basal metabolic rate (expressed in kcal per day). |
| PA (Phase Angle): The phase angle is a measure, expressed in degrees, of the relationship between resistance and capacitive reactance. A very low value indicates a system with cell membranes poorly undamaged, while a very high degree indicates a system with intact membranes and a good cell mass. The value of this parameter has a significant relationship with the sex of the subject analyzed, hence a difference in the ideal value of at least 6° for men and at least 5° for women. It is an important prognostic indicator for monitoring the presence and evolution of chronic inflammatory processes in the course of stress. |
| The web portal DINU determines the other BIA-ACC parameters: Na, K, Cl, Ca, Mg, TBP (phosphates), glycogen (Gly), bone mineral; body cell mass (BCM), active cell mass (ACM), muscle FFM (skeletal muscle in Kg), muscle ratio (skeletal muscle % of FFM), muscle FFM/ FM ratio ( fitness index); anions protein, extracellular matrix proteins (ECM) and catabolites in the extracellular fluids; essential lipids (Le), adipose tissue (AT) and abdominal adipose tissue (AAT). |
| Statistical evaluation |
| All the parameter changes relate to the time of enrollment (T0) and after weight loss (T1) have been normalized with respect to the mean value and standard deviation of changes (Z-score normalization). Then, we performed the Student’s t-tests and bi-hierarchical clustering, using as distance one minus Pearson’s correlation, to classify both patients according to variation of the variables and variables according to their variations in all patients. |
| The statistical program SAS (Statistical Analysis System) was used to perform the following tests: |
| • Student’s t-test to measure the difference in the average values of the parameter changes from T0 to T1, using as a significance threshold a p-value<0.05. |
| • Principal Component Analysis (PCA) is a technique for simplification of the data used in multivariate statistics and belongs to factor analysis. The primary purpose of this technique is the reduction of a greater or lesser number of variables (representing many features of the phenomenon) in some latent variables (feature reduction). This is achieved through a linear transformation of the variables that projects those originating in a new Cartesian system in which the new variable with the greatest variance is projected on the first axis, the new variable, the second dimension for the variance, second axis and so on. The reduction of complexity occurs when analyzing the main components that explain most of the variance of the data. |
| • ANOVA to compare two or more groups of data comparing the internal variability in these groups with the variability between groups. We use these techniques when the explanatory variables are nominal type as in the case of sex, of sarcopenia and cardiovascular risk. We used ANOVA to test the correlation between these variables and the nominal principal components. |
| Results |
| Statistical analysis has demonstrated that the variance of the data around the mean is minimal. Therefore, differences in mean values between T0 and T1 are significant as described from the 33 parameters considered. All patients examined at the first visit and after standard nutritional strategy reduced their weight and consequently their BMI. |
| In Table 1, we report the values of principal demographic characteristic of the patients (age, gender, physical activity, etc...) at the time of enrolment (T0), and the variability range of the principal parameters both at the time of enrolment and after a follow-up of about 2 months (T1). |
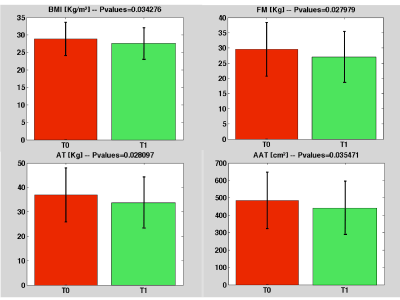
| 60% of the patients at the first visit indicated the following MUS: persistent tiredness or fatigue; insomnia or night-time awakenings; anxiety; apathy; changes in appetite (excessive hunger); feeling of fullness, bloating after every meal, irritable bowel. At the subsequent visit (T1) only 7.3% of patients continued to complain about the persistence of the following MUS: tiredness; insomnia; anxiety. However it is interesting to note the significant decrease in FM, AT, and especially AAT in all patients examined-an observation that might be directly related to inflammatory processes that were low-grade but persistent at the basis of the MUS as in Figure 1. |
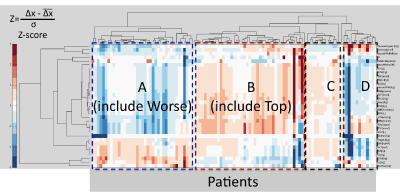
| The results of the cluster analysis are shown in Figure 2 where the red color represents a greater variation in the parameter changes compared to the average value; the white color corresponds to parameter changes equal to the average value; the blue color represents a decrease of the parameter changes with respect to the average value. |
| The hierarchical clustering performed on the 33 variables reveals a clear separation into two groups: one related to the FFM and the other related to FM. On the basis of this variable classification patients fell into four groups, as follows: A) FFM and all related components change less than the average while FM and all related components change greater than the average; B) FFM and all related components change greater than the average while FM and all related components change less than the average; C) FFM and all related components as well as FM and all related components change greater than the average; D) FFM and all related components as well as FM and all related components change less than the average. This result clearly indicates that all patients who have reduced weight and BMI did not diminish the only FM but the weight loss has also come at the expense of the FFM. |
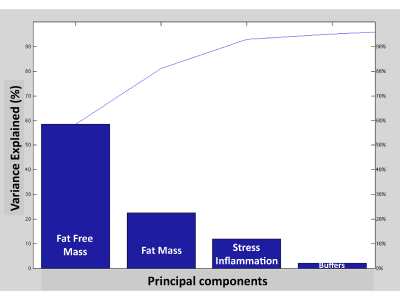
| The principal components analysis (PCA) revealed that the first 4 main components explain nearly all (95%) of the information present in the original variables differential (delta). This means that there exists 4 “reasons” or factors which explain the variability in the 33 parameters studied. In particular two explain 80% of these variations (Figure 3). Correlation analysis between each of the 33 variables with the first two principal components identifies the first PCA with the FFM (i.e. TBP, TBMg, TBCa, TBW, BCM, BMR, ACM and skeletal muscle) and the second (PCA2) is associated with adipose tissue (i.e. AT, FM, AAT). |
| This means that FFM and adipose tissue are the main reasons of the variation of this parameter of the patient cohort. Finally, the remaining 20% of the parameter variation can be explained by variation in the third and four principal components that are highly correlated with stress or inflammation (i.e. k/mg ratio and the phase angle PA) and buffer, respectively (Figure 3). |
| Given the importance of the FFM, we divided the patients according to the variation of this parameter, and we retrieved 3 different subgroups in response to the decrease in BMI (Figure 4): |
| • Patients who lost FM and FFM, even if the loss of FFM is minimal (labeled “Others”, corresponding to 75.23% of the cohort). |
| • Patients who lost FM but keep constant or increase FFM (labeled “Top”, 17.43%). |
| • Patients who lost FFM (labeled “Worse”, 7.34%) with persistent MUS: tiredness, insomnia, anxiety. |
| The group “Top” not only increased FFM in general but especially skeletal muscle mass; in contrast the group “Worse” showed losses in FFM especially skeletal muscle mass (Figure 5). |
| About cardiovascular risk (CVR), this parameter decreased at T1 in the groups “Top” and “Others” while remaining unchanged in the group “Worse” (data not shown). Patients who responded better to nutritional strategy indicated they had changed their lifestyle introducing a moderate physical activity. |
| Discussion |
| The results described in this paper and interpreted in the light of modern scientific knowledge confirm that weight loss improves all the parameters that underlie metabolic alteration, obesity with risk of chronic diseases. In fact, in addition to the total fat and especially visceral fat we found decreased extracellular water and sodium, indicators of edema/inflammation; catabolites of the extracellular matrix considered “danger signals” that can activate macrophages through Toll-likeR4 causing neurogenic inflammation and that determine adipogenesis in mesenchymal precursors [43,44]. |
| Undoubtedly important is the role of bio-psychological connection between stress and dysregulation of the feeding system that may explain how many environmental stimuli can affect the destabilization of the lipostatic system [45,46]. For all these reasons we can explain why in Italy, as in the Western world (with higher incidence in North America and Great Britain), the problem of body weight, defined as being overweight, affects more and more individuals [1,47]. |
| The cause of this situation is twofold: on one hand there is an increasing availability of food, the other a increasingly sedentary lifestyle [48,49]. Certain life cycle phases appear to be especially important for health promotion and disease prevention as the development of chronic diseases can take several decades. Such complex health issues often require system-wide, multifactorial, and multidisciplinary solutions [50]. |
| Our findings are in accordance with the Position Statement of the Academy of Nutrition and Dietetics which states that primary prevention is the most effective, affordable method to prevent chronic disease, and that dietary intervention positively impacts health outcomes across the life span [50]. In this regard it should be noted that caloric restriction by a standard nutritional therapy is not accepted by all patients, who turn to a specialist nutritionist for help. Such lack of success can be therefore considered a stress [51,52] and recent data indicate that combined physical activity and dietary intervention was not effective at improving diet or physical activity level [53]. In fact, in this study, the largest group, despite having decreased fat mass, has somehow lost part of lean body mass and this phenomenon is often related to the presence of stressful processes, such as body dissatisfaction [54], inflammatory processes, activating the immune system which requires additional energy from other organs and systems [15-17]. This observation is more prevalent in the group of patients who responded worst to dietary restriction in which it is found that the weight loss coincides only with the loss of lean body mass and sarcopenia with varying degrees of MUS and cardiovascular risk. |
| Therefore, a preventive intervention that focusing on lifestyle modification and energy balance and helps to maintain healthy weight compared with surgery and medications is thus highly cost-effective. Standard care with physician advice-giving can cause resistance to change, especially when the patient has little or no willingness to change [55]. For this reason we recommend, according to the analysis of body composition, an appropriate and personalized nutritional protocol for each individual and to follow subsequent check-ups at brief intervals [56]. We recall in this regard the recent words of Umberto Veronesi: “The 4 P that characterize the medicine of the future are Predictive, Preventive, Personalized and Participatory” [57]. |
| In addition, this study emphasizes another new concept: the role of the preservation of FFM especially skeletal muscle during weight loss management. When we compared the parameters most indicative for stress and inflammation in the 2 groups of patients with different approach to weight loss: best (Top) and worst (Worse) which is already possible to distinguish in the dendrogram. Stress and an improper nutrition result in an altered body composition at the expense of lean body mass (FFM) composed overwhelmingly of muscle and bone tissue, alteration of extracellular pH, with a tendency to acidosis that perpetuate the request of alkalizing buffers mainly to the detriment of bone. We should recall that the k/mg ratio stabilizes lean mass and in patients with index less than 4.3 we found sarcopenia and osteopenia for probable loss of action potentials aggravated by the presence of stress. |
| The activity of the HPA axis is highlighted by the decrease of Tbprotein, TbK, PA with concomitant increase of ECK, ECW. This phenomenon is at the basis of the MUS concerning psychological (depression), muscular (fatigue, cramping) gastrointestinal alterations (reflux, irritable bowel syndrome), are all related to immunometabolic alteration recently described as a new field of study called “immunometabolism” [58,59]. The loss of skeletal muscle leads to a decrease of TBK where is contained for the most part. Therefore, the recovery of TBK can be obtained with the recovery of the skeletal muscle and proteins [6,15,38,60-63]. |
| Conclusion |
| This study, although preliminary, suggests three important findings. |
| i. BMI shows several limitations as indicator of fatness. Individuals with increased skeletal muscle may have increased BMI; and individuals with decreased FFM and increased adiposity may be misclassified by assessment with BMI; this index does not measure the accumulation of abdominal fat, which mainly increases the risk of diabetes, hypertension and cardiovascular diseases; finally BMI is relatively insensible to body composition changes. |
| ii. It is well known that psychological stress contributes to exacerbations of inflammatory conditions accumulating AAT. Advanced bio-impedance analysis provides a useful, bloodless and rapid tool in the clinical setting, especially in the early stages when the first signs of immune-metabolic dysregulation are only MUS. It correlates MUS with negative changes in body composition. |
| iii. Among all the parameters analyzed it was possible with the statistical analysis to highlight 4 main components that affect the variation between the first visit (T0) and subsequent control (T1). Unexpectedly, the decrease of FM is not as important in reducing the MUS as the retention or increase of FFM. In fact our data furnish the Fitness index defined as Muscle FFM/FM ratio. |
| Our results emphasize that during weight loss strategy the most important component is FFM with total body water, phosphates, calcium and magnesium, and mostly skeletal muscle, followed by adipose tissue. Only third in importance is the result on phase angle and k/mg ratio, which is an indirect indicator of stress and inflammation. In this regard recently the association of body composition measurements was evaluated using the same advanced BIA-ACC device with chronic stress-inflammatory biomarkers in a large Caucasian population of 160,768 subjects [40]. |
| In this way we can identify patients with chronic stress and inflammation related chronic diseases, such as metabolic syndrome and its manifestations and sequelae, and distinguish them from lean or overweight healthy subjects. Therefore, to obtain best results, the specialist nutritionist should always be concerned more with an individual nutritional strategy than with caloric restriction alone. Besides this, during subsequent check-up, patients need to be willing to accept and be compliant in regards to all requirements of a behavioral weight loss program including: self monitoring, physical activity, addressing personal barriers to their own weight loss, committing to improved diet and lifestyle changes both during and after weight loss, participation in individual and group sessions, and strategizing how to maintain lifestyle changes [61-63]. |
| Recent data suggest that muscle contraction induces the release of cytokine-like molecules namely “myokines” which, like hormones, counteract inflammation related to AAT by stimulating fat oxidation [64,65]. In our opinion, BIA-ACC can readily reveal to the patient himself an objective improvement or worsening of the different subcomponents of body composition during nutritional strategy. In addition, we suggest the use of BIA-ACC to obtain diagnostic and prognostic parameters in neuro-immune dysfunctions that induce chronic diseases. Finally, our work may stimulate further studies related to the role of the skeletal muscle as a new or additional endocrine system. |
| Future Directions |
| Based on the review of literature, there are still several areas that could benefit from further research, for example, to evaluate how patient compliance with published guidelines [50] affects the rate of weight loss. We are currently studying how different levels of physical activity affect weight loss. Regular physical activity that allows muscle contraction through resistance training leading to muscle hypertrophy rather than aerobic exercise, tailored to suit patient capability and with increasing intensity, is fundamental to stimulate an optimal restoration of skeletal muscle mass and immune system, an integral part of the FFM. This important measure, which is now supported by experimental work, allows the patient to deal with and better manage the various daily stressors. |
| Acknowledgements |
| We thank Dr. Philippa Mungra for the revision of the manuscript. |
References
- Micciolo R, Canal L, Minniti A, Mazzali G, Fantin F, et al. (2013) The association between excess weight and comorbidity and self-rated health in the Italian population. Ann Epidemiol 23: 172-178.
- Siervo M, Wells JC, Cizza G (2009) The contribution of psychosocial stress to the obesity epidemic: an evolutionary approach. Horm Metab Res 41: 261-270.
- Black PH (2006) The inflammatory consequences of psychologic stress: relationship to insulin resistance, obesity, atherosclerosis and diabetes mellitus, type II. Med Hypotheses 67: 879-891.
- Chrousos GP, Gold PW (1992) The concepts of stress and stress system disorders. Overview of physical and behavioral homeostasis. JAMA 267: 1244-1252.
- Chrousos GP (2009) Stress and disorders of the stress system. Nat Rev Endocrinol 5: 374-381.
- Ippoliti F, Canitano N, Businaro R (2013) Stress and obesity as risk factors in cardiovascular diseases: a neuroimmune perspective. J Neuroimmune Pharmacol 8: 212-226.
- Nimnuan C, Hotopf M, Wessely S (2001) Medically unexplained symptoms: an epidemiological study in seven specialities. J Psychosom Res 51: 361-367.
- Ivetic V, Kersnik J, Klemenc-Ketis Z, Svab I, Kolsek M, et al. (2013) Opinions of Slovenian family physicians on medically unexplained symptoms: a qualitative study. J Int Med Res 41: 705-715.
- Galimberti U (2009) Man in the age of technology. J Anal Psychol 54: 3-17.
- Kuo LE, Czarnecka M, Kitlinska JB, Tilan JU, Kvetnansky R, et al. (2008) Chronic stress, combined with a high-fat/high-sugar diet, shifts sympathetic signaling toward neuropeptide Y and leads to obesity and the metabolic syndrome. Ann N Y Acad Sci 1148: 232-237.
- Kyrou I, Chrousos GP, Tsigos C (2006) Stress, visceral obesity, and metabolic complications. Ann N Y Acad Sci 1083: 77-110.
- Matarese G, La Cava A (2004) The intricate interface between immune system and metabolism. Trends Immunol 25: 193-200.
- Matarese G, Procaccini C, Menale C, Kim JG, Kim JD, et al. (2013) Hunger-promoting hypothalamic neurons modulate effector and regulatory T-cell responses. Proc Natl Acad Sci U S A 110: 6193-6198.
- Bollyky PL, Falk BA, Wu RP, Buckner JH, Wight TN, et al. (2009) Intact extracellular matrix and the maintenance of immune tolerance: high molecular weight hyaluronan promotes persistence of induced CD4+CD25+ regulatory T cells. J Leukoc Biol 86: 567-572.
- Straub RH, Cutolo M, Buttgereit F, Pongratz G (2010) Energy regulation and neuroendocrine-immune control in chronic inflammatory diseases. J Intern Med 267: 543-560.
- Straub RH (2011) Concepts of evolutionary medicine and energy regulation contribute to the etiology of systemic chronic inflammatory diseases. Brain Behav Immun 25: 1-5.
- Straub RH (2012) Evolutionary medicine and chronic inflammatory state--known and new concepts in pathophysiology. J Mol Med (Berl) 90: 523-534.
- Ho RC, Neo LF, Chua AN, Cheak AA, Mak A (2010) Research on psychoneuroimmunology: does stress influence immunity and cause coronary artery disease? Ann Acad Med Singapore 39: 191-196.
- Chrousos GP, Kino T (2009) Glucocorticoid signaling in the cell. Expanding clinical implications to complex human behavioral and somatic disorders. Ann N Y Acad Sci 1179: 153-166.
- Gustafson B (2010) Adipose tissue, inflammation and atherosclerosis. J Atheroscler Thromb 17: 332-341.
- Elenkov IJ, Iezzoni DG, Daly A, Harris AG, Chrousos GP (2005) Cytokine dysregulation, inflammation and well-being. Neuroimmunomodulation 12: 255-269.
- Wardle J, Steptoe A, Oliver G, Lipsey Z (2000) Stress, dietary restraint and food intake. J Psychosom Res 48: 195-202.
- Nyberg ST, Fransson EI, Heikkila K, Alfredsson L, Casini A, et al. (2013) Job Strain and Cardiovascular Disease Risk Factors: Meta-Analysis of Individual- Participant Data from 47,000 Men And Women. Plos One 8: e67323.
- Businaro R, Ippoliti F, Ricci S, Canitano N, Fuso A (2012) Alzheimer's disease promotion by obesity: induced mechanisms-molecular links and perspectives. Curr Gerontol Geriatr Res 2012: 986823.
- Vachharajani V, Granger DN (2009) Adipose tissue: a motor for the inflammation associated with obesity. IUBMB Life 61: 424-430.
- Wajchenberg BL (2000) Subcutaneous and visceral adipose tissue: their relation to the metabolic syndrome. Endocr Rev 21: 697-738.
- Warne JP, Dallman MF (2007) Stress, diet and abdominal obesity: Y? Nat Med 13: 781-783.
- Warne JP (2009) Shaping the stress response: interplay of palatable food choices, glucocorticoids, insulin and abdominal obesity. Mol Cell Endocrinol 300: 137-146.
- Ibrahim MM (2010) Subcutaneous and visceral adipose tissue: structural and functional differences. Obes Rev 11: 11-18.
- Libby P, Okamoto Y, Rocha VZ, Folco E (2010) Inflammation in atherosclerosis: transition from theory to practice. Circ J 74: 213-220.
- Reaven GM (2011) Insulin resistance: the link between obesity and cardiovascular disease. Med Clin North Am 95: 875-892.
- Enriori PJ, Evans AE, Sinnayah P, Cowley MA (2006) Leptin Resistance and Obesity. Endocr J 14: 254S-258S.
- Xu H, Barnes GT, Yang Q, Tan G, Yang D, et al. (2003) Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112: 1821-1830.
- Capeau J, Magré J, Lascols O, Caron M, Béréziat V, et al. (2005) Diseases of adipose tissue: genetic and acquired lipodystrophies. Biochem Soc Trans 33: 1073-1077.
- Hu G, Tuomilehto J, Silventoinen K, Sarti C, Männistö S, et al. (2007) Body mass index, waist circumference, and waist-hip ratio on the risk of total and type-specific stroke. Arch Intern Med 167: 1420-1427.
- Blijdorp K, van den Heuvel-Eibrink MM, Pieters R, Boot AM, Delhanty PJ, et al. (2012) Obesity is underestimated using body mass index and waist-hip ratio in long-term adult survivors of childhood cancer. Plos One 7: e43269.
- Bibiloni Mdel M, Pons A, Tur JA (2013) Defining body fatness in adolescents: a proposal of the AFAD-A classification. Plos One 8: e55849.
- Ippoliti F, Boschiero D (2013) A Simple Non-Invasive Screening to Prevent Obesity through Body Composition Analysis (BIA-ACC). J Obes Wt Loss Ther 3: 169.
- Di Rienzo V, Minelli M, Sambugaro R, Agostinis F, Nucera E, et al. (2007) Applicability of extracellular electrical impedance tomography in monitoring respiratory tract inflammation. J Investig Allergol Clin Immunol 17: 34-38.
- Stefanaki C, Boschiero D, Chrousos GP (2013) Stress, Inflammatory and Metabolic Biomarkers Correlate with Bio-Impedance Measurements Obtained with Novel, Advanced Bio-Impedance Analyser (BIA-ACC): A Cross-Sectional Study in Healthy And Diseased Caucasians. Endocr Rev 34: FP32-3.
- Kyle UG, Bosaeus I, De Lorenzo AD, Deurenberg P, Elia M, et al. (2004) Bioelectrical impedance analysis-part I: review of principles and methods. Clin Nutr 23: 1226-1243.
- Jaffrin MY, Morel H (2008) Body fluid volumes measurements by impedance: A review of bioimpedance spectroscopy (BIS) and bioimpedance analysis (BIA) methods. Med Eng Phys 30: 1257-1269.
- Caso JR, Pradillo JM, Hurtado O, Leza JC, Moro MA, et al. (2008) Toll-like receptor 4 is involved in subacute stress-induced neuroinflammation and in the worsening of experimental stroke. Stroke 39: 1314-1320.
- Mauney J, Volloch V (2010) Human bone marrow-derived stromal cells show highly efficient stress-resistant adipogenesis on denatured collagen IV matrix but not on its native counterpart: Implications for obesity. Matrix Biol 29:9-14.
- Breitling R (2009) Robust signaling networks of the adipose secretome. Trends Endocrinol Metab 20: 1-7.
- Berthoud HR (2012) The neurobiology of food intake in an obesogenic environment. Proc Nutr Soc 71: 478-487.
- Relatic KS (2012) Overweight and Obesity. J Obes Wt Loss Ther S1: e001.
- Adam TC, Epel ES (2007) Stress, eating and the reward system. Physiol Behav 91: 449-458.
- Tsatsoulis A, Mantzaris MD, Bellou S, Andrikoula M (2013) Insulin resistance: an adaptive mechanism becomes maladaptive in the current environment - an evolutionary perspective. Metabolism 62: 622-633.
- Fitzgerald N, Morgan KT, Slawson DL (2013) Practice Paper of the Academy of Nutrition and Dietetics Abstract: The Role of Nutrition in Health Promotion and Chronic Disease Prevention. J Acad Nutr Diet 117: 983.
- Capuron L, Su S, Miller AH, Bremner JD, Goldberg J, et al. (2008) Depressive symptoms and metabolic syndrome: is inflammation the underlying link? Biol Psychiatry 64: 896-900.
- Capuron L, Poitou C, Machaux-Tholliez D, Frochot V, Bouillot JL, et al. (2011) Relationship between adiposity, emotional status and eating behaviour in obese women: role of inflammation. Psychol Med 41: 1517-1528.
- Soon HK, Saad HA, Taib MN, Rahman HA, Mun CY (2013) Effects of combined physical activity and dietary intervention on obesity and metabolic parameters in adults with abdominal obesity. Southeast Asian J Trop Med Public Health 44: 295-308.
- Siervo M, Montagnese C, Muscariello E, Evans E, Stephan BC, et al. (2013) Weight loss expectations and body dissatisfaction in young women attempting to lose weight. J Hum Nutr Diet .
- Zeidi IM, Hajiagha AP (2013) Effect of Motivational Interviewing on Eating Habits and Weight Losing among Obese and Overweight Women. J Obes Weight Loss Ther 3: 172.
- Fallaize R, Macready AL, Butler LT, Ellis JA, Lovegrove JA (2013) An insight into the public acceptance of nutrigenomic-based personalised nutrition. Nutr Res Rev 26: 39-48.
- Veronesi U (2013) www.mdwebtv.it
- Schipper HS, Prakken B, Kalkhoven E, Boes M (2012) Adipose tissue-resident immune cells: key players in immunometabolism. Trends Endocrinol Metab 23: 407-415.
- Granger A, Emambokus N (2013) Focus on immunometabolism. Cell Metab 17: 807.
- Boudreault L, Cifelli C, Bourassa F, Scott K, Renaud JM (2010) Fatigue preconditioning increases fatigue resistance in mouse flexor digitorum brevis muscles with non-functioning K(ATP) channels. J Physiol 588: 4549-4562.
- Esch T, Stefano GB (2010) Endogenous reward mechanisms and their importance in stress reduction, exercise and the brain. Arch Med Sci 6: 447-455.
- Houston K (2013) A Systematic Review of Literature on the Effectiveness of Behavioral Weight Loss Programs to Achieve Weight Reduction. J Obes Wt Loss Ther 3: 156.
- Balducci S, Zanuso S, Cardelli P, Salvi L, Bazuro A, et al. (2012) Effect of High-Versus Low-Intensity Supervised Aerobic and Resistance Training on Modifiable Cardiovascular Risk Factors in Type 2 Diabetes; The Italian Diabetes and Exercise Study (IDES). Plos One 7: e49297.
- Pedersen BK (2011) Exercise-induced myokines and their role in chronic diseases. Brain Behav Immun 25: 811-816.
- Pedersen BK, Febbraio MA (2012) Muscles, exercise and obesity: skeletal muscle as a secretory organ. Nat Rev Endocrinol 8: 457-465.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Android Obesity
- Anti Obesity Medication
- Bariatric Surgery
- Best Ways to Lose Weight
- Body Mass Index (BMI)
- Child Obesity Statistics
- Comorbidities of Obesity
- Diabetes and Obesity
- Diabetic Diet
- Diet
- Etiology of Obesity
- Exogenous Obesity
- Fat Burning Foods
- Gastric By-pass Surgery
- Genetics of Obesity
- Global Obesity Statistics
- Gynoid Obesity
- Junk Food and Childhood Obesity
- Obesity
- Obesity and Cancer
- Obesity and Nutrition
- Obesity and Sleep Apnea
- Obesity Complications
- Obesity in Pregnancy
- Obesity in United States
- Visceral Obesity
- Weight Loss
- Weight Loss Clinics
- Weight Loss Supplements
- Weight Management Programs
Recommended Journals
Article Tools
Article Usage
- Total views: 14469
- [From(publication date):
October-2013 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 9841
- PDF downloads : 4628
