Review Article Open Access
IBD Impact of Colonic pH, Onset of Action and other Factors in Modern Therapeutic Approach
Newton AMJ* and Kumar N
Rayat Bahra Institute of Pharmacy, Rayat–Bahra University, Punjab, India
- *Corresponding Author:
- Newton AMJ
Institute of Pharmacy
Rayat–Bahra University
Punjab, India
Tel: +919963638468
E-mail: mariajohnnewton@gmail.com
Received date: October 01, 2014; Accepted date: October 29, 2014; Published date: October 31, 2014
Citation: Newton AMJ, Kumar N (2014) IBD–Impact of Colonic pH, Onset of Action and other Factors in Modern Therapeutic Approach. Microinflammation 1:116. doi: 10.4172/2381-8727.1000116
Copyright: © Newton AMJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at International Journal of Inflammation, Cancer and Integrative Therapy
Abstract
Pharmacotherapy rediscovered the management of ulcerative colitis and Crohn’s disease. Novel drug delivery systems are popular in treating IBD. The treatment of IBD with novel drug delivery system and other medicines involves complicated mechanism. The onset of action, pH conditions of the colon in normal and diseased condition of the patient and adverse effects of the drugs makes the greatest impact in designing successful IBD therapy.
Keywords
Inflammatory bowel disease; Crohn’s disease; Diarrhea; Hypokalemia
Introduction
Inflammatory bowel disease (IBD) is an idiopathic disease. Novel drug delivery systems are very successful in the treatment of colonic diseases. The colonic environment can be explored for local and systemic delivery of drugs and other bioactive compounds such as hormones, insulin, vasopressin and other plant ingredients. The colon is the major region of the GIT. The common colonic disease such as diverticular inflammatory bowel disease (IBD) which includes Crohn’s disease and ulcerative colitis, colitis ulcerosa diversional colitis, ischemic colitis, colon cancer and lymphoma of the colon can be treated successfully by modern therapeutic approaches. In past decades the general pathophysiology of inflammatory bowel disease was described on the basis of clinical manifestation. The investigators and clinicians are struggled to provide the effective therapy for IBD due to its dismaying clinical manifestation The causes of inflammatory bowel disease is multi factorial and may be resulted from inappropriate activation of mucosal immune system, inflammatory responses, generic factors, candidate genes, chromosome location etc., The infectious organism such as Escherichia coli, measles virus, cytomegalo virus and factor like saturated fats, milk products, allergic foods may also be the cause of the IBD. General pathophysiology of ulcerative colitis and Crohn’s disease is limited to large intestine often inflammation and ulcers occurs in the inner lining of the large intestine or in mucosal layer. The ulcerative colitis resulting in diarrhea, blood and pus. Crohn’s disease, otherwise called regional enteritis. Crohn’s disease involves any part of the gastrointestinal tract from mouth to anus with the inflammation extending through the bowel wall to the serosal surface. Both the diseases used to have waxing and waning intensity and severity [1-3].
Crohn’s disease and ulcerative colitis significantly differ from each. The treatment methods are common to both the diseases. Many extra intestinal manifestations are shared by both the diseases occurs in adults and children. The signs and symptoms of ulcerative colitis involves diarrhea with the presence of blood and mucus. Weight loss, abdominal pain, painful bowel movements, abdominal cramps and extra intestinal symptoms like arthritic knees may be observed in youngsters. The pathophysiology of ulcerative colitis showed an increased amount of colonic sulfate reducing bacteria. This may be due to the result of higher concentration of hydrogen sulfide toxic gas. Some reports suggested that sulfur containing red meat, alcohol consumption also increased the disease relapsing in patients in remission. The ulcerative colitis occur in 38-100 for every 100,000 in the US. The disease occurs predominantly in northern countries 0.1% population. Ulcerative colitis has no known cause and it is treated as autoimmune disease.
General pathophysiology of IBD
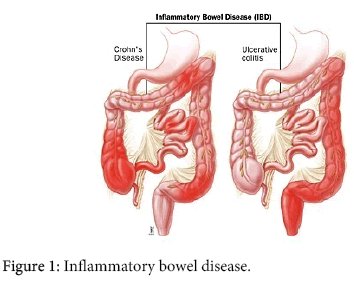
The pathophysiology of IBD is yet to be revealed. The IBD is still under active research for its cause. The general pathway is the inflammation of the mucosal lining of the intestinal tract, which causes ulceration, edema, bleeding associated with fluid and electrolyte loss. The researches have been struggling to identify the gene involved in beginning of IBD. The early linkage discovered was on chromosome 16 (IBD 1 gene). The identification of ‘IBD 1 gene’ leads to the identification of NOD2 gene also called as CARD 15 which was declared as the first gene clearly associated with IBD. This gene also has the susceptibility to Crohn’s disease. Studies also identified the susceptibility genes on chromosome 5 and 6 (5Q31, 6P21, 19P). CARD 15 is a polymorphic gene involved in the innate immune system, which show 60 different variations. Three of these variants played a vital role in IBD development. This means that these genes allowing the IBD to occur, but not a causative source. The main point to be considered here is a presence of genes does not develop the disease, but may allow the disease to occur (Figure 1).
Diagnosis and endoscopy
H and E biopsy of colonic tissue usually showing the crypts. Abscess is an indicator for ulcerative colitis. The initial blood diagnostic tests involves blood count test for the assessment of anemia, thrombocytosis, high platelet count, the renal function test, test for chronic diarrhea associated with hypokalemia, hypomagnesemia, liver function test, primary sclerosing cholangitis, X ray, urine analysis also used as a diagnostic tool to investigate ulcerative colitis. Endoscopy is the best available tool to diagnose for ulcerative colitis. The endoscopy reveals the loss of vascular appearance of the colon and also identifies erythema and damaged mucosa, superficial ulceration and pseudopolyps in the colon [4].
Management of IBD
The treatment approaches depending on the severity of the disease. Pharmacotherapy is significantly successful in the treatment of ulcerative colitis. The optimized medical approach differs with a physician. The main objective of the treatment is to induce the remission followed by the maintenance therapy to prevent relapse. The drug treatment involves aminosalicylates such as sulfasalsasine cortico steroids (Prednisolone), immune suppressive agents (azathioprine) and biological agents such as infliximab. Ulcerative colitis generally be cured by surgical removal of the large intestine, which is not recommended in the early stages. Drug delivery systems with modified and targeted drug delivery to the site and prodrugs approach can also successfully used in IBD management. The list of the drugs approved commonly for ulcerative colitis and Crohn’s are given below [5] (Table 1).
| Corticosteroids | hydrocortisone, methylprednisolone, Prednisolone as I.V route, oral or retention enemas. |
| 5-Aminosalicylic acid compounds | Sulphasalazine combination of sulphapyridine and 5-aminosalicylic acid joined by an ace - bond. Poorly absorbed, split by bacteria in the colon. 5-ASA part is the active moiety; sulphapyridine part can cause sulfonamide toxicity. Reduces relapses in UC and used for treatment of exacerbations. |
| Mesalamine | 5-ASA. Delayed release, pH-dependent preparations to allow release in the colon. Better tolerated than sulphasalazine, but still carries risk of hematological side effects. |
| Olsalazine | 2 molecules of 5-ASA linked by azo-bond split by colon bacteria. |
| Balsalazide | prodrug of 5-ASA |
| Immunosuppressants | Azathioprine |
| Metronidazole | Perianal Crohn’s disease. |
| Infliximab | For severe active Crohn’s disease refractory to treatment with steroids . |
| Monoclonal Antibody | Inhibits the pro-inflammatory cytokine TNF-α. |
| NSAID | Ibuprofen, Diclofenac, Indomethacin Analgesic – rapid (full effect within 1 week) Anti-inflammatory (full effect within 3 weeks) |
Table 1: List of the drugs approved commonly for ulcerative colitis and Crohn’s.
Various studies on colonic pH conditions
The various studies conducted worldwide by following different techniques registered the pH changes in normal and IBD colon. The Table 2 displays the colonic pH conditions in the normal healthy volunteer patient with ulcerative colitis and Crohn's disease studied by various reserarchers. Changes in the intestine and colonic pH also considered as an important factor in the treatment of ulcerative colitis and IBD. The design and development of novel treatment and novel drug delivery systems are also significantly influenced by the changes in the luminal pH conditions and that should be considered in the treatment of IBD. The formulation also developed to deliver an active agent directly to the inflammation site. This approach reduces the absorption of drugs in the upper GI tract as well as the systemic side effects. This method involves pH dependent drug delivery systems (Asacol, Mesacol and Salofalk). Another common technique involves bacterial enzymatic metabolism (sulphasalazine, olsalazine and balsalazide) which also affected by changes in colonic pH.
| S.no | Study | Patient | Smallbowel pH | Colonic pH | ||
|---|---|---|---|---|---|---|
| Proximal | Distal | Ceacum/ right colon |
Left colon |
|||
| 1 | [6] | 39 normals | 6.4 | 7.3 | 5.7 | 6.6 |
| 2 | [7] | 13 normals | 6.4 | 7.4 | 5.8 | - |
| 3 | [8] | 7 normals | 6.6 | 7.4 | 6.7 | - |
| 4 | [9] | 2 normal+7 GI disorder cases | 5.5-7.5 | 6.5 -7.5 | 5.5-7.5 | 6.5-7.5 |
| 5 | [10] | 66 normals | 6.6 | 7.5 | 6.4 | 7.1 |
| Patient with Ulcerative Colitis | ||||||
| 6 | [11] | 7 acitive 6 inactive |
6.1 5.9-6.6 |
7.2 6.9-7.4 |
4.7 4.9-5.5 |
- - |
| 7 | [12] | 3 active 3 very active |
Normal Normal |
Normal Normal |
Normal 2.3-3.4 |
- - |
| 8 | [13] | 6 active | 7.3 | 8.3 | 6.7 | 6.7 |
| 9 | [14] | 7 active 4 nactive |
6.8 6.6 |
8.2 7.9 |
7.2 6.5 |
6.8 6.5 |
| 10 | Eve [15] |
4 active | 6.5 | 6.8 | 5.5 | 7.5 |
| Patient with Crohn’s disease | ||||||
| 11 | [7] | 9 withileocecal resection | 6.3 | 7.3 | 6.7 | NA |
| 12 | [16] | 3 acitive 1 inactive |
7.2 | 7.8 | 5.3 | 5.3 |
| 13 | [15] | 12 active | 6.5 | 7.5 | 6.2 | 6.5 |
| 14 | [14] | 5 active 7 inactive |
6.5 6.8 |
7.9 8.2 |
6.5 6.5 |
6.5 6.5 |
Table 2: pH conditions in normal and inflamed colon.
Treatment methods for IBD and its limitations
Treatment usually based on reports of clinical history, physical parameters endoscopy, radiology, histology and regular laboratory tests. The study on these reports gives the clear idea about IBD and also distinguishes the ulcerative colitis and Crohn’s disease, but it is very difficult to distinguish ulcerative colitis and Crohn's disease in at least 10% of the population for them IBD is limited to the colon [17,18]. Long time management of inflammatory bowel disease involves the drug therapy and lifestyle management. The therapy may be started with antidiarrheal in the beginning to give the symptomatic relief and the treatment should be focused on reducing the inflammation once the symptoms are subsiding.
A correct diet and nutritions are advisable as a supporting measures for the successful IBD management. A drugs such as 5 amino salicylic acid (Mesalamine) were used in the treatment of IBD [19]. 5–ASA widely replaces the sulfasalazine for its safety and less adverse effects. Mesalamine (5-ASA) not considered as the very potent anti-inflammatory agent, but shown to be effective in IBD patients, but also fails to show significant improvement in the set of patients Affected with IBD .
Important considerations of amino salicylates
•Amino salicylates are unstablets in gastric acid
•Rapidly absorbed in the small intestine.
•The safety and tolerability of amino salicylates are the reason behind the withdrawal of these agents.
•The greater number of withdrawals was reported with sufasalazine 3 g/day than balsalazide 6.75 g/day [20,21].
•Balsalazide has a more adverse drug reactions than delayed release Mesalamine [22].
•The unstablets nature of Mesalamine in the upper GI region paves the way for developing them into novel drug delivery systems such as delayed release formulation based on enteric coating pH dependent release system which breaks at ileal or colonic PH or environment. Prodrug based systems, microflora activated system based on poly surcharges such as Pectin, Guar gum, Chitosan, timed release system, etc [23,24].
Corticosteroids
•Corticosteroids are recommended when 5–ASA compounds are inadequate in producing the expected results.
•Topical corticosteroids (enemas) used in the patient with ulcerative colitis, Prednisolone 60 mg/day is used orally in the treatment of ulcerative colitis and Crohn’s disease. The mechanism of action of corticosteroids was well known and is acted by inhibiting the several inflammatory pathways and stimulation of lymphocyte apoptosis [25].
•Corticosteroids are known for its systemic side effects in which adrenal suppression and osteoporosis, corticosteroids induced hypertension and diabetes are well noted.
•Intravenous administration of Prednisolone also recommended when the condition of the patient is severe [26,27]
•The budenonide usage may minimize the side effects of Prednisolone and also available in the form of enema [26,27].
•Budensonide efficacy somewhat less than the conventional corticosteroids due to first pass metabolism. Fluticasone was not effective in distal disease [28,29].
•The main disadvantage is the usage of these corticosteroids are difficult in Crohn’s disease than ulcerative colitis due to the variation in colonic pH, transit time and bacterial metabolism [30,31].
Immune modulatory therapy
•Azathiopurine and Mercaptopurine (6-mercapropurine) are the most commonly used immune modulator. These are the derived products of thioguanides. This recommended when corticosteroids cannot be withdrawn from the patient.
•Although azathiopurine earlier reported for side effects and producing an increased risk of lymphoma, which is becoming a highly recommended immune suppressive agent [32-35].
•The efficacy of the drug was mostly depend on the dose, and the optimal dosage was 2.0-2.5 mg/kg/day and 1.0-1.5 mg/kg/day was found optimal for Azathiopurine and Mercaptropurine respectively [36].
•The side effects of these agents are limited the usage of Azathiopurine and Mercaptopurine. So that Azathiopurine should be prescribed with caution and step wise approach. The serious adverse effects include bone marrow suppression, variation in the white cell counts [37,38].
•Cyclosporine is recommended in the patient with steroid refractory ulcerative colitis [39]. Cyclosporin inhibits the cellular immune response by blocking cytokinine production by T lymphocytes through calcineuron dependent pathway [40,41].
•Cyclosporins provide the rapid onset of action by intravenous route with significant clinical improvement about a week [42] cyclosporins should not be recommended in the treatment of Crohn's disease which may cause severe personal or cutaneous fistula [42]. Although cyclosporins are considered as a alternative for corticosteroid therapy their adverse effects limits the usage.
•Tacrolimus and mycopholate mefetil also effective in the treatment of IBD. Tacrolimus is a macrolide immune suppression which inhibits the immune response through a calcineurin dependent pathway [43] Tacrolimus can induce remission in adults and children [44,45] Recent days studies supported the usage in the treatment of corticosteroids dependent Crohn’s disease in remission and relapsing [46-49].
•It can be given as weekly injection 15 mg and 25 mg weekly by IM and SC respectively. The mechanism of action of this drug is unclear and also known for its side effects such as immune suppression, interstitial pneumonitis associated with non-productive cough, dypnea and hepatic fibrosis.
Biological agents
•Biological agents such as infliximab (protypical anti – TNF agent) made the significant advancements in the treatment of crohns disease. The mechanism of action of infliximab yet to be explained completely. It is a chimeric monoclonal antibody. It is an agent which shows the significant results in the treatment of crohn’s disease but not in ulcerative colitis [50,51].
•Basiliximab was showing significant clinical remission in ulcerative colitis in pilot scale study [52].
•Daclizumab infusion showed the decreased clinical activity score in refractive ulcerative colitis patients. Natalizumab demonstrated a significant clinical response in active ulcerative colitis patients [53]. The rapid immuno modulatory agents are known for its severe adverse effects which sometimes fatal.
Probiotics and antibiotics in IBD
The studies worldwide supported the recognition of antibiotics in the treatment of IBD [54]. Other reports on probiotic also revealed that probiotic can be used as a supporting agent in the treatment of IBD. The usage of antibiotics in the treatment of ulcerative colitis is limited. In crohn’s disease metronidazole (750 mg/day/tid) found to be effective. The side effects of metronidazole such as neurotoxicity to be taken into consideration before and during the treatment. Metronidazole is effective in the treatment of Crohn’s disease, but showed no significant response in the treatment of ulcerative colitis.
The administration of probiotics is an excellent supporting approach in the management of crohn’s disease which is free of any side effects [55,56]. Lactobacillus acidophilus LA1 have the reported effect in immune enhancement adherent to human intestinal cells and balancing the microflora. Lactobacillus acidophilus NCFB is effective is effective in lowering faecal enzyme activity decreased fecal mutagenecity in the treatment of rotavirus diarrhea Crohn’s disease and antagonistic against carcinogenic bacteria. Lactobacillus casei shirota is effective in prevention of intestinal disturbances balancing intestinal bacteria and immune enhancement. Bifido bacterium bifidum is effecvtive in treatment of rotavirus diarrhea and balancing intestinal microflora. Lactobacillus gasseric (ADH) is effective in the treatment of IBD [57-60].
Importance of onset of Action in IBD Treatment
•Pharmacotherapy brought the excellent changes in the management of ulcerative colitis and crohn’s disease. The onset of action plays a major role in various treatment. In case of the IBD onset of action is most important in management, maintenance of remission of disease.
•In multicentre trial revealed that onset of action of balsalazide was earlier than Mesalamine [61].
•The patient with Sulfasalazine intolerance can be successfully treated with Balsalazide, Olsalazine or Mesalamine.
•Although corticosteroids have role in maintenance and remission of ulcerative colitis. Their efficacy relying on rapid onset of action and anti-inflammatory activity which gives the consistency in treatment with corticosteroids in ulcerative colitis.
•The study on immunomodulatory agents revealed that the clinical benefits of thioguanine derivatives desired only after 4 months of therapy in Crohn’s disease [62].
•The clinical reports demonstrated that infliximab is effective with rapid onset of action that gives the improvement within days in crohns disease but it is not effective in ulcerative colitis treatment [63,64].
The onset of action of therapy is most important in the treatment of IBD especially in the treatment of ulcerative colitis. Although novel biological agents, immune modulator and other novel agents are available, therapy is dominated by amino salicylates and corticosteroids. The importance of onset of action in IBD or UC therapy determines the efficacy of therapeutic agents and therapeutic stratergies (Table 3).
| Drug | Marketed product | Polymers (or) technology used | Site of release |
|---|---|---|---|
| Mesalamine | Asacol | Eudrgit S coating dissolves at pH >7 | Distal part of intestine and colon |
| Mesren | Eudrgit S coating dissolves at pH>7 | Distal part of intestine and colon | |
| Salofalk | Eudrgit L coated tabletdissolves at pH>6 | Middle and Distal part of intestine and colon | |
| Pentasa | Ethyl cellulose coated granules membrane controlled release | Stomach to colon | |
| Budesonide | Entocort | Eudragit L 100-55 coated ethyl cellulose granules dissolves at pH>5.5 | Proximal intestine and colon |
| Sulfasalazine | Salazopyrine | Azo bond cleaved by colonic bacteria | Colon |
| Olsalazine | Pipentum | Two Mesalamineazo bond cleaved by colonic bacteria | Colon |
| Balsalazide | Colazide | Mesalamine with inert azo bond carries cleaved by colonic bacteria | Colon |
Table 3: Various marketed products of IBD drugs.
Advanced drug delivery systems in IBD
•Targeting the drugs to the colon gaining the importance in treating GI disorders. The local disorder such as IBD, irritable bowel syndrome (IBS), carcinoma can be successfully treated by colonic deliveries.
•The advanced drug delivery systems prepared for the treatment of IBD mainly based on pH, transit time and micro flora activation.
•The coated systems with pH dependent polymers such as polymethacrylic acid derivatives (Eudrgits) are widely used for this purpose [65]. Polysachhrides such as Pectin, Chitosan, amylose and Guar gum can be successfully explored as colon drug delivery systems. The polysaccharide systems are found to be more successful because of their practicality and the abundant microflora of the colon.
•By combining the knowledge of threshold pH of the polymer and their solubility in different pH environments, duly, the system has been designed to release the drugs at target site exclusively on the colon [66,67].
•According to the various studies worldwide revealed and suggested fluctuation in the pH of the colon is due to various reasons [65].
•Some reports suggested that change in the G.I profile may occur in patient with IBD, which should be considered in developing delayed release formulations [65].
•Apparently the colon has lower pH value (6.5) than the small intestine (pH 7.0-7.8). The behavior of various pH sensitive polymers coated marketed products (Pentasa®, Asacol®, Salofalk®) with human subjects indicated that there was a marked individual variation in urinary recovery of these drugs [66].
•When observed in patients after administration of pentasa®, tablets there was an individual variation in urinary recovery [67].
•Mesalamine tablets manufactured by different companies have a different release profile when tested in various pH media.
•Research reports have clearly stated that the pH sensitive polymer-based colonic deliveries may not release the drug in the colon as expected.
•There are possibilities of the drug being released in advance, prior to entry of the terminal part of the G.I tract and or poor cumulative percentage of drug release occuring due to variation in the colonic pH during IBD [68]. Various studies proved that there was a fall in colonic pH in the IBD diseased colon [69].
Conclusion
Treatment and management of IBD is always a challenging aspect. The pharmacotherapy approaches moderately successful in the treatment of ulcerative colitis. The medical approach to treat this disease extensively differs with physician. The condition of patient and severity of the disease also influence the treatment method. The main objective of the IBD therapy is to induce the remission and to prevent the relapse. Since, there is no tailor made approach for this disease various factor to be consider before designing the treatment method to the patient. The marketed products are dominated by pH sensitive polymer based mechanism but it has its own drawbacks which were discussed in this work. The treatment methods such as amino-salicylates, corticosteroid, immunosuppressive agent, biological agents, surgical methods have reported disadvantages in the treatment of IBD. The longtime management of IBD must be well designed with the proper life style management. The onset of action plays a vital role in the management and treatment of ulcerative colitis and it has to be considered as an important factor in pharmacotherapy. All the advance drug delivery systems are not completely perfect devices. Study reports says that drug delivery systems in the treatment of IBD has to be monitored carfully. Before selecting the drug delivery system, a physician has to understand the mechanism of drug release in drug delivery system. The various natural polymers based drug delivery system also under research. Which can be considered as a alternative to pH sensitive devices. This review discussed some crucial parameters to be considered in the treatment of better IBD therapy.
References
- Goh J, O'Morain CA (2003) Review article: nutrition and adult inflammatory bowel disease.Aliment PharmacolTher 17: 307-320.
- Blumberg RS, Strober W (2001) Prospects for research in inflammatory bowel disease.JAMA 285: 643-647.
- Podolsky DK (2002) Inflammatory bowel disease.N Engl J Med 347: 417-429.
- http://www.bcm.edu/medicine/ibd/infodiagnostic
- William A Rowe, Julian Katz, Inflammatory bowel disease medication
- Fallingborg J (1999) Intraluminal pH of the human gastrointestinal tract.Dan Med Bull 46: 183-196.
- Fallingborg J, Pedersen P, Jacobsen BA (1998) Small intestinal transit time and intraluminal pH in ileocecal resected patients with Crohn's disease.Dig Dis Sci 43: 702-705.
- Raimundo AH, Evans DF, Rogers J (1992) Gastrointestinal pH profiles in ulcerative colitis. Gastroenterology, 102: 681.
- Watson BW, Meldrum SJ, Riddle HC, Brown RL, Sladen GE (1972) pH profile of gut as measured by radiotelemetry capsule.Br Med J 2: 104-106.
- Raimundo AH, Patil DH, Frost PG, Silk DB (1991) Effects of olsalazine and sulphasalazine on jejunal and ileal water and electrolyte absorption in normal human subjects. Gut 32: 270-274.
- Fallingborg J, Christensen LA, Jacobsen BA, Rasmussen SN (1993) Very low intraluminal colonic pH in patients with active ulcerative colitis.
- Nugent S G, Rampton D S, Kumar D (2000) Gut pH and transit time in ulcerative colitis appear sufficient for complete dissolution of pH dependent 5-ASA containing capsules. Gut 47.
- Press AG, Hauptmann IA, Hauptmann L, Fuchs B, Fuchs M, et al. (1998) Gastrointestinal pH profiles in patients with inflammatory bowel disease.Aliment PharmacolTher 12: 673-678.
- Ewe K, Schwartz S, Petersen S, Press AG (1999) Inflammation does not decrease intraluminal pH in chronic inflammatory bowel disease.Dig Dis Sci 44: 1434-1439.
- Sasaki Y, Hada R, Nakajima H, Fukuda S, Munakata A (1997) Improved localizing method of radiopill in measurement of entire gastrointestinal pH profiles: colonic luminal pH in normal subjects and patients with Crohn's disease.Am J Gastroenterol 92: 114-118.
- Rigaud D, Cosnes J, Le Quintrec Y, René E, Gendre JP, et al. (1991) Controlled trial comparing two types of enteral nutrition in treatment of active Crohn's disease: elemental versus polymeric diet.Gut 32: 1492-1497.
- Wallace JL (2003) Nitric oxide-releasing mesalamine: potential utility for treatment of inflammatory bowel disease.Dig Liver Dis 35 Suppl 2: S35-40.
- Green JR, Mansfield JC, Gibson JA, Kerr GD, Thornton PC (2002) A double-blind comparison of balsalazide, 6.75 g daily, and sulfasalazine, 3 g daily, in patients with newly diagnosed or relapsed active ulcerative colitis.Aliment PharmacolTher 16: 61-68.
- Mansfield JC, Giaffer MH, Cann PA, McKenna D, Thornton PC, et al. (2002) A double-blind comparison of balsalazide, 6.75 g, and sulfasalazine, 3 g, as sole therapy in the management of ulcerative colitis.Aliment PharmacolTher 16: 69-77.
- Green JR, Lobo AJ, Holdsworth CD, Leicester RJ, Gibson JA, et al. (1998) Balsalazide is more effective and better tolerated than mesalamine in the treatment of acute ulcerative colitis. The Abacus Investigator Group.Gastroenterology 114: 15-22.
- Basit AW (2005) Advances in colonic drug delivery.Drugs 65: 1991-2007.
- Newton AMJ, Prabakaran L, Jayaveera KN (2012)Effect of luminal pH changes on Guar gum-HPMC E15 LV mixed matrix tablets for Mesalamine drug delivery to colon and study on in vitro charecteristics in two different dissolution models Vs marketed formulations, Int J Pharm Sci res, 3: 2337-2347.
- Franchimont D, Kino T, Galon J, Meduri GU, Chrousos G (2002) Glucocorticoids and inflammation revisited: the state of the art. NIH clinical staff conference.Neuroimmunomodulation 10: 247-260.
- Faubion WA Jr, Loftus EV Jr, Harmsen WS, Zinsmeister AR, Sandborn WJ (2001) The natural history of corticosteroid therapy for inflammatory bowel disease: a population-based study.Gastroenterology 121: 255-260.
- Thomsen OO, Cortot A, Jewell D, Wright JP, Winter T, et al. (1998) A comparison of budesonide and mesalamine for active Crohn's disease. International Budesonide-Mesalamine Study Group.N Engl J Med 339: 370-374.
- Angus P, Snook JA, Reid M, Jewell DP (1992) Oral fluticasone propionate in active distal ulcerative colitis.Gut 33: 711-714.
- Hawthorne AB, Record CO, Holdsworth CD, Giaffer MH, Burke DA, et al. (1993) Double blind trial of oral fluticasone propionate v prednisolone in the treatment of active ulcerative colitis.Gut 34: 125-128.
- Campieri M, Adamo S, Valpiani D, D'Arienzo A, D'Albasio G, et al. (2003) Oral beclometasonedipropionate in the treatment of extensive and left-sided active ulcerative colitis: a multicentre randomised study.Aliment PharmacolTher 17: 1471-1480.
- Friend DR (1998) Review article: issues in oral administration of locally acting glucocorticosteroids for treatment of inflammatory bowel disease.Aliment PharmacolTher 12: 591-603.
- Lewis JD, Bilker WB, Brensinger C, Deren JJ, Vaughn DJ, et al. (2001) Inflammatory bowel disease is not associated with an increased risk of lymphoma.Gastroenterology 121: 1080-1087.
- Farrell RJ, Ang Y, Kileen P, O'Briain DS, Kelleher D, et al. (2000) Increased incidence of non-Hodgkin's lymphoma in inflammatory bowel disease patients on immunosuppressive therapy but overall risk is low.Gut 47: 514-519.
- Rosenberg JL, Wall AJ, Levin B, Binder HJ, Kirsner JB (1975) A controlled trial of azathioprine in the management of chronic ulcerative colitis.Gastroenterology 69: 96-99.
- Hawthorne AB, Logan RF, Hawkey CJ, Foster PN, Axon AT, et al. (1992) Randomised controlled trial of azathioprine withdrawal in ulcerative colitis.BMJ 305: 20-22.
- Nielsen OH, Vainer B, Rask-Madsen J (2001) Review article: the treatment of inflammatory bowel disease with 6-mercaptopurine or azathioprine.Aliment PharmacolTher 15: 1699-1708.
- Corominas H, Domènech M, González D, Diaz C, Roca M, et al. (2000) Allelic variants of the thiopurine S-methyltransferase deficiency in patients with ulcerative colitis and in healthy controls.Am J Gastroenterol 95: 2313-2317.
- Colombel JF, Ferrari N, Debuysere H (2002) Genotypic analysis of thiopurine S-methyltransferase in patients with Crohn’s disease and severe myelosuppression during azathioprine therapy. Gastroenterology, 118: 1025-30.
- Lichtiger S, Present DH, Kornbluth A, Gelernt I, Bauer J, et al. (1994) Cyclosporine in severe ulcerative colitis refractory to steroid therapy.N Engl J Med 330: 1841-1845.
- Mastuda S, Present DH, Kornbluth A (2000) Mechanism of action of cyclosporine. Immunopharmacology, 47: 119-125.
- D’Haens G, Lemmens L, Geboes K (2001) Intravenous cyclosporine versus intravenous corticosteroids as single therapy for severe attacks of ulcerative colitis. Gastroenterology, 120: 1323-9.
- Stange EF, Modigliani R, Peña AS, Wood AJ, Feutren G, et al. (1995) European trial of cyclosporine in chronic active Crohn's disease: a 12-month study. The European Study Group.Gastroenterology 109: 774-782.
- Gummert JF, Ikonen T, Morris RE (1999) Newer immunosuppressive drugs: a review.J Am SocNephrol 10: 1366-1380.
- Fellermann K, Tanko Z, Herrlinger KR, Witthoeft T, Homann N, et al. (2002) Response of refractory colitis to intravenous or oral tacrolimus(FK506).Inflamm Bowel Dis 8: 317-324.
- Baumgart DC, Wiedenmann B, Dignass AU (2003) Rescue therapy with tacrolimus is effective in patients with severe and refractory inflammatory bowel disease.Aliment PharmacolTher 17: 1273-1281.
- Feagan BG, Fedorak RN, Irvine EJ, Wild G, Sutherland L, et al. (2000) A comparison of methotrexate with placebo for the maintenance of remission in Crohn's disease. North American Crohn's Study Group Investigators.N Engl J Med 342: 1627-1632.
- Feagan BG, Rochon J, Fedorak RN, Irvine EJ, Wild G, et al. (1995) Methotrexate for the treatment of Crohn's disease. The North American Crohn's Study Group Investigators.N Engl J Med 332: 292-297.
- Oren R, Arber N, Odes S, Moshkowitz M, Keter D, et al. (1996) Methotrexate in chronic active ulcerative colitis: a double-blind, randomized, Israeli multicenter trial.Gastroenterology 110: 1416-1421.
- Alfadhli A A, McDonald JW , Fegan B G (2003) Metrotrexate for induction of remission in refractory crohn’s. Cochrane Database Syst Rev.
- ten Hove T, van Montfrans C, Peppelenbosch MP, van Deventer SJ (2002) Infliximab treatment induces apoptosis of lamina propria T lymphocytes in Crohn's disease.Gut 50: 206-211.
- Lügering A, Schmidt M, Lügering N, Pauels HG, Domschke W, et al. (2001) Infliximab induces apoptosis in monocytes from patients with chronic active Crohn's disease by using a caspase-dependent pathway.Gastroenterology 121: 1145-1157.
- Creed TJ, Norman MR, Probert CS, Harvey RF, Shaw IS, et al. (2003) Basiliximab (anti-CD25) in combination with steroids may be an effective new treatment for steroid-resistant ulcerative colitis.Aliment PharmacolTher 18: 65-75.
- Van Assche G, Dalle I, Noman M, Aerden I, Swijsen C, et al. (2003) A pilot study on the use of the humanized anti-interleukin-2 receptor antibody daclizumab in active ulcerative colitis.Am J Gastroenterol 98: 369-376.
- Sutherland L, Singleton J, Sessions J, Hanauer S, Krawitt E, et al. (1991) Double blind, placebo controlled trial of metronidazole in Crohn's disease.Gut 32: 1071-1075.
- Rembacken BJ, Snelling AM, Hawkey PM, Chalmers DM, Axon AT (1999) Non-pathogenic Escherichia coli versus mesalazine for the treatment of ulcerative colitis: a randomised trial.Lancet 354: 635-639.
- Gionchetti P, Rizzello F, Venturi A, Brigidi P, Matteuzzi D, et al. (2000) Oral bacteriotherapy as maintenance treatment in patients with chronic pouchitis: a double-blind, placebo-controlled trial.Gastroenterology 119: 305-309.
- Hartmann G, Bidlingmaier C, Siegmund B, Albrich S, Schulze J, et al. (2000) Specific type IV phosphodiesterase inhibitor rolipram mitigates experimental colitis in mice.J PharmacolExpTher 292: 22-30.
- Yue G, Sun FF, Dunn C, Yin K, Wong PY (1996) The 21-aminosteroid tirilazadmesylate can ameliorate inflammatory bowel disease in rats.J PharmacolExpTher 276: 265-270.
- Krawisz JE, Sharon P, Stenson WF (1984) Quantitative assay for acute intestinal inflammation based on myeloperoxidase activity. Assessment of inflammation in rat and hamster models.Gastroenterology 87: 1344-1350.
- Jagtap AG, Shirke SS, Phadke AS (2004) Effect of polyherbal formulation on experimental models of inflammatory bowel diseases.J Ethnopharmacol 90: 195-204.
- Slonim AE, Bulone L, Damore MB, Goldberg T, Wingertzahn MA, et al. (2000) A preliminary study of growth hormone therapy for Crohn's disease.N Engl J Med 342: 1633-1637.
- Present DH, Rutgeerts P, Targan S, Hanauer SB, Mayer L, et al. (1999) Infliximab for the treatment of fistulas in patients with Crohn's disease.N Engl J Med 340: 1398-1405.
- Nikolaus S, Raedler A, Kühbacker T, Sfikas N, Fölsch UR, et al. (2000) Mechanisms in failure of infliximab for Crohn's disease.Lancet 356: 1475-1479.
- Khan MZ, Prebeg Z, KurjakoviÄN (1999) A pH-dependent colon targeted oral drug delivery system using methacrylic acid copolymers. I. Manipulation Of drug release using Eudragit L100-55 and Eudragit S100 combinations.J Control Release 58: 215-222.
- Follonier N, Cole E T (1994)Evolution of hot melt extrusion as a new technique for the production of polymer based pellets for sustained release capsule containing high loadings freely soluble drugs. Drug DevInd Pharm., 20: 1323-1339.
- Ashford M, Fell J T. Attwood D, Sharma H, Woodhead P (1993) An in vitro investigation into the suitability of pH- dependent polymers for colon targeting, Int J Pharm., 91: 241-245.
- Adkin DA, Kenyon CJ, Lerner EI, Landau I, Strauss E, et al. (1997) The use of scintigraphy to provide "proof of concept" for novel polysaccharide preparations designed for colonic drug delivery.Pharm Res 14: 103-107.
- Rijk MC, van Schaik A, van Tongeren JH (1988) Disposition of 5-aminosalicylic acid by 5-aminosalicylic acid-delivering compounds.Scand J Gastroenterol 23: 107-112.
- Stolk LM, Rietbroek R, Wiltink EH, Tukker JJ (1990) Dissolution profiles of mesalazine formulations in vitro.Pharm WeekblSci 12: 200-204.
- Jose S, Dhanya K, Cinu TA, Litty J, Chacko AJ (2009) Colon targeted drug delivery: different approaches. J Young pharmacist 1: 13-19.
- Nugent SG, Kumar D, Rampton DS, Evans DF (2001) Intestinal luminal pH in inflammatory bowel disease: possible determinants and implications for therapy with aminosalicylates and other drugs.Gut 48: 571-577.
Relevant Topics
Recommended Journals
- Journal of Lung Cancer Diagnosis & Treatment
- Advances in Cancer Prevention
- Breast Cancer: Current Research
- Cancer Surgery
- Immunology: Current Research
- Current Trend in Gynecologic Oncology
- Journal of Cancer Diagnosis
- Journal of Gastrointestinal Cancer and Stromal Tumors
- Cervical Cancer: Open Access
- Journal of Mucosal Immunology Research
- Journal of Oncology Research and Treatment
- Journal of Orthopedic Oncology
- Journal of Prostate Cancer
- Research and Reviews on Pathogens
Article Tools
Article Usage
- Total views: 17278
- [From(publication date):
December-2014 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 12591
- PDF downloads : 4687