Case Report Open Access
Reversible Splenial Lesion Syndrome (RESLES) in a Patient with Clinically Mild Tick-Borne Encephalitis and Hyponatremia
| Thomas Grimm1, Filip Barinka1, Martin Uhl1, Wilhelm Schulte-Mattler1, Berthold Schalke1, Schuierer Gerhard1, Ulrich Bogdahn1 Gerhard Schuierer2, Susanne Schwab-Malek1, Klemens Angstwurm1, Peter Hau1, Markus Hutterer1 | |
| 1University Hospital Regensburg, Department of Neurology, Regensburg, Germany | |
| 2 University Hospital and Regional Hospital Regensburg, Center of Neuroradiology, Regensburg, Germany | |
| Corresponding Author : | Markus Hutterer MD Department of Neurology and Wilhelm-Sander NeuroOncology Unit University of Regensburg Franz-Josef- Strauß-Allee 11 D-93053 Regensburg Germany Tel: 004909419413200 Fax: 004909419413205 E-mail: Markus.Hutterer@ukr.de |
| Received September 30, 2015; Accepted October 21, 2015; Published October 29, 2015 | |
| Citation:Grimm T, Barinka F, Uhl M, Schulte-Mattler W, Schalke B et al. (2015) Reversible Splenial Lesion Syndrome (Resles) in a Patient with Clinically Mild Tick- Borne Encephalitis and Hyponatremia. J Neuroinfect Dis 6:192. doi:10.4172/2314-7326.1000192 | |
| Copyright: © 2015 Grimm T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Introduction: Reversible splenial lesion syndrome (RESLES) is a clinicoradiological syndrome of varied etiology, characterized by transient lesions involving the splenium of the corpus callosum (SCC). Clinical presentation is nonspecific and depends on etiology. In the case of infectious disease the syndrome is also called mild encephalitis with reversible splenial lesion (MERS). Hyponatremia is often described in patients with RESLES. Here we present a patient case of RESLES/MERS in a patient with tick-borne encephalitis (TBE) accompanied by mild hyponatremia. Case Presentation: A 46-year-old man presented with malaise, fever, headache, discrete nuchal rigidity, brain stem symptoms (disturbance of ocular movements, gait ataxia) and mild cognitive and psychomotor impairment. Cerebrospinal fluid analysis at two different time points showed a lymphocytic pleocytosis and seroconversion for anti-TBEIgM/- IgG, serum biochemical analysis a mild hyponatremia. Magnetic resonance imaging (MRI) of the brain on day four after admission revealed a distinct signal hyperintensity on T2/FLAIR sequences in the SCC associated with diffusion restriction and low apparent diffusion coefficient (ADC) values on diffusion-weighted sequences. On T1-weighted images no contrast enhancement was detectable. Until the diagnosis of TBE the patient was treated with intravenous ceftriaxone, ampicillin and acyclovir. The patient recovered completely within three weeks. The T2/FLAIR hyperintense and diffusion-restricted lesion of the SCC was completely resolved ten days after the first MRI. Conclusion: TBE accompanied by hyponatremia may lead to RESLES/MERS, a clinicoradiological syndrome with reversible non-enhancing lesion of the SCC and excellent prognosis. Neuroradiological findings in RESLES are very similar to findings described in patients with osmotic demyelination syndromes like central pontine myelinolysis or extrapontine myelinolysis.
| Keywords |
| Reversible splenial lesion syndrome; Mild encephalitis with reversible splenial lesion; Tick-borne encephalitis; Hyponatremia |
| Abbreviations |
| ADC: Apparent Diffusion Coefficient; CNS: Central Nervous System; CPM: Central Pontine Myelinolysis; CSF: CerebroSpinal Fluid; DWI: Diffusion-Weighted Imaging; EBV: Epstein Barr Virus; EPM: Extrapontine Myelinolysis; TBE: Tick-Borne Encephalitis; MERS : Mild Encephalitis With Reversible Splenial Lesion; MRI: Magnetic Resonance Imaging; RESLES: Reversible Splenial Lesion Syndrome; SIAD: Syndrome Of Inappropriate Secretion Of Antidiuretic Hormone; SCC: Splenium Of The Corpus Callosum |
| Introduction |
| Reversible splenial lesion syndrome (RESLES) involving the splenium of the corpus callosum (SCC) is a clinicoradiological syndrome described in a variety of disorders including central nervous system (CNS) infections, seizures, anticonvulsive drug withdrawal, high-altitude cerebral edema and metabolic disturbances like hyponatremia [1,2]. RESLES is defined as transient, non-contrast enhancing, T2/ FLAIR hyperintensity associated with diffusion-restriction and low apparent diffusion coefficient (ADC) values on diffusion-weighted imaging (DWI), indicating cytotoxic edema. In rare cases high ADC values consistent with vasogenic edema were reported [1]. In cases with clinically mild encephalitis (viral as well as bacterial) the syndrome is also named MERS (mild encephalitis with a reversible splenial lesion) [3]. Reported causative pathogens are epstein barr virus (EBV), influenza type A/B [4], Salmonella enteritis, mumps virus and mumps vaccination virus [5], varicella zoster virus [3], adenovirus [6], parvovirus B19 [7], HHV 6 [8] and rubella virus [9]. |
| The pathophysiology of RESLES, especially the reversibility of a localized homogenous diffusion-restriction, remains largely unknown. It is assumed that a transient vasogenic, intramyelinic and/or interstitial edema in tightly packed fibers or an edema due to an inflammatory process might be important mechanisms [3,10,11]. An accompanying hyponatremia is frequently described [2,5,12,13]. On a molecular and biochemical level it was observed that serum and CSF levels of interleukin- 6 (IL-6) and IL-10 were significantly elevated in RESLES patients [14-17]. Further, increased CSF levels of 8-hydroxy-2’-deoxyguanosine (8-OHdG) and hexanoyl-lysine in MERS patients may indicate augmented oxidative stress levels [17]. As RESLES complicates different disorders, Polster et al. [10] suggested that such a transient lesion in SCC occurs as a nonspecific endpoint of various disease processes leading to a vasogenic edema. Here we present a patient case of RESLES in a patient with clinically mild tick-borne encephalitis (TBE) and mild hyponatremia. |
| Case Presentation |
| In October 2014 a 46-year old man presented with symptoms of a meningoencephalitis (malaise, fever of 39,3°C, sinus tachycardia of 113/min, nuchal rigidity, occipital headache, phonophobia, pain during ocular movement and myalgia), brain stem symptoms including binocular diplopia, upward gaze palsy, horizontal gaze-evoked nystagmus as well as slight gait ataxia and mild neurocognitive deficits and psychomotor impairment. Blood white cell count of 17000 cells/μl was accompanied by normal C-reactive protein level. Hyponatremia of 133 mmol/l (normal 135-145 mmol/l) was seen one day after admission. Sodium blood concentration showed normalization within six days. Cerebrospinal fluid (CSF) analysis showed granulocytic pleocytosis (111 cells/μl) and moderately increased protein content (859 mg/l) and lactate (2,76 mmol/l). A detailed serological and microbiological examination – including ELISA and PCR from serum and CSF probes – for Borrelia burgdorferi, Listeria monocytogenes, Leptospira interrogans, Treponema pallidum, Mycobacterium tuberculosis, HSV 1/2, TBE-virus and EBV revealed a positive blood anti-TBE-IgM/IgG-titer, but not in CSF. Eight days later we saw a shift to a lymphocytic pleocytosis (162 cells/μl, Figure 1) with further increased protein level (1069 mg/l) in CSF and a seroconversion of CSF anti-TBE-IgM/IgG (antibody index for TBE-IgG of 14,1, normal <1,6). Blood and CSF ELISA and PCR for all other pathogenic agents remained negative. In cerebral MRI four days after admission a non-T1-contrast enhancing, T2/FLAIR hyperintense lesion in the SCC with distinct diffusion-restriction and low apparent diffusion coefficient (ADC) values in diffusion-weighted imaging (DWI) was detected (Figure 1). In neuropsychological examination cognitive deficits in verbal working memory, attention and concentration could be found. There was no evidence of hemispheric disconnection. Starting on the day of admission, patient was treated intravenously with ceftriaxon 2 g once daily for two weeks and acyclovir 750 mg three times daily until negative result of HSV 1/2-PCR in CSF could be acquired. Supportive therapy included intravenous rehydration as well as antipyretic and analgesic sub-stances as paracetamol and ibuprofen. |
| After three weeks the patient presented with complete clinical recovery without any neurological or neuropsychological deficit. A follow- up MRI ten days after first MRI demonstrated normalization of the T2/FLAIR hyperintense and diffusion-restricted lesion within the SCC (Figure 1). This indicates an initial cytotoxic edema in the sense of a reversible splenial lesion syndrome (RESLES). Because of the infectious etiology (TBE-virus infection) the syndrome is also called mild encephalitis with a reversible splenial lesion (MERS). |
| Discussion |
| This is the second reported patient case with clinically mild TBE and RESLES [12]. TBE was confirmed by seroconversion for IgG/IgMTBE in CSF and high antibody index. Brain MRI in the first week after symptom onset showed the typical signs of RESLES. The patient recovered within three weeks without neurocognitive sequelae or defects in MRI. Thus, we came to the diagnosis of RESLES in TBE. |
| Both patient cases with clinically mild TBE and RESLES were accompanied by a mild hyponatremia (this case and [12]. Hyponatremia is an often reported finding in patients with RESLES/MERS [2,5,12,13] as well as in patients with TBE [18]. Hyponatremia in TBE is often caused by hypovolemic dehydration, less common by the syndrome of inappropriate secretion of antidiuretic hormone [18]. This raises the question, whether hyponatremia is a part of pathophysiology of RESLES or only an accompanying circumstance. |
| Interestingly, similar MRI findings as are typically described in RESLES can be shown in several patients with osmotic demyelination syndromes like central pontine myelinolysis (CPM) or extrapontine myelinolysis (EPM) [19]. Hyponatremia and rapid correction of sodium blood-concentration are known risk factors for developing CPM/EPM [19]. In CPM/EPM rapid improvement of ADC values predicts a good clinical recovery [20], which is also characteristic in RESLES. Weather RESLES and CPM/EPM have a similar pathophysiology or RESLES is a specific type of EPM remains to be elucidated in future studies. |
References
- Garcia-Monco JC, Cortina IE, Ferreira E, Martinez A, Ruiz L, et al. ( 2011) Reversible splenial lesion syndrome (RESLES): what's in a name? Journal of neuroimaging : official journal of the American Society of Neuroimaging 21: e1-14.
- Zhang S, Ma Y, Feng J (2015) Clinicoradiological Spectrum of Reversible Splenial Lesion Syndrome (RESLES) in Adults: A Retrospective Study of a Rare Entity. Medicine 94: e512.
- Tada H, Takanashi J, Barkovich AJ, Oba H, Maeda M, et al. (2004) Clinically mild encephalitis/encephalopathy with a reversible splenial lesion. Neurology 63: 1854-1858.
- Takanashi J, Barkovich AJ, Yamaguchi K, Kohno Y (2004) Influenza-associated encephalitis/encephalopathy with a reversible lesion in the splenium of the corpus callosum: a case report and literature review. AJNR Am J Neuroradiol 25: 798-802
- Takanashi J, Shiihara T, Hasegawa T, Takayanagi M, Hara M, et al. (2015) Clinically mild encephalitis with a reversible splenial lesion (MERS) after mumps vaccination. J Neurol Sci 349: 226-228.
- Takanashi J, Barkovich AJ, Shiihara T, Tada H, Kawatani M, et al. (2006) Widening spectrum of a reversible splenial lesion with transiently reduced diffusion. AJNR Am J Neuroradiol 27:836-838.
- Suzuki H, Kusaka T, Okada H (2014) Clinically mild encephalitis/encephalopathy with a reversible splenial lesion caused by human parvovirus b19 infection: a case of two brothers with hereditary spherocytosis. Pediatric neurology 51: 470-472.
- Hatanaka M, Kashiwagi M, Tanabe T, Nakahara H, Ohta K, et al. (2014) Overlapping MERS and mild AESD caused by HHV-6 infection. Brain Dev 37: 334-338.
- Jinnai A, Kikuchi T, Ishikawa M, Nishimura Y, Shibata K, et al. (2014)[A case of rubella encephalitis presenting as clinically mild encephalitis/encephalopathy with a reversible splenial lesion]. Rinsho Shinkeigaku 54: 668-670.
- Polster T, Hoppe M, Ebner A (2001)Transient lesion in the splenium of the corpus callosum: three further cases in epileptic patients and a pathophysiological hypothesis. J Neurol Neurosurg Psychiatry 70:459-463.
- Takanashi J (2009) Two newly proposed infectious encephalitis/encephalopathy syndromes.Brain Dev 31: 521-528.
- Vollmann H, Hagemann G, Mentzel HJ, Witte OW, Redecker C (2011) Isolated reversible splenial lesion in tick-borne encephalitis: a case report and literature review. Clinical neurology and neurosurgery 113: 430-433.
- Pan JJ, Zhao YY, Lu C, Hu YH, Yang Y (2015) Mild encephalitis/encephalopathy with a reversible splenial lesion: five cases and a literature review. Neurol sci 2: 1-9.
- Watanabe T, Matsuda T, Kitagata R, Tajima I, Ono H et al. (2014) Transient renal dysfunction with reversible splenial lesion. Pediatr Int 56: e68-71.
- Kometani H, Kawatani M, Ohta G, Okazaki S, Ogura K, et al. (2014) Marked elevation of interleukin-6 in mild encephalopathy with a reversible splenial lesion (MERS) associated with acute focal bacterial nephritis caused by Enterococcus faecalis.Brain Dev 36: 551-553.
- Shiihara T, Kato M, Hayasaka K (2005) Clinically mild encephalitis/encephalopathy with a reversible splenial lesion. Neurology 64: 1487.
- Miyata R, Tanuma N, Hayashi M, Imamura T, Takanashi J, et al (2012) Oxidative stress in patients with clinically mild encephalitis/encephalopathy with a reversible splenial lesion (MERS). Brain Dev 34:124-127.
- Czupryna P, Moniuszko A, Garkowski A, Pancewicz S, Guziejko K, et al. (2014) Evaluation of hyponatraemia in patients with tick-borne encephalitis--a preliminary study. Ticks and tick-borne diseases 5:284-286.
- Forster A, Nolte I, Wenz H, Al-Zghloul M, Kerl HU, et al. (2013) Value of diffusion-weighted imaging in central pontine and extrapontine myelinolysis. Neuroradiology 55:49-56.
- Dervisoglu E, Yegenaga I, Anik Y, Sengul E, Turgut T (2006) Diffusion magnetic resonance imaging may provide prognostic information in osmotic demyelination syndrome: report of a case. Acta Radiol 47:208-212.
Figures at a glance
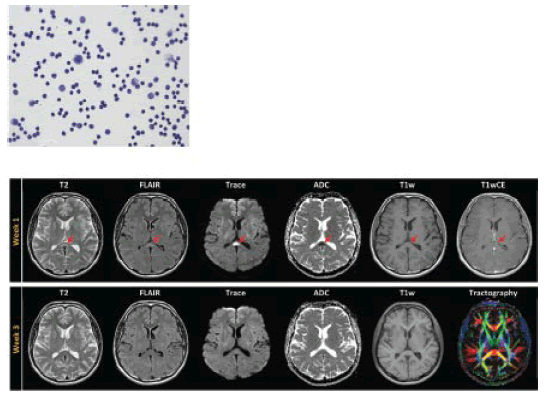 |
| Figure 1 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 12488
- [From(publication date):
December-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 11407
- PDF downloads : 1081
