Case Report Open Access
Sandfly Virus Encephalitis in Israel: Two Case Reports and a Review
Regev Cohen1,2*, Babushkin Frida2, Shimoni Zvi1,3, Shapiro Maurice4, Lustig Yaniv5,6 and Brosh-Nissimov Tal71The Ruth and Bruce Rappaport Faculty of Medicine, Technion, Haifa, Israel
2Infectious Diseases Unit, Sanz Medical Center, Laniado Hospital, Netanya, Israel
3Internal Medicine Department B, Sanz Medical Center, Laniado Hospital, Netanya, Israel
4Intensive Care Unit, Sanz Medical Center, Laniado Hospital, Netanya, Israel
5National Center for Zoonotic Viruses, Central Virology Laboratory, Public Health Services, Israel
6Chaim Sheba Medical Center, Ramat Gan, Israel
7Infectious Diseases Unit, Chaim Sheba Medical Center, Ramat Gan, Israel
- *Corresponding Author:
- Regev Cohen
Infectious Diseases Unit
Sanz Medical Center, Laniado Hospital
22 Divrei Haim St., 42150, Netanya, Israel
Tel: 972502172175
E-mail: regevco@gmail.com
Received date: March 28, 2016; Accepted date: March 22, 2017; Published date: March 24, 2017
Citation: Cohen R, Frida B, Zvi S, Maurice S, Yaniv L, et al. (2017) Sandfly Virus Encephalitis in Israel: Two Case Reports and a Review . J Neuroinfect Dis 8:240. doi:10.4172/2314-7326.1000240
Copyright: © 2017 Cohen R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
Background: Infections due to Sand-fly virus (SFV) are common in the Mediterranean region, but are rarely diagnosed in Israel. Until recently, no cases of severe neuro-invasive SFV infections were reported. In this study, we describe two cases of encephalitis associated with seroconversion to SFV acquired in Israel. We further try to postulate about the infecting strain of the SFV, its local phlebotomine vector, and the reasons for the emergence of this infection in Israel.
Methods: Clinical data were collected from hospital records. Laboratory diagnosis was obtained using mosaic indirect immunofluorescence tests (IFT) against several SFVs.
Results: Two patients with severe encephalitis presented during the same 2014 summer season. Both have acquired their infection in Hasharon district of central coastal Israel. Their encephalitis developed after a prolonged prodrome of 7 and 14 days, and was associated with severe neurological complications. Both patients exhibited a late seroconversion beyond twenty days from symptom onset.
Conclusion: SFVs are possible etiological agents of febrile illnesses and central nervous system infections in Israel. The SFV we report is suspected to be a Toscana virus-like strain, and is probably transmitted by Phlebotomus perfiliewi. A review of the spread of phlebotomine vectors is presented.
Background
Sand-fly fever viruses (SFVs) are arthropod transmitted viruses that belong to the Phlebovirus genus of the Bunyaviridae family. SFVs, maintained and transmitted by various Phlebotomines, are divided into two serogroups, the Sand-fly Sicilian viruses (SFSV) and the Sandfly Naples viruses (SFNV). Most of the SFVs cause acute influenza-like illness ("Pappataci fever", "3 days fever”) [1]. Some SFVs, most notably the Toscana virus (TOSV), belonging to the SFNV serogroup, are also associated with neuro-invasive illness, including aseptic meningitis and meningoencephalitis. SFVs infections and the neuro-invasive diseases associated with them are common in some Mediterranean countries, mainly Italy [2]. These agents are rarely suspected nor diagnosed in cases of meningitis or meningoencephalitis of unknown etiology in Israel, and the first series from Israel were described only recently [3]. We report on two cases of severe meningoencephalitis caused by SFVs, acquired in the coastal area of central Israel.
Methods
Patients
Patients' data were retrospectively collected from medical records of the Sanz medical center in Netanya, Israel.
Laboratory analysis
Samples were analyzed using the mosaic IFT for Phleboviruses detecting antibodies against SFSV, Sand-fly Cyprus virus (SFCV), SFNV and TOSV (Euroimmun, Lübeck, Germany). Briefly, serum and CSF samples were diluted 1:10 and 1:2, respectively, in sample buffer for IgG detection or in Eurosorb (Euroimmun, Lübeck, Germany) for detection of IgM. Serum samples were further diluted to 1:100 in sample buffer and all samples were processed according to manufacturer's recommendations. An anti-human IgG- or IgMFluorescein isothiocyanate (FITC)-conjugate (DAKO, Hamburg, Germany) was used for detection. To determine the titer of the IgG antibodies, quantitative evaluation of 2 convalescent samples was performed using serum samples diluted 1:10 to 1:10000 according to the manufacturer's recommendations.
For the detection of phlebovirus sequences in CSF samples: RNA extraction was performed using the NucliSENS easyMAG (BioMerieux, France) following the manufacturer’s instructions. Eluted RNA was collected and stored at -80°C when not immediately used. RT-PCR and nested PCR were performed using degenerated primer pairs specific for TOSV L genomic segment as described by Sanchez- Seco et al. [4] with minor modifications. To avoid any risk of contamination, 5 μL of RNA were used in a one-step RT-PCR reaction with NPhlebo1+/NPhlebo1-primers rather than the two-step protocol described.
Presentation of Cases and Serological Analysis
Patient 1
On May 2014, a 52 years old male was admitted with acute confusion and fever. His medical history included type 2 diabetes mellitus, hypertension, mild renal failure and hypertrophic obstructive cardiomyopathy. He lived in Netanya located in Hasharon district, in central Israel but had travelled to Tiberius (a Leishmaniasis endemic area) 4 weeks earlier. He had no reported exposures to arthropods or animals. A week before admission he suffered a febrile illness accompanied with headaches, myalgia and weakness. Other family members reported a similar illness. On the day of admission, he presented with acute confusion and high fever, and within a few hours developed generalized tonic-clonic seizures, highly resistant to antiepileptic drugs. Physical examination showed tachycardia of 130 beats per minute, systolic hypertension, and conjunctival injection. On neurological examination, he was sedated and ventilated, with a decerebrated posture and bilateral extensor Babinski reflexes. Blood urea nitrogen and creatinine levels were similar to previous measurements, other chemistry tests were normal and more laboratory results are shown in Table 1. Chest X ray showed clear lung fields. Ceftriaxone, ampicillin, doxycycline, oseltamivir and acyclovir were empirically administered. Brain CT showed mild periventricular ischemic changes. Cerebrospinal fluid (CSF) analysis results are shown in Table 1.
| Parameter (normal range) | Patient 1 | Patient 2 | ||
|---|---|---|---|---|
| On admission | HD 14th | On admission | ||
| WBC (4-11) K/µl | 5.9 | 9.2 | ||
| Polymorphonuclears (40-75)% | 75 | 62 | ||
| Lymphocytes (20-45)% | 15 | 25 | ||
| Large Unspecified cells (0-4)% | 2.6 | 8 | ||
| Hemoglobin (11.5-16.5) g/dL | 13.7 | 12.8 | ||
| Platelets (150-400)K/µl | 196 | 393 | ||
| C-reactive protein (0-5)mg/L | 233 (HD 3) | 23 | ||
| Serum antibody tests | WNV, Coxiella burnetii, Leptospira, Mycoplasma, Chikungunya virus, HIV, HBV, HCV-negative; EBV, CMV-past infection |
WNV, Coxiella burnetii, Rickettsia, HIV-negative; EBV, CMV-past infection |
||
| Nasopharyngeal PCR for Influenza A+B | Negative | |||
| CSF | White blood cells (0-5/)µl | 13 | 25 | 42 |
| Mononuclears, % | NA | 90 | 15 | |
| Polymorphonuclears, % | NA | 10 | 85 | |
| Red Blood cells, cells/µl | 910 | 80 | 90 | |
| Protein (12-60) mg/dL | 126 | 68 | 40 | |
| Glucose (4-70) mg/dL | 172 | 129 | 59 | |
| PCR | HSV1, HSV2, VZV, Enteroviruses, pan-bacterial 16s rRNA, pan-fungal 28s rRNA and ITS, mycobacteria-negative | HSV1, HSV2, VZV, Enteroviruses-negative | ||
| Â Serology tests | WNV-negative | |||
Abbreviations: HD-hospitalization day, WBC-white blood cell, CSF-cerebrospinal fluid, WNV-West Nile virus, HIV-Human immunodeficiency virus, HBV-Hepatitis B virus, HCV-Hepatitis C virus, EBV-Epstein Barr virus, CMV-Cytomegalovirus, PCR-Polymerase chain reaction, HSV-Herpes simplex virus, VZV-Varicella zoster virus, ITS-Internal transcribed spacer
Table 1: Projected mean annual rainfall for Amibara, Dansha and Kebabo under RCP 4.5 and 8.5 RCPs.
Electroencephalography (EEG) study showed generalized periodic lateralized epileptiform discharges (PLEDs) with bursts every 1-4 seconds. Laboratory studies for various pathogens associated with CNS infection were negative and are presented in Table 1. The patient was treated in the intensive care unit, and during the course of his illness suffered acute renal failure, ventilator associated pneumonia and catheter associated urinary tract infection. After 4 weeks, he was transferred to a rehabilitation center for 8 weeks during which his motor abilities returned to his baseline status, but some cognitive impairment remained. Serological tests for SFVs were obtained on December 2014 from five family members who reported a febrile illness at the same time as the patient, and were negative.
Patient 2
On August 2014, a 20 years old female was admitted with meningoencephalitis. She lived and worked in central Israel, in areas known to be non-endemic for Leishmaniasis. She denied traveling outside her residence area in Israel or abroad, or exposure to animals or arthropods. Her medical history was notable only for an asymptomatic pituitary prolactinoma. Two weeks prior to admission she began suffering from severe headaches and fever. Watery diarrhea was noted during the first days of fever but resolved spontaneously. She received only non-steroidal anti-inflammatory drugs. On physical examination, her temperature was 38°C, she was coherent with mild nuchal rigidity, and without focal neurological signs. Laboratory results are shown in Table 1.
Brain CT was normal. She was empirically treated with intravenous ceftriaxone and acyclovir. On the second day of hospitalization a neurological deterioration was documented, including slowed reactions, nuchal rigidity, Kerning sign, myoclonic movements of her upper limbs, tendon hyperreflexia, plantar clonus and fasciculations of the tongue. Due to urinary retention, a urinary catheter was placed intermittently for a week. Ceftriaxone was discontinued and Doxycycline was given. Several EEG studies showed irregular background activity and non-rhythmical frontal intermittent bursting activity during sleeping phase interpreted as signs of frontal encephalitis. Phenytoin was administered. Magnetic resonance imaging (MRI) was interpreted as normal except for a small nonspecific lesion in the posterior limb of the left internal capsule, not evident in diffusion weighted imaging, and of unknown significance. The patient's neurological signs and EEG tests improved gradually and she was discharged after 16 days without any sequella, with instructions for phenytoin tapering.
Serological analysis
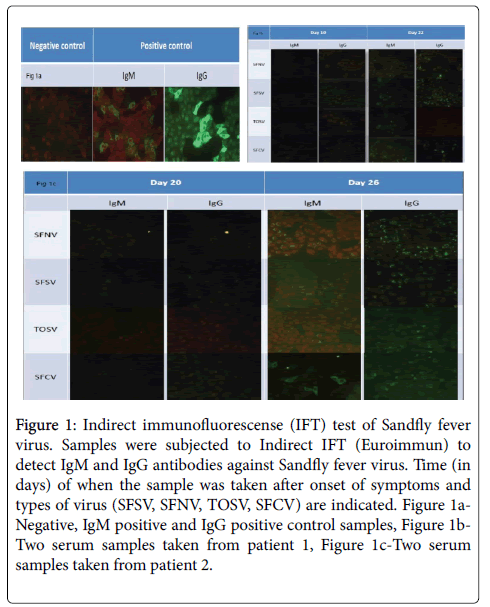
IFT against SFVs was performed on samples taken from patient 1 on the 10th and the 22nd days from symptoms onset, and from patient 2 on day 20th and 26th. Results demonstrated acute seroconversion and are presented in Table 2 and in Figure 1. PCR and serological tests from the CSF from both patients were negative for Sandfly viruses.
Figure 1: Indirect immunofluorescense (IFT) test of Sandfly fever virus. Samples were subjected to Indirect IFT (Euroimmun) to detect IgM and IgG antibodies against Sandfly fever virus. Time (in days) of when the sample was taken after onset of symptoms and types of virus (SFSV, SFNV, TOSV, SFCV) are indicated. Figure 1a-Negative, IgM positive and IgG positive control samples, Figure 1b-Two serum samples taken from patient 1, Figure 1c-Two serum samples taken from patient 2.
| Case 1 | Case 2 | |||||||
|---|---|---|---|---|---|---|---|---|
| Day 10a | Day 22a | Day 20a | Day 26a | |||||
| IgM | IgG | IgM | IgG | IgM | IgG | IgM | IgG | |
| SFNV | Weakly Positive | Negative | Positive | 1:320 | Weakly Positive | Negative | Positive | 1:3200 |
| SFSV | Negative | Negative | Positive | 1:100 | Weakly Positive | Negative | Positive | 1:3200 |
| TOSV | Negative | Negative | Positive | Negative | Negative | Negative | Positive | 1:3200 |
| SFCV | Weakly Positive | Negative | Positive | 1:320 | Negative | Negative | Positive | 1:3200 |
afrom symptom onset
Abbreviations: SFNV-Sandfly Naples Virus, SFSV-Sandfly Sicilian Virus, TOSV-Toscana Virus, SFCV-Sandfly Cyprus Virus
Table 2: Patient’s laboratory data, tumor markers as on June 20, 2016.
Discussion
Sand-fly virus encephalitis has been reported from many countries in the Middle East and the Mediterranean basin, including Italy, Spain, Portugal, France, Greece, Croatia, Bosnia, Serbia, Kosovo, Albania, Malta, Cyprus, Egypt, Algeria, Turkey, Iran, Iraq and others [1,2,5-12]; but clinical case reports from Israel were lacking since world war II [13]. In 1999 Cohen et al reported high seroprevalence to SFNV (30.8%) and to SFSV (23.7%) in sera of Israeli soldiers aged 40-55 years [14]. This report, added to many other reports from neighboring countries indicates that sand-fly fever is probably a common asymptomatic or paucisymptomatic disease in Israel. We assume that this fact and the unawareness of physicians to the (re)-existence of the sand-fly virus serocomplex in Israel contribute to its under diagnosis. Even cases of aseptic meningitis or encephalitis of unknown etiology are rarely considered for sand-fly virus diagnosis, with less than 1% of CSF specimens analyzed for Herpes viruses in the national virology laboratory analysis are also analyzed for sand-fly viruses (Y. Lustig , data not shown). Recently, Makranz et al. described a series of 9 patients from the Jerusalem district with a febrile disease associated with meningitis or encephalitis, characterized by severe neurologic sequelae, 5 needed intensive care [3]. Most of them presented seroconversion to SFNV serotype, predominantly to TOSV.
Among the SFVs, only TOSV is related to neuro-invasive disease, while other sand-fly variants cause a mild flu-like illness, but the serological differentiation between the serotypes is very difficult and they are usually regarded as one serocomplex. In recent years, the geographical distribution of TOSV (or closely related other phleboviruses) has been extended dramatically within the old world and antigenically similar novel viruses have been reported [2,15-18]. Therefore, our cases might represent a TOSV-related neuro-invasive strain, even though the immunofluorecsence assays were unable to distinguish between the viruses within the sand-fly virus serocomplex.
Important clinical aspects of our cases include the prolonged febrile illness before the onset of neurological involvement, the severity of the meningoencephalitis including epileptic activity and the late IgGseroconversion.
As with other arthropod borne viral encephalitides (WNV, Japanese Encephalitis virus etc.), a febrile prodrome precedes the neurological manifestation of SFV encephalitis. Variable prodrome durations were previously reported, from less than one day [19-24], 3-5 days [11,21,25,26], and rarely more than two weeks [27]. Both our cases presented after particularly long prodromes of 7 and 14 days.
Most cases (80%) of diagnosed TOSV infections present as aseptic meningitis rather than encephalitis [28], but severe cases of meningoencephalitis have been reported [19-27]. The disease is rarely lethal [19]. Likewise, accompanied generalized seizures are infrequently reported during TOSV infection [8,23,25,27,29]. In contrast, our reported cases, as well as the cases reported by Makranz et al. from Israel, suffered severe epileptic activity and were severely ill [3]. Patient 1 was comatose and suffered recurrent uncontrolled epileptic activity. Patient 2 also needed anti-epileptic therapy to control subclinical epileptic activity. Seven out the 9 cases from Jerusalem were reported to have seizures. In these cases, as in our patients, the hospitalization period was prolonged and a cognitive impairment ensued.
Using IFT, we could detect IgG seroconversion in the blood of both our cases. In patient 1 levels of IgG were negative on day 10 and seroconversion was seen on day 22. In case 2, levels of IgG were still negative by the 20th day since disease onset, and a clear seroconversion was seen on day 26. This late serologic reaction to the virus (and consequently maybe also the late clinical improvement) could hamper diagnosis of SFVs encephalitis in future cases. These findings should be taken into consideration before ruling out SFV encephalitis in patients with early negative serology and without an alternative etiology.
The two presented patients received empiric treatment with antimicrobials aimed at important and common bacterial and viral pathogens pending results of the microbiological investigation. After ruling these out, only supportive treatment was given, as is recommended for most viral CNS infections, including SFV infections. Although ribavirin and some experimental antiviral agents were shown to be effective against SFVs in vitro and in animal and clinical studies, none is used or recommended [12].
The geographic exposure for sandflies in this case report is somewhat surprising, since both cases were contracted in the Hasharon district, a Leishmaniasis non-endemic area of Israel. The first patient's travel to the Tiberius-area was four weeks before admission, while the incubation period of SFVs is considered to be up to 14 days (and typically 3-6 days). Israeli ministry of health tracks sandflies through the National Program to Reduce Leishmanisasis in Israel [30] but this program is focused on Leishmaniasis-endemic areas. Table 3 lists the known endemic sandflies in Israel, and the species identified in sporadic collections of sandflies along the Mediterranean seashore including Hasharon district (L. orshan , Laboratory of Entemology, Israeli Ministry of Health, personal communication).
| SFSV | SFNV | TOSV | L. major | L. tropica | L. infantum | |
|---|---|---|---|---|---|---|
| P. paptasi* | + | + | Never | + | - | - |
| P. sergenti* | - | - | - | - | + | - |
| P. perfiliewi* | + | - | + | - | - | + |
| P. neglectus | + | + | - | - | - | + |
| P. perniciosus | + | + | + | - | - | - |
| P. tobbi* | - | - | - | - | - | + |
| P. arabicus | + | |||||
| P. syriacus* | + |
* Phlebotomine species captured and identified in Hasharon district P.phlebotomus; L. leishmania, SFSV-Sandfly Sicilian Virus, SFNV-Sandfly Naples Virus, TOSV-Toscana Virus
Table 3: Phlebotomine species and their respective transmitted viruses and parasites.
Leishmaniasis is not endemic in this area, since no rock Hyraxes, the natural reservoir, exist there. Out of the Israeli sand-fly species known to be vectors and reservoir of SFVs, only P. perfiliewi can be the vector of TOSV or a variant of it. Investigation of the Sand-fly species in these Leishmaniasis non-endemic areas as well as trying to cultivate SFVs from captured sandflies is essential. Prevention of SFV infection is based on eliminating exposure to vectors either by avoiding contact (i.e. using bed nets) or by decreasing their population (i.e. spraying insecticides). There are no available vaccines against SFVs. [12]
What is the reason for reappearance of sand-fly encephalitis in Israel? The answer could be related to ecological and climate changes affecting the vectors. In the last decade the incidence of cutaneous Leishmaniasis in Israel increased dramatically from 0.4 to 4.4 cases per 100,000 between 2001 and 2012, and the disease emerged in areas where its presence had previously been minimal, including reported cases from Haifa district in northern seashore [30]. A similar trend was noted globally [31]. Investigators speculate that changes to the vectorreservoir- human population interface resulting from land development and construction and changes in land use created favorable conditions for mammalian reservoirs and sand-fly populations to breed in close proximity to human habitations [32,33]. Other theories indicate climate changes and its effect on vector life cycles [34]. The vector of Leishmania tropica in northern and central Israel is P. sergenti which is not related to transmission of SFVs to humans, but the same mechanisms probably affect other Phlebotomus species in central Israel that could transmit SFVs.
Summary
We describe two recent cases of severe encephalitis caused by SFV serocomplex contracted in the seashore areas of central Israel. Since molecular techniques failed to identify SFV, the exact species remains unknown, but probably represent a type of TOSV when considering the resulting severe neuro-invasive disease. This report should help raise awareness of clinicians to suspect SFV meningitis/encephalitis acquired in Israel and other Middle Eastern countries, including ones that are not considered endemic, and to facilitate early diagnosis. In suspected cases, serum and CSF samples should be sent for PCR tests during the early clinical course, and negative serological tests should be repeated up to 21 days from clinical presentation. The severe cases presented should also trigger health authorities to investigate the epidemiology of sandflies in central Israel and prevalence of SFVs in sandflies as well as in the human population.
References
- Dionisio D, Esperti F, Vivarelli A, Valassina M, (2003) Epidemiological, clinical and laboratory aspects of sandfly fever. Curr Opin Infect Dis 16: 383-388.
- CharrelRN, Gallian P, Navarro-Mari JM, Nicoletti L, Papa A, et al. (2005) Emergence of Toscana virus in Europe. Emerg Infect Dis 11: 1657-1663.
- Makranz C, Qutteineh H, Bin H, Lustig Y, Gomori JM, et al. (2016) Sandfly virus seroconversion associated with neurologic presentation. Neurol Neuroimmunol Neuroinflamm3: e184.
- Sanchez-Seco MP, Echevarria JM, Hernandez L, Estevez D, Navarro-Mari JM, et al. (2003) Detection and identification of Toscana and other phleboviruses by RT-nested-PCR assays with degenerated primers. J Med Virol 71: 140-149.
- Di Nicuolo G, Pagliano P, Battisti S, Starace M, Mininni V, et al. (2005) Toscana virus central nervous system infections in southern Italy. J Clin Microbiol 43:6186-6188.
- Dupouey J, Bichaud L, Ninove L, Zandotti C, Thirion-Perrier L, et al. (2014) Toscana virus infections: A case series from France. J Infect 68: 290-295.
- Ergunay K, Saygan MB, Aydogan S, Lo MM, Weidmann M, et al. (2011) Sandfly fever virus activity in central/northern Anatolia, Turkey: first report of Toscana virus infections. Clin Microbiol Infect17:575-581.
- Jaijakul S, Arias CA, Hossain M, Arduino RC, Wootton SH, et al. (2012) Toscana meningoencephalitis: A comparison to other viral central nervous system infections. J Clin Virol 55:204-208.
- Schultze D, Korte W, Rafeiner P, Niedrig M, (2012) First report of Sandfly fever virus infection imported from Malta into Switzerland, October 2011. Euro Surveill 17(27).
- Tyler KL (2009) Emerging viral infections of the central nervous system: Part 1. Arch Neurol 66: 939-948.
- Papa A, Kontana A, Tsergouli K (2015) Phlebovirus infections in Greece. J Med Virol87: 1072-1076.
- Alkan C, Bichaud L, de Lamballerie X, Alten B, Gould EA, et al. (2013) Sandfly-borne phleboviruses of Eurasia and Africa: Epidemiology, genetic diversity, geographic range, control measures. Antiviral Res 100: 54-74.
- Sabin AB (1951) Experimental studies on Phlebotomus (Pappataci, sandfly) fever during World War II. Arch Gesamte Virusfo rsch 4:367-410.
- Cohen D, Zaide Y, Karasenty E, Schwarz M, LeDuc JW, et al. (1999) Prevalence of antibodies to West Nile fever, Sandfly fever Sicilian, and Sandfly fever Naples viruses in healthy adults in Israel. Public Health Rev 27: 217-230.
- Collao X, Palacios G, de Ory F, Sanbonmatsu S, Perez-Ruiz M, et al. (2010) Granada virus: A natural phlebovirus reassortant of the sandfly fever Naples serocomplex with low seroprevalence in humans. Am J Trop Med Hyg 83: 760-765.
- Remoli ME, Fortuna C, Marchi A, Bucci P, Argentini C, et al. (2014) Viral isolates of a novel putative phlebovirus in the Marche Region of Italy. Am J Trop Med Hyg 90:760-763.
- Charrel RN,Moureau G, Temmam S, Izri A, Marty P, et al. (2009) Massilia virus, a novel Phlebovirus (Bunyaviridae) isolated from sandflies in the Mediterranean. Vector Borne Zoonotic Dis 9:519-530.
- Zhioua E, Moureau G, Chelbi I, Ninove L, Bichaud L, et al. (2010) Punique virus, a novel phlebovirus, related to sandfly fever Naples virus, isolated from sandflies collected in Tunisia. J Gen Virol 91: 1275-1283.
- Bartels S, de Boni L, Kretzschmar HA, Heckmann JG (2012) Lethal encephalitis caused by the Toscana virus in an elderly patient. J Neurol 259: 175-177.
- Braito A, Corbisiero R, Corradini S, Fiorentini C, Ciufolini M(1998) Toscana virus infections of the central nervous system in children: A report of 14 cases. J Pediatr 132: 144-148.
- Dionisio D, Valassina M, Ciufolini MG, Vivarelli A, Esperti F, et al. (2001) Encephalitis without meningitis due to sandfly fever virus serotype toscana. Clin Infect Dis 32: 1241-1243.
- Kay MK, Gibney KB, Riedo FX, Kosoy OL, Lanciotti RS, et al. (2010) Toscana virus infection in American traveler returning from Sicily, 2009. Emerg Infect Dis 16:1498-1500.
- Kuhn J, Bewermeyer H, Klosterkoetter UH, Emmerich P, Schilling S, et al. (2005) Toscana virus causing severe meningoencephalitis in an elderly traveller. J Neurol Neurosurg Psychiatry 76:1605-1606.
- Gamez SS, Perez-Ruiz M, Palop-Borras B, Navarro-Mari JM (2009) Unusual manifestation of toscana virus infection, Spain. Emerg Infect Dis 15: 347-348.
- Anagnostou V, Sdouga M, Volakli H, Violaki A, Papa A (2011) Phlebovirus meningoencephalis complicated by Pseudomonas aeruginosa pneumonia: A case report. Vector Borne Zoonotic Dis 11: 595-596.
- Epelboin L, Hausfater P, Schuffenecker I, Riou B, Zeller H, et al. (2008) Meningoencephalitis due to Toscana virus in a French traveler returning from central Italy. J Travel Med 15: 361-363.
- Baldelli F, Ciufolini MG, Francisci D, Marchi A, Venturi G, et al. (2004) Unusual presentation of life-threatening Toscana virus meningoencephalitis. Clin Infect Dis 38: 515-520.
- Charrel RN, Bichaud L, de Lamballerie X (2012) Emergence of Toscana virus in the mediterranean area. World J Virol 1: 135-141.
- Papa A, Mallias J, Tsergouli K, Markou F,Poulou A, et al. (2014) Neuroinvasive phlebovirus infection in Greece: A case report. Intervirology 57: 393-395.
- Gandacu D, Glazer Y, Anis E, Karakis I, Warshavsky B, et al. (2014) Resurgence of cutaneous Leishmaniasis in Israel, 2001-2012. Emerg Infect Dis 20: 1605-1611.
- Khatami A, Firooz A, Gorouhi F, Khamesiour A, Dowlati Y (2008) Cutaneous leishmaniasis. Lancet Infect Dis 8: 458.
- Orshan L (2011) A sharp increase in the natural abundance of sand flies in Kfar Adummim, Israel. J Vector Ecol 36 Suppl 1: S128-S131.
- Jacobson RL, Eisenberger CL, Svobodova M, Baneth G, Sztern J, et al. (2003) Outbreak of cutaneous Leishmaniasis in northern Israel. J Infect Dis 188: 1065-1073
- Cross ER, Newcomb WW, Tucker CJ (1996) Use of weather data and remote sensing to predict the geographic and seasonal distribution of Phlebotomus papatasi in southwest Asia. Am J Trop Med Hyg 54: 530-536.
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 3708
- [From(publication date):
March-2017 - Aug 28, 2025] - Breakdown by view type
- HTML page views : 2829
- PDF downloads : 879