Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Image Open Access
Neurobrucellosis Presented as Wallenberg Syndrome
| Ya-Fen Li, Xin-Gang Sun*, Gai-Qing Wang, Yi-Peng Ma, Li Wang and Wei-min Hu | |
| Department of Neurology, the Second Hospital of Shanxi Medical University, Taiyuan, China | |
| Corresponding Author : | Xin-Gang Sun Department of Neurology the Second Hospital of Shanxi Medical University Taiyuan 030001, Shanxi Province, China Tel: 030001 E-mail: sunyanxia820701@163.com |
| Received June 17, 2015; Accepted June 18, 2015; Published June 2, 2015 | |
| Citation: Ya-Fen L, Xin-Gang S, Gai-Qing W, Yi-Peng M, Li W, et al. (2015) Neurobrucellosis Presented as Wallenberg Syndrome. J Neuroinfect Dis S1:006. doi:10.4172/2314-7326.S1-006 | |
| Copyright: © 2015 Ya-Fen L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
| Introduction |
| A 54 years old male patient, who had long time contact with flocks and herds, was diagnosed as Wallenberg Syndrome by clinical symptoms and Magnetic Resonance Imaging (Figure 1a) at first, but he did not had any stroke risk factors and there was nothing abnormal detected in the intracranial vascular (Figure 1b). inflammationAbout one month later, fever and headache happened, then Chest CT showed in inferior lobe lung and a little effusion in chest (Figure 1c), and brucella blood serum agglutination test was positive (1:200). This case showed that neurobrucellosis may sometimes be presented as stroke at first. |
Figures at a glance
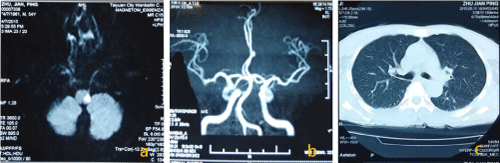 |
| Figure 1 |
Post your comment
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 13965
- [From(publication date):
specialissue-2015 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 9288
- PDF downloads : 4677
