Research Article Open Access
Sinogenic Complications Involving Orbit, Frontal Sinus, Anterior and Middle Cranial Fossa Treated Using Endoscopic Techniques
| Krzysztof Oles1*, Jacek Skladzien1, Joanna Leszczynska1, Krzysztof Bartus2 and Joanna Mika3 | |
| 1Department of Otolaryngology, Medical College Jagiellonian University, Poland | |
| 2Department of Cardiac and Vascular Surgery and Transplantology, The Institute of Cardiology, Medical College Jagiellonian University, John Paul II Hospital, Poland | |
| 3Department of Pain Pharmacology, Institute of Pharmacology, Krakow, Poland | |
| Corresponding Author : | Krzysztof Oles Department of Otolaryngology Head and Neck Surgery of the Jagiellonian University 31-531 Cracow Poland Tel: 0048124247900 Fax: 0048124247925 E-mail: olokrista@op.pl |
| Received June 22, 2015; Accepted October 17, 2015; Published October 27, 2015 | |
| Citation: Oles K, Skladzien J, Leszczynska J, Bartus K, Mika J (2015) Sinogenic Complications Involving Orbit, Frontal Sinus, Anterior and Middle Cranial Fossa Treated Using Endoscopic Techniques. J Neuroinfect Dis 6:189. doi:10.4172/2314-7326.1000189 | |
| Copyright: © 2015 Oles K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Neuroinfectious Diseases
Abstract
The purpose of this study was to determine the treatment modalities with sinogenic complications. We present a retrospective assessment of 11 patients who developed various types of complications, including an abscess within the temporal bone pyramid, frontal sinus and orbital mucocele, and a subperiosteal abscess with orbital apex syndrome. Three patients have suffered from decreased visual acuity of one eye during the course of chronic sinusitis. Six of the eleven patients had a history of earlier surgeries from external access sites. All patients were treated with Expanded Endonosal Approach at the Otolaryngology Clinic of the Jagiellonian University Medical College. Postoperative follow-up periods were 1 to 5 years. All patients were treated with empirical antibiotic therapy, glucocorticoids and antithrombotics during the peri- and postoperative periods. Postoperative improvement was observed in all patients. No orbital or neurological complications were observed due to the surgical procedure. Summing up, untreated chronic paranasal sinusitis may lead to severe orbital and intracranial complications. Transnasal endoscopy is the gold standard for the treatment of sinogenic complications.
| Keywords |
| Endoscopic sinus surgery; Skull base; Sinusitis complications; Mucopyocele; Orbital abscess |
| Introduction |
| Paranasal sinusitis is estimated to be the cause of up to 75% of bacterial infections in the orbit [1]. This infection rate occurs because paranasal sinuses are located in the direct vicinity of orbits. The estimated incidence of orbital sinogenic complications is 5-7% [1,2]. Cavernous sinus thrombophlebitis is a rare but serious sinogenic complication that is characterized by a high mortality of 20-30% [3,4]. Causes of sinusitis are either posttraumatic or iatrogenic. The portal of entry of infection includes venous vessels and natural bone defects. Conjunctival edema, exophthalmos and painful ophthalmoplegia are a triad of particularly acute symptoms. Particularly alarming symptoms include paresis and palsy of oculomotor nerves, retroocular pain, amblyopia leading to blindness, lack of pupillary light reflex, high body temperature and consciousness disturbances [3-5]. Laboratory analyses reveal positive blood cultures in 70% of cases [2-5].Timely diagnosis is crucial to prevent severe sinogenic complications. Sinogenic complications involving the frontal sinus, orbit and the anterior and middle cranial fossa are increasingly rare in the age of widespread antibiotic use and the systematically growing expertise of specialist physicians [2]. However, complications, including mucoceles and mucopyoceles within the frontoorbital region and the orbit itself and intracranial abscesses, remain a significant therapeutic challenge and contribute to the increase in patient mortality [1,6-8]. The most common locations of mucoceles include the frontal sinus (60-65%), followed by (20-30%), ethmoid (20-30%), maxilla (10%) and sphenoid sinus (2-3%) [1,6,7,9]. Mucosal hypertrophy, allergy, inflammations, injuries, fibrosis, scars, fibrous dysplasia and tumors may hamper ventilation and mucocilliary drainage. Mucus production followed by purulent superinfection leads to damage and a remodeling of bone walls, which increases symptoms of obstruction of the natural sinus outlets. A history of surgical procedures, cerebrocranial injuries, nasal polyps, and chronic sinusitis precede and cause secondary mucoceles [8,10,11]. We present a series of cases that were successfully treated in the Otolaryngology Clinic of the Jagiellonian University Medical College in Cracow using only endoscopic access sites. |
| Materials and Methods |
| Our retrospective analysis included 11 patients (10 males and 1 female) aged 16-77 years who were treated between 2009 and 2014. Subjects included orbital and intracranial complications due to sinusitis. All patients were treated at the Otolaryngology Clinic of the Jagiellonian University Medical College by Krzysztof Ole�. Postoperative followup periods were 1 to 5 years. Surgical procedures were performed under neuronavigation (DigiPointer, Collin, Poland). All patients were treated with empirical antibiotic therapy, glucocorticoids and antithrombotics during the peri- and postoperative periods. Clinical case summaries, radiological documentation, information on surgical access, histopathology results and treatment outcomes are presented. |
| Case reports |
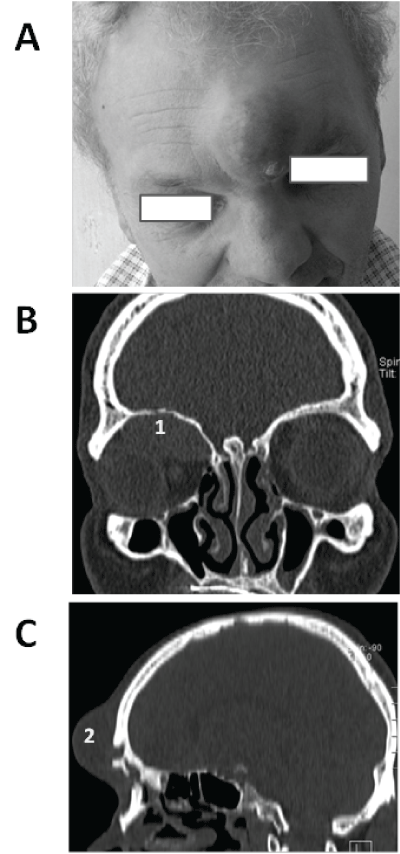
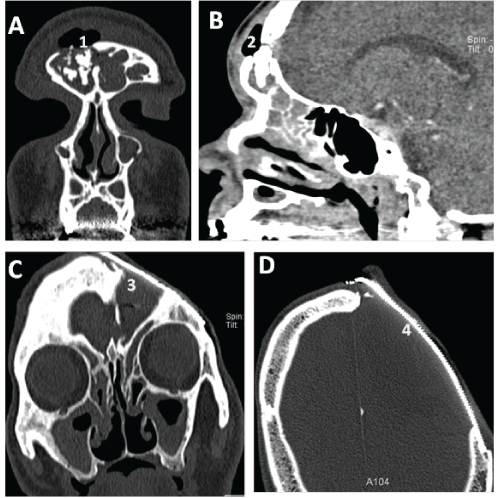
| Patient 1: A 56-year-old male who was admitted to the clinic due to an abscess within the right orbit accompanied by exophthalmos and double vision in all directions with symptoms of cerebrospinal meningitis. Patient had a history of severe cerebrocranial injury and craniotomy 3 years earlier. The patient was in severe condition on admission (Figure 1A). CT of paranasal sinuses revealed a significant asymmetry of eyeball positions (Figure 1B), exophthalmos of the right eye, intraorbital abscess, and Pott’s puffy tumor) (Figure 1C). ESS including evacuation of the orbital abscess within the retroocular space was performed. Exophthalmos resolved following recovery from anesthesia, and vision gradually improvement until a final and complete resolution. |
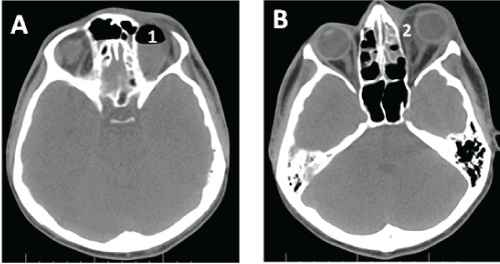
| Patient 2: A 20-year-old male who was admitted to the clinic with an abscess within the left orbit accompanied by exophthalmos and double vision in all directions. Ophthalmological examination 12 hours before the surgical procedure had confirmed sudden decreased visual acuity in the left eye. History included conservative treatment of sinusitis in the affected region. The patient was in a severe condition with symptoms of cavernous sinus involvement, and he underwent nighttime surgery in our clinic. CT of paranasal sinuses revealed an asymmetrical positioning of the eyeballs, exophthalmos of the left eye, retroocular gas within the left orbit, and an intraorbital abscess (Figure 2A and 2B). ESS including evacuation of the orbital abscess within the orbital apex was performed. Exophthalmos resolved following recovery from anesthesia, and vision gradually improved until a final and complete resolution. |
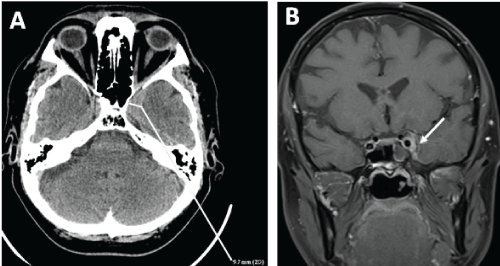
| Patient 3: A 42-year-old male who was admitted to the clinic because of a tumor within the sphenoid sinus with left cavernous sinus involvement. According to medical history he had suffered from decreased visual acuity of left eye for 4 weeks. The patient had also had a history of recurrent paranasal sinusitis subject to pharmacological treatment and hypothyroidism. Ophthalmological examination prior to admission revealed a disturbed mobility of the left eye, double vision in all directions, and decreased visual eye acuity. The general condition of the patient deteriorated during hospitalization and during the course of the diagnostic process, with upper eyelid ptosis and pulsatile exophthalmos of the left eyeball. CT of paranasal sinuses revealed the following levolateral lesions: asymmetrically dilated cavernous sinus, thickened oculomotor muscles, exophthalmos, thickened optic nerve in the orbital apex and widened superior and inferior orbital fissures (Figure 3A and 3B). The patient qualified for emergency surgery because of his deteriorating condition. Optic nerve decompression was performed with exposure of the medial wall of the left cavernous sinus. Exophthalmos gradually resolved during the first 24 hours after surgery, and the patient reported resolution of subjective pulsation within the orbit. Systematic improvement in his general condition started on day 3, which was accompanied by improvement in visual acuity and lead to complete visual recovery on day 7. Complete resolution of complaints, including ptosis of the upper left eyelid, was observed. No relapses were reported during the two-year follow-up period. The function of the visual organ remains normal. |
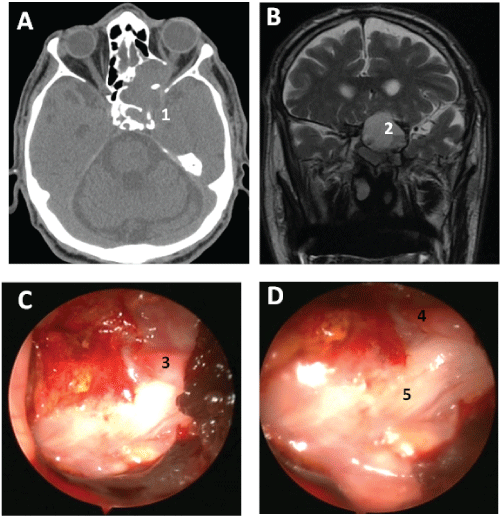
| Patient 4: A 77-year-old male who was admitted to the clinic because of a tumor within the left sphenoid sinus and temporal bone pyramid apex and according to medical history he had suffered from decreased visual acuity of left eye for 2 months. The patient was referred to the clinic from the Department of Ophthalmology who was diagnosed with optic nerve atrophy and left eye exophthalmos. CT of the sinuses revealed a tumor within the sphenoid sinus that involved the apex of the temporal bone pyramid. The tumor was in direct contact with the optic nerve in the intracranial segment to the optic nerve junction (Figure 4A and 4B). A surgical procedure was performed because of the increasing incidence of short-term lapses of consciousness, transient amblyopia within the functional eye and symptoms of involvement of the apex of the temporal bone pyramid. Endoscopic removal of a skull base tumor was performed. An exposed internal carotid artery without a bone canal within the paraclival segment and a largely exposed optic nerve that was impinged by the tumor all the way to the optic nerve junction were revealed intraoperatively (Figures 4C,4D and 5). S. aureus was cultured from the material collected during surgery. Intravenous targeted antibiotic (vancomycin and meropenem) and antithrombotic therapies at maximum doses per kg of body weight were initiated. The patient “was able to count his fingers” using decreased visual acuity of his eye 48 hours after surgery. Follow-up ophthalmological examination confirmed a marked improvement in the function of the left eye. Histopathological examination confirmed chronic inflammation. |
| Results |
| Some patients were subjected to CT and MRI scans prior to surgery, and ophthalmological examinations were performed in each patient. The 11 patients were treated using ESS for sinogenic complications that affected the frontal and sphenoid sinus, orbits and/ or anterior and middle cranial fossa. Three patients (Table 1, patients 3, 4, and 10) with subperiosteal orbital abscesses presented with orbital apex syndrome symptoms that required decompression of the optic nerve. One patient (Table 1, patient 3) presented with symptoms of cavernous sinus thrombosis. All patients had a history of chronic sinusitis, and 4 patients also had a history of neurosurgical procedures (Table 1, patients 1, 5, 6, and 7). Two patients (Table 1, patients 9 and 11) had undergone laryngological procedures from external access points, and the authors subsequently treated these patients using only laparoscopic procedures. The average latency period between the primary surgery and the development of complications was 2 years. All patients had defects in skeletal constrains of either the orbit or skull base, and they were treated intranasally using endoscopic methods (Table 1). All patients reported postoperative improvements in their general condition and ocular function. Postoperative CT and MRI scans correlated with patient-reported subjective improvements. Follow-up imaging studies revealed no relapses of the primary disease. Methicillin-resistant Staphylococcus aureus and Streptococcus viridans were encountered in microbial examination results. Empirical broadspectrum antibiotic therapy was administered postoperatively for 2-3 days, followed by targeted antibiotic treatment. |
| Discussion |
| Recently, intranasal endoscopic techniques have replaced conventional external access surgeries. ESS is an efficient and safe alternative for the treatment of sinogenic complications of the orbital apex and the vicinity of frontal and sphenoid sinuses [2,12]. Initial symptoms are usually discrete and non-characteristic. However, impingement of critical neurovascular structures leads to an infection or mass effect, including breakage of the intracranial barrier and serious neurological consequences [10]. Severe symptoms develop only upon expansion into critical structures, including the orbit and intracranial structures [13,14]. It is absolutely crucial to monitor the ophthalmological conditions of the patient (visual acuity, color vision, and pupillary light reflexes) every 4 hours [10,15,16]. |
| Extended endoscopic access, including Draf III, was used when radiological examinations revealed defects in the skull base bone framework. The design of surgical procedures included the possibility of using external access, but none of these possible procedures was used in the reported cases. Cerebral meninges were separated from the surrounding bone, abscesses were drained, and the surgical fields were flushed with physiological saline. Intracranial endoscopic examination was performed to ensure no further purulent processes developed intracranially. |
| Patients often remained asymptomatic until they experienced sudden orbital or intracranial symptoms. Headache was the most commonly reported symptom, and it was also accompanied by exophthalmos, retroocular pain, double vision and disturbed visual acuity [10,15]. Orbital symptoms are present in 70% of frontoethmoidal locations of inflammatory lesions [11]. Nasal obstruction may accompany other diseases in other sinus disorders. Physical examination may be unremarkable or reveal tension and hyperesthesia of the frontal region, orbital region edema, exophthalmos, visual acuity disturbances and restricted eyeball mobility, less commonly. Endoscopic examination of nasal cavity may be unremarkable or confirm the presence of secretion and mucosal swelling [10,15]. CT and MRI scans in sagittal and coronary planes facilitate determinations of shape, size, location and pathology extent. The affected sinuses and their skeletal framework usually present with thinning or defects accompanied by translocations of adjacent structures, including neural and vascular structures [15,17]. The type of surgical access depends on the location, extent and accompanying complications and physicians should consider maximum lesion exposure and cosmetic optimization of the procedure. Purulent conditions may affect multiple critical structures in special cases, particularly the orbit, frontal sinus, anterior and middle cranial fossa, orbital apex, cavernous sinus and temporal bone pyramid. Possible treatments of perioperative complications include cerebrospinal fluid leak management, optic nerve decompression and tumor removal. The lateral orbital compartment and some skull base regions may be inaccessible despite the use of angular optics and appropriate surgical instruments. |
| External access points are still used, but the development of advanced endoscopic techniques and the availability of extensive instrumentation make transnasal surgery a more efficient and less invasive treatment method. The effects of this technique are satisfying, and the relapse rate, estimated at 0.9-17%, is lower [1]. The open removal of mucosa that is adjacent to the meninx is usually not necessary if the operated lesion is not a malignant tumor, which avoids the risk of complications. However, open transcranial access may be required in cases of intracranial locations of the pathology. Limited craniotomy may be required in cases of more lateral or more posterior lesion advancement [18]. If the pathological process or surgery damages the meninx, primary management is required using techniques that are recommended for the management of cerebrospinal fluid leaks. Multilayered techniques were used for the reconstruction of skull base defects. Emergency surgical intervention is required to prevent neurological consequences in rare cases of increasing risks to life or the complications that accompany the inflammatory process, including orbital or cerebral abscesses and cerebrospinal meningitis. Long-term follow-up is required. No major postoperative complications were observed in the 11 patients subjected to ESS treatment. Radiological follow-up is required at least once every two years [9]. ESS provides a valuable and state of the art method for the treatment of sinogenic orbital complications in well-selected patients. |
| Conclusions |
| 1. ESS is a safe and efficient method for the treatment of sinogenic complications involving the orbit, frontal sinus, sphenoid sinus and the anterior and middle cranial fossa. |
| 2. Sinogenic complications should be differentiated from orbital tumors. |
| 3. Transnasal endoscopy is the gold standard for the treatment of sinogenic complications, but open access surgeries play an important role in cases of advanced complications, including intracranial complications. |
| Acknowledgement |
| This research was supported by statutory funds of the Department of Otolaryngology of the Jagiellonian University, Krakow, Poland. |
References
- Aggarwal SK, Bhavana K, Keshri A, Kumar R, Srivastava A (2012) Frontal sinus mucocele with orbital complications: Management by varied surgical approaches. Asian J Neurosurg. 7:135-140
- Lim JH, Sardesai MG, Ferreira M Jr, Moe KS (2012) Transorbitalneuroendoscopic management of sinogenic complications involving the frontal sinus, orbit, and anterior cranial fossa. J NeurolSurg B Skull Base 73: 394-400.
- Ebright JR, Pace MT, Niazi AF (2001) Septic thrombosis of the cavernous sinuses. Arch Intern Med 161: 2671-2676.
- Kojan S, Al-Jumah M. (2006) Infection related cerebral venous thrombosis. J Pak Med Assoc 56: 494-497
- Berdai AM, Shimi A, Khatouf M (2013) Cavernous sinus thrombophlebitis complicating sinusitis. Am J Case Rep 14: 99-102
- Borkar S, Tripathi AK, Satyarthee G, Sharma BS, Mahapatra AK (2008) Frontal mucocele presenting with forehead subcutaneous mass: an unusual presentation. Turk Neurosurg 18: 200-203.
- Kamoshima Y, Terasaka S, Nakamaru Y, Takagi D, Fukuda S, et al. (2012) Giant frontal mucocele occurring 32 years after frontal bone fracture: a case report. Case Rep Neurol 4: 34-37
- Ichimura K, Ohta Y, Maeda YI, and Sugimura H. (2001) Mucoceles of the paranasal sinuses with intracranial extension-postoperative course. Am J Rhinol 15:243-247
- Devars du Mayne M, Moya-Plana A, Malinvaud D, Laccourreye O, Bonfils P. (2012) Sinus mucocele: natural history and long-term recurrence rate. Eur Ann Otorhinolaryngol Head Neck Dis. 129: 125-130
- Lee JT, Brunworth J, Garg R, Shibuya T, Keschner DB, et al. (2013) Intracranialmucocele formation in the context of longstanding chronic rhinosinusitis: A clinicopathologic series and literatur� review. Allergy Rhinol (Providence). 4: e166-75.
- Obeso S, Llorente JL, Díaz-Molina JP, Sánchez-Fernández R, Rodrigo JP, et al. (2009) Paranasal sinus mucoceles. Our experience in 72 patients. Acta Otorrinolarigol 60: 332-339
- Page EL, Wiatrak BJ. (1996) Endoscopic vs external drainage of orbital subperiosteal abscess. Arch Otolaryngol Head Neck Surg 122: 737-774
- Timperley D, Banks C, Robinson D, Roth J, Sacks R, et al. (2011) Lateral frontal sinus access in endoscopic skull-base surgery. Int Forum Allergy Rhinol 1: 290-295.
- Becker SS, Bomeli SR, Gross CW, Han JK. (2006) Limits of endoscopic visualization and instrumentation in the frontal sinus. Otolaryngol Head Neck Surg 135: 917-921.
- Weitzel EK, Hollier LH, Calzada G, Manolidis S. (2002) Single stage management of complex fronto-orbital mucoceles. J Craniofacial Surg 13: 739-745.
- Delfini R, Missori P, Iannetti G, Ciappetta P, Cantore G. (1993) Mucoceles of the paranasal sinuses with intracranial and intraorbital extension: Report of 28 cases. Neurosurgery 32: 901-906.
- Har-El G. (2001) Endoscopic management of 108 sinus mucoceles. Laryngoscope 111:2131-2140.
- Patel RS, Yousem DM, Maldjian JA, Zager EL (2000) Incidence and clinical significance of frontal sinus or orbital entry during pterionalfrontotemporal) craniotomy. AJNR Am J Neuroradiol 21: 1327-1330.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Bacteria Induced Neuropathies
- Blood-brain barrier
- Brain Infection
- Cerebral Spinal Fluid
- Encephalitis
- Fungal Infection
- Infectious Disease in Children
- Neuro-HIV and Bacterial Infection
- Neuro-Infections Induced Autoimmune Disorders
- Neurocystercercosis
- Neurocysticercosis
- Neuroepidemiology
- Neuroinfectious Agents
- Neuroinflammation
- Neurosyphilis
- Neurotropic viruses
- Neurovirology
- Rare Infectious Disease
- Toxoplasmosis
- Viral Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 11662
- [From(publication date):
December-2015 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 10512
- PDF downloads : 1150
