Case Report Open Access
Neuroleptospirosis: Aseptic Meningoencephalitis or Invasion into the Central Nervous System?
| Schiefecker AJ1*, Beer R1, Pfausler B1, Lackner P1, Broessner G1, Kofler M1, Richter S2, Allerberger F2, Muhr T3, Goris M4, Helbok R1 and Schmutzhard E1 | |
| 1Neurologic Intensive Care Unit, Department of Neurology, Medical University of Innsbruck, Innsbruck, Austria | |
| 2AGES (Austrian Agency for Health and Food Safety), Moedling, Austria | |
| 3Department of Medicine, Landeskrankenhaus Graz West, Graz, Austria | |
| 4Royal Tropical Institute (KIT), KIT Biomedical Research, WHO/FAO/OIE and National Collaborating Centre for Reference and Research on Leptospirosis, Amsterdam, The Netherlands | |
| Corresponding Author : | Dr. Alois Josef Schiefecker, M.D. Neurologic Intensive Care Unit Department of Neurology Medical University of Innsbruck Innsbruck, Austria Tel: 82-2-958-8295 E-mail: alois.schiefecker@tirol-kliniken.at |
| Received: July 18, 2015 Accepted: August 19, 2015 Published: August 22, 2015 | |
| Citation: Schiefecker AJ, Beer R, Pfausler B, Lackner P, Broessner G, et al. (2015) Neuroleptospirosis: Aseptic Meningoencephalitis or Invasion into the Central Nervous System?. J Neuroinfect Dis S2:001. doi:10.4172/2314-7326.S2-001 | |
| Copyright: © 2015 Schiefecker AJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Leptospirosis is a zoonotic disease of global importance with a mortality of up to 50% among patients requiring intensive care medicine. Meningitis or meningoencephalitis due to leptospires are considered to be an immunologically mediated disease and to occur mainly during the second phase of disease. Herein, we report a patient with severe meningo-encephalitis due to leptospirosis with evidence of direct bacterial invasion into the central nervous system (CNS). A 36-year-old otherwise healthy male farmer, without recent travel history, presented with recurrent fever, peaking >39°C, cough and conjunctivitis 10 days after high-pressure cleaning of a piggery without eye protection. Diagnostic work-up revealed meningoencephalitis due to Leptospira species (spp.). Serology (microscopic agglutination test) yielded elevated antibody titers (1:400) for Leptospira interrogans. Polymerase chain reaction (PCR) and electron micrograph of cerebrospinal fluid (CSF) demonstrated direct invasion of Leptospires into the CSF. Magnetic resonance imaging (MRI) of the brain and spine did not reveal any pathologic findings; electroencephalography (EEG) indicated right-hemispheric slowing. Due to severe abdominal pain, gastroscopy was performed. Histology showed signs of vasculitis. Conventional abdominal angiography demonstrated vasculitis resembling panarteriitis nodosa. Combined antibiotic and steroid therapy lead to clinical improvement.
Neuroleptospirosis is an important differential diagnosis of occupational meningoencephalitis in Central Europe. This case supports the hypothesis of direct invasion of leptospires into the CNS.
Neuroleptospirosis is an important differential diagnosis of occupational meningoencephalitis in Central Europe. This case supports the hypothesis of direct invasion of leptospires into the CNS.
Through periodically contractions of the axial filament and therefore rotation of the spiral shaped bacteria, leptospires are highly motile. The rotational movement of leptospires enables penetration through mucous membranes. Therefore, inhalation or direct contact with the eyes may cause invasion of leptospires through physiologic barriers into the blood stream [4].
It is hypothesized that neuroleptospirosis is rather caused by immunologic reactions to the spirochaetes than by direct invasion of the bacteria into the CNS [1]. Direct invasion of leptospires into the CNS is very rare and has been reported only in two post-mortem cases [5].
The ability of leptospires to penetrate tissues is influenced by 12 methyl-accepting chemotaxis proteins and the spiral movements [6]. The outer membrane of leptospires is rich of lipopolysaccharides and attached with proteins for evading the hosts immune system and for penetrating tissue [6]. Electron microscopy and PCR findings in this patient’s CSF proofed direct bacterial invasion of leptospires into the central nervous system. Electron microscopy findings typically show a helically wound spiral shaped bacterium (0.01–0.02 µm in diameter) with characteristic hooked ends [1]. A TaqMan-based multi-gene targeted real-time PCR has a specificity of up to 100% and can detect a variety of pathogenic and non-pathogenic Leptospira strains [7].
Neurologic manifestations of leptospirosis include aseptic meningitis, polyneuritis, meningoencephalitis, subarachnoid or intracerebral hemorrhage [1,8,9]. The patient had clinical and electroencepahlographic evidence of meningoencephalitis, although MRI scan did not reveal any pathologic findings. It is known from previous studies that MRI abnormalities are very rare in encephalitis caused by leptospires, but may include reversible corpus callosum T2 and FLAIR hyperintense lesions [10].
The course of disease during was prolonged in this patient. The initially combined therapy with bacteriostatic and bactericide antibiotics (doxycycline and piperacllin/tazobactam) could have caused an interaction between the bacteriocid effects of penicillin and the bacteriostatic properties of tetracyclin. As observed in this patient, the association between leptospirosis and vasculitis has been reported in several cases [11-15] indicating a strong autoimmunologic response triggered by leptospires.
References
- Bharti AR, Nally JE, Ricaldi JN, Matthias MA, Diaz MM, et al (2003) Leptospirosis: a zoonotic disease of global importance. The Lancet Infectious diseases 3: 757-771.
- Goris MG, Kikken V, Straetemans M, Alba S, Goeijenbier M, et al. (2013) Towards the burden of human leptospirosis: duration of acute illness and occurrence of post-leptospirosis symptoms of patients in the Netherlands. PloS one 8: e76549.
- Panicker JN, Mammachan R, Jayakumar RV (2001) Primary neuroleptospirosis. Postgraduate medical journal 77: 589-590.
- Langner-Wegscheider BJ, Krause R (2015) Images in clinical medicine. Hyphema. The New England journal of medicine 372: 1549.
- Brown PD, Carrington DG, Gravekamp C, van de Kemp H, Edwards CN, et al. (2003) Direct detection of leptospiral material in human postmortem samples. Research in microbiology 154: 581-586.
- Haake DA, Zuckert WR (2015) The leptospiral outer membrane. Current topics in microbiology and immunology 387: 187-221.
- Ferreira AS, Costa P, Rocha T, Amaro A, Vieira ML, et al. (2014) Direct detection and differentiation of pathogenic Leptospira species using a multi-gene targeted real time PCR approach. PloS one 9: e112312.
- Bezerra HM, Ataide Junior L, Hinrichsen SL, Travassos FM, Travassos PT, et al. (1993) Involvement of the nervous system in leptospirosis. I. Evaluation of neurologic aspects. Arquivos de neuro-psiquiatria 51: 457-463.
- Forwell MA, Redding PJ, Brodie MJ, Gentleman DD (1984) Leptospirosis complicated by fatal intracerebralhaemorrhage. British medical journal 289: 1583.
- Khanra D, Talukdar A (2013) 'Mini-boomerang sign': reversible corpus callosal signal change in neuroleptospirosis. International journal of infectious diseases : IJID : official publication of the International Society for Infectious Diseases 17: e70-71.
- Wong ML, Kaplan S, Dunkle LM, Stechenberg BW, Feigin RD (1977) Leptospirosis: a childhood disease. The Journal of pediatrics 90: 532-537.
- Panagopoulos P, Terzi I, Karanikas M, Galanopoulos N, Maltezos E (2014) Myocarditis, pancreatitis, polyarthritis, mononeuritis multiplex and vasculitis with symmetrical peripheral gangrene of the lower extremities as a rare presentation of leptospirosis: a case report and review of the literature. Journal of medical case reports, 8: 150.
- George P (2011) Two uncommon manifestations of leptospirosis: Sweet's syndrome and central nervous system vasculitis. Asian Pacific journal of tropical medicine 4: 83-84.
- Cai Z (1983) Cerebral arteritis due to leptospirosis. Zhonghuashenjingjingshenkezazhi = Chinese journal of neurology and psychiatry 16: 356-358.
- Gong YH (1984) Leptospiral cerebral arteritis: report of 4 autopsy cases. ActaAcademiaeMedicinae Wuhan = Wu-hanihsuehyuanhsuehpao 4: 44-49.
Figures at a glance
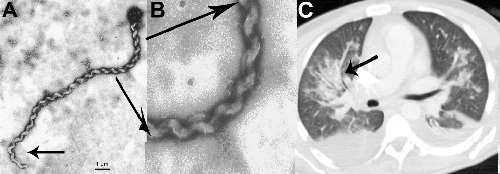 |
| Figure 1 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 18762
- [From(publication date):
specialissue-2015 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 13789
- PDF downloads : 4973
